Published online Mar 9, 2026. doi: 10.5492/wjccm.v15.i1.112345
Revised: August 15, 2025
Accepted: November 13, 2025
Published online: March 9, 2026
Processing time: 219 Days and 18 Hours
Emergency endotracheal intubation is a high-risk procedure in patients who are critically ill and associated with complications such as hypoxia, hemodynamic instability, and airway trauma. The intubating laryngeal mask airway (ILMA) and video laryngoscope (VL) are alternative devices to conventional direct laryngo
To compare the first-attempt success rate, intubation time, hemodynamic res
A prospective randomized study was conducted on 64 patients who were critically ill and requiring emergency intubation. Patients were divided into the VL (n = 32) and ILMA (n = 32) groups. Primary outcomes included first-attempt success rate and intubation time. Secondary outcomes assessed hemodynamic changes (mean arterial pressure, heart rate, oxygen saturation) and complications (trauma, desaturation, sore throat).
The VL group had a significantly higher first-attempt success rate (87.5% vs 53.1%, P = 0.009) and shorter total intubation time (44.0 ± 19.7 seconds vs 82.5 ± 14.5 seconds, P < 0.001). Hemodynamic responses were comparable, but ILMA was associated with more complications (mouth damage: 26.9% vs 0%, P = 0.002; sore throat: 26.9% vs 3.1%, P = 0.009).
VL is superior to ILMA for emergency intubation, offering higher first-pass success, faster intubation, and fewer complications. VL should be prioritized in critical care settings.
Core Tip: This randomized controlled trial demonstrated video laryngoscope (VL) outperformed intubating laryngeal mask airway (ILMA) for emergency intubation in patients who were critically ill, showing significantly higher first-attempt success (87.5% vs 53.1%), faster intubation (44.0 ± 19.7 seconds vs 82.5 ± 14.5 seconds), and fewer complications. The superior visualization of VL and reduced need for adjunctive maneuvers make it the preferred first-line device for emer
- Citation: Aggarwal A, Mustahsin M, Shishir P. Comparison of intubating laryngeal mask airway and video laryngoscope during emergency intubation in patients who are critically ill. World J Crit Care Med 2026; 15(1): 112345
- URL: https://www.wjgnet.com/2220-3141/full/v15/i1/112345.htm
- DOI: https://dx.doi.org/10.5492/wjccm.v15.i1.112345
Airway management remains a cornerstone of anesthetic practice and critical care with tracheal intubation serving as a vital life-saving intervention in emergency settings. Since its inception in the early 19th century, direct laryngoscopy (DL) has been the gold standard for endotracheal intubation (ETI)[1]. However, this procedure is not without risks as stimulation of the pharyngeal and laryngeal structures during laryngoscopy often triggers significant hemodynamic fluctuations due to sympathetic activation[2]. Moreover, ETI carries substantial morbidity with complications occurring in 25%-40% of cases and a 1.6%-2.7% risk of cardiac arrest following failed intubation attempts[3-5]. The likelihood of adverse events escalates with repeated attempts, emphasizing the need for reliable first-pass success, particularly in high-risk environments such as the intensive care unit (ICU) where difficult intubation rates range from 10% to 20%[6,7].
Emergency airway management presents unique challenges, including time constraints, suboptimal patient positioning, and the potential for hemodynamic instability. Rapid sequence intubation is commonly employed to mitigate aspiration risk and facilitate prompt airway control, yet improper execution can lead to catastrophic outcomes. Con
To address the limitations of DL, alternative intubation devices have been developed. Among these the intubating laryngeal mask airway (ILMA) and video laryngoscope (VL) have emerged as valuable tools. The ILMA enables blind or fiberoptic-guided tracheal intubation while maintaining ventilation, making it particularly advantageous in cases of difficult anatomy, cervical spine immobilization, or failed DL. Despite its utility ILMA has drawbacks, including a lower first-pass success rate compared with VL and limitations in patients with upper airway obstruction[8,9].
VL, introduced in the early 2000s, offers superior glottic visualization by using a camera-equipped blade to transmit real-time images to a monitor. This technology facilitates intubation even in patients with challenging airway anatomy and has gained widespread adoption, particularly in the United States where it is now the first-line approach in over 90% of ICU intubations[10]. However, VL is not without limitations as issues such as fogging, secretions obscuring the camera, and difficulty in tube delivery despite optimal glottic view can hinder performance. Furthermore, its role in emergency intubations remains debated with meta-analyses failing to conclusively demonstrate improved first-attempt success rates in patients who are critically ill[11].
While previous studies have compared ILMA and VL to DL in controlled settings, data on their efficacy in emergency and ICU intubations are scarce. Given the high stakes of airway management in patients who are critically ill, a direct comparison of these devices in emergency scenarios is warranted. This study evaluated the performance of ILMA (LMA-Fastrach™; LMA North America, Inc., San Diego, CA, United States) vs VL (King Vision Videolaryngoscope, Aircraft Medical, Edinburgh, United Kingdom) for emergency intubation in patients in the ICU, assessing metrics such as first-pass success rate, time to intubation, and hemodynamic stability to guide clinical decision-making in high-acuity settings.
