Published online Nov 9, 2021. doi: 10.5409/wjcp.v10.i6.177
Peer-review started: January 19, 2021
First decision: May 6, 2021
Revised: May 13, 2021
Accepted: August 17, 2021
Article in press: August 17, 2021
Published online: November 9, 2021
Processing time: 293 Days and 23.7 Hours
Pulmonary hypertension (PH) has serious short- and long-term consequences. PH is gaining increasing importance in high risk groups such as Down syndrome (DS) as it influences their overall survival and prognosis. Hence, there is a dire need to collate the prevalence rates of PH in order to undertake definitive mea
To determine the prevalence of PH in children with DS.
The authors individually conducted a search of electronic databases manually (Cochrane library, PubMed, EMBASE, Scopus, Web of Science). Data extraction and quality control were independently performed by two reviewers and a third reviewer resolved any conflicts of opinion. The words used in the literature search were “pulmonary hypertension” and “pulmonary arterial hypertension”; “Down syndrome” and “trisomy 21” and “prevalence”. The data were analyzed by Comprehensive Meta-Analysis Software Version 2. Risk of bias assessment and STROBE checklist were used for quality assessment.
Of 1578 articles identified, 17 were selected for final analysis. The pooled pre
This review highlights the increasing prevalence of PH in children with DS. It is crucial for pediatricians to be aware of this morbid disease and channel their efforts towards earlier diagnosis and successful management. Community-based studies with a larger sample size of children with DS should be carried out to better characterize the epidemiology and underlying etiology of PH in DS.
Core Tip: The objective of this review is to provide quantitative data on the prevalence of pulmonary hypertension (PH) in pediatric patients with Down syndrome (DS). In addition, we also wish to address the lack of consensus on screening guidelines for PH in DS, as it is frequently missed unless associated with an underlying congenital heart disease. We conclude that children with DS require early echocardiography irrespec
- Citation: Taksande A, Pujari D, Jameel PZ, Taksande B, Meshram R. Prevalence of pulmonary hypertension among children with Down syndrome: A systematic review and meta-analysis. World J Clin Pediatr 2021; 10(6): 177-191
- URL: https://www.wjgnet.com/2219-2808/full/v10/i6/177.htm
- DOI: https://dx.doi.org/10.5409/wjcp.v10.i6.177
Down syndrome (DS) was first clinically observed and described by Dr. Down[1] in his report on the “Observations on an ethnic classification of idiots” in 1866. The incidence of DS is approximately 1 in every 733 live births, which makes it the most common human malformation[2,3]. Children with DS are at an increased risk of developing pulmonary hypertension (PH). DS is the most common genetic syndrome associated with PH (with or without congenital heart disease), the others being DiGeorge syndrome, Scimitar syndrome, Noonan syndrome, Dursun syndrome and Cantu syndrome[4]. Regardless of the underlying etiology, PH has debilitating consequences on the health of the child and also reduces life expectancy. Approximately 75% of all deaths in DS may be attributed to pneumonia and infectious lung disease, congenital heart disease (CHD) and circulatory disease (vascular diseases such PH)[5]. There have been no studies estimating the precise disease burden of PH in children with DS even though PH is independently associated with death among children with DS[6]. This reflects the need to provide a multidisciplinary approach for children with DS and PH for better management. Recent recommendations from the pediatric task force of the 6th World Symposium on Pulmonary Hypertension (WSPH) have defined PH in the pediatric age group as a resting mean pulmonary artery pressure (mPAP) > 20 mmHg (decreased from 25 mmHg) in children greater than 3 months of age at sea level and includes children with pulmonary vascular resistance (PVR) ≥ 3 WU[4,7]. PH is classified into 5 groups on the basis of each category sharing similar hemodynamics, pathological findings as well as similar management strate
The risk factors associated with the development of PH in DS are multifactorial. Chromosomal abnormalities such as trisomy 21 have been attributed to an increased risk of developing PH with an odds ratio of 36 (95%CI: 4.15-312.24), implying a genetic contribution to PH development using univariate logistic regression[9]. The presence of congenital heart disease (CHD) is a major contributing factor to PH in the DS population. Other risk factors include defects in lung development (due to overexpression of anti-angiogenesis genes on chromosome 21)[10], pulmonary hypoplasia[11], endothelial dysfunction[12,13], pulmonary diseases[14-18], gastrointestinal disea
Herein, we describe the first systematic review and meta-analysis which consolidates our existing knowledge on the prevalence of PH in DS. Our objective was to establish the prevalence of PH in children with DS. This systematic review also aims to provide sufficient evidence which could guide policy-making aimed at the prevention and effective management of PH as well as underpin further research.
Meta-analysis of observational studies in epidemiology (MOOSE) guidelines were followed for this systematic review[23]. The protocol for this systematic review and meta-analysis was registered at the International Prospective Register of Systematic Reviews (PROSPERO # CRD42020204914).
A two-stage search strategy was used for this study.
Electronic databases (PubMed, Cochrane library, EMBASE, Scopus, Web of Science) were searched. The search was restricted by English language with published studies including human subjects only, but not restricted by date or publication types. Studies with insufficient data such as abstracts only, studies with adult participants, con
An individual manual search was also performed which included examining the references of all the eligible papers and other related review articles as well as recent conference proceedings or recommendations on PH. Additional studies from these sources were then included in the review, provided they fulfilled the inclusion criteria.
All studies were handled by the literature management software Endnote X7. This was carried out to ensure no duplication. A preliminary screening of studies was performed by 2 independent authors (AT and PZJ). Screening of all titles and abstracts was done, and the full text was studied for any article considered relevant. After the initial round of screening, sorting was carried out again by re-reading all the articles. Methods were adapted as per PRISMA (Preferred Reporting Items for Systematic reviews and Meta-analyses) guidelines for meta-analyses[24].
Any observational study which determined the prevalence of PH in DS was consi
(1) All cross-sectional, case–control or cohort studies including children with DS reporting the prevalence of PH; (2) Studies must use either right heart catheterization for diagnosis with the cut-off being mPAP ≥ 25 mmHg or a 2D echocardiogram for determination of pulmonary arterial systolic pressure (PASP) (> 25 mmHg); and (3) All published studies from 1st January 1980 to 30th June 2020 were included.
(1) Studies performed in non-human subjects; (2) Case series, reviews, letters, com
Two investigators (PZJ and DP) separately reviewed articles and screened them for eligibility. Full texts were downloaded for any articles which were deemed eligible. The investigators also checked the full texts of each study and studies which met the inclusion criteria were included. A third author (AT) was consulted to resolve any disagreements. A screening test was used to ensure that all review authors reliably applied the selection criteria. Agreement was measured using the kappa (κ) statistic[25].
A standard data extraction form was used to retrieve relevant information. Two review authors (PZJ and DP) participated in data extraction independently. PZJ and DP extracted data which included general information (authors, year, and country), study design, diagnostic criteria for PH, and prevalence of PH. In studies where only preliminary data were provided, such as sample size or number of outcomes, other required data were calculated based on these values. Data were extricated using a preconceived and standardized data abstraction form. Studies with un-interpretable data were excluded from the analysis. Level of agreement was ascertained by the κ statistic[25].
