Published online Jun 20, 2026. doi: 10.5662/wjm.v16.i2.114604
Revised: October 30, 2025
Accepted: December 8, 2025
Published online: June 20, 2026
Processing time: 211 Days and 23.9 Hours
Nearly 259 million people are living with chronic hepatitis B globally, with just 7 million of them receiving life-saving treatment. In 2022, 83% of all viral hepatitis deaths were attributed to hepatitis B. Despite the availability of effective vaccines, diagnostics, and treatments, hepatitis B continues to be underprioritized on the global health agenda. Stigma and discrimination have been pervasive and en
Core Tip: The article explores why chronic hepatitis B infection, despite affecting 259 million people globally, remains underprioritized. Only 3% of those infected receive treatment, and stigma, discrimination, and systemic neglect persist. Through lived experiences of people with hepatitis B worldwide, this article explores barriers to progress-such as marginalization of impacted population and inequitable funding among others, and draws lessons from human immunodeficiency virus, coronavirus disease 2019, and Ebola, where advocacy, political will, and investment drove change. It calls for stronger collaboration, greater investment in care and prevention, integration of disease programs, and inclusion of patient-reported outcomes to accelerate elimination and improve the lives of people living with hepatitis B.
- Citation: Ibrahim Y, Qureshi A, Jackson M, Zovich B, Freeland C, Flomo M, Alik K, Yakubov R, Chen LH, Yeboah PK, Cohen C. Why does hepatitis B remain underprioritized? A view through lived experience. World J Methodol 2026; 16(2): 114604
- URL: https://www.wjgnet.com/2222-0682/full/v16/i2/114604.htm
- DOI: https://dx.doi.org/10.5662/wjm.v16.i2.114604
In Ghana, Philip’s brother was not diagnosed with hepatitis B until after his doctor discovered he had liver cancer. With only one hospital serving the entire region, Philip’s brother was unable to get treatment to manage his quickly progress
Kenson found out about his hepatitis B diagnosis while living in the Marshall Islands. After learning that treatment options were limited where he lived, he moved to Hawaii with his family to seek better care. In Hawaii, Kenson learned that medication was not enough for his condition. He needed to get a liver transplant to restore his health.
Rav was two years old when he was infected with hepatitis B through a dirty needle during routine vaccination. He was told by his doctors that he could not play sports or participate in any physical education classes at school. As a result, Rav felt isolated from friends and the community around him. When he moved to Canada from Uzbekistan, his doctor discovered that he had liver cirrhosis and a co-infection with hepatitis delta. He finds hope and comfort in his family as he awaits new treatment options for hepatitis B and delta.
Bol lives in Uganda. Her family struggled to afford medication to manage her hepatitis B viral load, so she had to stop taking it. When her son was born, he was diagnosed with neonatal hepatitis B, as the preventative birth dose was not available at the hospital. Within four months, Bol’s son died in her arms, while her doctor blamed her for his death.
An international student from Liberia relocated to the United States to pursue his dream of becoming a nurse, only to face unexpected challenges due to his hepatitis B status. After being accepted into a nursing program in the United States, the student, excited to start his journey in healthcare, was met with an unanticipated hurdle; the school informed him that he could not continue his education due to his hepatitis B diagnosis.
Lynette was diagnosed with hepatitis B while studying to become a nurse. The doctors in Taiwan told her that she did not need to be treated despite displaying physical symptoms and a high viral load. Before she was approved to begin treatment to manage her hepatitis B, Lynette’s viral load had increased substantially, and she had significant fibrosis, showing signs of liver damage.
These are true experiences of people around the world who face unnecessary challenges due to the lack of priori
Hepatitis B is the most common liver infection in the world, with nearly 259 million people living with chronic hepatitis B[4]. It is often referred to as “silent infection” due to its few, nonspecific, symptoms and limited documentation on the physical, emotional, and social impacts of living with the virus[4-7]. Hepatitis B can have significant physical impacts if left undiagnosed or untreated[4-7]. Those living with hepatitis B are also at risk of contracting hepatitis D - the most severe form of viral hepatitis. Hepatitis B and hepatitis D infection significantly increase the progression of liver compli
The tools to prevent and eliminate hepatitis B - effective vaccines, sensitive diagnostic tests (including rapid tests), and antiviral treatments - are inexpensive to manufacture and widely available for countries to purchase. However, only 13% of people with chronic hepatitis B have been diagnosed, and a scant 3% receive treatment. Even more egregious, there were 1.2 million new global infections in 2022, and only 45% of infants received the life-saving birth dose vaccine[1]. While there are systemic and logistical challenges to eliminating hepatitis B, the sheer burden of morbidity and mortality should compel us to prioritize immediate implementation of models, best practices, and solutions to meet the 2030 World Health Assembly elimination goals[1].