This prospective randomized comparative study was conducted in Critical Care Unit of the Department of Anaesthe
Written informed consent was obtained from all the participants’ legal representatives prior to enrollment. The study included 64 adult patients (> 18 years) requiring emergency ETI due to acute respiratory failure. Patients were randomly allocated into two equal groups (n = 32 each) using the sequentially numbered opaque sealed envelope technique: (1) The VL group received intubation with the King Vision Videolaryngoscope (Aircraft Medical); and (2) The ILMA group received intubation with the LMA-Fastrach™ (LMA North America, Inc.).
If possible, patients underwent standardized airway evaluation including thyromental, interincisor, and sternomental distances, neck circumference, modified Mallampati classification. Patients with suspected difficult airway (Mallampati class IV, thyromental distance < 6 cm), oral cavity pathology preventing device insertion, mouth opening < 18 mm, or cervical spine injury were excluded from the study.
All patients were premedicated with intravenous midazolam (0.03-0.05 mg/kg), fentanyl (1-2 µg/kg), and glyco
In the VL group the VL was introduced into the patient’s mouth after ensuring adequate anesthesia depth and muscle relaxation. The epiglottis and vocal cords were visualized on the video monitor, and the endotracheal tube (7.0-7.5 mm internal diameter for females and 8.0-8.5 mm internal diameter for males) was guided through the vocal cords. The tube placement was confirmed by visualizing the tube passing through the cords and by positive end-tidal carbon dioxide on capnography and chest rise. The time from insertion of the device to confirmation of intubation was recorded. The maneuvers performed in the VL group in cases of difficulty in visualization of the glottis were backward, upward, right pressure applied on the cricoid for better visualization of the glottis and turning the VL right or left or slightly removing the VL for better visualization of the glottis.
In the ILMA group the ILMA was inserted following standard procedures, ensuring proper placement by confirming the absence of resistance during ventilation. The prewarmed endotracheal tube (7.0 mm internal diameter for females and 8.0 mm internal diameter for males) was then advanced through the ILMA into the trachea. Placement of the tube in the trachea was confirmed by capnography and chest rise, and the time from ILMA insertion to confirmation of correct tube placement was recorded. ILMA was removed while stabilizing the tube with tube stabilizer. Chandy’s maneuvers (1 and 2) and up-down maneuver were employed as needed[12].
In either group if the first attempt at intubation was unsuccessful, subsequent attempts were made. After three unsuccessful attempts, the intubation was considered failed, and a DL approach was employed. After intubation the patient was placed on mechanical ventilation with cuff pressure maintained at 20-30 cm H2O.
The primary outcomes of our study were first-attempt success rate and time to successful intubation. Secondary outcomes were hemodynamic changes (mean arterial pressure, heart rate, oxygen saturation) at baseline, post-induction, post-device insertion, and 1-minute post-intubation up to 3 minutes. Other secondary outcomes were incidence of desa
The sample size was calculated at the department of Social and Preventive Medicine, Era’s Lucknow Medical College and Hospital based on the variation in intubation time between the two study groups using the following formula: N = (Zα/2 + Zβ)2 × (σ12 + σ22) × d2 × kn = d2 × (Zα/2 + Zβ)2 × (σ12 + σ22) × k [where σ1 = 22.1 SD of intubation time in the VL group, σ2 = 42.7 SD of intubation time in the ILMA group[13], d = mean (μ1, μ2) clinically significant difference between groups, k = 1.0 design effect (assuming equal group sizes), type I error (α) = 5% corresponding to a 95% confidence level (Zα/2 = 1.96), and type II error (β) = 10% for 90% study power (Zβ= 1.28)]. Assuming a clinically significant difference derived from prior data[13], the required sample size per group was 32 per group.
Data were analyzed using Statistical Package for the Social Sciences v25.0 software (IBM Corp., Armonk, NY, United States). Continuous variables were measured using the independent t-test or Mann-Whitney U test. Categorical variables were measured using the χ2 test or Fisher’ s exact test. P < 0.05 was considered significant.
