Published online Jun 20, 2026. doi: 10.5662/wjm.v16.i2.114180
Revised: October 21, 2025
Accepted: January 13, 2026
Published online: June 20, 2026
Processing time: 222 Days and 22.3 Hours
Gender disparities across nearly all surgical specialties have become an issue of increasing attention, reflecting persistent inequities in representation, leadership, and career advancement. Despite growing numbers of female medical graduates worldwide, women continue to remain underrepresented in surgery, particularly in subspecialties such as transplantation surgery.
To explore gender inequalities among transplant surgeons from the perspective of transplant unit directors and female surgeons worldwide.
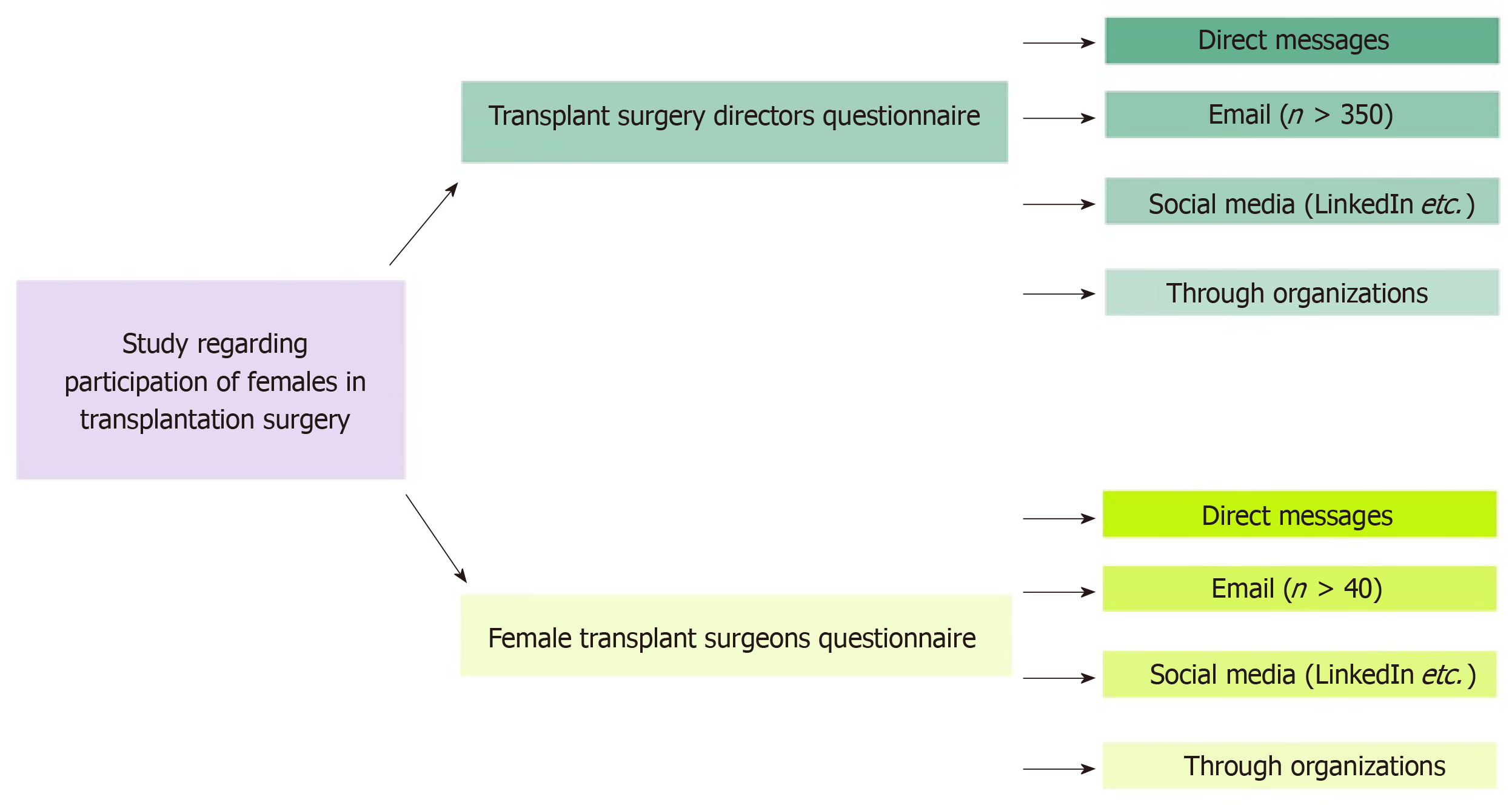
This study consists of two arms: (1) An 8-item anonymous questionnaire was sent to transplant centers to assess the gender distribution of consultant surgeons’ positions and academic roles among female and male surgeons; and (2) A 23-item anonymous questionnaire with closed and open questions was distributed to female transplant surgeons worldwide, addressing demographic profile, working experiences, and suggestions towards professional equality. The questionnaires were promoted through email, social media and professional platforms.
Of 46 transplant units participated. Among the 381 board-certified surgeons re
This is the first cross-sectional study addressing gender equity within the field of transplantation surgery wor
Core Tip: This manuscript presents the results of the first worldwide cross-sectional study to document gender inequities in transplantation surgery. By surveying both transplant unit directors and female transplant surgeons, it reveals disparities in academic and leadership roles, frequent experiences of gender discrimination and sexual harassment, and highlights the need for mentorship, equitable leadership opportunities, and institutional policies that support work-life balance.
