Published online Apr 27, 2025. doi: 10.4240/wjgs.v17.i4.102020
Revised: January 20, 2025
Accepted: February 13, 2025
Published online: April 27, 2025
Processing time: 174 Days and 15.7 Hours
Esophageal and gastric variceal bleeding is a catastrophic complication of portal hypertension, most commonly caused by cirrhosis of various etiologies. Although a considerable body of research has been conducted in this area, the complexity of the disease and the lack of standardized treatment strategies have led to frag
To evaluate research trends and advancements in esophagogastric variceal bleeding (EGVB) over the past twenty years.
Relevant publications on EGVB were retrieved from the Web of Science Core Collection. VOSviewer, Pajek, CiteSpace, and the bibliometrix package were then employed to perform bibliometric visualizations of publication volume, countries, institutions, journals, authors, keywords, and citation counts.
The analysis focused on original research articles and review papers. From 2004 to 2023, a total of 2097 records on EGVB were retrieved. The number of relevant publications has increased significantly over the past two decades, especially in China and the United States. The leading contributors in this field, in terms of countries, institutions, authors, and journals, were China, Assistance Publique-Hôpitaux de Paris, Bosch Jaime, and World Journal of Gastroenterology, respectively. Core keywords in this field include portal hypertension, management, liver cirrhosis, risk, prevention, and diagnosis. Future research directions may focus on optimizing diagnostic methods, personalized treatment, and multidisciplinary collaboration.
Using bibliometric methods, this study reveals the developmental trajectory and trends in research on EGVB, underscoring risk assessment and diagnostic optimization as the core areas of current focus. The study provides an innovative and systematic perspective for this field, indicating that future research could center on multidisciplinary collaboration, personalized treatment approaches, and the development of new diagnostic tools. Moreover, this work offers practical research directions for both the academic community and clinical practice, driving continued advancement in this domain.
Core Tip: This study provides a comprehensive analysis of research trends in esophagogastric variceal bleeding over the past two decades through bibliometric methods. By systematically reviewing a wide range of publications, it identifies key areas of focus, particularly in risk assessment and diagnosis, which are crucial for advancing clinical decision-making. Additionally, the findings highlight the importance of emerging technologies and innovative approaches in the management of this condition. Future research directions may focus on optimizing diagnostic techniques, personalized treatment strategies, and fostering multidisciplinary collaboration to improve patient outcomes and enhance understanding of esophagogastric variceal bleeding.
- Citation: Wang DX, Wu XJ, Yu JZ, Zhan JY, Xing FF, Liu W, Chen JM, Liu P, Liu CH, Mu YP. Visualizing global progress and challenges in esophagogastric variceal bleeding. World J Gastrointest Surg 2025; 17(4): 102020
- URL: https://www.wjgnet.com/1948-9366/full/v17/i4/102020.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v17.i4.102020
Esophagogastric variceal bleeding (EGVB) is a severe complication arising from various forms of portal hypertension (PH), with liver cirrhosis being the most frequent underlying cause[1]. Liver cirrhosis ranks as the 11th most common cause of death globally and the 3rd leading cause of mortality among individuals aged 45-64, accounting for approximately one million deaths annually; it affects men and women at a ratio of 6:4[2]. In addition to liver cirrhosis, noncirrhotic PH (NCPH), including conditions such as portosinusoidal vascular liver disease and portal vein thrombosis (PVT), can also result in EGVB[3]. In patients with cirrhosis, the incidence of esophageal and gastric varices (GV) is approximately 50%, with 10%-30% of these patients experiencing EGVB each year. The mortality rate for the first bleeding episode ranges from 20% to 35%, and the six-week mortality rate can reach 15%-20%. EGVB is extremely severe and, if not promptly and effectively controlled, can lead to serious clinical consequences[4]. However, for EGVB patients, conventional treatment methods are often unable to reverse the pathological basis of portal vein blood flow obstruction[5], which continues to pose significant challenges for the prevention and management of EGVB.
These challenges are reflected not only in the complexity of clinical treatments but also in the current state of research in this field. In recent years, research on EGVB has gradually increased, but the fragmentation and complexity of the literature make it difficult for researchers to comprehensively grasp the progress of EGVB studies. These studies predominantly focus on specific etiologies, treatment methods, or clinical manifestations, yet they lack a systematic perspective to integrate existing findings, thereby failing to reveal the main directions and potential gaps in EGVB research.
Bibliometric methods, which employ mathematical and statistical techniques for qualitative and quantitative analysis of publications, can objectively provide a unique perspective that comprehensively highlights the current state of EGVB research and reveals the context of related studies. These methods not only enable researchers to identify the countries or regions, institutions, and authors from which the publications originate but also allow for the summarization and categorization of the research status, publication trends, future research hotspots, academic frontiers, and knowledge maps in this field, which holds significant value. Furthermore, bibliometric analysis has been widely applied in research related to liver disease, including liver fibrosis[6,7] and liver cirrhosis[8,9]. However, no such studies have been identified in the field of EGVB. Therefore, this study employs bibliometric analysis methods to comprehensively summarize and review the research status of EGVB over the past two decades for the first time. This approach is expected to help researchers and clinicians gain a better understanding of the current state of EGVB research and to identify new directions for future studies.
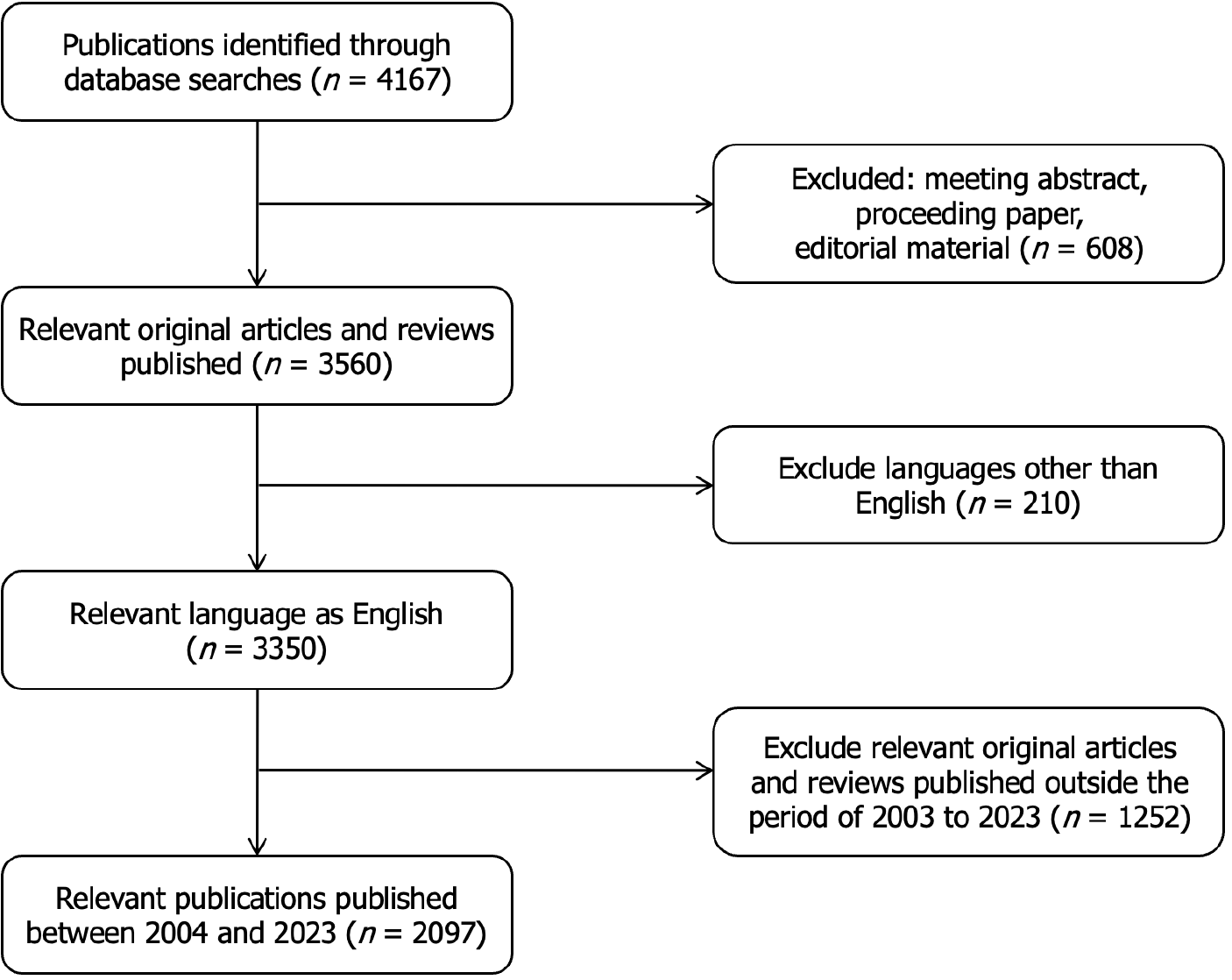
The literature search was performed on June 25, 2024, at the Affiliated Shuguang Hospital of Shanghai University of Traditional Chinese Medicine, utilizing the Web of Science Core Collection (WoSCC). As one of the most comprehensive and authoritative databases, WoSCC is especially well-suited for conducting bibliometric analyses in the fields of natural sciences and medicine. Our search strategy included: Topic = “esophagogastric variceal bleeding” or “esophageal variceal bleeding” or “esophageal gastric variceal bleeding” or “esophageal varices bleeding” or “esophagogastric varices bleeding” or “stomach esophagus varicosity burst hemorrhage” or “esophageal gastric varices bleeding” or “gastroesophageal variceal hemorrhage” or “esophagogastric variceal hemorrhage”. The WoSCC was selected as the database, with the search covering the period from January 1, 2004, to December 31, 2023. Only original research articles and review papers were included, and the language was restricted to English. Articles published before January 1, 2004, were excluded. Furthermore, conference abstracts, proceedings papers, editorials, and other article types were also excluded. Figure 1 presents a flowchart detailing the search strategy employed in this study.
The bibliographic data retrieved through the query was downloaded from the WoSCC on June 25, 2024. Detailed information, including authors, titles, sources, sponsors, citation counts, accession numbers, abstracts, addresses, document types, and references, was downloaded in TXT format for subsequent analysis. The h-index of the top 10 most prolific authors was obtained from the Web of Science platform. Additionally, the 2023 impact factor (IF) and Journal Citation Report category quartile for 2023 of the top 10 core journals in EGVB research were extracted from Web of Science.
This study employed various tools for statistical analysis, including VOSviewer (version 1.6.18), Pajek (version 5.17), CiteSpace (version 6.2.R6), and the Bibliometrix R package (version 4.1.4, running on R version 4.3.3). Information related to authors, institutions, countries, and journals was collected and processed using these tools. Parameters such as the number of articles, IF, centrality, and burst citations/occurrences were analyzed. Productivity was assessed by the number of published articles, enabling the identification of prolific individuals or institutions. The IF was used to gauge the global influence of journals, with data sourced from the 2023 journal citation reports. VOSviewer, a software tool designed for constructing and visualizing bibliometric networks, was employed to analyze collaborative relationships among countries, authors, and institutions, as well as to assess keyword co-occurrence patterns. In addition, VOSviewer, combined with Pajek software, was used for the visualization of author keyword analysis[10]. CiteSpace, a widely-used visualization tool for trend and hotspot research, was employed to conduct burst detection analysis and timeline visualization of keyword clusters[11]. Bibliometrix, an open-source tool based on the R programming language, was used to visualize country collaboration maps[12].
