Published online Mar 16, 2026. doi: 10.4253/wjge.v18.i3.116646
Revised: December 21, 2025
Accepted: January 19, 2026
Published online: March 16, 2026
Processing time: 116 Days and 15.7 Hours
Single-operator colonoscopy is widely used in clinical practice; however, research on bilateral upper limb surface electromyography (sEMG) activity during ins
To analyze bilateral upper limb muscle activation and fatigue during single-operator colonoscopy insertion under different bowel loop configurations. We also propose strategies for ergonomic improvements and occupational health ma
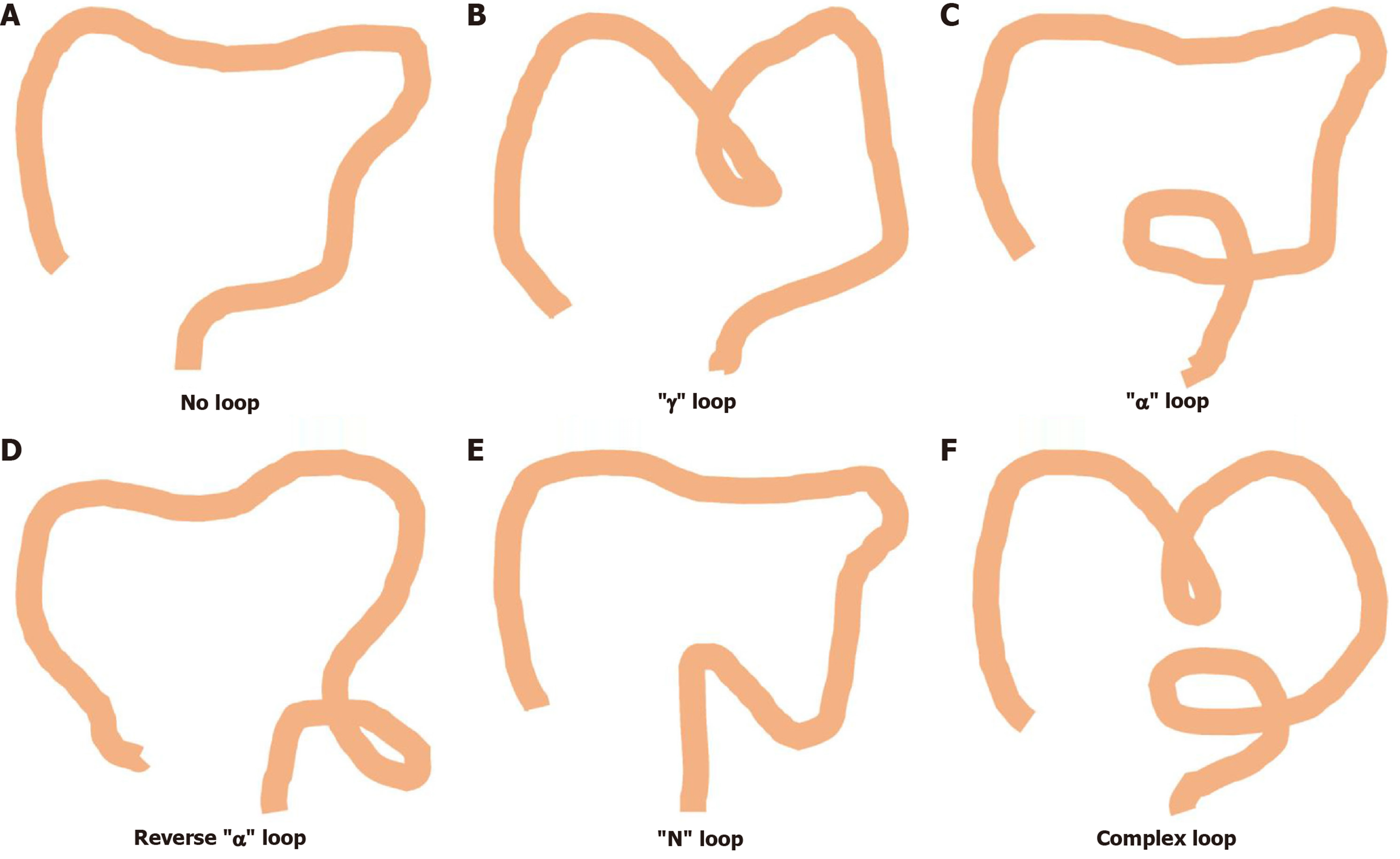
The sEMG signals were recorded from 14 bilateral upper limb muscles of an experienced endoscopist performing a colonoscopy on a simulated colorectal model. Six loop configurations (no loop, “α” loop, reverse “α” loop, “N” loop, “γ” loop, complex loop) were tested. Muscle activation intensity (root mean square) and fatigue [median power frequency (MPF)] were analyzed using myoMUSCLE at a sampling rate of 1500 Hz. Statistical correlations between loop complexity, procedure time, and muscle load were evaluated.
The insertion time of various intestinal loops is between 53.6 seconds and 112.0 seconds. Significant differences in bilateral upper limb sEMG activity were observed across various intestinal loop states (no loop vs other loops, P < 0.05). Complex loop induced the highest muscle load (left extensor digitorum root mean square at 370.6 μV) and rapid fatigue (right extensor digitorum MPF difference: 31.8%). A marked bilateral asymmetry was observed: The left extensor digitorum maintained consistently high activation across all tasks, while the right forearm muscles exhibited load-specificity to fine control maneuvers. A positive correlation was found between insertion time and MPF slope decline, strongest for the left flexor carpi radialis (r = 0.59) and right middle deltoid (r = 0.57), indicating time-sensitive fatigue in these stabilizer muscles. The data objectively quantify the elevated biomechanical demand imposed by challenging endoscopic maneuvers.
This exploratory biomechanical investigation suggests that complex loops significantly increase muscle strain and fatigue risk. Ergonomic solutions and time-restricted protocols are proposed to mitigate occupational injuries. This study provides biomechanical evidence for optimizing colonoscopy workflows and device design.
Core Tip: This surface electromyography study quantitatively reveals that complex intestinal loops during single-operator colonoscopy induce significant bilateral upper limb muscle strain, with the left extensor digitorum bearing the highest load. Rapid fatigue occurs in specific muscles during prolonged maneuvers. We propose evidence-based ergonomic solutions, including motor-assisted handles, variable-stiffness colonoscopes, and time-restricted operating protocols for high-risk loops, to mitigate occupational injuries and guide the design of next-generation endoscopic devices.
- Citation: Wang RG, Wang YQ, Cao H. Bilateral upper limb surface electromyography analysis during single-operator colonoscopy: Implications for ergonomics and occupational health. World J Gastrointest Endosc 2026; 18(3): 116646
- URL: https://www.wjgnet.com/1948-5190/full/v18/i3/116646.htm
- DOI: https://dx.doi.org/10.4253/wjge.v18.i3.116646
Colonoscopy is a key method for diagnosing and treating colorectal diseases and is widely used in clinical practice. Single-operator colonoscopy not only improves operational efficiency but also reduces the dependence on medical resources[1]. Compared with the traditional two-person operation, single-operator colonoscopy requires the operator to coordinate the bilateral upper limbs to complete the compound actions of “rotation-advancement-loop resolution”. The repetitiveness and asymmetry of the operation impose a huge biomechanical load on endoscopists, leading to a high inci
Single-operator colonoscopy requires maintaining operational precision while coordinating the complex movements of the bilateral upper limbs. The mechanical load during loop resolution is a key factor leading to operational fatigue, but the relevant biomechanical mechanisms are not clear. Surface electromyography (sEMG) technology can record muscle electrical activity in real time, and analyzing the electromyographic characteristics of muscles can provide an in-depth understanding of muscle contraction status, fatigue degree, and motor control patterns[4,5]. The utility of sEMG extends beyond fatigue assessment, serving as a cornerstone for quantifying muscle strength and rehabilitation outcomes, as demonstrated in upper limb rehabilitation assessment systems[6].
