Published online Mar 9, 2026. doi: 10.5492/wjccm.v15.i1.117127
Revised: December 23, 2025
Accepted: January 19, 2026
Published online: March 9, 2026
Processing time: 91 Days and 20.5 Hours
This editorial comments on the randomized controlled trial by Aggarwal et al, which demonstrates video laryngoscope (VL) superiority over intubating laryn
Core Tip: This editorial highlights Aggarwal et al’s trial showing video laryngoscopy (VL) outperforming intubating laryngeal mask airway (ILMA) in critically ill patients, with higher first-attempt success (87.5% vs 53.1%), faster intubation (44.0 ± 19.7 seconds vs 82.5 ± 14.5 seconds), and fewer complications. Superior glottic visualization positions VL as first-line for emergency airways, with ILMA as rescue. Findings advocate protocol revisions, VL training, and resource prioritization for better out
- Citation: Feyissa GD. Advancing emergency airway management: Video laryngoscope vs intubating laryngeal mask airway in critical care. World J Crit Care Med 2026; 15(1): 117127
- URL: https://www.wjgnet.com/2220-3141/full/v15/i1/117127.htm
- DOI: https://dx.doi.org/10.5492/wjccm.v15.i1.117127
Airway management remains a cornerstone of critical care, especially in emergency settings where patients often have deteriorated physiological reserve and anatomical challenges[1].
Emergency airway management is a vital lifesaving intervention but carries significant risks, including hypoxia, hyp
This editorial comments on the randomized controlled trial by Aggarwal et al[5], comparing VL and ILMA for emer
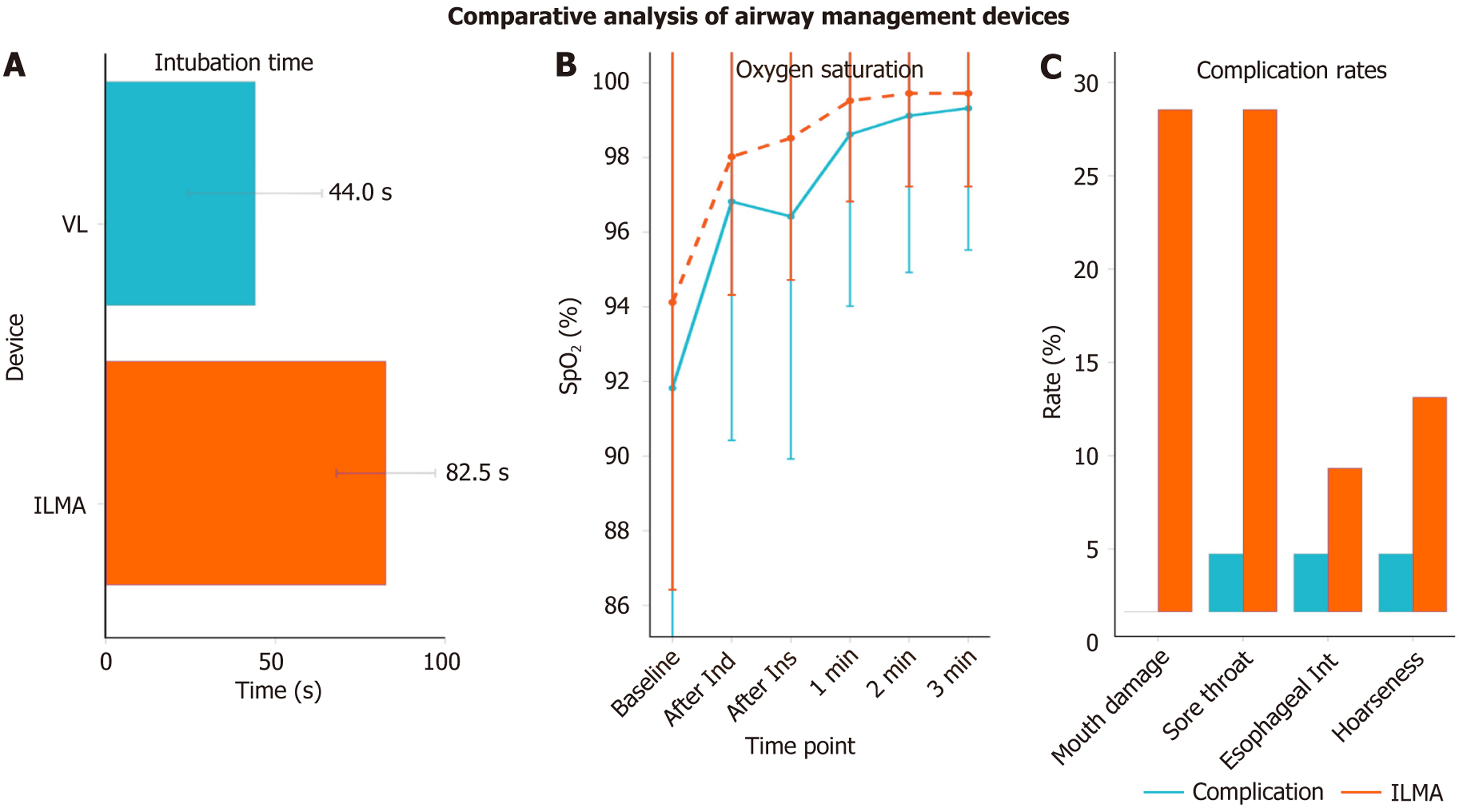
Aggarwal et al[5] demonstrated VL superiority over ILMA in 64 critically ill patients, with first-attempt success rates of 87.5% (VL) vs 53.1% (ILMA) and intubation times of 44.0 ± 19.7 seconds (VL) vs 82.5 ± 14.5 seconds (ILMA) (Table 1, Figure 1). These findings align with prior studies, including Jakhar et al[6] (96.97% VL vs 81.25% ILMA) and Tienpratarn et al[7] (96.88% VL vs 81.25% ILMA), confirming VL's consistent efficiency across contexts. Additional evidence shows VL first-attempt success ranging from 80% to 83.3% in intensive care unit (ICU) and emergency settings, supporting its pre
| Outcome | Video laryngoscope group (n = 32) | Intubating laryngeal mask airway group (n = 32) |
| First-attempt success | 28 (87.5) | 17 (53.1) |
| Attempts distribution | ||
| 1 attempt | 28 (87.5) | 17 (53.1) |
| 2 attempts | 4 (12.5) | 7 (21.9) |
| 3 attempts | 0 (0) | 2 (6.2) |
| Failed intubation | 0 (0) | 6 (18.8) |
VL maintained stable oxygen saturation (no desaturation) and hemodynamic parameters comparable to ILMA, with fewer complications: No peri-intubation mouth damage (0% VL vs 26.9% ILMA), lower sore throat incidence (3.1% VL vs 26.9% ILMA), and minimal esophageal intubation (3.1% VL vs 7.7% ILMA) (Figure 1). ILMA’s blind insertion increased tissue trauma risks, underscoring VL’s visualization advantage in emergency settings.