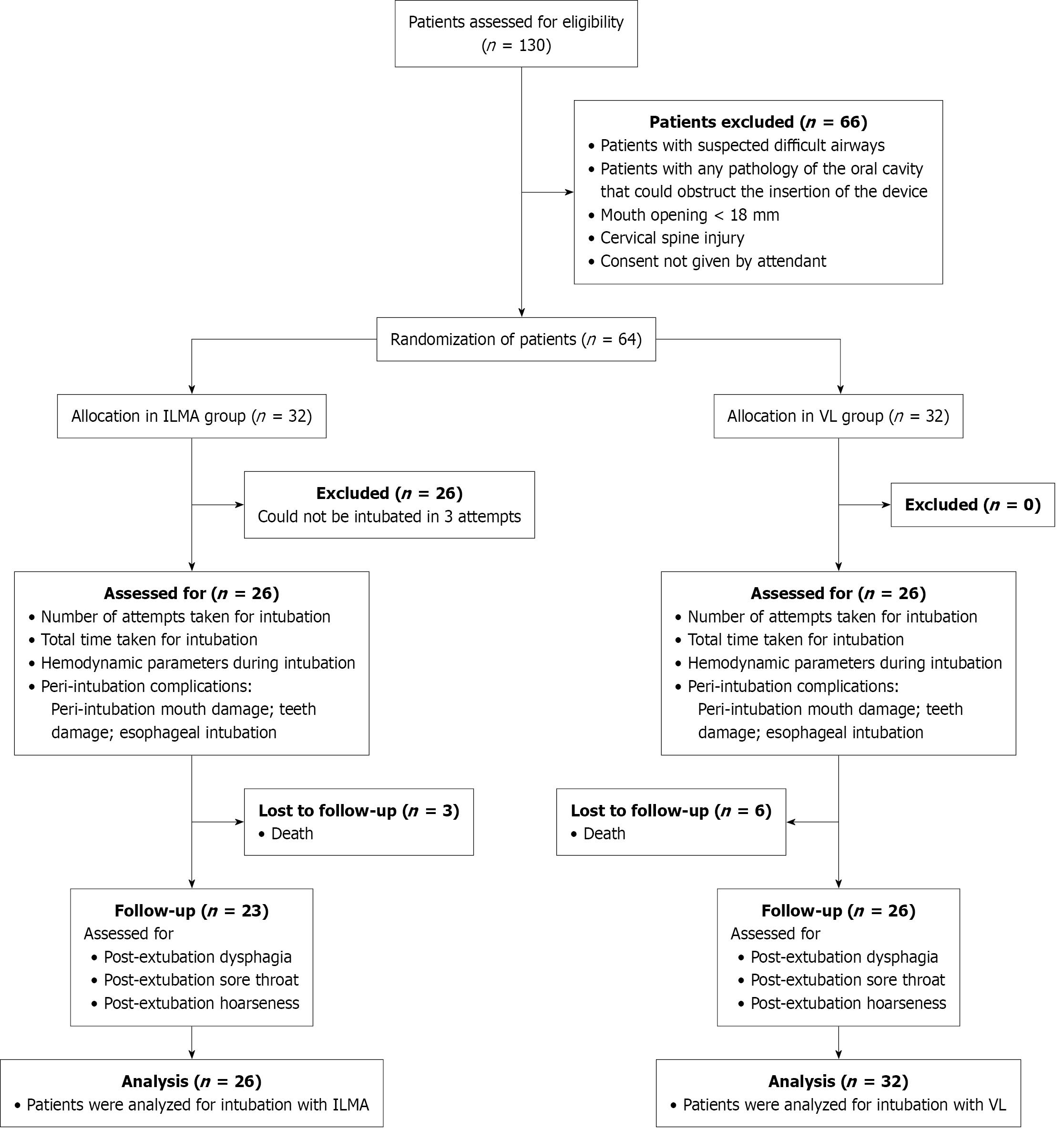
From 130 patients initially assessed for eligibility, 64 met the inclusion criteria and were randomized equally into the VL and ILMA groups (Figure 1). In the ILMA group 6 patients were excluded due to unsuccessful intubation after three attempts. Additionally, 3 patients in the ILMA group and 6 patients in the VL group were lost to follow-up. As a result, the final intention-to-treat analysis included 26 patients in the ILMA group and 32 patients in the VL group.
The study groups demonstrated comparable demographic profiles (Table 1). The mean age in the VL group was 53.9 ± 19.5 years vs 56.6 ± 15.0 years in the ILMA group (P = 0.535). The VL group consisted of 62.5% males, whereas 53.1% of the ILMA group was male. The sex ratio in the VL and ILMA groups was statistically insignificant (P = 0.448). Anthropometric measures showed no significant differences in height, weight, or body mass index (P > 0.05 for all).
| Characteristic | Video laryngoscope group (n = 32) | Intubating laryngeal mask airway group (n = 32) | P value |
| Age (years) (mean ± SD) | 56.63 ± 15.0 | 53.91 ± 19.5 | 0.535 |
| Male sex | 20 (62.5) | 17 (53.1) | 0.448 |
| Body mass index (kg/m²) (mean ± SD) | 23.9 ± 3.5 | 25.3 ± 3.1 | 0.098 |
| Comorbidities | |||
| Type 2 diabetes mellitus | 9 (28.1) | 3 (9.4) | 0.055 |
| Hypertension | 13 (40.6) | 13 (40.6) | 1.000 |
| Chronic obstructive pulmonary disease | 11 (34.4) | 6 (18.8) | 0.157 |
| Stroke | 1 (3.1) | 3 (9.4) | 0.302 |
| Acute coronary syndrome | 4 (12.5) | 2 (6.2) | 0.391 |
Comorbidity prevalence was similar between the groups except for a trend toward higher type 2 diabetes mellitus in the VL group (28.1% vs 9.4%, P = 0.055) (Table 1). Airway characteristics including thyromental distance, sternomental distance, inter-incisor distance, and neck circumference showed no significant differences (P > 0.05). Mallampati scores and mandibular protrusion classification were similarly distributed (Table 2).
