Published online Dec 15, 2024. doi: 10.4239/wjd.v15.i12.2293
Revised: September 3, 2024
Accepted: October 8, 2024
Published online: December 15, 2024
Processing time: 117 Days and 15.4 Hours
Individuals with diabetes mellitus have a higher risk of developing malignant tumors, and diagnosing these tumors can be challenging.
To confirm the benefits of using peripherally inserted central catheters (PICCs) in contrast-enhanced computerized tomography (CECT) for diagnostic imaging in diabetic patients with malignant tumors and to provide a research basis for follow-up research.
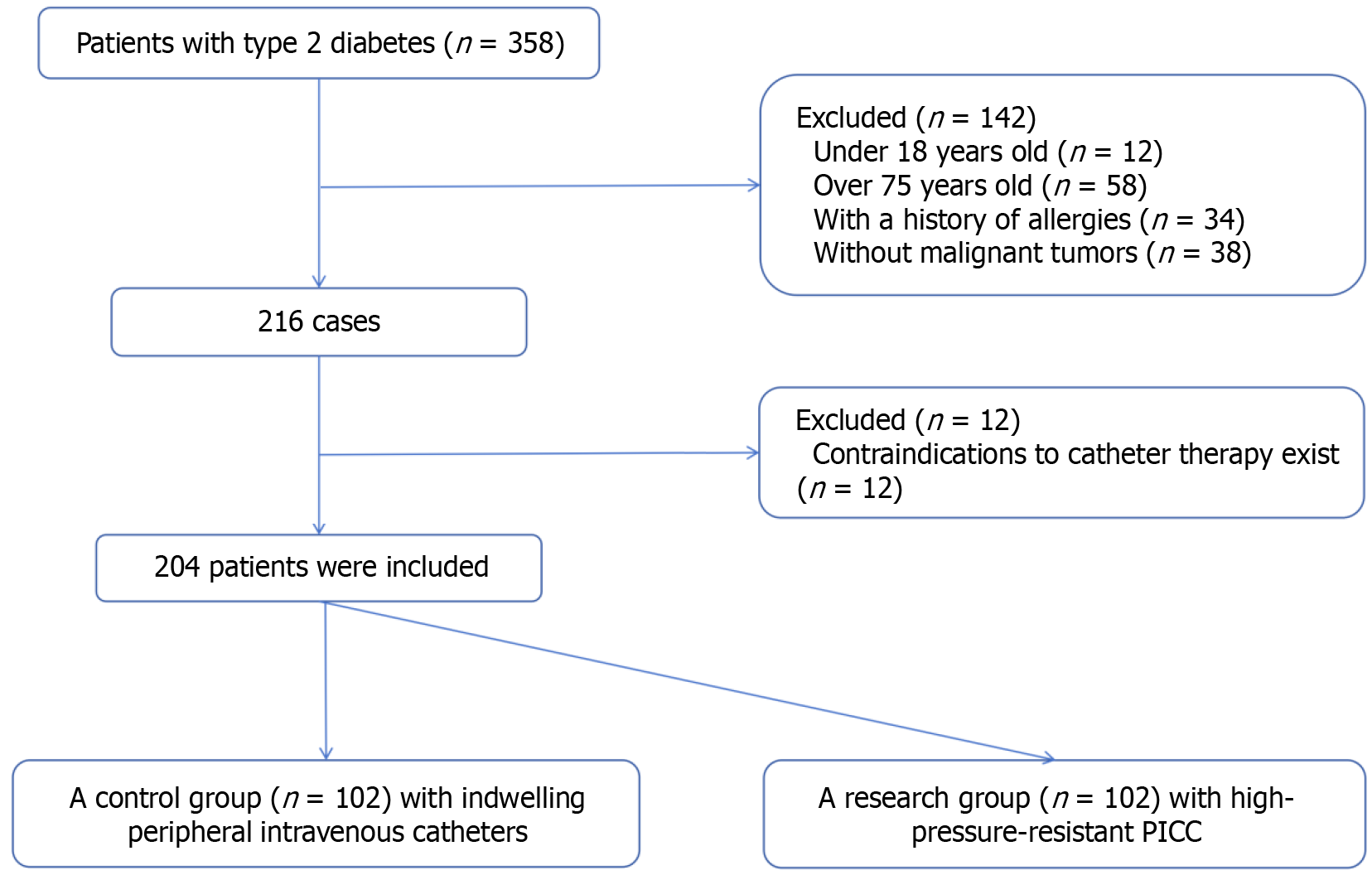
This retrospective study analyzed 204 diabetic patients with malignancies treated at The Second Affiliated Hospital, Jiangxi Medical College, Nanchang University, from January 2024 to June 2024. The patients were divided into two groups: A control group (n = 102) with indwelling peripheral intravenous catheters and a research group (n = 102) with high-pressure-resistant PICC. The study compared baseline data, the incidence of iodine contrast extravasation during CECT, the incidence of adverse events (discomfort, redness and swelling at the puncture site, and blood oozing), imaging quality, nursing time, intubation success rate, number of venipuncture attempts, and catheter maintenance cost.
