Published online Mar 16, 2026. doi: 10.4253/wjge.v18.i3.113096
Revised: November 20, 2025
Accepted: February 3, 2026
Published online: March 16, 2026
Processing time: 198 Days and 16 Hours
Hereditary angioedema (HAE) is a rare, potentially fatal disorder that may pre
We report a 30-year-old woman with a 10-year history of recurrent, unexplained abdominal pain and vomiting, without any cutaneous edema. The initial pre
HAE can be fatal from laryngeal edema and intestinal involvement and should be considered in patients with recurrent abdominal pain.
Core Tip: This study highlights that hereditary angioedema should be considered in cases of recurrent abdominal pain, even in the absence of typical edema or family history. Although the initial presentation mimicked acquired angioedema, the early onset prompted SERPING1 gene testing, revealing a novel frameshift mutation. This case emphasizes the importance of genetic confirmation for hereditary angioedema diagnosis in atypical cases, as timely diagnosis is crucial because the condition can be potentially life-threatening.
- Citation: Matsuura K, Ueda C, Hashimura C, Yakushiji H, Horiuchi T. Hereditary angioedema with recurrent abdominal pain in a patient with a novel SERPING1 gene mutation: A case report. World J Gastrointest Endosc 2026; 18(3): 113096
- URL: https://www.wjgnet.com/1948-5190/full/v18/i3/113096.htm
- DOI: https://dx.doi.org/10.4253/wjge.v18.i3.113096
Hereditary angioedema (HAE) is an autosomal dominant disorder characterized by recurrent, transient, and localized angioedema of the skin, gastrointestinal (GI) tract, and airway mucosa, where laryngeal involvement carries a fatal risk[1]. This condition results from a quantitative or qualitative deficiency of C1 esterase inhibitor (C1-INH) caused by mutations in the SERPING1 gene, leading to uncontrolled bradykinin production and increased vascular permeability[2]. HAE has an estimated prevalence of 1 in 50000[3].
HAE is classified into type 1 (decreased C1-INH levels) and type 2 (functionally abnormal C1-INH), collectively de
In the present case, we report a case of HAE with a novel T frameshift mutation involving a thymine in exon 5 (c.852dupT) of SERPING1, confirming HAE-C1-INH.
A 30-year-old woman presented to the emergency department with a 5-day history of abdominal pain and vomiting.
The patient had experienced recurrent abdominal symptoms with a similar presentation once a year over the past 10 years. During this period, no obvious symptoms of cutaneous or laryngeal edema were noted.
She had no past medical history other than recurrent episodes of acute gastroenteritis and no history of surgery. Her only regular medication was rebamipide. Three months prior, she was hospitalized elsewhere for similar symptoms. Although computed tomography revealed ileal edema, upper and lower endoscopy performed after symptom resolution were unremarkable. A capsule endoscopy conducted 2 months before the current visit also yielded no abnormal findings.
The patient initially denied any family history of edema, though her father had experienced recurrent gastroenteritis-like symptoms.
Upon presentation, the patient exhibited epigastric tenderness but no facial, peripheral, or laryngeal edema. Her re
Blood tests showed a red blood cell count of 5.48 million/μL (reference range: 4.35-5.55 million/μL), white blood cell count of 21500/μL (3300-8600/μL), platelet count of 418000/μL (158000-348000/μL), and glucose level of 149 mg/dL (73-109 mg/dL). Blood urea nitrogen, creatinine, cholesterol, triglycerides, C-reactive protein, and amylase levels were within normal ranges. Complement studies confirmed low C4 levels (3.3 mg/dL) and severely reduced C1-INH function.
