Published online Apr 18, 2026. doi: 10.5312/wjo.v17.i4.115014
Revised: November 24, 2025
Accepted: January 28, 2026
Published online: April 18, 2026
Processing time: 187 Days and 13.7 Hours
Intramedullary headless screw (IMHS) fixation for metacarpal and phalanx fractures has shown comparable, and sometimes superior, outcomes compared with other management techniques; however, this option is not standard in our area.
To evaluate our early experience of using IMHS fixation for managing extraarticular metacarpal and proximal phalanx fractures by reporting the functional, radiographic, and complication outcomes from a North African level one trauma center.
In the current prospective single surgeon case series, 53 patients having a mean age of 33.79 ± 12.69 years presented with 67 extraarticular fractures (51 meta
wide awake local anaesthesia was utilized in 70.2% of the cases; the mean operative time was 14.37 ± 3.46 minutes, and closed fracture reduction was achieved in 95.5% of the fractures. Fracture union was achieved in all patients after a mean of 5.62 ± 0.99 weeks. At a mean last follow-up of 101.19 ± 52.31 days, the mean total active range of motion was 253.15° ± 10.29°. The mean percentage of grip strength was 98.66% ± 1.31% of the contralateral hand, and the mean Quick Disabilities of the Arm, Shoulder, and Hand score was 15.08 ± 11.95. The overall complication rate was 7.51%; all were considered minor, including shortening with or without metal protrusion (2.99%) and malunion (1.49%). There were no cases of nonunion, infection, or refracture, and there were no secondary sur
We achieved promising early functional and radiological results after adopting IMHS fixation for extraarticular metacarpal and proximal phalanx fractures, with a relatively lower complication rate. These results have led to changes in our institution’s practice for managing hand fractures.
Core Tip: Although intramedullary headless screw fixation is a well-documented management option for metacarpal and phalanx fractures, its broad adoption in our area is limited. We conducted this prospective study to evaluate the efficiency and outcomes of intramedullary headless screw fixation for metacarpal and proximal phalanx fractures, using either retrograde or antegrade fixation techniques. The clinical, radiological, and complication outcomes we observed after managing 67 extraarticular fractures in 53 patients were promising and comparable to those reported in the literature, which helped change our institutional management protocol for such fractures.
- Citation: Saleh WR, Khalifa AA, Ragheb YF, El-Sayed A, Megahed AA. Intramedullary headless screw fixation of extraarticular metacarpal and proximal phalanx fractures, North African trauma center early experience. World J Orthop 2026; 17(4): 115014
- URL: https://www.wjgnet.com/2218-5836/full/v17/i4/115014.htm
- DOI: https://dx.doi.org/10.5312/wjo.v17.i4.115014
Metacarpal and phalangeal fractures represent about 20% to 40% of all fractures in the hand and forearm, making them one of the common upper extremity fractures[1-3]. Furthermore, they have estimated annual incidence rates of 13.6 and 68 per 100000 United States persons/year for metacarpal and phalangeal fractures, respectively[4,5]. Treating these fractures operatively or non-operatively depends on various factors related to the patient, the surgeon, and the injury, including, but not limited to, their location, severity, displacement, and involvement of the articular surface[6-8]. Suppose the fracture is amenable to operative management; in that case, the aim is to reduce the fracture to restore the alignment in different planes and to secure this reduction by various fixation methods. The surgeon might choose from a broad armamentarium of surgical techniques, including open or closed fracture reduction, followed by fracture fixation with Kirschner wires (K-wires), external fixators, plates, and screws[6-8].
Regarding metacarpal and proximal phalanx fractures, most of these methods yielded excellent outcomes; however, they still have drawbacks. While K-wire fixation is considered a percutaneous and economic solution, it might hinder early rehabilitation; on the other hand, plate and screws fixation offers robust fixation, allowing early mobilization; however, they require considerable soft tissue dissection with the possibility of postoperative tendon adhesions and joint stiffness[8-11].
A step toward combining the benefits of percutaneous minimally invasive techniques and rigid fixation was to use intramedullary headless screws (IMHS) for the management of metacarpal and phalanx fractures. This technique proved efficient and superior to other methods in terms of biomechanical stability, clinical and radiological outcomes, and considerably lower complication rates[12-17].
After its first description by Boulton et al[18] about 15 years ago, IMHS fixation for managing hand fractures has become a well-known and widely adopted surgical technique; however, it is less prevalent in our area, and surgeons are reluctant to adopt it. Therefore, the primary objective of the current study was to report our early experience with IMHS fixation to manage extra-articular metacarpal and proximal phalanx fractures, including functional, radiological, and complication outcomes. The secondary objective was to compare our results with previous studies through an updated literature review.
This prospective case series was conducted at a North African (Egyptian) tertiary trauma unit over one year, starting from March 2024. Ethical approval was obtained from our institutional review board (approval No. 04-2024-200749), and the study was conducted in accordance with the principles of the Declaration of Helsinki. Written informed consent was obtained from all participants before inclusion. This manuscript was prepared in accordance with the Strengthening the Reporting of Observational Studies in Epidemiology guidelines.
Patient selection: We included skeletally mature patients with extraarticular closed or open Gustilo type I fractures of metacarpals and/or proximal phalanges (single, multiple, or combined) who had no previous hand deformities and had completed at least two months of follow-up. We excluded skeletally immature patients with open physis, open Gustilo type II or III fractures of phalanges or metacarpals, fractures associated with neurovascular or tendon injuries necessitating open management, intraarticular fractures, associated dislocation at either end of fractured bone, pathological fractures, fractures managed by other techniques (K-wires or plating), and patients presented with preinjury hand deformities.
Sample size consideration: As this study was designed as a case series, we included all eligible patients who presented with metacarpal or proximal phalanx fractures and underwent IMHS fixation during the defined one-year study period. Of 256 patients who presented with metacarpal or proximal phalanx fractures during the study period, 53 met the inclusion criteria, yielding a complete, consecutive sample. Given the total coverage of the target population during the study period, formal sample size calculations and power analyses were not applicable.
