Published online Mar 9, 2026. doi: 10.5409/wjcp.v15.i1.114242
Revised: October 14, 2025
Accepted: December 2, 2025
Published online: March 9, 2026
Processing time: 171 Days and 14.9 Hours
Umbilical venous catheterisation (UVC) is frequently used in neonates but may be complicated by malposition or migration. Extravasation is rare and can mimic other abdominal pathologies.
We report a preterm infant, born at 27 weeks’ gestation, who developed bilateral pneumothorax and spontaneous intestinal perforation requiring drainage. On day 8, the infant clinically deteriorated with persistent high-volume clear peritoneal drain output and worsening dehydration despite fluid escalation. Abdominal radiography confirmed UVC migration into the liver with possible extravasation. Following catheter removal, peritoneal drainage reduced dramatically, and the infant improved rapidly. He was discharged at 38 weeks’ corrected age and remained well with age-appropriate development.
UVC extravasation can masquerade as high-output peritoneal drainage in the setting of intestinal perforation, thereby delaying diagnosis. Persistent, unusually high peritoneal drainage should prompt consideration of catheter leakage. This rare presentation expands the spectrum of UVC-related complications described in the literature and emphasizes the importance of prompt recognition and management.
Core Tip: We describe the first case of umbilical venous catheterization extravasation masquerading as high-output peritoneal drainage in the context of spontaneous intestinal perforation. Unlike typical presentations of abdominal distension or metabolic derangements, our patient exhibited persistently clear drain output, delaying diagnosis. Radiographic confirmation and prompt catheter removal led to rapid recovery. This case underscores the need for vigilance, early imaging, and multidisciplinary collaboration when managing unexplained peritoneal drainage in preterm infants with central lines.
- Citation: Kumar A, Sidaraddi S, Patil P, Ghawade AP, Moralwar P, Pillai A. Not all that drains is gut - umbilical venous catheter extravasation masquerading as intestinal perforation: A case report. World J Clin Pediatr 2026; 15(1): 114242
- URL: https://www.wjgnet.com/2219-2808/full/v15/i1/114242.htm
- DOI: https://dx.doi.org/10.5409/wjcp.v15.i1.114242
Umbilical venous catheterisation (UVC) is a common procedure in neonatal intensive care units (NICU). It is quick to perform, requires less technical expertise compared to peripherally inserted central catheters, and allows safe delivery of total parenteral nutrition and hyperosmolar fluids[1]. Correct placement of the UVC tip, at the junction of the inferior vena cava and right atrium, is essential to avoid complications, and is usually confirmed radiographically[2]. Migration or malposition of the catheter may lead to serious complications, including vascular, hepatic, and gastrointestinal injuries[2,3]. We report a preterm neonate with spontaneous intestinal perforation in whom UVC migration led to the rare and unexpected presentation of markedly elevated peritoneal drain output. Prompt recognition and management were life-saving for this extremely low birth weight infant.
The infant was born at 27 weeks’ gestation with a birth weight of 890 g via emergency caesarean section in view of prolonged preterm premature rupture of membranes and anhydramnios.
