Copyright: ©Author(s) 2026.
World J Gastrointest Endosc. Mar 16, 2026; 18(3): 116697
Published online Mar 16, 2026. doi: 10.4253/wjge.v18.i3.116697
Published online Mar 16, 2026. doi: 10.4253/wjge.v18.i3.116697
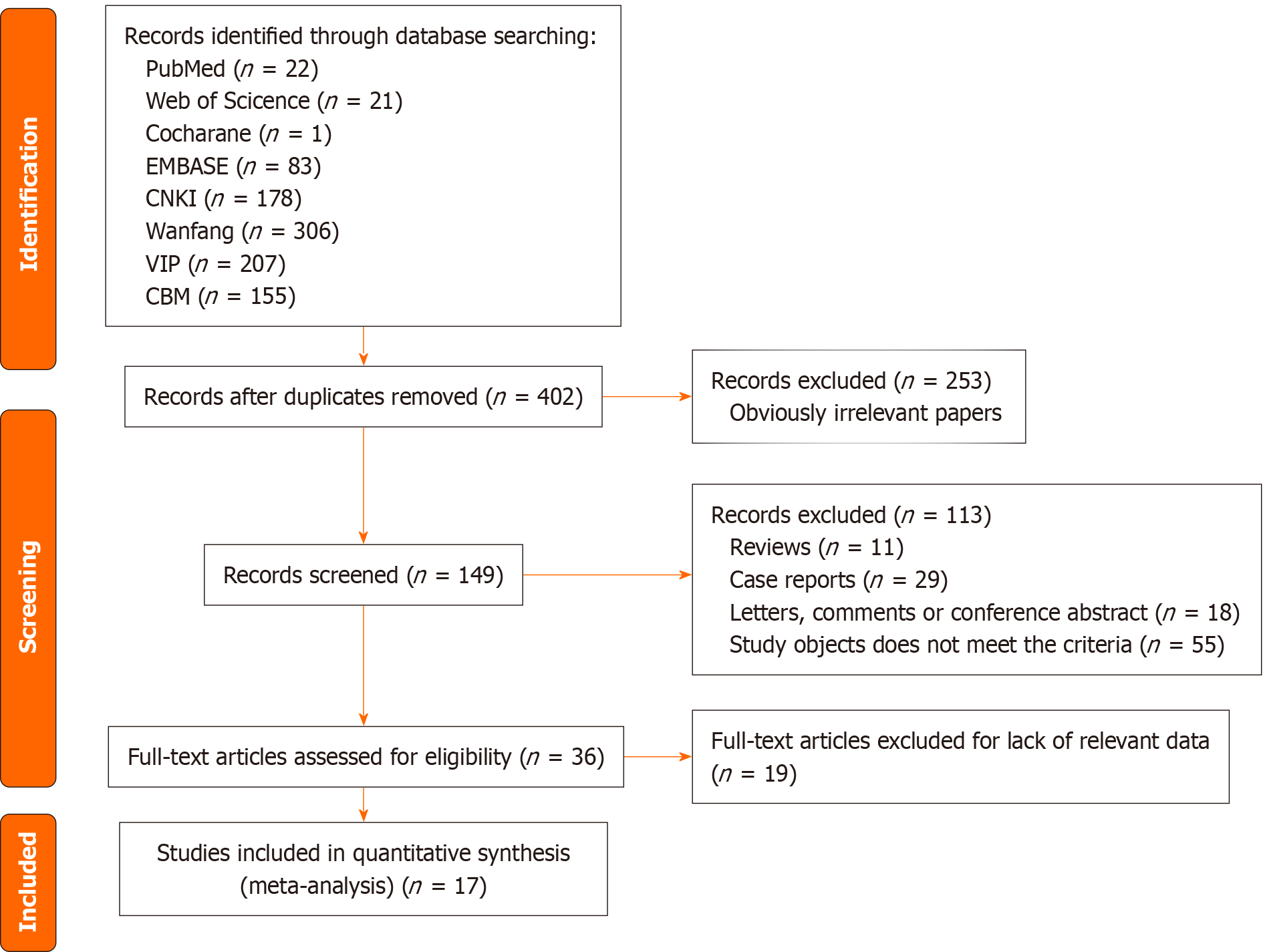
Figure 1 Preferred reporting items for systematic reviews and meta-analysis flow diagram.