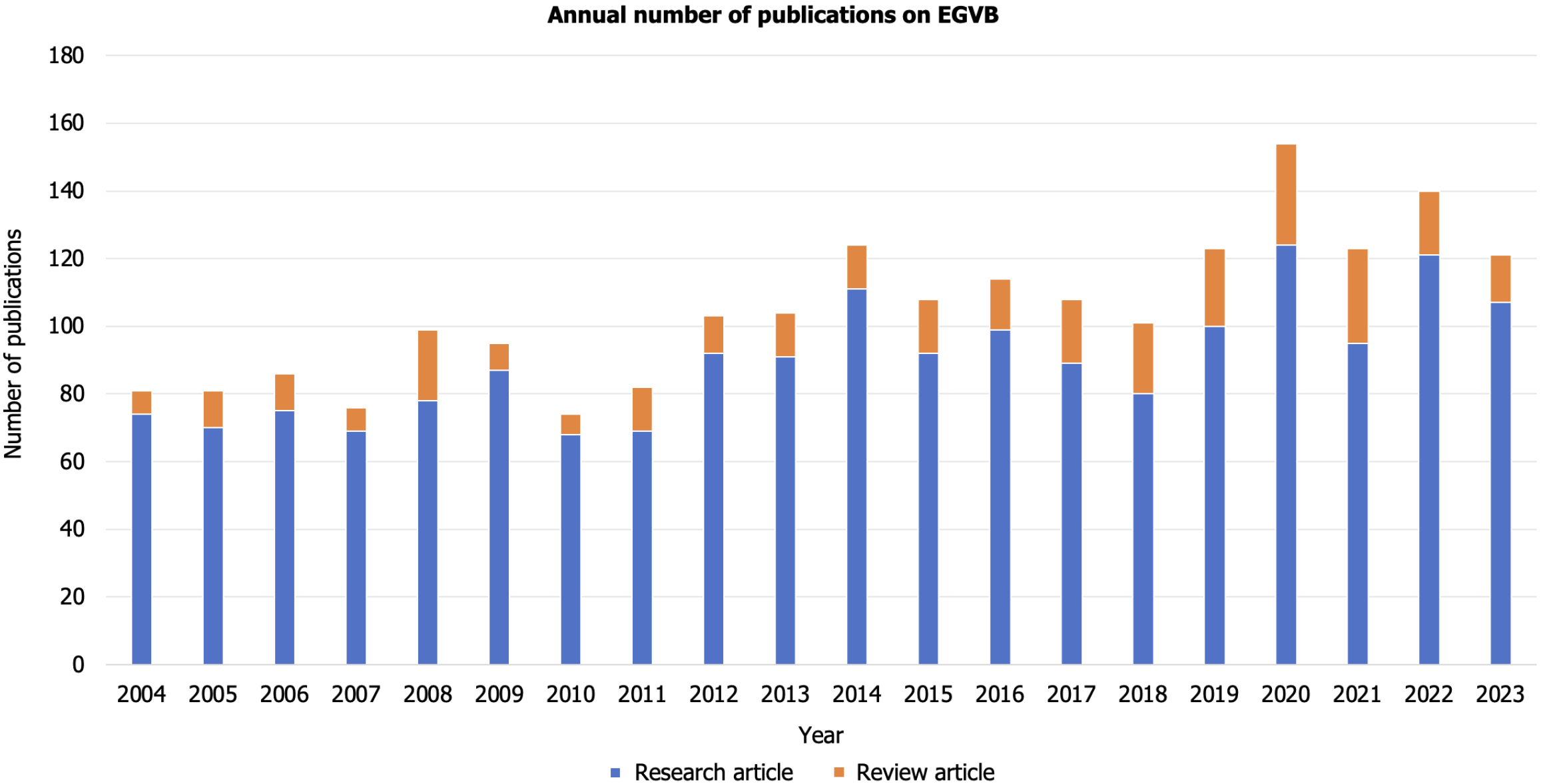
Overall, 2097 articles related to EGVB were identified in the WoSCC database between 2004 and 2023, comprising 1791 original articles and 306 reviews. Figure 2 displays the annual number of publications on EGVB, revealing a steady increase in research activity in this field, consistent with the general growth pattern of scientific literature. Compared to other fields, such as liver cirrhosis and its associated immunological factors where publication trends are surging, research in the EGVB field has been growing progressively. Despite causing significant clinical consequences, this area currently does not receive adequate attention. Moreover, the number of high-impact journals and their IFs in the EGVB field have not yet reached the level of specialized and mature research areas seen in other disciplines, indicating that research in this field remains to be fully explored[8,9].
As presented in Table 1, the frequency analysis of countries/regions from 2004 to 2023 indicates that China and the United States are the dominant contributors to EGVB research. The major research hubs are located in Asia, Europe, and North America. It can be observed that the majority of research on EGVB originates from the world’s two largest economies, China and the United States. This also indicates that studying EGVB requires substantial funding and talent. Adequate research funding support and robust infrastructure are more conducive to EGVB research. Among the main sponsors are the National Natural Science Foundation of China and the National Institutes of Health of the United States. Besides China and Iran, most of the countries conducting research in this field are developed nations, suggesting that developing countries have started their research in this area relatively late. Based on a comprehensive analysis of publishing institutions and countries, the most authoritative and central countries and institutions are concentrated in China and the United States. Although China began later than the United States, it has already become a world leader in this research field through strong investments in capital and talent.
| Rank | Country/region | Count | Institution | Count | Author | Count | Journal | Count | 2023 IF/JCR partition |
| 1 | China | 1638 | Univ Barcelona | 43 | Bosch Jaime | 31 | World Journal of Gastroenterology | 115 | Q1/4.30 |
| 2 | United States | 1391 | Capital Med Univ | 42 | Abraldes Juan g | 17 | Journal of Gastroenterology and Hepatology | 61 | Q2/3.70 |
| 3 | Japan | 782 | Mayo Clin, Natl Yang Ming Univ | 34 | Berzigotti Annalisa | 12 | European Journal of Gastroenterology & Hepatology | 56 | Q3/2.30 |
| 4 | South Korea | 644 | Univ Milan | 33 | Garcia-Tsao Guadalupe | 11 | Gastrointestinal Endoscopy and Medicine | 46 | Q1/6.70, Q2/1.30 |
| 5 | Australia | 540 | Shandong Univ | 28 | Carlos Garcia-Pagan Juan | 11 | Journal of Clinical Gastroenterology | 44 | Q2/2.80 |
| 6 | Italy | 369 | Hosp Clin Barcelona | 27 | Tripathi Dhiraj | 10 | Digestive Diseases and Sciences | 43 | Q2/2.50 |
| 7 | United Kingdom | 273 | Fudan Univ | 26 | Garcia-Pagan Juan Carlos | 7 | American Journal of Gastroenterology, Hepatology | 40 | Q1/8.00, Q1/12.90 |
| 8 | Belgium | 263 | Yonsei Univ | 24 | Stanley Adrian j | 5 | Journal of Pediatric Gastroenterology and Nutrition | 37 | Q1/2.40 |
| 9 | Iran | 259 | Taipei Vet Gen Hosp, Yale Univ | 23 | Patch David | 5 | Journal of Hepatology | 35 | Q1/26.80 |
| 10 | Germany | 221 | Chang Gung Univ | 22 | Hayes Peter c. | 5 | Endoscopy, BMC Gastroenterology | 31 | Q1/11.50, Q2/2.50 |
The University of Barcelona and Capital Medical University emerge as the most prominent institutions, exhibiting the highest levels of collaboration in EGVB research. The top author with the most publications is Bosch, Jaime from the University of Barcelona, followed by Abraldes Juan G, and Berzigotti Annalisa. Nine out of the top ten authors are from Spain and the United Kingdom. The three leading journals are World Journal of Gastroenterology, Journal of Gastroenterology and Hepatology, and European Journal of Gastroenterology and Hepatology, collectively publishing 508 papers. These journals are predominantly focused on gastroenterology, hepatology, and endoscopy, with some general medical journals also included.
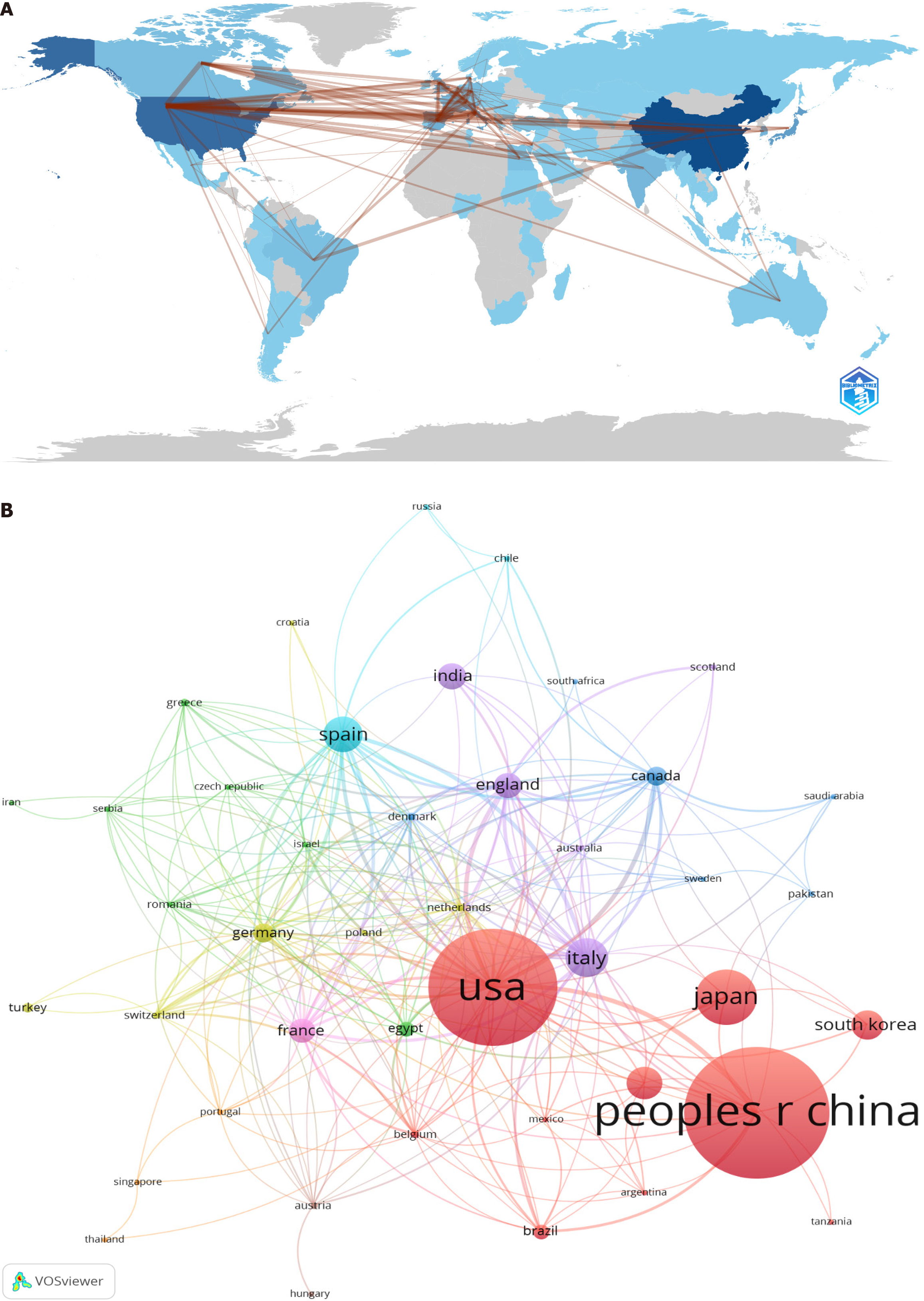
A total of 192 authors from 43 countries or regions have published 2097 articles. As shown in Figure 3, the United States and China have the highest number of collaborations, and the United States also maintains close collaborative relationships with Spain, Italy, and France. For these 200 institutions and 190 authors, the total strength of their collaborations with other organizations or authors will be calculated, selecting those organizations and authors that exhibit the highest link strength in the collaboration network, i.e., the most “active” organizations and authors. A basic manifestation of collaboration centrality is the size of the nodes. Typically, nodes with higher centrality (i.e., authors, institutions, or countries that collaborate frequently) are displayed as larger nodes. VOSviewer automatically adjusts the node size based on collaboration frequency or the number of “connections” in the network. Larger nodes usually represent researchers, institutions, or countries that hold more important positions in the collaboration network.