Surgical technique: A single surgeon performed all surgeries under general or wideawake [wide awake local anaesthesia (WALANT)] anesthesia based on the patient’s condition and presence of concomitant injuries. The patient was supine, and the affected limb was placed on an arm table. We followed the surgical details as described in the literature[17,19,20]. A retrograde IMHS insertion was performed for the metacarpal fractures, while the IMHSs were inserted in an antegrade fashion for proximal phalanx fractures. All screws were inserted percutaneously, and open fracture reduction was decided if the reduction was not achieved by closed maneuvers, for the possibility of soft tissue entrapment within the fracture.
Postoperative protocol: No splinting, only buddy taping of the fingers was applied. All patients were encouraged to start early motion as tolerated. Usually, patients were discharged on the same day and advised to follow up in the outpatient clinic after 2 weeks, 6 weeks, 3 months, and 12 months.
Clinical outcomes: Range of motion (ROM): (1) Individual joint ROM [Metacarpophalangeal (MCP), proximal interphalangeal (PIP), distal interphalangeal (DIP)]: The active motion of an individual digit’s MCP joint, PIP joint, and DIP joint was measured using a goniometer. Normal ranges were defined according to the American Society for Surgery of the Hand: MPJ from 0 to 85, PIP joint from 0 to 110, and DIP joint from 0 to 65; (2) Finger extension lag: Was calculated after considering the imperial weight of each individual joint contribution of the fingers’ motion, where the 40-40-20 weighting was used (MCP: 40%, PIP: 40%, and DIP: 20%)[21]. The extension deficit for each joint was calculated by subtracting the measured value from what is considered normal (A = extension lag at MCP, B = extension lag at PIP, and C = extension lag at DIP). Then this final formula was used to determine the total weighted extension lag: Weighted extension lag = 0.4 × A + 0.4 × B + 0.2 × C; and (3) Total active motion (TAM): Was calculated according to the American Society of Hand Therapists’ recommendations as the sum of active flexion at the MCP, PIP, and DIP joints, minus the sum of any extension deficits at these joints[22].
The Quick Disabilities of the Arm, Shoulder, and Hand (QuickDASH) score[23]: Formed of two components: The disability/symptom section (11 items, scored 1-5) and the optional high-performance sport/music or work modules (4 items, scored 1-5). We used the main disability/symptom section only in this study. Disability/symptom score: At least 10 of the 11 items must be completed to calculate a score. The assigned values for all completed responses are summed and averaged to produce a score out of five. This value is then transformed to a score of 100 by subtracting one and multiplying by 25. This transformation is done to make the score easier to compare with other measures scaled to 0-100. A higher score indicates greater disability. Pain outcome assessed per the pain visual analogue scale (VAS). Hand grip strength: The operated hand grip strength was reported as the strength percentage of the contralateral side. The assessment was conducted using a digital hand dynamometer[24].
Radiographic outcomes: This evaluation included standard posteroanterior, lateral, and oblique radiographs of the injured hand. Union was defined as the presence of a bridging trabecula across the fracture site in at least three cortices on orthogonal views. Time to union (weeks) was recorded.
Complications outcomes: Any perioperative complications were documented and reported. The following specific complications were monitored throughout the follow-up period: Joint stiffness, peri-implant infection, fracture non-union, hardware failure (protrusion or breakage), secondary operation, joint arthritis, and neurovascular injuries.
For each patient, demographic details (age, sex, hand dominance), injury mechanism, fracture location, and characteristics were recorded. The operative details and outcomes measured during the last follow-up were reported. Patients were divided into two groups based on fracture location: Group A, metacarpal fractures; and group B, phalanx fractures.
Data was entered and analyzed using Microsoft Excel (Microsoft Corporation, Redmond, WA, United States) and SPSS v26 (IBM Inc., Chicago, IL, United States). Continuous variables were summarized as mean ± SD with the corresponding range, while categorical variables were expressed as n (%). Continuous variables were compared between group a and group B using independent-samples t-tests with Welch correction, based on summary statistics (mean ± SD and sample sizes). While categorical variables were compared using Fisher’s exact test. A two-sided P < 0.05 was considered statistically significant.
A total of 53 patients (67 fractures) were included, 51 metacarpal fractures (group A) and 16 proximal phalanx fractures (group B). The mean patient’s age was 33.79 ± 12.69 years, and 88.7% were males. Multiple fractures occurred in 12 patients (22.6%). The most common fracture location was the 5th metacarpal (40.3%), followed by the 4th (29.9%). Fracture patterns were predominantly transverse (31.3%) and comminuted (29.9%). Most fractures were diaphyseal (62.7%). Full details of patients’ demographics and injury characteristics are provided in Table 1.
