Published online Sep 14, 2016. doi: 10.3748/wjg.v22.i34.7797
Peer-review started: April 18, 2016
First decision: May 12, 2016
Revised: June 28, 2016
Accepted: July 31, 2016
Article in press: August 1, 2016
Published online: September 14, 2016
Processing time: 39 Days and 15.1 Hours
To analyze the risk factors for pancreatic fistula after pancreaticoduodenectomy.
We conducted a retrospective analysis of 539 successive cases of pancreaticoduodenectomy performed at our hospital from March 2012 to October 2015. Pancreatic fistula was diagnosed in strict accordance with the definition of pancreatic fistula from the International Study Group on Pancreatic Fistula. The risk factors for pancreatic fistula were analyzed by univariate analysis and multivariate logistic regression analysis.
A total of 269 (49.9%) cases of pancreatic fistula occurred after pancreaticoduodenectomy, including 71 (13.17%) cases of grade A pancreatic fistula, 178 (33.02%) cases of grade B, and 20 (3.71%) cases of grade C. Univariate analysis showed no significant correlation between postoperative pancreatic fistula (POPF) and the following factors: age, hypertension, alcohol consumption, smoking, history of upper abdominal surgery, preoperative jaundice management, preoperative bilirubin, preoperative albumin, pancreatic duct drainage, intraoperative blood loss, operative time, intraoperative blood transfusion, Braun anastomosis, and pancreaticoduodenectomy (with or without pylorus preservation). Conversely, a significant correlation was observed between POPF and the following factors: gender (male vs female: 54.23% vs 42.35%, P = 0.008), diabetes (non-diabetic vs diabetic: 51.61% vs 39.19%, P = 0.047), body mass index (BMI) (≤ 25 vs > 25: 46.94% vs 57.82%, P = 0.024), blood glucose level (≤ 6.0 mmol/L vs > 6.0 mmol/L: 54.75% vs 41.14%, P = 0.002), pancreaticojejunal anastomosis technique (pancreatic duct-jejunum double-layer mucosa-to-mucosa pancreaticojejunal anastomosis vs pancreatic-jejunum single-layer mucosa-to-mucosa anastomosis: 57.54% vs 35.46%, P = 0.000), diameter of the pancreatic duct (≤ 3 mm vs > 3 mm: 57.81% vs 38.36%, P = 0.000), and pancreatic texture (soft vs hard: 56.72% vs 29.93%, P = 0.000). Multivariate logistic regression analysis showed that gender (male), BMI > 25, pancreatic duct-jejunum double-layer mucosa-to-mucosa pancreaticojejunal anastomosis, pancreatic duct diameter ≤ 3 mm, and soft pancreas were risk factors for pancreatic fistula after pancreaticoduodenectomy.
Gender (male), BMI > 25, pancreatic duct-jejunum double-layer mucosa-to-mucosa pancreaticojejunal anastomosis, pancreatic duct diameter ≤ 3 mm, and soft pancreas were risk factors for pancreatic fistula after pancreaticoduodenectomy.
Core tip: Pancreaticoduodenectomy remains the standard surgical approach for tumors involving the lower bile duct, the pancreatic head, the duodenal papilla, and the ampulla. This operation is considered risky because of high rates of postoperative mortality and complications. In this study, we collected a large sample of 539 cases and analyzed several potential risk factors for pancreatic fistula. A statistical analysis of the case data showed that gender (male), pancreatic duct-jejunum double-layer mucosa-to-mucosa pancreaticojejunal anastomosis, pancreatic duct diameter ≤ 3 mm, and soft pancreas were risk factors for pancreatic fistula after pancreaticoduodenectomy.
- Citation: Hu BY, Wan T, Zhang WZ, Dong JH. Risk factors for postoperative pancreatic fistula: Analysis of 539 successive cases of pancreaticoduodenectomy. World J Gastroenterol 2016; 22(34): 7797-7805
- URL: https://www.wjgnet.com/1007-9327/full/v22/i34/7797.htm
- DOI: https://dx.doi.org/10.3748/wjg.v22.i34.7797
Core tip: Pancreaticoduodenectomy remains the standard surgical approach for tumors involving the lower bile duct, the pancreatic head, the duodenal papilla, and the ampulla. This operation is considered risky because of high rates of postoperative mortality and complications. In this study, we collected a large sample of 539 cases and analyzed several potential risk factors for pancreatic fistula. A statistical analysis of the case data showed that gender (male), pancreatic duct-jejunum double-layer mucosa-to-mucosa pancreaticojejunal anastomosis, pancreatic duct diameter ≤ 3 mm, and soft pancreas were risk factors for pancreatic fistula after pancreaticoduodenectomy.
Pancreaticoduodenectomy is the primary treatment for malignant tumors involving the pancreatic head, the lower bile duct, and the duodenal ampulla[1,2]. The safety of pancreaticoduodenectomy has been greatly improved; however, perioperative mortality rate still ranges from 0%-5%[3-5]. Studies have reported that the incidence of pancreatic fistula after pancreaticoduodenectomy is approximately 11.4%-64.3%[6-16]. Pancreatic fistula remains the most common complication after pancreaticoduodenectomy, and this complication prolongs hospital stays and leads to high medical expenses. Pancreatic fistula is associated with delayed gastric emptying, abdominal abscesses, infection at the incision, sepsis, and bleeding after pancreaticoduodenectomy[17-20]. Several approaches may reduce the incidence of pancreatic fistula after pancreaticoduodenectomy; however, to date, a definitive approach that prevents pancreatic fistula is still lacking[21-23]. In this study, we conducted a retrospective analysis of 539 successive cases of pancreaticoduodenectomy performed over more than 3 years in the Department of Hepatobiliary Surgery of the PLA General Hospital, China, to determine the potential risk factors for pancreatic fistula.
