Published online Mar 9, 2026. doi: 10.5409/wjcp.v15.i1.114064
Revised: October 29, 2025
Accepted: January 6, 2026
Published online: March 9, 2026
Processing time: 177 Days and 0.8 Hours
Burns are a common cause of morbidity and mortality in children, especially in developing countries like India. Unless fatal, burns can lead to lifelong disability, affecting social and psychological well-being of the child. It further exacerbates the financial strain on parents and adversely impacts the mental well-being of siblings.
To understand the epidemiological profile as well as the psychosocial and ec
An observational study was conducted at tertiary care teaching hospital over a period of 20 months in which pediatric burn patients of age less than 15 years of age were evaluated. Demographic profile, circumstances of injury, type of burns (scalds, flame burns, electric burns), adult supervision at the time injury, time lapse and condition of patient at initial reporting, severity of burns, length of hospital stay and stay in intensive care unit, surgical procedures performed, outcome, deaths, adverse behavioral changes, financial impact on parents and impact on siblings were studied.
Majority of pediatric burns enrolled in the study were below 5 years of age (63.4%). Male (59.7%) to female (40.3%) ratio was 1.5:1. Scalds were the most common cause in all ages (55.07%). Flame burns (28.6%) and electric burns (16.3%) were more common in older children between age group 5-15 years. Patients who presented early with total body surface area burnt less than 50% had better outcomes. Mean loss of number of working days of parents in our study was 27.77 ± 13.07 days. Most common behavioral alteration reported in patients was irritability and anger (5.18%). Mean number of losses of school days for siblings was 20.59 ± 14.72 days. Multiple behavioral changes were observed in the siblings.
Majority of pediatric burns are caused by preventable factors. Public awareness regarding risk factors and preventive strategies can go a long way in reducing both pediatric disability as well as financial impact on the family.
Core Tip: Pediatric burns remain a significant cause of morbidity in developing countries, with children under five most affected. This prospective study highlights the predominantly preventable nature of such injuries, with scalds being the most common cause. Beyond physical trauma, burns impose a profound psychosocial and economic burden on families - ranging from emotional distress and behavioral changes in both patients and siblings, to substantial loss of workdays for parents. Early intervention and standardized management improve outcomes. Public awareness, education on prevention, and improved burn care infrastructure are essential to reduce incidence, disability, and long-term financial impact on affected families and the healthcare system.
- Citation: Parashar A, Thakur S, Sharda R. Pediatric burns: Key insights from cohort of 325 patients. World J Clin Pediatr 2026; 15(1): 114064
- URL: https://www.wjgnet.com/2219-2808/full/v15/i1/114064.htm
- DOI: https://dx.doi.org/10.5409/wjcp.v15.i1.114064
Burn-related injuries affect approximately eleven million people globally each year, with around 300000 annual fatalities as per World Health Organization reports[1,2]. Children are disproportionately affected, constituting about 50% of burn cases, with one-third under the age of 10 and nearly a quarter requiring hospitalization for severe injuries[3,4]. Burns rank as the fifth most common cause of non-lethal injuries and the third leading cause of accidental death among children aged 5 years to 9 years[5,6].
The incidence of burns correlates with a region’s economic status, being more prevalent in low and middle-income countries and declining in developed nations like the United States[7]. In countries like India, the actual burden is likely underreported. Burn injuries lead to physical impairments, chronic pain, and psychological distress for both children and their families, with complications like contractures and hypertrophic scars even in cases with less than 20% total body surface area (TBSA) involvement.
At our tertiary care center in North India, we manage severe cases often referred from Punjab, Haryana, Himachal Pradesh, Jammu, Kashmir, Leh, Ladakh, Uttarakhand and parts of Uttar Pradesh, Bihar. Many patients arrive late, without proper first aid, and are from low socioeconomic, less-educated backgrounds, complicating treatment and rehabilitation efforts. This study aims to explore the epidemiological profile and the psychosocial and economic impacts of burns, guiding strategies for improved management and prevention of these largely avoidable injuries.