Male patients accounted for 51.96% in the control group and 55.88% in the research group; the average age was (59.68 ± 11.82) years in the control group and (61.41 ± 12.92) years in the research group; the proportions of lung cancer, colorectal cancer, and gastric cancer patients in the control group were 42.16%, 38.24%, and 19.61%, respectively, while those in the research group were 34.31%, 37.25%, and 28.43%, respectively. Except for the gender distribution, age, and cancer type mentioned above, other general information such as underlying diseases, puncture location, and long-term chemotherapy shows no significant differences as tested (P > 0.05). The results showed that the research group had significantly reduced incidence of iodine contrast extravasation (7 vs 1, P = 0.031), similar incidence of adverse events (11 vs 7, P = 0.324), reduced nursing time [(18.50 ± 2.68) minutes vs (13.26 ± 3.00) minutes, P = 0.000], fewer venipuncture attempts [(2.21 ± 0.78) times vs (1.49 ± 0.58) times, P = 0.000], lower catheter maintenance cost [(1251.79 ± 205.47) China yuan (CNY) vs (1019.25 ± 117.28) CNY, P = 0.000], increased intubation success rate (16.67% vs 58.82%, P = 0.000), and better imaging quality (85.29% vs 94.12%, P = 0.038).
High-pressure-resistant PICCs can lessen the physical burden of diabetic patients during nursing, reduce treatment costs, and improve the efficiency and quality of imaging for diagnosis malignant tumors.
Core Tip: For patients with diabetes mellitus complicated by malignant tumors, there is potential for improving the administration of intravenous contrast agents during contrast-enhanced computerized tomography (CECT). High-pressure-resistant peripherally inserted central catheters (PICCs) may be a better option for this improvement. This study has demonstrated the advantages of using high-pressure-resistant PICC in CECT for such patients, including reducing the physical burden during nursing, lowering treatment costs, and enhancing the efficiency and quality of imaging. These novel findings offer a strong research foundation for future research.
- Citation: Zhang L, Yan HF. Application value of high-pressure-resistant peripherally inserted central catheters in enhanced computer tomography of diabetic patients with malignant tumors. World J Diabetes 2024; 15(12): 2293-2301
- URL: https://www.wjgnet.com/1948-9358/full/v15/i12/2293.htm
- DOI: https://dx.doi.org/10.4239/wjd.v15.i12.2293
Diabetes mellitus (DM) is a common chronic metabolic disorder, characterized by chronic hyperglycemia caused by insulin resistance or insulin deficiency[1-3]. Diabetic patients are more prone to developing malignancies. It is estimated that DM patients have a significantly higher risk of colorectal, hepatocellular, gallbladder, breast, endometrial, and pancreatic cancers than non-diabetic individuals[4]. However, diagnosing DM complicated by malignancies is challenging, and some antidiabetic agents may mask the symptoms and features of malignancies. Recent advancements in anatomical imaging techniques have significantly improved the detection of malignant diseases. Among these, contrast-enhanced computed tomography (CECT) shows great advantages because of its high sensitivity, high specificity, and higher quality of imaging. In addition, CECT scans are well-tolerated and artifact-free with rapid imaging[5]. Therefore, CECT is expected to be used for early diagnosis and identification of malignancies in DM patients.