Despite advances in endoscopy technology, few studies have quantified the state of bilateral upper limb muscles during colonoscopy loop resolution, which is key to colonoscopy and highly biomechanically complex[7,8]. From clinical practice, we know that the precise and complex movements of the bilateral upper limb muscles play a decisive role in single-operator colonoscopy. Therefore, studying the sEMG of bilateral upper limb muscles during single-operator colo
Therefore, this exploratory case study aimed to: (1) Quantify bilateral upper limb muscle activation and fatigue during six standardized loop configurations; and (2) Identify specific muscles and maneuvers associated with the highest bio
An experienced male endoscopist from the Department of Gastroenterology, Beijing Tsinghua Changgung Hospital, was included. His basic information is as follows: Age: 35 years, height: 185 cm, weight: 92.5 kg, body mass index: 27.0 kg/m2; upper limb length: 71.5 cm, palm length: 20.8 cm, palm width: 11 cm; he has 10 years of experience in digestive endo
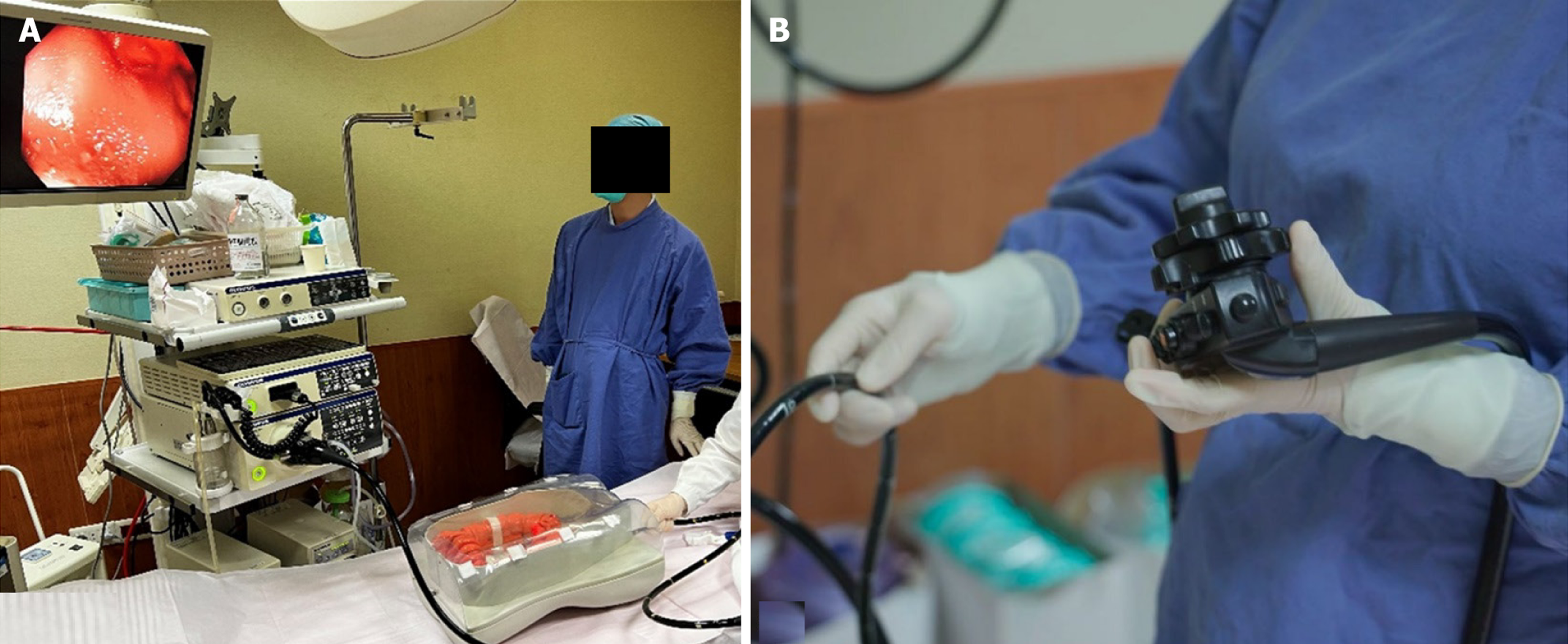
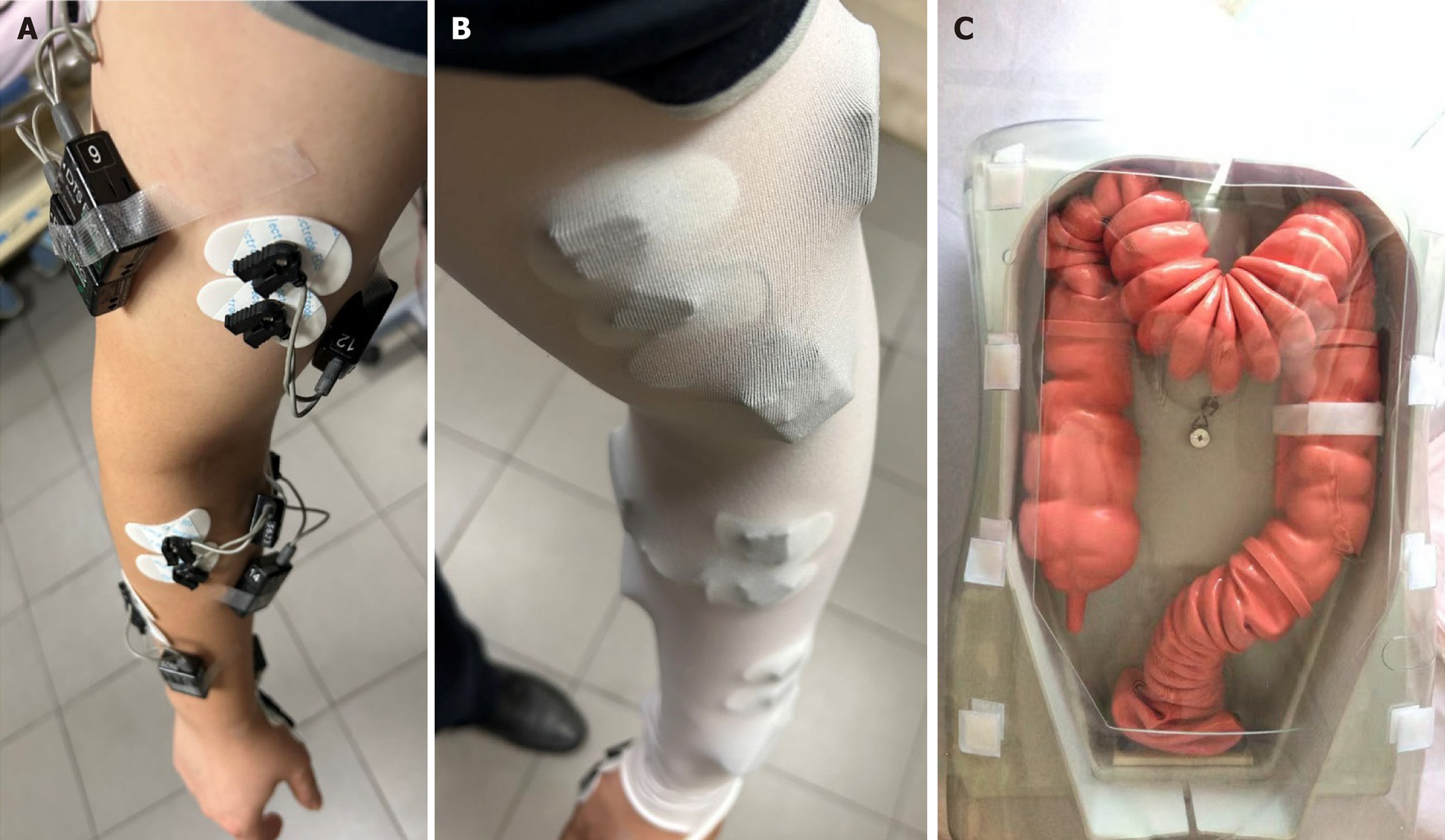
Equipment: (1) Endoscopy system: EVIS LUCERA ELITE CV-290 (Olympus, Japan), colonoscope: CF-HQ290 (Olympus, Japan); (2) Colonoscopy training model (KOKEN, Japan), which can set different intestinal loops in the sigmoid colon and transverse colon (Figure 1); (3) sEMG acquisition equipment: Ultium EMG (Noraxon, AZ, United States); and (4) Analysis software: MyoRESEARCH (Noraxon, AZ, United States).