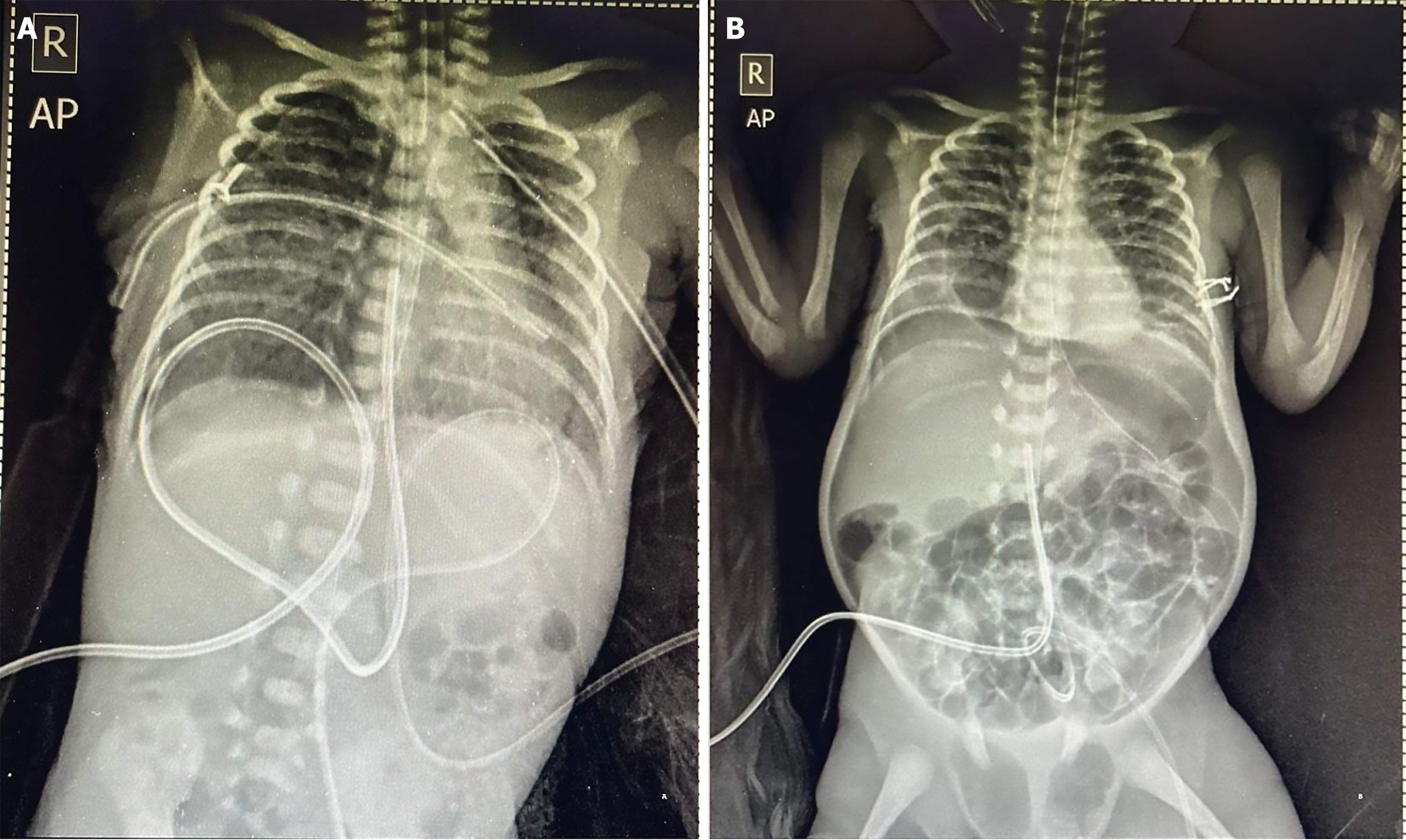
The neonate had poor respiratory drive at birth and required ventilation and surfactant therapy. Umbilical venous access was secured, and total parenteral nutrition was initiated soon after admission to the NICU. The UVC was confirmed to be in the central position by radiograph (body of T8 vertebra) (Figure 1A). The catheter was then sutured in place, and additional tape was used to further secure the catheter to the infant’s abdomen. At around 3 hours of life, the infant developed desaturation episodes with reduced air entry on auscultation. Chest radiography revealed a right-sided pneumothorax, for which an intercostal drain was inserted. Soon, the infant developed a left-sided pneumothorax, requiring insertion of a left intercostal drain.
Since it is a newborn, there is no past medical history.
Since it is a newborn, there is no personal or family history.
Respiratory status improved on ventilator support over the next few days. Feeds were not initiated in view of dark brown gastric aspirates noted from the orogastric tube. On day 7, the infant developed acute abdominal distension with fluctuating oxygen saturation. Transillumination was suggestive of pneumoperitoneum, for which a peritoneal glove drain was inserted, resulting in drainage of gas and around 3 mL of serous fluid. Abdominal radiograph confirmed pneumoperitoneum and outward migration of UVC (L1-L2 vertebra level), with a straight course (Figure 1B). Since the baby was unstable and had poor perfusion, establishing a new vascular access was difficult. Lipid infusion was stopped, and calcium was removed from the parenteral fluid. Partial parenteral nutrition with dextrose, amino acids, and electrolytes was continued through the low-lying UVC. It was planned to insert a new peripherally inserted central catheter after 1-2 days, once the neonate was stable. Neonate improved clinically post insertion of the glove drain.