We reviewed the data from 539 successive cases of pancreaticoduodenectomy performed in the Department of Hepatobiliary Surgery of the PLA General Hospital, China, from March 2012 to October 2015. The following patient data were collected: gender, age, hypertension, diabetes, alcohol consumption, smoking, body mass index (BMI), history of upper abdominal surgery, preoperative jaundice management, blood sugar, preoperative bilirubin, preoperative albumin, pancreatic duct drainage, intraoperative blood loss, intraoperative blood transfusion, operative time, pancreaticojejunal anastomosis technique, Braun anastomosis, pylorus preservation, diameter of the pancreatic duct, and pancreatic texture. Additionally, all postoperative complications and postoperative pathological findings (especially information about pancreatic fistula) were recorded. All 539 cases were included in this comprehensive study.
Prior to surgery, the patients underwent routine tests, examinations, and evaluations of organ function. To date, no uniform standard exists for preoperative jaundice management. We believe that patients with obstructive jaundice who have a poor mental state, severe dehydration, poor nutrition, or severe jaundice should undergo jaundice management and supportive therapy to improve their nutritional intake and replenish fluids. Patients should subsequently undergo surgery after their general condition has improved.
In this study, 275 patients underwent classic pancreaticoduodenectomy, of whom 13 had portal vein resection and reconstruction. Additionally, 264 patients underwent pylorus-preserving pancreaticoduodenectomy, of whom six had portal vein resection and reconstruction. Child’s technique (pancreaticojejunal anastomosis, biliary-jejunal anastomosis, and gastrojejunal anastomosis in sequential order) was used for the gastrointestinal reconstruction. A support tube was placed in the pancreatic duct of all patients. The support tube was drained via the jejunal loop to outside the body in 127 patients. In the remaining patients, the tube was placed in the jejunum via biliary-jejunal anastomosis. The following two approaches were used for pancreaticojejunal anastomosis: (1) pancreatic duct-jejunum double-layer mucosa-to-mucosa pancreaticojejunal anastomosis in 398 patients; and (2) pancreatic-jejunum single-layer mucosa-to-mucosa anastomosis in 141 patients.
Pancreatic fistula was defined according to the International Study Group on Pancreatic Fistula (ISGPF) as any measurable volume of drainage fluid output via operatively or postoperatively placed drains on or after postoperative day 3 with amylase content greater than three times the upper normal serum value. Three grades of pancreatic fistulas were determined according to their clinical severity. The grades were determined only after complete healing of the fistula (Table 1)[24].
| Grade | A | B | C |
| Clinical conditions | Well | Often well | Ill appearing/bad |
| Specific treatment1 | No | Yes/no | Yes |
| US/CT (if obtained) | Negative | Negative/positive | Positive |
| Persistent drainage (after 3 wk)2 | No | Usually yes | Yes |
| Reoperation | No | No | Yes |
| Death related to POPF | No | No | Possibly yes |
| Signs of infection | No | Yes | Yes |
| Sepsis | No | No | Yes |
| Readmission | No | Yes/no | Yes/no |
All clinical data were entered into an Excel spreadsheet, and SPSS 19.0 software was used for statistical analyses. Measurement data are expressed as the mean ± SD. A t-test was performed for between-group comparisons. Categorical variables were analyzed using Fisher’s exact test and the χ2 test. All variables were incorporated into a univariate analysis. P < 0.05 was considered statistically significant. Statistically significant variables demonstrated in the univariate analysis were incorporated into a multivariate logistic regression analysis to identify the independent risk factors for pancreatic fistula after pancreaticoduodenectomy.
This study included 343 male patients and 196 female patients with a mean age of 56.42 ± 10.75 years. The mean hospital stay was 30.03 ± 8.86 d. The condition (confirmed by postoperative pathology) of the 539 patients is shown in Table 2. Among the 539 patients, 349 (64.75%) experienced complications, and 269 (49.9%) had POPF, including 71 (13.17%) cases of grade A pancreatic fistula, 178 (33.02%) cases of grade B, and 20 (3.71%) cases of grade C. Additionally, 198 (36.73%) patients had clinically relevant POPFs. The following complications were identified: 25 (4.64%) cases of abdominal bleeding, 59 (10.95%) cases of bile leakage, 120 (22.63%) cases of delayed gastric emptying, 9 (1.67%) cases of pancreaticojejunal anastomotic bleeding, 66 (12.24%) cases of abdominal infection, and 45 (8.35%) cases of incision infection. Moreover, 15 (2.78%) patients underwent a second operation, and 6 (1.11%) patients died after surgery due to abdominal bleeding associated with a pancreatic fistula.
| Pathological type | n |
| Pancreatic head cancer | 126 |
| Neuroendocrine tumor of the pancreatic head | 12 |
| Benign tumor of the pancreatic head | 12 |
| Solid pseudopapillary tumor of the pancreatic head | 16 |
| Autoimmune pancreatitis | 3 |
| Chronic pancreatitis | 11 |
| Lower bile duct cancer | 145 |
| Benign tumor of the lower bile duct | 13 |
| Ampullary cancer | 76 |
| Benign ampullary tumor | 6 |
| Duodenal stromal tumor | 7 |
| Duodenal cancer | 10 |
| Chronic mucosal inflammation of the descending duodenum | 3 |
| Duodenal papillary cancer | 90 |
| Benign duodenal papillary tumor | 6 |
| Duodenal papillary neuroendocrine tumor | 3 |
| Total | 539 |
Univariate analysis showed no significant correlation between POPF and the following factors: age, hypertension, alcohol consumption, smoking, history of upper abdominal surgery, preoperative jaundice management, preoperative bilirubin, preoperative albumin, pancreatic duct drainage, intraoperative blood loss, operative time, intraoperative blood transfusion, Braun anastomosis, and pancreaticoduodenectomy (with or without pylorus preservation). Conversely, a significant correlation was observed between POPF and the following factors: gender (male vs female: 54.23% vs 42.35%, P = 0.008), diabetes (non-diabetic vs diabetic: 51.61% vs 39.19%, P = 0.047), BMI (≤ 25 vs > 25: 46.94% vs 57.82%, P = 0.024), blood glucose level (≤ 6.0 mmol/L vs > 6.0 mmol/L: 54.75% vs 41.14%, P = 0.002), pancreaticojejunal anastomosis technique (pancreatic duct-jejunum double-layer mucosa-to-mucosa pancreaticojejunal anastomosis vs pancreatic-jejunum single-layer mucosa-to-mucosa anastomosis: 57.54% vs 35.46%, P = 0.000), diameter of the pancreatic duct (≤ 3 mm vs > 3 mm: 57.81% vs 38.36%, P = 0.000), and pancreatic texture (soft vs hard: 56.72% vs 29.93%, P = 0.000) (Table 3).
