Copyright: ©Author(s) 2026.
World J Gastrointest Endosc. Apr 16, 2026; 18(4): 118485
Published online Apr 16, 2026. doi: 10.4253/wjge.v18.i4.118485
Published online Apr 16, 2026. doi: 10.4253/wjge.v18.i4.118485
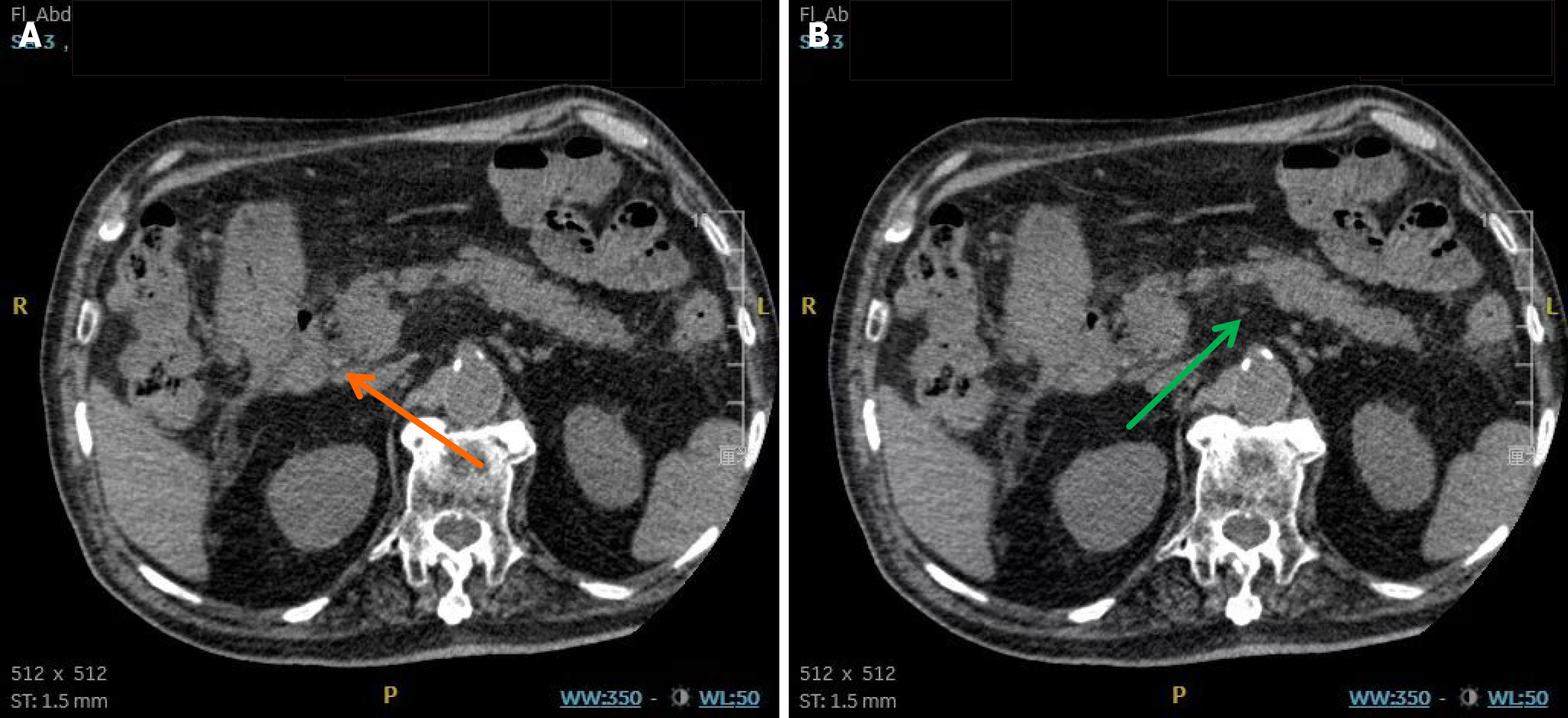
Figure 1 Abdominal computed tomography performed on June 27, 2024.