- Citation: Avramidou E, Tsoulfas G, Alexiou M, Papachristou C. Breaking the scalpel ceiling: Gender inequality in global transplant surgery. World J Methodol 2026; 16(2): 114180
- URL: https://www.wjgnet.com/2222-0682/full/v16/i2/114180.htm
- DOI: https://dx.doi.org/10.5662/wjm.v16.i2.114180
The history of women in medicine can be traced to Elizabeth Blackwell, who, in 1849, became the first woman to graduate from a medical school in the United States, influencing future generations of female physicians[1]. Recent years have seen an exponential growth of women among medical trainees, with women now comprising more than half of medical students in certain countries[2]. Despite the recent increase in the number of female doctors and the recognized value of diversity in medicine, gender disparities in surgery remain pronounced, with women representing fewer than 25% of surgeons, with significant differences among different specialties[3]. This discrepancy is even further emphasized when it comes to academic and leadership roles with female surgeons holding fewer positions at each level as one moves up the surgical ranks, with less than 5% of surgical director positions currently being held by female surgeons[4,5]. Although the participation of female doctors in surgical specialties has increased, their representation in transplantation surgery remains limited, accounting for only 10%-15%, with ethnic minorities being even more underrepresented[6,7]. Over the last couple of decades, several studies have attempted to explain the reasons behind the underrepresentation of females in surgery. Multiple factors may be associated with the persistently low representation of female surgeons in tran
The aim of this study is to identify and map potential gender disparities between transplant surgeons from the per
We conducted a cross-sectional study, in accordance with the Strengthening the Reporting of Observational Studies in Epidemiology guidelines, which was based on the collection of data through two anonymous online questionnaires developed by the research team. We conducted a cross-sectional study, in accordance with the Strengthening the Reporting of Observational Studies in Epidemiology guidelines, addressing two distinct professional groups: (1) Tran
One questionnaire was sent to surgical directors, clinical leads, heads of departments of tran
Two anonymous questionnaires were developed for the aims of this study using the Google Forms platform (Google, Mountain View, CA, United States). The questionnaires were developed de novo by members of the Department of Transplantation Surgery and the Department of Psychology of Aristotle University of Thessaloniki (Avramidou E and Papachristou C) based on existing literature on gender disparities and equity in surgery to ensure conceptual relevance. A pilot test included 4 transplant centers and 3 female transplant surgeons from Greece, evaluating item clarity, completion time, and overall coherence. Minor revisions were made to improve the flow and remove redundant or ambiguous wording. The questionnaires included an initial question of declaration of participants’ informed consent to participate in this research. The questionnaire for the directors included 8 short open-ended questions regarding the quantitative data about the distribution of various positions across male and female surgeons, particularly the number of male and female surgeons working in the transplantation centers they direct. The questionnaire for the female transplant surgeons included a mix of 23 open-ended and multiple-choice questions. The first 4 questions focused on demographic data of the participants. The following 17 questions included multiple choice questions regarding their work position and their experience and perception of equity in the field of transplant surgery. Perceptions were scored on a 5-point Likert scale ranging from “strongly agree” to “strongly disagree”. The last 2 questions were open-ended questions about their experience as female surgeons and suggestions on improving gender equity in transplantation surgery. The full questionnaires’ questions can be found in the Supplementary Tables 1 and 2. The online questionnaires were open from July 2024 to October 2024, when national data from Greece were being collected, and again from February 2025 to August 2025 to gather further responses internationally. The questionnaires were distributed through email communication, newsletters of professional societies and various social media channels. Specifically, for the directors’ questionnaire, transplant centers were identified through publicly available directories of international transplant societies, like European Society for Organ Transplantation (ESOT), and institutional websites. Directors and department leads were contacted directly via email and the survey link was also shared through professional networks. For the female surgeons’ questionnaire, re
Data collection and statistical analysis of the quantitative data were performed using IBM SPSS Statistics, version 31 (IBM Corp., Armonk, NY, United States). Descriptive statistics were performed on the demographic data and the answers to the close-ended questions of the questionnaire. Categorical data were presented as absolute frequencies and percentages. Differences between categorical variables were tested using Fisher’s exact test or χ2 test as appropriate. P value ≤ 0.05 (2-tailed) was considered statistically significant. Data collected from open-ended questions were analyzed according to qualitative research methods. Particularly, Avramidou E performed content analysis of the participants statements and their meanings, symbolic qualities, and expressive content in line with Krippendorff’s content analysis principles[11-15]. Initially, all responses were read thoroughly to obtain a general sense of the content. After this process, they were divided into meaning units, consisting of single words or parts of sentences. These meaning units were formulated into categories and sub-categories. Through a holistic analysis of the content within each category, the latent meaning in each passage was interpreted and illustrated by themes. The coding was performed by the first author, so no interrater reliability is available. Nevertheless, the coding and the themes emerged were discussed and reflected upon with a second person in
Results of the analysis of directors’ questionnaire responses: A total of 46 transplant surgery directors responded to the anonymous questionnaire. Most of the respondents were directors of European transplant centers (65.2%). Based on their responses a total of 381 transplant surgeons are employed in these centers in consultant/attending positions, 102 of which are female [27%, 95% confidence interval (CI): 22.3%-31.2%]. Regarding academic participation of female transplant surgeons, 38.9% (95%CI: 32.3%-45.5%) of academic fellow positions and 24.3% (95%CI: 17.9%-30.7%) of professor positions are hold by female surgeons. Descriptive analysis with Fisher-Freeman-Halton test was performed and showed that while the distribution of female surgeons, PhD candidates and academic fellow positions did not vary significantly across continents (simulated P > 0.05), the female professor distribution varied significantly (P = 0.009). After Bonferroni correction (α = 0.0083), the only statistically significant difference was found to be between Europe and North America, with North America presenting a statistically significantly higher percentage of female professors (34.9%). Table 1 presents the analytic distribution of transplant surgery positions among female and male surgeons in different countries, based on the responses of sample A, clinic directors.