Blood test performed on day 7 showed sodium 135 mEq/L, potassium 4.2 mEq/L, and glucose 78 mg/dL. There was minimal peritoneal drain (total 2 mL) over the next 24 hours. However, on day 8, around 30 hours post the drain insertion, the peritoneal drain volume started increasing (30 mL in 24 hours). In response, the total parenteral fluid volume was increased. Repeat blood tests showed sodium 132 mEq/L, potassium 3.9 mEq/L, and sugar level 64 mg/dL. However, by the next day, the peritoneal drain output had increased to 120 mL/day. The fluid was clear, and over the next 24 hours, the drain output further increased in proportion to the escalation of parenteral fluids. The neonate started showing signs of dehydration and low blood sugar levels. Blood tests revealed hyponatremia (sodium 127 mEq/L), potassium level 3.6 mEq/L, and borderline-low sugar levels (48 mg/dL).
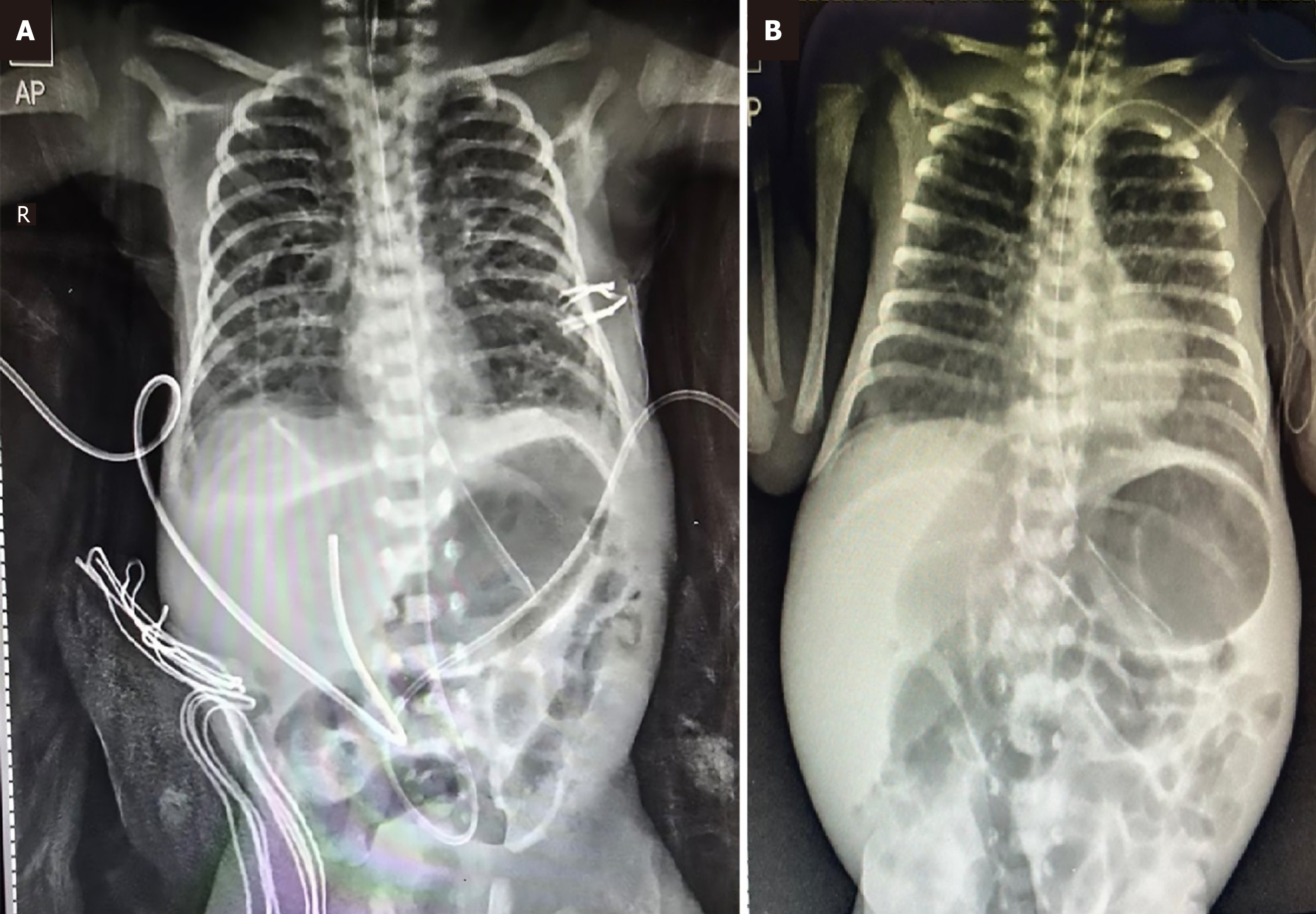
Repeat abdominal radiograph on day 8 confirmed further UVC migration into the liver (Figure 2A). An abdominal ultrasound was performed, which showed deviation of the UVC tip toward the portal vein along with inflammation/edema of the surrounding liver parenchyma. Blood tests showed elevated alanine transaminase levels of 129 U/L, with other liver function tests showing normal results.