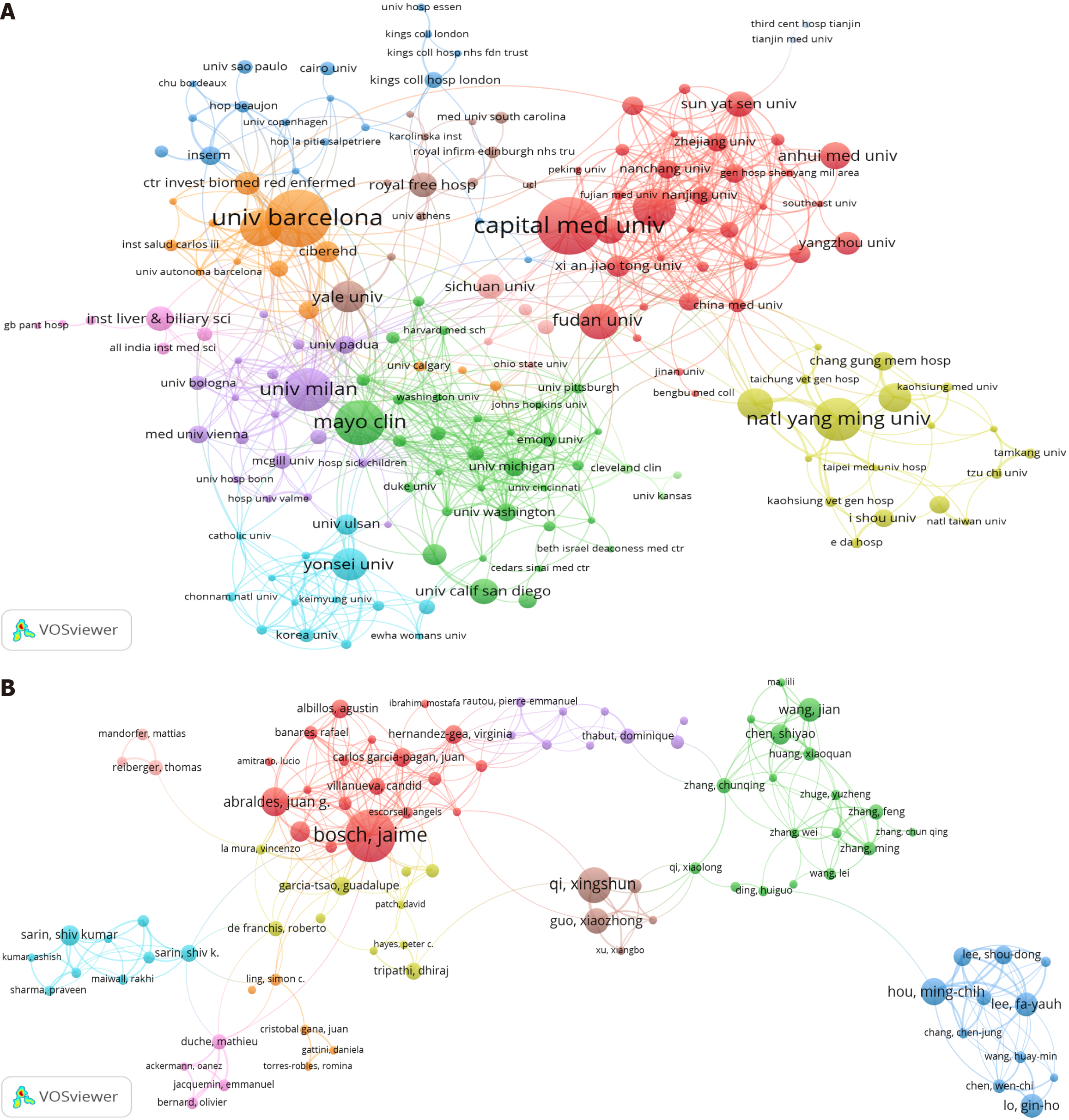
In terms of institutions, Figure 4 identifies six collaborative clusters among the institutions, with the University of Barcelona exhibiting the highest level of collaboration centrality, followed by the University of Milan and Hospital Clínic Barcelona (Figure 4A). Collaboration among authors is relatively close, with five clusters emerging (Figure 4B). Bosch, Jaime demonstrates the highest level of collaboration centrality, followed by Abraldes, Juan G, Carlos Garcia-Pagan, Juan, and Berzigotti, Annalisa.
As shown in Table 2, the most cited article is the 2017 guideline by the American Association for the Study of Liver Diseases (AASLD), authored by Garcia-Tsao et al[13] and published in Hepatology, with 1242 citations. The guideline offers evidence-based recommendations for the risk stratification, diagnosis, and management of PH in patients with liver cirrhosis. It emphasizes the use of non-invasive tools, such as transient elastography (TE), for diagnosing clinically significant PH (CSPH) and esophagogastric varices (EGV). Additionally, it advocates for the use of non-selective beta-blocker (NSBB), particularly carvedilol, as the first-line therapy for managing PH[13].
| Rank | Year | Title | Journal | First author | Citations |
| 1 | 2017 | Portal hypertensive bleeding in cirrhosis: Risk stratification, diagnosis, and management: 2016 practice guidance by the American Association for the Study of Liver Diseases | Hepatology | Garcia-Tsao Guadalupe | 1242 |
| 2 | 2006 | Diagnosis of cirrhosis by transient elastography (fibroscan): A prospective study | Gut | Foucher J | 989 |
| 3 | 2004 | Risk factors and clinical presentation of portal vein thrombosis in patients with liver cirrhosis | Journal of Hepatology | Amitrano L | 382 |
| 4 | 2015 | UK guidelines on the management of variceal haemorrhage in cirrhotic patients | Gut | Tripathi Dhiraj | 371 |
| 5 | 2004 | Influence of portal hypertension and its early decompression by tips placement on the outcome of variceal bleeding | Hepatology | Monescillo A | 341 |
| 6 | 2006 | Hepatic vein pressure gradient reduction and prevention of variceal bleeding in cirrhosis: A systematic review | Gastroenterology | D’Amico Gennaro | 339 |
| 7 | 2014 | Competing risks and prognostic stages of cirrhosis: A 25-year inception cohort study of 494 patients | Alimentary Pharmacology and Therapeutics | D’Amico G | 315 |
| 8 | 2005 | Systematic review: The model for end-stage liver disease - should it replace Child-Pugh’s classification for assessing prognosis in cirrhosis? | Alimentary Pharmacology and Therapeutics | Cholongitas E | 312 |
| 9 | 2015 | Causes and consequences of portal vein thrombosis in 1243 patients with cirrhosis: Results of a longitudinal study | Hepatology | Nery Filipe | 294 |
| 10 | 2011 | Best practice guidance for the diagnosis and management of cystic fibrosis-associated liver disease | Journal of Cystic Fibrosis | Debray Dominique | 273 |
The guideline was updated in 2023, with several significant revisions. It now incorporates systematic reviews, evidence quality assessments, and stronger recommendations based on recent research. The updates also include new dosing guidelines for carvedilol to address non-liver-related conditions. Furthermore, the updated guideline establishes a hepatic venous pressure gradient (HVPG) of ≥ 10 mmHg as the diagnostic threshold for CSPH. These additional recommendations are grounded in the latest research, making the guideline more authoritative and applicable in clinical practice[14].
Foucher et al[15] published a prospective study in Gut in 2006 on the application of FibroScan technology for the diagnosis of liver cirrhosis. Over the subsequent two decades, TE has been widely applied in the field of EGVB and has been incorporated into the Baveno VI consensus[15]. As a non-invasive method, TE demonstrates a strong correlation with liver stiffness measurement (LSM) and HVPG. However, it cannot fully replace HVPG measurement or upper gastrointestinal endoscopy, which remain the “gold standards” for evaluating EGV[16].
Amitrano et al[17] investigated the occurrence of PVT in patients with liver cirrhosis and found that PVT is not uncommon among these patients. PVT may present as asymptomatic or with severe symptoms, such as bleeding due to PH or intestinal infarction. Although clinical manifestations are diverse, only the prothrombin gene 20210 mutation showed a significant independent association with PVT, suggesting that this gene mutation may be an important risk factor[17]. The Liver Department of the British Society of Gastroenterology led the development of the “United Kingdom Guidelines On The Management Of Variceal Haemorrhage In Cirrhotic Patients”, which focuses on the management of variceal bleeding in patients with liver cirrhosis. This guideline replaces the older version published in 2000, reflecting the latest medical practices and research findings. It primarily includes primary prevention, management of acute variceal bleeding (AVB), secondary prevention, and treatment of GV, but does not address the management of underlying liver diseases or the treatment of variceal bleeding in pediatric patients[18].
Monescillo et al[19] explored the impact of PH and early decompression through Transjugular Intrahepatic Portosystemic Shunt (TIPS) on patients with variceal bleeding. The study measured HVPG in 116 cases of AVB patients and found that high-risk patients who underwent TIPS treatment had significantly reduced rates of treatment failure, transfusion requirements, and intensive care unit admissions, along with lower one-year mortality rates. The results indicate that early measurement of HVPG and timely application of TIPS are crucial for high-risk patients, as they can improve treatment outcomes and survival rates[19].
D’Amico et al[20] systematically evaluated the impact of reducing the HVPG on variceal bleeding in patients with liver cirrhosis. The results indicated that lowering HVPG to 12 mmHg or achieving a reduction of more than 20% from baseline significantly decreased the risk of bleeding and, when reduced by 20%, significantly lowered mortality rates. Additionally, the study discussed the heterogeneity between different reduction targets, emphasizing the importance of applying these hemodynamic goals in clinical practice. Furthermore, based on a 25-year cohort study involving 494 patients, the research explored the competing risks and prognostic stages of liver cirrhosis, finding that various competing mortality risks are prevalent among patients. By stratifying patients based on risk factors (ascites, bleeding, jaundice, or encephalopathy), their prognosis can be better assessed, and targeted treatment plans can be developed. The authors noted that future research should focus on how to effectively implement these risk assessment models in clinical practice[20].
Cholongitas et al[21] examined the effectiveness of the Model for End-Stage Liver Disease (MELD) score compared to the Child-Turcotte-Pugh (CTP) score in prognostically evaluating patients with liver cirrhosis outside of transplant settings. With the emergence of new therapies, the prognosis of liver cirrhosis patients has attracted widespread attention. The MELD score is currently used to allocate patients on the liver transplant waiting list, but its effectiveness in other contexts remains controversial. In studies involving 1360 patients with liver cirrhosis, only five indicated that the MELD score was superior to the CTP score in predicting 3-month mortality, while there was no significant difference in predicting 12-month mortality. A study involving 2569 patients showed no significant difference between short-term and long-term prognostic scores. In a study of 411 Liver cirrhosis patients with variceal bleeding, there was also no difference in prognostic performance between the MELD and CTP scores. According to existing literature, in non-transplant settings, the MELD score does not outperform the CTP score. Further evaluation of the modified CTP score and the MELD score is necessary to determine their applications in clinical practice[21].
PVT in liver cirrhosis may be a cause or a consequence of disease progression. The study analyzed 1243 patients with liver cirrhosis without PVT, with a follow-up period of 47 months. It was found that the cumulative incidence of PVT was 10.7%, and its occurrence was significantly associated with baseline esophageal varices (EV) and prothrombin time, but not with recent progression of liver disease. The conclusion indicates that in patients with liver cirrhosis, the development of PVT reflects the severity of liver disease but does not lead to further progression of the disease[22].
After conducting an in-depth analysis of the literature related to liver cirrhosis and PH, we can extract several important clinical insights from the highly cited papers. First, the most frequently cited studies indicate that early assessment using non-invasive detection techniques, such as TE (FibroScan) and HVPG, holds significant value for risk stratification and management of patients with liver cirrhosis. These techniques are particularly valuable in providing crucial guidance for monitoring variceal bleeding and PVT. For instance, the guidelines and related research by Garcia-Tsao et al[13] offer a systematic approach to the diagnosis and treatment of PH in liver cirrhosis, and these findings have a substantial impact on clinical practice. Additionally, HVPG, as a key hemodynamic indicator, is widely recognized for its role in prognostic evaluation and treatment decision-making. Timely therapeutic interventions, such as TIPS, have been shown to significantly reduce patient mortality and treatment failure rates[23].
However, despite the aforementioned studies achieving certain successes in clinical applications, issues remain, such as differences in the effectiveness of various clinical scoring systems (e.g., MELD and CTP) in evaluating the prognosis of liver cirrhosis. Future research should further explore how to optimize existing scoring models to enhance their accuracy and practicality in clinical practice. Additionally, with the continuous advancement of new therapeutic methods, integrating these new findings and improving the clinical applicability of existing guidelines will be important directions for future research.
In summary, these highly cited papers not only provide clinicians with an in-depth understanding of liver cirrhosis and PH but also emphasize the importance of early intervention, precise assessment, and individualized treatment. Further research should continue to deepen these findings and promote the translation of more effective diagnostic and therapeutic strategies into clinical practice. The usage frequency within 180 days reflects the extent to which the articles meet users' information needs. This can be verified by users clicking on the full-text links on publisher websites or saving metadata for future use. By sorting the results retrieved from the WoSCC accordingly, this assessment can be achieved. Although it takes time for high usage frequency to translate into high citations, new literature is more likely to be adopted by researchers due to its novelty. Meanwhile, older articles with high citation rates can also drive a resurgence in usage frequency. Therefore, the usage frequency within 180 days can, to some extent, reflect current research hotspots and cutting-edge areas[24].