| Country | Number of transplant surgeons | Number of PhD candidates | Number of academic fellows | Number of professors |
| Europe (n = 30) | Male 196 (72.9); female 73 (27.1) | Male 34 (69.4); female 15 (30.6) | Male 81 (61.4); female 51 (38.6) | Male 60 (84.5); female 11 (15.5) |
| United Kingdom (n = 5) | Male 17 (68); female 8 (32) | Male 2 (100); female 0 (0) | Male 15 (71.4); female 6 (28.6) | Male 5 (100); female 0 (0) |
| Poland (n = 4) | Male 36 (66.7); female 18 (33.3) | Male 10 (62.5); female 6 (37.5) | Male 36 (66.7); female 18 (33.3) | Male 12 (100); female 0 (0) |
| Greece (n = 4) | Male 17 (85); female 3 (15) | Male 1 (75); female 3 (25) | Male 1 (100); female 0 (0) | Male 4 (100); female 0 (0) |
| Belgium (n = 3) | Male 16 (57.1); female 12 (42.9) | Male 2 (66.7); female 1 (33.3) | Male 10 (40); female 15 (60) | Male 10 (62.5); female 6 (37.5) |
| Hungary (n = 3) | Male 15 (83.4); female 3 (16.6) | Male 2 (100); female 0 (0) | Male 0 (0); female 2 (100) | Male 2 (100); female 0 (0) |
| Czech Republic (n = 1) | Male 6 (85.7); female 1 (14.3) | Male 0 (0); female 0 (0) | Male 1 (100); female 0 (0) | Male 1 (100); female 0 (0) |
| Croatia (n = 1) | Male 5 (83.3); female 1 (16.7) | Male 1 (50); female 1 (50) | Male 2 (100); female 0 (0) | Male 2 (100); female 0 (0) |
| Bosnia and Herzegovina (n = 1) | Male 4 (80); female 1 (20) | Male 0 (0); female 1 (100) | Male 3 (75); female 1 (25) | Male 2 (66.7); female 1 (33.3) |
| Estonia (n = 1) | Male 8 (87.5); female 1 (12.5) | Male 2 (100); female 0 (0) | Male 0 (0); female 0 (0) | Male 1 (100); female 0 (0) |
| Finland (n = 1) | Male 6 (54.6); female 5 (45.4) | Male 1 (100); female 0 (0) | Male 0 (0); female 0 (0) | Male 0 (0); female 0 (0) |
| Ireland (n = 1) | Male 6 (85.7); female 1 (14.3) | Male 0 (0); female 0 (0) | Male 1 (100); female 0 (0) | Male 0 (0); female 0 (0) |
| Italy (n = 1) | Male (555.6); female 4 (44.4) | Male 1 (50); female 1 (50) | Male 2 (66.7); female 1 (33.3) | Male 1 (50); female 1 (50) |
| Latvia (n = 1) | Male 5 (83.3); female (116.7) | Male 0 (0); female 0 (0) | Male 3 (75); female 1 (25) | Male 3 (100); female 0 (0) |
| Romania (n = 1) | Male 38 (95); female 2 (5) | Male 10 (100); female 0 (0) | Male 6 (60); female 4 (40) | Male 13 (86.7); female 2 (13.3) |
| Spain (n = 1) | Male 3 (50); female 3 (50) | Male 0 (0); female 0 (0) | Male 1 (50); female 1 (50) | Male 1 (50); female 1 (50) |
| Sweden (n = 1) | Male 9 (50); female 9 (50) | Male 2 (50); female 2 (50) | Male 0 (0); female 2 (100) | Male 3 (100); female 0 (0) |
| North America (n = 10) | Male 60 (70.6); female 25 (29.4) | Male 0 (0); female 1 (100) | Male 28 (65.7); female 16 (36.3) | Male 56 (65.2); female 30 (34.8) |
| United States (n = 9) | Male 57 (70.4); female 24 (29.6) | Male 0 (0); female 1 (100) | Male 24 (60); female 16 (40) | Male 53 (64.7); female 29 (35.3) |
| Canada (n = 1) | Male 3 (75); female 1 (25) | Male 0 (0); female 0 (0) | Male 4 (100); female 0 (0) | Male 3 (75); female 1 (25) |
| Oceania (n = 1) | Male 3 (75); female 1 (25) | Male 0 (0); female 0 (0) | Male 0 (0); female 0 (0) | Male 0 (0); female 0 (0) |
| New Zeeland (n = 1) | Male 3 (75); female 1 (25) | Male 0 (0); female 0 (0) | Male 0 (0); female 0 (0) | Male 0 (0); female 0 (0) |
| Asia (n = 4) | Male 16 (87.5); female 2 (12.5) | Male 1 (100); female 0 (0) | Male 5 (71.4); female 2 (28.6) | Male 11 (100); female 0 (0) |
| India (n = 2) | Male 8 (87.5); female 1 (12.5) | Male 1 (100); female 0 (0) | Male 1 (50); female 1 (50) | Male 8 (100); female 0 (0) |
| Pakistan (n = 1) | Male 3 (100); female 0 (0) | Male 0 (0); female 0 (0) | Male 4 (80); female 1 (20) | Male 3 (100); female 0 (0) |
| United Arab Emirates (n = 1) | Male 5 (83.3); female 1 (16.7) | Male 0 (0); female 0 (0) | Male 0 (0); female 0 (0) | Male 0 (0); female 0 (0) |
| Africa (n = 1) | Male 4 (80); female 1 (20) | Male 1 (100); female 0 (0) | Male 13 (52); female 12 (48) | Male 4 (80); female 1 (20) |
| South Africa (n = 1) | Male 4 (80); female 1 (20) | Male 1 (100); female 0 (0) | Male 13 (52); female 12 (48) | Male 4 (80); female 1 (20) |
Results of the analysis of female surgeons’ questionnaire responses: A total of 75 female transplant surgeons responded to the anonymous questionnaire. The respondents had a mean age of 43.7 ± 8.8 years (24-70), with most of them working in European transplant centers (65.3%) and self-identifying as White/Caucasian (76%). Table 2 presents the demographic data of respondents. Regarding their marital status, 68% are in a relationship or married and 38.6% have children, 58.9% of female surgeons with children stated that they received sufficient support for maternity leave and return-to-work transitions from their hospitals or institutions, 80% of the respondents perceive that balancing family responsibilities and professional commitments is more challenging for them compared to their male colleagues.