An observational study was conducted at our tertiary care center on 325 pediatric burn patients less than 15 years of age over a period of 24 months. This being the pediatric Population, ethics committee approval, informed consent process, and confidentiality safeguards for pediatric participants was ensured. Demographic profile, circumstances of injury, type of burns (scalds, flame burns, electric burns), adult supervision at the time injury, initial reporting, status at the time of reporting, severity of burns, stay in intensive care unit (ICU), surgical procedures performed, hospital stay, outcome, deaths, adverse behavioral changes, financial impact on parents and siblings were studied.
Descriptive statistical analysis was performed to calculate the mean ± SD. Test of proportion was used to find the standard normal deviate (Z) to compare the difference proportions and χ2 test was performed to find the associations. P < 0.05 was taken to be statistically significant.
The mean age of the patients included in the study was 5.05 ± 4.07 years. 46.15% of the total enrolled patients were between 1-5 years of age. Males were affected more than females with a male/female ratio of 1.5:1. Punjab contributed 32.6% to the total number of pediatric burns received during the study, followed by Himachal Pradesh (22.7%; Table 1). The mean time lapse from injury to presentation to our institute was 4.82 ± 10.24 days. 82.4% of the patients reported within 7 days of injury, out of which 16.9% reached within few hours on the day of injury. This was significantly higher than the patients who reported after one week of injury. 5.2% patients reached us more than 21 days after they sustained the burn injuries (Table 2).
| Number of patients | Percentage (%) | |
| Age (years) | ||
| ≤ 1 | 56 | 17.23 |
| > 1 to ≤ 5 | 150 | 46.15 |