As shown in Table 3, the article with the highest usage frequency within 180 days is the study by Seven et al[25], which compared the efficacy of endoscopic ultrasound-guided coil deployment with and without cyanoacrylate injection in the treatment of GV. The results demonstrated minimal differences between the two methods in terms of rebleeding rates, need for reintervention, or overall survival[25]. The second article, published in Journal of Digital Imaging, is by Wang et al[26], who integrated endoscopic images and clinical data using machine learning to predict the likelihood of esophageal variceal bleeding (EVB) in patients[26]. Additionally, Gao et al[27] developed a machine learning model utilizing contrast-enhanced computed tomography (CT) to predict clinical outcomes in patients with AVB associated with liver cirrhosis[27]. Wang et al[28] created an artificial intelligence (AI) system by establishing multiple machine learning models, offering a novel interpretable system for identifying risk factors in EGVB[28]. Whether the integration of machine learning and AI technologies will enhance the accuracy of predicting bleeding risk in EGVB patients remains to be determined. The AASLD and the Chinese Medical Association have also updated their guidelines, reflecting the medical community's widespread attention to EGVB and providing new standards for the future diagnosis, treatment, and management of EGVB[14,29].
| Rank | Year | Title | Journal | First author | Usage count |
| 1 | 2022 | Comparison of endoscopic ultrasound-guided coil deployment with and without cyanoacrylate injection for gastric varices | Arab Journal of Gastroenterology | Seven G | 11 |
| 2 | 2023 | Automated multimodal machine learning for esophageal variceal bleeding prediction based on endoscopy and structured data | Journal of Digital Imaging | Wang Y | 9 |
| 3 | 2023 | Prevalence, clinical characteristics, and outcomes of spontaneous portosystemic shunt in patients with hepatitis b-related cirrhosis: A multicenter study from china | Digestive and Liver Disease | Ke Q | 8 |
| 4 | 2022 | Optimal treatment for patients with cavernous transformation of the portal vein | Frontiers in Medicine | Wei B | 7 |
| 5 | 2015 | Intraoperative salvage endoscopy performed during orthotopic liver transplantation due to esophageal bleeding | Videosurgery and Other Miniinvasive Techniques | Kobryn K | 7 |
| 6 | 2023 | AASLD practice guidance on risk stratification and management of portal hypertension and varices in cirrhosis | Hepatology | Kaplan DE | 6 |
| 7 | 2023 | Guidelines for the management of esophagogastric variceal bleeding in cirrhotic portal hypertension | Journal of Clinical and Translational Hepatology | Xu XY | 6 |
| 8 | 2023 | An imaging-based machine learning model outperforms clinical risk scores for prognosis of cirrhotic variceal bleeding | European Radiology | Gao Y | 6 |
| 9 | 2023 | Diagnosis and management of esophagogastric varices | Diagnostics | Pallio S | 6 |
| 10 | 2022 | An interpretable artificial intelligence system for detecting risk factors of gastroesophageal variceal bleeding | NPJ Digital Medicine | Wang J | 5 |
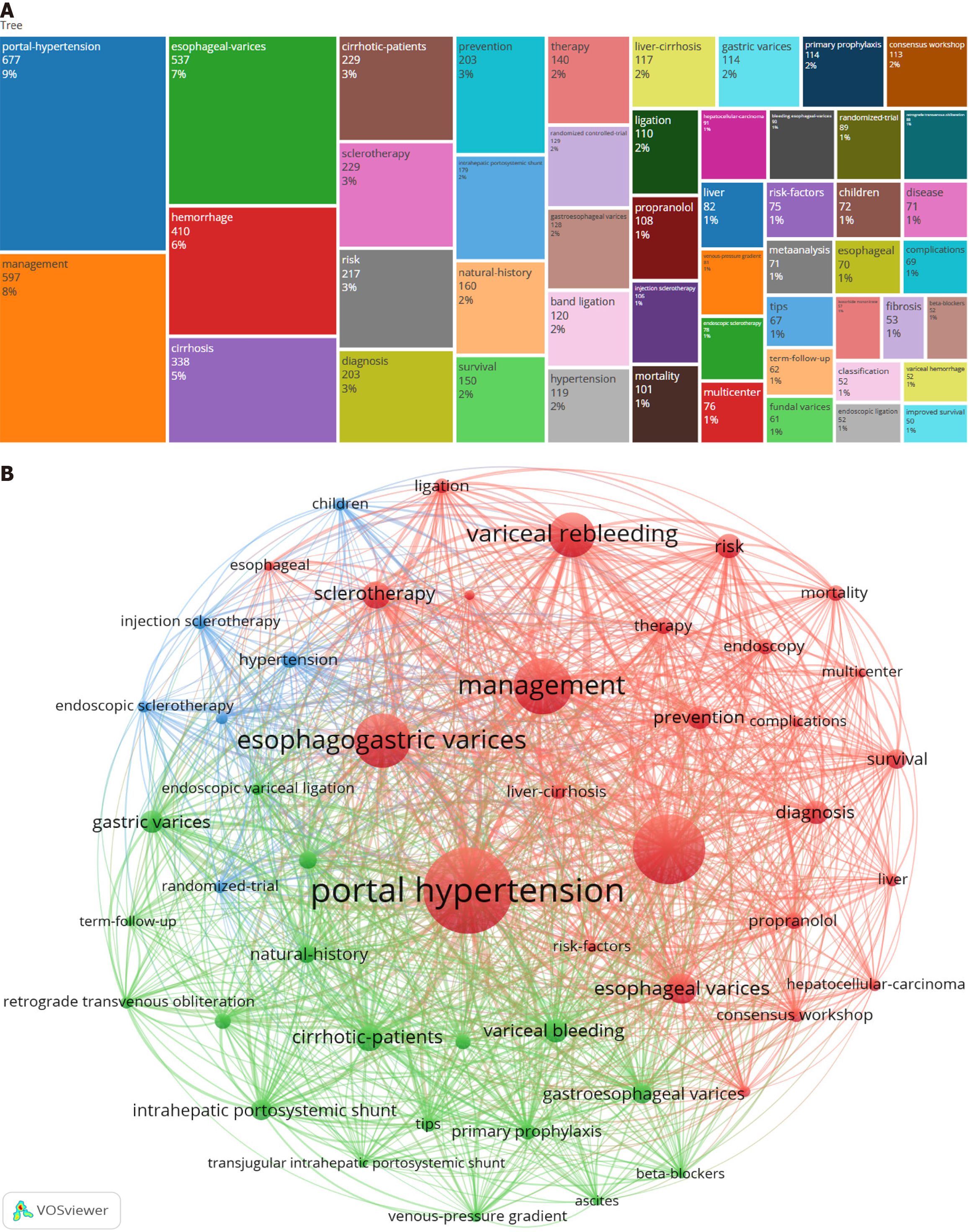
Keyword frequency is a key indicator that directly reveals the research focus, hotspots, and emerging trends in a field. Figure 5 lists the top 50 keywords extracted using the Bibliometrix package, and synonymous terms were combined for analysis.
There is a certain correlation among the keywords presented in the text, which can be represented by their co-occurrence frequency. It is generally believed that the more keyword themes appear within the same document, the closer the relationship between these two themes. Among the top 50 keywords, three clusters were identified based on keyword contribution, as shown in Figure 5. After excluding title-related keywords such as “esophageal varices”, “hemorrhage”, “variceal bleeding”, “gastric varices”, and “gastroesophageal varices”, the core keywords of EGVB include “portal hypertension”, “management”, “cirrhosis”, “risk”, “prevention”, and “diagnosis”. It is evident that the research focus of EGVB centers on studying its risk factors and diagnostic methods.
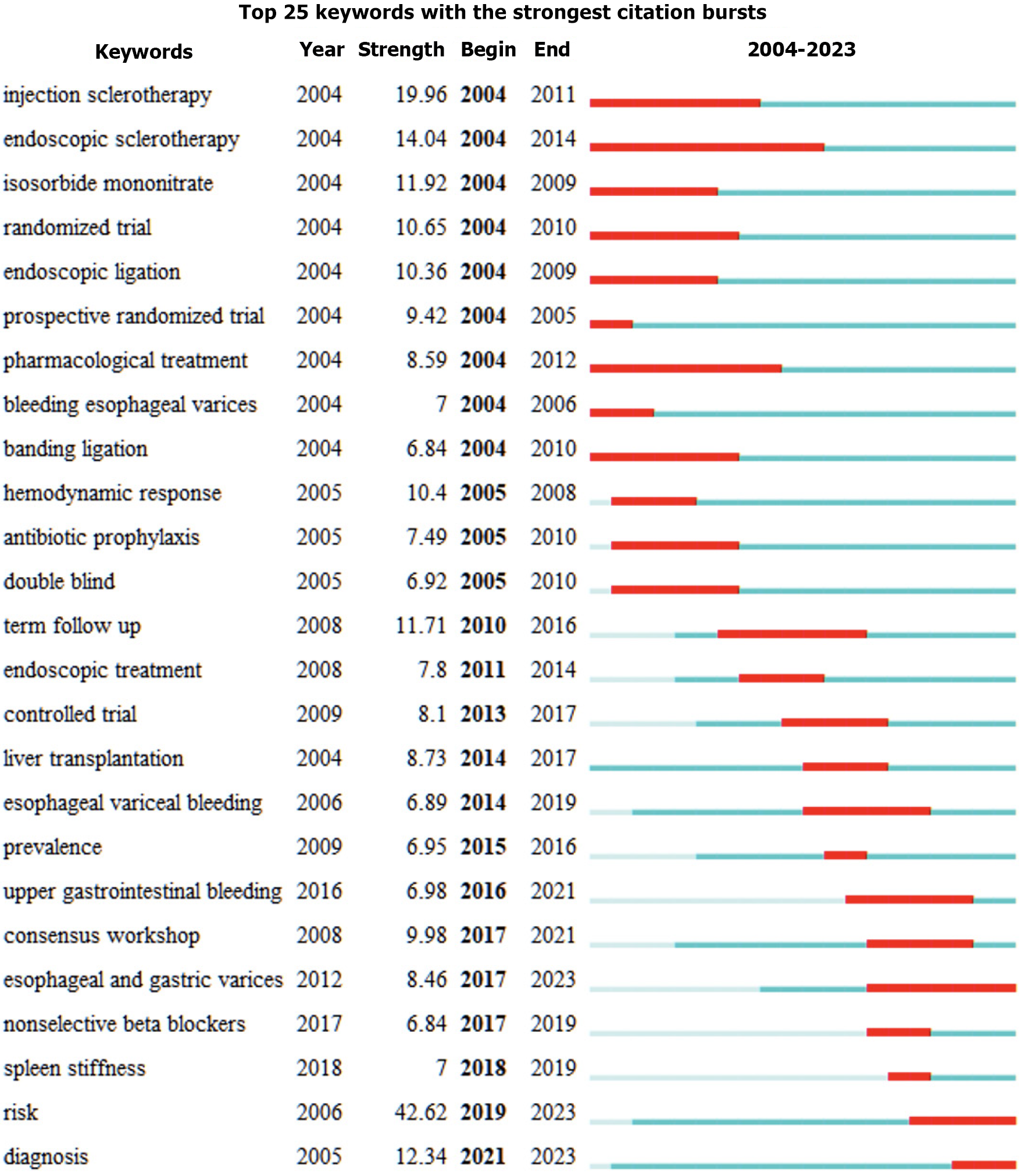
A keyword burst refers to a rapid rise in the frequency of a keyword over a specific period, effectively highlighting research hotspots and emerging frontiers in the field during that time (Figure 6). CiteSpace was used to analyze the keyword burst for studies related to EGVB from 2004 to 2023. The keyword burst detection can track research frontiers, and several emerging research topics have already been identified. The Figure 6 displays the top 25 keywords with the highest burst intensity. The blue line represents the timeline, while the red segments indicate the period when the burst occurred. “Year” marks the first appearance of the keyword, “Begin” and “End” show the start and end years of the burst, and “Strength” indicates the intensity of the burst. This figure highlights the research frontiers over different periods. After excluding title-related keywords, “risk” became a research focus from 2019 to 2023, and “diagnosis” has been at the forefront of research from 2021 to 2023.