| Parameter | Video laryngoscope group (n = 23) | Intubating laryngeal mask airway group (n = 22) | P value |
| Thyromental distance (cm) (mean ± SD) | 6.79 ± 0.25 | 6.77 ± 0.18 | 0.780 |
| Sternomental distance (cm) (mean ± SD) | 12.72 ± 0.17 | 12.77 ± 0.15 | 0.287 |
| Interincisor distance (cm) (mean ± SD) | 4.40 ± 0.26 | 4.37 ± 0.22 | 0.647 |
| Neck circumference (cm) (mean ± SD) | 30.56 ± 5.1 | 30.50 ± 5.4 | 0.962 |
| Mallampati score | 0.667 | ||
| Class I | 4 (17.4) | 6 (27.3) | |
| Class II | 7 (30.4) | 7 (31.8) | |
| Class III | 12 (52.2) | 9 (40.9) | |
| Easy mask ventilation | 22 (68.8) | 15 (46.9) | > 0.050 |
| Mandibular protrusion | 0.316 | ||
| A | 20 (87.0) | 21 (95.5) | |
| B | 3 (13.0) | 1 (4.5) |
The VL group demonstrated superior first-attempt success rates (87.5% vs 53.1%, P = 0.009). The ILMA group required more multiple attempts (21.9% requiring 2 attempts vs 12.5% in VL) and had 18.8% unsuccessful intubations compared with none in the VL group (Table 3). VL significantly reduced procedural times compared with the ILMA. Device insertion time was shorter with VL (18.8 ± 10.2 seconds vs 24.9 ± 8.1 seconds, P = 0.015), and intubation time was markedly faster in the VL group (25.6 ± 14.5 seconds vs 57.2 ± 14.7 seconds, P < 0.001). Consequently, the total intubation time was nearly halved with VL (44.0 ± 19.7 seconds vs 82.5 ± 14.5 seconds, P < 0.001), highlighting its efficiency in accelerating airway management (Table 4).
| Outcome | Video laryngoscope group (n = 32) | Intubating laryngeal mask airway group (n = 32) | P value |
| First-attempt success | 28 (87.5) | 17 (53.1) | 0.009 |
| Attempts distribution | 0.009 | ||
| 1 attempt | 28 (87.5) | 17 (53.1) | |
| 2 attempts | 4 (12.5) | 7 (21.9) | |
| 3 attempts | 0 (0) | 2 (6.2) | |
| Failed intubation | 0 (0) | 6 (18.8) |
| Airway management values of patients | Video laryngoscope group (n = 32) | Intubating laryngeal mask airway group (n = 26) | P value |
| Insertion time (seconds) | 18.75 ± 10.2 | 24.92 ± 8.1 | t = -2.497; P = 0.015 |
| Intubation time (seconds) | 25.63 ± 14.5 | 57.2 ± 14.7 | t = -8.212; P ≤ 0.001 |
| Total intubation time (seconds) | 44.0 ± 19.7 | 82.5 ± 14.5 | t = 8.56; P ≤ 0.001 |
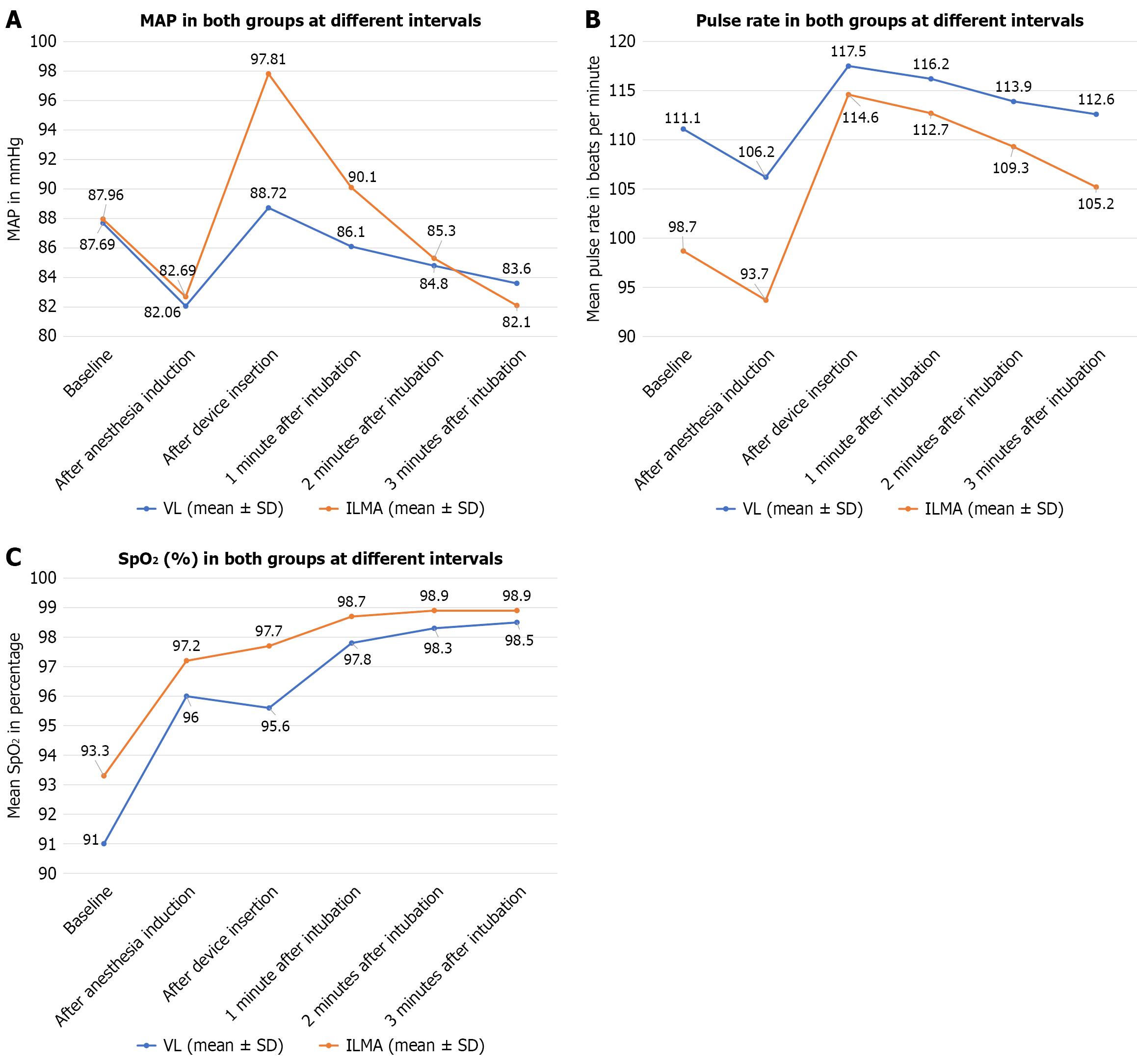
The ILMA group required significantly more airway maneuvers (57.7% vs 25.0%, P = 0.011) (Table 5). Hemodynamic stability was maintained in both groups with no significant differences in mean arterial pressure at any measured time point (Figure 2A). Pulse rate showed a transient elevation in the VL group post-induction (106.2 ± 25.1 vs 93.7 ± 21.3, P = 0.048), but there were no other significant differences (Figure 2B). Oxygen saturation remained comparable throughout the procedure in both groups (Table 6, Figure 2C).
| Maneuver | Video laryngoscope group (n = 32) | Intubating laryngeal mask airway group (n = 26) | P value |
| Present | 8 (25.0) | 15 (57.7) | χ2 = 6.407; df = 1; P = 0.011 |