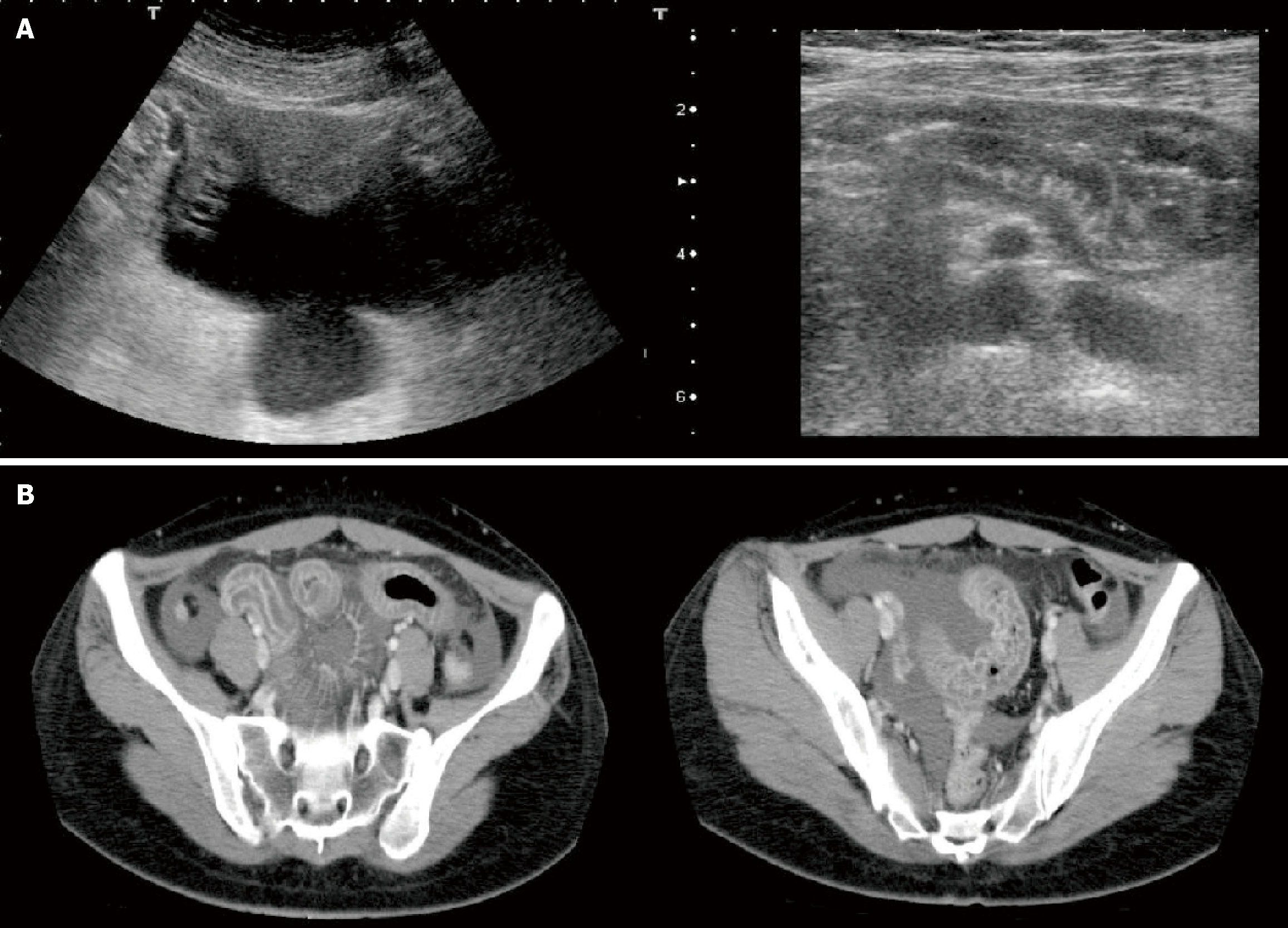
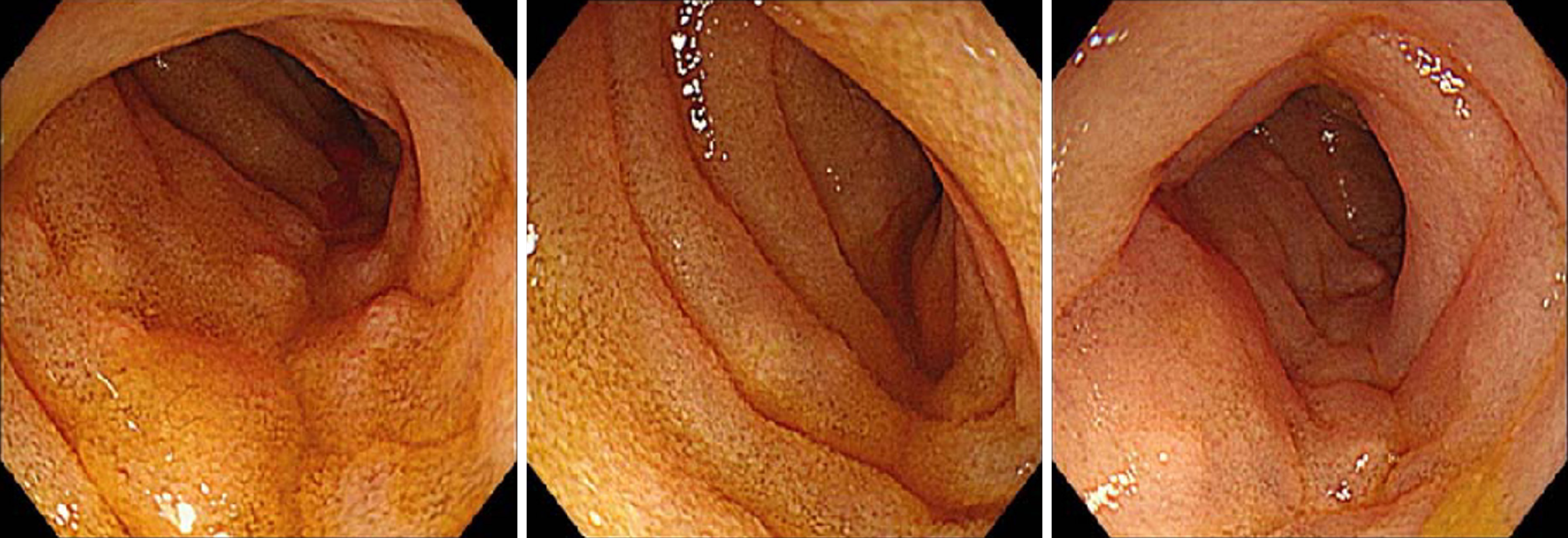
Ultrasound and computed tomography imaging studies demonstrated marked edema of the pelvic small intestine and ascending colon with moderate ascites (Figure 1). Crucially, lower endoscopy performed during the acute episode revealed pronounced edema of the terminal ileum (Figure 2).
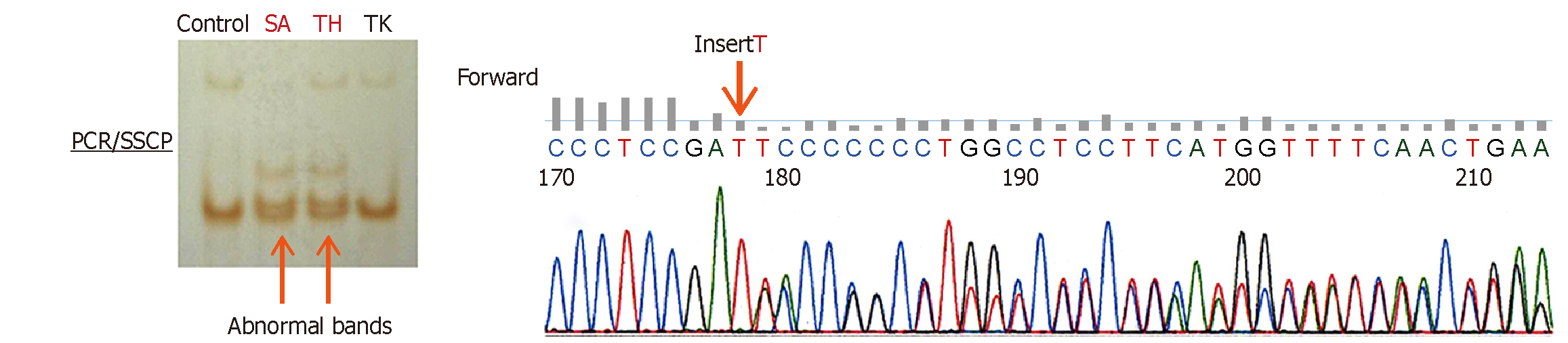
Because the family history was initially unremarkable, HAE and AAE were both considered. However, the patient’s young age and recurrent episodes, combined with the profound C4 and C1-INH activity reduction, strongly suggested HAE. Genetic testing of the SERPING1 gene was performed after obtaining informed consent. Direct sequencing of exon 5 identified a novel heterozygous insertion of T:C.852dupT, resulting in a frameshift mutation (Figure 3). This finding confirmed the diagnosis of HAE type 1. Subsequent testing of her father, whose history of recurrent enteritis was then re-evaluated, identified the same SERPING1 variant, establishing familial inheritance.