The KOKEN model was used to generate standardized loop geometries under controlled, repeatable conditions. It must be noted that the material properties (e.g., viscoelasticity, compliance, surface friction) of the simulated bowel differ inherently from those of living human intestine. Furthermore, the model cannot simulate physiological peristalsis, vas
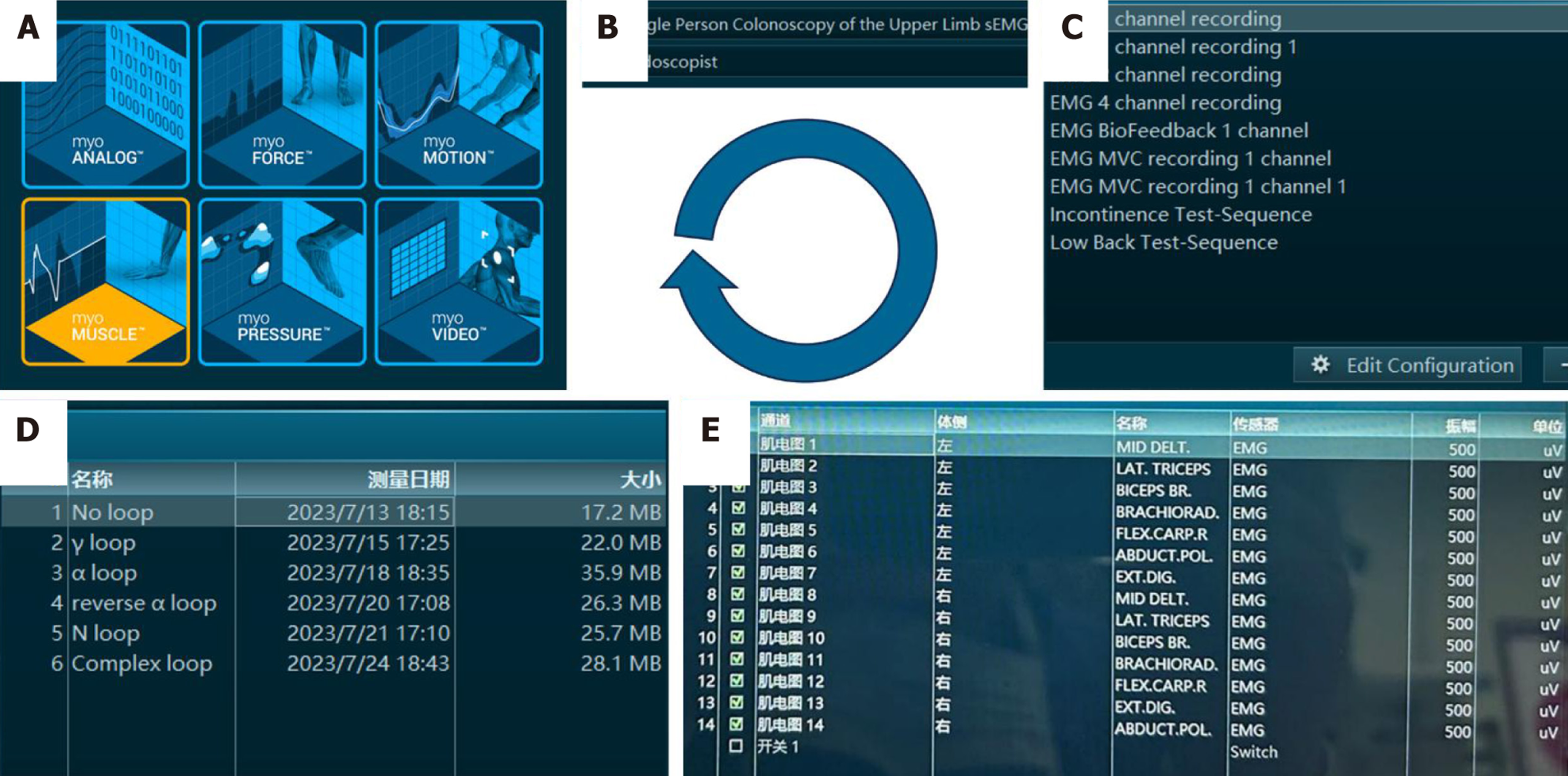
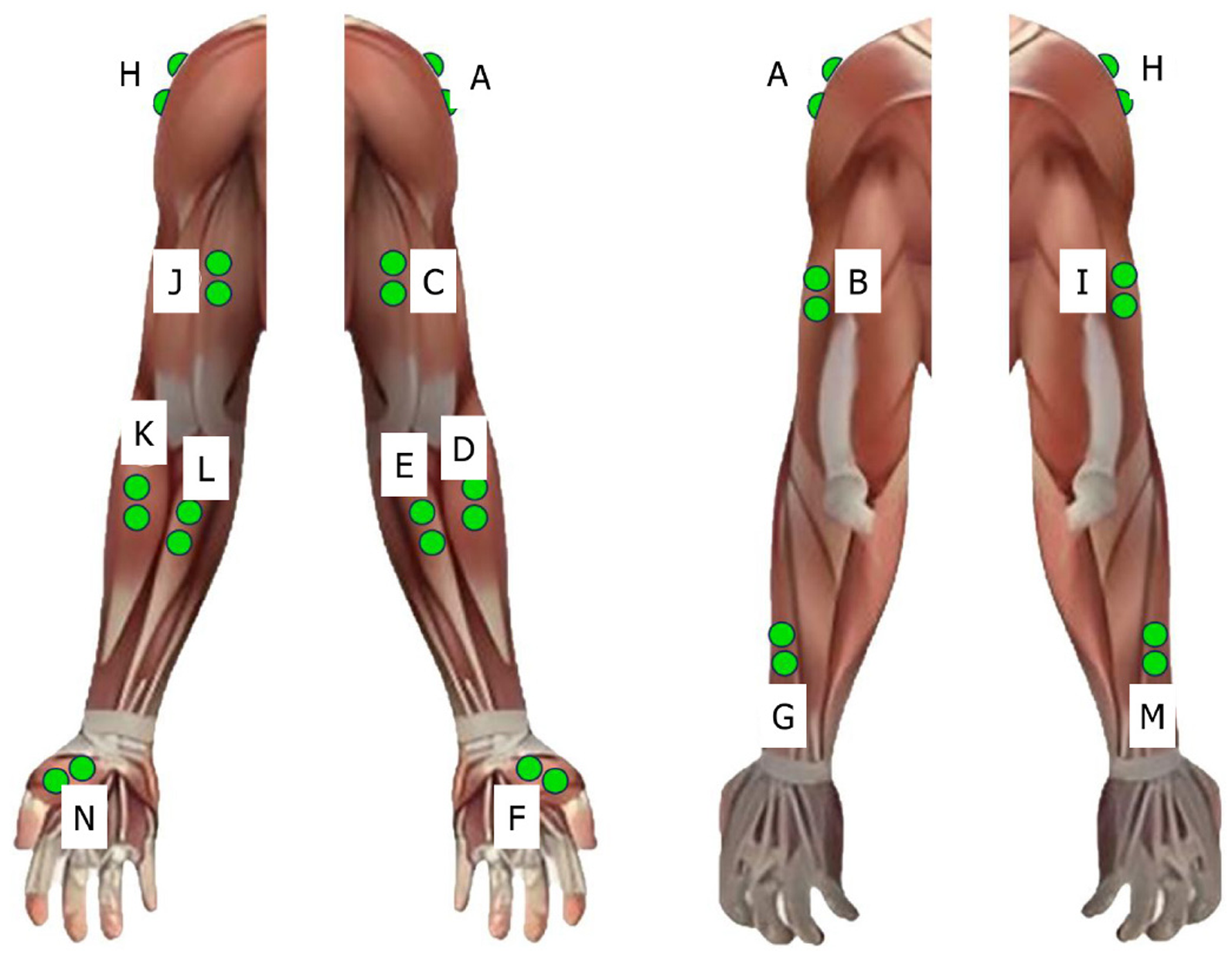
sEMG acquisition: The sEMG acquisition procedure in this study was as follows (Figure 2): First, open the myoRE
The data analysis process of this study included three main parts: Data preprocessing, feature extraction, and descriptive analysis. The electromyographic signals were preprocessed (including filtering and noise reduction), and the root mean square (RMS) of the electromyographic activity was calculated to assess muscle activity intensity. In assessing muscle fatigue degree, this study chose the median power frequency (MPF) due to the short insertion time of colonoscopy. MPF is the frequency point that divides the power spectrum area into two equal parts and is more sensitive to changes in the low-frequency components of the spectrum, allowing earlier detection of muscle fatigue-induced spectral shift to the left (low-frequency conversion). MPF is less affected by high-frequency noise (such as equipment interference), resulting in higher data stability. The MPF difference was calculated through linear regression analysis to reflect the rate of fatigue development, and the intercept indicated the initial activation intensity. We acknowledge the growing sophistication of sEMG analysis. Advanced methods, such as optimization algorithms for feature selection and dynamic time warping techniques for movement pattern analysis[9,10], represent promising avenues for future, more granular biomechanical investigations.