| Characteristics | Responses n (%) |
| Age | |
| < 30 | 2 (2.6) |
| 30-40 | 26 (34.6) |
| 41-50 | 32 (42.6) |
| 51-65 | 13 (17.3) |
| 66+ | 2 (2.6) |
| Continent | |
| Africa | 1 (1.3) |
| Asia | 4 |
| Europe | 49 |
| North America | 11 |
| Oceania | 5 |
| South America | 4 |
| NA | 1 (1.3) |
| Ethnicity | |
| White/Caucasian | 57 (76) |
| Asian | 7 (9.3) |
| Hispanic or Latino | 5 (6.6) |
| Black or African American | 2 (2.6) |
| Middle Eastern | 1 (1.3) |
| Mixed | 1 (1.3) |
| Other | 1 (1.3) |
| NA | 1 (1.3) |
| Marital status | |
| In a relationship or married | 27 (36) |
| In a relationship or married with children | 24 (32) |
| Single | 16 (21.3) |
| Single with children | 5 (6.7) |
| NA | 3 (4) |
| Doctor grade | |
| Attending/consultant | 59 (78.6) |
| Fellowship trainee | 9 (12) |
| Medical director | 6 (8) |
| NA | 1 (1.3) |
| Academic position | |
| Academic Fellow | 7 (9.3) |
| Research Fellow | 7 (9.3) |
| Assistant Professor | 9 (12) |
| Associate Professor | 7 (9.3) |
| Full Professor | 1 (1.3) |
| No academic position | 40 (53.3) |
| NA | 4 (5.3) |
About 48% (95%CI: 36.7%-59.3%) of the respondents either hold a PhD (32%) or they are PhD candidates (16%). In total 41.3% hold an academic position, with 54.8% of them being professors (assistant, associate or full), 22.6% of the res
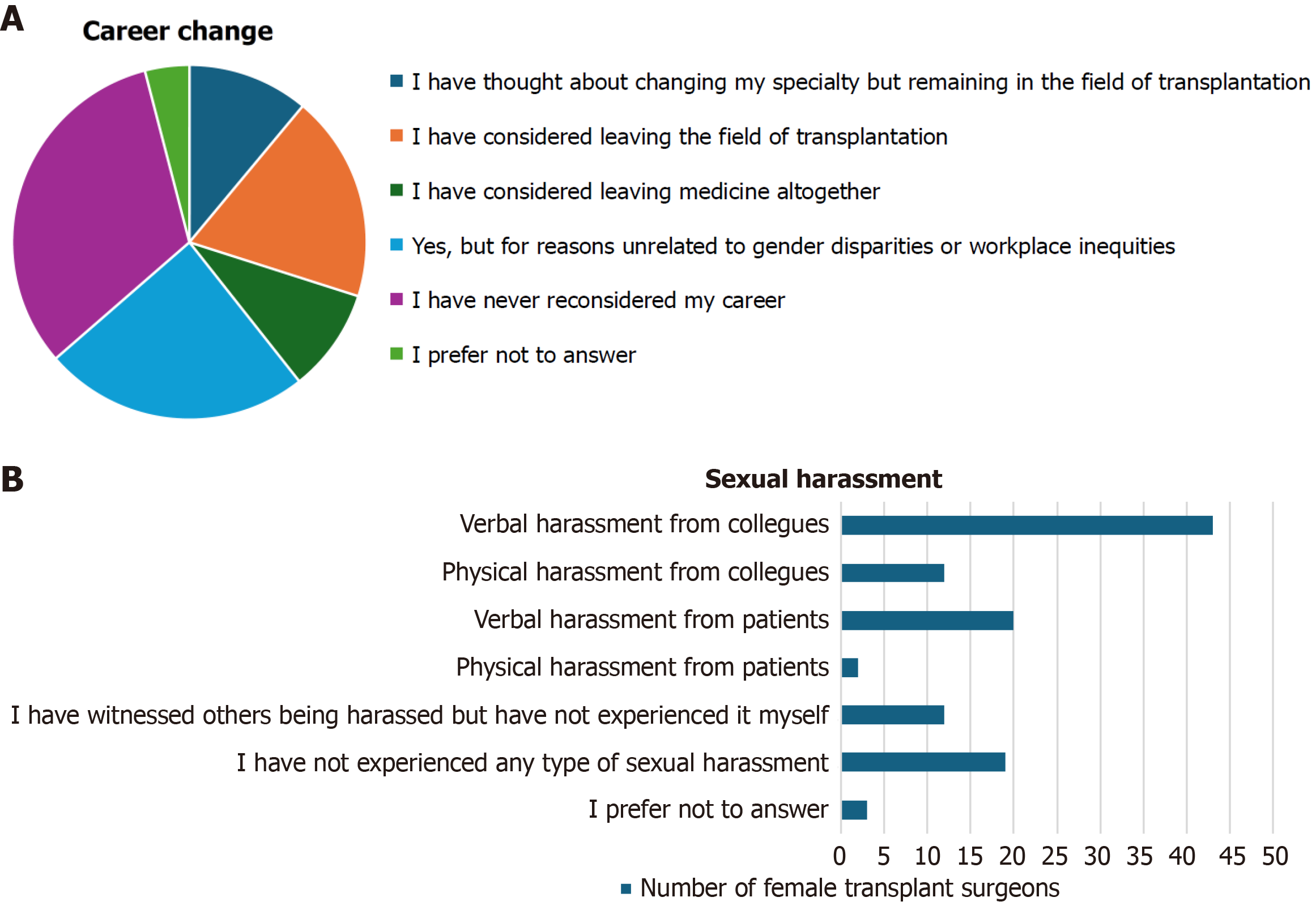
Gender discrimination was the most frequent form of discrimination female transplant surgeons have experienced (72%, 95%CI: 61.9%-82.2%) followed by country-of-origin discrimination (14.6%, 95%CI: 6.7%-22.7%). There was no statistically significant association between country and reported discrimination according to Fisher-Freeman-Halton exact test (P = 0.063) and binary logistic regression (P = 0.565). Compared with Europe, neither the United States (P = 0.999) nor other regions (P = 0.286) showed significantly different odds of reporting discrimination. Additionally, 58.6% (95%CI: 47.5%-69.8%) report sexual harassment incidents, including verbal and physical harassment, most commonly by colleagues (57.3%), but also by patients (25.3%). The frequency of these incidents’ ranges, with 40% of the responses stating that they occur occasionally (a few times a year).