These findings supported the possibility of total parenteral nutrition extravasation secondary to UVC migration.
The UVC was promptly removed, and fluid replacement was provided with a peripheral intravenous catheter. Within 12 hours of removing the UVC, the peritoneal drain output reduced. Parenteral nutrition was provided by a peripherally inserted central catheter inserted over the left arm (Figure 2B). Over the next three days, the intestinal perforation healed, and the glove drain could be removed. Feeds were initiated the following week, and the neonate had a smooth NICU course thereafter. Blood reports, including alanine transaminase levels, normalized after one week.
The neonate was discharged at 38 weeks corrected gestational age. At 9 months of age, he demonstrated age-appropriate developmental milestones and is on regular follow-up. No abnormalities in liver function were observed at 9 months of age.
Umbilical venous catheterization remains an indispensable intervention in the management of critically ill neonates, providing reliable central access for fluid resuscitation, parenteral nutrition, and medications. Although generally safe, UVCs are prone to malposition and migration, particularly in preterm infants, due to vessel fragility and anatomical variability[4]. The UVC has a dwell time of 7-10 days, reducing the need for invasive, painful vascular procedures[5]. A prospective study of 65 preterm infants showed that UVC tip migration occurred in 50% of neonates at any time during the first week[6]. Migration of UVC may result in complications, including hepatic parenchymal injury, vascular perforation, and extravasation of infusate[7-9]. Neonatal cases of UVC extravasation presenting with ascites and electrolyte imbalance have been described[10,11], but the co-existence of spontaneous intestinal perforation has not been previously reported as a diagnostic confounder.
In our patient, the simultaneous presence of an intraperitoneal drain obscured the clinical picture, leading to a delay in recognizing UVC extravasation. The neonate first developed pneumoperitoneum on day of life 7, for which glove drain insertion was performed at bedside. After the abdominal drain insertion, only 2 mL of fluid was obtained for the first 24 hours, with predominantly air drainage. During this period, the abdominal distension improved, and the neonate had normal blood sugar and electrolytes. Approximately 30 hours after the glove drain insertion, the peritoneal drain output started increasing, likely due to UVC extravasation. The following day (day of life 9), drain output increased significantly, leading to hypoglycemia, dehydration, and decreased urine output. This could be related to displacement of the UVC tip, resulting in vessel injury and subsequent leakage of infusate into the peritoneal cavity. Unlike previously reported cases, where extravasation typically presented with progressive abdominal distension, fluid retention, or metabolic derangements[12], our neonate exhibited persistently high-output clear peritoneal drainage. Edison et al[12] reported a premature baby that presented on day 7 of life with abdominal distension and migration of UVC to below the T10 level. Abdominal radiograph was suspicious of ascites, and aspiration revealed around 100 mL of milky peritoneal fluid[12]. In our case, due to the presence of a peritoneal drain, we noted the high peritoneal drain output that mimicked an ongoing gastrointestinal pathology and contributed to diagnostic uncertainty. Ultimately, the combination of excessive drain output and refractory dehydration despite fluid replacement raised suspicion of catheter leakage, which was confirmed by radiography and ultrasound. Prompt catheter removal resulted in rapid clinical improvement, underscoring the reversibility of this complication when identified early.
This case highlights several key learning points. First, persistent or disproportionately high peritoneal drainage in neonates should raise suspicion, even in the presence of concomitant gastrointestinal pathology. Second, prompt use of radiography to recheck catheter position is critical, particularly when the clinical course deviates from expectations. The potential role of ultrasound as a valuable adjunct for initial confirmation and subsequent assessment of catheter tip position also needs to be explored. Finally, multidisciplinary collaboration among neonatologists, radiologists, and surgeons is vital to avoid morbidity and ensure timely intervention.