| > 5 to ≤ 15 | 119 | 36.61 |
| Total | 325 | 100.0 |
| Gender | ||
| Male | 194 | 59.7 |
| Female | 131 | 40.3 |
| Residential area | ||
| Punjab | 106 | 32.6 |
| HP | 74 | 22.7 |
| Chandigarh | 56 | 17.2 |
| Haryana | 53 | 16.3 |
| UP | 34 | 10.5 |
| Bihar | 1 | 0.3 |
| Uttarakhand | 1 | 0.3 |
| Time lapse from injury to admission | n (%) |
| 0 | 55 (16.9) |
| 1-7 | 213 (65.5) |
| 8-13 | 30 (9.2) |
| 14-21 | 10 (3.1) |
| > 21 | 17 (5.2) |
| Total | 325 (100.0) |
| mean ± SD | 4.82 ± 10.24 |
| Median (interquartile range) | 2 (1-98) |
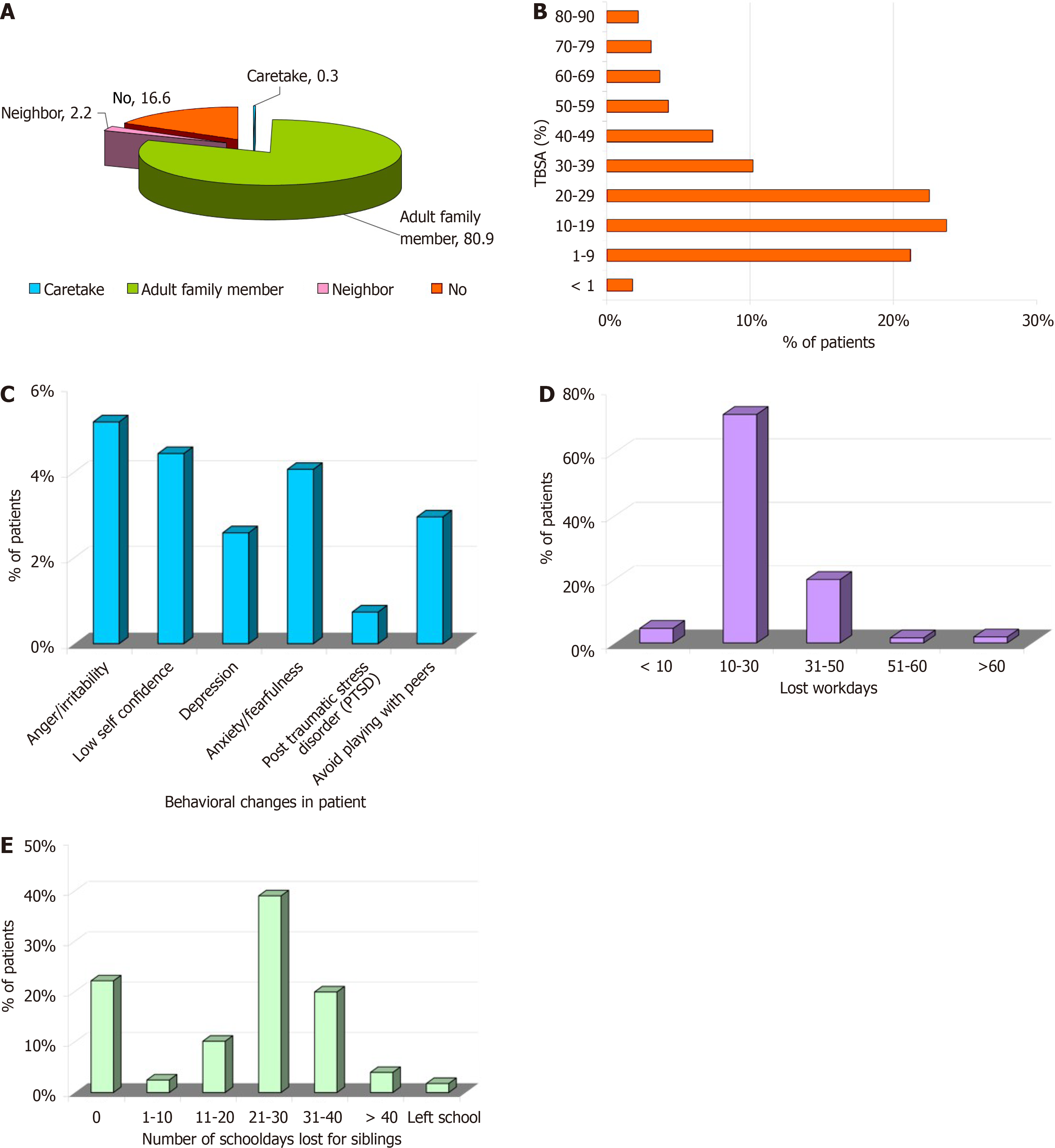
In 98.5% of cases, burn injuries were accidental in nature, while 1.5% cases were assault (Z = 13.85; P < 0.0001). Out of the 98.5% of accidental burns, 77.84% occurred in indoor or domestic settings, while 20.61% occurred outdoors (Table 3). In 55.07% patients, cause of burn injury was scald, in 28.6% patients the cause was thermal burn and in 16.30% patients it was electric burn. Scald was significantly higher among the patients with age ≤ 5 years (87%) than the patients with age > 5 years (12.9%; Z = 10.46; P < 0.0001). Thermal and electric burns were significantly higher among the patients aged > 5 years than the patients with age ≤ 5 years (P < 0.0001). Out of 56 infants (≤ 1 year), scald was the cause of burn in 80.35% cases (Table 4). The most common causative agent for scalds was hot water (51.42%), followed by hot milk (26.55%). Most common causative factor for flame burns was liquefied petroleum gas leak (79.56%), and that for electrical burn was contact with high voltage electricity (76.36%; Table 4). At the time of injury, 80.92% patients were accompanied by adult family member, while in 16.61% no adult was around when the injury happened. This difference was statistically significant (Z = 9.05; P < 0.0001; Figure 1A).