| Total of 53 patients (67 fractures) | Group A (n = 38 patients) (51 fractures) | Group B (n = 15 patients) (16 fractures) | P value for comparisons between group A vs group B | ||
| Age (years) | 33.79 ± 12.69 (17-65) | 35.08 ± 13.04 (17-60) | 32.53 ± 12.17 (19-65) | 0.517 | |
| Sex | Male | 47 (88.68) | 35 (92.11) | 12 (80) | 0.334 |
| Female | 6 (11.32) | 3 (7.89) | 3 (20) | ||
| Frequency | Multiple fracture | 12 patients | 24 (47.06) (11 patients) | 2 (12.5) (1 patient) | 0.002a |
| Single fracture | 41 patients | 27 (52.94) (27 patients) | 14 (87.5) (14 patients) | 0.144 | |
| Side of fracture | Right hand | 27 (50.94) | 20 (52.63) | 7 (46.67) | 0.766 |
| Left hand | 26 (49.06) | 18 (47.37) | 8 (53.33) | ||
| Dominant hand | 45 (84.9) | 34 (89.47) | 11 (73.33) | 0.202 | |
| Mode of trauma | MCA | 14 (26.42) | 11 (28.95) | 3 (20) | 0.732 |
| HOT | 1 (1.89) | 1 (2.63) | 0 (0) | 1.000 | |
| FOG | 22 (41.51) | 14 (36.84) | 8 (53.33) | 0.357 | |
| MBA | 4 (7.55) | 3 (7.89) | 1 (6.67) | 1.000 | |
| AFO | 12 (22.64) | 9 (23.68) | 3 (20) | 1.000 | |
| Associated injuries | Radius fracture | 1 (1.89) | 1 (2.63) | 0 (0) | 1.000 |
| Ulna fracture | 3 (5.66) | 3 (7.89) | 0 (0) | 0.550 | |
| Lunate fracture | 1 (1.89) | 1 (2.63) | 0 (0) | 1.000 | |
| Femur fracture | 2 (3.77) | 1 (2.63) | 1 (6.67) | 0.490 | |
| Tibia fracture | 2 (3.77) | 1 (2.63) | 1 (6.67) | 0.490 | |
| Spine fracture | 1 (1.89) | 0 (0) | 1 (6.67) | 0.283 | |
| Fractures characteristics | |||||
| Fractures location | 1st | 0 (0) | 0 (0) | 0 (0) | 1.000 |
| 2nd | 11 (16.42) | 7 (13.73) | 4 (25) | 0.438 | |
| 3rd | 9 (13.43) | 7 (13.73) | 2 (12.5) | 1.000 | |
| 4th | 20 (29.85) | 16 (31.37) | 4 (25) | 0.760 | |
| 5th | 27 (40.30) | 21 (41.18) | 6 (37.5) | 1.000 | |