| Absent | 24 (75.0) | 11 (42.3) |
| Oxygen saturation (%) | Video laryngoscope group (n = 32) | Intubating laryngeal mask airway group (n = 26) | P value |
| Baseline | 91.0 ± 9.7 | 93.3 ± 7.7 | t = -1.015; P = 0.315 |
| After anesthesia induction | 96.0 ± 6.4 | 97.2 ± 3.7 | t = -0.843; P = 0.403 |
| After device insertion | 95.6 ± 6.5 | 97.7 ± 3.8 | t = -1.470; P = 0.147 |
| 1 minute after intubation | 97.8 ± 4.6 | 98.7 ± 2.7 | t = -0.885; P = 0.380 |
| 2 minutes after intubation | 98.3 ± 4.2 | 98.9 ± 2.5 | t = -0.573; P = 0.569 |
| 3 minutes after intubation | 98.5 ± 3.8 | 98.9 ± 2.5 | t = -0.450; P = 0.654 |
The ILMA group showed higher rates of several complications (Table 7). Peri-intubation mouth damage was sig
| Complication | Video laryngoscope group (n = 32) | Intubating laryngeal mask airway group (n = 26) | P value |
| Peri-intubation mouth damage | 0 (0.0) | 7 (26.9) | χ2 = 9.798; df = 1; P = 0.002 |
| Post-extubation dysphagia | 0 (0.0) | 0 (0.0) | NA |
| Post-extubation sore throat | 1 (3.1) | 7 (26.9) | χ2 = 6.832; df = 1; P = 0.009 |
| Peri-intubation teeth damage | 0 (0.0) | 0 (0.0) | NA |
| Post-extubation hoarseness | 1 (3.1) | 3 (11.5) | χ2 = 1.581; df = 1; P = 0.209 |
| Peri-intubation esophageal intubation | 1 (3.1) | 2 (7.7) | χ2 = 0.610; df = 1; P = 0.435 |
This comprehensive randomized controlled trial provided critical insights into the comparative effectiveness of VL vs ILMA for emergency ETI in patients who were critically ill. Our findings contributed substantially to the evolving understanding of optimal airway management strategies in high-acuity settings with important implications for clinical practice, training protocols, and patient outcomes.
The most striking findings of our study related to the superior performance of VL in both first-attempt success rates and time to successful intubation. The 87.5% first-attempt success rate with VL compared with 53.1% with ILMA (P = 0.009) represents a clinically significant difference that could substantially impact patient care in emergency situations. This advantage persisted throughout multiple attempts with no failed intubations in the VL group compared with an 18.8% failure rate with ILMA after three attempts.
The time differential between devices was particularly noteworthy. VL demonstrated significantly shorter insertion times (18.8 ± 10.2 seconds vs 24.9 ± 8.1 seconds, P = 0.015), intubation times (25.6 ± 14.5 seconds vs 57.2 ± 14.7 seconds, P < 0.001), and total intubation times (44.0 ± 19.7 seconds vs 82.5 ± 14.5 seconds, P < 0.001). These time savings assume critical importance in emergency airway management in which rapid oxygenation and ventilation are paramount. The nearly 40-s average difference in total intubation time could prove lifesaving in scenarios such as cardiac arrest, severe hypoxia, or traumatic brain injury in which every second of apnea time contributes to potential morbidity.