A: Common bile duct stone (orange arrow); B: Hazy peripancreatic fat stranding (green arrow).
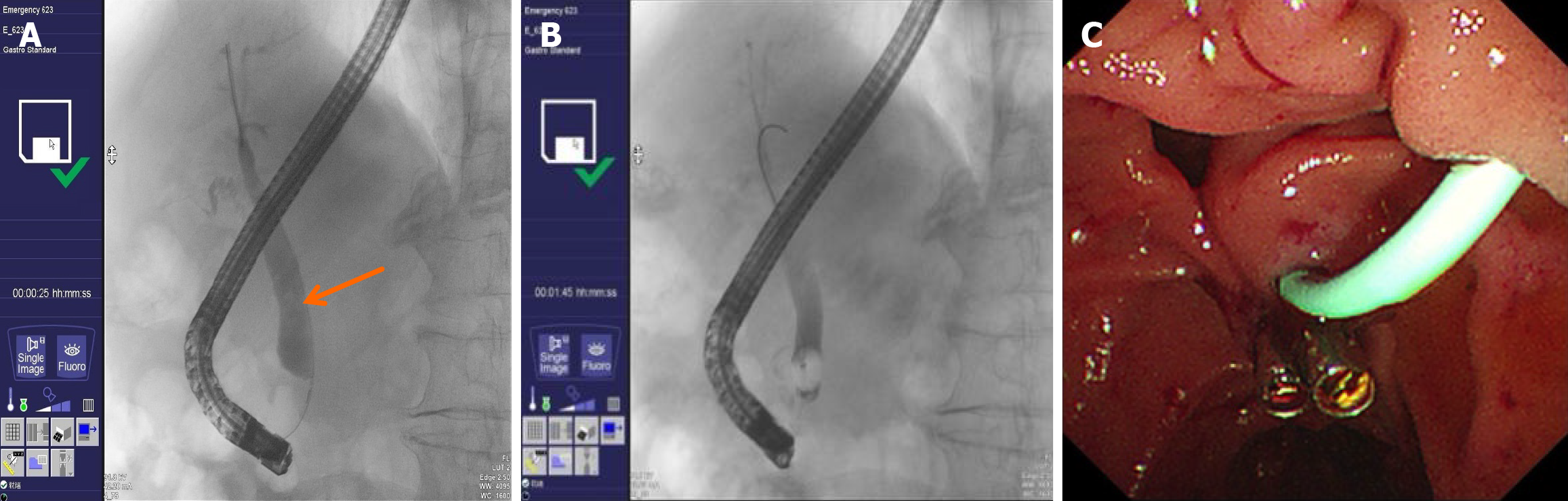
Figure 2 Endoscopic retrograde cholangiopancreatography with endoscopic sphincterotomy, stone extraction, and endoscopic retrograde biliary drainage performed on July 1, 2024.
A: Cholangiography shows dilation of the distal common bile duct (maximal diameter: 1.5 cm) (orange arrow) with an unclear stone shadow; B: The cholangiography showed no residual stones; C: One 5 Fr × 5 cm plastic stent was placed in the common bile duct.