The differential performance between VL and ILMA largely stems from intrinsic design differences. VL’s camera-assisted visualization enables precise airway navigation, reducing intubation failures and shortening procedure duration[9], an advantage particularly critical for patients with limited cardiorespiratory reserves where every second of hypoxia impacts outcomes. This study corroborates prior meta-analyses advocating VL’s benefits and extends knowledge by directly comparing it with ILMA, a widely used alternative device[10].
While the study excluded difficult airway cases, limiting broad generalizability, it provides valuable evidence sup
Aggarwal et al’s sample (n = 64) yielded statistically significant differences (e.g., first-attempt success P < 0.05) despite no formal power calculation statement[5], suggesting adequate detection for primary outcomes. The single-center design limits generalizability; multicenter trials across diverse ICU populations would strengthen external validity. Exclusion of predicted difficult airways likely underestimates VL’s real-world advantage, as unanticipated challenges prevail in rou
First-line device selection: VL carry higher upfront costs than ILMA, but offer greater versatility through reusable handles with multiple blade sizes compatible across patients, potentially offsetting expenses in high-volume ICUs. ILMAs provide autoclaving/reuse advantages but require size-specific variants for different endotracheal tubes, plus dem
VL achieves superior first-attempt success (87.5% vs 53.1%), faster intubation times (44.0 ± 19.7 seconds vs 82.5 ± 14.5 seconds), and lower complication rates than ILMA, establishing VL as the preferred first-line device for emergency intubation in critical care. This performance edge supports VL’s reliability in high-stakes scenarios, where rapid airway securement is critical for survival in patients with limited physiological reserve. The shift aligns with Difficult Airway Society 2025 guidelines prioritizing VL in emergencies and ICU airway consensus recommendations for VL first-line, with ILMA reserved as rescue[13,14].
Rescue strategy planning: ILMA retains value as an immediate backup when VL fails, offering ventilation during atte
Training considerations: Significant performance disparities necessitate prioritizing VL proficiency in critical care cur
Protocol development: Institutions should revise airway management protocols to prioritize VL in time-sensitive emer
Resource allocation: One versatile VL with multiple blades suffices across cases, unlike ILMA requiring size-specific variants for different endotracheal tubes-potentially offsetting VL’s upfront cost. However, VL demands careful handling and disposable blades/covers, while reusable ILMA supports autoclaving for repeated use, influencing long-term economics in resource-limited settings.