Our findings aligned with several recent studies comparing advanced airway devices. Jakhar et al[14] reported similar success rate differentials (96.97% for VL vs 81.25% for ILMA) in patients undergoing cervical spine surgery. The time advantage we observed was consistent with multiple previous reports, including Özdil et al[15] who found ILMA intubation times approximately double those of GlideScope (85.6 ± 13.0 seconds vs 43.5 ± 13.0 seconds, P < 0.0001). This consistency across study populations and settings strengthens the validity of our findings and suggests they may be generalizable to broader critical care contexts.
The superior performance of VL likely stems from several fundamental design and operational characteristics.
Direct visualization: VL provides real-time, magnified visualization of glottic structures, eliminating the need for perfect alignment of anatomical axes. This contrasts with the reliance of ILMA on blind insertion and tactile feedback that becomes particularly challenging in emergency situations with potential airway edema, secretions, or anatomical abnormalities.
Learning curve: While both devices require training, VL may offer a more intuitive interface for clinicians already familiar with DL. The ability to share the visual field among team members during emergency intubation represents another advantage in high-stress situations.
Maneuver requirements: Our finding that ILMA required significantly more adjunctive maneuvers (57.7% vs 25.0%, P = 0.011) highlighted the technical challenges of blind insertion techniques. The frequent need for Chandy’s maneuvers or device repositioning with ILMA contributed to both prolonged intubation times and increased risk of complications[12].
Patient factors: Patients who are critically ill often present with physiological challenges (e.g., airway edema, obesity, limited cervical mobility) that may disproportionately affect ILMA performance. The maintained advantage of VL across our study population suggests its robustness in diverse clinical scenarios.
An important finding of our study was the comparable hemodynamic profile between devices. Despite the more rapid intubation times with VL, we observed no significant differences in mean arterial pressure at any measured time point. Pulse rate showed only a transient elevation in the VL group post-induction (106.2 ± 25.1 vs 93.7 ± 21.3, P = 0.048) with no lasting differences.
This finding contrasts with some previous reports suggesting VL might produce greater hemodynamic responses due to more vigorous manipulation[16,17]. Our data suggested that any such effect is either minimal or offset by the shorter duration of airway manipulation with VL. The maintenance of oxygen saturation in both groups (with no desaturation events) likely reflects our rigorous preoxygenation protocol and the three-attempt limit for any single device.
The hemodynamic stability observed with both devices is particularly reassuring for patients who are critically ill and may have limited physiological reserve. This finding supports the safety of VL in patients who are hemodynamically unstable in which concerns about pressor responses might otherwise favor supraglottic devices.
Our complication data revealed significant differences between the devices that warrant careful consideration.
Tissue trauma: The complete absence of mouth damage in the VL group compared with 26.9% with ILMA (P = 0.002) represents a major safety advantage. This aligns with Jakhar et al[14] who observed increased soft tissue injuries with ILMA, likely due to blind insertion techniques and frequent repositioning requirements.
Post-intubation morbidity: The significantly higher incidence of sore throat with ILMA (26.9% vs 3.1%, P = 0.009) has important implications for patient comfort and recovery, particularly in patients requiring prolonged mechanical ventilation.
Esophageal intubation: While not statistically significant in our study (3.1% VL vs 7.7% ILMA), the numerical difference in esophageal intubation rates merits attention given the potentially catastrophic consequences of unrecognized esopha
The superior safety profile of VL reinforces its appropriateness as a first-line device for emergency airway manage
Our results both confirmed and extended previous research in this area.
Success rates: The first-attempt success advantage we observed with VL (87.5%) was consistent with multiple previous studies although the magnitude of difference varied[18,19]. Jiang et al[20] conducted a meta-analysis and found that VL improved first-attempt success across diverse patient populations, supporting our findings.
Time efficiency: Our time savings with VL aligned with the report by Özdil et al[15] in which there were significantly shorter intubation times with GlideScope vs ILMA. The consistency of this finding across studies suggested that it represented a true advantage of VL rather than a study-specific artifact.
Complications: The reduced complication rate with VL matches previous reports of decreased airway trauma with video-assisted techniques. This safety advantage appears robust across different VL models and clinical settings. Interestingly, some studies in specific populations (e.g., patients with obesity) have found more modest differences between devices. This highlights the importance of context in device selection and suggests the advantages of VL may be most pronounced in emergency general critical care populations[13].
Based on our findings, we propose several evidence-based recommendations for clinical practice.
First-line device selection: VL should be considered the preferred first-line device for emergency intubation in critical care settings, given its superior first-attempt success rates, faster intubation times, and reduced complication rates.
Rescue strategy planning: ILMA remains an important backup device and should be immediately available when VL is used as the primary approach. Our 18.8% ILMA failure rate after three attempts underscores the need for alternative strategies when both devices fail.
Training considerations: The significant performance differences we observed suggest that VL training should be prioritized in critical care airway management curricula. However, maintaining proficiency with ILMA remains important for rescue scenarios.