| Nature of injury | Frequency | % |
| Accidental | ||
| Indoor | 253 | 77.84 |
| Outdoor | 67 | 20.61 |
| Assault | 5 | 1.5 |
| Total | 325 | 100 |
| Causative agents | Number of patients | % |
| Scald | ||
| Hot water | 91 | 51.42 |
| Hot milk | 47 | 26.55 |
| Hot tea | 21 | 11.86 |
| Hot oil | 11 | 6.21 |
| Hot dal | 5 | 2.82 |
| Hot caramel | 1 | 0.56 |
| Steam | 1 | 0.56 |
| Thermal/flame burn | ||
| LPG leak | 74 | 79.56 |
| Bonefire | 4 | 4.30 |
| Firecracker | 15 | 16.12 |
| Electric burn | ||
| HVEB (contact) | 42 | 76.36 |
| LVEB (contact) | 8 | 14.54 |
| Flash burn | 5 | 9.09 |
In this study, 58.46% patients had visited nearest government hospital before reaching our institute, 28.30% patients had visited private hospital, while 7.07% had received home treatment for burn injuries (Z = 4.42; P < 0.0001; Table 5). Time lapse from the time of injury to admission was less than 24 hours in 146 (44.92%) patients. When the patients presented to our institute, 55.07% patients were under resuscitated, whereas 44.92% patients were adequately re
| Place of initial reporting | Frequency | % |
| Government hospital | 190 | 58.46 |
| Private hospital | 92 | 28.30 |
| Home treatment | 23 | 7.07 |
| None | 20 | 6.15 |
| Total | 325 | 100 |
| Resuscitation | Frequency | % |
| Under resuscitated | 179 | 55.07 |
| Adequately resuscitated | 146 | 44.92 |
| Over resuscitated | 0 | 0 |
| Total | 325 | 100 |
Total 325 pediatric burn patients had visited our center during the study period, out of which 314 patients were admitted, while 11 patients were not admitted either due to death of the patient at presentation or due to minor burns which were managed on outpatient basis. Majority of the patients enrolled in the study had TBSA burnt below 30% (69.2%), while only 9% patients had TBSA burnt above 60% (Z = 7.91; P < 0.0001; Figure 1B). Mean TBSA involved in the study was 23.74% ± 19.60%, with a range of 0.2% to 90.56%. Out of 314 admitted patients, 75% patients were admitted to ICU. Length of ICU stay was less than 7 days for majority (45.5%) of patients, while in 2.5% cases, length of ICU stay was more than 35 days. The mean duration of ICU stay was 10.43 ± 9.41 days (Table 7).
| ICU stay (days) | Frequency | % |
| < 7 | 110 | 45.5 |
| 7-13 | 72 | 29.8 |
| 14-20 | 29 | 12.0 |
| 21-34 | 25 | 10.3 |
| 35+ | 6 | 2.5 |
| Total | 242 | 100.0 |
| mean ± SD | 10.43 ± 9.41 | |
| Median (interquartile range) | 7 (1-50) | |
177 patients required surgical procedures. Most commonly performed procedure was debridement and split-thickness skin graft (52.30%). Other procedures included shoulder disarticulation/limb or digit amputation, fasciotomy, flap surgeries, tracheostomy, interventional radiology guided glue injection, amniotic membrane transplant, and colostomy/abdominal mesh placement in decreasing order (Table 8). The mean duration of hospital stay in this study was 21.89 ± 18.12 days with a range of 1-125 days. Most (72.6%) of the patients were discharged within one month (Table 9).
| Procedures done | Frequency | % |
| Fasciotomy | 6 | 1.84 |
| Debridement/SSG | 170 | 52.30 |
| Shoulder disarticulation/limb or digit amputation | 20 | 6.15 |
| Tracheostomy | 2 | 0.61 |
| Amniotic membrane transplant | 1 | 0.30 |
| IR guided glue injection | 1 | 0.30 |
| Flap surgeries | 5 | 1.53 |
| Colostomy/abdominal mesh placement | 1 | 0.30 |
| None | 148 | 45.53 |
| Total | 325 | 100 |
| Length of hospital stay (days) | Number of patients | % |
| < 7 | 71 | 22.6 |
| 7-14 | 74 | 23.6 |
| 15-30 | 83 | 26.4 |
| 31-45 | 53 | 16.9 |
| 46-60 | 25 | 8.0 |
| > 60 | 8 | 2.5 |
| Total | 314 | 100.0 |
| mean ± SD | 21.89 ± 18.12 | |
| Median (interquartile range) | 17 (1-125) | |
Patients who presented early (within 48 hours) with TBSA < 50% had better outcome, of which 72.5% healed completely at the time of discharge, 24.75% had few raw areas left, whereas 2.75% succumbed to their injuries. Among patients who presented late (after 48 hours), 67% patients were healed, 17% partially healed and 16% died. Outcomes in patients with TBSA > 50% were poor with 75% of early presenters and 90% late presenters succumbing to their injuries (Table 10). Most common behavioral alteration reported in patients was irritability and anger (5.18%), followed by low confidence (4.44%), fearfulness and anxiety (4.07%). 2.96% of patients have started avoiding playing with friends, 2.59% were depressed and 0.74% patients suffered post-traumatic stress disorder (Figure 1C).