During CECT examination, iodine contrast, an intravenous contrast agent, is injected through a scalp steel needle or an intravenous indwelling needle, which may cause adverse reactions in the patient. Moreover, high-pressure injection may increase the risk of iodine contrast extravasation (ICE) and cause symptoms like pain, fever, and vomiting[6,7]. Therefore, there is potential for improvement in how intravenous contrast media is administered. Clinical data suggest that high-pressure-resistant peripherally inserted central catheters (PICCs) are associated with a significantly reduced risk of deep venous thrombosis, accidental catheter removal, and catheter-related infection compared to indwelling central venous catheters[8,9], indicating a wider application prospect of high-pressure-resistant PICCs in clinical imaging.
Previous studies have used high-pressure-resistant PICCs in diagnosing and detecting malignant tumors and obtained high-quality lesion images[10]. However, there is a lack of research on the application of PICCs in CECT examinations for DM patients with malignant tumors. To address this problem, this study intends to select diabetic patients with malignancies as the research subjects, dividing them into a control group and a research group according to the catheter placement method, to compare their differences in terms of safety during CECT, imaging quality, nursing time, catheter maintenance cost, etc., in order to confirm the advantages of using PICCs in CECT examination of such patients and provide a research basis for future research.
From January to June 2024, patients with type 2 DM (T2DM) complicated by malignant tumors, who were admitted to The Second Affiliated Hospital, Jiangxi Medical College, Nanchang University, and scheduled for CECT scanning were selected.
Inclusion criteria were as follows: Patients were diagnosed with T2DM by biochemical indicators, etc., and met the Chinese Guidelines for the Prevention and Treatment of T2DM (2020 Edition) (I) diagnostic criteria; patients were diagnosed with malignant tumor by histopathological examination, and were to undergo chemotherapy treatment and CECT scanning; patients met the indications for PICC catheterization and peripheral venous catheterization; patients were 18-75 years old and voluntarily participated in this study with informed consent.
Exclusion criteria were as follows: Contraindications to catheter therapy; contraindications to CECT scanning; history of allergies.
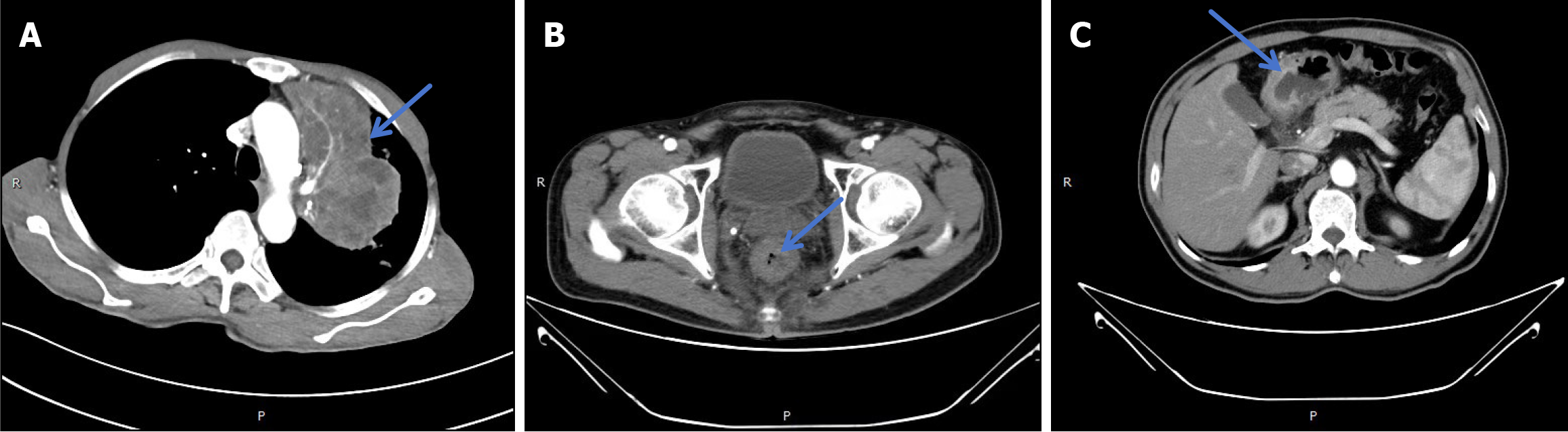
A total of 204 patients strictly following the inclusion criteria were enrolled in this study. The flowchart of specific inclusion and exclusion criteria for patients is shown in Figure 1. They were grouped depending on the difference in the catheter type used: A control group (n = 102) receiving indwelling peripheral intravenous catheters and a research group (n = 102) receiving high-pressure-resistant PICC. The control group consisted of 53 males and 49 females aged (59.68 ± 11.82) years on average, with 43 cases of lung cancer, 39 cases of colorectal cancer, and 20 cases of gastric cancer (imaging results shown in Figure 2). The research group had a male-to-female ratio of 57:45, an average age of 61.41 ± 12.92 years, and 35 cases of lung cancer, 38 cases of colorectal cancer, and 29 cases of gastric cancer.