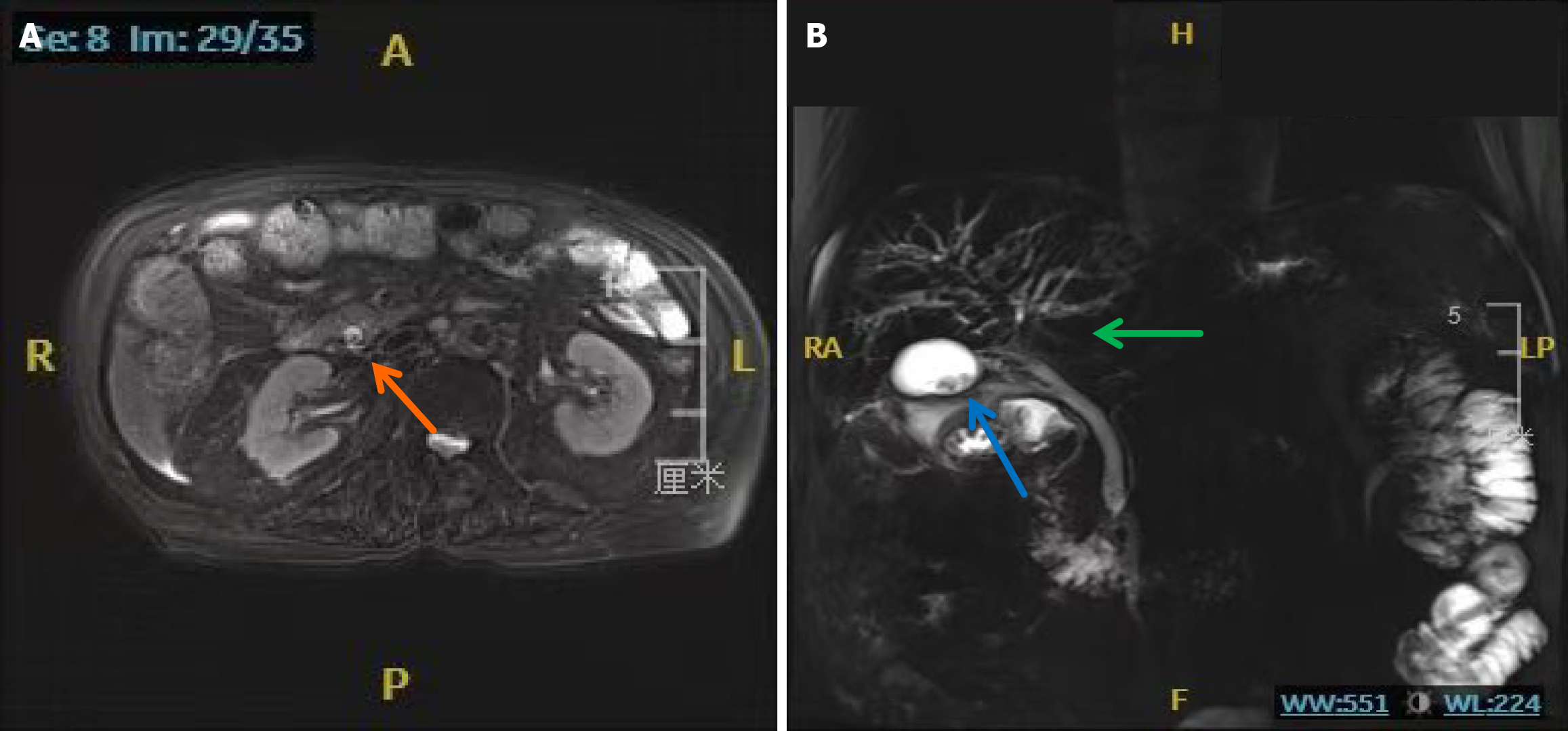
Figure 3 Upper abdominal magnetic resonance imaging with magnetic resonance cholangiopancreatography performed on September 18, 2024.
A: Common bile duct stone (orange arrow); B: Gallbladder stones (blue arrow), poor visualization of the bile duct at the hepatic portal region (green arrow).