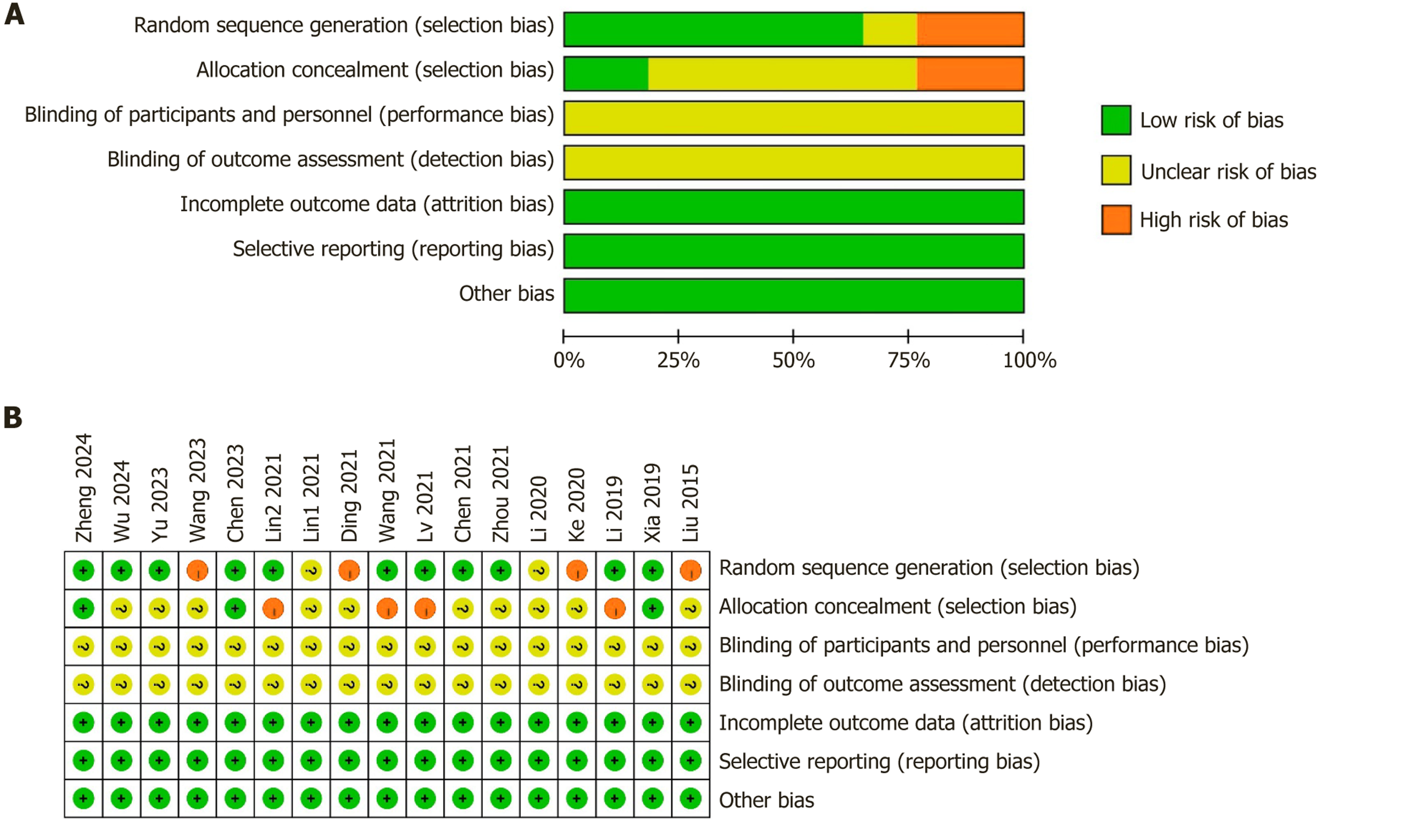
Figure 2 Risk of bias assessment of the included studies.
A: Risk of bias graph: Review authors’ judgements about each risk of bias item presented as percentages across all included studies; B: Risk of bias summary: Review authors’ judgements about each risk of bias item for each included study. Green (+): Low risk of bias; Yellow (?): Unclear risk of bias; Orange (-): High risk of bias.