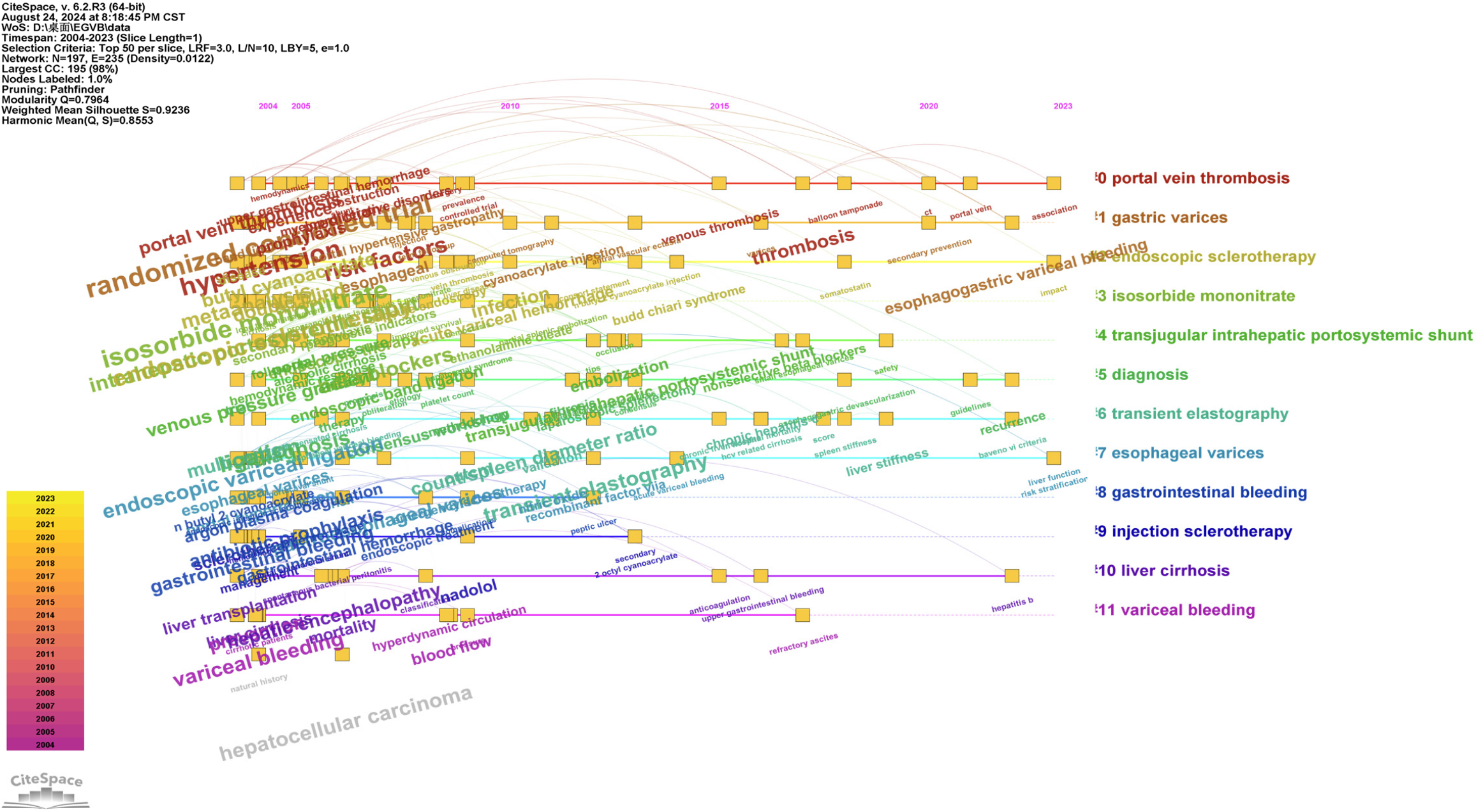
In bibliometric studies, the keyword timeline is a crucial indicator. The strongest burst segments of citations are considered the knowledge base of research frontiers. The clusters along the horizontal timeline are displayed in Figure 7, a timeline visualization from CiteSpace. Each cluster is shown from left to right, with the publication timeline legend located at the top. Keywords are anchored to the year they first appeared in the analyzed dataset. Once a keyword emerges, it remains fixed to its initial year, even if it continues to appear in later papers; it will only be displayed in the year of its first occurrence. Keywords are clustered and numbered sequentially, starting from 0, with Cluster 0 being the largest. In this study, the largest cluster is 0, “PVT,” reflecting a major research focus in recent years. This is followed by Cluster 1, “GV,” 2, “endoscopic sclerotherapy,” 3, “isosorbide mononitrate,” 4, “transjugular intrahepatic portosystemic shunt,” and 5, “diagnosis.” Some clusters have remained active until 2023. The keyword timeline diagram, created using CiteSpace, reflects the changing trends in research topics over time in this field.
We performed a quantitative analysis of the EGVB research literature published over the past 20 years, which revealed a consistent upward trend in the number of publications and strong connections to conditions such as PH, PVT, liver fibrosis, liver cirrhosis, and NCPH. As one of the most severe complications of chronic liver disease, EGVB continues to attract considerable attention in hepatology research. Summarizing the trends in EGVB research helps researchers understand recent developments and hotspots, guiding future studies. In terms of publication volume, the fields of gastroenterology and hepatology are the most representative. Jaime Bosch from the Hospital Clínic of Barcelona, Spain, is the most prolific expert, whereas the University of Barcelona leads in institutional output. China ranks first in terms of the number of publications, followed by the United States, with both countries significantly outpacing others. As shown in Figure 3B, China and the United States also present the strongest collaborative ties. This information allows us to identify authors working in similar research directions, providing a reference for collaboration and communication between researchers.
The core journals in the field of EGVB include the World Journal of Gastroenterology, the Journal of Gastroenterology and Hepatology, the European Journal of Gastroenterology and Hepatology, Gastrointestinal Endoscopy and Medicine, and the Journal of Clinical Gastroenterology. These journals have significant influence and academic reputation within the EGVB research domain, and we can expect to identify more cutting-edge research topics published in these journals in the future. The most cited and highly recognized article in this field is by Garcia-Tsao et al[13], published in Hepatology, titled “Portal hypertensive bleeding in cirrhosis: Risk stratification, diagnosis, and management: 2016 practice guidance by AASLD” with 977 citations. Although this article was published in 2017, it presented important consensus recommendations. The guidelines have been updated to the 2023 version, offering clear recommendations for both primary and secondary prevention of EGVB in patients with cirrhosis[13,14].
The core keywords in EGVB include “portal hypertension”, “management”, “cirrhosis”, “risk”, “prevention”, and “diagnosis”. EGVB is a life-threatening complication of PH. Lesmana et al[30] conducted a thorough review on the development and management of PH and varices in cirrhotic patients, integrating international guidelines with real-world experiences from Indonesia. Several noninvasive and minimally invasive tools, including Doppler ultrasound, contrast-enhanced ultrasound, and TE, have been developed in clinical practice as alternatives to HVPG. However, despite having a certain degree of specificity, their sensitivity is not high, and some specific patients, such as those with obesity, have a high failure rate in measurements. TE is currently one of the most important noninvasive measurement methods. The Baveno VI consensus workshop recommends that an LSM with a TE ≥ 20-25 kPa, either alone or in combination with platelet count and spleen size, can be used to identify CSPH in patients with viral cirrhosis. Jindal et al[31] analyzed the clinical outcomes of patients with severe alcoholic hepatitis who developed acute-on-chronic liver failure. Although variceal bleeding and variceal severity are not associated with mortality, patients with an HVPG ≥ 20 mmHg have a significantly greater incidence of large varices and variceal bleeding[31]. Hagström et al[32] and colleagues conducted a cohort study in Sweden from 2006 to 2020 on 3592 patients who experienced their first episode of EGVB, focusing on the effectiveness of secondary prevention. The results revealed that secondary prevention measures were not widely implemented, with 65% of patients dying during the follow-up period. Patients who received standardized secondary prevention had better overall survival rates, highlighting the need to improve awareness of proper preventive strategies among clinicians and patients[32]. Additionally, PH in children is also worth attention. Alkhasov et al[33] used portosystemic shunt surgery to treat pediatric patients with hepatic PH, achieving good outcomes with all children, eliminating the risk of EVB. Unlike in adults, where PH is caused primarily by liver fibrosis and cirrhosis, PH in children is often due to PVT or congenital malformations[33]. Goel et al[34] utilized TE and von Willebrand factor antigen to predict PH and decompensation in children, which helps clinicians diagnose clinically significant varices while avoiding unnecessary invasive procedures.
The management of patients with EGVB is crucial for preventing bleeding. In 2023, the AASLD updated their 2017 guidelines on the management of PH and EGV. In addition to the previously mentioned content, the updated guidelines place special emphasis on the concept of compensated advanced chronic liver disease, noninvasive assessments of portal pressure, emerging drug options for PH, and its vascular etiology. The guidelines also suggest potential future guidance for managing pediatric PH[14]. Cheung et al[35] conducted a network meta-analysis comparing the effects of carvedilol and other NSBBs on variceal bleeding rates and mortality. The results indicated that while carvedilol was slightly less effective than nadolol in reducing variceal bleeding rates, it ranked highest in reducing all-cause mortality and had the lowest incidence of adverse effects, making it the preferred NSBB for treating varices[35]. Ryu et al[36] conducted a retrospective analysis of 285 cirrhotic patients who underwent endoscopic variceal ligation (EVL). They discovered that EV with a larger diameter, as observed via CT, was associated with a greater risk of early bleeding following EVL treatment. Early identification of this high-risk group could allow for adjustments in treatment strategies, potentially improving patient outcomes[36]. Gan et al[37] evaluated the use of prophylactic antibiotics in patients with acute upper gastrointestinal bleeding. The results showed that prophylactic antibiotic use significantly reduced mortality in patients with variceal bleeding compared with those not treated with antibiotics, demonstrating clinical significance[37].
Liver cirrhosis is the leading cause of EGVB, as it increases portal vein pressure, forcing blood to seek alternative pathways. Fragile varices in the esophagus and gastric fundus are prone to rupture, and if bleeding occurs without timely intervention, it poses a life-threatening risk. In 2023, the Chinese Medical Association published the latest guidelines for the prevention and treatment of cirrhosis-related EGVB. These guidelines focus on a noninvasive diagnosis, screening for high-risk patients, primary and secondary prevention, and treatment of EGVB. The guidelines also highlighted several key issues and prospects in the field of cirrhosis-related EGVB. These include defining the concept and clinical indicators of cirrhosis recompensation and PH reversal, exploring whether relevant biomarkers can predict the risk of EGVB, and investigating the mechanisms of traditional Chinese medicine in antifibrosis and cirrhosis treatment[37]. Li et al[38] used the international normalized ratio (INR) and albumin-bilirubin to predict EGVB after endoscopic treatment in cirrhotic patients. Their model’s albumin-bilirubin receiver operating characteristic curve and assessments at 1 month, 3 months, and 12 months demonstrated significant advantages over existing models, especially in predicting early rebleeding, which may be helpful for clinical diagnosis and treatment in the future[38]. For cirrhotic patients with refractory ascites, NSBB reduces the incidence of variceal bleeding but may impair cardiac function, potentially worsening ascites. Mingpun et al[39] conducted a retrospective study on this issue and demonstrated that maintaining a heart rate between 55 beats and 60 beats per minute in these patients is a safe approach for preventing variceal bleeding. Huang et al[40] evaluated the efficacy and safety of an emergency TIPS in cirrhotic patients with hepatocellular carcinoma (HCC) and AVB. Among 33 cirrhotic patients with HCC, one patient died from acute liver failure postoperatively, while the remaining patients did not experience rebleeding within five days. The 6-week and 1-year survival rates were 87% and 65%, respectively, suggesting that an emergency TIPS is both feasible and effective. Additionally, splenectomy can reduce portal pressure, decrease blood flow, improve hematologic parameters, and lower the risk of EGVB in cirrhotic patients with PH[40]. Wang et al[41] conducted a 10-year single-center follow-up study on the use of anticoagulants after laparoscopic splenectomy plus esophagogastric devascularization. The findings revealed that patients who received perioperative anticoagulant therapy had significantly lower rates of portal venous system thrombosis, rebleeding, and PVT formation than did those who did not receive anticoagulation therapy. These results were especially pronounced in women with a history of variceal bleeding, larger portal vein diameters, and slower portal venous flow[41].
Liver cirrhosis is an inevitable outcome in the progression of chronic liver disease to its end stage, with EGVB being a significant risk factor for cirrhosis-related complications and the leading cause of death in patients with cirrhosis and PH. Identifying the risk factors for EGVB is crucial for controlling the prognosis of patients with cirrhosis. The relationship between gastroesophageal reflux disease and cirrhosis has rarely been discussed, but some studies suggest that reflux esophagitis may be a risk factor for EGVB. Proton pump inhibitors (PPIs) have been widely used to reduce the risk of EGVB in cirrhotic patients. Increased gastric pressure and the frequency of transient lower esophageal sphincter relaxation are considered key factors contributing to gastroesophageal reflux disease in cirrhotic patients[42]. Yardeni et al[43] investigated the prevalence of CSPH in patients with chronic liver disease. In their study of 326 patients, those with metabolic dysfunction-associated steatotic liver disease had a higher rate of EVB than patients with viral liver disease, alcoholic liver disease, or both, despite having significantly lower MELD-Na scores. These findings suggest that the MELD-Na score may underestimate the severity and bleeding risk in metabolic dysfunction-associated steatotic liver disease patients[43]. A multicenter international study evaluated whether first-line treatment with lenvatinib in patients with advanced HCC increases the risk of EGVB. A total of 535 patients from 12 centers across Italy, Korea, and Japan participated. The results revealed that while the overall risk of EGVB was low in HCC patients treated with lenvatinib, the risk was significantly greater in those with high-risk EV at baseline[44].