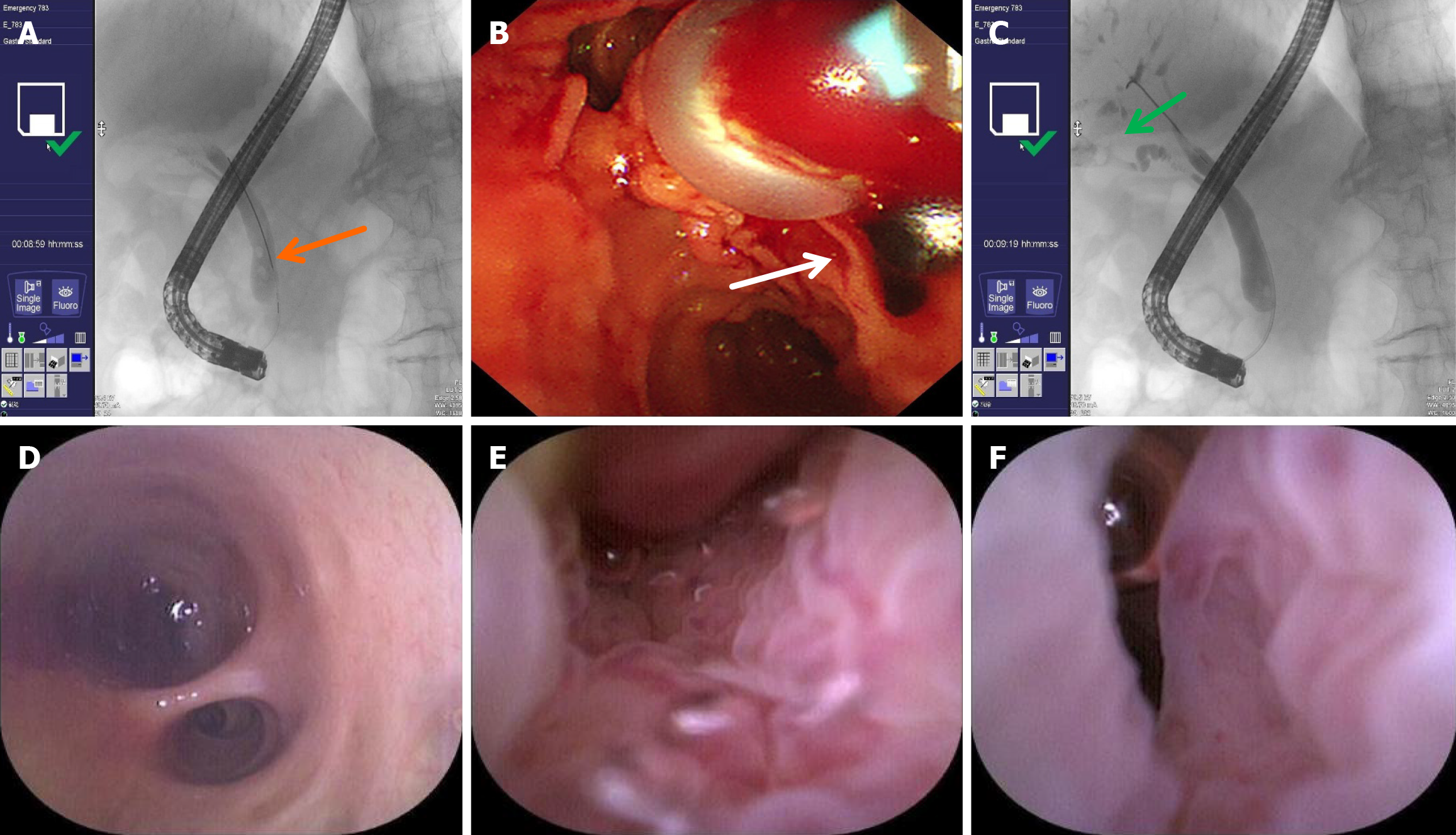
Figure 4 endoscopic retrograde cholangiopancreatography performed on September 19, 2024.
A: Common bile duct stones on cholangiography (orange arrow); B: Stones extracted with balloon (white arrow); C: Poor visualization of the bile duct at the hepatic portal region on cholangiography (green arrow); D: Common bile duct is normal; E: The mucosa of the common bile duct is rough with large, tortuous and irregular blood vessels; F: Narrow bile duct lumen.