Despite having the necessary tools to address hepatitis B and numerous nongovernmental organizations (NGOs) around the world poised and eager to address the issues, hepatitis B remains an afterthought to many governments and funding institutions worldwide[10]. This begs one simple question: Why? Why is a disease that impacts so many people so underprioritized? Why do we still have 1.2 million people newly infected every year[11,12]? Why is a disease with a vaccine that has been available for more than thirty years taking twice as long to eliminate compared to other vaccine-preventable diseases[13]? Why are there six million children under-five living with chronic hepatitis B, having to navigate a lifelong, potentially life-threatening illness[8]?
The answer is both simple and complex. Simply stated, the people living with hepatitis B face the same challenge that has persisted for centuries: The marginalization of vulnerable populations[14,15]. The implementation of solutions, however, is what makes the answer complex.
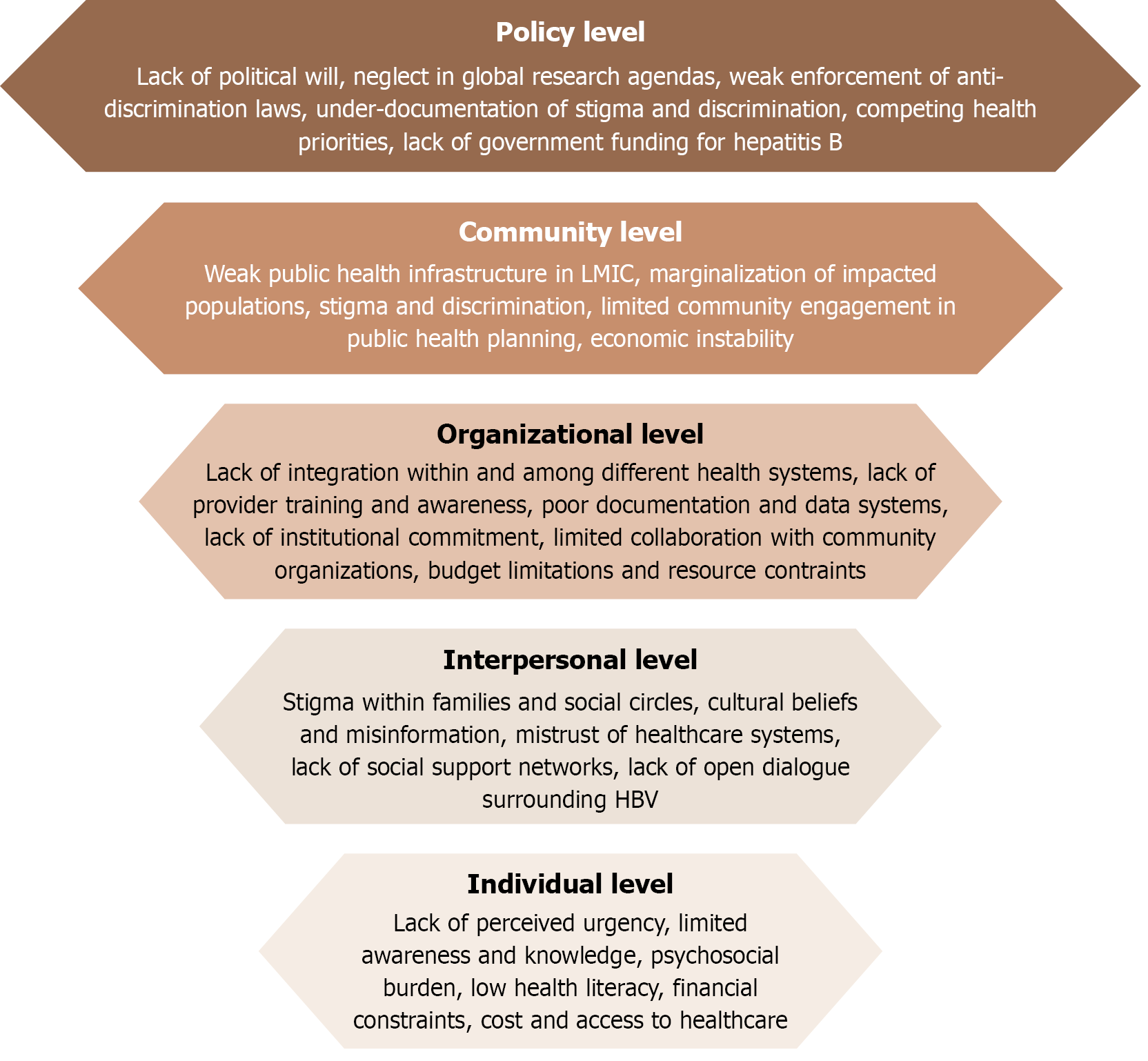
We can look to history to answer the question of why hepatitis B remains an underprioritized disease decades after its discovery. Table 1 presents clear definitions of key terminology used throughout this article. Figure 1 uses the social ecological model[16] to illustrate the intricate levels of barriers hindering global hepatitis B elimination. The virus is endemic to many countries and populations that have been marginalized by the global community for centuries. This marginalization has profoundly impacted the public health infrastructure and its ability to respond to certain diseases in many low- and middle-income countries. The all-too-common truth is that public health initiatives are often developed without input from those who will feel their impact. Much of the global public health movement is embedded in centuries-old colonialism that preserves a cycle of inequity[17]. Because of this, we often see that the flow of money from institutions to countries in need reflects the priorities of the donor and not the true needs of the recipient country[18,19]. This inequitable distribution of funds can perpetuate the idea that underfunded diseases - such as hepatitis B - must not be a public health concern[19]. Thus, NGOs and civil society organizations that attempt to resolve the problems identified by their communities are left with few resources to match the scope of the issue. Similarly, the global clinical research agenda is driven by the health needs that have the largest impact on wealthier nations[20,21]. This has contributed to inadequate research funding for diseases that have minimal social and economic consequences on those wealthy nations, like hepatitis B.
| Term | Definition |
| Marginalization | The systemic process through which persons are excluded/denied basic rights based on their identities, experiences, geographical location, race, gender, or class |
| Under-prioritization | The failure to allocate resources effectively and fairly, leading to delayed or suboptimal care and compromising patient safety and health outcomes. It may occur at the health system level, where institutions don’t meet the health demands of their community, or at the healthcare provider level, where healthcare providers don’t prioritize necessary treatment or interventions |