| Variable | POPF occurrence | |||
| Yes | No | χ2 | P value | |
| Sex | 7.042 | 0.008 | ||
| Male | 186 | 157 | ||
| Female | 83 | 113 | ||
| Age (yr) | 2.132 | 0.144 | ||
| ≥ 60 | 99 | 116 | ||
| < 60 | 170 | 154 | ||
| Body mass index (kg/m2) | 5.066 | 0.024 | ||
| > 25 | 85 | 62 | ||
| ≤ 25 | 184 | 208 | ||
| Hypertension | 0.938 | 0.332 | ||
| Yes | 62 | 53 | ||
| No | 207 | 217 | ||
| Diabetes mellitus | 3.941 | 0.047 | ||
| Yes | 29 | 45 | ||
| No | 240 | 225 | ||
| Drinking history | 0.169 | 0.681 | ||
| Yes | 77 | 73 | ||
| No | 193 | 197 | ||
| Smoking history | 1.426 | 0.232 | ||
| Yes | 78 | 66 | ||
| No | 191 | 204 | ||
| Epigastrium surgery | 0.640 | 0.424 | ||
| Yes | 18 | 23 | ||
| No | 251 | 247 | ||
| Preoperative biliary drainage | 0.406 | 0.524 | ||
| Yes | 65 | 59 | ||
| No | 204 | 211 | ||
| Preoperative total bilirubin (μmol/L) | 0.378 | 0.539 | ||
| > 171 | 73 | 67 | ||
| ≤ 171 | 196 | 203 | ||
| Serum albumin (g/L) | 0.000 | 0.985 | ||
| < 35 | 41 | 41 | ||
| ≥ 35 | 228 | 229 | ||
| Blood glucose (mmol/L) | 9.157 | 0.002 | ||
| ≤ 6.0 | 190 | 157 | ||
| > 6.0 | 79 | 113 | ||
| Pancreaticojejunostomy | 20.323 | 0.000 | ||
| Double-layer mucosa-to-mucosa | 229 | 169 | ||
| Single-layer mucosa-to-mucosa | 50 | 91 | ||
| Blood loss (mL) | 0.134 | 0.715 | ||
| > 600 | 34 | 37 | ||
| ≤ 600 | 235 | 225 | ||
| Pancreatic duct diameter (mm) | 19.687 | 0.000 | ||
| ≤ 3 | 185 | 135 | ||
| > 3 | 84 | 135 | ||
| Pylorus-preserving | 0.017 | 0.897 | ||
| Yes | 131 | 133 | ||
| No | 138 | 137 | ||
| Pancreatic duct drainage | 0.016 | 0.900 | ||
| External | 64 | 63 | ||
| Enteral | 205 | 207 | ||
| Intraoperative blood infusion | 1.310 | 0.252 | ||
| Yes | 36 | 46 | ||
| No | 233 | 224 | ||
| Operative time (min) | 0.299 | 0.584 | ||
| > 300 | 196 | 191 | ||
| ≤ 300 | 73 | 79 | ||
| Braun anastomosis | 2.274 | 0.132 | ||
| Yes | 78 | 94 | ||
| No | 192 | 175 | ||
| Pancreatic texture | 29.330 | 0.000 | ||
| Soft | 228 | 174 | ||
| Hard | 41 | 96 | ||
The risk factors for pancreatic fistula (gender, diabetes, BMI, blood glucose level, pancreaticojejunal anastomosis technique, the diameter of the pancreatic duct, and pancreatic texture) demonstrated in the univariate analysis were incorporated into the logistic regression analysis. The results showed that gender (male), BMI > 25, pancreatic duct-jejunum double-layer mucosa-to-mucosa pancreaticojejunal anastomosis, pancreatic duct diameter ≤ 3 mm, and soft pancreas were risk factors for pancreatic fistula after pancreaticoduodenectomy (Table 4).
| Variable | B | SE | Wals | P value | OR | 95%CI |
| Sex | 0.579 | 0.196 | 8.688 | 0.003 | 1.784 | 1.214-2.622 |
| Body mass index | 0.518 | 0.213 | 5.941 | 0.015 | 1.679 | 1.107-2.546 |
| Pancreaticojejunostomy | 0.743 | 0.217 | 11.723 | 0.001 | 2.102 | 1.374-3.216 |
| Pancreatic duct diameter | 0.724 | 0.192 | 14.254 | 0.000 | 2.062 | 1.416-3.003 |
| Pancreatic texture | 1.115 | 0.227 | 24.102 | 0.000 | 3.048 | 1.953-4.757 |
The causes of pancreatic fistula include pancreaticojejunal anastomotic leak, leak from pancreatic resection, leak associated with damage to the pancreatic capsule, and leak via the puncture channel. Pancreatic fistula after pancreaticoduodenectomy is a common and serious complication and the most important cause of subsequent complications and death after this procedure[8,24-26]. The dilemma of pancreatic fistula after pancreaticoduodenectomy has not yet been resolved[27]. Currently, researchers believe that the following factors are related to pancreatic fistula: gender, age, preoperative jaundice, intraoperative blood loss, operative time, pancreatic texture, BMI, diameter of the main pancreatic duct, and pancreaticojejunal anastomosis[14,28-32]. Peng et al[33] suggested that bundled pancreaticogastrostomy was a safe and effective anastomosis technique to prevent the leakage of pancreatic juice from pancreaticojejunal anastomosis. Shubert et al[34] believed that the clinical risk score for pancreatic fistula (CRS-PF) could effectively predict pancreatic fistula after pancreaticoduodenectomy. In this study, multivariate logistic regression analysis showed that gender (male), BMI > 25, pancreatic duct-jejunum double-layer mucosa-to-mucosa pancreaticojejunal anastomosis, pancreatic duct diameter ≤ 3 mm, and soft pancreas were risk factors for pancreatic fistula after pancreaticoduodenectomy.