Prevention has always been a primary focus for hepatologists and researchers. Research on noninvasive risk stratification tools (primarily prediction models), pharmacological treatments, endoscopic treatments, surgical interventions, imaging techniques, metabolomics, and combination therapies remains at the forefront of the EGVB field. Among the risk stratification tools, the Baveno VII criteria are the most prominent, but they are primarily designed to predict variceal risk in cirrhotic patients; however, their applicability in patients with advanced HCC has not yet been validated[45-47]. Wu et al[48] successfully validated the Baveno VII criteria as a safe and accurate model for predicting high-risk varices and liver-related events in patients with HCC. The rate of missed varices requiring treatment was 3.5%, and a 5% missed diagnosis rate was deemed acceptable when alternative LSM and platelet thresholds were considered. Noninvasive prevention of EGVB in the advanced HCC population may become a critical focus moving forward[48]. Wang et al[49] identified EGVB in cirrhotic patients via the liver stiffness-spleen diameter-to-platelet ratio (LSPS) model and applied this model for risk stratification in the secondary prevention of EGVB. The results showed that LSPS-based stratification is a reliable noninvasive method that effectively detects high-risk events in the secondary prevention of EGVB[49]. Research related to CT and shear wave elastography has been considered a potential noninvasive measurement for PH, with potential predictive value for cirrhosis-related EGVB[50-53]. CSPH is considered a key milestone in the progression of cirrhosis. Previous studies have suggested that visceral volume measurements may serve as a predictive tool for the development of PH. Romero-Cristóbal et al[54] applied multidetector computerized tomography to predict CSPH in HCC patients, followed by HVPG assessments. The results indicated that quantifying liver and spleen volume could accurately predict PH. Whether this research can be expanded for broader application remains to be determined[54].
PH is the primary driving factor for decompensated cirrhosis. Carvedilol, a newer NSBB, is more effective at reducing portal pressure due to its additional α-blocking properties; it also has antioxidant, anti-inflammatory, and antifibrotic properties. Carvedilol, the preferred drug for EGVB prevention according to the Baveno VII guidelines, is recommended for both primary and secondary prevention of EGVB. Compared with EVL, carvedilol is more effective in the primary prevention of EGVB. Compared with propranolol, another NSBB, carvedilol reduces the risk of liver decompensation through a greater hemodynamic response rate. For secondary prevention, the combination of EVL and carvedilol has better efficacy than EVL or propranolol alone[55]. In terms of safety, carvedilol is safe for patients with ascites and EGVB, and maintaining adequate arterial blood pressure can improve survival rates. Increasing evidence suggests that carvedilol may delay decompensation and improve survival in patients with advanced cirrhosis and refractory ascites. As a result, a broader range of patients with advanced chronic liver disease should be considered in the future[56]. PPIs are widely used to treat various digestive system diseases related to excess stomach acid. However, there is still controversy regarding the occurrence of complications, particularly gastrointestinal bleeding, after EVT. Zhang et al[57] investigated the effects of PPIs use on complications in cirrhotic patients, including 143 patients during hospitalization after endoscopic variceal treatment (EVT). The results revealed that the incidence rates of gastrointestinal bleeding and other post-EVT complications were 4.90% and 46.85%, respectively. PPIs use did not significantly reduce the risk of complications; therefore, PPIs are not recommended for preventing complications during hospitalization after EVT[57].
Endoscopic treatment is the first-line emergency method for EGVB and plays a critical role in reducing mortality from acute bleeding and preventing rebleeding. Compared with pharmacological or surgical interventions, endoscopic techniques have a higher hemostasis rate and a lower risk of complications. The main treatment methods include EVL, endoscopic band ligation (EBL), endoscopic injection sclerotherapy (EIS), and gastroscopic tissue adhesive injection. These techniques effectively control bleeding and prevent recurrence by cutting off blood flow or rapidly coagulating the blood. Wei et al[58] conducted a multicenter randomized controlled trial in cirrhotic patients with AVB and hypersplenism comparing partial splenic embolization combined with endoscopic treatment vs endoscopic treatment alone. The results demonstrated that the 5-year rebleeding and variceal recurrence rates in the combined treatment group were significantly lower than those in the endoscopic-only group. Combined treatment was identified as the sole independent risk factor influencing outcomes and improved peripheral blood counts and liver function[58]. Lv et al[59] examined whether nonmalignant PVT affects outcomes in cirrhotic patients with AVB, a topic not addressed in the Baveno VII consensus. Multiple models adjusted for confounding factors to assess the impact of PVT on clinical outcomes. The results revealed no direct evidence that PVT influences prognosis, either positively or negatively, in cirrhotic AVB patients receiving standard treatment[59]. Zhang et al[60] analyzed the safety and efficacy of endoscopic submucosal dissection for cirrhotic patients with early-stage cancer or precancerous lesions in the upper gastrointestinal tract via data from a 10-year cohort at major Chinese medical institutions. No patients experienced liver function deterioration after completing treatment, and neither endoscopic submucosal dissection, liver function impairment, nor gastrointestinal tumors themselves caused death, with severe adverse events being rare[60]. Taki et al[61] reviewed the effects of EIS and balloon-occluded retrograde transvenous obliteration in the secondary prevention of gastric variceal bleeding and their impact on liver function. The results demonstrated that EIS is an effective treatment method, with no significant changes in liver function after treatment[61]. One research team evaluated the safety of EBL in cirrhotic patients with platelet counts < 50 g/L or INRs ≥ 1.5. They reported that the incidence of procedure-related bleeding within 30 days post-EBL was less than 2.6%. High MELD scores, particularly elevated bilirubin levels, were found to be significantly associated with an increased risk of variceal bleeding following EBL[62].
TIPS is an interventional technique used to manage complications of PH. By creating a channel between the portal vein and the hepatic vein within the liver, TIPS effectively reduces pressure in the portal venous system. This procedure is widely used in conditions caused by PH, such as cirrhosis, and is typically recommended for secondary prevention of EGVB when standard treatments fail. Li et al[63] assessed the safety and efficacy of emergency TIPS as a first-line treatment for cirrhotic patients with acute EGVB. The study reported a 100% success rate for TIPS procedures, with all patients transferred to general wards after surgery. No rebleeding occurred within five days, and the rebleeding rates at six weeks and two years were 6.6% and 1.3%, respectively. The transplant-free survival rates at six weeks, one year, and two years were 94.7%, 93.4%, and 84.6%, respectively. Major complications, including acute liver failure, hepatic encephalopathy, and shunt dysfunction, occurred at rates of 5.3%, 25%, and 5.3%, respectively. Overall, TIPS is a highly effective and safe treatment option for patients with advanced cirrhosis and acute EGVB, offering a stable management strategy, particularly in centers lacking immediate access to emergency endoscopy[63]. Mukund et al[64] demonstrated that performing emergency TIPS within eight hours significantly improved survival rates in patients with refractory variceal bleeding, underscoring the critical importance of timely intervention in TIPS therapy. However, for high-risk patients prone to rebleeding, there are currently no specific guidelines for treating those with HCC and symptomatic PH[64]. Chen et al[65] investigated patients with PH and HCC who had failed standard treatments and compared the efficacy of TIPS vs endoscopy combined with NSBB in preventing rebleeding. Their findings revealed that TIPS not only significantly reduced rebleeding rates but also improved adherence to targeted therapies for HCC and extended overall survival[65]. Studies comparing TIPS and endoscopy plus NSBB standard treatments for variceal bleeding patients have shown that when the HVPG is greater than 16 mmHg, TIPS can significantly improve transplant-free survival rates[66]. Wu et al[67] compared balloon-compression endoscopic injection sclerotherapy(bc-EIS) with TIPS for treating rebleeding after EVL and reported that the incidence of hepatic encephalopathy and total bilirubin levels were lower in the bc-EIS group than in the TIPS group, with no significant difference in rebleeding rates; this suggests that bc-EIS could be a suitable alternative for medical centers unable to perform TIPS[67].
Metabolomics, following genomics and proteomics, is an emerging field that studies the changes in metabolites or the variations in metabolite levels over time in biological systems (cells, tissues, or organisms) after they have been stimulated or disturbed. Metabolomics offers a powerful means to investigate biological systems by analyzing metabolic changes under disease conditions, thereby aiding in the identification of potential biomarkers for early diagnosis. Ai et al[68] utilized serum metabolomics based on ultra-performance liquid chromatography coupled with tandem mass spectrometry to screen for specific biomarkers of EGVB-specifically citrulline and alpha-aminobutyric acid-in a discovery cohort. These biomarkers were subsequently validated in two independent validation cohorts[68].
AI technologies and machine learning methods have also been widely applied in the field of EGVB, particularly in the identification, prediction, and management of the disease. In addition to the previously mentioned ENDOANGEL-GEV AI system, which segments and classifies gastroesophageal varices via six models, deep learning-based techniques have been employed to automatically measure the spleen volume from CT images. These findings provide new indicators for detecting high-risk varices in patients with compensated hepatitis B cirrhosis[69]. A novel machine learning-driven radiomic model was developed to identify patients with EV at high risk of bleeding. The study included 796 eligible participants, including patients with EV at low- and high-bleeding-risk. The model demonstrated a high AUROC value of 0.983 and exhibited good sensitivity and specificity in internal validation[70]. Additionally, advancements in endoscopic treatment technologies and standardized nursing measures have significantly improved the efficacy of upper gastrointestinal bleeding management. New hemostatic techniques, such as over-the-scope clips and hemostatic powders, have shown potential in treating refractory cases[71].
In economically developed countries with abundant medical resources, newer technologies and treatment options may help reduce health care costs and alleviate the financial burden on patients. In contrast, in developing countries, the lack of medical resources and preventive measures directly affects the cost-effectiveness of liver disease treatments and disease control outcomes. In Spain, Bañares et al[72] evaluated the cost-effectiveness of TIPS in treating EGVB and refractory ascites, tracking treatment costs and unrelated adverse events over a two-year period. The study indicated that TIPS may be a cost-effective and cost-saving alternative to standard therapies[72]. A cross-sectional study from Ethiopia on chronic liver disease patients revealed that higher-grade varices, a lack of NSBB use, infections, thrombocytopenia, and age were associated with higher bleeding rates, most of which are preventable factors[73]. Additionally, PH caused by NCPH deserves attention, such as in cases of polycythemia vera (PV). Previously considered a separate disease from NCPH, some case reports have shown that PV patients present with moderate to severe EV, PVT, and splenomegaly, while liver function remains relatively preserved. PV patients are recommended to undergo early esophagogastroduodenoscopy screening, and primary preventive measures should be taken if necessary[74].
In summary, EGVB is a common and severe complication in patients with liver cirrhosis. In recent years, significant progress has been made in areas such as risk assessment, early diagnosis, and personalized treatment. The development of non-invasive diagnostic techniques, such as the widespread application of TE, along with treatment methods based on individualized risk stratification, has markedly improved the prevention and management of EGVB. However, despite these advancements, several key issues remain unresolved, necessitating further research and exploration. In the future, research on EGVB should focus on the following key directions to address current challenges and advance clinical practice:
Building on existing research findings, explore novel treatment methods for EGVB to enhance therapeutic outcomes and improve patients' quality of life. This includes identifying new drug targets and developing comprehensive treatment plans that combine endoscopic surgery with TIPS.
Incorporating AI and machine learning technologies can more accurately predict the bleeding risk of EGVB and formulate personalized treatment plans, achieving precision medicine. This will aid in risk stratification and bleeding prevention, further reducing recurrence and complications.
In recent years, the importance of gut microbiota in various diseases has become increasingly evident. Future research should focus on the specific roles of gut microbiota in the pathogenesis of EGVB to identify potential intervention targets and provide new treatment avenues.
Further enhance the sensitivity and accuracy of diagnostic tools such as TE, particularly in non-invasive risk stratification models. For example, studies based on LSM with platelet count (LSPS) have shown great potential in secondary prevention. Continued development of such models will aid in early screening and risk assessment.
Standardizing multidisciplinary collaborative treatments is imperative. Clinicians should place greater emphasis on interdisciplinary cooperation, integrating new technologies such as imaging and metabolomics to achieve breakthroughs in early screening and personalized treatment. This will promote the optimization of diagnostic methods and the innovation of treatment strategies.
Conduct long-term follow-up studies to evaluate the prognosis and sustained treatment efficacy in EGVB patients, providing more comprehensive evidence for clinical decision-making. This will help in understanding the long-term impacts of different treatment methods and optimizing treatment protocols.