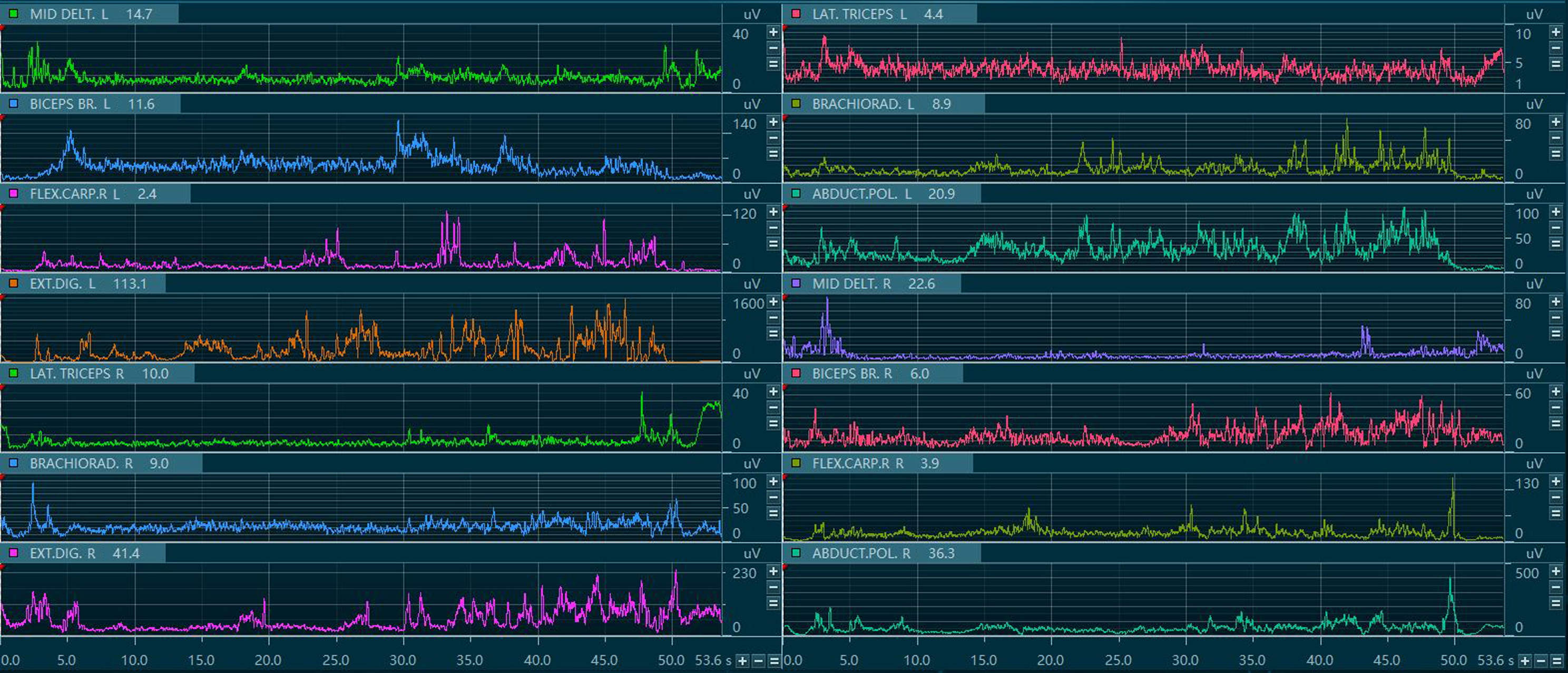
Data preprocessing: To ensure the quality and reliability of the electromyographic signals, the original sEMG data were preprocessed. The main purpose of preprocessing was to remove noise and interference while retaining effective information in the signals. Specific steps included: Applying a bandpass filter to the original electromyographic signals with a frequency range of 20-200 Hz; smoothing filtering of the original signals based on the RMS algorithm (Figure 6).
Feature extraction: In the preprocessed electromyographic signals, the RMS and MPF were extracted as characteristic parameters to represent muscle activation intensity and fatigue degree. Specifically, the calculation of RMS used a 100 milliseconds sliding window, a step size with 50% overlap (1 second) was used to balance temporal resolution with signal stationarity, a common practice for analyzing dynamic, non-stationary muscle contractions. This window width is suitable for capturing sustained muscle activity typical in colonoscopy maneuvers.
The RMS value of each window was obtained by squaring, averaging, and then taking the square root of the ele
To analyze the differences in bilateral upper limb electromyographic activity under different intestinal loop states and their correlation with colonoscopy status, this study used repeated measures analysis of variance. Repeated measures analysis of variance can effectively analyze data changes in the same subject under different conditions while considering the differences and inherent correlations of repeated measurements. In this study, the intestinal loop state was used as the repeated measurement factor, and RMS and MPF were used as dependent variables to statistically analyze the elec
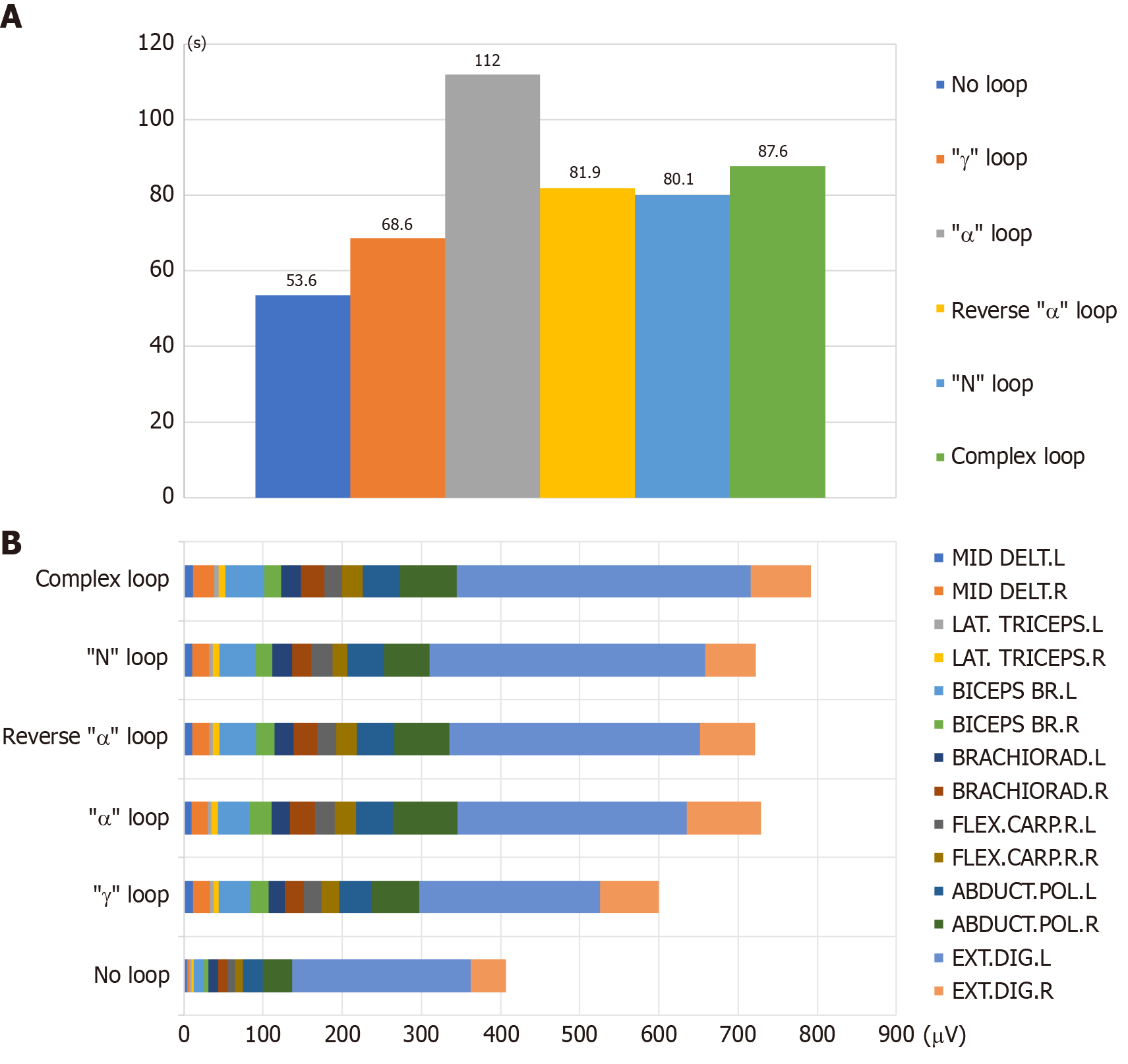
The insertion times for each intestinal loop are shown in the figure below (Figure 7A). The longest insertion time was in the “α” loop state (112.0 seconds), followed by the complex loop state (87.6 seconds), and the shortest was in the no loop state (53.6 seconds).
