©The Author(s) 2024.
World J Methodol. Jun 20, 2024; 14(2): 89809
Published online Jun 20, 2024. doi: 10.5662/wjm.v14.i2.89809
Published online Jun 20, 2024. doi: 10.5662/wjm.v14.i2.89809
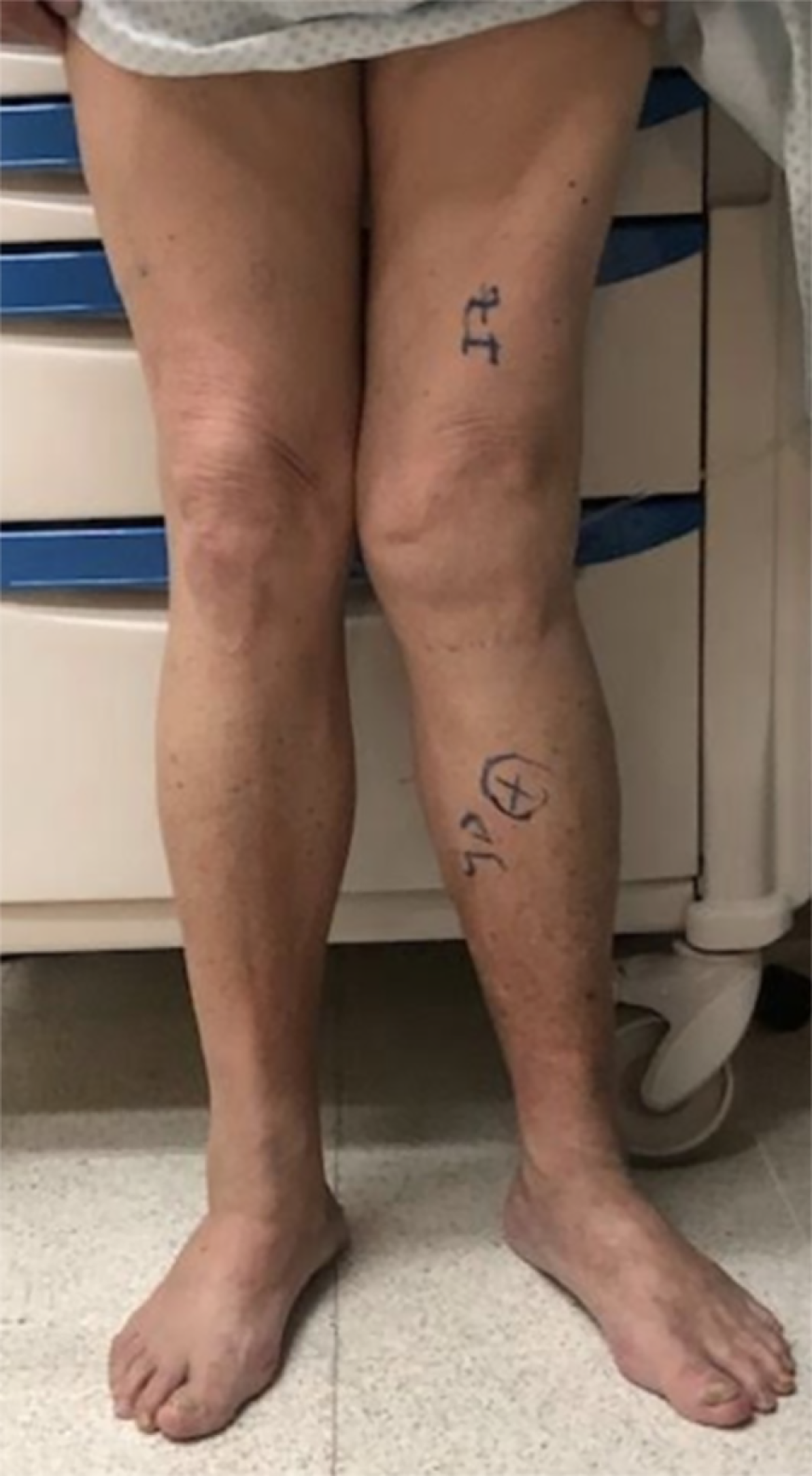
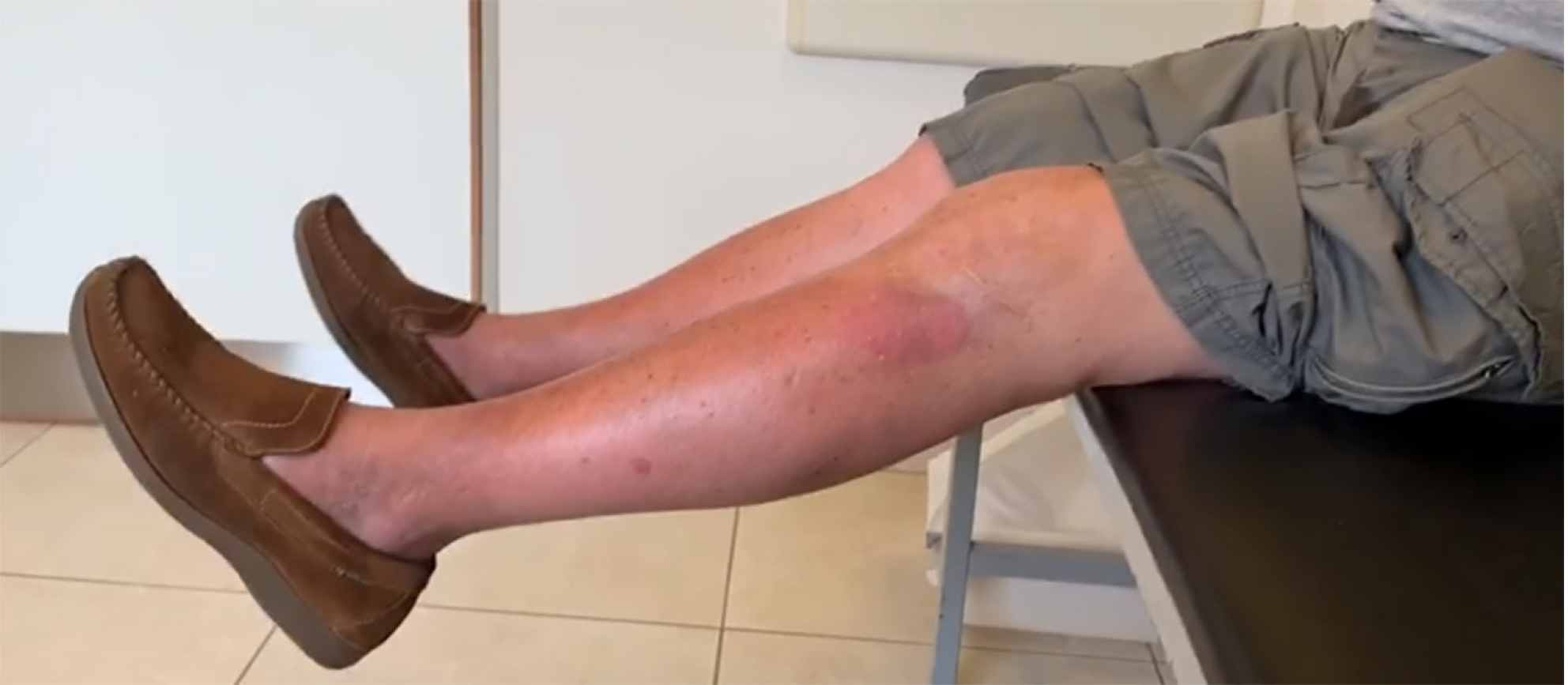
Figure 1 Pre-operative physical examination.
It shows valgus misalignment in the left knee on the coronal view.