| Discrimination | The unjust, unfair, or prejudicial treatment of a person on the grounds of their hepatitis B status |
| Stigma | A social process experienced or anticipated, and is characterized by exclusion, rejection, blame, or devaluation resulting from experience, perception, or reasonable anticipation of an adverse social judgment about a person or a group |
Unlike similar diseases, such as human immunodeficiency virus (HIV), where funding decisions are centered upon moral and humanitarian bases, decisions about hepatitis B are often weighed based on the nature of the virus itself and not how it impacts individuals or communities[21]. The complex nature of hepatitis B virus (HBV) and the persistence of the infection are often cited to excuse the failure to satisfactorily fund programs addressing prevention and treatment. For hepatitis B to receive similar prioritization, there is a need to make the condition more visible and to document and share the human impact of living with it. Highlighting the social, emotional, and economic burden can help position hepatitis B not only as a medical issue but also as a public and social justice concern. Other diseases have gained remarkable global attention because of their impacts in high-income countries, stirring fear and vulnerability among the public, and urging officials to take immediate action. In contrast, the significance of living with hepatitis B is often ignored due to the absence of visible and more immediate consequences. The concerning health outcomes that bring widespread attention to other public health threats, such as the high mortality rates associated with the emergence of the coronavirus disease 2019 infection or the external bleeding caused by the Ebola virus, for example, are not present with hepatitis B. In contrast, hepatitis B has not yet benefited from comparable advocacy emphasizing its long-term, life-threatening consequences. Despite efforts from community-based organizations and people with lived experience, there remains limited awareness of the ultimate trajectory of hepatitis B infection, and its casual connection to liver cancer. Increasing education and awareness about this connection can underscore the high mortality burden associated with hepatitis B and foster greater urgency for action and resource allocation. Chronic hepatitis B infection can be equally devastating over time, but this is rarely visible. When visible symptoms do appear, they emerge many years after the infection was contracted. Hepatitis B-related health experiences, such as fatigue, pain, anxiety, and fear of disease progression, significantly impact QoL, yet are not considered in clinical endpoints or treatment decisions[4-7]. The disconnect between clinically defined outcomes and the lived experience enables a dismissive attitude towards the severity of the disease[5-7]. Moreover, a key gap lies in the lack of coordinated efforts between advocacy organizations and healthcare providers to highlight the physical, emotional, and psychological toll of living with hepatitis B[22]. Documenting lived experiences and amplifying the voices of those affected can help make the disease’s impact more tangible and human, highlighting its progressively debilitating nature and the urgent need for stronger response systems.