| Outcomes | Patients presenting early (≤ 48 hours) | Patients presenting late (> 48 hours) | ||
| TBSA < 50% | TBSA > 50% | TBSA < 50% | TBSA > 50% | |
| Healed | 132 | 3 | 67 | 0 |
| Partially healed | 45 | 5 | 17 | 1 |
| Death | 5 | 25 | 16 | 9 |
| Total | 182 | 33 | 100 | 10 |
| P value | < 0.001 | < 0.001 | ||
Average monthly family income of 57.86% patients was below 20000 Indian rupee, which was significantly higher than other average monthly family income (Z = 2.97; P = 0.0029; Table 11). In 35.07% cases, hospital expense was covered through Ayushman Bharat scheme (Z = 4.86; P < 0.0001), in 6% cases through Himcare, in 4% cases through government medical reimbursement and in 1.84% cases through company medical insurance policy. However, in most of the cases (52.30%) hospital expense was not covered under any medical insurance (Z = 0.56; P = 0.56; Table 12).
| Income (Indian rupee) | Frequency | % |
| < 20000 | 188 | 57.86 |
| 20000-40000 | 120 | 36.92 |
| 40001-60000 | 15 | 4.6 |
| 60000+ | 2 | 0.6 |
| Total | 325 | 100.0 |
| Covered under insurance | Frequency | % |
| Ayushman Bharat | 114 | 35.07 |
| Company medical insurance | 6 | 1.84 |
| Government medical reimbursement | 13 | 4.0 |
| Himcare | 22 | 6.76 |
| No coverage | 170 | 52.30 |
| Total | 325 | 100.0 |
The mean number of working days lost of parents was 27.77 ± 13.07 days, with a median of 29 days and range from 3 days to 100 days. In 76.61% cases, number of work days loss was ≤ 30 days (Z = 6.78; P < 0.0001; Figure 1D). Total loss of income ranged up to 90000 INR in this study. In majority of cases the total income loss was up to 40000 Indian rupee (97.33%; Z = 13.29; P < 0.0001). Mean and median loss of total income was 19225.71 ± 12632.91 Indian rupee and 20000 Indian rupee, respectively (Table 13). Due to patients burns, their siblings also lost schooldays. 59.1% of siblings have lost school days between 21 and 40 days (Z = 5.32; P < 0.0001). Mean number of losses of school days for siblings was 20.59 ± 14.72 days, with a range from 0% to 100.4% siblings had lost more than 40 days of school. Six siblings have left school to take care of the patient (Figure 1E). 12.92% siblings became fearful of burn injuries, while 11.38% siblings became more sympathetic and caring towards the patient (Table 14).
| Income (Indian rupee) | Number of patients | % |
| < 20000 | 133 | 44.33 |
| 20000-40000 | 159 | 53 |
| > 40000 | 8 | 2.66 |
| Total | 300 | 100.0 |
| mean ± SD | 19225.71 ± 12632.91 | |
| Median (interquartile range) | 20000 (0-90000) | |
| Behavioral changes in siblings | Frequency | % |
| Anxiety | 28 | 8.61 |
| Fearful of burn injury | 42 | 12.92 |
| Irritable/jealous/anger | 7 | 2.15 |
| More sympathetic and caring towards patient | 37 | 11.38 |
Burns are a major global health issue, causing around 180000 deaths annually[7]. Each day, over 30000 individuals experience severe burns that necessitate medical intervention, leading to an estimated 11 million new burn cases annually[8]. In India, over 1 million people suffer moderate to severe burns each year[7]. Approximately 70% of burn cases are concentrated in low and middle-income countries[8]. While high-income nations see declining burn death rates, child fatalities from burns are over seven times higher in low-income and middle-income countries[7]. Burns rank as the fifth most common cause of non-fatal childhood injuries, often occurring in domestic kitchens due to hot liquids, flames, or cook stove explosions[5].