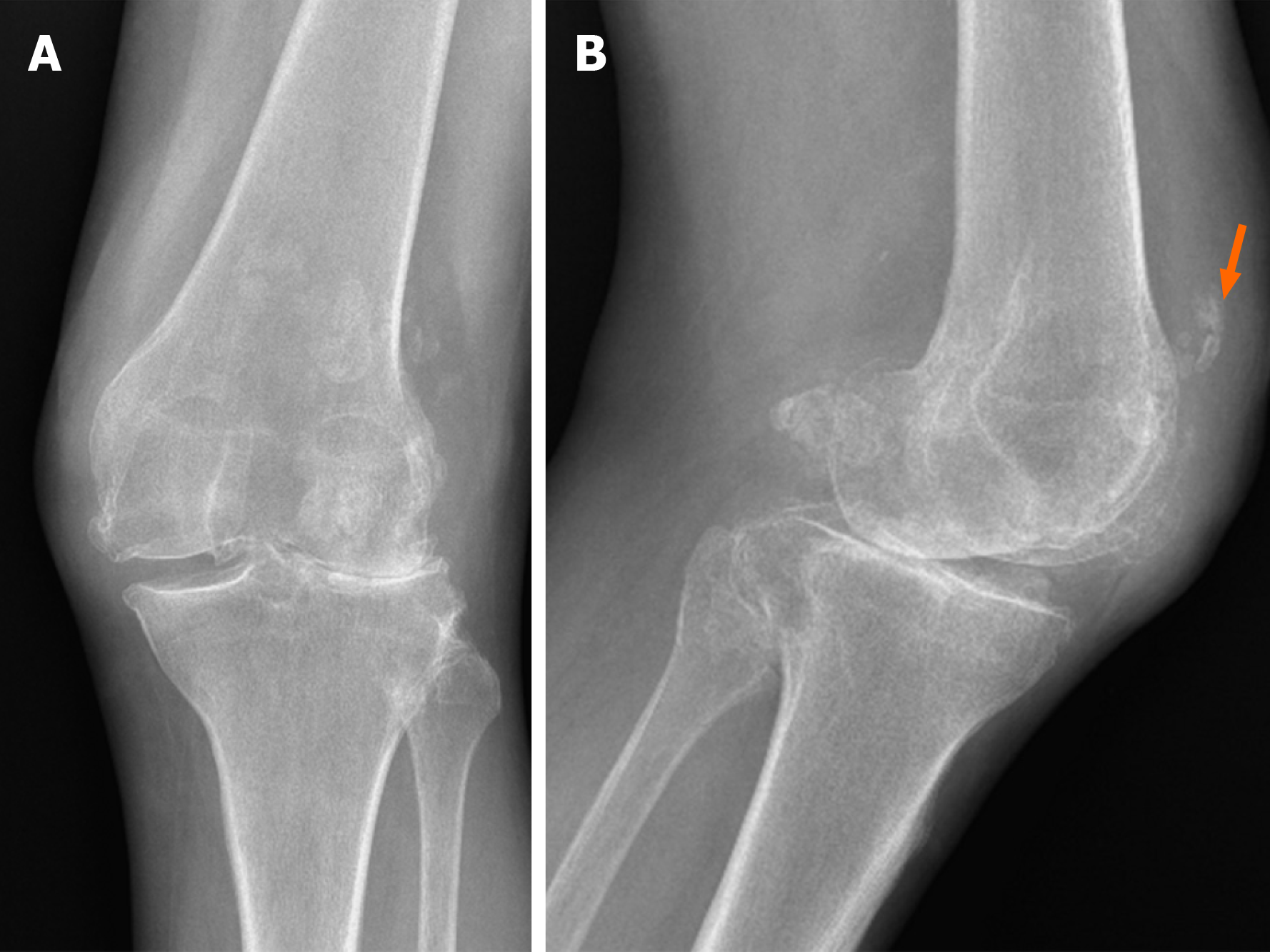
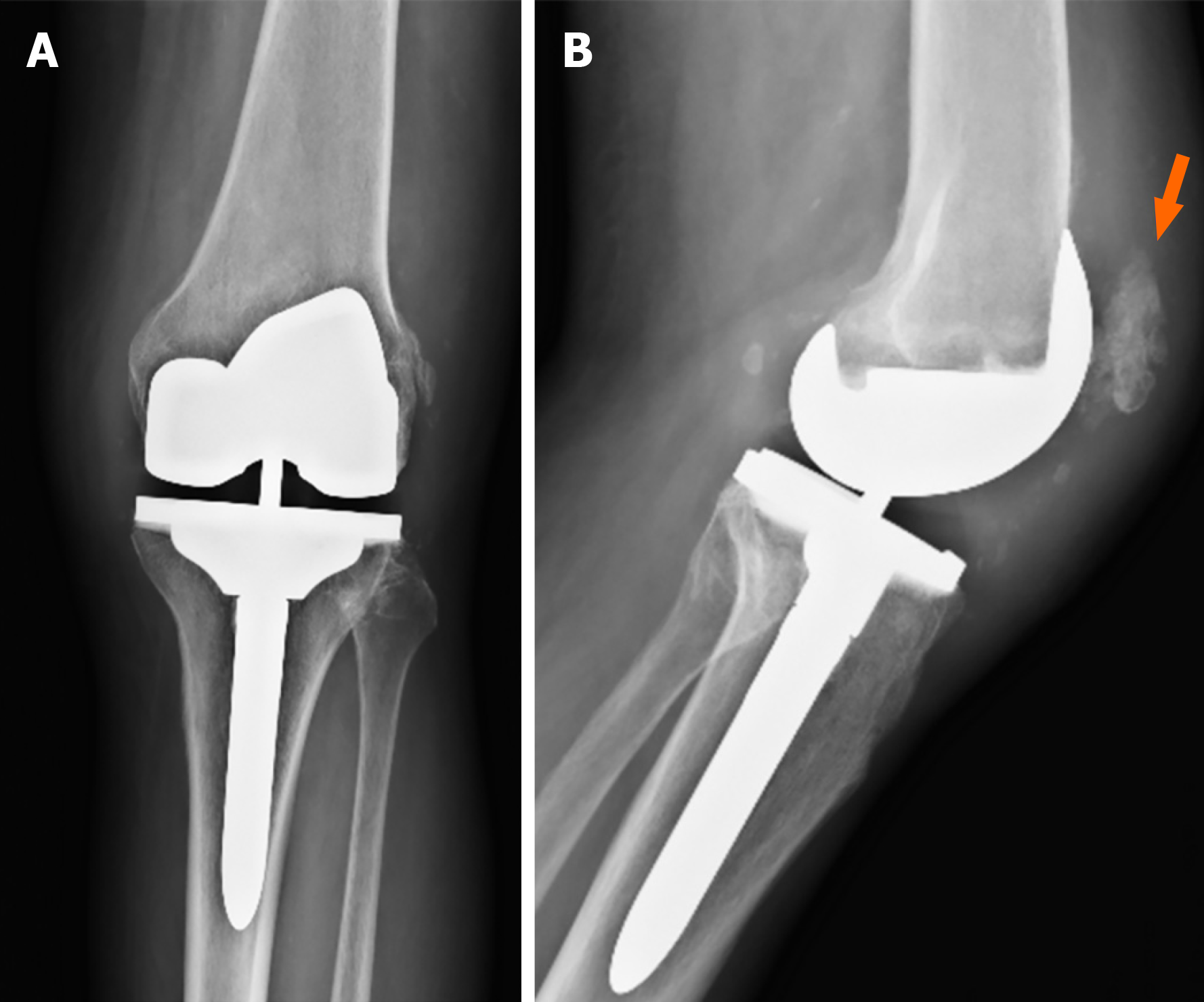
Figure 2 Pre-operative X-rays.
A and B: It shows severe valgus osteoarthritis in the anteroposterior view (A) and the absence of the patella with