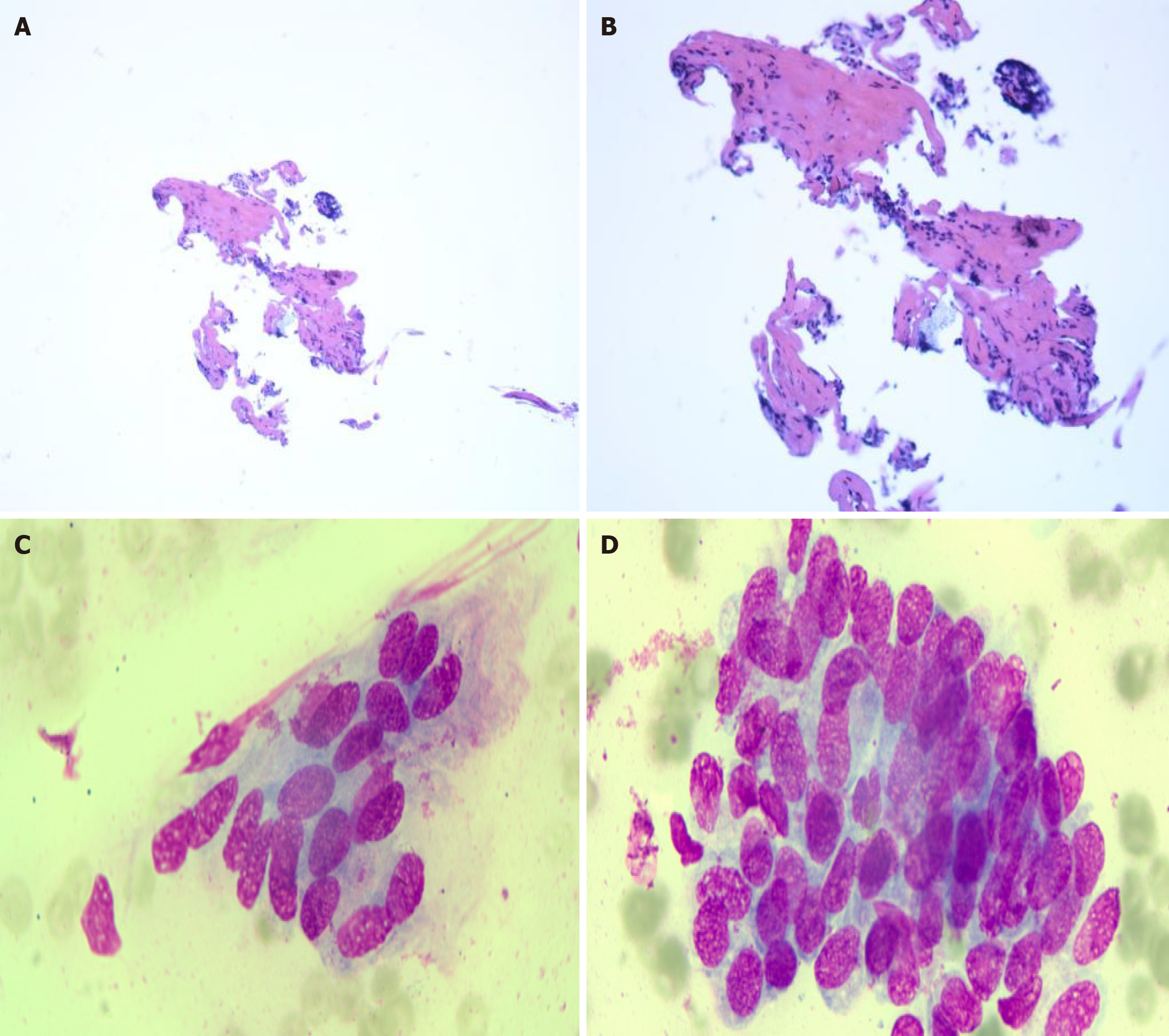
Figure 5 Histopathology and cytopathology.
A and B: Sections of the common bile duct extending to the hepatic bifurcation show minimal fibrosis with chronic inflammatory cell infiltration (A: Hematoxylin and eosin staining, magnification × 40; B: Hematoxylin and eosin staining, magnification × 100); C and D: Bile duct brushings reveal epithelial cells with focal nuclear enlargement, an increased nuclear-to-cytoplasmic ratio, coarse hyperchromatic chromatin, and mild atypia. Correlation with clinical, radiologic, and histologic data is recommended (Wright-Giemsa staining, magnification × 1000).