Each included study was evaluated for quality of methodology and risk of bias by two investigators (PZJ and DP) using an adapted version of the Risk of Bias Tool for Prevalence Studies developed by Hoy et al[26]. The STROBE checklist[27] was utilized to assess the reporting quality of each study. Reporting of Observational Studies in Epidemiology (STROBE) was performed by two authors. The STROBE statement has a total of 22 items on the checklist. These items relate to various parts of the study such as the article’s title and abstract (item 1), the introduction (items 2 and 3), methods (items 4–12), results (items 13–17) and discussion sections (items 18–21), and other information (item 22 on funding). Agreement was measured using the κ statistic[25].
Each included study reported the prevalence of pulmonary hypertension as a pro
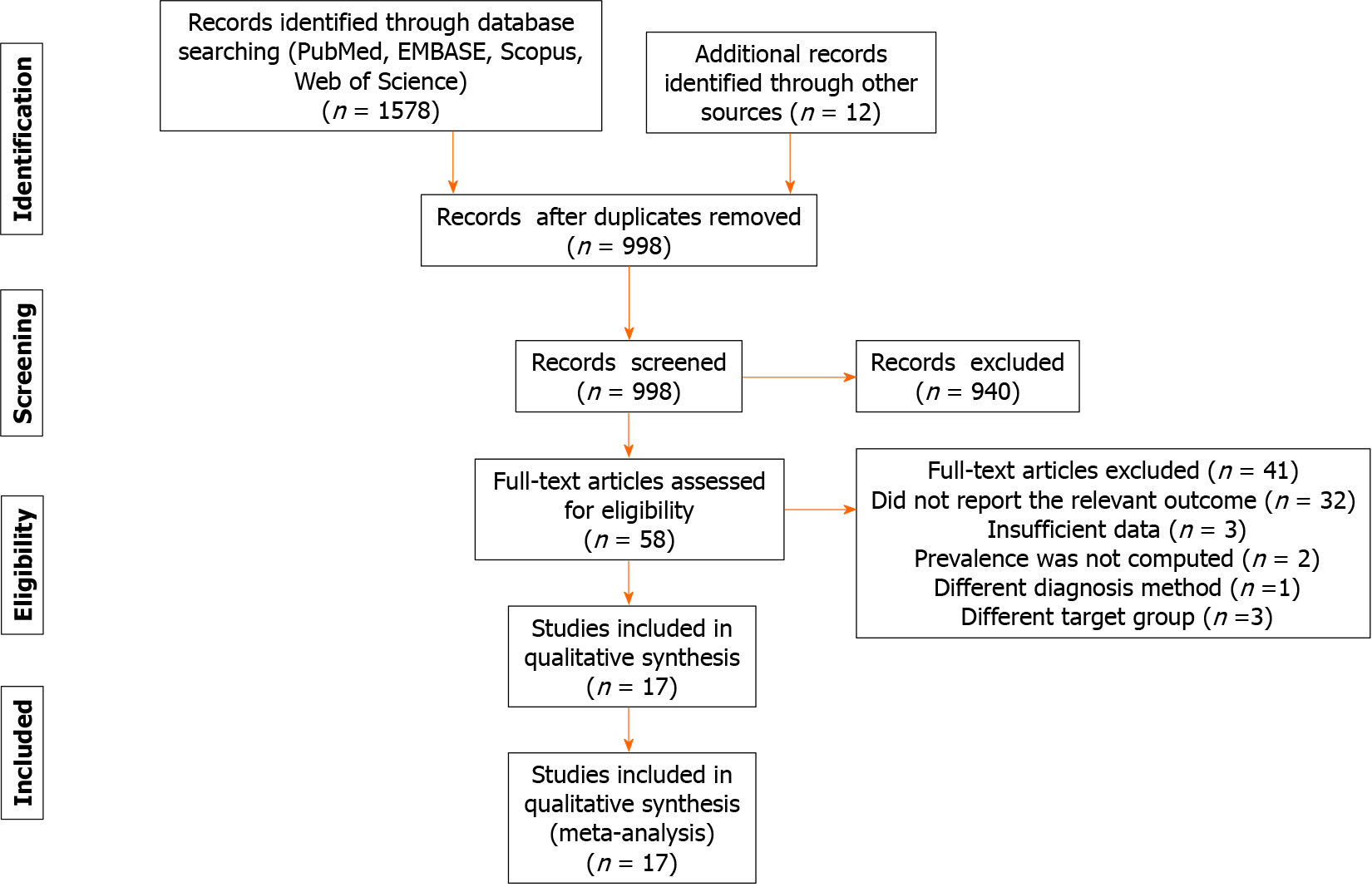
Initially, a total of 1578 articles were identified (Figure 1). After elimination of dup
All 17 studies noted the prevalence of PH without any analysis and no study reported the incidence of PH. The studies included were published from 2003 to 2020. Ten studies collected data retrospectively and seven studies collected the data pro
| Ref. | Year | Timing of data collection | Study design | Country | Population size | Cases with PH | Prevalence of PH |
| De Rubens et al[48] | 2003 | Retrospective | Observational | Mexico | 275 | 41 | 14.90909 |
| Shah et al[33] | 2004 | Retrospective | Observational | Canada | 175 | 24 | 13.71429 |
| Cua et al[35] | 2007 | Retrospective | Observational | USA | 58 | 7 | 12.06897 |
| Weijerman et al[40] | 2010 | Prospective | Cohort | Netherlands | 820 | 25 | 3.04878 |
| Banjar et al[41] | 2012 | Retrospective | Observational | Saudi Arabia | 59 | 44 | 74.57 |
| Mourato et al[42] | 2013 | Retrospective | Cross-sectional | Brazil | 138 | 42 | 30.43478 |
| Sharma et al[43] | 2013 | Prospective | Observational | India | 35 | 18 | 51.42857 |
| Shrestha et al[36] | 2013 | Prospective | Observational | Nepal | 50 | 21 | 42 |
| Espinola-Zavaleta et al[44] | 2015 | Prospective | Observational | Mexico city | 127 | 102 | 80.31496 |
| Bermudez et al[34] | 2015 | Retrospective | Observational | Brazil | 1207 | 57 | 4.722452 |
| Zonouzi et al[45] | 2015 | Prospective | Cross-sectional | Iran | 110 | 23 | 20.90909 |
| Joffre et al[6] | 2016 | Retrospective | Observational | France | 66 | 19 | 28.78788 |
| Okeniyi et al[37] | 2017 | Prospective | Observational | Nigeria | 70 | 14 | 20 |
| Bush et al[38] | 2018 | Retrospective | Cohort | USA | 1252 | 346 | 27.63578 |
| Martin et al[39] | 2018 | Retrospective | Cohort | Ireland | 121 | 41 | 33.8843 |
| Zahari et al[46] | 2019 | Retrospective | Cohort | Malaysia | 754 | 160 | 21.22016 |
| Alsuwayfee et al[47] | 2020 | Prospective | Cross-sectional | Iraq | 76 | 23 | 30.26 |
| Ref. | Diagnosis established by | Age group, (mean ± SD, yr) | Sex (M:F) | Diagnostic criteria for PH |
| De Rubens et al[48] | Echocardiography | Less than 16 yr | 1:1 | NM |
| Shah et al[33] | Echocardiography | Newborn | 10:7 | Right to left shunting at ductal or atrial level in the absence of severe pulmonary parenchymal disease |
| Cua et al[35] | Echocardiography | Neonate | 25:33 | Right-to-left shunt at the ductal level or flattening of the IVS in the absence of a PDA |
| Weijerman et al[40] | Echocardiography | Neonate | NM | Right-to-left shunt at the ductal level |