Through cross-institutional collaboration, increase sample sizes and the scope of studies to enhance the generalizability and credibility of research findings. This is crucial for validating new discoveries and promoting effective treatment strategies. In conclusion, with the continuous integration of cutting-edge technologies and clinical practice, research in the EGVB field will achieve greater progress in optimizing diagnostic methods, personalized treatment, and multidisciplinary collaboration. We anticipate witnessing more groundbreaking developments that will provide safer and more effective treatment options for EGVB patients worldwide.
| 1. | Yoshida H, Mamada Y, Taniai N, Yoshioka M, Hirakata A, Kawano Y, Mizuguchi Y, Shimizu T, Ueda J, Uchida E. Treatment modalities for bleeding esophagogastric varices. J Nippon Med Sch. 2012;79:19-30. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 15] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 2. | Devarbhavi H, Asrani SK, Arab JP, Nartey YA, Pose E, Kamath PS. Global burden of liver disease: 2023 update. J Hepatol. 2023;79:516-537. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1738] [Cited by in RCA: 1401] [Article Influence: 467.0] [Reference Citation Analysis (3)] |
| 3. | Gioia S, Nardelli S, Ridola L, Riggio O. Causes and Management of Non-cirrhotic Portal Hypertension. Curr Gastroenterol Rep. 2020;22:56. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 72] [Cited by in RCA: 58] [Article Influence: 9.7] [Reference Citation Analysis (1)] |
| 4. | McDonald SA, Barclay ST, Hutchinson SJ, Stanley AJ, Fraser A, Dillon JF, Innes HA, Peters E, Kennedy N, Bathgate A, Bramley P, Morris J, Goldberg DJ, Hayes PC. Uptake of endoscopic screening for gastroesophageal varices and factors associated with variceal bleeding in patients with chronic hepatitis C infection and compensated cirrhosis, 2005-2016: a national database linkage study. Aliment Pharmacol Ther. 2019;50:425-434. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 10] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 5. | Gunarathne LS, Rajapaksha H, Shackel N, Angus PW, Herath CB. Cirrhotic portal hypertension: From pathophysiology to novel therapeutics. World J Gastroenterol. 2020;26:6111-6140. [PubMed] [DOI] [Full Text] |
| 6. | Zhao Q, Liang L, Zhai F, Ling G, Xiang R, Jiang X. A bibliometric and visualized analysis of liver fibrosis from 2002 to 2022. J Gastroenterol Hepatol. 2023;38:359-369. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 10] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 7. | Dai YK, Zhao ZM, Liu C. Treatment of Liver Fibrosis: A 20-Year Bibliometric and Knowledge-Map Analysis. Front Pharmacol. 2022;13:942841. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 11] [Article Influence: 2.8] [Reference Citation Analysis (1)] |
| 8. | Gan PL, Huang S, Pan X, Xia HF, Zeng XY, Ren WS, Zhou X, Lv MH, Tang XW. Global research trends in the field of liver cirrhosis from 2011 to 2020: A visualised and bibliometric study. World J Gastroenterol. 2022;28:4909-4919. [PubMed] [DOI] [Full Text] |
| 9. | Zhang D, Liu BW, Liang XQ, Liu FQ. Immunological factors in cirrhosis diseases from a bibliometric point of view. World J Gastroenterol. 2023;29:3899-3921. [PubMed] [DOI] [Full Text] |
| 10. | van Eck NJ, Waltman L. Software survey: VOSviewer, a computer program for bibliometric mapping. Scientometrics. 2010;84:523-538. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 15743] [Cited by in RCA: 5816] [Article Influence: 363.5] [Reference Citation Analysis (1)] |
| 11. | Wang WH, Lu C. Visualization analysis of big data research based on Citespace. Soft Comput. 2020;24:8173-8186. [RCA] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 39] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 12. | Aria M, Cuccurullo C. bibliometrix : An R-tool for comprehensive science mapping analysis. J Informetr. 2017;11:959-975. [RCA] [DOI] [Full Text] [Cited by in Crossref: 1736] [Cited by in RCA: 2705] [Article Influence: 300.6] [Reference Citation Analysis (1)] |
| 13. | Garcia-Tsao G, Abraldes JG, Berzigotti A, Bosch J. Portal hypertensive bleeding in cirrhosis: Risk stratification, diagnosis, and management: 2016 practice guidance by the American Association for the study of liver diseases. Hepatology. 2017;65:310-335. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1775] [Cited by in RCA: 1551] [Article Influence: 172.3] [Reference Citation Analysis (5)] |
| 14. | Kaplan DE, Ripoll C, Thiele M, Fortune BE, Simonetto DA, Garcia-Tsao G, Bosch J. AASLD Practice Guidance on risk stratification and management of portal hypertension and varices in cirrhosis. Hepatology. 2024;79:1180-1211. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 314] [Cited by in RCA: 279] [Article Influence: 139.5] [Reference Citation Analysis (18)] |
| 15. | Foucher J, Chanteloup E, Vergniol J, Castéra L, Le Bail B, Adhoute X, Bertet J, Couzigou P, de Lédinghen V. Diagnosis of cirrhosis by transient elastography (FibroScan): a prospective study. Gut. 2006;55:403-408. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1012] [Cited by in RCA: 965] [Article Influence: 48.3] [Reference Citation Analysis (0)] |
| 16. | Castera L, Pinzani M, Bosch J. Non invasive evaluation of portal hypertension using transient elastography. J Hepatol. 2012;56:696-703. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 270] [Cited by in RCA: 234] [Article Influence: 16.7] [Reference Citation Analysis (1)] |
| 17. | Amitrano L, Guardascione MA, Brancaccio V, Margaglione M, Manguso F, Iannaccone L, Grandone E, Balzano A. Risk factors and clinical presentation of portal vein thrombosis in patients with liver cirrhosis. J Hepatol. 2004;40:736-741. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 462] [Cited by in RCA: 384] [Article Influence: 17.5] [Reference Citation Analysis (0)] |
| 18. | Tripathi D, Stanley AJ, Hayes PC, Patch D, Millson C, Mehrzad H, Austin A, Ferguson JW, Olliff SP, Hudson M, Christie JM; Clinical Services and Standards Committee of the British Society of Gastroenterology. U.K. guidelines on the management of variceal haemorrhage in cirrhotic patients. Gut. 2015;64:1680-1704. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 495] [Cited by in RCA: 438] [Article Influence: 39.8] [Reference Citation Analysis (0)] |
| 19. | Monescillo A, Martínez-Lagares F, Ruiz-del-Arbol L, Sierra A, Guevara C, Jiménez E, Marrero JM, Buceta E, Sánchez J, Castellot A, Peñate M, Cruz A, Peña E. Influence of portal hypertension and its early decompression by TIPS placement on the outcome of variceal bleeding. Hepatology. 2004;40:793-801. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 423] [Cited by in RCA: 335] [Article Influence: 15.2] [Reference Citation Analysis (1)] |
| 20. | D'Amico G, Garcia-Pagan JC, Luca A, Bosch J. Hepatic vein pressure gradient reduction and prevention of variceal bleeding in cirrhosis: a systematic review. Gastroenterology. 2006;131:1611-1624. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 424] [Cited by in RCA: 349] [Article Influence: 17.5] [Reference Citation Analysis (2)] |
| 21. | Cholongitas E, Papatheodoridis GV, Vangeli M, Terreni N, Patch D, Burroughs AK. Systematic review: The model for end-stage liver disease--should it replace Child-Pugh's classification for assessing prognosis in cirrhosis? Aliment Pharmacol Ther. 2005;22:1079-1089. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 259] [Cited by in RCA: 292] [Article Influence: 13.9] [Reference Citation Analysis (0)] |
| 22. | Nery F, Chevret S, Condat B, de Raucourt E, Boudaoud L, Rautou PE, Plessier A, Roulot D, Chaffaut C, Bourcier V, Trinchet JC, Valla DC; Groupe d'Etude et de Traitement du Carcinome Hépatocellulaire. Causes and consequences of portal vein thrombosis in 1,243 patients with cirrhosis: results of a longitudinal study. Hepatology. 2015;61:660-667. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 405] [Cited by in RCA: 359] [Article Influence: 32.6] [Reference Citation Analysis (0)] |
| 23. | Debray D, Kelly D, Houwen R, Strandvik B, Colombo C. Best practice guidance for the diagnosis and management of cystic fibrosis-associated liver disease. J Cyst Fibros. 2011;10 Suppl 2:S29-S36. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 348] [Cited by in RCA: 293] [Article Influence: 19.5] [Reference Citation Analysis (0)] |
| 24. | Wang XW, Fang ZC, Sun XL. Usage patterns of scholarly articles on Web of Science: a study on Web of Science usage count. Scientometrics. 2016;109:917-926. [RCA] [DOI] [Full Text] [Cited by in Crossref: 42] [Cited by in RCA: 47] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 25. | Seven G, Musayeva G, Seven OO, Herdan E, Ince AT, Senturk H. Comparison of endoscopic ultrasound-guided coil deployment with and without cyanoacrylate injection for gastric varices. Arab J Gastroenterol. 2022;23:115-119. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 5] [Article Influence: 1.3] [Reference Citation Analysis (1)] |
| 26. | Wang Y, Hong Y, Wang Y, Zhou X, Gao X, Yu C, Lin J, Liu L, Gao J, Yin M, Xu G, Liu X, Zhu J. Automated Multimodal Machine Learning for Esophageal Variceal Bleeding Prediction Based on Endoscopy and Structured Data. J Digit Imaging. 2023;36:326-338. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 38] [Cited by in RCA: 31] [Article Influence: 10.3] [Reference Citation Analysis (0)] |
| 27. | Gao Y, Yu Q, Li X, Xia C, Zhou J, Xia T, Zhao B, Qiu Y, Zha JH, Wang Y, Tang T, Lv Y, Ye J, Xu C, Ju S. An imaging-based machine learning model outperforms clinical risk scores for prognosis of cirrhotic variceal bleeding. Eur Radiol. 2023;33:8965-8973. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 23] [Article Influence: 7.7] [Reference Citation Analysis (0)] |
| 28. | Wang J, Wang Z, Chen M, Xiao Y, Chen S, Wu L, Yao L, Jiang X, Li J, Xu M, Lin M, Zhu Y, Luo R, Zhang C, Li X, Yu H. An interpretable artificial intelligence system for detecting risk factors of gastroesophageal variceal bleeding. NPJ Digit Med. 2022;5:183. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 22] [Cited by in RCA: 20] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 29. | Xu X, Tang C, Linghu E, Ding H; Chinese Society of Hepatology, Chinese Medical Association; Chinese Society of Gastroenterology, Chinese Medical Association; Chinese Society of Digestive Endoscopy, Chinese Medical Association. Guidelines for the Management of Esophagogastric Variceal Bleeding in Cirrhotic Portal Hypertension. J Clin Transl Hepatol. 2023;11:1565-1579. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 28] [Article Influence: 9.3] [Reference Citation Analysis (1)] |
| 30. | Lesmana CRA, Raharjo M, Gani RA. Managing liver cirrhotic complications: Overview of esophageal and gastric varices. Clin Mol Hepatol. 2020;26:444-460. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 93] [Cited by in RCA: 86] [Article Influence: 14.3] [Reference Citation Analysis (0)] |
| 31. | Jindal A, Sharma MK, Vijayaraghavan R, Sm S, Kumar G, Sarin SK. Severity of Acute Portal Hypertension Determines the Clinical Outcomes in Severe Alcoholic Hepatitis. Dig Dis Sci. 2024;69:298-307. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 3] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 32. | Hagström H, Shang Y, Tapper EB, Wester A, Widman L. Secondary Prevention of Esophageal Variceal Bleeding Is Often Imperfect: A National, Population-Based Cohort Study of 3592 Patients. Clin Gastroenterol Hepatol. 2023;21:3336-3345.e2. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 4] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 33. | Alkhasov A, Komina E, Ratnikov S, Saveleva M, Romanova E, Gusev A, Lochmatov M, Yatsyk S, Dyakonova E. Surgical Treatment of Portal Hypertension in Children. J Laparoendosc Adv Surg Tech A. 2023;33:1231-1235. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 34. | Goel A, Hegarty R, Dixit S, Tucker B, Douiri A, Kyrana E, Jain V, Dhawan A, Grammatikopoulos T. Transient elastography and von Willebrand factor as predictors of portal hypertension and decompensation in children. JHEP Rep. 2023;5:100935. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 35. | Cheung KS, Mok CH, Lam LK, Mao XH, Mak LY, Seto WK, Yuen MF. Carvedilol Versus Other Nonselective Beta Blockers for Variceal Bleeding Prophylaxis and Death: A Network Meta-analysis. J Clin Transl Hepatol. 2023;11:1143-1149. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 6] [Article Influence: 2.0] [Reference Citation Analysis (4)] |