| Fracture pattern | Spiral | 11 (16.42) | 10 (19.61) | 1 (6.25) | 0.274 |
| Oblique | 15 (22.39) | 10 (19.61) | 5 (31.25) | 0.327 | |
| Comminuted | 20 (29.85) | 17 (33.33) | 3 (18.75) | 0.356 | |
| Transverse | 21 (31.34) | 14 (27.45) | 7 (43.75) | 0.234 | |
| Anatomical site | Diaphysis | 42 (62.69) | 34 (66.67) | 8 (50) | 0.251 |
| Metaphysis | 25 (37.31) | 17 (33.33) | 8 (50) | ||
| Operative details | |||||
| Anaesthesia | General | 20 (29.85) | 17 (33.33) | 3 (18.75) | 0.356 |
| Wideawake | 47 (70.15) | 34 (66.67) | 13 (81.25) | ||
| Operative time (minutes) | 14.37 ± 3.46 (10-30) | 14.43 ± 3.81 (10-30) | 14.19 ± 2.07 (11-19) | 0.747 | |
| Fracture Reduction | Open | 3 (4.48) | 3 (5.88) | 0 (0) | 1.000 |
| Closed | 64 (95.52) | 48 (94.12) | 16 (100) | ||
| Type of screw | Acutrak 4 mm (fully threaded) | 38 (56.72) | 31 (60.78) | 7 (43.75) | 0.260 |
| Herbert 3.5 (partially threaded) | 18 (26.87) | 12 (23.53) | 6 (37.5) | 0.336 | |
| Herbert 2.7 (partially threaded) | 11 (16.42) | 8 (15.69) | 3 (18.75) | 0.716 | |
WALANT was used in 70.2% of cases; the mean operative time was 14.37 ± 3.46 minutes. Closed reduction was achieved in 95.5% of fractures. The most frequently used implant was the Acutrak 4 mm fully threaded screw (56.7%) (Table 1).
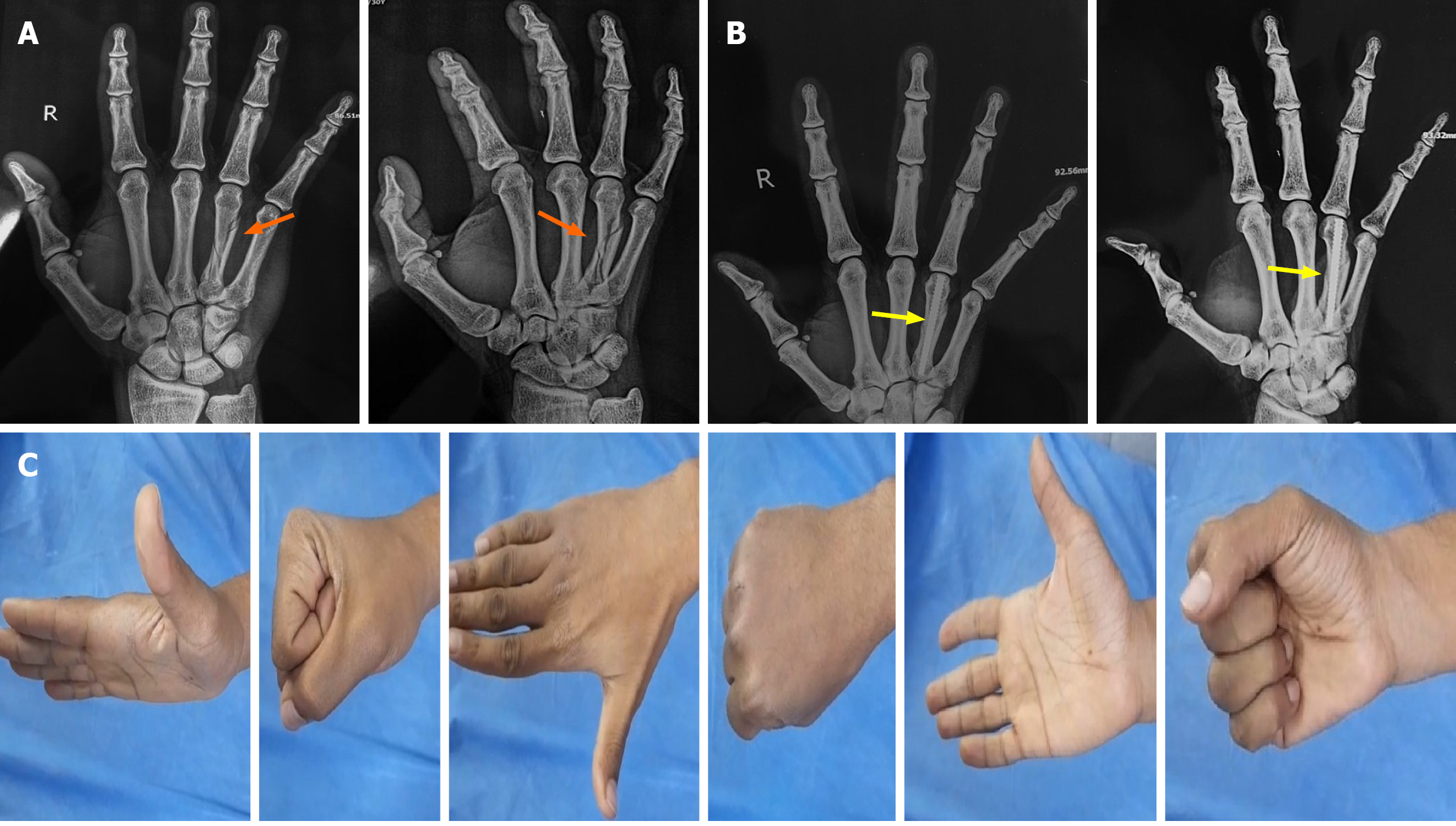
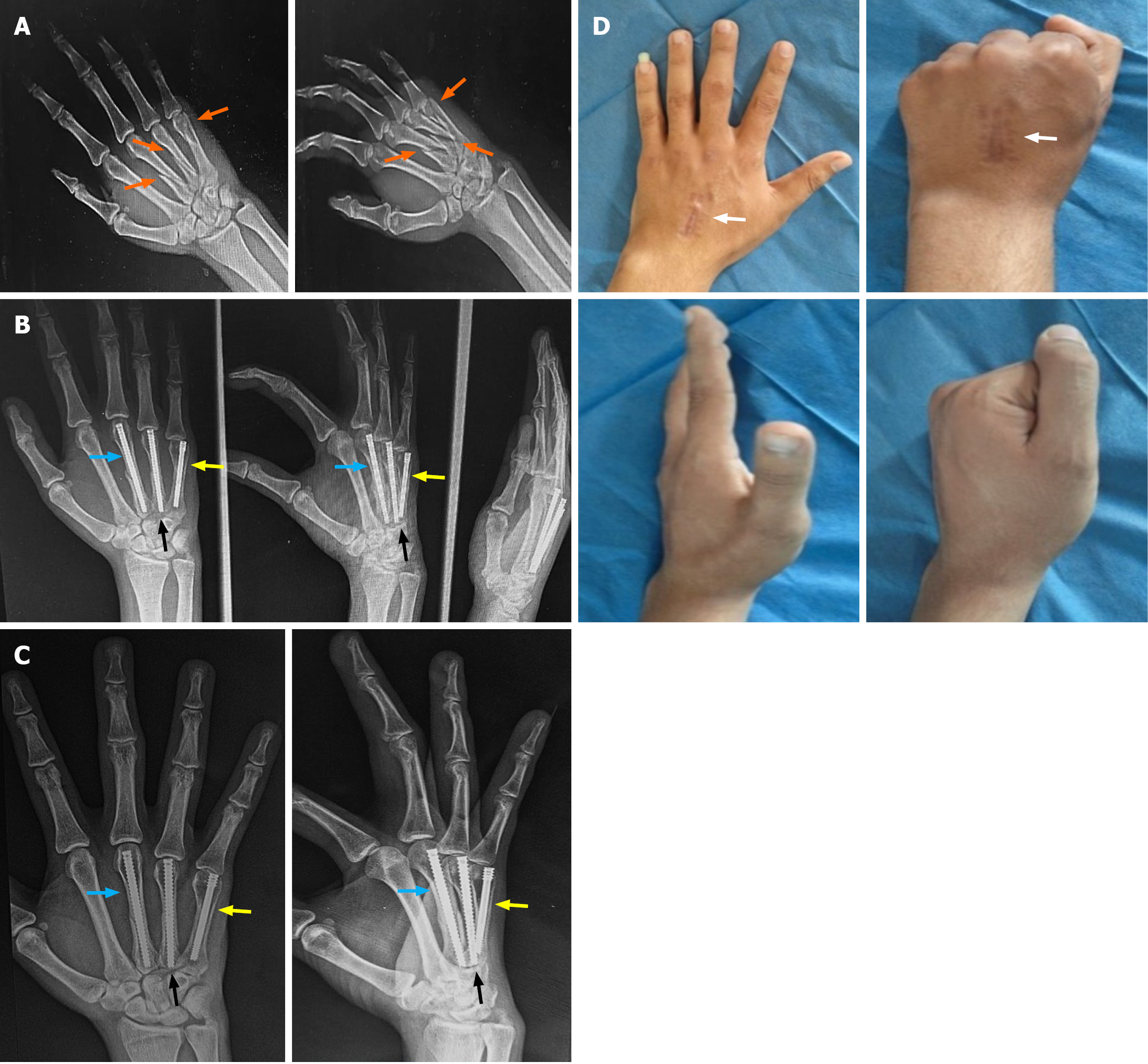
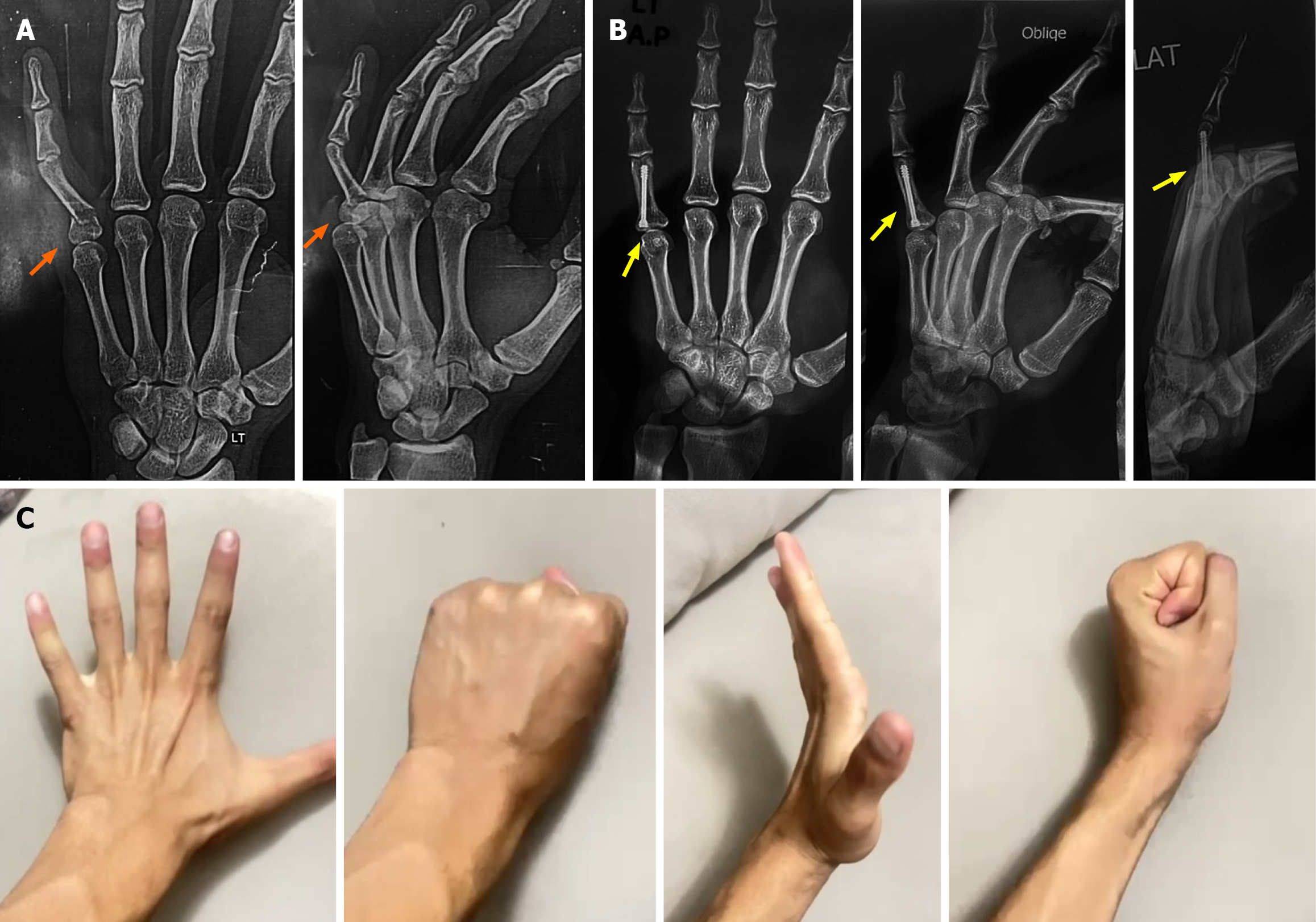
Fracture union was achieved in all patients after a mean of 5.62 ± 0.99 weeks. At a mean last follow-up of 101.19 ± 52.31 days, the mean TAM was 253.15° ± 10.29°. The mean percentage of grip strength was 98.66% ± 1.31% of the contralateral hand. The mean QuickDASH score was 15.08 ± 11.95, and the mean VAS was 0.69 ± 1.10 (Table 2) (Figures 1, 2 and 3).