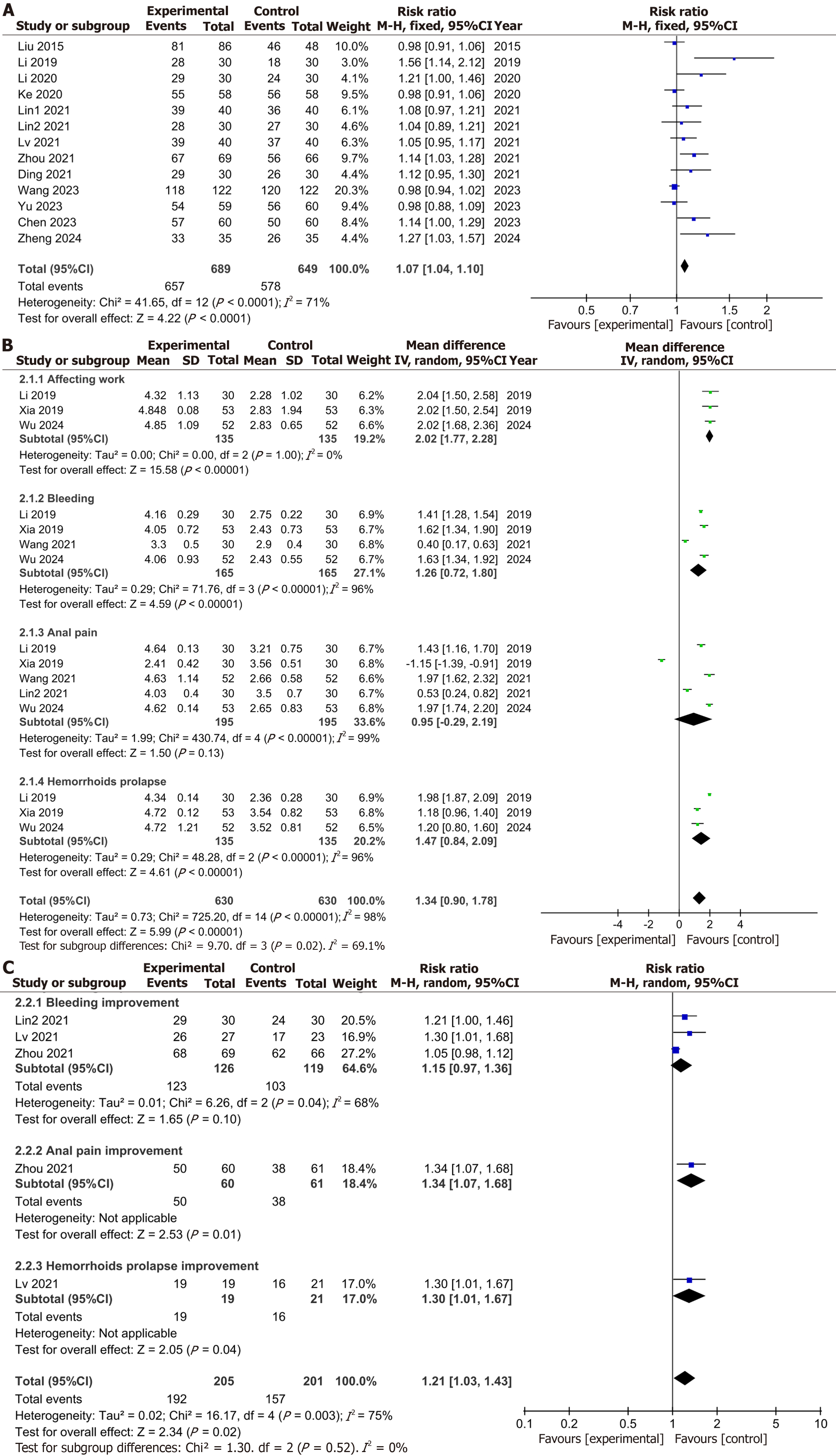
Figure 3 Forest plot of clinical efficacy.
A: Clinical efficacy; B: Symptom score; C: Symptom improvement rate.