areas of tendon calcification (orange arrow) in the lateral view (B).
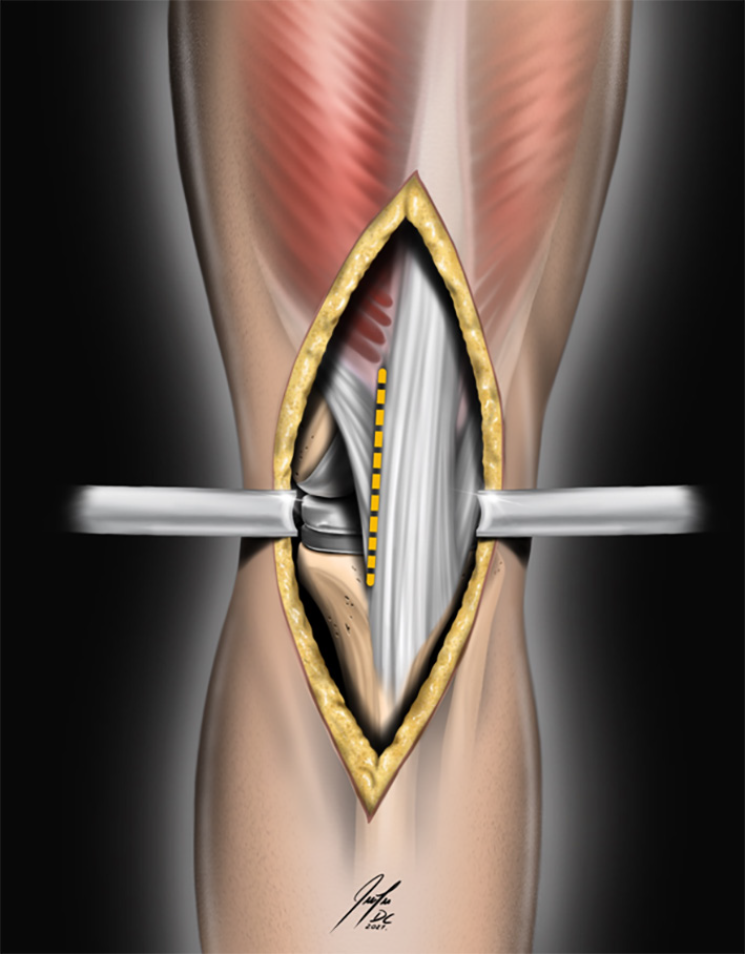
Figure 3 The picture illustrates the localization of the tendon incision to create an intra-tendon pocket (dashed line).