| Total of 53 patients | Group A (n = 38 patients) (n = 51 fractures) | Group B (n = 15 patients) (n = 16 fractures) | P value for comparisons between group A vs group B | ||
| Time till fracture union (weeks) | 5.62 ± 0.99 (4-8) | 5.57 ± 0.94 (4-8) | 5.68 ± 1.04 (5-8) | 0.706 | |
| Last follow up (days) | 101.19 ± 52.31 (60-350) | 102.06 ± 53.92 (60-350) | 98.43 ± 48.31 (60-244) | 0.812 | |
| ROM MCPJ 85 (°) | 82 ± 1.9 (65-85) | 82.92 ± 2.97 (65-85) | 79.88 ± 5.44 (65-85) | 0.033 | |
| ROM PIPJ 110 (°) | 107.4 ± 4.93 (87-110) | 108.49 ± 2.76 (95-110) | 102.63 ± 7.19 (87-110) | 0.001a | |
| ROM DIPJ 65 (°) | 63.84 ± 2.66 (50-65) | 64.22 ± 2.32 (55-65) | 61.43 ± 3.81 (50-65) | 0.006a | |
| TAM (°) | 253.15 ± 10.29 (202-260) | 255.14 ± 9.11 (223-260) | 244.31 ± 15.12 (202-260) | 0.007a | |
| Extension lag | 2.53 ± 3.77 (0-20.2) | 1.15 ± 2.08 (0-13.8) | 2.01 ± 1.74 (0-6.2) | 0.100 | |
| Hand grip strength (% of the contralateral side) | 98.66 ± 1.31 (92.2 to 99.8) | 98.84 ± 1.07 (92.2-99.8) | 98.11 ± 1.8 (93.5-99.7) | 0.124 | |
| QuickDASH score | 15.08 ± 11.95 (2-57) | 2.9 ± 4.99 (0-34) | 6.88 ± 9.32 (0-34) | 0.030a | |
| VAS score | 0.69 ± 1.10 (0-5) | 0.35 ± 0.77 (0-3) | 1.94 ± 1.57 (0-5) | < 0.001a | |
| Complications | Infection | 0 (0.00) | 0 (0) | 0 (0) | 1.000 |
| Nonunion | 0 (0.00) | 0 (0) | 0 (0) | 1.000 | |
| Shortening with metal protrusion | 2 (2.99) | 1 (1.96) | 1 (6.25) | 0.423 | |
| Shortening without metal protrusion | 2 (2.99) | 1 (1.96) | 1 (6.25) | 0.423 | |
| Malunion | 1 (1.49) | 0 (0) | 1 (6.25) | 0.239 | |
No cases of infection, nonunion, hardware failure, or refracture. The overall complication incidence was 7.51%; all were considered minor, including shortening with or without metal protrusion, two cases each (2.99%), and malunion in one case (1.49%); however, none of these required secondary surgery (Table 2).