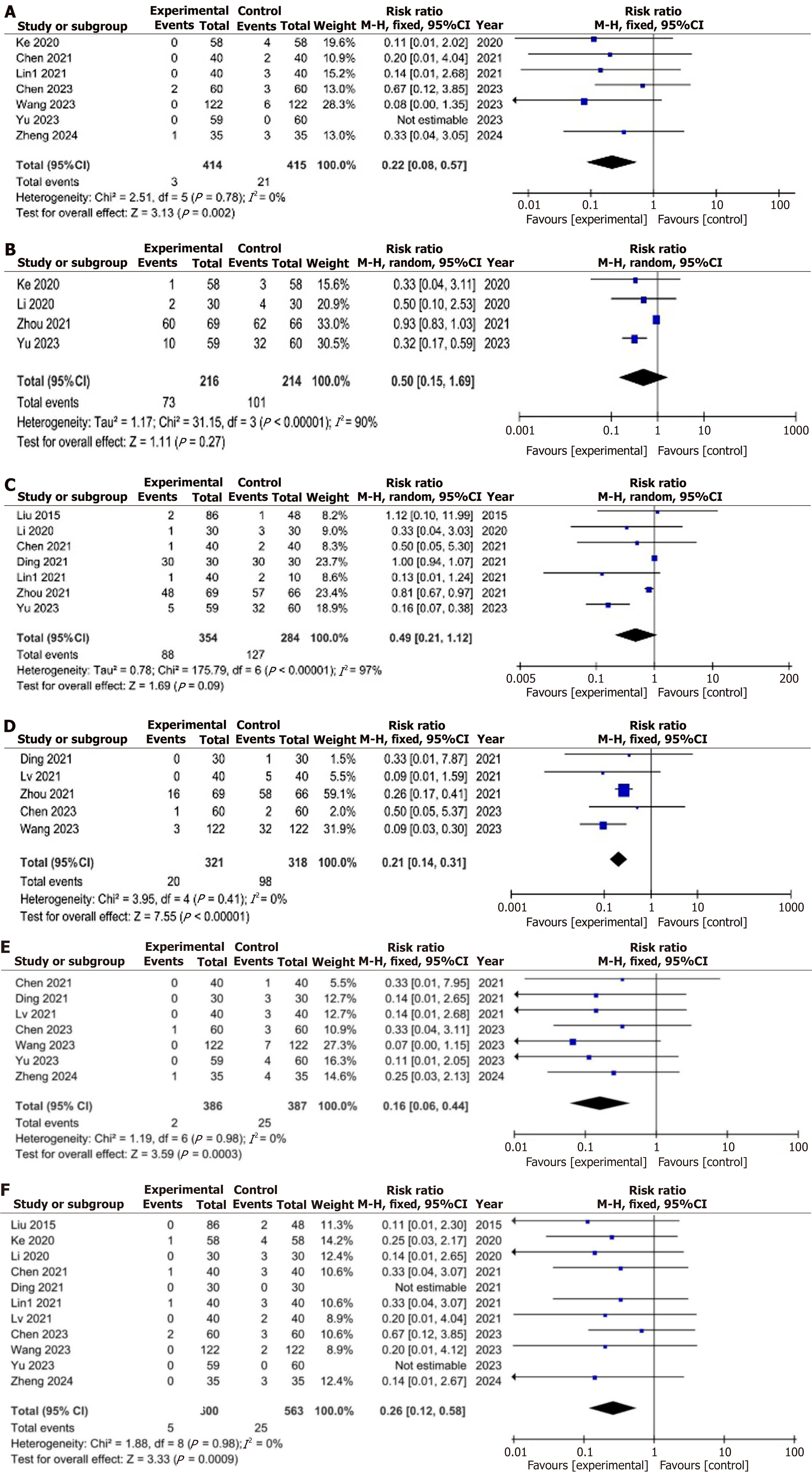
Figure 4 Forest plot of complications after endoscopic sclerotherapy.
A: Postoperative bleeding; B: Anal bulge; C: Anal pain; D: Anal edema; E: Urinary retention; F: Infection.