To our knowledge, this is the first reported case of UVC extravasation masquerading as high-output peritoneal drainage in the setting of spontaneous intestinal perforation. Recognition of this rare presentation expands the spectrum of UVC-related complications described in the literature and emphasizes the importance of vigilance in the ongoing care of preterm neonates with central lines.
| 1. | Anderson J, Leonard D, Braner DA, Lai S, Tegtmeyer K. Videos in clinical medicine. Umbilical vascular catheterization. N Engl J Med. 2008;359:e18. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 57] [Cited by in RCA: 56] [Article Influence: 3.1] [Reference Citation Analysis (1)] |
| 2. | Schlesinger AE, Braverman RM, DiPietro MA. Pictorial essay. Neonates and umbilical venous catheters: normal appearance, anomalous positions, complications, and potential aid to diagnosis. AJR Am J Roentgenol. 2003;180:1147-1153. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 72] [Cited by in RCA: 45] [Article Influence: 2.0] [Reference Citation Analysis (1)] |
| 3. | Goh SSM, Kan SY, Bharadwaj S, Poon WB. A review of umbilical venous catheter-related complications at a tertiary neonatal unit in Singapore. Singapore Med J. 2021;62:29-33. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 18] [Article Influence: 3.6] [Reference Citation Analysis (1)] |
| 4. | Yeung CY. Complications of umbilical venous catheters in neonates: A safety reappraisal. Pediatr Neonatol. 2020;61:1-2. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 13] [Article Influence: 2.2] [Reference Citation Analysis (1)] |
| 5. | Hess S, Poryo M, Ruckes C, Papan C, Ehrlich A, Ebrahimi-Fakhari D, Bay JS, Wagenpfeil S, Simon A, Meyer S. Assessment of an umbilical venous catheter dwell-time of 8-14 days versus 1-7 days in very low birth weight infacts (UVC - You Will See): a pilot single-center, randomized controlled trial. Early Hum Dev. 2023;179:105752. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 15] [Reference Citation Analysis (1)] |
| 6. | Franta J, Harabor A, Soraisham AS. Ultrasound assessment of umbilical venous catheter migration in preterm infants: a prospective study. Arch Dis Child Fetal Neonatal Ed. 2017;102:F251-F255. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 59] [Article Influence: 6.6] [Reference Citation Analysis (1)] |
| 7. | Gibson K, Smith A, Sharp R, Ullman A, Morris S, Esterman A. Adverse events associated with umbilical vascular catheters in the neonatal intensive care unit: A retrospective cohort study. Aust Crit Care. 2024;37:747-754. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 11] [Article Influence: 5.5] [Reference Citation Analysis (1)] |
| 8. | Dubbink-Verheij GH, Visser R, Tan RNGB, Roest AAW, Lopriore E, Te Pas AB. Inadvertent Migration of Umbilical Venous Catheters Often Leads to Malposition. Neonatology. 2019;115:205-210. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 22] [Article Influence: 3.1] [Reference Citation Analysis (1)] |
| 9. | Perl JR, Crabtree-Beach T, Olyaei A, Hedges M, Jordan BK, Scottoline B. Reducing umbilical catheter migration rates by using a novel securement device. J Perinatol. 2024;44:1359-1364. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (1)] |
| 10. | Egyepong J, Jain A, Chow P, Godambe S. Parenteral nutrition--ascites with acute renal failure as a complication from an umbilical venous catheter in an extremely low birth weight infant. BMJ Case Rep. 2011;2011:bcr0220113813. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 5] [Article Influence: 0.3] [Reference Citation Analysis (1)] |
| 11. | Pegu S, Murthy P. Ascites with hepatic extravasation of total parenteral nutrition (TPN) secondary to umbilical venous catheter (UVC) malposition in an extremely preterm baby. BMJ Case Rep. 2018;2018:bcr2018226377. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 7] [Article Influence: 0.9] [Reference Citation Analysis (1)] |
| 12. | Edison P, Arunachalam S, Baral V, Bharadwaj S. Varying clinical presentations of umbilical venous catheter extravasation: A case series. J Paediatr Child Health. 2021;57:1123-1126. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 2] [Article Influence: 0.4] [Reference Citation Analysis (1)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/