Children’s limited risk awareness, inquisitiveness and inadequate adult supervision heighten their vulnerability. Some burn injuries also result from child maltreatment. Unless fatal, burns can lead to lifelong disability, affecting social and psychological well-being of the child[9]. It further exacerbates the financial strain on parents and adversely impacts the mental well-being of siblings. Pediatric burns also impose a substantial economic burden on national healthcare systems[10]. Worldwide patterns reveal that the direct financial expenses of burn treatment range between 26 million and 211 million dollars annually[9]. This study aimed to analyze the epidemiological profile of pediatric burn patients at our tertiary care center in North India, identifying environmental and patient-related risk factors, causative agents, and the social and economic impacts on affected children and families.
The study included 325 pediatric burn patients, providing insights into demographic trends and factors contributing to burn injuries. The mean age was 5.05 years (median: 2 years), with most burns occurring in children under 5 years (63.4%), consistent with previous reports of 59.7% and 74.8%[11,12], reflecting the increased vulnerability of younger children due to limited risk awareness. Males were more frequently affected (59.7%) than females (40.3%), with a male-to-female ratio of 1.5:1 (P = 0.0046), in line with other studies suggesting greater involvement of boys in risk-prone activities[13-16]. Accidental burns accounted for 98.5% of cases, aligning with previous studies by Dhopte et al[14] (97.5%) and García-Díaz et al[15] (98.6%). Indoor burns were predominant (79.06%), emphasizing domestic environments as high-risk settings. Scalds were the leading cause of burns (55.07%), particularly among children aged ≤ 5 years (87%), consistent with global trends. Flame burns (28.61%) and electric burns (16.92%) also represented significant proportions. Flame injuries were frequently associated with liquefied petroleum gas leaks and firecrackers, whereas electric burns were often linked to high-voltage exposures, especially in poorly constructed urban areas.
Scald injuries predominantly occurred in kitchens and bathrooms, involving hot water (51.42%) and hot milk (26.5%). The majority of burns were reported in low socioeconomic families living in small, single-room homes with floor-level cooking. Mothers, who often managed both childcare and household chores, frequently left hot liquids - such as water, milk, tea, or dal - within children’s reach. Scald injuries commonly occurred when hot water for bathing was left unattended, resulting in children falling into or pulling over buckets. During winter, water was boiled to higher temperatures to retain warmth, further increasing the risk. Contributing factors included parental distraction, lack of safety measures, and the socioeconomic constraints of families, many of whom could not afford safer appliances such as geysers. Seasonal variations influenced burn incidence, with peaks in winter (34.5%) due to increased use of hot water and fire-related activities. Electric burns were more common during the rainy season (43.63%), likely due to increased conductivity on wet surfaces. Most burns occurred in the presence of adults (80.92%); however, injuries frequently happened when caregivers were preoccupied, highlighting the importance of continuous supervision and targeted safety education.
The mean time interval between injury and arrival at our center was 4.82 ± 10.24 days. Most patients (82.4%) presented within one week of injury, including 16.9% who reported on the same day. Delayed presentation was observed in 9.2% during the second week, 3.1% during the third week, and 5.2% after three weeks. A review of available literature on pediatric burns revealed no data correlating adult supervision with the meantime lapse from injury to presentation. At presentation to our institute, 55.07% of patients were under-resuscitated. Patients referred early from other hospitals typically arrived within one week. In contrast, those treated at multiple facilities or managed at home for prolonged periods often presented with complications such as sepsis, septic shock, or acute kidney injury. These patients demonstrated higher mortality rates, prolonged ICU and hospital stays, and required multiple surgical interventions. To our knowledge, no previous studies have reported the resuscitation status of burn patients at admission.