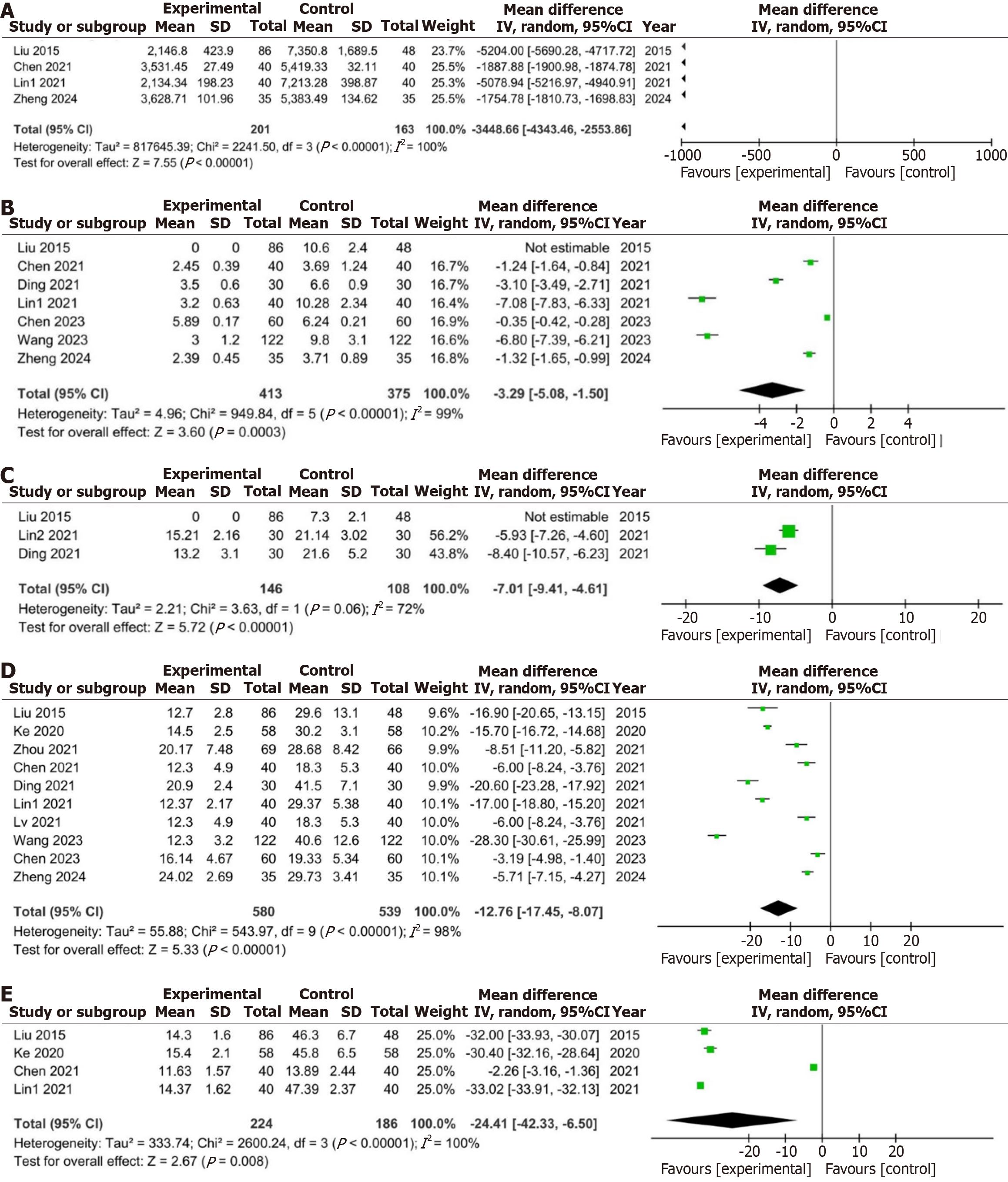
Figure 5 Forest plot of core clinical outcomes.
A: Treatment costs; B: Hospital stay; C: Healing time; D: Operation time; E: Surgical blood loss.
- Citation: Wu SY, Chen YS, Li XH, Yu TJ, Xie F, Jiang QF, Lan Y, He P, Li SC, Li WS, Chen WD. Efficacy and safety of endoscopic sclerotherapy vs traditional surgery in the treatment of internal hemorrhoids: A meta-analysis. World J Gastrointest Endosc 2026; 18(3): 116697
- URL: https://www.wjgnet.com/1948-5190/full/v18/i3/116697.htm
- DOI: https://dx.doi.org/10.4253/wjge.v18.i3.116697