| 36. | Ryu H, Kim TU, Yoon KT, Hong YM. Predicting the risk of early bleeding following endoscopic variceal ligation in cirrhotic patients with computed tomography. BMC Gastroenterol. 2023;23:410. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 4] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 37. | Gan M, Zong L, Yu X, Xu J. The effect of prophylactic antibiotics in acute upper gastrointestinal bleeding patients in the emergency department. World J Emerg Med. 2023;14:442-447. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 38. | Li F, Wang T, Liang J, Qian B, Tang F, Gao Y, Lv J. Albuminbilirubin grade and INR for the prediction of esophagogastric variceal rebleeding after endoscopic treatment in cirrhosis. Exp Ther Med. 2023;26:501. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 4] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 39. | Mingpun W, Sobhonslidsuk A, Chumnumwat S. Optimal resting heart rate and ascites-related death in patients with cirrhosis and ascites using nonselective beta-blockers (ORCA). Clin Transl Sci. 2024;17:e13681. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 40. | Huang JT, Zhong BY, Li WC, Jiang N, Qian D, Hu ZX, Nie H, Zhang S, Shen J, Zhu XL. Emergent TIPS for acute gastroesophageal variceal bleeding in cirrhotic patients with hepatocellular carcinoma. Abdom Radiol (NY). 2024;49:900-907. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 41. | Wang D, Chen X, Lv L, Yang T, Huang B, Cao Y, Lu J, Yin J. The Early Initiation of Perioperative Anticoagulation Therapy in Cirrhotic Patients with Portal Hypertension After Laparoscopic Splenectomy Plus Esophagogastric Devascularization: A 10-Year Single-Center Experience. J Laparoendosc Adv Surg Tech A. 2023;33:1064-1073. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 3] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 42. | Yu F, Zhu Y, Li N, Fu HF, Jiang Z, Zhang XY, Zeng L, Hu XY. Gastrooesophageal reflux disease in liver cirrhosis: Possible pathogenesis and clinical intervention (Review). Exp Ther Med. 2023;26:414. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 43. | Yardeni D, Shiloh A, Lipnizkiy I, Nevo-Shor A, Abufreha N, Munteanu D, Novack V, Etzion O. MELD-Na score may underestimate disease severity and risk of death in patients with metabolic dysfunction-associated steatotic liver disease (MASLD). Sci Rep. 2023;13:22113. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 8] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 44. | Iavarone M, Alimenti E, Tada T, Shimose S, Suda G, Yoo C, Soldà C, Piscaglia F, Tosetti G, Marra F, Vivaldi C, Conti F, Schirripa M, Iwamoto H, Sho T, Lee SH, Rizzato MD, Tonnini M, Rimini M, Campani C, Masi G, Foschi F, Bruccoleri M, Kawaguchi T, Kumada T, Hiraoka A, Atsukawa M, Fukunishi S, Ishikawa T, Tajiri K, Ochi H, Yasuda S, Toyoda H, Hatanaka T, Kakizaki S, Kawata K, Tada F, Ohama H, Itokawa N, Okubo T, Arai T, Imai M, Naganuma A, Casadei-Gardini A, Lampertico P. Incidence and Predictors of Esophagogastric Varices Bleeding in Patients with Hepatocellular Carcinoma in Lenvatinib. Liver Cancer. 2024;13:215-226. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 10] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 45. | Galizzi HO, Couto CA, Taranto DOL, Araújo SIO, Vilela EG. Accuracy of non-invasive methods/models for predicting esophageal varices in patients with compensated advanced chronic liver disease secondary to nonalcoholic fatty liver disease. Ann Hepatol. 2021;20:100229. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 12] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 46. | Hu Y, Wen Z. Validation and comparison of non-invasive prediction models based on liver stiffness measurement to identify patients who could avoid gastroscopy. Sci Rep. 2021;11:150. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9] [Cited by in RCA: 7] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 47. | Shin S, Kim SU, Park JY, Kim DY, Ahn SH, Kim BK. Validation of PH and Varices Risk Scores for Prediction of High-Risk Esophageal Varix and Bleeding in Patients with B-Viral Cirrhosis. Diagnostics (Basel). 2022;12:441. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 48. | Wu CW, Lui RN, Wong VW, Yam TF, Yip TC, Liu K, Lai JC, Tse YK, Mok TS, Chan HL, Ng KK, Wong GL, Chan SL. Baveno VII Criteria Is an Accurate Risk Stratification Tool to Predict High-Risk Varices Requiring Intervention and Hepatic Events in Patients with Advanced Hepatocellular Carcinoma. Cancers (Basel). 2023;15:2480. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 19] [Cited by in RCA: 17] [Article Influence: 5.7] [Reference Citation Analysis (1)] |
| 49. | Wang X, Han H, Yang J, Cheng Y, Yin X, Gu L, Xiao J, Wang Y, Zou X, Wang L, Zhang M, Zhuge Y, Zhang F. Liver stiffness-spleen diameter to platelet ratio score (LSPS model) predicts variceal rebleeding for cirrhotic patients. Eur J Gastroenterol Hepatol. 2023;35:488-496. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 1.0] [Reference Citation Analysis (5)] |
| 50. | Dong B, Chen Y, Lyu G, Chen Y, Qin R. Quantitative Assessment of Portal Hypertension by Two-Dimensional Shear Wave Elastography in Rat Models of Nonalcoholic Fatty Liver Disease: Comparison With Four Composite Scores. Front Med (Lausanne). 2022;9:844558. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 51. | Xuan J, Shi Z. Shear wave elastography measured liver stiffness-spleen size-to-platelet ratio for the prediction of high-risk oesophageal varices: a meta-analysis. Eur J Gastroenterol Hepatol. 2023;35:753-760. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 52. | Fu S, Chen D, Zhang Z, Shen R. Predictive Value of Spectral Computed Tomography Parameters in Esophageal Variceal Rupture and Bleeding in Cirrhosis. Turk J Gastroenterol. 2023;34:339-345. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 3] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 53. | Wang L, Zhang Y, Wu YF, Yue ZD, Fan ZH, Zhang CY, Liu FQ, Dong J. Computed tomography perfusion in liver and spleen for hepatitis B virus-related portal hypertension: A correlation study with hepatic venous pressure gradient. World J Gastroenterol. 2022;28:6068-6077. [PubMed] [DOI] [Full Text] |
| 54. | Romero-Cristóbal M, Clemente-Sánchez A, Ramón E, Téllez L, Canales E, Ortega-Lobete O, Velilla-Aparicio E, Catalina MV, Ibáñez-Samaniego L, Alonso S, Colón A, Matilla AM, Salcedo M, Albillos A, Bañares R, Rincón D. CT-derived liver and spleen volume accurately diagnose clinically significant portal hypertension in patients with hepatocellular carcinoma. JHEP Rep. 2023;5:100645. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 17] [Cited by in RCA: 20] [Article Influence: 6.7] [Reference Citation Analysis (0)] |
| 55. | Turco L, Reiberger T, Vitale G, La Mura V. Carvedilol as the new non-selective beta-blocker of choice in patients with cirrhosis and portal hypertension. Liver Int. 2023;43:1183-1194. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 82] [Cited by in RCA: 68] [Article Influence: 22.7] [Reference Citation Analysis (1)] |
| 56. | Gillespie SL, Hanrahan TP, Rockey DC, Majumdar A, Hayes PC. Review article: controversies surrounding the use of carvedilol and other beta blockers in the management of portal hypertension and cirrhosis. Aliment Pharmacol Ther. 2023;57:454-463. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 18] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 57. | Zhang YY, Wang L, Shao XD, Zhang YG, Ma SZ, Peng MY, Xu SX, Yin Y, Guo XZ, Qi XS. Effects of postoperative use of proton pump inhibitors on gastrointestinal bleeding after endoscopic variceal treatment during hospitalization. World J Gastrointest Surg. 2023;15:82-93. [PubMed] [DOI] [Full Text] |
| 58. | Wei M, Chen Y, Wang M, Li J, Zeng Y, Sun X, Zhang A, Liu X, Zhou T, Gao Y. Partial splenic embolization combined with endoscopic therapies and vasoconstrictive drugs reduces rebleeding in cirrhosis patients with acute variceal bleeding and hypersplenism: a multicenter randomized controlled trial. J Gastroenterol. 2023;58:1144-1153. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 2] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 59. | Lv Y, Bai W, Zhu X, Xue H, Zhao J, Zhuge Y, Sun J, Zhang C, Ding P, Jiang Z, Zhu X, Ren W, LiZhang YK, Zhang W, Li K, Wang Z, Luo B, Li X, Yuan J, Yang Z, Guo W, Xia D, Xie H, Yang C, Pan Y, Yin Z, Fan D, Han G. Association of nonmalignant portal vein thrombosis and clinical outcomes in patients with cirrhosis and acute variceal bleeding: a multicenter observational study. Hepatol Int. 2023;17:1192-1204. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 8] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 60. | Zhang S, Liu YD, Chai NL, Yao Y, Gao F, Liu B, He ZD, Bai L, Huang X, Gao C, Linghu EQ, Li LY. Endoscopic submucosal dissection for early cancers or precancerous lesions of the upper GI tract in cirrhotic patients with esophagogastric varices: 10-year experience from a large tertiary center in China. Gastrointest Endosc. 2023;97:1031-1044. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 7] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 61. | Taki S, Iguchi M, Maekita T, Kinoshita J, Takao M, Kitano M. Endoscopic N-butyl-2-cyanoacrylate and ethanolamine oleate injection is equivalent to balloon-occluded retrograde transvenous obliteration for preventing gastric variceal bleeding. Surg Endosc. 2023;37:6008-6014. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 62. | Pfisterer N, Schwarz M, Jachs M, Putre F, Ritt L, Mandorfer M, Madl C, Trauner M, Reiberger T. Endoscopic band ligation is safe despite low platelet count and high INR. Hepatol Int. 2023;17:1205-1214. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 9] [Article Influence: 3.0] [Reference Citation Analysis (1)] |
| 63. | Li WC, Zhong BY, Zhang S, Shen J, Wang W, Zhu XL. Emergent Transjugular Intrahepatic Portosystemic Shunt as a First-Line Therapy in Patients with Cirrhosis with Acute Gastroesophageal Variceal Hemorrhage. J Vasc Interv Radiol. 2023;34:344-350. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 64. | Mukund A, Vasistha S, Jindal A, Patidar Y, Sarin SK. Emergent rescue transjugular intrahepatic portosystemic shunt within 8 h improves survival in patients with refractory variceal bleed. Hepatol Int. 2023;17:954-966. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 8] [Article Influence: 2.7] [Reference Citation Analysis (1)] |
| 65. | Chen Y, Ma X, Zhang X, Luo J, An L, Zhang Y, Chang X, Dong Z, Zhang W, Kong H, Zhao J, Ding H, Liu F, Yang Y. Prevention of variceal rebleeding in cirrhotic patients with advanced hepatocellular carcinoma receiving molecularly targeted therapy: a randomized pilot study of transjugular intrahepatic portosystemic shunt versus endoscopic plus β-blocker. Hepatol Int. 2022;16:1379-1389. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 12] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 66. | Wang XX, Yin XC, Gu LH, Guo HW, Cheng Y, Liu Y, Xiao JQ, Wang Y, Zhang W, Zou XP, Wang L, Zhang M, Zhu-Ge YZ, Zhang F. Pre-transjugular-intrahepatic-portosystemic-shunt measurement of hepatic venous pressure gradient and its clinical application: A comparison study. World J Gastroenterol. 2023;29:3519-3533. [PubMed] [DOI] [Full Text] |
| 67. | Wu W, Zhang F, Mei X, Zhang Q, Jin J, Kong D. Balloon-compression endoscopic injection sclerotherapy versus transjugular intrahepatic portosystemic shunt for esophageal variceal rebleeding. Surg Endosc. 2023;37:5766-5774. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 68. | Ai Y, Huang X, Chen W, Wu L, Jiang S, Chen Y, Chen S. UPLC-MS/MS-Based Serum Metabolomics Signature as Biomarkers of Esophagogastric Variceal Bleeding in Patients With Cirrhosis. Front Cell Dev Biol. 2022;10:839781. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 12] [Cited by in RCA: 6] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 69. | Lee CM, Lee SS, Choi WM, Kim KM, Sung YS, Lee S, Lee SJ, Yoon JS, Suk HI. An index based on deep learning-measured spleen volume on CT for the assessment of high-risk varix in B-viral compensated cirrhosis. Eur Radiol. 2021;31:3355-3365. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 33] [Article Influence: 6.6] [Reference Citation Analysis (0)] |
| 70. | Yan Y, Li Y, Fan C, Zhang Y, Zhang S, Wang Z, Huang T, Ding Z, Hu K, Li L, Ding H. A novel machine learning-based radiomic model for diagnosing high bleeding risk esophageal varices in cirrhotic patients. Hepatol Int. 2022;16:423-432. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 28] [Article Influence: 7.0] [Reference Citation Analysis (0)] |
| 71. | Lau LHS, Sung JJY. Treatment of upper gastrointestinal bleeding in 2020: New techniques and outcomes. Dig Endosc. 2021;33:83-94. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 38] [Article Influence: 7.6] [Reference Citation Analysis (0)] |
| 72. | Bañares R, Albillos A, Nakum M, Gea S, Varghese A, Green W. An Economic Analysis of Transjugular Intrahepatic Portosystemic Covered Stent Shunt for Variceal Bleeding and Refractory Ascites in a Spanish Setting. Adv Ther. 2023;40:3006-3020. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 6] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 73. | Baye ML, Abay Z, Tesfaye T, Ahmed E, Arage G, Zewude EA, Anley DT. Gastroesophageal variceal hemorrhage in patients with chronic liver diseases attending university of Gondar Specialized comprehensive hospital in Ethiopia: Institutional based cross-sectional study. Heliyon. 2023;9:e15133. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 74. | Zhang L, Wang Y, Lv W, Hu J, Gou C. Association of polycythemia vera with noncirrhotic portal hypertension in five patients: A case series. Exp Ther Med. 2023;25:149. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 2] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/