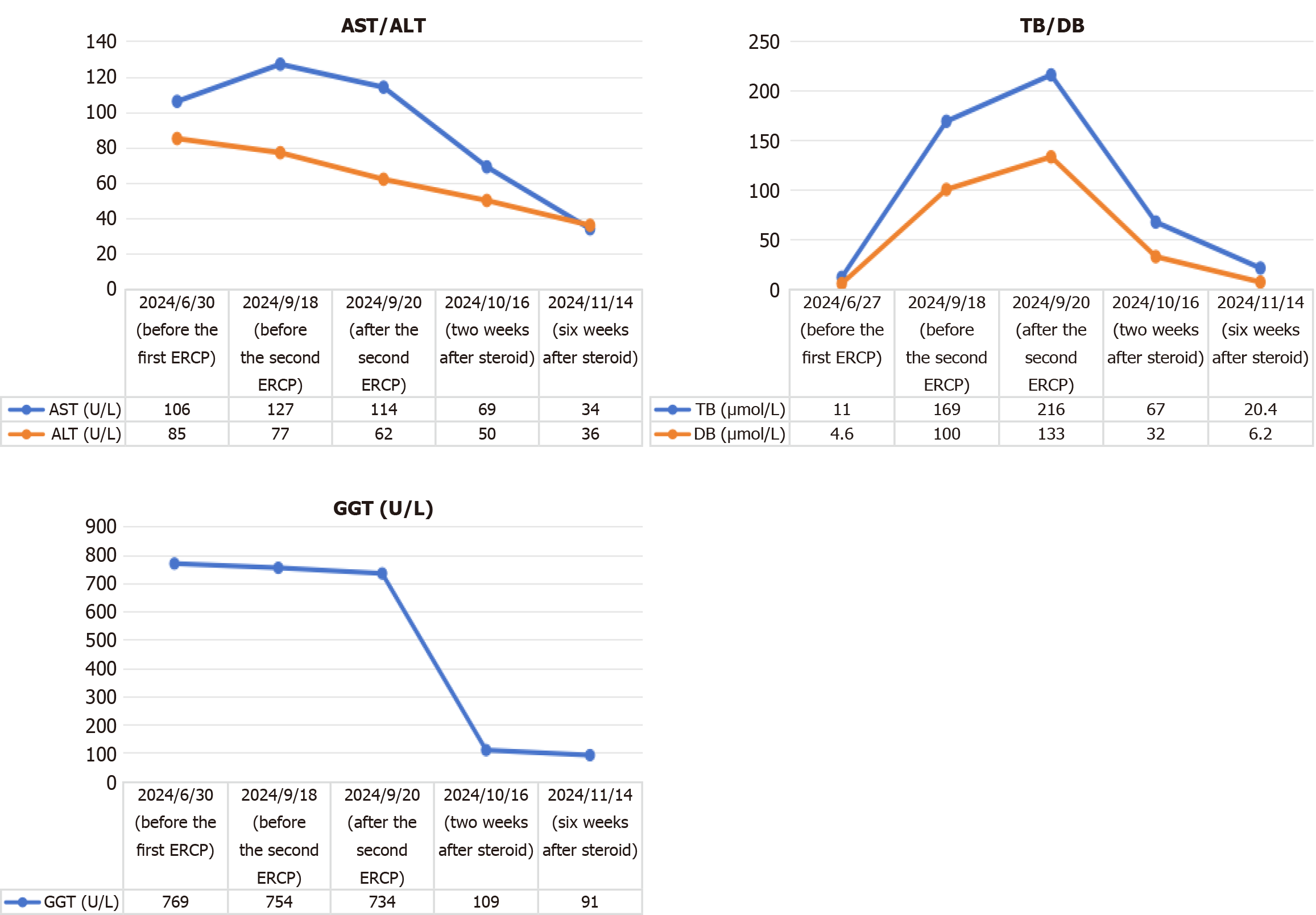
Figure 6 Trends in liver biochemistry during treatment.