Future research should focus on large-scale, multicenter randomized controlled trials in heterogeneous patient popu
Aggarwal et al[5] establish VL as the superior first-line device for emergency intubation in critically ill patients, demon
| 1. | Levitan RM, Heitz JW, Sweeney M, Cooper RM. The complexities of tracheal intubation with direct laryngoscopy and alternative intubation devices. Ann Emerg Med. 2011;57:240-247. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 117] [Cited by in RCA: 128] [Article Influence: 8.5] [Reference Citation Analysis (1)] |
| 2. | Garcia SI, Smischney NJ, Sandefur BJ, D'Andria Ursoleo J, Kelm DJ, Wieruszewski PM. Peri-intubation Cardiovascular Collapse During Emergency Airway Management. Pulm Ther. 2025;11:569-585. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 3. | Chowdhury R, Orishchak O, Mascarella MA, Aldriweesh B, Alnoury MK, Bousquet-Dion G, Yeung J, Nguyen LHP. Emergency Airway Management: A Systematic Review on the Effectiveness of Cognitive Aids in Improving Outcomes and Provider Performance. Clin Pract. 2025;15:13. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |
| 4. | Shaikh S, Hejazi H, Shaikh S, Sajid A, Shahab R, Deed A, Afnan R, Hashmi A, Sharieff REA, Naureen A, Ribeiro MAF Jr. Suction-Assisted Laryngoscopy and Airway Decontamination (SALAD) for Emergency Airway Management: A Systematic Review of Evidence and Implementation. J Clin Med. 2025;14:7430. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 5. | Aggarwal A, Mustahsin M, Shishir P. Comparison of intubating laryngeal mask airway and video laryngoscope during emergency intubation in patients who are critically ill. World J Crit Care Med. 2026;15:112345. [RCA] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (1)] |
| 6. | Jakhar R, Saigal D, Kale S, Aggarwal S. Comparison of Videolaryngoscope and Intubating Laryngeal Mask Airway for Tracheal Intubation with Manual-in-line Stabilization in Patients Undergoing Cervical Spine Surgery. Anesth Essays Res. 2020;14:485-491. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 9] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 7. | Tienpratarn W, Boonyingsatit M, Yuksen C, Leela-Amornsin S, Jamkrajang P, Chrunarm T, Rienrakwong S. Comparison of Video Laryngoscope (VL) and Intubating Laryngeal Mask Airway (I-LMA) for Endotracheal Intubation in a Manikin with Restricted Neck Motion. Arch Acad Emerg Med. 2025;13:e1. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (2)] |
| 8. | Keshari U, Thakur R, Soni S, Yadav A. Ease of intubation: King vision video laryngoscope versus macintosh laryngoscope. Bioinformation. 2025;21:1234-1238. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 9. | Driver BE, Prekker ME, Klein LR, Reardon RF, Miner JR, Fagerstrom ET, Cleghorn MR, McGill JW, Cole JB. Effect of Use of a Bougie vs Endotracheal Tube and Stylet on First-Attempt Intubation Success Among Patients With Difficult Airways Undergoing Emergency Intubation: A Randomized Clinical Trial. JAMA. 2018;319:2179-2189. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 157] [Cited by in RCA: 220] [Article Influence: 27.5] [Reference Citation Analysis (5)] |
| 10. | Jiang J, Ma DX, Li B, Wu AS, Xue FS. Videolaryngoscopy versus direct laryngoscopy for nasotracheal intubation: A systematic review and meta-analysis of randomised controlled trials. J Clin Anesth. 2019;52:6-16. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 24] [Article Influence: 3.0] [Reference Citation Analysis (1)] |
| 11. | Özdil S, Arslan Aydın Zİ, Baykara ZN, Toker K, Solak ZM. Tracheal intubation in patients immobilized by a rigid collar: a comparison of GlideScope and an intubating laryngeal mask airway. Turk J Med Sci. 2016;46:1617-1623. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 9] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 12. | Villareal A, de Somocurcio AR, Schauweker C, Fisher R, Cornelius B. Endotracheal Tube Replacement in the Prone Position With Intubating Laryngeal Mask Airway/Flexible Fiberoptic Scope Combination or Glidescope® Video Laryngoscope: A Manikin-Based Study. AANA J. 2025;93:339-344. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 1.0] [Reference Citation Analysis (1)] |
| 13. | Ahmad I, El-Boghdadly K, Iliff H, Dua G, Higgs A, Huntington M, Mir F, Nouraei SAR, O'Sullivan EP, Patel A, Rivett K, McNarry AF. Difficult Airway Society 2025 guidelines for management of unanticipated difficult tracheal intubation in adults. Br J Anaesth. 2026;136:283-307. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 51] [Article Influence: 51.0] [Reference Citation Analysis (1)] |
| 14. | Cook TM, El-Boghdadly K, McGuire B, McNarry AF, Patel A, Higgs A. Consensus guidelines for managing the airway in patients with COVID-19: Guidelines from the Difficult Airway Society, the Association of Anaesthetists the Intensive Care Society, the Faculty of Intensive Care Medicine and the Royal College of Anaesthetists. Anaesthesia. 2020;75:785-799. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 725] [Cited by in RCA: 630] [Article Influence: 105.0] [Reference Citation Analysis (1)] |
| 15. | De Jong A, Molinari N, Terzi N, Mongardon N, Arnal JM, Guitton C, Allaouchiche B, Paugam-Burtz C, Constantin JM, Lefrant JY, Leone M, Papazian L, Asehnoune K, Maziers N, Azoulay E, Pradel G, Jung B, Jaber S; AzuRéa Network for the Frida-Réa Study Group. Early identification of patients at risk for difficult intubation in the intensive care unit: development and validation of the MACOCHA score in a multicenter cohort study. Am J Respir Crit Care Med. 2013;187:832-839. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 202] [Cited by in RCA: 225] [Article Influence: 17.3] [Reference Citation Analysis (4)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/