Primary outcome measures: (1) Occurrence, specific grade, and definition of ICE during CT scanning (Table 1). No extravasation, mild extravasation, moderate extravasation, and severe extravasation were rated as grades 0, 1-2, 3, and 4, respectively; (2) Image quality of CECT: Table 2 for specific grades and definitions; and (3) Daily care time: The time spent in daily nursing refers to the total duration of nursing services provided by nurses every day. Nursing services mainly included preoperative assessment, pre-catheterization life care, health education, psychological care, catheteri
| Symptom | Grade |
| No obvious symptoms | 0 |
| Edema diameter < 2.54 cm | 1 |
| 2.54 cm < edema diameter < 15.24 cm | 2 |
| Translucent edema (diameter > 15.24 cm) | 3 |
| Edema diameter > 15.24 cm, combined with blood oozing, circulatory disturbance, and moderate to severe pain | 4 |
| Image | Grade |
| Clear vascular display and no artifacts or only a few artifacts, which does not affect the diagnosis | Good |
| Blurred development of important blood vessels or interrupted display of blood vessels, with a large number or all artifacts in arteries, which cannot be used for diagnosis | Poor |
Secondary outcome measures: (1) Adverse events: Discomfort, redness and swelling at the puncture site, and blood oozing; (2) Number of venipuncture attempts; (3) First-attempt intubation success rate; and (4) Catheter maintenance cost after 6 months.
Statistical analysis was conducted using SPSS software (version 21; IBM Corp., Armonk, NY, United States), while image rendering was performed with GraphPad 9.0 software. Categorical variables, expressed as the number of cases (percentage), were analyzed using χ2 tests. Continuous variables, represented as the mean ± variance, were compared using independent samples t-tests. The sample size of this study adhered to the inclusion and exclusion criteria for screening, while meeting the minimum requirement of approximately 55 participants for each group, as determined by the binomial proportion sample size estimation formula. All statistical analyses were two-tailed and relied upon a P < 0.05 statistical criterion.
By independent sample t-test or χ2 test analysis, it was found that the sex distribution (χ2 = 0.316, P = 0.574), age (t = 0.995, P = 0.321), cancer type (χ2 = 2.487, P = 0.288), hypertension (χ2 = 0.179, P = 0.673), coronary heart disease (χ2 = 0.666, P = 0.186), puncture site (χ2 = 0.766, P = 0.682), and long-term chemotherapy (χ2 = 0.091, P = 0.763) were not statistically different, with comparability between groups (Table 3).
| | Control group (n = 102) | Research group (n = 102) | χ2/t | P value |
| Sex | 0.316 | 0.574 | ||
| Male | 53 (51.96) | 57 (55.88) | ||
| Female | 49 (48.04) | 45 (44.12) | ||
| Age (years) | 59.68 ± 11.82 | 61.41 ± 12.92 | 0.995 | 0.321 |
| Cancer type | 2.487 | 0.288 | ||
| Lung cancer | 43 (42.16) | 35 (34.31) | ||
| Colorectal cancer | 39 (38.24) | 38 (37.25) | ||
| Gastric cancer | 20 (19.61) | 29 (28.43) | ||
| Underlying diseases | ||||
| Hypertension | 0.179 | 0.673 | ||
| With | 55 (53.92) | 58 (56.86) | ||
| Without | 47 (46.08) | 44 (43.14) | ||
| Coronary heart disease | 0.666 | 0.186 | ||
| With | 38 (37.25) | 41 (40.20) | ||
| Without | 64 (62.75) | 61 (59.80) | ||
| Puncture site | 0.766 | 0.682 | ||
| Median cubital vein | 14 (13.73) | 11 (10.78) | ||
| Basilic vein | 84 (82.35) | 85 (83.33) | ||
| Cephalic vein | 4 (3.92) | 6 (5.88) | ||
| Long-term chemotherapy | 0.091 | 0.763 | ||
| With | 69 (67.65) | 71 (69.61) | ||
| Without | 33 (32.35) | 31 (30.39) |
Regarding the safety of high-pressure-resistant PICCs, this study first counted the ICE of two groups of patients. As shown in Table 4, there were seven cases of ICE in the control group and one case in the research group. The incidence of extravasation was significantly lower in the research group than in the control group (χ2 = 4.684, P = 0.031).