Serial measurements of aspartate aminotransferase, alanine aminotransferase, total bilirubin, direct bilirubin, and gamma-glutamyl transferase in the patient during the treatment process. ALT: Alanine aminotransferase; AST: Aspartate aminotransferase; ERCP: Endoscopic retrograde cholangiopancreatography; TB: Total bilirubin; DB: Direct bilirubin; GGT: Gamma-glutamyl transferase.
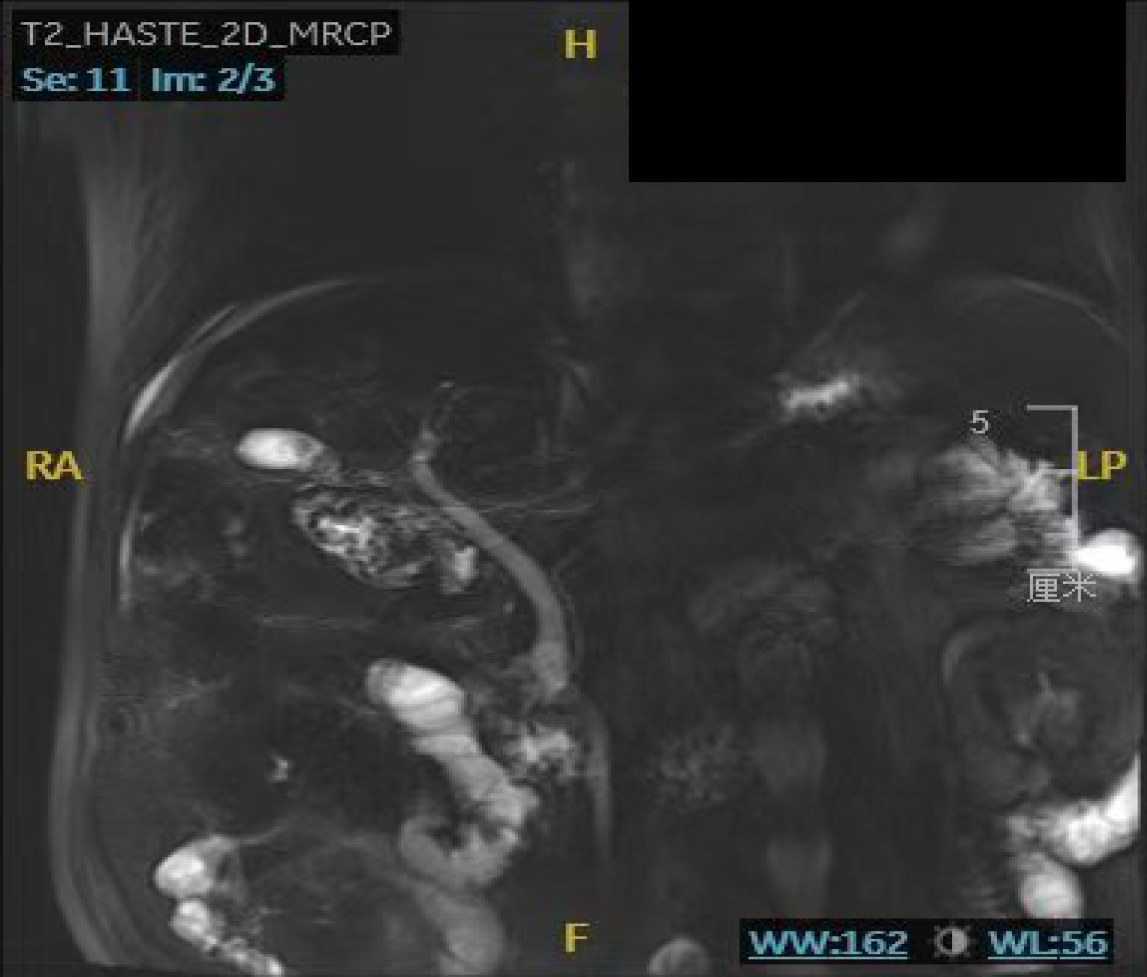
Figure 7 Upper abdominal magnetic resonance imaging with magnetic resonance cholangiopancreatography performed on November 14, 2024, shows cholelithiasis, cholecystitis, and cholangitis, with overall improvement compared to previous findings.