Kawai retrospectively analyzed the perioperative data from 1239 patients treated at 11 medical facilities from 2005 to 2009 and summarized that the male gender was a risk factor for pancreatic fistula after pancreaticoduodenectomy[35]. This study included 343 male patients (POPF rate: 54.23%) and 196 female patients (POPF rate: 42.35%). Univariate analysis showed that the difference in the POPF rate was significant (P = 0.008), suggesting that male patients were at a higher risk than female patients for the development of pancreatic fistula after pancreaticoduodenectomy. Additionally, multivariate logistic regression analysis showed that the difference was significant (P = 0.003), suggesting that gender (male) was a risk factor for pancreatic fistula after pancreaticoduodenectomy. The odds ratio (OR = 1.784; 95%CI: 1.214-2.622) showed that the risk of developing pancreatic fistula after pancreaticoduodenectomy was 1.784-fold higher in male patients than in female patients.
El Nakeeb et al[36] analyzed 471 cases of pancreaticoduodenectomy and found that BMI > 25 was a risk factor for POPF. Gaujoux et al[28] analyzed 100 successive cases of pancreaticoduodenectomy and similarly found that BMI > 25 was a risk factor for pancreatic fistula after pancreaticoduodenectomy. In our study, 392 patients had a BMI ≤ 25 (POPF rate: 46.94%), and 147 patients had a BMI > 25 (POPF rate: 57.82%). Univariate analysis showed that the difference in the POPF rates was significant (P = 0.024), suggesting that patients with a BMI > 25 were at a higher risk of developing pancreatic fistula after pancreaticoduodenectomy than patients with a BMI ≤ 25. Additionally, multivariate logistic regression analysis showed that the difference was significant (P = 0.015 < 0.05), which indicated that BMI > 25 was a risk factor for pancreatic fistula after pancreaticoduodenectomy. The OR (1.679, 95%CI: 1.107-2.546) showed that the risk of developing a pancreatic fistula after pancreaticoduodenectomy was 1.679-fold higher in patients with a BMI > 25 than in patients with a BMI ≤ 25. The higher incidence of pancreatic fistula after pancreaticoduodenectomy in patients with a BMI > 25 may be associated with the following factors: increased difficulty in exposing the pancreas during surgery due to a higher volume of abdominal fat and peripancreatic fat, a higher risk of damage to the pancreatic capsule during separation due to a soft and brittle pancreas, and a higher risk of pancreatic leakage caused by damage to the pancreatic tissue and fine pancreatic ducts due to suturing and knotting during pancreaticojejunal anastomosis.
Pancreaticojejunal anastomosis is a critical step during pancreaticoduodenectomy and affects the surgical outcome. However, pancreaticojejunal anastomosis is a complex procedure during pancreaticoduodenectomy, and the choice of an appropriate pancreaticojejunal anastomosis technique should reduce the incidence of pancreatic fistula[33,37-40]. Fu et al[32] retrospectively analyzed 532 cases of pancreaticoduodenectomy and found that the pancreaticojejunal anastomosis technique was a risk factor for pancreatic fistula after pancreaticoduodenectomy. In this study, pancreatic duct-jejunum double-layer mucosa-to-mucosa pancreaticojejunal anastomosis was performed in 398 patients (POPF rate: 57.54%), and pancreatic-jejunum single-layer mucosa-to-mucosa anastomosis was performed in 141 patients (POPF rate: 35.46%). Univariate analysis showed that the difference in the POPF rates was significant (P = 0.000), suggesting that patients who underwent pancreatic duct-jejunum double-layer mucosa-to-mucosa pancreaticojejunal anastomosis were at a higher risk of developing pancreatic fistula after pancreaticoduodenectomy than patients who underwent pancreatic-jejunum single-layer mucosa-to-mucosa anastomosis. Additionally, multivariate logistic regression analysis showed that the difference was significant (P = 0.001), suggesting that pancreatic duct-jejunum double-layer mucosa-to-mucosa pancreaticojejunal anastomosis was an independent risk factor for pancreatic fistula after pancreaticoduodenectomy. The OR (2.102, 95%CI: 1.374-3.216) indicated that the risk of developing a pancreatic fistula after pancreaticoduodenectomy was 2.102-fold higher in patients who underwent pancreatic duct-jejunum double-layer mucosa-to-mucosa pancreaticojejunal anastomosis than in patients who underwent pancreatic-jejunum single-layer mucosa-to-mucosa anastomosis. The higher incidence of pancreatic fistula after pancreaticoduodenectomy in patients who underwent pancreatic duct-jejunum double-layer mucosa-to-mucosa pancreaticojejunal anastomosis may be related to the following factors: use of the 6-0 PDS II suture during pancreatic duct-jejunum anastomosis because the fine suture can easily cut the pancreatic duct during suturing and knotting, thereby resulting in a pancreaticojejunal anastomotic leak, and the use of the 5-0 PDS II suture to suture the pancreatic section and the jejunal seromuscular layer because this suture can easily cut the pancreas and fine pancreatic ducts during suturing and may not tightly secure the pancreatic section and the jejunal seromuscular layer, thereby resulting in pancreatic leakage and leakage from the fine pancreatic ducts. In contrast, the 4-0 Vicryl suture is used for full-layer suturing of the pancreas, the pancreatic duct, and the jejunum during pancreatic-jejunum single-layer mucosa-to-mucosa anastomosis; therefore, the suture is secure and reduces the risk of cutting the pancreas. Moreover, the jejunal seromuscular layer covers the entire pancreatic section and presses the fine pancreatic ducts at the pancreatic section, thereby reducing pancreatic leakage[38].