The RMS data of the bilateral upper limbs during insertion in six intestinal loop states are as follows (Table 1): In the no loop insertion, the RMS of the tested bilateral upper limb muscles was the lowest, indicating relatively low elec
| Loop types | MID DELT | LAT. TRICEPS | BICEPS BR | BRACHIORAD | FLEX.CARP.R | ABDUCT.POL | EXT.DIG | |||||||
| Left | Right | Left | Right | Left | Right | Left | Right | Left | Right | Left | Right | Left | Right | |
| No loop | 3.9 | 3.2 | 2.5 | 3.1 | 13.2 | 5.1 | 11.8 | 12.8 | 8.8 | 10.6 | 25.0 | 37.1 | 225.1 | 44.5 |
| “γ” loop | 11.2 | 21.5 | 5.1 | 6.7 | 39.6 | 22.9 | 20.8 | 24.0 | 22.2 | 21.9 | 40.9 | 60.5 | 228.5 | 74.3 |
| “α” loop | 9.9 | 20.2 | 4.8 | 8.0 | 40.4 | 27.5 | 23.6 | 31.1 | 24.8 | 27.0 | 46.4 | 82.2 | 289.1 | 93.8 |
| Reverse “α” loop | 11.1 | 21.3 | 4.7 | 8.0 | 46.6 | 23.0 | 23.8 | 29.8 | 24.4 | 26.1 | 46.8 | 70.2 | 316.3 | 69.6 |
| “N” loop | 10.8 | 21.0 | 5.2 | 8.3 | 45.2 | 21.0 | 25.0 | 24.9 | 26.2 | 18.9 | 46.3 | 58.0 | 347.2 | 64.8 |
| Complex loop | 12.0 | 26.9 | 5.5 | 8.4 | 48.9 | 21.6 | 25.0 | 29.6 | 22.4 | 25.2 | 47.9 | 71.5 | 370.6 | 76.1 |
During insertion in the “γ” loop and “N” loop states, the RMS of the tested bilateral upper limb muscles was high, respectively, with increased electromyographic activity compared to the no loop state. The left extensor digitorum had the highest activity intensity, at 228.5 μV and 347.2 μV, followed by the right extensor digitorum at 74.3 μV and 64.8 μV, and the left lateral head of the triceps had the lowest muscle activity intensity, at 5.1 μV and 5.2 μV.
During insertion in the “α” loop and reverse “α” loop states, the RMS of the tested bilateral upper limb muscles was higher, respectively, with further increased electromyographic activity compared to the no loop state. The left extensor digitorum had the highest activity intensity, at 289.1 μV and 316.3 μV, followed by the right abductor pollicis longus and extensor digitorum at 70.2 μV and 93.8 μV, and the left lateral head of the triceps had the lowest muscle activity intensity, at 4.8 μV and 4.7 μV.
During insertion in the complex loop state, the RMS of the tested bilateral upper limb muscles was the highest level of electromyographic activity, and the RMS of multiple muscle groups in the bilateral upper limbs was significantly higher than in other states, indicating the most intense muscle activity in various loop states (as shown in Figure 7B). Among them, the left extensor digitorum had the highest activity intensity, at 370.6 μV, followed by the right extensor digitorum and abductor pollicis longus at 76.1 μV and 71.5 μV, and the left lateral head of the triceps had the lowest muscle activity intensity, at 5.5 μV.
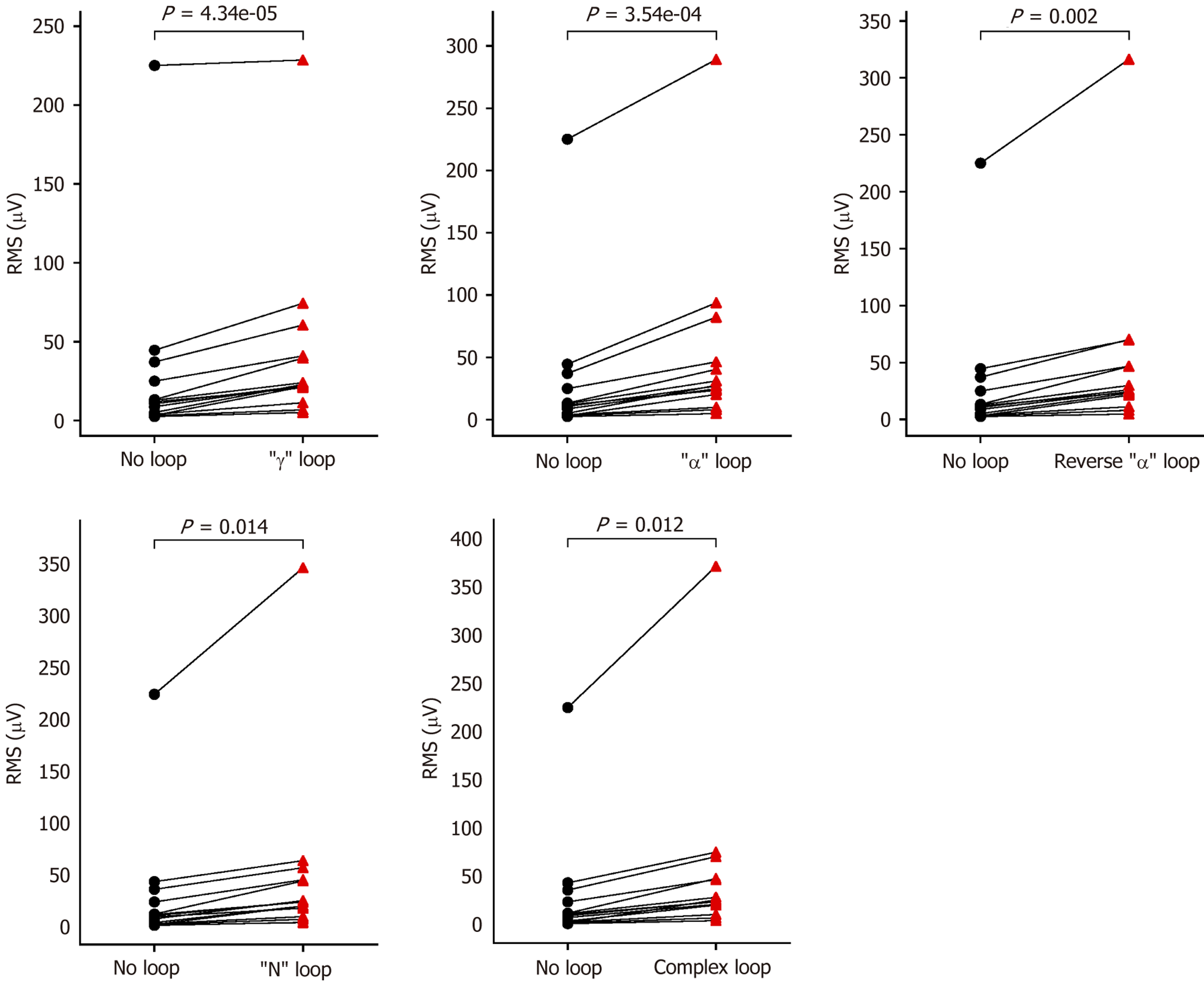
The activity intensity of the 14 bilateral upper limb muscles during insertion in the no loop state was significantly decreased compared to that in other intestinal loop states (P < 0.05), indicating that muscle load significantly increased with operational complexity (Figure 8). After normalization in the time dimension, the RMS value in the complex loop state reached almost 800 μV. The key muscle groups were as follows: (1) The left extensor digitorum had the strongest activation in all states (225.1-370.6 μV), contributing 46.8%-55.3% of the RMS value; and (2) The right extensor digitorum and abductor pollicis longus had specific activation in the complex loop state.