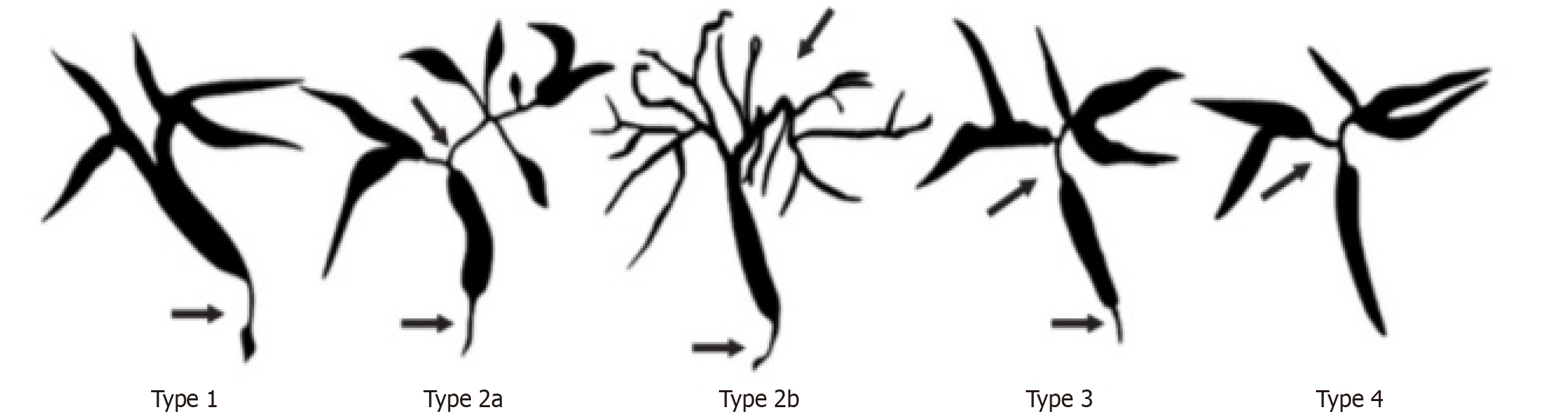
Figure 8 Classification of immunoglobulin G4-related sclerosing cholangitis biliary strictures[9].
Type 1 stricture confined to the intrapancreatic bile duct. Type 2 diffuse strictures involve both intrahepatic and extrahepatic bile ducts. Subtype 2a: Intrahepatic duct strictures with prestenotic dilation. Subtype 2b: Intrahepatic duct strictures without prestenotic dilation and with decreased biliary arborization. Type 3 combined strictures of the hilar bile ducts and the intrapancreatic bile duct. Type 4 isolated strictures of the hilar bile ducts. Arrow(s) indicate the location of the bile duct strictures. Citation: Naitoh I, Nakazawa T. Classification and Diagnostic Criteria for IgG4-Related Sclerosing Cholangitis. Gut Liver 2022; 16: 28-36. Copyright© Gut and Liver. This is an open-access article (Supplementary material).
- Citation: Xia Y, Zhu JD, Su T, Shi L, Zhao SL, Xu HW, Xu CQ. Immunoglobulin G4-related sclerosing cholangitis: A case report. World J Gastrointest Endosc 2026; 18(4): 118485
- URL: https://www.wjgnet.com/1948-5190/full/v18/i4/118485.htm
- DOI: https://dx.doi.org/10.4253/wjge.v18.i4.118485