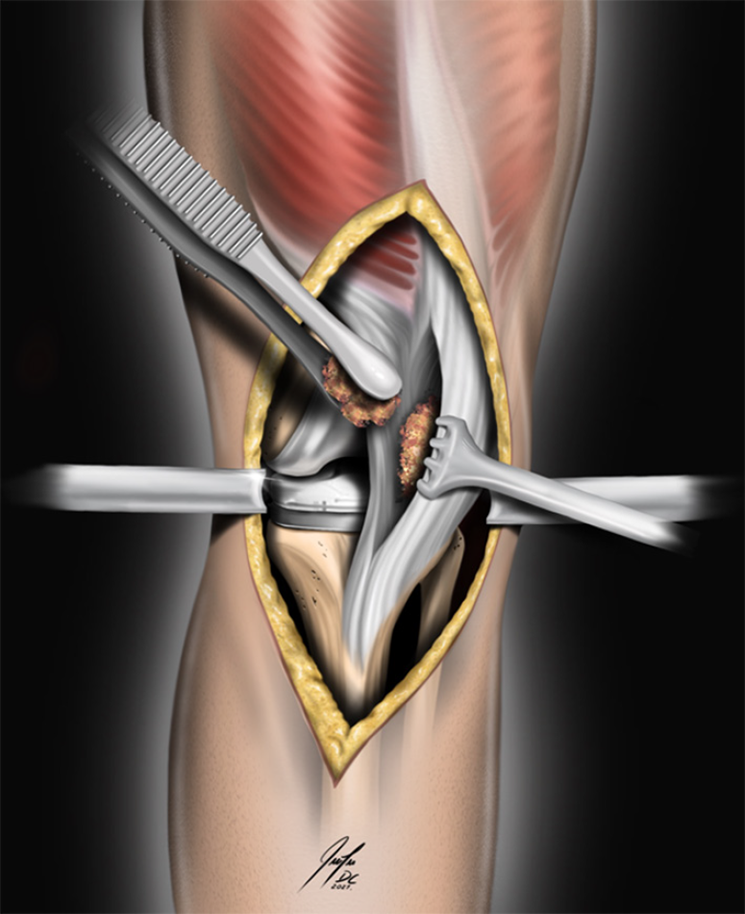
Figure 4 The picture demonstrates the fitting of autogenous bone chips from the remaining routine cuts into the intra-tendon pocket.