| Control group (n = 102) | Research group (n = 102) | χ2 | P value | |
| No extravasation | 95 (93.14) | 101 (99.02) | ||
| Mild extravasation | 4 (3.92) | 1 (0.98) | ||
| Moderate extravasation | 1 (0.98) | 0 (0.00) | ||
| Severe extravasation | 2 (1.96) | 0 (0.00) | ||
| Incidence of extravasation | 7 (6.86) | 1 (0.98) | 4.684 | 0.031 |
This study further examined the incidence of adverse events to assess the safety of high-pressure-resistant PICCs (Table 5). In the control group, 5 patients experienced discomfort, 2 redness and swelling at the puncture site, and 4 blood oozing. In the research group, 3 experienced discomfort, 1 redness and swelling at the puncture site, and 3 blood oozing. There was no statistically significant difference in the incidence of adverse events between the research and control groups (χ2 = 0.975, P = 0.324).
| Control group (n = 102) | Research group (n = 102) | χ2 | P value | |
| Discomfort | 5 (4.90) | 3 (2.94) | ||
| Redness and swelling at the puncture site | 2 (1.96) | 1 (0.98) | ||
| Blood oozing | 4 (3.92) | 3 (2.94) | ||
| Incidence rate of adverse events | 11 (10.78) | 7 (6.86) | 0.975 | 0.324 |
In this study, CECT scan quality was assessed to evaluate the benefits of using high-pressure-resistant PICCs. As shown in Table 6, there were 87 cases with good image quality and 15 cases with poor image quality in the control group, and 96 cases with good image quality and six cases with poor image quality in the research group. The research group had significantly higher image quality than the control group (χ2 = 4.300, P = 0.038).
| Control group (n = 102) | Research group (n = 102) | χ2 | P value | |
| 4.300 | 0.038 | |||
| Good | 87 (85.29) | 96 (94.12) | ||
| Poor | 15 (14.71) | 6 (5.88) |
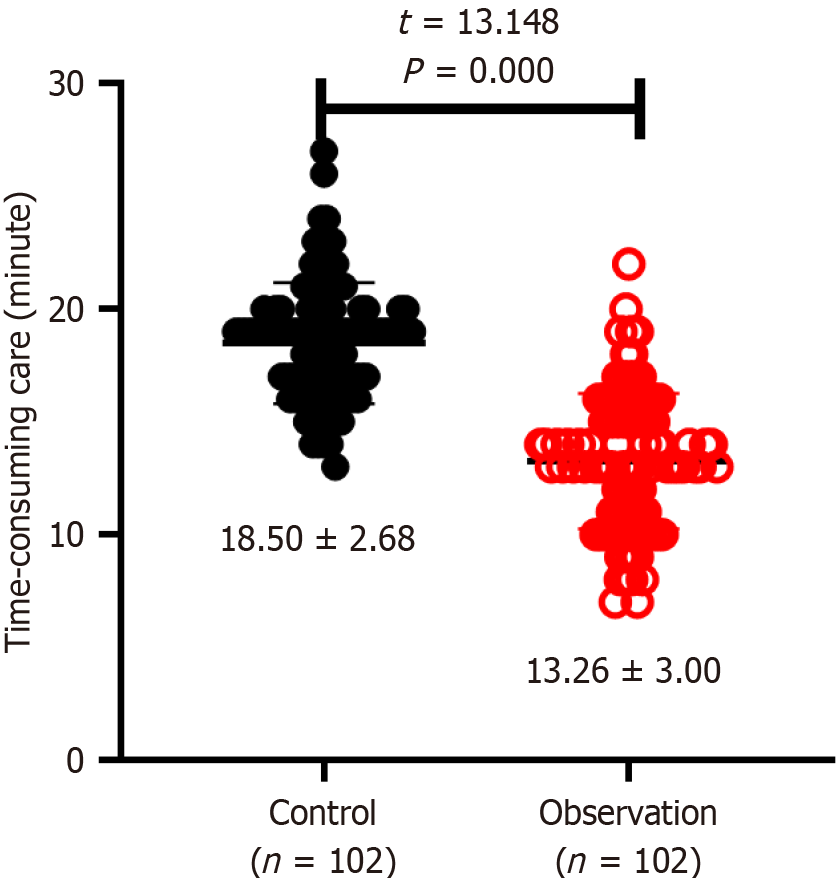
Figure 3 shows the time spent on each nursing session by two patient groups. The duration of each nursing session was 18.50 ± 2.68 minutes in the control group and 13.26 ± 3.00 minutes in the research group. The independent sample t-test showed that the research group had significantly less nursing time than the control group (t = 13.148, P = 0.000).