Underprioritization of hepatitis B programs aggravates stigma and discrimination related to hepatitis B. Intervention strategies to reduce hepatitis B-related stigma are usually integrated within larger hepatitis B educational outreach programs focused on raising awareness about transmission, prevention, and treatment. Although such programs exist, insufficient funds prevent the growth and expansion required to adequately address stigma and discrimination. Further
One of the current considerations for organizations supporting those with hepatitis B is integrating hepatitis B services into other public health programs like HIV and maternity programs. Thanks to generously funded HIV programs worldwide, a robust community-based infrastructure exists in most countries that are also impacted by hepatitis B. The similarities between HIV and hepatitis B infections make the case that integration would result in efficiency and better use of resources[15,23,24]. For example, many HIV programs already have the diagnostic equipment and well-trained personnel to successfully address hepatitis B. Both viruses can be treated with the same class of antivirals, and since both diseases share transmission routes, much of the prevention education is similar. However, programmatic integration has its own set of challenges. From patients’ perspective, people living with hepatitis B may be fearful of accessing care through HIV portals, and often feel that the stigma associated with HIV is worse than that of hepatitis B[23]. On the other hand, funding institutions will often provide funds that can only be used for HIV services, leaving out those with hepatitis B. This has led to a situation where the same antiviral treatments are being offered at no cost to people living with HIV, while being prohibitively expensive for people with hepatitis B in the same country[25]. Similar challenges face pregnant women who are living with hepatitis B, who often need to visit two different healthcare providers, and receive care for their hepatitis B separate from their antenatal care, creating a challenge for them to maintain their hepatitis B care[26].
These challenges exist despite the countless NGOs and civil society organizations that have mobilized advocates and encouraged their local governments to provide support for people living with hepatitis B. However, their efforts can’t help but fall short of addressing the massive problem when medical societies and healthcare providers fail to prioritize patient-centered approach to hepatitis B care, and when there are so few national governments and institutions making financial commitments and investments in hepatitis B elimination broadly[22,23].
With available and effective diagnostic tools, vaccines, and treatments, there is no reason that hepatitis B cannot be eliminated. So, why has this not happened? How much longer do people with hepatitis B have to wait for collective global action? It may be difficult to identify simple answers to the complexities surrounding hepatitis B, but one thing is certain: There is no justification for the underprioritization of hepatitis B. Philip, Bol, Kenson, Lynette, Rav, and the millions of people around the world living with hepatitis B deserve much more. With the call to eliminate viral hepatitis by the World Health Organization, and with other influential stakeholders beginning to include viral hepatitis in their efforts, we have a critical window of opportunity to prioritize hepatitis B. Without an effective collaboration between such powers, the goal of eliminating viral hepatitis will not be attainable. As priority and funding decisions for the coming years are being made, we must not forget the names or faces of the 259 million people suffering from hepatitis B, D, or liver cancer.
Achieving tangible progress toward hepatitis B elimination requires strategic investment and coordinated policy action. Governments, global partners, and industry partners must increase targeted investments to expand access to diagnostics, antiviral treatment, and preventive interventions, particularly in low- and middle-income countries where the burden remains highest.
There is an urgent need for greater integration across disease programs that currently operate in silos. To strengthen efficiency and reduce duplication, governments and international donor organizations should work together to align efforts, leveraging lessons from HIV, tuberculosis, and maternal health programs, to serve patients holistically as whole persons rather than through isolated disease-focused approaches.
Finally, medical and professional associations must incorporate patient-reported outcomes into the routine monitoring and evaluation of hepatitis B care. Centering patient experience in defining what effective care looks like will not only improve the quality of treatment and adherence but also ensure that care systems reflect the real needs and priorities of those living with hepatitis B.