There was no statistically significant difference between group a and group B regarding age, sex distribution, side of injury, or hand dominance (all P > 0.05). Group A had a significantly higher proportion of patients with multiple fractures than group B (P = 0.002). In contrast, single fractures predominated in group B. Fracture location, pattern, anatomical site (diaphyseal vs metaphyseal), anesthesia type (general vs WALANT), and screw type did not differ significantly between groups.
Regarding outcomes, time to fracture union, duration of last follow-up, and MCP joint ROM did not differ between the groups. However, PIP and DIP joint ROM were significantly greater in group A, resulting in a better TAM. Furthermore, QuickDASH scores were significantly better in group A (P = 0.030), whereas VAS pain scores were significantly higher in group B (P < 0.001). The incidence of complications did not differ significantly between the two groups (Tables 1 and 2).
The results of the current study are encouraging and demonstrate the efficacy of IMHS fixation for the management of metacarpal and proximal phalanx fractures, with slightly better functional outcomes in metacarpal fractures. Besides a relatively straightforward and fast operative technique, it yielded excellent functional and radiological outcomes with minimal complications. Although we acknowledged that this was our early experience with this technique, the biomechanical advantages of intramedullary fixation are well described in the traumatology literature; furthermore, the efficiency and reproducibility of IMHS fixation of hand fractures have already been demonstrated[6,12,13,15-17]. To fulfil our secondary objective, we will discuss our early findings and compare them to the most recent literature reports.
As the technique is considered minimally invasive and localized to the hand, it can be performed with local or regional anesthesia, unless the patient’s condition necessitates general anesthesia. About 70% of the cases in the current series were operated under WALANT. In a systematic review by Hug et al[15], which included 18 studies involving 837 patients with 958 fractures distributed as follows: 693 metacarpal, 222 proximal phalangeal, and 43 middle phalangeal fractures, WALANT was the most commonly used anesthesia technique in 65.2% of the cases. Besides avoiding complications associated with other anesthesia techniques, WALANT offers the advantage of real-time range-of-motion assessment and evaluation of proper finger cascade.
One proposed advantage of IMHS fixation is that it is a closed maneuver with a relatively shorter operative time. We required a mean operative time of 14.37 ± 3.46 minutes, ranging from 10 minutes to 30 minutes, and nearly 96% of cases were treated by closed reduction.
Hug et al[15] reported a mean operative time of 26.4 minutes (range 5 to 60), which aligns with our results. On the contrary, Humar et al[25] evaluated the results of IMHS fixation for treating 92 fractures (metacarpals and phalangeal) in 69 patients having a mean age of 45 ± 18 years; the median operative time was longer, reaching up to 54 minutes; however, the authors attributed the longer operative time to patients with multiple injuries.
The rates of open reduction were higher in some studies than in our findings. In a multicenter study by Gehring et al[26], 101 metacarpal fractures in 82 patients with a mean age of 33 years were treated with IMHS fixation; they reported relatively higher rates of open reduction, up to 31.7%. Furthermore, Hug et al[15] reported equal incidences of percutaneous and open approaches for fracture reduction and fixation, 46.2% and 53.8%, respectively.
DelPrete et al[14] carried out a systematic review and meta-analysis where they evaluated 26 studies, including K-wire fixation in 762 patients, plating in 195 patients, and IMHS fixation in 304 patients, where patients had a similar mean age of 31.4 years, 32.2 years, and 31.1 years for the three fixation groups, respectively. They found that the mean operative time was comparable between IMHS (21.0 minutes) and K-wires (20.8 minutes) fixation techniques, and both were shorter than plate fixation (52.6 minutes).
Generally, fracture union rates are excellent with IMHS fixation; we achieved a 100% union rate at a mean of 5.62 ± 0.99 weeks. Hug et al[15] reported fracture union in nearly all patients included in their systematic review, which occurred after a mean of 5.7 weeks (range 2-12 weeks). Poggetti et al[27] evaluated the results of IMHS fixation in 152 patients having a mean age of 34 years who presented with 173 fractures (135 metacarpals and 38 phalangeal), all fractures were extraarticular and of unstable pattern (oblique, transverse, and complex or comminuted), they reported that all fractures achieved union after a mean of 35 days, except for three open proximal phalangeal fractures and seven replantations (5.8% of all fractures), achieved radiological union after 90 days. A systematic review and meta-analysis by Morway et al[28], which evaluated 13 studies, included 603 metacarpal fractures in patients with a mean age of 32.1 years, treated with retrograde IMHS fixation. The mean time to fracture union was 5.5 ± 1.1 weeks, as reported in 8 studies, and the fracture union rate was 93.9% (range, 75.6%-100%), as reported in 4 studies.