| Banjar et al[41] | Echocardiography | 3.3 ± 3.9 | 34:25 | > 50% of systolic systemic pressure |
| Mourato et al[42] | Echocardiography | Infant | 61:77 | mPAP > 25 mmHg |
| Sharma et al[43] | Echocardiography | Less than 12 yr | 4:3 | mPAP >25 mmHg |
| Shrestha et al[36] | Echocardiography | 4 mo to 12 yr | 1:1.4 | NM |
| Espinola-Zavaleta et al[44] | Echocardiography | Up to 18 yr | 64:63 | mPAP > 30 mm Hg |
| Bermudez et al[34] | Echocardiography | Up to 11 mo | NM | mPAP > 25 mmHg |
| Zonouzi et al[45] | Echocardiography | 1 mo-20 yr | 53:57 | NM |
| Joffre et al[6] | Echocardiography | 1mo-16 yr | 2:1 | NM |
| Okeniyi et al[37] | Echocardiography | 3 mo-9 yr | 3:4 | NM |
| Bush et al[38] | Echo or catheterization | Birth to 21 yr | 688:564 | mPAP > 25 mmHg; IVS flattening, RV dilation, or presence of RV hypertrophy |
| Martin et al[39] | Echocardiography | Neonate | 62:59 | Right to-left shunt across the PDA, IVS bowing into the left ventricle, or the presence of a TR jet |
| Zahari et al[46] | Echocardiography | Newborn | 189:225 | IVS flattening, a dilated main pulmonary artery, and dilated right cardiac chambers |
| Alsuwayfee et al[47] | Echocardiography | < 15 yr | 0.85:1 | mPAP > 25 mmHg |
The quality assessment results are presented in Table 3. No study met all criteria of the quality assessment score. Study quality varied from 10 to 17 as per the STROBE criteria. A score of < 14 was considered low quality, and > 14 was considered good/fair quality. The quality of reporting was low for two studies[33,34] and was good/fair for the remaining 15 studies. The most common limitations faced during STROBE assessment were inability to gauge the required sample size and poor projection of the results to the general population.
| STROBE quality of reporting | ||||||
| Ref. | The title and abstract (Item 1) | Introduction (Item 2-3) | Methods (Item 4-12) | Results (Item 13-17) | Discussion and other information (Item 18-22) | Quality score (0-22) |
| De Rubens et al[48] | 1 | 2 | 6 | 4 | 2 | 15 |
| Shah et al[33] | 0 | 2 | 5 | 2 | 3 | 12 |
| Cua et al[35] | 1 | 2 | 5 | 3 | 4 | 15 |
| Weijerman et al[40] | 1 | 2 | 4 | 4 | 4 | 15 |
| Banjar et al[41] | 1 | 2 | 4 | 4 | 4 | 15 |
| Mourato et al[42] | 1 | 2 | 5 | 2 | 4 | 14 |
| Sharma et al[43] | 1 | 2 | 5 | 3 | 4 | 15 |
| Shrestha et al[36] | 1 | 2 | 4 | 4 | 4 | 15 |
| Espinola-Zavaleta et al[44] | 1 | 2 | 5 | 3 | 3 | 14 |
| Bermudez et al[34] | 1 | 2 | 4 | 2 | 4 | 13 |
| Zonouzi et al[45] | 1 | 2 | 4 | 3 | 5 | 15 |
| Joffre et al[6] | 1 | 2 | 5 | 2 | 4 | 14 |
| Okeniyi et al[37] | 1 | 2 | 5 | 3 | 3 | 14 |
| Bush et al[38] | 1 | 2 | 5 | 3 | 5 | 16 |
| Martin et al[39] | 1 | 2 | 5 | 4 | 4 | 16 |
| Zahari et al[46] | 1 | 2 | 5 | 3 | 4 | 15 |
| Alsuwayfee et al[47] | 1 | 2 | 5 | 4 | 4 | 16 |
Quality assessment was also conducted for each study using the risk of bias assess
| Ref. | Representation | Sampling | Random selection | Non response bias | Data collection | Case definition | Reliability and validity of study tool | Method of data collection | Prevalence period | Numerator and denominator | Summary assessment |
| De Rubens et al[48] | HR | HR | HR | HR | HR | HR | LR | LR | HR | LR | HR |
| Shah et al[33] | HR | HR | HR | HR | HR | HR | LR | LR | HR | LR | HR |
| Cua et al[35] | LR | LR | LR | LR | LR | LR | LR | LR | HR | LR | LR |
| Weijerman et al[40] | HR | HR | HR | HR | HR | LR | LR | LR | HR | LR | MR |
| Banjar et al[41] | HR | HR | LR | HR | LR | HR | LR | LR | LR | LR | MR |
| Mourato et al[42] | HR | HR | HR | HR | LR | LR | LR | LR | HR | LR | MR |
| Sharma et al[43] | HR | LR | LR | HR | LR | LR | LR | LR | LR | LR | LR |
| Shrestha et al[36] | LR | LR | LR | HR | LR | LR | LR | LR | HR | LR | LR |
| Espinola-Zavaleta et al[44] | LR | LR | LR | HR | HR | HR | LR | LR | HR | LR | MR |
| Bermudez et al[34] | LR | LR | HR | HR | LR | HR | LR | LR | HR | LR | MR |
| Zonouzi et al[45] | HR | HR | HR | HR | LR | HR | LR | LR | HR | LR | MR |
| Joffre et al[6] | HR | HR | HR | HR | HR | HR | HR | HR | LR | LR | HR |
| Okeniyi et al[37] | LR | LR | LR | HR | HR | LR | LR | LR | HR | LR | LR |
| Bush et al[38] | LR | LR | LR | HR | HR | LR | LR | LR | HR | LR | LR |
| Martin et al[39] | LR | LR | LR | HR | HR | LR | LR | LR | HR | LR | LR |
| Zahari et al[46] | HR | LR | HR | HR | LR | HR | LR | LR | HR | LR | MR |
| Alsuwayee et al[47] | HR | HR | HR | HR | LR | LR | LR | LR | LR | LR | MR |
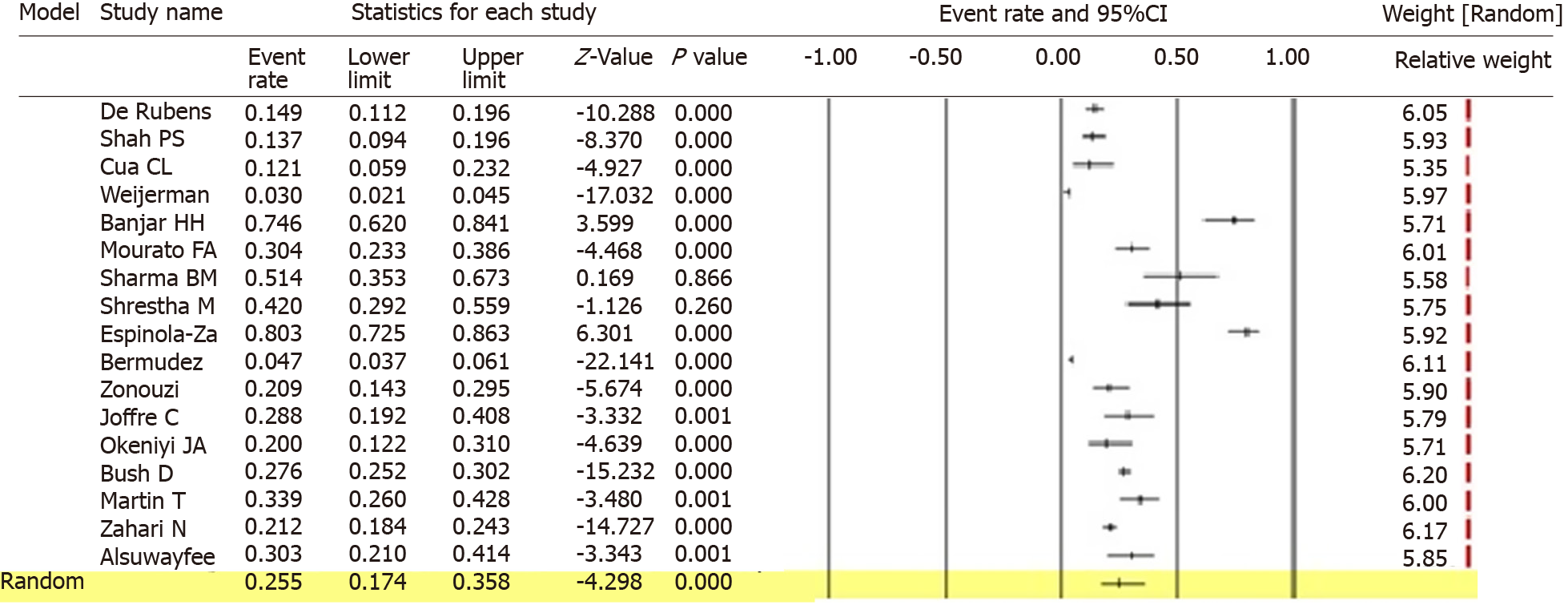
Prior studies have estimated the prevalence of PH in children with DS to be as high as 6% and 15% at 1 and 10 years of life, respectively, but data from large populations are lacking[44]. A wide disparity was seen among the various studies for PH prevalence. The heterogeneity was high (I2 = 97.20%, P < 0.001). The overall prevalence of the meta-analysis of 17 studies, according to the Der Simonian-Laird random-effects model, revealed that the pooled prevalence of PH among children with DS was 25.5% (95%CI: 17.4%–35.8%). The forest plot is shown in Figure 2.
Stability of the meta-analysis was assessed by sensitivity analysis. The observations remained largely the same. This similarity between the results showed the stability of our meta-analysis. Also, no significant factor influencing the heterogeneity was identified by the sensitivity analysis.
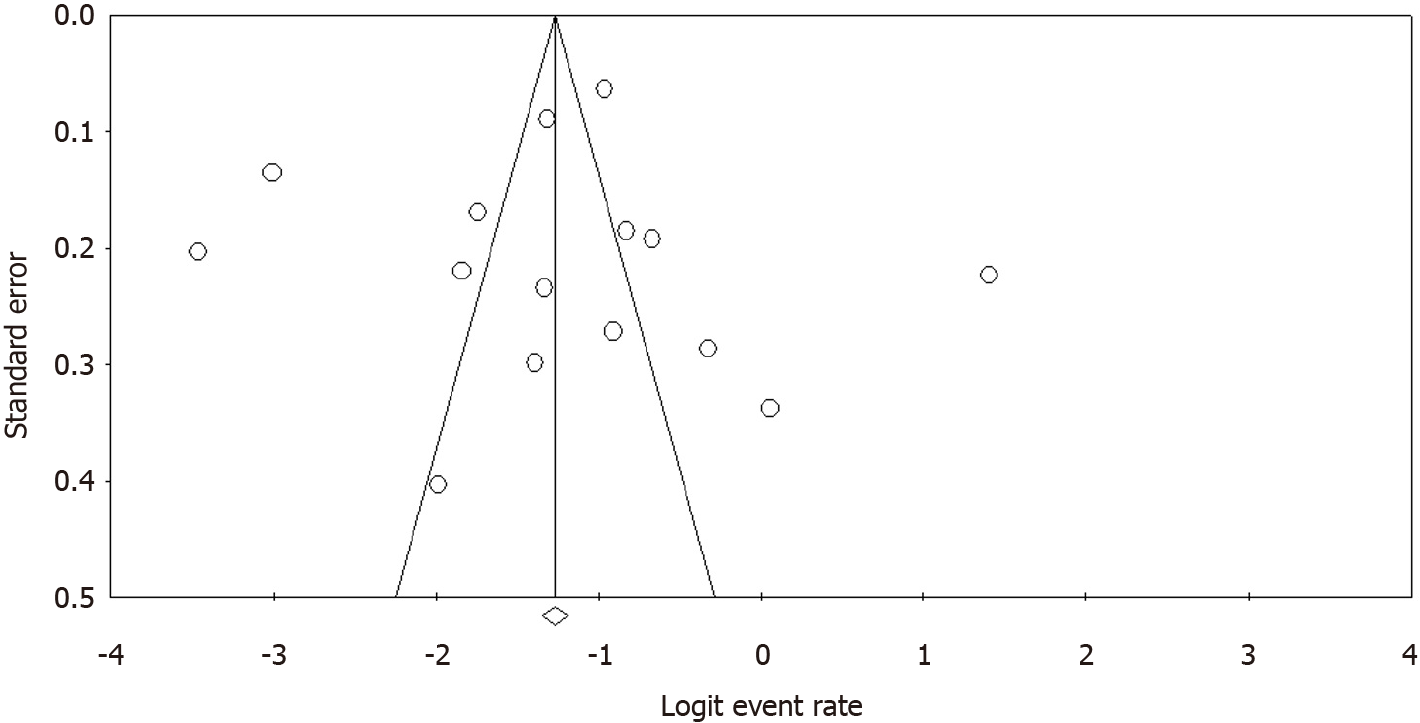
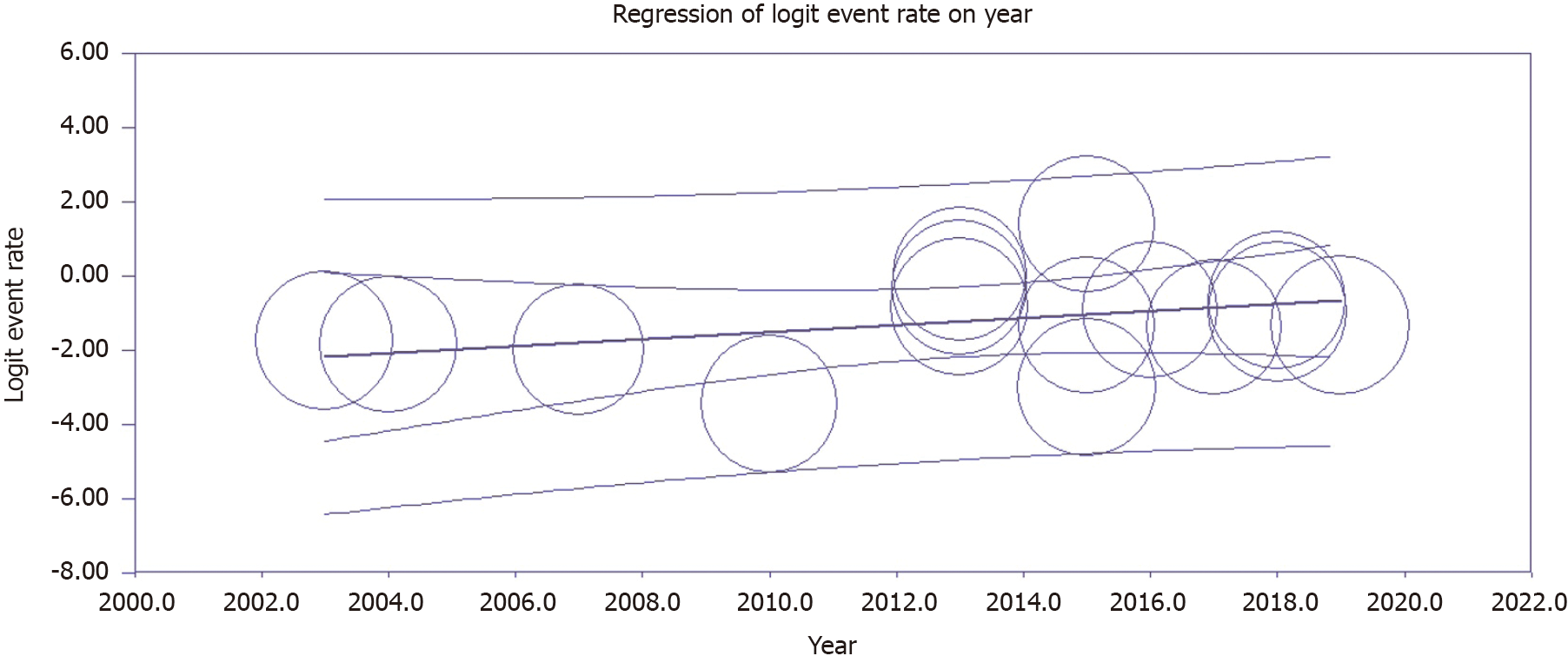
Subgroup analysis was used to reduce heterogeneity. The pooled prevalence of different subgroups is illustrated in Table 5. There were noteworthy differences for subgroups of gender, age group, region, year of publication, risk of bias and etiology of PH (P < 0.05). Four articles[35,38,45,47] presented prevalence linked to gender, with a prevalence of 24.3% among males and 26.2% among females. Some studies reported age distribution while others reported prevalence relating to each age group, which made the results difficult to compare. According to age group, 16 studies were sub-grouped into two categories: studies conducted in infants (less than one year) (4 studies), and studies conducted in infants and children (12 studies). The prevalence of PH among studies including infants and children (33.7%; 95%CI: 22.6%-47%) was higher than studies including only infants (13.4%; 95%CI: 6.6%-25.4%). The prevalence of PH among children with DS from the Asian continent (38.4%; 95%CI: 23.7%-55.7%) was higher than non-Asian continents (19.8%; 95%CI: 10.9%-33.2%). The prevalence of PH was higher in studies published after 2011 (29.8%; 95%CI: 20.2%-41.7%) than those published before 2011 (0.09%; 95%CI: 0.04%-20.0%). Subgroup analyses showed the prevalence of PH among children with DS in studies with moderate risk (34%; 95%CI: 16%-57%) and low risk (20%; 95%CI: 9%-37%) to be higher than studies with high risk of bias (17.8%; 95%CI: 11.6%-26.5%). According to the etiology of PH, 7 studies included were divided into two categories i.e. with CHD and without CHD. The prevalence of PH attributable to CHD (14.4%; 95%CI: 7%-26.1%) was higher than in those without CHD etiology (8.9%; 95%CI: 4.4%-17.5%). Only one study, Bush et al[38] classified the etiologies as per WHO classification[8]. The diagnosis of PH was made in 82% of children, with 45% being associated with CHD, and 38% having persistent pulmonary hypertension of the newborn (PPHN). The Egger weighted regression statistics (P = 0.94) and Begg rank correlation statistics (P = 0.45) indicated no evidence of publication bias. There was no sign of publication bias and asymmetry in the funnel plot (Figure 3). The meta-regression model in Figure 4 shows that the prevalence of PH among children with DS has increased in recent years. However, this relationship was not statistically significant (meta-regression coefficient: 0.0947, 95%CI: -0.035 to 0.22, P = 0.153).
| Stratification group | Number of studies | Total number of subjects | Total number of events | I2 | P value | Prevalence | 95%CI |
| Sex | |||||||
| Male | 4 | 801 | 210 | 28.22 | 0.243 | 24.3 | 18.8-30.6 |
| Female | 4 | 695 | 189 | 56.44 | 0.076 | 26.2 | 18.8-35.3 |
| Age | |||||||
| Infant (< 1 yr) | 7 | 3273 | 356 | 95.35 | 0.000 | 13.4 | 6.6-25.4 |
| Children (> 1 yr) | 9 | 2061 | 607 | 94.68 | 0.000 | 33.7 | 22.6-47.0 |
| Region | |||||||
| Asia | 6 | 1084 | 289 | 93.68 | 0.000 | 38.4 | 23.7-55.7 |
| Not Asia | 11 | 4309 | 718 | 97.92 | 0.000 | 19.8 | 10.9-33.2 |
| Studies published | |||||||
| Before 2011 | 4 | 1328 | 97 | 93.79 | 0.000 | 9.4 | 4.1-20.2 |
| 2011 - 2020 | 13 | 4065 | 910 | 97.13 | 0.000 | 33.0 | 22.5-45.4 |
| Risk of bias | |||||||
| High risk | 3 | 516 | 84 | 76.20 | 0.015 | 17.8 | 11.6-26.5 |
| Moderate risk | 8 | 2119 | 437 | 97.91 | 0.000 | 34.0 | 16.6-57.1 |
| Low risk | 6 | 2758 | 486 | 97.63 | 0.000 | 20.0 | 9.3-37.7 |
| Etiology | |||||||
| Cardiac | 7 | 724 | 372 | 97.06 | 0.000 | 14.4 | 7.4-26.1 |
| Non-cardiac | 7 | 724 | 352 | 96.63 | 0.000 | 8.9 | 4.4-17.5 |
Children with DS are known to be at a higher risk of developing pulmonary hy
In light of this, this is the first systematic review evaluating PH in children with DS. Despite extensive literature, there is large heterogeneity in the prevalence of PH in DS. The heterogeneity arises from multiple overlapping etiologies which are commonly associated with DS. The present study found the overall prevalence to be 25.5% (95%CI: 17.4%-35.8%) from a pool of 17 studies which met the inclusion criteria. This finding has shown concordance with multiple studies[6,37,38,45,46]. In order to reduce heterogeneity, subgroup analysis was carried out according to age, gender, region, etiology of PH and bias. In neonates, the incidence of PH is estimated at 2 per 1000 live births, which is notably less when compared to that observed in neonates with DS[52]. Earlier studies assessing PH in children with DS report an incidence ranging from 1% to 5%, with the majority of these infants being classified as having pulmonary arterial hypertension (PAH). More recent studies, however, have noted a much higher figure ranging between 27% and 34%[38]. Additionally, children with DS have an increased risk of developing PPHN even in the absence of structural heart disease and should be followed up until resolution of PH[33].
According to age group, 16 of the included studies were divided into 2 subgroups: studies conducted in children < 1 year of age (7 studies) and studies conducted in children > 1 year of age (9 studies). The prevalence of PH in DS was highest in children followed by infants and neonates. This contrast was highlighted because of the identification that infants with DS have a higher prevalence of PPHN and ab
The risk of bias was high in 3 studies with the prevalence of PH being 17.8%, 6 studies had low risk of bias with a prevalence of 20% and 8 studies with moderate risk showed a prevalence of 34%. There were 7 studies which assessed the prevalence of PH in children with DS with an underlying CHD. These studies had a prevalence of 14.4% while studies having no underlying CHD (7 studies) had a prevalence of 8.9%. Patients with an underlying CHD showed a higher prevalence of PH. Other studies have observed similar findings. Smith et al[54] reported that DS patients had a higher prevalence of PH with or without an underlying CHD and the difference between the two groups lies in the underlying etiology and the age of presentation. Iwaya et al[55] reported a lower pulmonary arterial compliance in individuals with CHD in DS when compared to CHD without DS. A noteworthy association was found between low pre-operative pulmonary compliance in DS and the need for postoperative oxygen therapy after discharge.
This is the only systematic review and meta-analysis assessing the prevalence of PH in the pediatric population with DS. A comprehensive search was undertaken wherein we included any study that reported the prevalence of PH in children with DS. Despite considerable heterogeneity between studies, our review provides the most comprehensive estimate of PH prevalence in children with DS to date, and most importantly, allows the comparison of prevalence between various groups of interest. Heterogeneity may arise from the data sources, populations examined and subjects with different ages, sex, risk of bias etc. This is not unexpected in view of the different populations studied and the nature of variations associated with the different methods used in estimating the prevalence. However, the sensitivity analysis showed that the heterogeneity had no significant impact on the pooled prevalence and a meta-analysis might still provide insights on the overall prevalence. The quality of the results and risk of bias of the studies included was at most, moderate, further highlighting that further such research may have a significant impact on our confidence in the estimate and might also change it. All included studies were observational; therefore, a cause effect relationship cannot be concluded between PH in children with DS. Longitudinal and interventional studies are still needed to determine the nature of any cause and effect relationship. Finally, some methodological limitations of the current meta-analysis were inevitable and should be taken into consideration while interpreting the results. Our study, although strengthened by rigid quality assessment, was limited by the fact that not all studies had classified all the etiologies of PH as per the WHO classification. The paucity of etiological data made it difficult to delineate individual causes of PH in patients with DS. This added to existing heterogeneity while analyzing the exact prevalence of PH in DS. More studies, specifically, ones with community screening for PH in DS are required to come to an exact estimate.
This article highlights the increasing prevalence of PH in children with DS. In order to improve the care given and reduce the disease burden, the attending pediatrician has a crucial role in being aware of this morbid disease and to channel his/her efforts towards routine screening of PH, earlier diagnosis and successful management. In addition, there should be early routine echocardiographic screening in children with DS even in the absence of CHDs. Community-based studies with a larger sample size of children with DS may be carried out to better characterize the epidemiology and underlying etiology. Our study reinforces what is already known and provides, in addition, reliable information about the prevalence of PH in DS.
Children with Down syndrome (DS) have an increased likelihood of developing pulmonary hypertension (PH) with serious short- and long-term consequences. Approximately 75% of all deaths in DS may be attributed to pneumonia and infectious lung disease, congenital heart disease (CHD) and circulatory disease (vascular diseases such PH). Despite the overwhelming evidence of morbidity, there have been no studies estimating the precise disease burden of PH in children with DS.
Additional information is required to collate the prevalence rates of PH in order to undertake definitive measures for early diagnosis and management.
The objective of this study is to determine the prevalence of PH in children with DS.
The electronic databases (PubMed, Cochrane library, EMBASE, Scopus, Web of Science) were searched. Any observational study which determined the prevalence of PH in DS was considered for the analysis. Data were extricated using a preconceived and standardized data abstraction form. The data were analyzed by Comprehensive Meta-Analysis Software Version 2.
Of 1578 articles identified, 17 were selected for final analysis. The pooled prevalence of PH in these studies was 25.5% (95%CI: 17.4%–35.8%). Subgroup analysis was carried out for age, gender, region, year of publication, risk of bias and etiology of PH.
This article highlights the increasing prevalence of PH in children with DS. This is accounted for by the high prevalence of underlying CHDs in these children. In order to improve the care given and reduce the disease burden, the attending pediatrician has a crucial role in being aware of this morbid disease and to channel his/her efforts towards routine screening of PH, earlier diagnosis and successful management. In addition, there should be early routine echocardiographic screening in children with DS even in the absence of CHDs. Community-based studies with a larger sample size of children with DS may be carried out to better characterize the epidemiology and underlying etiology of PH in DS. Our study reinforces what is already known and provides, in addition, reliable information about the prevalence of PH in DS.
Further studies are required to better characterize the epidemiology, underlying etiology, pathogenesis and risk factors of PH in children with DS.
| 1. | Down JL. Observations on an ethnic classification of idiots. 1866. Ment Retard. 1995;33:54-56. [PubMed] |
| 2. | Lee B. Down Syndrome and other abnormalities of chromosome number. In: Nelson’s Textbook of Pediatrics. 21st ed. Philadelphia: Elsevier; 2020: 658-664. |
| 3. | Jones KL, Jones MC, Campo MD. Chromosomal Abnormality Syndromes Identifiable on Routine Karyotype. In: Smith’s Recognizable Patterns of Human Malformation. 7th ed. Philadelphia: Elsevier; 2013: 7-10. |
| 4. | Abman SH, Hansmann G, Archer SL, Ivy DD, Adatia I, Chung WK, Hanna BD, Rosenzweig EB, Raj JU, Cornfield D, Stenmark KR, Steinhorn R, Thébaud B, Fineman JR, Kuehne T, Feinstein JA, Friedberg MK, Earing M, Barst RJ, Keller RL, Kinsella JP, Mullen M, Deterding R, Kulik T, Mallory G, Humpl T, Wessel DL; American Heart Association Council on Cardiopulmonary, Critical Care, Perioperative and Resuscitation; Council on Clinical Cardiology; Council on Cardiovascular Disease in the Young; Council on Cardiovascular Radiology and Intervention; Council on Cardiovascular Surgery and Anesthesia; and the American Thoracic Society. Pediatric Pulmonary Hypertension: Guidelines From the American Heart Association and American Thoracic Society. Circulation. 2015;132:2037-2099. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 948] [Cited by in RCA: 820] [Article Influence: 74.5] [Reference Citation Analysis (0)] |
| 5. | Colvin KL, Yeager ME. What people with Down Syndrome can teach us about cardiopulmonary disease. Eur Respir Rev. 2017;26. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 76] [Article Influence: 8.4] [Reference Citation Analysis (0)] |
| 6. | Joffre C, Lesage F, Bustarret O, Hubert P, Oualha M. Children with Down syndrome: Clinical course and mortality-associated factors in a French medical paediatric intensive care unit. J Paediatr Child Health. 2016;52:595-599. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 24] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 7. | Rosenzweig EB, Abman SH, Adatia I, Beghetti M, Bonnet D, Haworth S, Ivy DD, Berger RMF. Paediatric pulmonary arterial hypertension: updates on definition, classification, diagnostics and management. Eur Respir J. 2019;53. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 525] [Cited by in RCA: 431] [Article Influence: 61.6] [Reference Citation Analysis (0)] |
| 8. | Simonneau G, Gatzoulis MA, Adatia I, Celermajer D, Denton C, Ghofrani A, Gomez Sanchez MA, Krishna Kumar R, Landzberg M, Machado RF, Olschewski H, Robbins IM, Souza R. Updated clinical classification of pulmonary hypertension. J Am Coll Cardiol. 2013;62:D34-D41. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1912] [Cited by in RCA: 1932] [Article Influence: 148.6] [Reference Citation Analysis (32)] |
| 9. | Naumburg E, Söderström L, Huber D, Axelsson I. Risk factors for pulmonary arterial hypertension in children and young adults. Pediatr Pulmonol. 2017;52:636-641. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 41] [Cited by in RCA: 35] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 10. | Galambos C, Minic AD, Bush D, Nguyen D, Dodson B, Seedorf G, Abman SH. Increased Lung Expression of Anti-Angiogenic Factors in Down Syndrome: Potential Role in Abnormal Lung Vascular Growth and the Risk for Pulmonary Hypertension. PLoS One. 2016;11:e0159005. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 71] [Cited by in RCA: 56] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 11. | Cooney TP, Thurlbeck WM. Pulmonary hypoplasia in Down's syndrome. N Engl J Med. 1982;307:1170-1173. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 217] [Cited by in RCA: 172] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 12. | George PM, Oliver E, Dorfmuller P, Dubois OD, Reed DM, Kirkby NS, Mohamed NA, Perros F, Antigny F, Fadel E, Schreiber BE, Holmes AM, Southwood M, Hagan G, Wort SJ, Bartlett N, Morrell NW, Coghlan JG, Humbert M, Zhao L, Mitchell JA. Evidence for the involvement of type I interferon in pulmonary arterial hypertension. Circ Res. 2014;114:677-688. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 138] [Cited by in RCA: 130] [Article Influence: 10.8] [Reference Citation Analysis (0)] |
| 13. | Maron BA, Zhang YY, White K, Chan SY, Handy DE, Mahoney CE, Loscalzo J, Leopold JA. Aldosterone inactivates the endothelin-B receptor via a cysteinyl thiol redox switch to decrease pulmonary endothelial nitric oxide levels and modulate pulmonary arterial hypertension. Circulation. 2012;126:963-974. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 172] [Cited by in RCA: 154] [Article Influence: 11.0] [Reference Citation Analysis (0)] |
| 14. | Chamseddin BH, Johnson RF, Mitchell RB. Obstructive Sleep Apnea in Children with Down Syndrome: Demographic, Clinical, and Polysomnographic Features. Otolaryngol Head Neck Surg. 2019;160:150-157. [PubMed] [DOI] [Full Text] |
| 15. | Maris M, Verhulst S, Wojciechowski M, Van de Heyning P, Boudewyns A. Prevalence of Obstructive Sleep Apnea in Children with Down Syndrome. Sleep. 2016;39:699-704. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 191] [Cited by in RCA: 157] [Article Influence: 15.7] [Reference Citation Analysis (0)] |
| 16. | Hamilton J, Yaneza MM, Clement WA, Kubba H. The prevalence of airway problems in children with Down's syndrome. Int J Pediatr Otorhinolaryngol. 2016;81:1-4. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 60] [Cited by in RCA: 51] [Article Influence: 5.1] [Reference Citation Analysis (0)] |
| 17. | Jackson A, Maybee J, Wolter-Warmerdam K, DeBoer E, Hickey F. Associations between age, respiratory comorbidities, and dysphagia in infants with down syndrome. Pediatr Pulmonol. 2019;54:1853-1859. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 27] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 18. | Chenbhanich J, Wu A, Phupitakphol T, Atsawarungruangkit A, Treadwell T. Hospitalisation of adults with Down syndrome: lesson from a 10-year experience from a community hospital. J Intellect Disabil Res. 2019;63:266-276. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 19] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 19. | Ravel A, Mircher C, Rebillat AS, Cieuta-Walti C, Megarbane A. Feeding problems and gastrointestinal diseases in Down syndrome. Arch Pediatr. 2020;27:53-60. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 57] [Cited by in RCA: 42] [Article Influence: 7.0] [Reference Citation Analysis (0)] |
| 20. | Amr NH. Thyroid Disorders in Subjects with Down Syndrome: An Update. Acta Biomed. 2018;89:132-139. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 34] [Reference Citation Analysis (0)] |
| 21. | Sullivan KD, Lewis HC, Hill AA, Pandey A, Jackson LP, Cabral JM, Smith KP, Liggett LA, Gomez EB, Galbraith MD, DeGregori J, Espinosa JM. Trisomy 21 consistently activates the interferon response. Elife. 2016;5. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 315] [Cited by in RCA: 266] [Article Influence: 26.6] [Reference Citation Analysis (0)] |
| 22. | Rabinovitch M, Guignabert C, Humbert M, Nicolls MR. Inflammation and immunity in the pathogenesis of pulmonary arterial hypertension. Circ Res. 2014;115:165-175. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 875] [Cited by in RCA: 820] [Article Influence: 68.3] [Reference Citation Analysis (0)] |
| 23. | Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D, Moher D, Becker BJ, Sipe TA, Thacker SB. Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis Of Observational Studies in Epidemiology (MOOSE) group. JAMA. 2000;283:2008-2012. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17770] [Cited by in RCA: 17106] [Article Influence: 657.9] [Reference Citation Analysis (5)] |
| 24. | Moher D, Liberati A, Tetzlaff J, Altman DG; PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ. 2009;339:b2535. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20160] [Cited by in RCA: 17906] [Article Influence: 1053.3] [Reference Citation Analysis (4)] |
| 25. | Viera AJ, Garrett JM. Understanding interobserver agreement: the kappa statistic. Fam Med. 2005;37:360-363. [PubMed] |
| 26. | Hoy D, Brooks P, Woolf A, Blyth F, March L, Bain C, Baker P, Smith E, Buchbinder R. Assessing risk of bias in prevalence studies: modification of an existing tool and evidence of interrater agreement. J Clin Epidemiol. 2012;65:934-939. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2133] [Cited by in RCA: 1985] [Article Influence: 141.8] [Reference Citation Analysis (3)] |
| 27. | Vandenbroucke JP, von Elm E, Altman DG, Gøtzsche PC, Mulrow CD, Pocock SJ, Poole C, Schlesselman JJ, Egger M; STROBE Initiative. Strengthening the Reporting of Observational Studies in Epidemiology (STROBE): explanation and elaboration. Int J Surg. 2014;12:1500-1524. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2437] [Cited by in RCA: 2159] [Article Influence: 179.9] [Reference Citation Analysis (3)] |
| 28. | Higgins JP, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327:557-560. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 29. | Barendregt JJ, Doi SA, Lee YY, Norman RE, Vos T. Meta-analysis of prevalence. J Epidemiol Community Health. 2013;67:974-978. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1749] [Cited by in RCA: 1645] [Article Influence: 126.5] [Reference Citation Analysis (3)] |
| 30. | Higgins J, Green S. Cochrane handbook for systematic reviews of interventions. Vol. 4. Wiley; 2011. |
| 31. | Borenstein M, Hedges LV, Higgins JPT, Rothstein HR. Meta-Regression. In: Introduction to meta-analysis. Chichester, UK: John Wiley & Sons Ltd. 2009: 187–203. [RCA] [DOI] [Full Text] [Cited by in Crossref: 9207] [Cited by in RCA: 5620] [Article Influence: 702.5] [Reference Citation Analysis (3)] |
| 32. | Borenstein M, Rothstein H. Comprehensive meta-analysis: A computer program for research synthesis computer program. Englewood Cliffs, NJ: Biostat, Inc; 1999. |
| 33. | Shah PS, Hellmann J, Adatia I. Clinical characteristics and follow up of Down syndrome infants without congenital heart disease who presented with persistent pulmonary hypertension of newborn. J Perinat Med. 2004;32:168-170. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 69] [Cited by in RCA: 58] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 34. | Bermudez BE, Medeiros SL, Bermudez MB, Novadzki IM, Magdalena NI. Down syndrome: Prevalence and distribution of congenital heart disease in Brazil. Sao Paulo Med J. 2015;133:521-524. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 31] [Cited by in RCA: 26] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 35. | Cua CL, Blankenship A, North AL, Hayes J, Nelin LD. Increased incidence of idiopathic persistent pulmonary hypertension in Down syndrome neonates. Pediatr Cardiol. 2007;28:250-254. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 89] [Cited by in RCA: 77] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 36. | Shreshtha M, Shakya U. Down Syndrome and Congenital Heart Disease: Single centre, Prospective Study. Nepal J Med Sci. 2013;2:96-101. [DOI] [Full Text] |
| 37. | Okeniyi JA, Onakpoya UU, Samuel I, Adegoke OT, Okolugbo J. Spectrum of congenital heart disease in children with Down syndrome in Ile-Ife, Nigeria. Curr Pediatr Res. 2017;21:410-415. |
| 38. | Bush D, Galambos C, Ivy DD, Abman SH, Wolter-Warmerdam K, Hickey F. Clinical Characteristics and Risk Factors for Developing Pulmonary Hypertension in Children with Down Syndrome. J Pediatr. 2018;202:212-219.e2. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 108] [Cited by in RCA: 83] [Article Influence: 10.4] [Reference Citation Analysis (0)] |
| 39. | Martin T, Smith A, Breatnach CR, Kent E, Shanahan I, Boyle M, Levy PT, Franklin O, El-Khuffash A. Infants Born with Down Syndrome: Burden of Disease in the Early Neonatal Period. J Pediatr. 2018;193:21-26. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 54] [Cited by in RCA: 48] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 40. | Weijerman ME, van Furth AM, van der Mooren MD, van Weissenbruch MM, Rammeloo L, Broers CJ, Gemke RJ. Prevalence of congenital heart defects and persistent pulmonary hypertension of the neonate with Down syndrome. Eur J Pediatr. 2010;169:1195-1199. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 152] [Cited by in RCA: 127] [Article Influence: 7.9] [Reference Citation Analysis (0)] |
| 41. | Banjar HH. Pulmonary Hypertension (PHT) in Patients with Down Syndrome: The Experience in a Tertiary Care Center in Saudi Arabia. J Pulmonar Respirat Med. 2012;2:1-5. [DOI] [Full Text] |
| 42. | Mourato FA, Villachan LR, Mattos Sda S. Prevalence and profile of congenital heart disease and pulmonary hypertension in Down syndrome in a pediatric cardiology service. Rev Paul Pediatr. 2014;32:159-163. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 34] [Cited by in RCA: 24] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 43. | Sharma M, Khera S, Sondhi V, Devgan A. A study to determine the prevalence of pulmonary arterial hypertension in children with Down syndrome and congenital heart disease. Med J Armed Forces India. 2013;69:241-245. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 25] [Cited by in RCA: 20] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 44. | Espinola-Zavaleta N, Soto ME, Romero-Gonzalez A, Gómez-Puente Ldel C, Muñoz-Castellanos L, Gopal AS, Keirns C, Lupi-Herrera E. Prevalence of Congenital Heart Disease and Pulmonary Hypertension in Down's Syndrome: An Echocardiographic Study. J Cardiovasc Ultrasound. 2015;23:72-77. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 56] [Cited by in RCA: 42] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 45. | Zonouzi AAP, Ahangari N, Rajai S, Zonouzi AP, Laleh MA, Nejatizadeh A. Congenital heart defects among Down syndrome patients: a clinical profiling. J Public Health. 2016;24:57-63. [RCA] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 3] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 46. | Zahari N, Mat Bah MN, A Razak H, Thong MK. Ten-year trend in prevalence and outcome of Down syndrome with congenital heart disease in a middle-income country. Eur J Pediatr. 2019;178:1267-1274. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 16] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 47. | Alsuwayfee KI, Allbu-Dawlah ME, Mohammed QN. Congenital heart disease and pulmonary hypertension among Down syndrome pediatric patients. Ann Coll Med Mosul. 2020;42:50-56. |
| 48. | de Rubens Figueroa J, del Pozzo Magaña B, Pablos Hach JL, Calderón Jiménez C, Castrejón Urbina R. [Heart malformations in children with Down syndrome]. Rev Esp Cardiol. 2003;56:894-899. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 42] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 49. | Hawkins A, Langton-Hewer S, Henderson J, Tulloh RM. Management of pulmonary hypertension in Down syndrome. Eur J Pediatr. 2011;170:915-921. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 45] [Cited by in RCA: 42] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 50. | Saji T. Clinical characteristics of pulmonary arterial hypertension associated with Down syndrome. Pediatr Int. 2014;56:297-303. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 56] [Cited by in RCA: 43] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 51. | Yang Q, Rasmussen SA, Friedman JM. Mortality associated with Down's syndrome in the USA from 1983 to 1997: a population-based study. Lancet. 2002;359:1019-1025. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 653] [Cited by in RCA: 518] [Article Influence: 21.6] [Reference Citation Analysis (0)] |
| 52. | Steurer MA, Jelliffe-Pawlowski LL, Baer RJ, Partridge JC, Rogers EE, Keller RL. Persistent Pulmonary Hypertension of the Newborn in Late Preterm and Term Infants in California. Pediatrics. 2017;139. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 137] [Cited by in RCA: 122] [Article Influence: 13.6] [Reference Citation Analysis (0)] |
| 53. | Laursen HB. Congenital heart disease in Down's syndrome. Br Heart J. 1976;38:32-38. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 55] [Cited by in RCA: 43] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 54. | Smith AM, Levy PT, Franklin O, Molloy E, El-Khuffash A. Pulmonary hypertension and myocardial function in infants and children with Down syndrome. Arch Dis Child. 2020;105:1031-1034. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 6] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 55. | Iwaya Y, Muneuchi J, Inoue Y, Watanabe M, Okada S, Ochiai Y. Relationship Between Pulmonary Arterial Resistance and Compliance in Patients with Down Syndrome. Pediatr Cardiol. 2019;40:841-847. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 9] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
Open-Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/Licenses/by-nc/4.0/
Manuscript source: Invited manuscript
Specialty type: Pediatrics
Country/Territory of origin: India
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): 0
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Tommasini A S-Editor: Ma YJ L-Editor: Webster JR P-Editor: Yuan YY