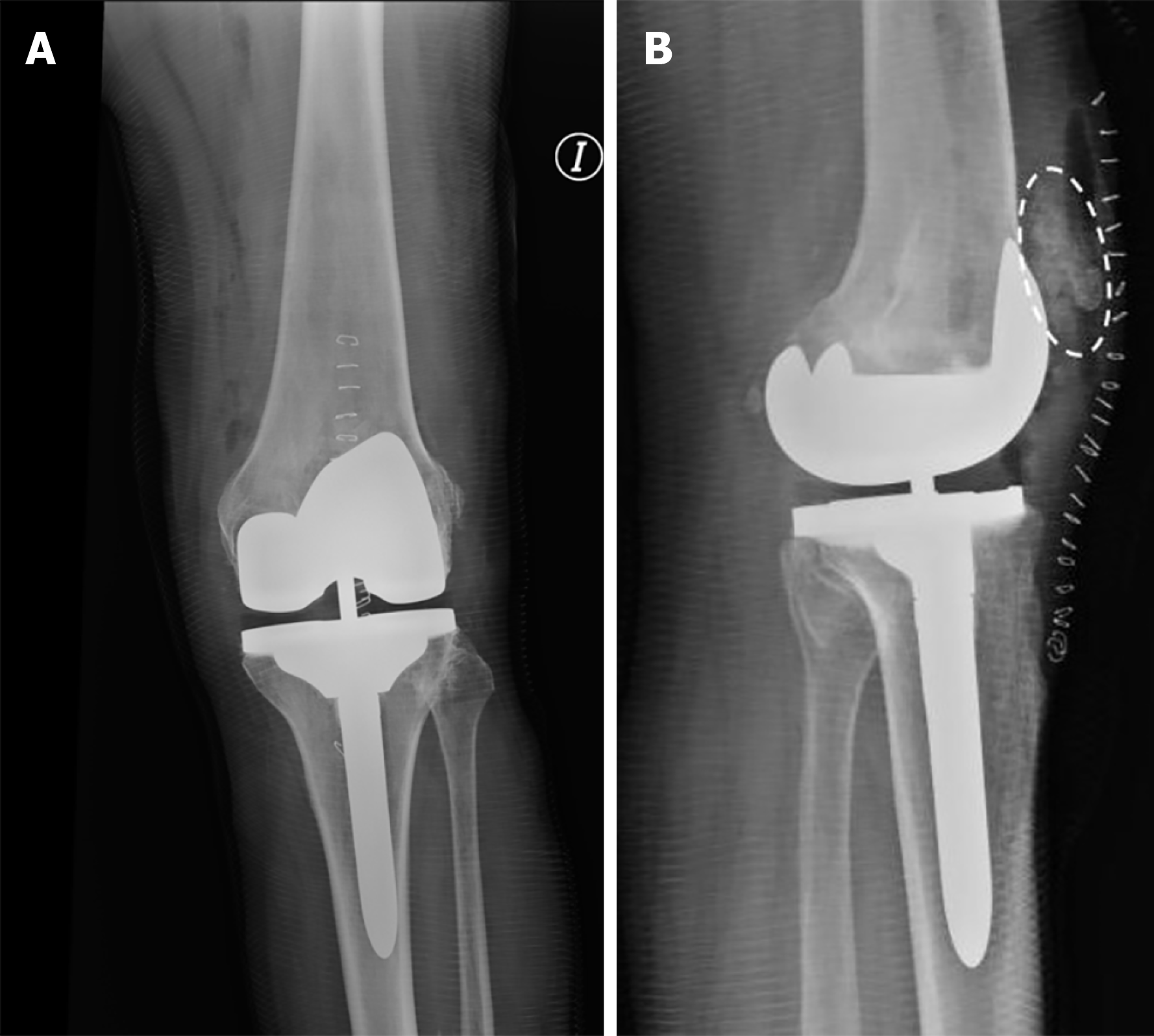
Figure 5 Immediate postoperative X-rays.
A: It demonstrates good alignment of total knee arthroplasty in the anteroposterior view; B: In the lateral view, the neo-patella evidence is filled with bone chips (dashed circle), giving the appearance of a fragmented patella.
Figure 6 Post-operative clinical image.
It was taken at five months showing complete recovery of knee extension.
Figure 7 Two-year follow-up.
A: No signs of prosthesis loosening are apparent in either the anteroposterior or lateral views; B: Moreover, in the lateral view, there is no evidence of neo-patellar resorption; instead, it shows an improved shape closely resembling the native patella. It is important to note that the patella appears slightly higher, although this does not manifest as clinical instability.
- Citation: Perez-Abdala JI, De Cicco FL, Nicolino T, Astoul J. Patellar reconstruction in primary total knee arthroplasty using bone chips from routine cuts: A case report and review of literature. World J Methodol 2024; 14(2): 89809
- URL: https://www.wjgnet.com/2222-0682/full/v14/i2/89809.htm
- DOI: https://dx.doi.org/10.5662/wjm.v14.i2.89809