ICU admission was required for 75% of patients, with a mean ICU stay of 10.43 ± 9.41 days. The mean duration of hospital stay was 21.89 ± 18.12 days. Early presentation (within 48 hours) and burns involving < 50% TBSA were associated with favorable outcomes, yielding a survival rate of 83.38% and a mortality rate of 16.6%. Delayed presentation and extensive burns (> 50% TBSA) were linked to poor prognosis.
At follow-up, 89.62% of patients were independent in age-appropriate daily activities, 7.03% were partially dependent, and 3.33% were completely dependent. Patients with bilateral limb amputations required parental assistance for basic activities, whereas those with single-limb or digital amputations, or nerve and tendon injuries, retained partial independence. Behavioral and psychological changes included irritability and anger (5.18%), low self-confidence (4.44%), fear and anxiety related to burn injuries (4.07%), depression (2.59%), social withdrawal (2.96%), and post-traumatic stress disorder (0.74%). Notably, behavioral outcomes in pediatric burn survivors have been inadequately described in existing literature.
In our study, most fathers (58.8%) were unskilled workers, mainly migrant laborers and most mothers (85%) were homemakers. This contrasts with the greater occupational diversity reported by Wang et al[16]. Most patients (67.4%) came from nuclear families, with mothers as primary caregivers. The economic impact of burns was substantial, with parents losing a mean of 27.77 ± 13.07 working days (median: 29; range: 3-100) and significant income losses for 97.33% of families. Over half the families (52.30%) had no health insurance coverage (P = 0.56), resulting in significant out-of-pocket expenditure for these families. Pediatric burns also affected siblings, with 59.1% missing 21-40 school days (P < 0.0001). Emotional impacts included fear of burns, anxiety and feelings of jealousy, anger, or irritability due to perceived parental neglect.
Pediatric burn injuries are largely preventable through improved awareness, supervision, and health system strengthening. Community-based and school-based education programs should focus on increasing awareness among parents, caregivers, and children regarding common causes of burns and preventive practices, with particular emphasis on the dangers of leaving young children unattended in high-risk areas such as kitchens and bathrooms. Electrical safety measures, including the use of childproof plugs, covered sockets, and restricted access to exposed wiring, should be promoted, along with strict enforcement of regulations ensuring safe distances between residential areas and high-tension power lines, fencing of electrical transformers, and clear warning signage. Public education on fire response and basic first aid should be incorporated into community outreach and school curricula. In addition, regular training programs for healthcare workers are essential to improve early burn severity assessment, appropriate fluid resuscitation, and pediatric-specific burn management, which requires intensive monitoring and specialized care. Strengthening referral networks and transport systems is also crucial to facilitate timely transfer of patients to tertiary care centers and ensure continuity of care, thereby reducing burn-related morbidity, long-term disability, and financial burden.
This observational study, though highlighting these points, does suffer from certain limitations like single-center design and only hospital-based sampling which can lead to potential reporting bias. There is need for multicentric and a larger study to address these limitations.
Pediatric burn injuries affect young children from socioeconomically disadvantaged backgrounds, where overcrowding, limited awareness, and unsafe domestic conditions increase vulnerability. Effective prevention therefore requires a multifaceted approach that prioritizes parental education, heightened supervision of young children, and the creation of safer home environments through improved cooking practices, electrical safety, and childproofing of high-risk areas. In addition to prevention, early recognition of burn injuries and prompt medical intervention are critical in reducing complications, mortality, and long-term disability. Comprehensive burn care, including timely resuscitation, surgical management, nutritional support, and rehabilitation; plays a vital role in optimizing functional recovery. Equally important is the provision of psychosocial support for affected children and their families, as burn injuries can have lasting emotional, behavioral, and socioeconomic consequences. Strengthening community awareness, healthcare systems, and social support mechanisms is essential to improve outcomes and minimize the long-term physical, psychological, and financial burden of pediatric burns.