Table 7 shows the number of venipuncture attempts, intubation success rate, and catheter maintenance cost for the two groups. The intubation success rate was higher in the research group than in the control group (χ2 = 38.570, P = 0.000). The research group had fewer venipuncture attempts (t = 7.486, P = 0.000) and lower catheter maintenance costs after 6 months (t = 9.927, P = 0.000) than the control group.
| Control group (n = 102) | Research group (n = 102) | χ2/t | P value | |
| Number of venipuncture attempts | 2.21 ± 0.78 | 1.49 ± 0.58 | 7.486 | 0.000 |
| Success intubation | 38.570 | 0.000 | ||
| Yes | 17 (16.67) | 60 (58.82) | ||
| No | 85 (83.33) | 42 (41.18) | ||
| Catheter maintenance cost after 6 months (CNY) | 1251.79 ± 205.47 | 1019.25 ± 117.28 | 9.927 | 0.000 |
DM patients are at significantly increased risk of developing malignancies[11-14]. Meanwhile, the survival rate of diabetic cancer patients is significantly lower compared to non-diabetic cancer patients[15-18]. Early cancer screening can help reduce mortality and prolong survival, but the consistency in cancer screening appears to be lower in DM patients than in non-diabetic patients[19], suggesting that DM can impact the effectiveness of early cancer diagnosis. Advancements in imaging technology offer solutions for improving cancer screening in diabetic patients, in which CECT plays a crucial role.
However, the traditional needle placement method used in CECT be burdensome for patients. Clinical data suggests that continuous and repeated venipunctures may lead to ICE. PICCs, on the conversely, offer an alternative to central venous catheterization via the jugular vein, providing central venous access with a reduced risk of intraoperative compli
This study also explored the impact of high-pressure-resistant PICC on CECT imaging quality. The findings indicate that high-pressure-resistant PICC significantly improved CECT imaging quality compared to conventional cathete
This study also found the economic advantages of using high-pressure-resistant PICC. An economic evaluation of PICC compared to other venous access devices pointed out that PICC may be more cost-effective[26]. Based on the results of this study, this type of PICC also helps improve the efficiency of care and reduce catheter maintenance costs. In this study, the use of high-pressure PICC shortened the time spent on each nursing session compared to conventional catheters, thereby reducing the clinical pressure on medical staff. This method also reduced the number of venipuncture attempts and improved the intubation success rate, effectively lessening the physical burden on patients during CECT. The results also showed a reduction in catheter maintenance costs with high-pressure-resistant PICC, suggesting it may help alleviate the economic burden. These findings align with the report by Wang et al[27], which also demonstrated that high-pressure-resistant PICC is more cost-effective than totally implanted venous access devices (ports) within a 3-9-month dwell time.
This study has some limitations. First, the sample size is limited because it was conducted at a single trial. Second, more detailed information on the types and severity of adverse events would have provided a better understanding of PICC safety. Third, the lack of long-term follow-up prevented exploration of factors affecting CECT imaging. Finally, for future research, a large-scale, multicenter prospective study and long-term follow-up are necessary to provide a research foundation for follow-up studies, which is crucial for evaluating long-term outcomes such as infection rates, long-term catheter-related complications, and patient satisfaction. The significance of this study lies in confirming the application advantages of high-pressure-resistant PICC in CECT examinations of DM patients complicated by malignant tumors, mainly manifested in minimizing the risk of ICE events to reduce the physical burden on patients and improving the imaging quality of CECT scans while reducing nursing time and catheter maintenance costs over a six-month period, which is of great value for reducing the medical and economic burdens of patients and society.