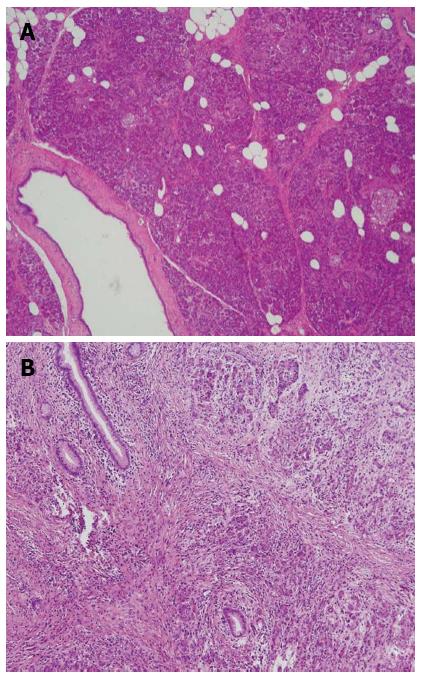
A soft pancreas is a risk factor for pancreatic fistula after pancreaticoduodenectomy[35-37,41,42]. The pancreatic stumps of all cases were submitted for pathological diagnosis of the degree of pancreatic fibrosis. All cases of pancreatic texture were divided into two groups (normal soft pancreas with no significant fibrosis, as shown in Figure 1A, and hard pancreas with fibrosis, as shown in Figure 1B). In this study, 402 patients had a soft pancreas (POPF rate: 56.72%), and 137 patients had a hard pancreas (POPF rate: 29.93%). Univariate analysis showed that the difference in the POPF rates was significant (P = 0.000), suggesting that patients with a soft pancreas were at a higher risk of developing a pancreatic fistula after pancreaticoduodenectomy than patients with a hard pancreas. Additionally, multivariate logistic regression analysis demonstrated that the difference was significant (P = 0.000), which indicated that a soft pancreas was an independent risk factor for pancreatic fistula after pancreaticoduodenectomy. The OR (3.048, 95%CI: 1.953-4.757) showed that the risk of developing a pancreatic fistula after pancreaticoduodenectomy was 3.048-fold higher in patients with a soft pancreas than in patients with a hard pancreas. The higher incidence of pancreatic fistula after pancreaticoduodenectomy in patients with a soft pancreas may be related to insecure suturing and knotting, which can result in unsatisfactory pancreaticojejunal anastomosis and a higher risk of damage to the pancreatic tissue and fine pancreatic ducts during suturing and knotting of a soft pancreas, resulting in pancreatic leakage. The lower incidence of pancreatic fistula after pancreaticoduodenectomy in patients with a hard pancreas may be related to pancreatic exocrine dysfunction due to prolonged pancreatic duct obstruction and pancreatic fibrosis, secure pancreaticojejunal anastomosis, and obstructed minor ducts at the cut-surface of the hard pancreas, and this could help reduce POPF[43] and risk of damage to the pancreatic tissue and fine pancreatic ducts during suturing and knotting. Pancreatic texture is the most significant single predictor of POPF, and clinicians should select a pancreaticojejunal anastomosis technique based on the texture of the pancreas to reduce the incidence of POPF[44].
Pancreatic duct diameter ≤ 3 mm is a risk factor for pancreatic fistula after pancreaticoduodenectomy[14,37]. In this study, the diameter of the pancreatic duct was ≤ 3 mm in 320 patients (POPF rate: 57.81%) and > 3 mm in 219 patients (POPF rate: 38.36%). Univariate analysis showed that the difference in the POPF rates was significant (P = 0.000), suggesting that patients with a pancreatic duct diameter ≤ 3 mm were at a higher risk of developing a pancreatic fistula after pancreaticoduodenectomy than patients with a pancreatic duct diameter > 3 mm. Additionally, multivariate logistic regression analysis indicated that the difference was significant (P = 0.000), suggesting that pancreatic duct diameter ≤ 3 mm was an independent risk factor for pancreatic fistula after pancreaticoduodenectomy. The OR (2.062, 95%CI: 1.416-3.003) showed that the risk of developing a pancreatic fistula after pancreaticoduodenectomy was 2.062-fold higher in patients with a pancreatic duct diameter ≤ 3 mm than in patients with a pancreatic duct diameter > 3 mm. The lower incidence of pancreatic fistula after pancreaticoduodenectomy in patients with a pancreatic duct diameter > 3 mm may be related to pancreatic duct obstruction, pancreatic duct fibrosis, pancreatic fibrosis, ease of suturing, and a lower risk of damage to the pancreatic duct during suturing and knotting. As a result, the incidence of pancreatic fistula after pancreaticoduodenectomy was lower in patients with pancreatic duct dilation than in patients without.
Univariate analysis demonstrated that the incidence of pancreatic fistula after pancreaticoduodenectomy was significantly lower in diabetic patients than in non-diabetic patients (39.19% vs 51.61%, P = 0.047) and was significantly lower in patients with a blood glucose level > 6.0 mmol/L than in patients with a blood glucose level ≤ 6.0 mmol/L (41.14% vs 54.75%, P = 0.002). However, multivariate logistic regression analysis showed that these differences were not significant (P = 0.268 and P = 0.115, respectively); therefore, diabetes was not a risk factor for POPF.
In conclusion, gender (male), BMI > 25, pancreatic duct-jejunum double-layer mucosa-to-mucosa pancreaticojejunal anastomosis, pancreatic duct diameter ≤ 3 mm, and soft pancreas were risk factors for pancreatic fistula after pancreaticoduodenectomy.
Pancreaticoduodenectomy remains the standard surgical treatment for tumors involving the lower bile duct, the pancreatic head, the duodenal papilla, and the ampulla. Pancreaticoduodenectomy is difficult to perform and is associated with high morbidity and mortality. Most complications after pancreaticoduodenectomy are associated with postoperative pancreatic fistula (POPF); however, no definitive approach can prevent pancreatic fistulas.