Protocol development: Institutional airway management protocols should account for the demonstrated advantages of VL, particularly in time-sensitive emergency scenarios where rapid airway securement is critical.
Resource allocation: Hospitals should consider the cost-benefit implications of our findings when allocating resources for airway equipment. While VL systems represent a significant investment, their performance advantages may justify the expenditure through improved patient outcomes and reduced complication-related costs.
While our study provided compelling evidence supporting VL use in emergency intubation, several limitations must be acknowledged.
Single-center design: Conducted at a tertiary care center, our results may not fully generalize to smaller hospitals or resource-limited settings.
Sample size constraints: While adequately powered for our primary outcomes, the sample size limited our ability to detect differences in rarer complications or perform meaningful subgroup analyses.
Operator factors: All intubations were performed by a single operator who had experience of using the devices in more than 25 patients, potentially limiting applicability to less experienced clinicians.
Exclusion of patients with difficult airways: The exclusion of patients with difficult airways in our study may limit the generalizability of our findings to real-world clinical scenarios in which such cases are frequently encountered. Future studies including patients with difficult airways are needed to validate these outcomes across a broader spectrum of clinical situations.
Device-specific considerations: We evaluated specific VL and ILMA models; performance characteristics may vary with other devices in these categories.
These limitations suggest several important directions for future research.
Multicenter studies: Larger, multicenter trials could validate our findings across diverse practice settings and patient populations.
Long-term outcomes: Research examining longer-term outcomes (e.g., ventilator-associated pneumonia, ICU length of stay) related to intubation method would provide valuable supplementary data.
Cost-effectiveness analyses: Formal economic evaluations comparing VL and ILMA would help inform resource allocation decisions.
Novice operator studies: Research focusing on less experienced providers could clarify the learning curve differences between devices.
Special populations: Dedicated studies in specific high-risk groups (e.g., patients with obesity, trauma, or obstetric-related issues) would help refine device selection algorithms.
This randomized controlled trial provided robust evidence supporting VL as the preferred method for emergency ETI in patients who were critically ill. The demonstrated advantages in first-attempt success rates, procedural efficiency, and complication profiles suggested that VL should be considered first-line in emergency airway management protocols. While ILMA remains an important rescue device, its inferior performance in our study supported a secondary role in most emergency scenarios. The findings of this study contributed meaningfully to the growing body of evidence guiding optimal airway management in critical care. As technology continues to evolve, ongoing research will be essential to refine device selection criteria and optimize patient outcomes. However, the current evidence strongly supports the preferential use of VL for emergency intubation in adult patients who are critically ill.
| 1. | Levitan RM, Heitz JW, Sweeney M, Cooper RM. The complexities of tracheal intubation with direct laryngoscopy and alternative intubation devices. Ann Emerg Med. 2011;57:240-247. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 117] [Cited by in RCA: 128] [Article Influence: 8.5] [Reference Citation Analysis (1)] |
| 2. | Lee LC. Two curves theory does not clearly explain laryngoscopy and intubation. Br J Anaesth. 2011;106:909-10; author reply 910. [PubMed] [DOI] [Full Text] |
| 3. | Heuer JF, Barwing TA, Barwing J, Russo SG, Bleckmann E, Quintel M, Moerer O. Incidence of difficult intubation in intensive care patients: analysis of contributing factors. Anaesth Intensive Care. 2012;40:120-127. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 36] [Article Influence: 2.6] [Reference Citation Analysis (1)] |
| 4. | Russotto V, Myatra SN, Laffey JG, Tassistro E, Antolini L, Bauer P, Lascarrou JB, Szuldrzynski K, Camporota L, Pelosi P, Sorbello M, Higgs A, Greif R, Putensen C, Agvald-Öhman C, Chalkias A, Bokums K, Brewster D, Rossi E, Fumagalli R, Pesenti A, Foti G, Bellani G; INTUBE Study Investigators. Intubation Practices and Adverse Peri-intubation Events in Critically Ill Patients From 29 Countries. JAMA. 2021;325:1164-1172. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 127] [Cited by in RCA: 416] [Article Influence: 83.2] [Reference Citation Analysis (5)] |
| 5. | De Jong A, Rolle A, Molinari N, Paugam-Burtz C, Constantin JM, Lefrant JY, Asehnoune K, Jung B, Futier E, Chanques G, Azoulay E, Jaber S. Cardiac Arrest and Mortality Related to Intubation Procedure in Critically Ill Adult Patients: A Multicenter Cohort Study. Crit Care Med. 2018;46:532-539. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 111] [Cited by in RCA: 171] [Article Influence: 24.4] [Reference Citation Analysis (1)] |