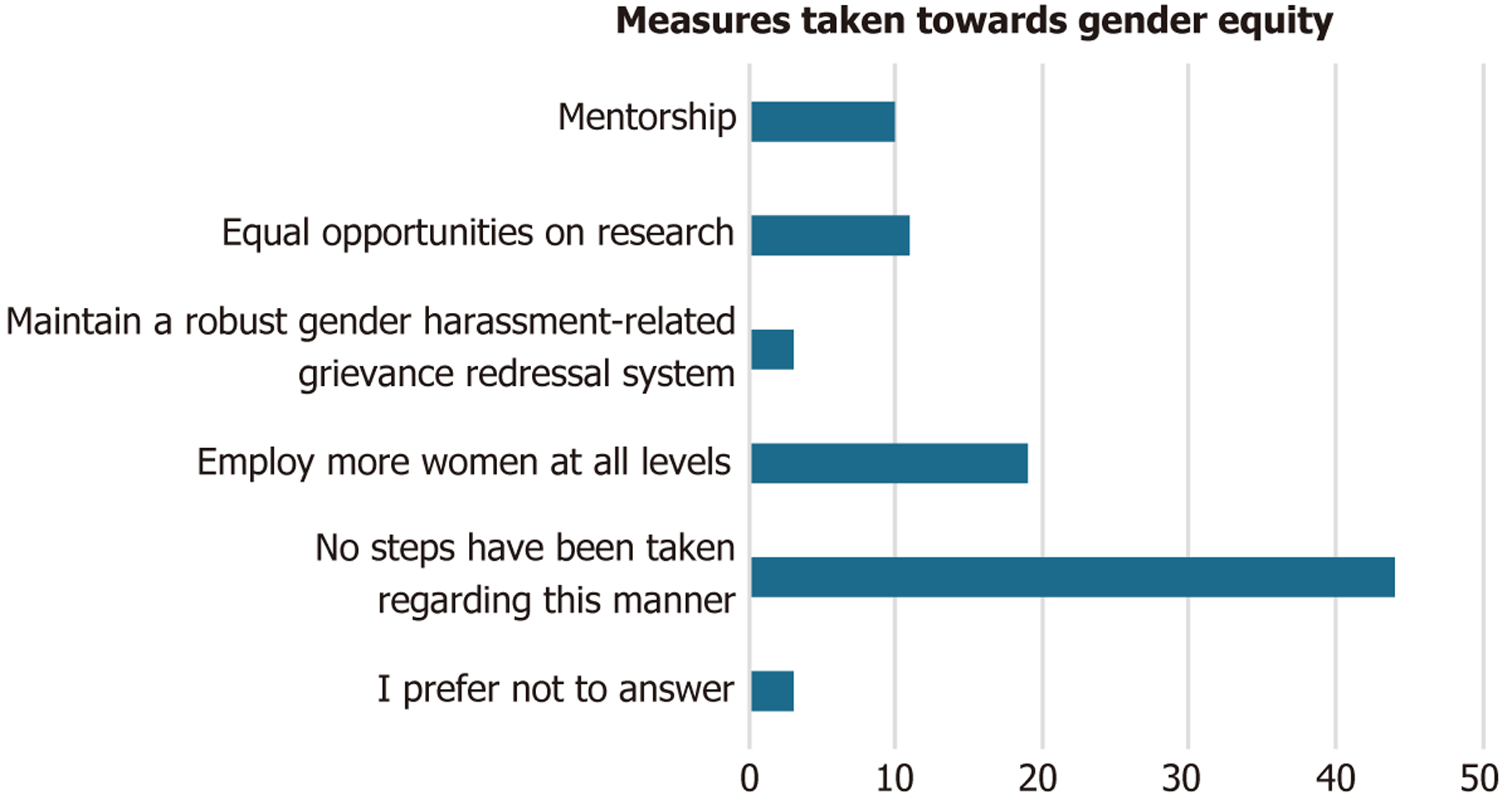
Lastly, 41.3% (95%CI: 30.2%-52.5%) declare not being satisfied regarding their work-life balance and 64% (95%CI: 53.1%-74.9%) would consider changing their career. According to female transplant surgeons, 58.7% (95%CI: 47.5%-69.8%) of the hospitals they are working in have not taken any steps regarding gender equity, 24% (95%CI: 14.3%-33.7%) have employed more female surgeons, 14.7% (95%CI: 6.7%-22.7%) provide equal research opportunities and 13.3% (95%CI: 5.6%-21%) provide mentorship. Figures 2 and 3 and Supplementary Figures 1-8 demonstrate the analytic res
Challenges that female surgeons have faced in the transplant surgery field: Analysis of the responses revealed several recurring challenges faced by females in transplantation surgery. A prominent theme according to Krippendorff’s content analysis was the systemic gender inequities female surgeons face. Particularly, gender bias reports such as “expecting a male surgeon” were frequently mentioned alongside other professional barriers like “operation room time limitations” or “not being considered for advanced cases”.