MPF is one of the common indicators for assessing muscle fatigue. When muscles are fatigued, MPF shifts towards the low-frequency direction. It has high sensitivity in reflecting muscle fatigue and can detect the occurrence of muscle fatigue earlier. The MPF data of bilateral upper limb sEMG during insertion in each intestinal loop state are as follows (Tables 2 and 3).
| Loop types | MID DELT | LAT. TRICEPS | BICEPS BR | BRACHIORAD | FLEX.CARP.R | ABDUCT.POL | EXT.DIG | ||||||||||||||
| S | I | Diff% | S | I | Diff% | S | I | Diff% | S | I | Diff% | S | I | Diff% | S | I | Diff% | S | I | Diff% | |
| No loop | 0.0 | 1.2 | 11.6 | 0.0 | 0.9 | 16.7 | 0.0 | 0.9 | 3.4 | 0.0 | 1.0 | 12.1 | 0.0 | 1.3 | 25.7 | 0.0 | 1.0 | 17.9 | 0.0 | 1.2 | 33.9 |
| “γ” loop | 0.0 | 1.1 | 15.1 | 0.0 | 1.0 | 19.8 | 0.0 | 0.9 | 27.6 | 0.0 | 0.9 | 65.2 | 0.0 | 0.9 | 10.1 | 0.0 | 1.1 | 15.7 | 0.0 | 1.8 | 8.8 |
| “α” loop | 0.0 | 0.9 | 49.0 | 0.0 | 1.1 | 23.5 | 0.0 | 1.1 | 0.2 | 0.0 | 1.2 | 41.8 | 0.0 | 1.5 | 33.0 | 0.0 | 1.1 | 2.7 | 0.0 | 1.6 | 1.9 |
| Reverse “α” loop | 0.0 | 1.2 | 46.8 | 0.0 | 0.9 | 14.2 | 0.0 | 1.0 | 24.6 | 0.0 | 1.1 | 33.5 | 0.0 | 1.3 | 35.7 | 0.0 | 1.0 | 18.0 | 0.0 | 1.5 | 22.4 |
| “N” loop | 0.0 | 1.0 | 9.0 | 0.0 | 1.0 | 8.9 | 0.0 | 1.0 | 5.6 | 0.0 | 1.2 | 12.7 | 0.0 | 0.9 | 7.3 | 0.0 | 1.2 | 44.5 | 0.0 | 1.4 | 56.2 |
| Complex loop | 0.0 | 1.1 | 0.6 | 0.0 | 1.0 | 13.2 | 0.0 | 1.0 | 4.0 | 0.0 | 1.2 | 16.1 | 0.0 | 1.3 | 36.1 | 0.0 | 1.2 | 34.4 | 0.0 | 1.3 | 16.2 |
| Loop types | MID DELT | LAT. TRICEPS | BICEPS BR | BRACHIORAD | FLEX.CARP.R | ABDUCT.POL | EXT.DIG | ||||||||||||||
| S | I | Diff% | S | I | Diff% | S | I | Diff% | S | I | Diff% | S | I | Diff% | S | I | Diff% | S | I | Diff% | |
| No loop | 0.0 | 1.3 | 15.9 | 0.0 | 1.1 | 2.4 | 0.0 | 1.3 | 29.6 | 0.0 | 1.1 | 16.9 | 0.0 | 1.2 | 12.2 | 0.0 | 1.1 | 11.3 | 0.0 | 1.2 | 22.4 |
| “γ” loop | 0.0 | 1.3 | 2.6 | 0.0 | 0.9 | 30.4 | 0.0 | 1.0 | 18.8 | 0.0 | 0.9 | 4.0 | 0.0 | 1.2 | 12.5 | 0.0 | 1.2 | 51.2 | 0.0 | 1.0 | 13.4 |
| “α” loop | 0.0 | 1.1 | 21.3 | 0.0 | 1.1 | 30.8 | 0.0 | 1.2 | 20.9 | 0.0 | 1.1 | 20.5 | 0.0 | 1.6 | 15.9 | 0.0 | 1.2 | 56.5 | 0.0 | 1.3 | 19.6 |
| Reverse “α” loop | 0.0 | 1.5 | 31.4 | 0.0 | 1.2 | 25.2 | 0.0 | 1.4 | 24.7 | 0.0 | 1.3 | 60.7 | 0.0 | 1.5 | 10.4 | 0.0 | 1.3 | 36.7 | 0.0 | 1.5 | 37.0 |
| “N” loop | 0.0 | 1.7 | 15.0 | 0.0 | 1.2 | 6.9 | 0.0 | 1.4 | 8.5 | 0.0 | 1.0 | 8.2 | 0.0 | 1.4 | 24.4 | 0.0 | 1.1 | 18.5 | 0.0 | 1.1 | 27.0 |
| Complex loop | 0.0 | 1.2 | 38.4 | 0.0 | 1.2 | 5.1 | -0.0 | 1.3 | 6.9 | 0.0 | 1.2 | 23.1 | 0.0 | 1.4 | 26.5 | 0.0 | 1.5 | 2.0 | 0.0 | 1.3 | 31.8 |
This study found that: (1) During single-operator colonoscopy insertion, the slope of the MPF difference of bilateral upper limb sEMG was close to zero in various intestinal loop states, indicating no significant change in MPF and rela
The specificity of the “α” loop during single-operator colonoscopy insertion is as follows: First, the insertion time takes the longest (112.0 seconds); second, the MPF difference of the left middle deltoid and left lateral head of the triceps was great (49.0% and 23.5%), indicating that prolonged operation directly accelerated fatigue. The complex loop also contains an “α” loop, the specificity of the complex loop during single-operator colonoscopy insertion is as follows (Table 3): First, the insertion time was relatively long (87.6 seconds); second, the MPF difference of the right middle deltoid, bilateral flexor carpi radialis and right extensor digitorum was great (38.4%, 36.1%, 26.5%, and 31.8%), indicating that prolonged operation directly accelerated fatigue; finally, the left extensor digitorum activity was at its peak intensity (RMS at 370.6 μV).
Further verification of the association between high load and low efficiency. Prolonged operation (such as in the “α” loop state) leads to sustained muscle contraction, accumulation of energy metabolism products (such as lactic acid), and causes a spectral shift to the left (decrease in MPF difference), which is consistent with the physiological mechanism of fatigue.
Statistical correlation analysis was performed using Pearson correlation coefficient (r) to analyze the relationship between colonoscopy insertion and bilateral upper limb muscles (Table 4). The insertion time of complex loop was paired with the corresponding key muscles (right middle deltoid, bilateral flexor carpi radialis and right extensor digitorum). The analysis reveals a positive correlation between insertion time and MPF slope for all muscles analyzed. This indicates that longer procedural times are generally associated with a greater rate of MPF decline, signifying accelerated muscle fatigue development. However, the strength of this relationship varies substantially across muscles.
| Loop type | Time (seconds) | MID DELT. R MPF slope (%) | FLEX.CARP.R. L MPF slope (%) | FLEX.CARP.R. R MPF slope (%) | EXT.DIG. L RMS (μV) | EXT.DIG. R MPF slope (%) |
| No loop | 53.6 | 15.9 | 25.7 | 12.2 | 225.1 | 22.4 |
| “γ” loop | 68.6 | 2.6 | 10.1 | 12.5 | 228.5 | 13.4 |
| “α” loop | 112.0 | 21.3 | 33.0 | 15.9 | 289.1 | 19.6 |
| Reverse “α” loop | 81.9 | 31.4 | 35.7 | 10.4 | 316.3 | 37.0 |
| “N” loop | 80.1 | 15.0 | 7.3 | 24.4 | 347.2 | 27.0 |
| Complex loop | 87.6 | 38.4 | 36.1 | 26.5 | 370.6 | 31.8 |
The complex loop consistently presents among the highest RMS value and MPF slope values across all four muscles. His pattern confirms that the complex loop is the most fatiguing maneuver, not solely due to its duration (which is not the longest), but because of its inherent technical complexity. It demands intense, coordinated activation from the right shoulder (deltoid) for positioning, the right wrist muscles (flexors/extensors) for precise torque and control, and the left wrist flexor for counter-stabilization and grip.