At a mean follow-up of 101.19 ± 52.31 days, our patients achieved excellent functional outcomes, with a mean TAM of 253.15 ± 10.29 degrees, a mean QuickDASH score of 15.08 ± 11.95, and a mean hand grip strength of 98.66% ± 1.31% of the contralateral side. The results we obtained is consistent with the literature findings, after a mean last follow up of 69 days patients in Gehring et al[26] study achieved a mean QuickDASH score of 17.4, and a mean TAM of 238°, furthermore, they reported that the mean TAM was significantly better in fractures treated by closed reduction (249°) compared to those who had open reduction (210°), P < 0.05. In the systematic review by Morway et al[28], the mean hand grip strength compared with the contralateral side was 96.0% ± 6.3 as reported in 8 studies. The mean TAM was 251.6° ± 4.3° as reported in 7 studies. The mean Disabilities of the Arm, Shoulder and Hand (DASH) score was 2.5 ± 2.1, as reported in 4 studies. Poggetti et al[27] reported a mean TAM of 245 and 226 for the metacarpal and phalangeal fractures, respectively. Patients included in Hug et al’s systematic review[15] had a mean TAM of 243°, a mean handgrip strength of 97.5% of the other intact side, and a mean DASH score of 3.7 points. A recent systematic review by Peckston et al[16] included 204 proximal phalanx fractures (from 16 studies) treated with IMHS fixation. Patients had a mean age of 39 years, by the last follow up, they reported a mean TAM of 237°, a mean QuickDASH of 3.58, and a hand grip strength of 92.6% of the contralateral side. When comparing IMHS fixation to other techniques, DelPrete et al[14] reported a significantly lower mean DASH score in patients who had IMHS fixation of 0.6 (95% confidence interval: 0.2-1.0) compared to K-wire (mean of 7.4, 95% confidence interval: 4.8-9.9) and plating (mean of 9.8, 95% confidence interval: 5.3-14.3) (both P < 0.05). However, there was no difference in the TAM (the mean was 248.4°, 253.7°, and 240.7° for the IMHS fixation, plating, and K-wires, respectively). Furthermore, it was noted that the average grip strength (compared to the other side) was significantly better in IMHS fixation patients, at 104.4%, compared to 88.5% and 90.3% for K-wires and plating, respectively.
IMHS fixation is accepted as a low-complication-rate technique; however, complication rates and types have varied in the literature. In the current series, we reported an overall complication rate of 7.5%, with four fractures demonstrating symptomless hardware protrusion and one malunion; however, none required additional surgery. Furthermore, we did not report any cases with nonunion, infection, osteoarthritis, or refracture.
Anene et al[29] conducted a systematic review to evaluate complications following IMHS fixation of metacarpal fractures. Twenty-six studies were assessed, including 1014 fractures. The overall complication rate was 4.6% (47 fractures), the most common complication was stiffness (0.9%), and the least common were extension lag and loss of reduction, each representing 0.5%. The authors reported that early onset osteoarthritis and tendon adhesions were very rare; furthermore, complications related to the screws, such as bending, breakage, and migration, were infrequent, ranging from 0.2% to 0.4%. Of the 47 fractures that had complications, 18 required revision surgeries, which included open reduction and plate fixation, hardware removal, or tenolysis.
The overall complication rate in Morway et al’s systematic review[28] was 2.8% (17 out of 603 fractures), where stiffness was the most commonly occurring (in six fractures, one required tenolysis). Apart from the reported complications, refracture incidence was reported as a separate entity, which reached up to 1.5% (9 out of 603), with a resultant bend or breakage of the screws. Hardware removal was required in seven cases with subsequent fixation using a plate and screws.
Poggetti et al[27] reported malunion in 2 (1.2%) cases; however, there was no nonunion, osteoarthritis, rotational deformity, or infection. Screw removal was required in three proximal phalanx fractures, one for protrusion, and the other two were comminuted fractures, and the screw prevented primary stabilization.
Hug et al[15] reported a complication rate of 3.2%, most of which was related to hand motion limitation (2%), and open surgical teno-arthrolysis was required in about half of these cases. The overall nonunion rate was 0.6%; however, the rate was higher for proximal phalanx fractures, at 2.3%. Fracture fixation failed in 6 patients (0.7%); implant removal and refixation were required in 2 patients. Screw protrusion occurred in four cases (0.4%), three of which required implant removal. Refractures occurred in nine metacarpal fractures; seven were due to new trauma, which were treated by implant removal and refixation using plates and screws. Peckston et al[16] reported a complication rate of 6.4%, where 8 patients required hardware removal, six for prominent implants and two for infection.
DelPrete et al[14] found no differences in infection rates among fixation methods: 5% for K-wires, 3% for plating, and 2% for IMHS fixation. However, the reoperation rates were significantly lower for the IMHS fixation group 4%, compared with K-wires at 11% (P < 0.05) and plating at 11% (0.07-0.17) (P < 0.05). The most common cause for reoperation in the IMHS fixation group was repeated trauma. Finally, the complication rate we reported is relatively higher than the literature, which might be attributed to our early experience with the technique and the learning curve encountered in the first few cases.
Concerns related to the articular surface damage: The possibility of osteoarthritis secondary to articular surface damage, owing to the trans-articular nature of the procedures, is a valid concern. However, till the last follow up visit, we did not encounter any case that developed osteoarthritis. The same finding was confirmed in a longer follow-up study by Poggetti et al[27]. For the metacarpal fractures retrograde fixation (MCP joint affection), ten Berg et al[30] showed in a computed tomography model of an intact metacarpal head that 2.4 mm and 3.0 mm screws led to articular cartilage defect of 4% and 5%, respectively, which is considered minimal injury.
For the proximal phalanx fixation, in a cadaver study by Borbas et al[31], it was reported that during antegrade IMHS insertion, a proximal phalanx articular surface cartilage defect (MCP joint) of 4.6% and 8.5% when using 2.2 mm and 3.0 mm headless screws, respectively. For the retrograde fixation fashion, in a computed tomography analysis study by del Piñal et al[32], the authors reported that 2.5 mm and 3.0 mm screws will lead to articular surface defect of the proximal phalanx head (PIP) of 18% and 25% respectively.