| 1. | Taylor SL, Lee D, Nagler T, Lawless MB, Curri T, Palmieri TL. A validity review of the National Burn Repository. J Burn Care Res. 2013;34:274-280. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 38] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 2. | Yadollahi M, Fazeli P, Naqi MA, Karajizadeh M, Parsaiyan S. Epidemiology of Burns in Pediatric and Adolescent Patients of Fars Province between 2017 and 2018. Bull Emerg Trauma. 2023;11:41-46. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 3. | Suman A, Owen J. Update on the management of burns in paediatrics. BJA Educ. 2020;20:103-110. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 31] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 4. | Pelizzo G, Lanfranchi G, Pantaloni M, Camporesi A, Tommasi P, Durante E, Costanzo S, Canonica CMP, Zoia E, Zuccotti G, Ruotolopalmi V, Donzelli C, Tosi GL, Calcaterra V. Epidemiological and Clinical Profile of Pediatric Burns in the COVID-19 Era: The Experience of a Reference Center. Children (Basel). 2022;9:1735. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 10] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 5. | Han D, Wei Y, Li Y, Zha X, Li R, Xia C, Li Y, Yang H, Xie J, Tian S. Epidemiological and Clinical Characteristics of 5,569 Pediatric Burns in Central China From 2013 to 2019. Front Public Health. 2022;10:751615. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 13] [Reference Citation Analysis (0)] |
| 6. | Romanowski KS, Palmieri TL. Pediatric burn resuscitation: past, present, and future. Burns Trauma. 2017;5:26. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 25] [Cited by in RCA: 41] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 7. | World Health Organization. Burns. 13 Oct 2023. Available from: https://www.who.int/news-room/fact-sheets/detail/burns. |
| 8. | Stokes MAR, Johnson WD. Burns in the Third World: an unmet need. Ann Burns Fire Disasters. 2017;30:243-246. [PubMed] |
| 9. | Parry I, Bell J. Associations between burn care services and impairment at discharge after burn injury: Analysis of the Global Burn Registry. Burns. 2024;50:813-822. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 10] [Reference Citation Analysis (0)] |
| 10. | Gerstl JVE, Ehsan AN, Lassarén P, Yearley A, Raykar NP, Anderson GA, Smith TR, Sabapathy SR, Ranganathan K. The Global Macroeconomic Burden of Burn Injuries. Plast Reconstr Surg. 2024;153:743-752. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 20] [Article Influence: 10.0] [Reference Citation Analysis (0)] |
| 11. | Tolouei M, Bagheri Toolaroud P, Letafatkar N, Feizkhah A, Sadeghi M, Esmailzadeh M, Daghighi Masooleh M, Mobayen M. An 11-year retrospective study on the epidemiology of paediatric burns in the north of Iran. Int Wound J. 2023;20:3523-3530. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 11] [Reference Citation Analysis (0)] |
| 12. | Mohammed M, Mekonen Y, Berhe H. Clinical Profile of Pediatric Burn Patients in Burn Care Unit of Halibet Hospital in 2018: Asmara, Eritrea. Pediatric Health Med Ther. 2021;12:13-21. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 7] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 13. | Garland K, Nahiddi N, Trull B, Malic C. Epidemiological evaluation paediatric burn injuries via an outpatient database in Eastern Ontario. Burns Open. 2018;2:204-207. [RCA] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 4] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 14. | Dhopte A, Tiwari VK, Patel P, Bamal R. Epidemiology of pediatric burns and future prevention strategies-a study of 475 patients from a high-volume burn center in North India. Burns Trauma. 2017;5:1. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 18] [Cited by in RCA: 37] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 15. | García-Díaz A, Gacto-Sánchez P, Durán-Romero AJ, Carrasco-García S, Ruiz-Moya A, Molina-Morales J, Sánchez-Tatay MV, Gómez-Cía T, Pereyra-Rodríguez JJ. Pediatric major burns: a monocentric retrospective review of etiology and outcomes (2008-2020). Eur J Plast Surg. 2022;45:967-975. [RCA] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 16. | Wang S, Li D, Shen C, Chai J, Zhu H, Lin Y, Liu C. Epidemiology of burns in pediatric patients of Beijing City. BMC Pediatr. 2016;16:166. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 19] [Cited by in RCA: 34] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/