| 6. | De Jong A, Molinari N, Terzi N, Mongardon N, Arnal JM, Guitton C, Allaouchiche B, Paugam-Burtz C, Constantin JM, Lefrant JY, Leone M, Papazian L, Asehnoune K, Maziers N, Azoulay E, Pradel G, Jung B, Jaber S; AzuRéa Network for the Frida-Réa Study Group. Early identification of patients at risk for difficult intubation in the intensive care unit: development and validation of the MACOCHA score in a multicenter cohort study. Am J Respir Crit Care Med. 2013;187:832-839. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 202] [Cited by in RCA: 225] [Article Influence: 17.3] [Reference Citation Analysis (4)] |
| 7. | Guitton C, Ehrmann S, Volteau C, Colin G, Maamar A, Jean-Michel V, Mahe PJ, Landais M, Brule N, Bretonnière C, Zambon O, Vourc'h M. Nasal high-flow preoxygenation for endotracheal intubation in the critically ill patient: a randomized clinical trial. Intensive Care Med. 2019;45:447-458. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 95] [Cited by in RCA: 87] [Article Influence: 12.4] [Reference Citation Analysis (1)] |
| 8. | Steel A. The intubating laryngeal mask airway. Emerg Med J. 2005;22:47-49. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 6] [Article Influence: 0.3] [Reference Citation Analysis (1)] |
| 9. | Cinar O, Cevik E, Yildirim AO, Yasar M, Kilic E, Comert B. Comparison of GlideScope video laryngoscope and intubating laryngeal mask airway with direct laryngoscopy for endotracheal intubation. Eur J Emerg Med. 2011;18:117-120. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 16] [Article Influence: 1.1] [Reference Citation Analysis (1)] |
| 10. | Driver BE, Prekker ME, Klein LR, Reardon RF, Miner JR, Fagerstrom ET, Cleghorn MR, McGill JW, Cole JB. Effect of Use of a Bougie vs Endotracheal Tube and Stylet on First-Attempt Intubation Success Among Patients With Difficult Airways Undergoing Emergency Intubation: A Randomized Clinical Trial. JAMA. 2018;319:2179-2189. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 157] [Cited by in RCA: 220] [Article Influence: 27.5] [Reference Citation Analysis (5)] |
| 11. | Arulkumaran N, Lowe J, Ions R, Mendoza M, Bennett V, Dunser MW. Videolaryngoscopy versus direct laryngoscopy for emergency orotracheal intubation outside the operating room: a systematic review and meta-analysis. Br J Anaesth. 2018;120:712-724. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 72] [Cited by in RCA: 114] [Article Influence: 14.3] [Reference Citation Analysis (1)] |
| 12. | Sarma R, Kumar R, Kumar NG, Agarwal M, Bhardwaj M, Ansari SA, Deepak GP. Comparative evaluation of Intubating Laryngeal Mask Airway (ILMA), I-gel and Ambu AuraGain for blind tracheal intubation in adults. J Anaesthesiol Clin Pharmacol. 2022;38:130-136. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (1)] |
| 13. | Turna CK, Arslan ZI, Alparslan V, Okyay K, Solak M. [Comparison of channelled videolaryngoscope and intubating laryngeal mask airway for tracheal intubation in obese patients: a randomised clinical trial]. Braz J Anesthesiol. 2020;70:118-124. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 4] [Article Influence: 0.7] [Reference Citation Analysis (1)] |
| 14. | Jakhar R, Saigal D, Kale S, Aggarwal S. Comparison of Videolaryngoscope and Intubating Laryngeal Mask Airway for Tracheal Intubation with Manual-in-line Stabilization in Patients Undergoing Cervical Spine Surgery. Anesth Essays Res. 2020;14:485-491. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 9] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 15. | Özdil S, Arslan Aydın Zİ, Baykara ZN, Toker K, Solak ZM. Tracheal intubation in patients immobilized by a rigid collar: a comparison of GlideScope and an intubating laryngeal mask airway. Turk J Med Sci. 2016;46:1617-1623. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 9] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 16. | Ardak Z TL, Arslan ZP, Cesur S, Aksu B. Comparison of haemodynamic response to tracheal intubation with two different videolaryngoscopes: A randomized clinical trial. Braz J Anesthesiol. 2023;73:548-555. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 3] [Article Influence: 1.0] [Reference Citation Analysis (1)] |
| 17. | Buhari FS, Selvaraj V. Randomized controlled study comparing the hemodynamic response to laryngoscopy and endotracheal intubation with McCoy, Macintosh, and C-MAC laryngoscopes in adult patients. J Anaesthesiol Clin Pharmacol. 2016;32:505-509. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 11] [Article Influence: 1.1] [Reference Citation Analysis (1)] |
| 18. | Raja R, Gupta S, Mehta N, Attal P. First-pass Success Rate and Number of Attempts Required for Intubation in Anticipated Difficult Airway: Comparison between Macintosh and Channeled King Vision Video Laryngoscopes. Anesth Essays Res. 2022;16:340-344. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 19. | Dharanindra M, Jedge PP, Patil VC, Kulkarni SS, Shah J, Iyer S, Dhanasekaran KS. Endotracheal Intubation with King Vision Video Laryngoscope vs Macintosh Direct Laryngoscope in ICU: A Comparative Evaluation of Performance and Outcomes. Indian J Crit Care Med. 2023;27:101-106. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 9] [Article Influence: 3.0] [Reference Citation Analysis (1)] |
| 20. | Jiang J, Ma DX, Li B, Wu AS, Xue FS. Videolaryngoscopy versus direct laryngoscopy for nasotracheal intubation: A systematic review and meta-analysis of randomised controlled trials. J Clin Anesth. 2019;52:6-16. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 23] [Article Influence: 2.9] [Reference Citation Analysis (1)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/