The right middle deltoid (r = 0.57): The shoulder stabilizer shows a moderate correlation, suggesting that prolonged procedures, especially those involving complex navigation (complex loop time: 87.6 seconds, MPF slope: 38.4%), demand sustained shoulder abduction and stabilization, leading to pronounced fatigue. The left flexor carpi radialis (r = 0.59): This left forearm muscle, critical for grip and wrist stabilization, exhibits the strongest correlation. Complex and reverse “α” loops, with both high MPF slopes (> 35%) and substantial insertion times (> 81 seconds), place significant endurance demands on the non-dominant arm’s grip mechanism. The right flexor carpi radialis (r = 0.30) and right extensor digitorum (r = 0.28): These muscles in the dominant arm show a weak linear relationship between time and MPF slope. This implies that fatigue in these muscles is less dependent purely on time and more on the specific technical demands (e.g., torque, fine control, force) of the loop type itself. For instance, the “N” loop (80.1 seconds) induces a high MPF slope in the right flexor (24.4%), while the longer “α” loop (112.0 seconds) induces a much lower slope (15.9%).
This study employed an in-depth case study design to delineate the detailed bilateral upper limb muscle activation patterns of an experienced endoscopist confronting standardized bowel loops in a simulated environment. This approach enabled high-resolution biomechanical observation of a complex task, free from inter-operator variability, serving as a hypothesis-generating investigation for technique optimization.
We found that the sEMG activity characteristics of the bilateral upper limbs during single-operator colonoscopy may be related to the colonoscopy operation method and muscle fatigue. First, the more complex the intestinal loop, the longer the insertion time[11,12]. Second, the left extensor digitorum dominated colonoscopy operation activities: In all intestinal loop states, the RMS value of the left extensor digitorum was the highest (225.1-370.6 μV), indicating that this muscle played a core role in colonoscopy torque adjustment[5]. Third, the right middle deltoid and right flexor carpi radialis showed elevated activation during complex maneuvers, highlighting the dominant arm’s role in scope advancement and fine control[13,14].
Therefore, in terms of operational technique improvement, for the case of high load on the left extensor muscles, it is recommended to adopt the “two-handed steering technique”, where the left hand maintains grip and gross torque while the right hand provides fine directional adjustments, which could help distribute load[15-17]. For resolving complex loops, emphasizing “withdrawal and torque” techniques over forceful advancement may reduce sustained, high-intensity contractions in the right deltoid and left forearm. Simulator-based training modules could incorporate real-time sEMG biofeedback, guiding trainees to maintain muscle activation below identified thresholds to build efficient, low-strain motor patterns[18,19].
Additionally, MPF differences indicate fatigue thresholds[20]. The MPF slope analysis, indicating the rate of spectral shift toward lower frequencies, served as a direct metric of localized muscle fatigue. A key finding was the strong performance of the complex loop, which, despite a moderate insertion time (87.6 seconds), elicited the highest or near-highest MPF slopes in multiple muscles (e.g., 38.4% in right middle deltoid, 36.1% in left flexor carpi radialis). The strongest correlations were observed for the left flexor carpi radialis (r = 0.59) and right middle deltoid (r = 0.57), suggesting that fatigue in these postural and stabilizing muscles is more time-sensitive. This study suggests that insertion time should be managed according to the type of intestinal loops: Based on RMS and MPF differences, intestinal loop states are divided into three levels: Low risk (no loop, “γ” loop), continuous operation is allowed; medium risk (reverse “α” loop, “N” loop), single operation ≤ 3 minutes; high risk (“α” loop, complex loop), single operation ≤ 1 minute, with taking appropriate rest. Standardized training module: Add real-time sEMG feedback in the simulator to train trainees to control the RMS value of the left extensor digitorum < 300 μV (80% of the current data) in complex loop states.
Based on muscle load distribution, colonoscopy design optimization: The high load of the left extensor digitorum reflects the current design defect of the handpiece, which requires excessive reliance on the left finger muscle group to maintain colonoscopy insertion section direction; the activity of the right abductor pollicis longus suggests that the thumb pressing area of the colonoscopy insertion part does not conform to ergonomics[21]. sEMG data-guided colonoscopy equipment design improvement: Redesign could focus on improving grip geometry or incorporating power-assisted steering mechanisms to share the torque-generation load[12,22]; similarly, the activation of the right abductor pollicis longus indicates friction and control challenges at the thumb-colonoscope interface; textured surfaces or tactile gloves could enhance control while reducing muscular effort[22].
Compared with single-operator colonoscopy insertion in the no loop and other loop state, the RMS of the right flexor carpi radialis was increased, which may be related to the excessive bending resistance of the colonoscopy insertion section. Colonoscopy insertion section mechanical property improvement plan: Develop a “smart soft-hard adjustment colonoscopy insertion section” that automatically reduces bending resistance when intestinal loops are detected[12,23,24], reducing the load on the wrist muscle group.
The sEMG profiles directly illuminate pathways to work-related musculoskeletal disorders. The chronic overuse of the right shoulder (deltoid) and left wrist extensors, evidenced by their high activation and rapid fatigue, aligns clinically with the high incidence of rotator cuff pathology and lateral epicondylitis among endoscopists. Furthermore, the pronounced bilateral asymmetry in muscle use (e.g., high right-side activation for manipulation, high left-side activation for stabilization) risks creating muscle imbalances that may contribute to postural abnormalities and compensatory injuries over time. These findings mandate the integration of structured micro-breaks during procedures, especially after complex loop resolution, and advocate for preventive strength and conditioning programs focused on shoulder sta
Additionally, we had also noticed: The overuse of the dominant side muscles (right) and the compensatory activity of the non-dominant side (left) may lead to bilateral muscle imbalance, increasing the risk of spinal lateral curvature or unilateral joint degeneration[26,27], and bilateral muscle asymmetry load is an important inducement for occupational musculoskeletal diseases[13,14].
This study has several limitations. Firstly, its single-subject design means the observed muscle activation and fatigue patterns may not be generalizable, being influenced by individual factors like technique and physiology. Secondly, the use of a physical simulator, while controlled, lacks the biological variability and psychological pressures of real clinical practice, limiting ecological validity. Thirdly, the data analysis in this study primarily serve descriptive and preliminary associative purposes, and only six standardized loop types, which may not encompass the full complexity encountered clinically, and did not account for procedural time pressures. Lastly, the analysis relied primarily on RMS and MPF, potentially overlooking nuanced muscle synergies, and did not employ advanced signal processing to mitigate noise.
Future research should expand to a diverse, multi-center cohort to establish generalizable biomechanical benchmarks. Validation in real clinical settings is essential to confirm the applicability of the identified metrics. Experimental protocols should incorporate more complex, non-standardized loops and introduce time constraints to better reflect clinical reality. Analytically, integrating additional sEMG features and advanced processing techniques would provide a more comprehensive understanding of muscle coordination and fatigue dynamics.
This exploratory case study provides initial quantitative evidence linking loop complexity during colonoscopy to specific patterns of upper limb muscular load and fatigue, as measured by sEMG. The findings suggest that complex maneuvers, particularly the “α” and complex loops, impose significantly higher activation and accelerated fatigue rates on key stabilizer muscles, including the right middle deltoid and left extensor digitorum. These muscle groups are thus iden
These data directly inform strategies for technique optimization and ergonomic innovation. The analysis supports the efficacy of a “withdrawal-torque” strategy to reduce sustained strain on the left forearm. Furthermore, it provides a biomechanical rationale for redesigning colonoscope handles, suggesting that integrated power-assisted steering and variable-stiffness insertion tubes could substantially mitigate load on the right wrist and shoulder musculature. From an occupational health perspective, the correlation between loop complexity, time, and fatigue justifies implementing a risk-tiered protocol that mandates structured rest breaks proportional to procedural difficulty.