In summary, this study confirms that high-pressure-resistant PICC can reduce the physical burden of patients during nursing, reduce treatment costs, and improve the efficiency and quality of CECT imaging. These findings reveal the value of using high-pressure-resistant PICC in DM patients with malignant tumors, which provides a strong research basis for future research.
| 1. | Petersmann A, Müller-Wieland D, Müller UA, Landgraf R, Nauck M, Freckmann G, Heinemann L, Schleicher E. Definition, Classification and Diagnosis of Diabetes Mellitus. Exp Clin Endocrinol Diabetes. 2019;127:S1-S7. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 425] [Cited by in RCA: 303] [Article Influence: 43.3] [Reference Citation Analysis (0)] |
| 2. | Cloete L. Diabetes mellitus: an overview of the types, symptoms, complications and management. Nurs Stand. 2022;37:61-66. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 272] [Cited by in RCA: 186] [Article Influence: 46.5] [Reference Citation Analysis (0)] |
| 3. | Antar SA, Ashour NA, Sharaky M, Khattab M, Ashour NA, Zaid RT, Roh EJ, Elkamhawy A, Al-Karmalawy AA. Diabetes mellitus: Classification, mediators, and complications; A gate to identify potential targets for the development of new effective treatments. Biomed Pharmacother. 2023;168:115734. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 468] [Cited by in RCA: 252] [Article Influence: 84.0] [Reference Citation Analysis (7)] |
| 4. | Pearson-Stuttard J, Papadimitriou N, Markozannes G, Cividini S, Kakourou A, Gill D, Rizos EC, Monori G, Ward HA, Kyrgiou M, Gunter MJ, Tsilidis KK. Type 2 Diabetes and Cancer: An Umbrella Review of Observational and Mendelian Randomization Studies. Cancer Epidemiol Biomarkers Prev. 2021;30:1218-1228. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 226] [Cited by in RCA: 190] [Article Influence: 38.0] [Reference Citation Analysis (0)] |
| 5. | Kulkarni NM, Fung A, Kambadakone AR, Yeh BM. Computed Tomography Techniques, Protocols, Advancements, and Future Directions in Liver Diseases. Magn Reson Imaging Clin N Am. 2021;29:305-320. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 53] [Cited by in RCA: 41] [Article Influence: 8.2] [Reference Citation Analysis (0)] |
| 6. | Huynh K, Baghdanian AH, Baghdanian AA, Sun DS, Kolli KP, Zagoria RJ. Updated guidelines for intravenous contrast use for CT and MRI. Emerg Radiol. 2020;27:115-126. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 47] [Article Influence: 7.8] [Reference Citation Analysis (0)] |
| 7. | Qiu H, Li WP. Contrast-induced ischemic colitis following coronary angiography: A case report. World J Clin Cases. 2023;11:4937-4943. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Reference Citation Analysis (0)] |
| 8. | Schears GJ, Ferko N, Syed I, Arpino JM, Alsbrooks K. Peripherally inserted central catheters inserted with current best practices have low deep vein thrombosis and central line-associated bloodstream infection risk compared with centrally inserted central catheters: A contemporary meta-analysis. J Vasc Access. 2021;22:9-25. [PubMed] [DOI] [Full Text] |
| 9. | Shimizu Y, Hatachi T, Takeshita J, Inata Y, Kyogoku M, Aoki Y, Taniguchi M, Kawamura A, Okumura J, Takeuchi M. Occurrence and Risk Factors for Unplanned Catheter Removal in a PICU: Central Venous Catheters Versus Peripherally Inserted Central Venous Catheters. Pediatr Crit Care Med. 2020;21:e635-e642. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 11] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 10. | Sapkota S, Sannur R, Naik R. Analysis of Peripherally Inserted Central Catheter Line in Cancer Patients: A Single-Center Experience. South Asian J Cancer. 2020;9:253-256. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 9] [Reference Citation Analysis (0)] |
| 11. | Lawler T, Walts ZL, Steinwandel M, Lipworth L, Murff HJ, Zheng W, Warren Andersen S. Type 2 Diabetes and Colorectal Cancer Risk. JAMA Netw Open. 2023;6:e2343333. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 62] [Article Influence: 20.7] [Reference Citation Analysis (0)] |
| 12. | Srivastava SP, Goodwin JE. Cancer Biology and Prevention in Diabetes. Cells. 2020;9:1380. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 20] [Cited by in RCA: 52] [Article Influence: 8.7] [Reference Citation Analysis (0)] |