The incidence of tumors involving the lower bile duct, the pancreatic head, the duodenal papilla, and the ampulla increases each year, and more patients are undergoing pancreaticoduodenectomy. Surgical techniques and perioperative management are improving; however, the incidence and postoperative mortality of POPF remain high.
Gender (male), BMI > 25, pancreatic duct-jejunum double-layer mucosa-to-mucosa pancreaticojejunal anastomosis, pancreatic duct diameter ≤ 3 mm, and soft pancreas are risk factors for pancreatic fistula after pancreaticoduodenectomy. Postoperative complications and deaths are related to pancreatic fistulas. For patients with a small pancreatic duct diameter or a soft pancreas, surgeons should select a pancreaticojejunal anastomosis technique that is associated with a lower incidence of POPF.
POPF was diagnosed in strict accordance with the definition of pancreatic fistula from the ISGPF. POPFs are more common in patients with relevant risk factors, such as male gender, BMI > 25, pancreatic duct-jejunum double-layer mucosa-to-mucosa pancreaticojejunal anastomosis, pancreatic duct diameter ≤ 3 mm, and soft pancreas. Care must be taken in patients with any of these risk factors, and an appropriate pancreaticojejunal anastomosis technique should be selected based on the texture of the pancreas and the diameter of the pancreatic duct. Patients must be closely monitored after surgery, and patients with a pancreatic fistula must be treated promptly to reduce the risk of fatal complications.
Pancreaticoduodenectomy remains the standard surgical treatment for tumors involving the lower bile duct, the pancreatic head, the duodenal papilla, and the ampulla. POPF is common after pancreaticoduodenectomy and is the leading cause of postoperative complications and death following this procedure.
This retrospective study was well designed, and the statistical analysis was highly accurate. The article has a sufficient number of references. The manuscript language is of high quality, and the conclusions of the study are rational. The findings from this study contribute to our understanding of pancreatic fistula after pancreaticoduodenectomy. Readers with an interest in pancreatic fistulas will find this paper beneficial and informative.
| 1. | Brown EG, Yang A, Canter RJ, Bold RJ. Outcomes of pancreaticoduodenectomy: where should we focus our efforts on improving outcomes? JAMA Surg. 2014;149:694-699. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 47] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 2. | Yamashita Y, Shirabe K, Tsujita E, Takeishi K, Ikeda T, Yoshizumi T, Furukawa Y, Ishida T, Maehara Y. Surgical outcomes of pancreaticoduodenectomy for periampullary tumors in elderly patients. Langenbecks Arch Surg. 2013;398:539-545. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 18] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 3. | Topal B, Aerts R, Hendrickx T, Fieuws S, Penninckx F. Determinants of complications in pancreaticoduodenectomy. Eur J Surg Oncol. 2007;33:488-492. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 33] [Cited by in RCA: 33] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 4. | Wang Q, Gurusamy KS, Lin H, Xie X, Wang C. Preoperative biliary drainage for obstructive jaundice. Cochrane Database Syst Rev. 2008;CD005444. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3850] [Cited by in RCA: 2777] [Article Influence: 925.7] [Reference Citation Analysis (4)] |
| 5. | Winter JM, Cameron JL, Yeo CJ, Alao B, Lillemoe KD, Campbell KA, Schulick RD. Biochemical markers predict morbidity and mortality after pancreaticoduodenectomy. J Am Coll Surg. 2007;204:1029-1036; discussion 1037-1038. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 104] [Cited by in RCA: 93] [Article Influence: 4.9] [Reference Citation Analysis (0)] |
| 6. | Hiyoshi M, Chijiiwa K, Fujii Y, Imamura N, Nagano M, Ohuchida J. Usefulness of drain amylase, serum C-reactive protein levels and body temperature to predict postoperative pancreatic fistula after pancreaticoduodenectomy. World J Surg. 2013;37:2436-2442. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 47] [Cited by in RCA: 58] [Article Influence: 4.8] [Reference Citation Analysis (1)] |
| 7. | Ansorge C, Nordin JZ, Lundell L, Strömmer L, Rangelova E, Blomberg J, Del Chiaro M, Segersvärd R. Diagnostic value of abdominal drainage in individual risk assessment of pancreatic fistula following pancreaticoduodenectomy. Br J Surg. 2014;101:100-108. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 62] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 8. | Andrianello S, Pea A, Pulvirenti A, Allegrini V, Marchegiani G, Malleo G, Butturini G, Salvia R, Bassi C. Pancreaticojejunostomy after pancreaticoduodenectomy: Suture material and incidence of post-operative pancreatic fistula. Pancreatology. 2016;16:138-141. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 32] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 9. | Chen Y, Zhu X, Huang J, Zhu Y. End-to-Side Penetrating-Suture Pancreaticojejunostomy: A Novel Anastomosis Technique. J Am Coll Surg. 2015;221:e81-e86. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 13] [Article Influence: 1.2] [Reference Citation Analysis (2)] |
| 10. | Sandini M, Bernasconi DP, Ippolito D, Nespoli L, Baini M, Barbaro S, Fior D, Gianotti L. Preoperative Computed Tomography to Predict and Stratify the Risk of Severe Pancreatic Fistula After Pancreatoduodenectomy. Medicine (Baltimore). 2015;94:e1152. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 39] [Cited by in RCA: 38] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 11. | Miller BC, Christein JD, Behrman SW, Drebin JA, Pratt WB, Callery MP, Vollmer CM. A multi-institutional external validation of the fistula risk score for pancreatoduodenectomy. J Gastrointest Surg. 2014;18:172-179; discussion 179-180. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 178] [Cited by in RCA: 165] [Article Influence: 13.8] [Reference Citation Analysis (0)] |