As a foundational investigation, this study highlights the utility of sEMG for objectively assessing procedural demand in endoscopy. The results, while derived from a single operator, generate important hypotheses for future validation in larger, clinically diverse cohorts. This work establishes a framework for advancing evidence-based strategies aimed at enhancing both procedural efficiency and long-term operator well-being in gastroenterology practice.
| 1. | Rex DK, Anderson JC, Butterly LF, Day LW, Dominitz JA, Kaltenbach T, Ladabaum U, Levin TR, Shaukat A, Achkar JP, Farraye FA, Kane SV, Shaheen NJ. Quality indicators for colonoscopy. Gastrointest Endosc. 2024;100:352-381. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 109] [Cited by in RCA: 81] [Article Influence: 40.5] [Reference Citation Analysis (2)] |
| 2. | Huang Q, Zhou J, Wang RG, Wei ZJ, Jiang X. [Investigation on the current situation of colonoscopy]. Zhongguo Yiyao Daobao. 2022;19:52-55. |
| 3. | Yung DE, Banfi T, Ciuti G, Arezzo A, Dario P, Koulaouzidis A. Musculoskeletal injuries in gastrointestinal endoscopists: a systematic review. Expert Rev Gastroenterol Hepatol. 2017;11:939-947. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 57] [Article Influence: 6.3] [Reference Citation Analysis (1)] |
| 4. | Kamavuako EN. On the Applications of EMG Sensors and Signals. Sensors (Basel). 2022;22:7966. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (1)] |
| 5. | Tang Z, Yu H, Yang H, Zhang L, Zhang L. Effect of velocity and acceleration in joint angle estimation for an EMG-Based upper-limb exoskeleton control. Comput Biol Med. 2022;141:105156. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 4] [Article Influence: 0.8] [Reference Citation Analysis (1)] |
| 6. | Wang S, Lai W, Zhang Y, Yao J, Gou X, Ye H, Yi J, Cao D. Design of upper limb muscle strength assessment system based on surface electromyography signals and joint motion. Front Neurol. 2024;15:1470759. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 7. | Shiang A, Wang JS, Cho DH, Kushner B, Panahi AK, Awad MM. Patient Factors Affect Ergonomic Strain of Endoscopists During Colonoscopy. Dig Dis Sci. 2023;68:736-743. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 8. | Eickhoff A, Jakobs R, Kamal A, Mermash S, Riemann JF, van Dam J. In vitro evaluation of forces exerted by a new computer-assisted colonoscope (the NeoGuide Endoscopy System). Endoscopy. 2006;38:1224-1229. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 28] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 9. | Zhou C, Wang S, Wu M, Lai W, Yao J, Gou X, Ye H, Yi J, Cao D. Development of an upper limb muscle strength rehabilitation assessment system using particle swarm optimisation. Front Bioeng Biotechnol. 2025;13:1619411. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 10. | Wang SQ, Wu XY, Lai W, Yao JY, Gou XY, Ye H, Yi J, Cao D. Rehabilitation evaluation method and application for upper limb post-stroke based on improved DTW. Biomed Signal Process Control. 2025;106:107775. [DOI] [Full Text] |
| 11. | Crockett SD, Cirri HO, Kelapure R, Galanko JA, Martin CF, Dellon ES. Use of an Abdominal Compression Device in Colonoscopy: A Randomized, Sham-Controlled Trial. Clin Gastroenterol Hepatol. 2016;14:850-857.e3. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 22] [Article Influence: 2.2] [Reference Citation Analysis (1)] |
| 12. | Kawai T, Kawai Y, Akimito Y, Hamada M, Iwata E, Niikura R, Nagata N, Sugimoto M, Yanagisawa K, Fukuzawa M, Itoi T. Investigation of the relationship between colonoscopy insertion difficulty factors and endoscope shape using an endoscopic position detection unit. J Clin Biochem Nutr. 2024;74:245-252. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 13. | Sturm N, Leukert J, Perkhofer L, Hann A, Wagner M, Mayer B, Seufferlein T, Mayerle J, Schulz C, Meining A, Kraft E, Walter BM. The impact of endoscopic activity on musculoskeletal disorders of high-volume endoscopists in Germany. Sci Rep. 2022;12:8538. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 17] [Reference Citation Analysis (1)] |
| 14. | Miller AT, Herberts MB, Hansel SL, Fox JC, Hallbeck MS, League J 3rd, Hinson C, Van Dyke C, Murray JA. Procedural and anthropometric factors associated with musculoskeletal injuries among gastroenterology endoscopists. Appl Ergon. 2022;104:103805. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 11] [Article Influence: 2.8] [Reference Citation Analysis (1)] |
| 15. | Markwell SA, Garman KS, Vance IL, Patel A, Teitelman M. Individualized ergonomic wellness approach for the practicing gastroenterologist (with video). Gastrointest Endosc. 2021;94:248-259.e2. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 17] [Article Influence: 3.4] [Reference Citation Analysis (1)] |
| 16. | Ruan W, Walsh CM, Pawa S, D'Souza SL, Banerjee P, Kothari S, McCreath GA, Fishman DS. Musculoskeletal injury and ergonomics in pediatric gastrointestinal endoscopic practice. Surg Endosc. 2023;37:248-254. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 11] [Article Influence: 3.7] [Reference Citation Analysis (1)] |
| 17. | Shergill AK, Rempel D, Barr A, Lee D, Pereira A, Hsieh CM, McQuaid K, Harris-Adamson C. Biomechanical risk factors associated with distal upper extremity musculoskeletal disorders in endoscopists performing colonoscopy. Gastrointest Endosc. 2021;93:704-711.e3. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 24] [Article Influence: 4.8] [Reference Citation Analysis (1)] |
| 18. | Shin H, Choe JW, Kim SY, Hyun JJ, Jung SW, Jung YK, Koo JS, Yim HJ. Comparison of One-Person Technique and Two-Person Technique for Colonoscope Insertion: A Randomized Controlled Trial. J Clin Med. 2024;13:3140. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 19. | Kim SE, Kang YJ, Jung CH, Jeon Y, Jung Y, Lee MG. A Pressure Sensing Device to Assist in Colonoscopic Procedures to Prevent Perforation-A Case Study. Sensors (Basel). 2024;24:5711. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 20. | McBride JM, Porcari JP, Scheunke MD. Effect of vibration during fatiguing resistance exercise on subsequent muscle activity during maximal voluntary isometric contractions. J Strength Cond Res. 2004;18:777-781. [PubMed] [DOI] [Full Text] |
| 21. | Tetteh E, Wang T, Kim JY, Smith T, Norasi H, Van Straaten MG, Lal G, Chrouser KL, Shao JM, Hallbeck MS. Optimizing ergonomics during open, laparoscopic, and robotic-assisted surgery: A review of surgical ergonomics literature and development of educational illustrations. Am J Surg. 2024;235:115551. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 23] [Article Influence: 11.5] [Reference Citation Analysis (1)] |
| 22. | Otero-González I, Caeiro-Rodríguez M, Rodriguez-D'Jesus A. Methods for Gastrointestinal Endoscopy Quantification: A Focus on Hands and Fingers Kinematics. Sensors (Basel). 2022;22:9253. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (1)] |
| 23. | Shah SG, Saunders BP, Brooker JC, Williams CB. Magnetic imaging of colonoscopy: an audit of looping, accuracy and ancillary maneuvers. Gastrointest Endosc. 2000;52:1-8. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 110] [Cited by in RCA: 95] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 24. | Pasternak A, Szura M, Solecki R, Matyja M, Szczepanik A, Matyja A. Impact of responsive insertion technology (RIT) on reducing discomfort during colonoscopy: randomized clinical trial. Surg Endosc. 2017;31:2247-2254. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 11] [Article Influence: 1.1] [Reference Citation Analysis (1)] |
| 25. | Ito Y, Matsumoto H, Ishida T, Suenaga N, Oizumi N. Electromyographic activities of glenohumeral joint muscles during shoulder forward flexion with isometric horizontal abduction loading. J Shoulder Elbow Surg. 2023;32:1718-1727. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (1)] |
| 26. | Bampouras TM, Wilson AJ, Papadopoulos K. Upper limb muscle strength and knee frontal plane projection angle asymmetries in female water-polo players. Sports Biomech. 2024;23:1398-1409. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 1.0] [Reference Citation Analysis (1)] |
| 27. | Han G, Zhou S, Qiu W, Fan Z, Yue L, Li W, Wang W, Sun Z, Li W. Role of the Paraspinal Muscles in the Sagittal Imbalance Cascade: The Effects of Their Endurance and of Their Morphology on Sagittal Spinopelvic Alignment. J Bone Joint Surg Am. 2023;105:1954-1961. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 26] [Reference Citation Analysis (1)] |