Together, these actions would move hepatitis B from a neglected condition to a global health priority - supported by data, guided by patient voices, and sustained through coordinated policy and financing mechanisms.
Our special thanks go to the people living with chronic hepatitis B who bravely and voluntarily shared their lived expe
| 1. | World Health Organization. Global hepatitis report 2024: action for access in low- and middle-income countries. [cited 25 November 2025]. Available from: https://www.who.int/publications/i/item/9789240091672. |
| 2. | Freeland C, Mendola L, Cheng V, Cohen C, Wallace J. The unvirtuous cycle of discrimination affecting people with hepatitis B: a multi-country qualitative assessment of key-informant perspectives. Int J Equity Health. 2022;21:77. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 15] [Reference Citation Analysis (0)] |
| 3. | Wallace J, Pitts M, Liu C, Lin V, Hajarizadeh B, Richmond J, Locarnini S. More than a virus: a qualitative study of the social implications of hepatitis B infection in China. Int J Equity Health. 2017;16:137. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 27] [Cited by in RCA: 43] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 4. | Hsu YC, Huang DQ, Nguyen MH. Global burden of hepatitis B virus: current status, missed opportunities and a call for action. Nat Rev Gastroenterol Hepatol. 2023;20:524-537. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 474] [Cited by in RCA: 417] [Article Influence: 139.0] [Reference Citation Analysis (2)] |
| 5. | Ibrahim Y, Umstead M, Wang S, Cohen C. The Impact of Living With Chronic Hepatitis B on Quality of Life: Implications for Clinical Management. J Patient Exp. 2023;10:23743735231211069. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 6. | Younossi ZM, Stepanova M, Younossi I, Papatheodoridis G, Janssen HLA, Agarwal K, Nguyen MH, Gane E, Tsai N, Nader F. Patient-reported outcomes in patients chronic viral hepatitis without cirrhosis: The impact of hepatitis B and C viral replication. Liver Int. 2019;39:1837-1844. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 26] [Article Influence: 3.7] [Reference Citation Analysis (3)] |
| 7. | Ibrahim Y, Zovich B, Ansah B, Freeland C, Jackson M, Tu T, Cohen C. Quality of life of people living with chronic hepatitis B: The role of social support system. PLOS Glob Public Health. 2024;4:e0003103. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 8] [Reference Citation Analysis (0)] |
| 8. | Terrault NA, Lok ASF, McMahon BJ, Chang KM, Hwang JP, Jonas MM, Brown RS Jr, Bzowej NH, Wong JB. Update on prevention, diagnosis, and treatment of chronic hepatitis B: AASLD 2018 hepatitis B guidance. Hepatology. 2018;67:1560-1599. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3558] [Cited by in RCA: 3195] [Article Influence: 399.4] [Reference Citation Analysis (6)] |
| 9. | World Health Organization. Guidelines for the prevention, diagnosis, care and treatment for people with chronic hepatitis B infection. [cited 25 November 2025]. Available from: https://www.who.int/publications/i/item/9789240090903. |
| 10. | O'Hara GA, McNaughton AL, Maponga T, Jooste P, Ocama P, Chilengi R, Mokaya J, Liyayi MI, Wachira T, Gikungi DM, Burbridge L, O'Donnell D, Akiror CS, Sloan D, Torimiro J, Yindom LM, Walton R, Andersson M, Marsh K, Newton R, Matthews PC. Hepatitis B virus infection as a neglected tropical disease. PLoS Negl Trop Dis. 2017;11:e0005842. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 57] [Cited by in RCA: 62] [Article Influence: 6.9] [Reference Citation Analysis (0)] |
| 11. | World Health Organization. Global progress report on HIV, viral hepatitis and sexually transmitted infections, 2021. Accountability for the global health sector strategies 2016-2021: actions for impact. [cited 25 November 2025]. Available from: https://www.who.int/publications/i/item/9789240090903. |
| 12. | Rumgay H, Arnold M, Ferlay J, Lesi O, Cabasag CJ, Vignat J, Laversanne M, McGlynn KA, Soerjomataram I. Global burden of primary liver cancer in 2020 and predictions to 2040. J Hepatol. 2022;77:1598-1606. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1781] [Cited by in RCA: 1561] [Article Influence: 390.3] [Reference Citation Analysis (5)] |