Work-life balance emerged as another major challenge and theme on content analysis, with female surgeons reporting obstacles on family planning such as “stopping (for) a while (due to) pregnancy” and lack of support from their institu
Barriers to career progression and leadership was another highlighted theme, with respondents mentioning that “men (were) promoted above female surgeons” and that “guy colleague got promoted because he ‘looks’ like a consultant”. Lastly, based on respondents’ reports, psychological and emotional toll of gender bias was another theme extracted from content analysis. Specifically, answers underscore feelings of isolation, impostor syndrome, and frustration, with female surgeons mentioning that their most significant challenge was “working in an extremely toxic male environment” or “Being under the leadership of a bully”. Figure 4 includes all the categories and themes extracted from the collected an
Suggestions for the achievement of professional equality in transplantation surgery: Analysis of open-ended responses identified three themes based on Krippendorff’s analysis of recommendations proposed by participants. The importance of mentorship, representation, and role models was one of the most emphasized areas of suggested improvement, with 31.5% of the recommendations addressing this theme. Particularly, suggestions under this theme involved increase in the number of female medical students interested in surgery (“we need to promote surgery with female medical student and increase female participation”), creation of strong women in surgery networks (“There are more female role models now but need to be more collegiate”) and representation in leadership (“Elect more diverse leadership at the C-suite level for representation reflecting the membership body”).
Respondents also highlighted the need for workforce equity through policy and support systems, with 20% of reco
Need for structural and cultural change in surgery was also frequently implied, with 31.5% of the respondents calling for mandatory training on gender bias, improved communication and transparency, and leadership models that prioritize quality of care and staff wellbeing. Representative statements included “mandatory training on gender bias”, “less prototypes, leaders with modern visions, leaders wanting to achieve quality not quantity (including healthy employees), transparency in training, transparent communication” and that surgeons should be “judged based on their skill”.
About 17% of the respondents did not suggested any measures towards gender equity and for this reason their responses were not included in the content analysis. The list of categories and themes extracted based on Krippendorff’s framework for content analysis can be found in Figure 5.
Transplantation surgery is a unique field combining research with manual skills for the treatment of complex patients. Nowadays, in many countries worldwide, the number of medical students and surgery trainees interested in this field is declining, a phenomenon closely associated with challenges in the achievement of work-life balance[14]. Despite medicine and surgery becoming more inclusive, these trends are not observed in the transplant surgery workforce[16].
Particularly, as expected, our study found disparities in the proportion of female transplant surgeons based on the quantitative data provided by transplant surgery directors. Our findings support the existing literature where it is reported that the percentage of female surgeons ranges from 12% in the United States to 28% in Italy[10,16,17]. Data from our survey demonstrate an international percentage of 28.2% participation, with female surgeons holding more positions in the United States and European countries like Poland and United Kingdom. Females remain significantly underrepresented in leadership positions within transplant surgery, with studies showing low percentages of female directors and presidents in transplant societies[16,18,19]. Specifically, American Society of Transplant Surgeons had only 4 female presidents, while it is notable that in ESOT since its foundation in 1982, there has only been one female president, Carla Baan[17,18]. Our study also highlights that despite the significant proportion of the respondents that aspire to hold a leadership position (53.3%), many of them perceive substantial barriers to career advancement.
Female surgeons frequently experience gender discrimination, which is also reflected in patient preferences, biased attitudes from colleagues, unequal opportunities, and professional barriers to career advancement[19]. The data in our study illustrate this phenomenon by presenting that 72% of the respondents have experienced some type of gender discrimination, that can range from microaggressions, lack of trust, pay inequities, fewer academic opportunities, and even sexual harassment. Specifically for sexual harassment[20], various studies have investigated such incidents across female surgeons with reported behaviors including inappropriate physical contact, sexualized comments centered on dressing or physical appearance, suggestive winking and smiling at female trainees etc.[21-25]. Our study suggest that sexual harassment was frequently reported, with 58.6% of the respondents indicating that they had experienced it at least once during their career, with another interesting observation being that the source of harassment were both colleagues and patients, a phenomenon reflecting societal beliefs.
Balancing family and a surgical career present significant challenges for female surgeons. The demographic profile of female surgeons that participated in our study showed that a significant proportion of them are in a relationship or married (68%), while 38.6% also have children. Despite the increased percentage of surgeons with children, 80% of the respondents reported that they find more challenging balancing family responsibilities with their careers compared to their male colleagues. Existing literature reports that female surgeons across various specialties during their early-career stage are likely to postpone marriage and family planning, considering it a career barrier, while surgeons who are also mothers experience more frequently disapproval and are given limited opportunities[26,27].
Despite many actions that need to be taken towards gender equity, a notable fraction of the respondents in our study answered that their hospitals/institutions have not taken any measures towards this direction. Mentorship is one of the most frequent recommendations derived from our study, with existing literature also reporting higher career satisfaction among surgeons who received mentorship, particularly from female surgeons[28-30]. Representation is also crucial, particularly in academic settings and leadership positions[31]. The presence of female surgical role models may play a pivotal role in encouraging female medical students to not only enter the field of surgery but also to take on higher academic roles in this field. Additionally, networking events, organizations dedicated to female in surgery initiatives and social media platforms enable the opportunity to promote achievements of female transplant surgeons while engaging new members to enter the field of transplant surgery. Lastly, legislation should ensure fairness in the hiring process as well as an anonymous reporting system in a hospital setting.
The present study provides the first international, descriptive snapshot of gender representation, professional experiences, and perceived inequities among transplant surgeons. By integrating perspectives from both transplant unit directors and female surgeons across multiple regions, this study offers preliminary, hypothesis-generating insights into the structural and cultural barriers faced by female transplant surgeons and highlights opportunities for institutional reform. Apart from the documentation of disparities, this work provides a foundation for future multicenter studies that can more rigorously evaluate gender dynamics in surgical training, academic advancement, and leadership within tran
The main strength of our study is that it was conducted among surgeons practicing in different countries and work settings. Despite its strengths, this study presents certain limitations. Firstly, due to the methodological setting of a questionnaire-based study, a potential limitation of this study is the risk of self-selection and response bias. Given the voluntary nature of this study, it is possible that surgeons with a particular interest in gender equity or with stronger personal experiences of discrimination were more likely to participate, potentially over-representing these perspectives.
An additional limitation of this study is the reliance on self-reported data from transplant directors regarding the gender distribution of surgeons and academic positions within their centers. This approach may be subject to recall or reporting bias, as responses were based on individual recollection rather than verified institutional records. Future studies would benefit from extracting official workforce data based on registries. Self-reported data are inherently subject to recall bias regarding answers of female transplant surgeons as well.
Even though the design was guided by existing literature on gender disparities in surgery and reviewed by multi
Our study’s small analytic samples respondents from Asia (4 transplant surgery directors participants and 4 female surgeons respondents), from Africa (1 transplant surgery director participant and 1 female surgeon respondent), from Oceania (1 transplant surgery director participant and 5 female surgeons respondents) and from South America (no transplant surgery director participant and 4 female surgeons respondents) were probably not representative of the actual gender composition of the leadership in these regions, neither the perceptions of female surgeons working there. For this reason, results may not be generalizable to all settings. Future investigations should focus on underrepresented areas as well as participation of surgeons during training. Additionally, a limitation of this study is the absence of defined deno
Lastly, a key limitation of this study is the absence of comparative data from male transplant surgeons. For this reason, it is not possible to determine whether the reported experiences related to work-life balance, career satisfaction, and hara
Our study is the first international study attempting to map the gender distribution of surgeons employed in transplants centers through reports of transplant clinic directors and to capture the perceptions of female transplant surgeons. The findings of this study should be interpreted as exploratory and descriptive, providing preliminary insights into gender inequities, persistent challenges and limitations female transplant surgeons face within the international transplant surgery workforce. Female transplant surgeons are based on our results systematically underrepresented compared to their male colleagues, and report perceived discrimination related to gender. The frequent reports of sexual harassment experienced by female surgeons, perpetrated by both male colleagues and patients, are particularly concerning and may point to persistent gender biases within professional and societal norms. The above suggests that professional associations, organizations, national and international legislations should focus on gender equity, inclusion and fairness in the field of transplantation surgery by taking measures in education, training and the working field as well as structural and cultural changes in this field. This study offers a valuable snapshot of current perceptions and experiences among transplant surgeons from multiple countries. Importantly, it establishes a foundation and reporting framework that future, larger, and more representative studies can build upon to further investigate gender equity in transplantation sur
| 1. | Ellis H. Elizabeth Blackwell: a pioneer female medical graduate. Br J Hosp Med (Lond). 2010;71:281. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 2. | Association of American Medical Colleges. New AAMC data show rising diversity in medical schools. Dec 12, 2023. [cited 25 January 2025]. Available from: https://www.aamc.org/news/press-releases/new-aamc-data-diversity-medical-school-enrollment-2023. |
| 3. | Association of American Medical Colleges. Diversity in Medicine: Facts and Figures 2019. [cited 25 January 2025]. Available from: https://www.aamc.org/data-reports/workforce/report/diversity-medicine-facts-and-figures-2019. |
| 4. | Columbus AB, Lu PW, Hill SS, Fields AC, Davids JS, Melnitchouk N. Factors Associated With the Professional Success of Female Surgical Department Chairs: A Qualitative Study. JAMA Surg. 2020;155:1028-1033. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 37] [Article Influence: 7.4] [Reference Citation Analysis (0)] |
| 5. | Seemann NM, Webster F, Holden HA, Moulton CA, Baxter N, Desjardins C, Cil T. Women in academic surgery: why is the playing field still not level? Am J Surg. 2016;211:343-349. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 110] [Cited by in RCA: 131] [Article Influence: 11.9] [Reference Citation Analysis (0)] |
| 6. | Valbuena VSM, Obayemi JE, Purnell TS, Scantlebury VP, Olthoff KM, Martins PN, Higgins RS, Blackstock DM, Dick AAS, Watkins AC, Englesbe MJ, Simpson DC. Gender and racial disparities in the transplant surgery workforce. Curr Opin Organ Transplant. 2021;26:560-566. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 31] [Article Influence: 6.2] [Reference Citation Analysis (0)] |
| 7. | Castillo N, Betterbed D, Martin S, Acosta E, Ortiz AC, Petrera P, Koizumi N, Ortiz J. Abdominal Transplant Surgeons: The Lack of Female Surgeons and People From Underrepresented Racial and Ethnic Minority Groups in Academic and Clinical Leadership. Exp Clin Transplant. 2024;22:258-266. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 8. | Schneidman J, Rice K, Armstrong N. Women in surgery: The social construction of gender in surgical practice. Am J Surg. 2025;247:116343. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 4] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 9. | Franchi E, Parini S, Capelli G, Perali C, Lombardi I, Amoroso A, Feltrin G, Gringeri E, Maggiore U, Amarelli C, Ferraresso M, Biancofiore G, Gruttadauria S, Cardillo M, Boggi U, Spolverato G. Women in Transplant Surgery in Italy. Transplantation. 2023;107:793-796. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 10. | Pengel LHM, Kaisar M, Benjamens S, Ibrahim M, Ricci V, Bellini MI, Breithaupt-Faloppa AC, Falk C, Maple H, Marson L, Ortiz F, Papalois V, Paredes D, Forsberg A. Equity, Diversity and Inclusion (EDI) in Organ Transplantation: An ESOT Survey About EDI Within ESOT as an Organization and its Educational Activities, and Transplantation Research and Science. Transpl Int. 2023;36:11331. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (1)] |
| 11. | Krippendorff K. Content Analysis: An Introduction to Its Methodology. 2nd ed. Thousand Oaks, CA: Sage Publications, 2003. |
| 12. | Verran D. On achieving gender equity within the liver transplantation medical and surgical workforce. Front Transplant. 2024;3:1396631. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 13. | Vaismoradi M, Turunen H, Bondas T. Content analysis and thematic analysis: Implications for conducting a qualitative descriptive study. Nurs Health Sci. 2013;15:398-405. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3303] [Cited by in RCA: 3828] [Article Influence: 294.5] [Reference Citation Analysis (0)] |
| 14. | Quillin RC 3rd, Cortez AR, Dageforde LA, Watkins A, Collins KM, Garonzik-Wang J, Glorioso JM, Tevar AD, Emond JC, Segev DL. Transplant Surgery Pipeline: A Report from the American Society of Transplant Surgeons Pipeline Taskforce. J Am Coll Surg. 2021;233:262-271. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 26] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 15. | Linscheid LJ, Holliday EB, Ahmed A, Somerson JS, Hanson S, Jagsi R, Deville C Jr. Women in academic surgery over the last four decades. PLoS One. 2020;15:e0243308. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 22] [Cited by in RCA: 80] [Article Influence: 13.3] [Reference Citation Analysis (0)] |
| 16. | Kaldas FM, Rocca JP, Bhati CS, Duan N, Evenson AR, Tan HP, Redfield RR, di Sabato DM, Yoshida A, Abt PL, Geevarghese SK. The Abdominal Transplant Surgery Workforce: Current state and future trends. Clin Transplant. 2019;33:e13659. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 31] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 17. | American Society of Transplant Surgeons. ASTS Past Presidents & Presidential Addresses. [cited 10 September 2025]. Available from: https://www.asts.org/about-asts/past-president-and-presidential-addresses. |
| 18. | The European Society for Organ Transplantation. Presidents. [cited 10 September 2025]. Available from: https://esot.org/about-us/presidents/. |
| 19. | Lim WH, Wong C, Jain SR, Ng CH, Tai CH, Devi MK, Samarasekera DD, Iyer SG, Chong CS. The unspoken reality of gender bias in surgery: A qualitative systematic review. PLoS One. 2021;16:e0246420. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 124] [Cited by in RCA: 101] [Article Influence: 20.2] [Reference Citation Analysis (0)] |
| 20. | Hinze SW. 'Am I being over-sensitive?' Women's experience of sexual harassment during medical training. Health (London). 2004;8:101-127. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 58] [Cited by in RCA: 51] [Article Influence: 5.1] [Reference Citation Analysis (0)] |
| 21. | Myers SP, Hill KA, Nicholson KJ, Neal MD, Hamm ME, Switzer GE, Hausmann LRM, Hamad GG, Rosengart MR, Littleton EB. A qualitative study of gender differences in the experiences of general surgery trainees. J Surg Res. 2018;228:127-134. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 67] [Article Influence: 8.4] [Reference Citation Analysis (0)] |
| 22. | Barnes KL, McGuire L, Dunivan G, Sussman AL, McKee R. Gender Bias Experiences of Female Surgical Trainees. J Surg Educ. 2019;76:e1-e14. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 92] [Cited by in RCA: 141] [Article Influence: 20.1] [Reference Citation Analysis (0)] |
| 23. | Bernardi K, Shah P, Lyons NB, Olavarria OA, Alawadi ZM, Leal IM, Holihan JL, Bass BL, Jakey CE, Kao LS, Ko TC, Kuo PC, Loor MM, Zheng F, Liang MK. Perceptions on gender disparity in surgery and surgical leadership: A multicenter mixed methods study. Surgery. 2020;167:743-750. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 52] [Article Influence: 8.7] [Reference Citation Analysis (0)] |
| 24. | Hill E, Solomon Y, Dornan T, Stalmeijer R. 'You become a man in a man's world': is there discursive space for women in surgery? Med Educ. 2015;49:1207-1218. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 48] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 25. | Brown JB, Fluit M, Lent B, Herbert C. Surgical culture in transition: gender matters and generation counts. Can J Surg. 2013;56:153-158. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 37] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 26. | Cochran A, Hauschild T, Elder WB, Neumayer LA, Brasel KJ, Crandall ML. Perceived gender-based barriers to careers in academic surgery. Am J Surg. 2013;206:263-268. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 185] [Cited by in RCA: 233] [Article Influence: 17.9] [Reference Citation Analysis (0)] |
| 27. | Hutchison K. Four types of gender bias affecting women surgeons and their cumulative impact. J Med Ethics. 2020;46:236-241. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 45] [Cited by in RCA: 46] [Article Influence: 7.7] [Reference Citation Analysis (0)] |
| 28. | Kaderli R, Muff B, Stefenelli U, Businger A. Female surgeons' mentoring experiences and success in an academic career in Switzerland. Swiss Med Wkly. 2011;141:w13233. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 12] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 29. | Faucett EA, McCrary HC, Milinic T, Hassanzadeh T, Roward SG, Neumayer LA. The role of same-sex mentorship and organizational support in encouraging women to pursue surgery. Am J Surg. 2017;214:640-644. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 58] [Cited by in RCA: 93] [Article Influence: 10.3] [Reference Citation Analysis (0)] |
| 30. | Dwyer KM, Clark CJ, MacDonald K, Paraskeva MA, Rogers N, Ryan J, Webster AC, Wong G. Gender Equity in Transplantation: A Report from the Women in Transplantation Workshop of The Transplantation Society of Australia and New Zealand. Transplantation. 2017;101:2266-2270. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 20] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 31. | Riner AN, Herremans KM, Neal DW, Johnson-Mann C, Hughes SJ, McGuire KP, Upchurch GR Jr, Trevino JG. Diversification of Academic Surgery, Its Leadership, and the Importance of Intersectionality. JAMA Surg. 2021;156:748-756. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 74] [Article Influence: 14.8] [Reference Citation Analysis (0)] |