| 12. | Sugimoto M, Takahashi S, Gotohda N, Kato Y, Kinoshita T, Shibasaki H, Konishi M. Schematic pancreatic configuration: a risk assessment for postoperative pancreatic fistula after pancreaticoduodenectomy. J Gastrointest Surg. 2013;17:1744-1751. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 41] [Cited by in RCA: 45] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 13. | Addeo P, Delpero JR, Paye F, Oussoultzoglou E, Fuchshuber PR, Sauvanet A, Sa Cunha A, Le Treut YP, Adham M, Mabrut JY. Pancreatic fistula after a pancreaticoduodenectomy for ductal adenocarcinoma and its association with morbidity: a multicentre study of the French Surgical Association. HPB (Oxford). 2014;16:46-55. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 133] [Cited by in RCA: 130] [Article Influence: 10.8] [Reference Citation Analysis (0)] |
| 14. | Liu QY, Zhang WZ, Xia HT, Leng JJ, Wan T, Liang B, Yang T, Dong JH. Analysis of risk factors for postoperative pancreatic fistula following pancreaticoduodenectomy. World J Gastroenterol. 2014;20:17491-17497. [PubMed] [DOI] [Full Text] |
| 15. | Roberts KJ, Sutcliffe RP, Marudanayagam R, Hodson J, Isaac J, Muiesan P, Navarro A, Patel K, Jah A, Napetti S. Scoring System to Predict Pancreatic Fistula After Pancreaticoduodenectomy: A UK Multicenter Study. Ann Surg. 2015;261:1191-1197. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 92] [Cited by in RCA: 124] [Article Influence: 12.4] [Reference Citation Analysis (1)] |
| 16. | Harnoss JC, Ulrich AB, Harnoss JM, Diener MK, Büchler MW, Welsch T. Use and results of consensus definitions in pancreatic surgery: a systematic review. Surgery. 2014;155:47-57. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 87] [Cited by in RCA: 116] [Article Influence: 8.9] [Reference Citation Analysis (0)] |
| 17. | Yeo CJ, Cameron JL, Sohn TA, Lillemoe KD, Pitt HA, Talamini MA, Hruban RH, Ord SE, Sauter PK, Coleman J. Six hundred fifty consecutive pancreaticoduodenectomies in the 1990s: pathology, complications, and outcomes. Ann Surg. 1997;226:248-257; discussion 257-260. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1440] [Cited by in RCA: 1326] [Article Influence: 45.7] [Reference Citation Analysis (2)] |
| 18. | Reid-Lombardo KM, Farnell MB, Crippa S, Barnett M, Maupin G, Bassi C, Traverso LW. Pancreatic anastomotic leakage after pancreaticoduodenectomy in 1,507 patients: a report from the Pancreatic Anastomotic Leak Study Group. J Gastrointest Surg. 2007;11:1451-1458; discussion 1459. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 189] [Cited by in RCA: 189] [Article Influence: 9.9] [Reference Citation Analysis (0)] |
| 19. | Lermite E, Pessaux P, Brehant O, Teyssedou C, Pelletier I, Etienne S, Arnaud JP. Risk factors of pancreatic fistula and delayed gastric emptying after pancreaticoduodenectomy with pancreaticogastrostomy. J Am Coll Surg. 2007;204:588-596. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 118] [Cited by in RCA: 124] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 20. | Schmidt CM, Choi J, Powell ES, Yiannoutsos CT, Zyromski NJ, Nakeeb A, Pitt HA, Wiebke EA, Madura JA, Lillemoe KD. Pancreatic fistula following pancreaticoduodenectomy: clinical predictors and patient outcomes. HPB Surg. 2009;2009:404520. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 67] [Cited by in RCA: 77] [Article Influence: 4.5] [Reference Citation Analysis (2)] |
| 21. | Hackert T, Büchler MW. Randomized clinical trial of isolated Roux-en-Y versus conventional reconstruction after pancreaticoduodenectomy (Br J Surg 2014; 101: 1084-1091). Br J Surg. 2014;101:1092. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 22. | Pessaux P, Sauvanet A, Mariette C, Paye F, Muscari F, Cunha AS, Sastre B, Arnaud JP. External pancreatic duct stent decreases pancreatic fistula rate after pancreaticoduodenectomy: prospective multicenter randomized trial. Ann Surg. 2011;253:879-885. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 236] [Cited by in RCA: 199] [Article Influence: 13.3] [Reference Citation Analysis (1)] |
| 23. | McKay A, Mackenzie S, Sutherland FR, Bathe OF, Doig C, Dort J, Vollmer CM, Dixon E. Meta-analysis of pancreaticojejunostomy versus pancreaticogastrostomy reconstruction after pancreaticoduodenectomy. Br J Surg. 2006;93:929-936. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 153] [Cited by in RCA: 141] [Article Influence: 7.1] [Reference Citation Analysis (0)] |
| 24. | Bassi C, Dervenis C, Butturini G, Fingerhut A, Yeo C, Izbicki J, Neoptolemos J, Sarr M, Traverso W, Buchler M. Postoperative pancreatic fistula: an international study group (ISGPF) definition. Surgery. 2005;138:8-13. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3690] [Cited by in RCA: 3341] [Article Influence: 159.1] [Reference Citation Analysis (1)] |
| 25. | Aranha GV, Hodul PJ, Creech S, Jacobs W. Zero mortality after 152 consecutive pancreaticoduodenectomies with pancreaticogastrostomy. J Am Coll Surg. 2003;197:223-231; discussion 231-232. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 67] [Cited by in RCA: 61] [Article Influence: 2.7] [Reference Citation Analysis (1)] |
| 26. | Rezvani M, O’Moore PV, Pezzi CM. Late pancreaticojejunostomy stent migration and hepatic abscess after Whipple procedure. J Surg Educ. 2007;64:220-223. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 25] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 27. | Grobmyer SR, Rivadeneira DE, Goodman CA, Mackrell P, Lieberman MD, Daly JM. Pancreatic anastomotic failure after pancreaticoduodenectomy. Am J Surg. 2000;180:117-120. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 66] [Cited by in RCA: 56] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 28. | Gaujoux S, Cortes A, Couvelard A, Noullet S, Clavel L, Rebours V, Lévy P, Sauvanet A, Ruszniewski P, Belghiti J. Fatty pancreas and increased body mass index are risk factors of pancreatic fistula after pancreaticoduodenectomy. Surgery. 2010;148:15-23. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 314] [Cited by in RCA: 286] [Article Influence: 17.9] [Reference Citation Analysis (0)] |
| 29. | Ross A, Mohammed S, Vanburen G, Silberfein EJ, Artinyan A, Hodges SE, Fisher WE. An assessment of the necessity of transfusion during pancreatoduodenectomy. Surgery. 2013;154:504-511. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 42] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 30. | Wang S, Wang X, Li L, Dai H, Han J. Association of preoperative obstructive jaundice with postoperative infectious complications following pancreaticoduodenectomy. Hepatogastroenterology. 2013;60:1274-1279. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 31. | Faraj W, Alameddine R, Mukherji D, Musallam K, Haydar A, Eloubiedi M, Shamseddine A, Halal A, Abou-Alfa GK, O’Reilly EM. Postoperative outcomes following pancreaticoduodenectomy: how should age affect clinical practice? World J Surg Oncol. 2013;11:131. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 18] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 32. | Fu SJ, Shen SL, Li SQ, Hu WJ, Hua YP, Kuang M, Liang LJ, Peng BG. Risk factors and outcomes of postoperative pancreatic fistula after pancreatico-duodenectomy: an audit of 532 consecutive cases. BMC Surg. 2015;15:34. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 68] [Cited by in RCA: 58] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 33. | Peng SY, Wang JW, Hong DF, Liu YB, Wang YF. Binding pancreaticoenteric anastomosis: from binding pancreaticojejunostomy to binding pancreaticogastrostomy. Updates Surg. 2011;63:69-74. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 38] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 34. | Shubert CR, Wagie AE, Farnell MB, Nagorney DM, Que FG, Reid Lombardo KM, Truty MJ, Smoot RL, Kendrick ML. Clinical Risk Score to Predict Pancreatic Fistula after Pancreatoduodenectomy: Independent External Validation for Open and Laparoscopic Approaches. J Am Coll Surg. 2015;221:689-698. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 68] [Cited by in RCA: 99] [Article Influence: 9.0] [Reference Citation Analysis (1)] |
| 35. | Kawai M, Kondo S, Yamaue H, Wada K, Sano K, Motoi F, Unno M, Satoi S, Kwon AH, Hatori T. Predictive risk factors for clinically relevant pancreatic fistula analyzed in 1,239 patients with pancreaticoduodenectomy: multicenter data collection as a project study of pancreatic surgery by the Japanese Society of Hepato-Biliary-Pancreatic Surgery. J Hepatobiliary Pancreat Sci. 2011;18:601-608. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 185] [Cited by in RCA: 169] [Article Influence: 11.3] [Reference Citation Analysis (1)] |
| 36. | El Nakeeb A, Salah T, Sultan A, El Hemaly M, Askr W, Ezzat H, Hamdy E, Atef E, El Hanafy E, El-Geidie A. Pancreatic anastomotic leakage after pancreaticoduodenectomy. Risk factors, clinical predictors, and management (single center experience). World J Surg. 2013;37:1405-1418. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 142] [Cited by in RCA: 137] [Article Influence: 10.5] [Reference Citation Analysis (0)] |
| 37. | Yang YM, Tian XD, Zhuang Y, Wang WM, Wan YL, Huang YT. Risk factors of pancreatic leakage after pancreaticoduodenectomy. World J Gastroenterol. 2005;11:2456-2461. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 214] [Cited by in RCA: 212] [Article Influence: 10.1] [Reference Citation Analysis (0)] |
| 38. | Hu BY, Leng JJ, Wan T, Zhang WZ. Application of single-layer mucosa-to-mucosa pancreaticojejunal anastomosis in pancreaticoduodenectomy. World J Gastrointest Surg. 2015;7:335-344. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 2] [Cited by in RCA: 2] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 39. | Erdmann J, van Eijick CHJ, Jeekel J. Standard resection of pancreatic cancer and chance of cure. Am J Surg. 2007;194:S104-S109. [RCA] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 40. | Kleespies A, Albertsmeier M, Obeidat F, Seeliger H, Jauch KW, Bruns CJ. The challenge of pancreatic anastomosis. Langenbecks Arch Surg. 2008;393:459-471. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 95] [Cited by in RCA: 89] [Article Influence: 4.9] [Reference Citation Analysis (0)] |
| 41. | Lin JW, Cameron JL, Yeo CJ, Riall TS, Lillemoe KD. Risk factors and outcomes in postpancreaticoduodenectomy pancreaticocutaneous fistula. J Gastrointest Surg. 2004;8:951-959. [PubMed] |
| 42. | Kiyochi H. Pathologic Assessment of Pancreatic Fibrosis for Objective Prediction of Pancreatic Fistula and Management of Prophylactic Drain Removal After Pancreaticoduodenectomy: Reply. World J Surg. 2016;40:1522-1523. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 20] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 43. | Kim EY, You YK, Kim DG, Hong TH. A simple pancreaticojejunostomy technique for hard pancreases using only two transpancreatic sutures with buttresses: a comparison with the previous pancreaticogastrostomy and dunking methods. Ann Surg Treat Res. 2016;90:64-71. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 11] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 44. | Wellner UF, Kayser G, Lapshyn H, Sick O, Makowiec F, Höppner J, Hopt UT, Keck T. A simple scoring system based on clinical factors related to pancreatic texture predicts postoperative pancreatic fistula preoperatively. HPB (Oxford). 2010;12:696-702. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 164] [Cited by in RCA: 161] [Article Influence: 10.1] [Reference Citation Analysis (0)] |
Manuscript source: Unsolicited manuscript
Specialty type: Gastroenterology and hepatology
Country of origin: China
Peer-review report classification
Grade A (Excellent): 0
Grade B (Very good): B, B
Grade C (Good): 0
Grade D (Fair): 0
Grade E (Poor): 0
Open-Access: This article is an open-access article which was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/
P- Reviewer: Adhoute X, De Paschale M S- Editor: Qi Y L- Editor: Wang TQ E- Editor: Ma S