| 13. | Ahmad I, Suhail M, Ahmad A, Alhosin M, Tabrez S. Interlinking of diabetes mellitus and cancer: An overview. Cell Biochem Funct. 2023;41:506-516. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 8] [Reference Citation Analysis (0)] |
| 14. | Suh S, Kim KW. Diabetes and Cancer: Cancer Should Be Screened in Routine Diabetes Assessment. Diabetes Metab J. 2019;43:733-743. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 65] [Cited by in RCA: 137] [Article Influence: 19.6] [Reference Citation Analysis (4)] |
| 15. | Storey S, Zhang Z, Luo X, Von Ah D, Metzger M, Zhang J, Jakka A, Huang K. Association of Comorbid Diabetes With Clinical Outcomes and Healthcare Utilization in Colorectal Cancer Survivors. Oncol Nurs Forum. 2021;48:195-206. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 2] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 16. | Chen S, Tao M, Zhao L, Zhang X. The association between diabetes/hyperglycemia and the prognosis of cervical cancer patients: A systematic review and meta-analysis. Medicine (Baltimore). 2017;96:e7981. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 29] [Cited by in RCA: 45] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 17. | Harborg S, Kjærgaard KA, Thomsen RW, Borgquist S, Cronin-Fenton D, Hjorth CF. New Horizons: Epidemiology of Obesity, Diabetes Mellitus, and Cancer Prognosis. J Clin Endocrinol Metab. 2024;109:924-935. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 63] [Article Influence: 31.5] [Reference Citation Analysis (2)] |
| 18. | Stein KB, Snyder CF, Barone BB, Yeh HC, Peairs KS, Derr RL, Wolff AC, Brancati FL. Colorectal cancer outcomes, recurrence, and complications in persons with and without diabetes mellitus: a systematic review and meta-analysis. Dig Dis Sci. 2010;55:1839-1851. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 116] [Cited by in RCA: 117] [Article Influence: 7.3] [Reference Citation Analysis (0)] |
| 19. | Miller EA, Pinsky PF. Cervical cancer screening and predictors of screening by diabetes status. Cancer Causes Control. 2022;33:1305-1312. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |
| 20. | Montanarella MJ, Agarwal A, Moon B. Peripherally Inserted Central Catheter (PICC) Line Placement. 2024 Jan 10. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. [PubMed] |
| 21. | Gravdahl E, Steine S, Augestad KM, Fredheim OM. Use and safety of peripherally inserted central catheters and midline catheters in palliative care cancer patients: a retrospective review. Support Care Cancer. 2023;31:580. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 22. | Maki J, Sumie M, Ide T, Nagamatsu M, Matsushita K, Shirozu K, Higashi M, Yamaura K. A pressure-resistant peripherally inserted central catheter is as useful as a central venous catheter for rapid fluid infusion: an in vitro study. BMC Anesthesiol. 2022;22:205. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 23. | Washio H, Kashimoto K, Sakashita N, Ohira S, Tanaka J, Maeda N, Shimada M, Kawamata M, Yoneda A, Nakanishi K. Practical use of the central venous access port for contrast-enhanced CT: comparison with peripheral intravenous access regarding enhancement and safety. Clin Radiol. 2024;79:213-220. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 24. | Owens TC, Anton N, Attia MF. CT and X-ray contrast agents: Current clinical challenges and the future of contrast. Acta Biomater. 2023;171:19-36. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 46] [Reference Citation Analysis (0)] |
| 25. | Zhang P, Ma X, Guo R, Ye Z, Fu H, Fu N, Guo Z, Zhang J, Zhang J. Organic Nanoplatforms for Iodinated Contrast Media in CT Imaging. Molecules. 2021;26. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 25] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 26. | Wang K, Zhong J, Huang N, Zhou Y. Economic evaluation of peripherally inserted central catheter and other venous access devices: A scoping review. J Vasc Access. 2020;21:826-837. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 27] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 27. | Wang K, Zhou Y, Huang N, Lu Z, Zhang X. Peripherally inserted central catheter versus totally implanted venous port for delivering medium- to long-term chemotherapy: A cost-effectiveness analysis based on propensity score matching. J Vasc Access. 2022;23:365-374. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 14] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
Open-Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/