| 13. | Vashishtha VM, Kamath S. A Brief History of Vaccines Against Polio. Indian Pediatr. 2016;53 Suppl 1:S20-S27. [PubMed] |
| 14. | Baah FO, Teitelman AM, Riegel B. Marginalization: Conceptualizing patient vulnerabilities in the framework of social determinants of health-An integrative review. Nurs Inq. 2019;26:e12268. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 48] [Cited by in RCA: 178] [Article Influence: 22.3] [Reference Citation Analysis (0)] |
| 15. | Martyn E, Eisen S, Longley N, Harris P, Surey J, Norman J, Brown M, Sultan B, Maponga TG, Iwuji C, Flanagan S, Ghosh I, Story A, Matthews PC. The forgotten people: Hepatitis B virus (HBV) infection as a priority for the inclusion health agenda. Elife. 2023;12:e81070. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 52] [Article Influence: 17.3] [Reference Citation Analysis (0)] |
| 16. | Ewald DR, Orsini MM, Strack RW. The path to good health: Shifting the dialogue and promoting social ecological thinking. SSM Popul Health. 2023;22:101378. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 11] [Reference Citation Analysis (0)] |
| 17. | Hussain M, Sadigh M, Sadigh M, Rastegar A, Sewankambo N. Colonization and decolonization of global health: which way forward? Glob Health Action. 2023;16:2186575. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 26] [Article Influence: 8.7] [Reference Citation Analysis (0)] |
| 18. | Maani N, Abdalla SM, Ettman CK, Parsey L, Rhule E, Allotey P, Galea S. Global Health Equity Requires Global Equity. Health Equity. 2023;7:192-196. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 14] [Reference Citation Analysis (0)] |
| 19. | Olusanya JO, Ubogu OI, Njokanma FO, Olusanya BO. Transforming global health through equity-driven funding. Nat Med. 2021;27:1136-1138. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 45] [Article Influence: 9.0] [Reference Citation Analysis (0)] |
| 20. | Binagwaho A, Allotey P, Sangano E, Ekström AM, Martin K. A call to action to reform academic global health partnerships. BMJ. 2021;375:n2658. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 22] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 21. | Shiffman J, Shawar YR. Framing and the formation of global health priorities. Lancet. 2022;399:1977-1990. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 52] [Article Influence: 13.0] [Reference Citation Analysis (0)] |
| 22. | Matthews PC, Jack K, Wang S, Abbott J, Bryce K, Cheng B, Ghosh I, Story A, Chen J, Munoz C, Bell J, Riddell S, Goldring A, Goddard C, Moraras K, Cohen C, Brown K, Lazarus JV, Elsharkawy AM. A call for advocacy and patient voice to eliminate hepatitis B virus infection. Lancet Gastroenterol Hepatol. 2022;7:282-285. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 18] [Reference Citation Analysis (0)] |
| 23. | Mutyoba JN, Wandera C, Ejalu D, Seremba E, Beyagira R, Amandua J, Mugagga K, Kambugu A, Muganzi A, Easterbrook P, Ocama P. Feasibility and acceptability of integrating hepatitis B care into routine HIV services: a qualitative study among health care providers and patients in West Nile region, Uganda. BMC Health Serv Res. 2023;23:59. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |
| 24. | Ejalu DL, Mutyoba JN, Wandera C, Seremba E, Kambugu A, Muganzi A, Beyagira R, Amandua J, Mugagga K, Easterbrook P, Ocama P. Integrating hepatitis B care and treatment with existing HIV services is possible: cost of integrated HIV and hepatitis B treatment in a low-resource setting: a cross-sectional hospital-based cost-minimisation assessment. BMJ Open. 2022;12:e058722. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 25. | Clinton Health Access Initiative. CHAI publishes the 2022 Hepatitis B Market Report. [cited 3 March 2025]. Available from: https://www.clintonhealthaccess.org/report/2022-hepatitis-b-market-report/. |
| 26. | Wulandari LPL, Lubis DS, Kurniati DPY, Sumintang K, Ardrini DAM, Mariani P, Januraga PP, Camellia A, Laksmi NMDP, Mahmudah L, Ong JJ, Causer L, Liverani M, Guy R, Wiseman V. Challenges to integrating programs for the elimination of mother-to-child transmission of HIV, syphilis, and hepatitis B into antenatal care: Experiences from Indonesia. PLOS Glob Public Health. 2024;4:e0002977. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |