Published online Jul 20, 2021. doi: 10.5662/wjm.v11.i4.187
Peer-review started: December 25, 2020
First decision: May 6, 2021
Revised: May 9, 2021
Accepted: May 20, 2021
Article in press: May 20, 2021
Published online: July 20, 2021
Processing time: 205 Days and 13.4 Hours
Cardiorenal syndrome (CRS) type 1 is the development of acute kidney injury in patients with acute decompensated heart failure. CRS often results in prolonged hospitalization, a higher rate of rehospitalization, high morbidity, and high mortality. The pathophysiology of CRS is complex and involves hemodynamic changes, neurohormonal activation, hypothalamic-pituitary stress reaction, inflammation, and infection. However, there is limited evidence or guideline in managing CRS type 1, and the established therapeutic strategies mainly target the symptomatic relief of heart failure. This review will discuss the strategies in the management of CRS type 1. Six clinical studies have been included in this review that include different treatment strategies such as nesiritide, dopamine, levosimendan, tolvaptan, dobutamine, and ultrafiltration. Treatment strategies for CRS type 1 are derived based on the current literature. Early recognition and treatment of CRS can improve the outcomes of the patients significantly.
Core Tip: Cardiorenal syndrome (CRS) type 1 is defined as the development of acute kidney injury or worsening renal function in patients with acute decompensated heart failure. Impaired renal function in acute decompensated heart failure is often associated with prolonged hospitalization, a higher rate of rehospitalization, high morbidity, and high mortality. The aim of this paper is to discuss the different treatment strategies and provide a guideline for the management of CRS type 1. Early recognition and treat
- Citation: Ong LT. Evidence based review of management of cardiorenal syndrome type 1. World J Methodol 2021; 11(4): 187-198
- URL: https://www.wjgnet.com/2222-0682/full/v11/i4/187.htm
- DOI: https://dx.doi.org/10.5662/wjm.v11.i4.187
Cardiorenal syndrome (CRS) type 1 is defined as the development of acute kidney injury or worsening renal function in patients with acute decompensated heart failure (HF)[1]. Acute CRS occurs in approximately 25% to 33% of patients admitted with acute decompensated HF[1]. CRS has been associated with adverse outcomes, increased risk of hospitalization, and death[2]. Impaired renal function is a stronger predictor of mortality compared to left ventricular ejection fraction or New York Heart Association class[3]. Besides that, the development of renal dysfunction in HF patients may worsen the preexisting HF[4].
The causes of CRS in hospitalized patients include venous renal congestion due to hemodynamic changes, neurohormonal activation, hypothalamic-pituitary stress reaction, inflammation, and infection[1]. Moreover, administration of intravenous diuretics in patients with acute decompensated failure may lead to worsening renal function[5]. The common underlying risk factors of developing CRS in the setting of acute decompensated HF include severe atherosclerotic disease, hypertension, diabetes mellitus, elderly age, and a history of renal insufficiency or HF[6]. Further
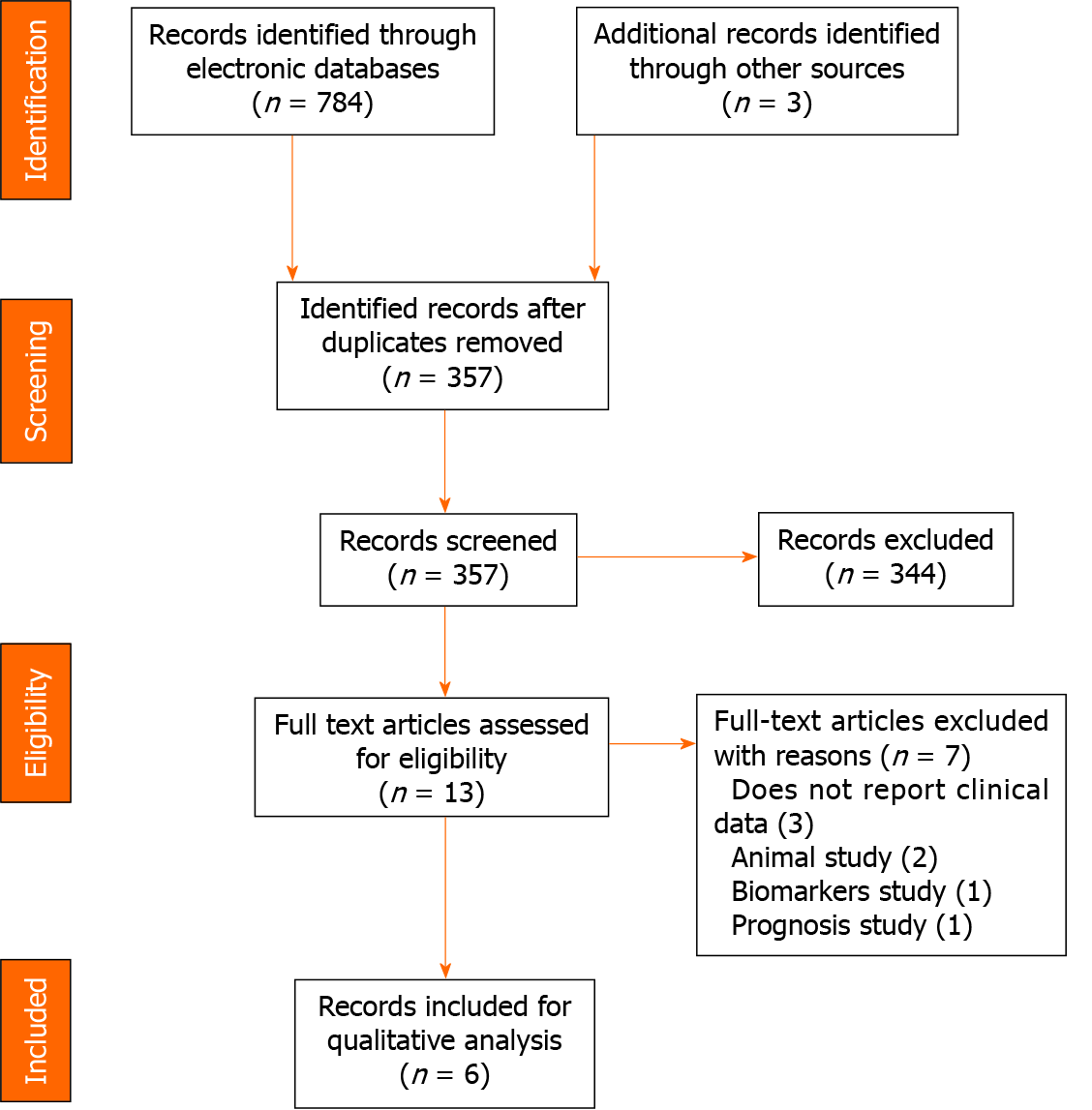
A systematic search was conducted using the two major electronic medical literature databases, PubMed and ScienceDirect. Search terms included the following keywords and word combinations: “cardiorenal syndrome type 1”, “heart failure”, “kidney injury”, and “renal failure”. Relevant articles published in English from 2005 to 2010 were identified. Additional articles of interest were retrieved from the reference list of selected papers. Review articles and case reports were excluded from this review. PRISMA guidelines were used as a basis for reporting the results of this systematic review.
The inclusion criteria for this review were randomized control trials and observational studies that investigated the efficacy of different therapeutic options for CRS and reported at least one biochemical datum. The exclusion criteria include studies on biochemical markers of CRS, prognosis studies, and prevalence studies. Review articles and case reports were also excluded. The outcomes used in this study were changes in renal function tests such as creatinine levels, glomerular filtration rate (GFR), blood urea nitrogen, cystatin C, urine output, and weight. The flow diagram of the study selection process is shown in Figure 1.
The main characteristics of the studies included in this review are shown in Table 1.
| Ref. | Population | Sample size | Intervention | Duration of follow-up | Main findings |
| Owan et al[10], 2008 | ADHF with renal dysfunction | 72 | Standard therapy vs standard therapy plus nesiritide (bolus of 0.2 mcg/kg followed by 0.01 mcg/kg per min) | 72 h | Nesiritide produced greater reduction in blood pressure and preserved renal function |
| Bart et al[11], 2012 | ADHF with worsened renal function | 188 | Ultrafiltration therapy vs stepped pharmacologic therapy (intravenous diuretics) | 96 h | Stepped pharmacologic-therapy with intravenous diuretics was superior to ultrafiltration |
| Fedele et al[12], 2014 | ADHF and renal impairment | 21 | Levosimendan (loading dose 6 μg/kg + 0.1 μg/kg per min) for 24 h vs placebo | 72 h | Levosimendan improves the laboratory markers of renal function and renal hemodynamic parameters |
| Chen et al[13], 2013 | AHF and renal dysfunction | 360 | Low dose dopamine (2 μg/kg per min for 72 h) vs low dose nesiritide (0.005 μg/kg per min for 72 h) vs placebo | 72 h | Neither low dose dopamine nor low dose nesiritide improved renal function when added to diuretic therapy |
| Inomata et al[14], 2017 | HF with diuretic resistance and renal impairment | 81 | Additive tolvaptan (≤ 15 mg/d) vs increased furosemide (≤ 40 mg/d) | 7 d | Additive tolvaptan increased urine volume compared with patients receiving an increased dose of furosemide |
| Lannemyr et al[15], 2018 | Chronic HF and impaired renal function | 32 | Levosimendan (loading dose 12 μg/kg + 0.1 μg/kg per min) vs dobutamine (7.5 μg/kg per min) for 75 min | 60 mo and 75 mo after treatment | Levosimendan is the preferred inotropic agent compared to dobutamine |
The study by Owan et al[10] enrolled 35 patients to standard therapy arm and 37 patients to standard therapy plus nesiritide arm. All the patients received standard therapy for HF as determined by the attending cardiologist and standardized diuretic therapy based on renal function. The patient in the nesiritide was administered intravenous nesiritide of a bolus of 0.2 mcg/kg followed by 0.01 mcg/kg per min[10].
The study by Bart et al[11] enrolled 94 patients in each pharmacologic therapy and ultrafiltration arm. Loop diuretics were discontinued in the ultrafiltration arm, and intravenous diuretics were used in pharmacologic therapy. The median duration of the pharmacologic therapy was 92 h (interquartile range, 56 to 138), while the median duration of ultrafiltration was 40 h (interquartile range, 28 to 67)[11].
The study by Fedele et al[12] enrolled 14 patients in levosimendan arm and 7 patients in the placebo arm. The patients in the levosimendan arm received 10 min intravenous loading dose of levosimendan (6 μg/kg) followed by an infusion (0.1 μg/kg per min) for 24 h. All the patients were on other drugs, which included angiotensin-converting enzyme (ACE) inhibitors, angiotensin receptor blockers (ARBs), aldosterone blocking agents (spironolactone), and beta-blockers (bisoprolol or carvedilol). Placebo group patients also received loop diuretics in addition[12].
The study by Chen et al[13] randomized 360 patients to nesiritide strategy and dopamine strategy in a 1:1 allocation ratio. In nesiritide strategy, 119 patients were allocated to low dose nesiritide, while 58 patients were allocated to placebo. In dopamine strategy, 122 patients were allocated to low dose dopamine while 61 patients were allocated to placebo. Patients in the nesiritide strategy were admini
The study by Inomata et al[14] enrolled 40 patients in additive tolvaptan arms and 41 patients in the increased furosemide arm. The mean dose of furosemide received by the patients before the study was 51 ± 25 mg/d, and the patients were also treated with pharmacotherapy such as ACE inhibitors, angiotensin II receptor blockers, β-blockers, and mineral corticoid receptor blockers. The patients were either admini
The study by Lannemyr et al[15] enrolled 16 patients in each levosimendan and dobutamine arm. The patients in the levosimendan arm were given a loading dose of 12 μg/kg given over 10 min, followed by a continuous infusion of 0.1 μg/kg per min for 65 min. The patients in the dobutamine arm were given as a continuous infusion started at 5.0 μg/kg per min for 10 min and thereafter increased to 7.5 μg/kg per min for 65 min[15].
The changes in the clinical parameters of the studies included in this review are shown in Tables 2-7.
| Intervention | Clinical parameters evaluated | ||||||||
| Ref. | Creatinine (mg/dL) | Change in BUN (mg/dL) | Cystatin C (mg/L) | Weight loss (kg) | Cumulative urine volume (mL) | ||||
| Baseline | Mean changes | Baseline | Mean changes | Baseline | Mean changes | Mean changes | |||
| Nesiritide | Owan et al[10], 2008 | 1.85 ± 0.71 | 0.04 ± 0.44 | 44.8 ± 23.3 | -1.3 ± 12.8 | NA | NA | -2.75 ± 3.27 | NA |
| Owan et al[10], 2008 (placebo) | 1.65 ± 0.42 | 0.09 ± 0.25 | 38.3 ± 16.6 | 2.4 ± 6.8 | NA | NA | -4.25 ± 3.42 | NA | |
| Chen et al[13], 2013 | 1.65 | 0.02 | NA | NA | 1.66 | 0.07 | NA | 8574 | |
| Chen et al[13], 2013 (placebo) | 1.70 | 0.02 | NA | NA | 1.86 | 0.11 | NA | 8296 | |
| Intervention | Clinical parameters evaluated | ||||||||||
| Ref. | Creatinine (mg/dL) | Change in BUN (mg/dL) | Cystatin C (mg/L) | Weight loss (kg) | Urine output (mL/d) | ||||||
| Baseline | Mean changes | Baseline | Mean changes | Baseline | Mean changes | Baseline | Mean changes | Baseline | Mean changes | ||
| Furosemide | Inomata et al[14], 2017 | 1.6 | 0.20 ± 0.27 | NA | NA | NA | NA | 61 | -2.1 ± 2.6 | 1251 ± 540 | 79 ± 341 |
| Intervention | Clinical parameters evaluated | ||||||||||
| Ref. | Creatinine (mg/dL) | Change in BUN (mg/dL) | Cystatin C (mg/L) | GFR (mL/min) | Urine output (mL/d) | ||||||
| Baseline | 72 h | Baseline | 72 h | Baseline | 72 h | Baseline | 72 h | Baseline | 72 h | ||
| Levosimendan | Fedele et al[12], 2014 | 1.76 ± 0.37 | 1.51 ± 0.5 | 45.08 ± 22.19 | 33.14 ± 16.63 | 2577.5 ± 700.6 | 2083 ± 731.4 | 38.71 ± 7.94 | 53.34 ± 14.93 | 1766.4 ± 514.2 | 2663.5 ± 721.2 |
| Fedele et al[12], 2014 (placebo) | 1.6 ± 0.2 | 1.7 ± 0.2 | 44.4 ± 13.1 | 47 ± 12.8 | 2498.5 ± 262 | 2470 ± 409.9 | 43.33 ± 7.99 | 40.24 ± 6.58 | 1571.4 ± 125.3 | 1778.51 ± 798.1 | |
| Ref. | Creatinine (mg/dL) | Change in BUN (mg/dL) | RBF (mL/min) | GFR (mL/min) | FF | ||||||
| Baseline | Treatment | Baseline | Treatment | Baseline | Treatment | Baseline | Treatment | Baseline | Treatment | ||
| Inomata et al[14], 2017 | NA | NA | NA | NA | 426 ± 197 | 518 ± 276 | 36.5 ± 18.3 | 44.5 ± 19.0 | 0.146 ± 0.080 | 0.143 ± 0.069 | |
| Intervention | Clinical parameters evaluated | ||||||||||
| Ref. | Creatinine (mg/dL) | Change in BUN (mg/dL) | Cystatin C (mg/L) | Weight loss (kg) | Cumulative urine volume (mL) | ||||||
| Baseline | Mean changes | Baseline | Mean changes | Baseline | Mean changes | Baseline | Mean changes | ||||
| Dopamine/dobutamine | Chen et al[13], 2013 (dopamine) | 1.59 | 0.00 | NA | NA | 1.71 | 0.12 | NA | NA | 8524 | |
| Chen et al[13], 2013 (placebo) | 1.63 | 0.02 | NA | NA | 1.66 | 0.11 | NA | NA | 8296 | ||
| Ref. | Creatinine (mg/dL) | Change in BUN (mg/dL) | RBF (mL/min) | GFR (mL/min) | FF | ||||||
| Baseline | Treatment | Baseline | Treatment | Baseline | Treatment | Baseline | Treatment | Baseline | Treatment | ||
| Lannemyr et al[15], 2018 (dobutamine) | NA | NA | NA | NA | 397 ± 121 | 499 ± 154 | 47.1 ± 14.5 | 47.3 ± 16.9 | 0.193 ± 0.070 | 0.161 ± 0.075 | |
| Intervention | Clinical parameters evaluated | ||||||||||
| Study | Creatinine (mg/dL) | Change in BUN (mg/dL) | Cystatin C (mg/L) | Weight loss (kg) | Urine output (mL/d) | ||||||
| Baseline | Mean changes | Baseline | Mean changes | Baseline | Mean changes | Baseline | Mean changes | Baseline | Mean changes | ||
| Tolvaptan | Inomata et al[14], 2017 | 1.5 | 0.06 ± 0.32 | NA | NA | NA | NA | 62 | -2.1 ± 1.8 | 1306 ± 494 | 459 ± 514 |
| Intervention | Clinical parameters evaluated | |||||||||
| Study | Creatinine (mg/dL) | Change in BUN (mg/dL) | GFR (mL/min per 1.73 m2) | Weight loss (Ib) | Urine output (mL/d) | |||||
| Baseline | Mean changes | Baseline | Mean changes | Mean changes | Baseline | Mean changes | Baseline | Mean changes | ||
| Ultrafiltration | Bart et al[11], 2012 | 2.09 | -0.04 ± 0.53 | 50.5 | 5.68 ± 18.29 | 1.67 ± 10.94 | 234 | 12.1 ± 11.3 | NA | NA |
| Bart et al[11], 2012 (pharmaco-logic therapy) | 1.90 | +0.23 ± 0.70 | 48.7 | 12.54 ± 24.81 | 0.93 ± 14.60 | 207 | 12.6 ± 8.5 | NA | NA | |
The study by Owan et al[10] showed that nesiritide patients had less increase in creatinine and blood urea nitrogen compared to patients on standard therapy. The cumulative weight loss was greater in patients on standard therapy than in nesiritide patients, however, the difference was not significant[10].
In the study by Bart et al[11], the mean change in the serum creatinine level from the baseline was a decrease of 0.04 ± 0.53 mg/dL and an increase of 0.23 ± 0.70 mg/dL in the pharmacologic-therapy group and ultrafiltration, respectively. There was no significant difference in weight loss in both intervention groups[11].
The study by Fedele et al[12] showed that levosimendan was beneficial, which was confirmed by the decrease in blood urea nitrogen, serum creatinine, and cystatin C. Besides that, levosimendan increased the GFR and urine output significantly com
The study by Chen et al[13] showed that low dose dopamine had no significant effect on cumulative urine volume in 72-h, change in creatinine, and change in cystatin-C compared to placebo. Similarly, low dose nesiritide also had no significant effect on cumulative urine volume in 72-h, change in creatinine, and change in cystatin-C compared to placebo[13].
In the study by Inomata et al[14], the changes in urine volume between baseline in the tolvaptan group were significantly higher compared to the furosemide group. Besides that, the tolvaptan group had a smaller increase in serum creatinine on day 7 from baseline compared to the furosemide group. However, there were no significant changes in body weight in both groups[14].
The study by Lannemyr et al[15] showed that levosimendan and dobutamine had similar increases in renal blood flow. However, the levosimendan group showed an increase in GFR by 22% but remained the same in the dobutamine group. Filtration fraction remained unchanged in levosimendan group but decreased by 17% in the dobutamine group[15].
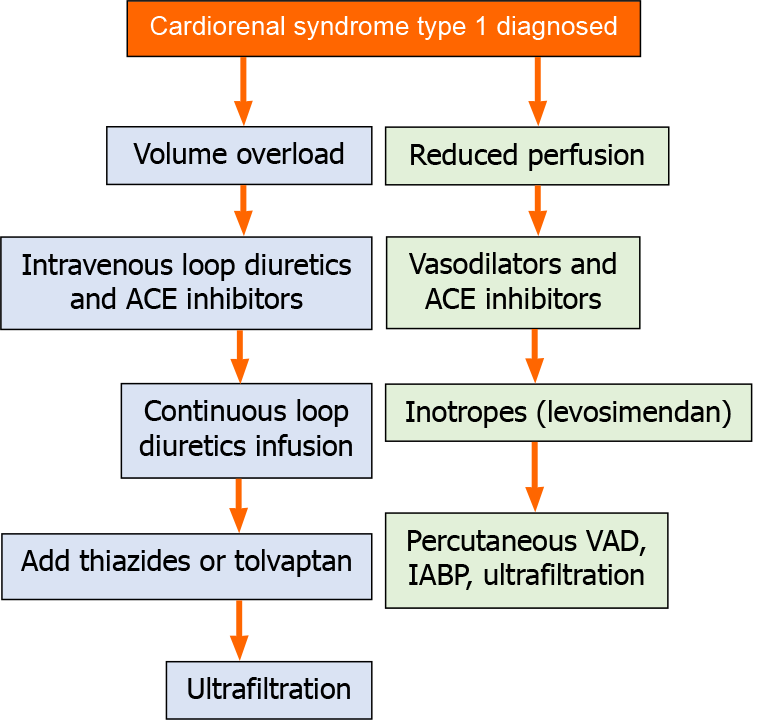
The treatment strategy for CRS type 1 is shown in Figure 2.
Loop diuretics are the primary class of diuretics in the management of acute HF with or without CRS[16]. Loop diuretics lead to natriuresis and volume loss in HF due to the inhibition of Na+K+2Cl- cotransporter in the thick ascending limb of the loop of Henle[16]. Studies suggested that torsemide is a more effective decongestive therapy compared with furosemide in patients with HF because torsemide has more predic
The study by Felker and Mentz[5] suggested that there were no significant diffe
Diuretics use can increase systemic vascular resistance, plasma renin, aldosterone activity, norepinephrine, and arginine vasopressin and indirectly lead to deterioration of left ventricular function[18]. Diuretics use can result in renal dysfunction through the above mechanisms[18]. However, the study by Ahmad et al[18] showed that kidney tubular injury detected by biomarkers in aggressive diuresis of patients with acute HF was not associated with worsening renal function. Furthermore, the study by Mentz et al[19] showed that high-dose loop diuretic therapy did not result in renin-angiotensin-aldosterone system (RAAS) activation greater than that with low-dose diuretic therapy. Ultrafiltration resulted in a greater increase in plasma renin activity compared with stepwise pharmacological care[19].
Loop diuretic resistance in HF can occur due to a decrease in renal perfusion, likely from low cardiac output[20]. Besides that, CKD reduces the excretion of diuretic into the tubular lumen thereby reducing and diminishing the filtered load of sodium[16]. HF can also increase proximal reabsorption of sodium through RAAS activation and increased expression of Na+K+Cl-, which then limits the peak effect of drug delivered to the lumen[21]. However, increased furosemide dose in loop diuretic resistance can cause aggressive fluid removal, which leads to depletion of intravascular volume without refilling from the extravascular space[22]. Moreover, hyperdiuresis can lead to prerenal renal dysfunction due to the potential risk of hypotension[23].
Diuretic resistance can be managed by continuous infusion of furosemide starting at 5 mg/dL to 10 mg/dL followed by an intravenous thiazide diuretic[6]. This combi
Clinical data have shown that RAAS inhibitors can slow CKD progression and are one of the components in managing patients with left ventricular systolic dysfunction in HF[6,16]. However, the use of RAAS inhibitors in acute CRS with underlying renal disease may lead to an increase in serum creatinine levels[16]. The Cooperative North Scandinavian Enalapril Survival Study (CONSENSUS) enrolled patients with severe HF with renal dysfunction with serum creatinine concentrations less than 3.4 mg/dL[25]. The study showed that patients who were in the enalapril arm had a reduction in symptom burden and HF-associated mortality compared to placebo but were associated with doubling the serum creatinine by 11%[25]. Besides that, the subgroup of HF patients with creatinine levels higher than 2 mg/dL showed improvement in symptoms and outcomes when treated with an ACE inhibitor[25].
A post hoc analysis of Study of Left Ventricular Dysfunction (SOLVD) study showed that patients with HF and CKD in the enalapril group had higher mortality benefits even with more advanced stages of CKD[26]. A study by Ahmed et al[27] followed 1165 patients age ≥ 65 years, with systolic HF (ejection fraction < 45%) and CKD (eGFR < 60 mL/min per 1.73 m2) where 1046 received ACE-inhibitors or ARBs for 8 years. The results showed that patients receiving ACE-inhibitors or ARBs had a significant reduction in all-cause mortality and HF hospitalization[27]. Therefore, patients with CRS should be started on the lowest dose of an ACE inhibitor, and the dosage titrated up carefully. Concomitant use of NSAIDs should be avoided to prevent further deterioration of kidney function[6]. ACE-inhibitors or ARB therapy should be continued in patients with CRS unless there is the development of severe renal dysfunction and hyperkalemia[6].
Nesiritide can reduce afterload and increase cardiac output via the coronary, arterial, and venous vasodilatory properties without inotropic effects[16]. The study by O’Connor et al[28] randomized 7141 patients with acute HF to receive either intra
The study by Chen et al[13] showed that patients treated low dose nesiritide did not enhance decongestion or improve renal function. Besides that, the study also showed that low dose dopamine neither improved decongestion nor preserved renal function[13]. However, the findings of the study are contrary to the guidelines for the management of acute HF that suggest the use of low dose dopamine can be considered to improve diuresis and preserve renal function[30]. Observational studies also indicate that the use of nesiritide and dopamine in acute HF is associated with longer length-of-stay, higher mortality, and higher costs[31]. Therefore, use of low dose dopamine or low dose nesiritide as renal adjuvant therapies is not recommended in patients with CRS as it does not provide benefits on renal function, decongestion, and clinical outcome[13].
Levosimendan is a positive inotrope with Ca2+ sensitization that improves the calcium sensitivity of cardiac muscle cells and therefore provides hemodynamic and symptomatic improvement[32]. Besides that, levosimendan has a vasodilatory effect on vasculature via activation of ATP-sensitive K+, voltage-dependent K+, and Ca2+-activated K+ channels[33]. Levosimendan can achieve maximal improvement in hemodynamic parameters at 1 to 3 d after starting the infusion and the effects can be sustained for at least a week[34,35]. Levosimendan can also improve renal function through the increased cardiac output[12]. Moreover, levosimendan can reduce the right-sided pressures, pulmonary artery wedge pressure, and central venous pressure, thereby improving the function of the right ventricles[36,37].
The study by Bragadottir et al[38] showed that levosimendan also increases both renal blood flow and GFR by inducing pre-glomerular vasodilation. The study by Lannemyr et al[15] showed that the renal filtration fraction remained unchanged in levosimendan group but decreased in dobutamine. This is due to levosimendan preferentially vasodilating the afferent arterioles, while dobutamine has balanced vaso
The study by Yilmaz et al[40] also suggested that levosimendan offered more beneficial effects in terms of ejection fraction, systolic pulmonary artery pressure, 24-h urine output, and creatinine compared to dobutamine in patients with biventricular HF. The study by Packer et al[41] showed that levosimendan provided rapid and durable symptomatic relief in the first 5 d but was associated with an increased risk of adverse cardiovascular events such as hypotension, cardiac arrhythmias, and a numerically higher risk of death at 90 d[41]. However, inotropic therapy should be reserved for patients with severe low cardiac output where vasodilatory agents cannot be used to avoid a further decrease in systemic pressure or systemic vascular resis
Ultrafiltration can be an effective decongestion strategy because of the ability to remove the isotonic plasma and therefore more sodium for the same amount of water[44]. The study by Costanzo et al[45] showed that weight loss and net fluid loss were greater in the ultrafiltration group compared to intravenous diuretics. Moreover, the rate of re-hospitalized for HF at 90 d was significantly lower in the ultrafiltration group[45]. However, there were no differences in episodes of hypotension within the first 48 h and serum creatinine at 90 d between the two groups[45]. On the contrary, the study by Bart et al[11] showed that there was a significant increase in serum creatinine level 96 h after enrollment in the ultrafiltration group compared with the pharmacologic therapy group, but there were no significant differences in weight loss. Patients who had ultrafiltration experienced an early rise in the creatinine level due to a transient decrease in intravascular volume[11]. GFR in patients with pharmacological therapy improved significantly after 60 d[11]. Besides that, a higher percentage of patients in the ultrafiltration group experienced a serious adverse event compared to the pharmacologic-therapy group over the 60-d period of follow-up[11]. The most common adverse events associated with ultrafiltration treatment included kidney failure, complications, and catheter-related complications[11]. Therefore, ultrafiltration treatment is not justified for patients with CRS due to the complexity and high cost of treatment[11]. Pharmacological therapy is recommended as the first-line therapy, and ultrafiltration should only be reserved in cases of refractory congestion[8].
CRS in patients with decompensated HF is associated with several cardiovascular and renal adverse events such as myocardial infarction, stroke, need for hemodialysis, high rates of hospitalization, and mortality[16,46,47]. However, management of CRS type 1 is often challenging due to the various underlying mechanisms of renal impairment and the lack of novel therapeutic options targeting renal impairment in HF patients[6,8]. Therefore, early recognition of the condition by using different novel biomarkers and imaging techniques is important to initiate optimal treatment and care of the patients[16]. Moreover, patients with underlying HF should be educated to manage their condition well to prevent decompensation. A multidisciplinary team approach with cooperation between internists, cardiologists, and nephrologists is important to establish an effective treatment plan for patients with CRS to improve their quality of life[6]. Further research on drugs targeting the pathophysiological mechanism CRS, which includes both cardiac and renal dysfunction, can be conducted to improve the survival of the patients.
| 1. | Ronco C, Cicoira M, McCullough PA. Cardiorenal syndrome type 1: pathophysiological crosstalk leading to combined heart and kidney dysfunction in the setting of acutely decompensated heart failure. J Am Coll Cardiol. 2012;60:1031-1042. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 271] [Cited by in RCA: 299] [Article Influence: 21.4] [Reference Citation Analysis (1)] |
| 2. | Hillege HL, Nitsch D, Pfeffer MA, Swedberg K, McMurray JJ, Yusuf S, Granger CB, Michelson EL, Ostergren J, Cornel JH, de Zeeuw D, Pocock S, van Veldhuisen DJ; Candesartan in Heart Failure: Assessment of Reduction in Mortality and Morbidity (CHARM) Investigators. Renal function as a predictor of outcome in a broad spectrum of patients with heart failure. Circulation. 2006;113:671-678. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 657] [Cited by in RCA: 658] [Article Influence: 32.9] [Reference Citation Analysis (13)] |
| 3. | Hillege HL, Girbes AR, de Kam PJ, Boomsma F, de Zeeuw D, Charlesworth A, Hampton JR, van Veldhuisen DJ. Renal function, neurohormonal activation, and survival in patients with chronic heart failure. Circulation. 2000;102:203-210. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 738] [Cited by in RCA: 682] [Article Influence: 26.2] [Reference Citation Analysis (7)] |
| 4. | Ronco C, Haapio M, House AA, Anavekar N, Bellomo R. Cardiorenal syndrome. J Am Coll Cardiol. 2008;52:1527-1539. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1723] [Cited by in RCA: 1456] [Article Influence: 80.9] [Reference Citation Analysis (0)] |
| 5. | Felker GM, Mentz RJ. Diuretics and ultrafiltration in acute decompensated heart failure. J Am Coll Cardiol. 2012;59:2145-2153. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 115] [Cited by in RCA: 110] [Article Influence: 7.9] [Reference Citation Analysis (0)] |
| 6. | Koniari K, Nikolaou M, Paraskevaidis I, Parissis J. Therapeutic options for the management of the cardiorenal syndrome. Int J Nephrol. 2010;2011:194910. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 10] [Article Influence: 0.6] [Reference Citation Analysis (1)] |
| 7. | Geisberg C, Butler J. Addressing the challenges of cardiorenal syndrome. Cleve Clin J Med. 2006;73:485-491. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 23] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 8. | Verbrugge FH, Grieten L, Mullens W. Management of the cardiorenal syndrome in decompensated heart failure. Cardiorenal Med. 2014;4:176-188. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 31] [Article Influence: 2.8] [Reference Citation Analysis (1)] |
| 9. | Kumar U, Wettersten N, Garimella PS. Cardiorenal Syndrome: Pathophysiology. Cardiol Clin. 2019;37:251-265. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 68] [Cited by in RCA: 129] [Article Influence: 18.4] [Reference Citation Analysis (0)] |
| 10. | Owan TE, Chen HH, Frantz RP, Karon BL, Miller WL, Rodeheffer RJ, Hodge DO, Burnett JC Jr, Redfield MM. The effects of nesiritide on renal function and diuretic responsiveness in acutely decompensated heart failure patients with renal dysfunction. J Card Fail. 2008;14:267-275. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 26] [Cited by in RCA: 29] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 11. | Bart BA, Goldsmith SR, Lee KL, Givertz MM, O'Connor CM, Bull DA, Redfield MM, Deswal A, Rouleau JL, LeWinter MM, Ofili EO, Stevenson LW, Semigran MJ, Felker GM, Chen HH, Hernandez AF, Anstrom KJ, McNulty SE, Velazquez EJ, Ibarra JC, Mascette AM, Braunwald E; Heart Failure Clinical Research Network. Ultrafiltration in decompensated heart failure with cardiorenal syndrome. N Engl J Med. 2012;367:2296-2304. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 842] [Cited by in RCA: 691] [Article Influence: 49.4] [Reference Citation Analysis (0)] |
| 12. | Fedele F, Bruno N, Brasolin B, Caira C, D'Ambrosi A, Mancone M. Levosimendan improves renal function in acute decompensated heart failure: possible underlying mechanisms. Eur J Heart Fail. 2014;16:281-288. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 66] [Article Influence: 5.1] [Reference Citation Analysis (0)] |
| 13. | Chen HH, Anstrom KJ, Givertz MM, Stevenson LW, Semigran MJ, Goldsmith SR, Bart BA, Bull DA, Stehlik J, LeWinter MM, Konstam MA, Huggins GS, Rouleau JL, O'Meara E, Tang WH, Starling RC, Butler J, Deswal A, Felker GM, O'Connor CM, Bonita RE, Margulies KB, Cappola TP, Ofili EO, Mann DL, Dávila-Román VG, McNulty SE, Borlaug BA, Velazquez EJ, Lee KL, Shah MR, Hernandez AF, Braunwald E, Redfield MM; NHLBI Heart Failure Clinical Research Network. Low-dose dopamine or low-dose nesiritide in acute heart failure with renal dysfunction: the ROSE acute heart failure randomized trial. JAMA. 2013;310:2533-2543. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 437] [Cited by in RCA: 379] [Article Influence: 29.2] [Reference Citation Analysis (0)] |
| 14. | Inomata T, Ikeda Y, Kida K, Shibagaki Y, Sato N, Kumagai Y, Shinagawa H, Ako J, Izumi T; Kanagawa Aquaresis Investigators. Effects of Additive Tolvaptan vs. Increased Furosemide on Heart Failure With Diuretic Resistance and Renal Impairment - Results From the K-STAR Study. Circ J. 2017;82:159-167. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 56] [Cited by in RCA: 56] [Article Influence: 6.2] [Reference Citation Analysis (0)] |
| 15. | Lannemyr L, Ricksten SE, Rundqvist B, Andersson B, Bartfay SE, Ljungman C, Dahlberg P, Bergh N, Hjalmarsson C, Gilljam T, Bollano E, Karason K. Differential Effects of Levosimendan and Dobutamine on Glomerular Filtration Rate in Patients With Heart Failure and Renal Impairment:A Randomized Double-Blind Controlled Trial. J Am Heart Assoc. 2018;7:e008455. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 45] [Cited by in RCA: 49] [Article Influence: 6.1] [Reference Citation Analysis (0)] |
| 16. | Rangaswami J, Bhalla V, Blair JEA, Chang TI, Costa S, Lentine KL, Lerma EV, Mezue K, Molitch M, Mullens W, Ronco C, Tang WHW, McCullough PA; American Heart Association Council on the Kidney in Cardiovascular Disease and Council on Clinical Cardiology. Cardiorenal Syndrome: Classification, Pathophysiology, Diagnosis, and Treatment Strategies: A Scientific Statement From the American Heart Association. Circulation. 2019;139:e840-e878. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1097] [Cited by in RCA: 923] [Article Influence: 131.9] [Reference Citation Analysis (0)] |
| 17. | Palazzuoli A, Pellegrini M, Ruocco G, Martini G, Franci B, Campagna MS, Gilleman M, Nuti R, McCullough PA, Ronco C. Continuous vs bolus intermittent loop diuretic infusion in acutely decompensated heart failure: a prospective randomized trial. Crit Care. 2014;18:R134. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 42] [Cited by in RCA: 51] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 18. | Ahmad T, Jackson K, Rao VS, Tang WHW, Brisco-Bacik MA, Chen HH, Felker GM, Hernandez AF, O'Connor CM, Sabbisetti VS, Bonventre JV, Wilson FP, Coca SG, Testani JM. Worsening Renal Function in Patients With Acute Heart Failure Undergoing Aggressive Diuresis Is Not Associated With Tubular Injury. Circulation. 2018;137:2016-2028. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 229] [Cited by in RCA: 283] [Article Influence: 35.4] [Reference Citation Analysis (0)] |
| 19. | Mentz RJ, Stevens SR, DeVore AD, Lala A, Vader JM, AbouEzzeddine OF, Khazanie P, Redfield MM, Stevenson LW, O'Connor CM, Goldsmith SR, Bart BA, Anstrom KJ, Hernandez AF, Braunwald E, Felker GM. Decongestion strategies and renin-angiotensin-aldosterone system activation in acute heart failure. JACC Heart Fail. 2015;3:97-107. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 74] [Cited by in RCA: 100] [Article Influence: 8.3] [Reference Citation Analysis (0)] |
| 20. | Ronco C, Di Lullo L. Cardiorenal syndrome. Heart Fail Clin. 2014;10:251-280. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 99] [Cited by in RCA: 100] [Article Influence: 8.3] [Reference Citation Analysis (0)] |
| 21. | Marumo R, Kaizuma S, Nogae S, Kanazawa M, Kimura T, Saito T, Ito S, Matsubara M. Differential upregulation of rat Na-K-Cl cotransporter, rBSC1, mRNA in the thick ascending limb of Henle in different pathological conditions. Kidney Int. 1998;54:877-888. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 34] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 22. | Goldsmith SR, Bart BA, Burnett J. Decongestive therapy and renal function in acute heart failure: time for a new approach? Circ Heart Fail. 2014;7:531-535. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 39] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 23. | Watanabe K, Dohi K, Sugimoto T, Yamada T, Sato Y, Ichikawa K, Sugiura E, Kumagai N, Nakamori S, Nakajima H, Hoshino K, Machida H, Okamoto S, Onishi K, Nakamura M, Nobori T, Ito M. Short-term effects of low-dose tolvaptan on hemodynamic parameters in patients with chronic heart failure. J Cardiol. 2012;60:462-469. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 48] [Cited by in RCA: 43] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 24. | Salvador DR, Rey NR, Ramos GC, Punzalan FE. Continuous infusion vs bolus injection of loop diuretics in congestive heart failure. Cochrane Database Syst Rev. 2004;CD003178. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 24] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 25. | Ljungman S, Kjekshus J, Swedberg K. Renal function in severe congestive heart failure during treatment with enalapril (the Cooperative North Scandinavian Enalapril Survival Study [CONSENSUS] Trial). Am J Cardiol. 1992;70:479-487. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 144] [Cited by in RCA: 129] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 26. | Khan NA, Ma I, Thompson CR, Humphries K, Salem DN, Sarnak MJ, Levin A. Kidney function and mortality among patients with left ventricular systolic dysfunction. J Am Soc Nephrol. 2006;17:244-253. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 105] [Cited by in RCA: 106] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 27. | Ahmed A, Fonarow GC, Zhang Y, Sanders PW, Allman RM, Arnett DK, Feller MA, Love TE, Aban IB, Levesque R, Ekundayo OJ, Dell'Italia LJ, Bakris GL, Rich MW. Renin-angiotensin inhibition in systolic heart failure and chronic kidney disease. Am J Med. 2012;125:399-410. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53] [Cited by in RCA: 60] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 28. | O'Connor CM, Starling RC, Hernandez AF, Armstrong PW, Dickstein K, Hasselblad V, Heizer GM, Komajda M, Massie BM, McMurray JJ, Nieminen MS, Reist CJ, Rouleau JL, Swedberg K, Adams KF Jr, Anker SD, Atar D, Battler A, Botero R, Bohidar NR, Butler J, Clausell N, Corbalán R, Costanzo MR, Dahlstrom U, Deckelbaum LI, Diaz R, Dunlap ME, Ezekowitz JA, Feldman D, Felker GM, Fonarow GC, Gennevois D, Gottlieb SS, Hill JA, Hollander JE, Howlett JG, Hudson MP, Kociol RD, Krum H, Laucevicius A, Levy WC, Méndez GF, Metra M, Mittal S, Oh BH, Pereira NL, Ponikowski P, Tang WH, Tanomsup S, Teerlink JR, Triposkiadis F, Troughton RW, Voors AA, Whellan DJ, Zannad F, Califf RM. Effect of nesiritide in patients with acute decompensated heart failure. N Engl J Med. 2011;365:32-43. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 979] [Cited by in RCA: 936] [Article Influence: 62.4] [Reference Citation Analysis (0)] |
| 29. | Wang DJ, Dowling TC, Meadows D, Ayala T, Marshall J, Minshall S, Greenberg N, Thattassery E, Fisher ML, Rao K, Gottlieb SS. Nesiritide does not improve renal function in patients with chronic heart failure and worsening serum creatinine. Circulation. 2004;110:1620-1625. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 149] [Cited by in RCA: 130] [Article Influence: 5.9] [Reference Citation Analysis (0)] |
| 30. | Yancy CW, Jessup M, Bozkurt B, Butler J, Casey DE Jr, Drazner MH, Fonarow GC, Geraci SA, Horwich T, Januzzi JL, Johnson MR, Kasper EK, Levy WC, Masoudi FA, McBride PE, McMurray JJ, Mitchell JE, Peterson PN, Riegel B, Sam F, Stevenson LW, Tang WH, Tsai EJ, Wilkoff BL. 2013 ACCF/AHA guideline for the management of heart failure: executive summary: a report of the American College of Cardiology Foundation/American Heart Association Task Force on practice guidelines. Circulation. 2013;128:1810-1852. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2469] [Cited by in RCA: 2335] [Article Influence: 179.6] [Reference Citation Analysis (0)] |
| 31. | Hauptman PJ, Swindle J, Burroughs TE, Schnitzler MA. Resource utilization in patients hospitalized with heart failure: insights from a contemporary national hospital database. Am Heart J. 2008;155:978-985.e1. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 25] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 32. | Kass DA, Solaro RJ. Mechanisms and use of calcium-sensitizing agents in the failing heart. Circulation. 2006;113:305-315. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 146] [Cited by in RCA: 143] [Article Influence: 7.2] [Reference Citation Analysis (0)] |
| 33. | Pataricza J, Krassói I, Höhn J, Kun A, Papp JG. Functional role of potassium channels in the vasodilating mechanism of levosimendan in porcine isolated coronary artery. Cardiovasc Drugs Ther. 2003;17:115-121. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 69] [Cited by in RCA: 65] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 34. | Lilleberg J, Laine M, Palkama T, Kivikko M, Pohjanjousi P, Kupari M. Duration of the haemodynamic action of a 24-h infusion of levosimendan in patients with congestive heart failure. Eur J Heart Fail. 2007;9:75-82. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 83] [Cited by in RCA: 101] [Article Influence: 5.1] [Reference Citation Analysis (0)] |
| 35. | McLean AS, Huang SJ, Nalos M, Ting I. Duration of the beneficial effects of levosimendan in decompensated heart failure as measured by echocardiographic indices and B-type natriuretic peptide. J Cardiovasc Pharmacol. 2005;46:830-835. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 25] [Article Influence: 1.2] [Reference Citation Analysis (1)] |
| 36. | Poelzl G, Zwick RH, Grander W, Metzler B, Jonetzko P, Frick M, Ulmer H, Pachinger O, Roithinger FX. Safety and effectiveness of levosimendan in patients with predominant right heart failure. Herz. 2008;33:368-373. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 34] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 37. | Russ MA, Prondzinsky R, Carter JM, Schlitt A, Ebelt H, Schmidt H, Lemm H, Heinroth K, Soeffker G, Winkler M, Werdan K, Buerke M. Right ventricular function in myocardial infarction complicated by cardiogenic shock: Improvement with levosimendan. Crit Care Med. 2009;37:3017-3023. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 80] [Cited by in RCA: 79] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 38. | Bragadottir G, Redfors B, Ricksten SE. Effects of levosimendan on glomerular filtration rate, renal blood flow, and renal oxygenation after cardiac surgery with cardiopulmonary bypass: a randomized placebo-controlled study. Crit Care Med. 2013;41:2328-2335. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 61] [Cited by in RCA: 78] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 39. | Zager RA, Johnson AC, Lund S, Hanson SY, Abrass CK. Levosimendan protects against experimental endotoxemic acute renal failure. Am J Physiol Renal Physiol. 2006;290:F1453-F1462. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 110] [Cited by in RCA: 109] [Article Influence: 5.5] [Reference Citation Analysis (1)] |
| 40. | Yilmaz MB, Yontar C, Erdem A, Karadas F, Yalta K, Turgut OO, Yilmaz A, Tandogan I. Comparative effects of levosimendan and dobutamine on right ventricular function in patients with biventricular heart failure. Heart Vessels. 2009;24:16-21. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 56] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 41. | Packer M, Colucci W, Fisher L, Massie BM, Teerlink JR, Young J, Padley RJ, Thakkar R, Delgado-Herrera L, Salon J, Garratt C, Huang B, Sarapohja T; REVIVE Heart Failure Study Group. Effect of levosimendan on the short-term clinical course of patients with acutely decompensated heart failure. JACC Heart Fail. 2013;1:103-111. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 259] [Cited by in RCA: 288] [Article Influence: 22.2] [Reference Citation Analysis (1)] |
| 42. | Elkayam U, Tasissa G, Binanay C, Stevenson LW, Gheorghiade M, Warnica JW, Young JB, Rayburn BK, Rogers JG, DeMarco T, Leier CV. Use and impact of inotropes and vasodilator therapy in hospitalized patients with severe heart failure. Am Heart J. 2007;153:98-104. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 185] [Cited by in RCA: 159] [Article Influence: 8.4] [Reference Citation Analysis (0)] |
| 43. | Felker GM, O'Connor CM. Inotropic therapy for heart failure: an evidence-based approach. Am Heart J. 2001;142:393-401. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 179] [Cited by in RCA: 146] [Article Influence: 5.8] [Reference Citation Analysis (0)] |
| 44. | Ali SS, Olinger CC, Sobotka PA, Dahle TG, Bunte MC, Blake D, Boyle AJ. Loop diuretics can cause clinical natriuretic failure: a prescription for volume expansion. Congest Heart Fail. 2009;15:1-4. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 55] [Cited by in RCA: 49] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 45. | Costanzo MR, Guglin ME, Saltzberg MT, Jessup ML, Bart BA, Teerlink JR, Jaski BE, Fang JC, Feller ED, Haas GJ, Anderson AS, Schollmeyer MP, Sobotka PA; UNLOAD Trial Investigators. Ultrafiltration vs intravenous diuretics for patients hospitalized for acute decompensated heart failure. J Am Coll Cardiol. 2007;49:675-683. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 900] [Cited by in RCA: 674] [Article Influence: 35.5] [Reference Citation Analysis (0)] |
| 46. | Billings FT 4th, Shaw AD. Clinical trial endpoints in acute kidney injury. Nephron Clin Pract. 2014;127:89-93. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 67] [Cited by in RCA: 133] [Article Influence: 11.1] [Reference Citation Analysis (0)] |
| 47. | Ronco C, Ronco F, McCullough PA. A Call to Action to Develop Integrated Curricula in Cardiorenal Medicine. Blood Purif. 2017;44:251-259. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 19] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
Open-Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/Licenses/by-nc/4.0/
Manuscript source: Invited manuscript
Specialty type: Medical laboratory technology
Country/Territory of origin: Malaysia
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): 0
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Greenway SC S-Editor: Gao CC L-Editor: Filipodia P-Editor: Yuan YY