During hospitalization, the patient received supportive therapy, including intravenous ranitidine hydrochloride (100 mg diluted in 100 mL saline solution, administered twice daily). Following the definitive diagnosis of HAE type 1, an intravenous infusion of human C1-INH concentrate (1000 IU, prepared by reconstituting and diluting two 500-IU vials in 100 mL normal saline) was administered during subsequent acute abdominal attacks.
The patient’s abdominal symptoms resolved rapidly, and she was discharged. For long-term management, she was prescribed subcutaneous icatibant acetate for on-demand use during intermittent abdominal attacks, achieving excellent long-term control under routine outpatient follow-up.
HAE must be incorporated into the differential diagnosis of recurrent, unexplained abdominal pain, regardless of con
HAE should be considered in recurrent, unexplained abdominal attacks, even without cutaneous manifestations or a clear family history. Because interval investigations may appear normal, evaluation should be prioritized during an active attack. Definitive diagnosis requires genetic testing, as demonstrated by identification of a novel SERPING1 mutation in this patient.
| 1. | Busse PJ, Christiansen SC. Hereditary Angioedema. N Engl J Med. 2020;382:1136-1148. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 153] [Cited by in RCA: 297] [Article Influence: 49.5] [Reference Citation Analysis (0)] |
| 2. | Hashimura C, Kiyohara C, Fukushi JI, Hirose T, Ohsawa I, Tahira T, Horiuchi T. Clinical and genetic features of hereditary angioedema with and without C1-inhibitor (C1-INH) deficiency in Japan. Allergy. 2021;76:3529-3534. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 17] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 3. | Osler W. Landmark publication from The American Journal of the Medical Sciences: Hereditary angio-neurotic oedema. 1888. Am J Med Sci. 2010;339:175-178. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 31] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 4. | Donaldson VH, Evans RR. A Biochemical Abnormality in Herediatry Angioneurotic Edema: Absence of Serum Inhibitor of C' 1-Esterase. Am J Med. 1963;35:37-44. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 663] [Cited by in RCA: 609] [Article Influence: 9.7] [Reference Citation Analysis (0)] |
| 5. | Carter PE, Duponchel C, Tosi M, Fothergill JE. Complete nucleotide sequence of the gene for human C1 inhibitor with an unusually high density of Alu elements. Eur J Biochem. 1991;197:301-308. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 83] [Cited by in RCA: 80] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 6. | Craig T, Aygören-Pürsün E, Bork K, Bowen T, Boysen H, Farkas H, Grumach A, Katelaris CH, Lockey R, Longhurst H, Lumry W, Magerl M, Martinez-Saguer I, Ritchie B, Nast A, Pawankar R, Zuraw B, Maurer M. WAO Guideline for the Management of Hereditary Angioedema. World Allergy Organ J. 2012;5:182-199. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 213] [Cited by in RCA: 223] [Article Influence: 17.2] [Reference Citation Analysis (0)] |
| 7. | Bork K, Barnstedt SE, Koch P, Traupe H. Hereditary angioedema with normal C1-inhibitor activity in women. Lancet. 2000;356:213-217. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 386] [Cited by in RCA: 388] [Article Influence: 14.9] [Reference Citation Analysis (0)] |
| 8. | Zuraw BL. Hereditary angioedema with normal C1 inhibitor: Four types and counting. J Allergy Clin Immunol. 2018;141:884-885. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 52] [Cited by in RCA: 63] [Article Influence: 7.9] [Reference Citation Analysis (0)] |