Bekisz et al[33] assessed the possibility of articular surface damage associated with antegrade IMHS insertion for treating proximal phalangeal fractures. They compared a single screw of 2.1 mm placed via the phalanx base vs two screws of 1.8 mm placed through collateral recesses of the phalanx base. There was no difference regarding the percentage of articular surface damage between both techniques, with an average defect of 3.21% ± 2.34% with the single screw and 2.71% ± 3.42% with the two screws (P = 0.11). Furthermore, they reported that with one screw, the articular surface injury ranged between 0% to 8%, while with two screws it ranged from 0% to 15.9%.
Extensor tendon damage: Percutaneous fixation may pose a risk of extensor tendon injury, especially during drilling and screw insertion. Bekisz et al[33] reported that damage to the extensor tendon was seen in three out of the 32 evaluated digits. The injury was in two digits with the 2.1 screw and once with the 1.8 mm screw. However, all the injuries were partial, involving less than 20% of the tendon width.
In a cadaveric study by Urbanschitz et al[34], comparing percutaneous to mini-open IMHS fixation for metacarpal and phalanx fracture fixation, they used an IMHS of size 2.2 mm for phalanx and 3.0 mm for metacarpals, they showed that mini-open approach had significantly less extensor tendon damage compared to the percutaneous technique (P > 0.001); however, no case in the percutaneous fixation had an extensor tendon damage of more than 50%, which is the threshold for repair of extensor tendon injuries[35]. Moreover, Mahylis et al[36] reported that complete extensor tendon rupture after percutaneous drilling is very rare, and even if tendon lacerations reach up to 75%, they may not fail under physiological loads.
Biomechanical stability: Vanmierlo et al[37] compared the efficacy of fully threaded vs partially threaded IMHS for the fixation of proximal phalanx fractures in a biomechanical study. They evaluated six fresh frozen cadavers; a proximal transverse osteotomy was created and fixed by IMHS in an antegrade fashion. The fully threaded screws showed lower maximum elastic force and deformation than the partially threaded screws (121 N and 134 N/mm vs 165 N and 166
Cost issues: Sivakumar et al[39] collected data from the Australian health facilities in a cost analysis study comparing IMHS fixation to plate osteosynthesis of phalangeal and metacarpal fractures. The implant costs more with the plate fixation, 1088 vs 355 Australian dollars (AUD), respectively. They found that plate fixation poses a longer operative duration than IMHS fixation, 32 minutes and 25 minutes, respectively. Plates required more hardware removal surgeries, 24% vs 4.6%. They finally reported that using a plate increased healthcare expenditure of AUD 1519.41 in the public system and AUD 1698.59 in the private sector.
Although the results of the current study are promising, they should be interpreted with the following limitations in mind. First, the inherent non-comparative and descriptive nature of the current case series hinder the ability to prove the superiority of IMHS fixation over other techniques. Second, the study was carried out in a single center, and all surgeries were performed by a single surgeon, which challenges the generalizability of the technique to other facilities and to be performed by different surgeons. Third, although we included patients over a year and the number of patients was comparable to some previous studies, the study might be criticized for its relatively small sample size. Fourth, a longer follow-up is required to document the consistency of improved outcomes. Lastly, we did not carry out a cost-effectiveness analysis.
IMHS fixation is a safe and effective technique for managing metacarpal and proximal phalangeal fractures in skeletally mature patients, yielding favorable functional and radiographic outcomes with a relatively low complication rate and slightly better functional outcomes with fixation of metacarpal fractures. The encouraging results of the current study led to changes in our institution’s practice guidelines for managing extra-articular metacarpal and proximal phalanx fractures, with more surgeons adopting this technique.
We want to thank Dr. Mostafa Fayez, MD, for his support.
| 1. | Chung KC, Spilson SV. The frequency and epidemiology of hand and forearm fractures in the United States. J Hand Surg Am. 2001;26:908-915. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 538] [Cited by in RCA: 585] [Article Influence: 23.4] [Reference Citation Analysis (0)] |
| 2. | Cavalcanti Kussmaul A, Kuehlein T, Langer MF, Ayache A, Unglaub F. The Treatment of Closed Finger and Metacarpal Fractures. Dtsch Arztebl Int. 2023;120:855-862. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 21] [Article Influence: 7.0] [Reference Citation Analysis (0)] |
| 3. | van Onselen EB, Karim RB, Hage JJ, Ritt MJ. Prevalence and distribution of hand fractures. J Hand Surg Br. 2003;28:491-495. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 137] [Cited by in RCA: 174] [Article Influence: 7.6] [Reference Citation Analysis (0)] |
| 4. | Nakashian MN, Pointer L, Owens BD, Wolf JM. Incidence of metacarpal fractures in the US population. Hand (N Y). 2012;7:426-430. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 54] [Cited by in RCA: 90] [Article Influence: 6.4] [Reference Citation Analysis (0)] |
| 5. | Ootes D, Lambers KT, Ring DC. The epidemiology of upper extremity injuries presenting to the emergency department in the United States. Hand (N Y). 2012;7:18-22. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 137] [Cited by in RCA: 175] [Article Influence: 12.5] [Reference Citation Analysis (0)] |
| 6. | Christodoulou N, Asimakopoulos D, Kapetanos K, Seah M, Khan W. Principles of management of hand fractures. J Perioper Pract. 2023;33:342-349. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |
| 7. | Boeckstyns MEH. Current methods, outcomes and challenges for the treatment of hand fractures. J Hand Surg Eur Vol. 2020;45:547-559. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 16] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 8. | Colmers-Gray IN, Louison H, Kadar A. Assessment and management of common hand fractures in adults. BMJ. 2025;388:e075436. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 9. | Robinson LP, Gaspar MP, Strohl AB, Teplitsky SL, Gandhi SD, Kane PM, Osterman AL. Dorsal versus lateral plate fixation of finger proximal phalangeal fractures: a retrospective study. Arch Orthop Trauma Surg. 2017;137:567-572. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 27] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 10. | Eberlin KR, Babushkina A, Neira JR, Mudgal CS. Outcomes of closed reduction and periarticular pinning of base and shaft fractures of the proximal phalanx. J Hand Surg Am. 2014;39:1524-1528. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 46] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 11. | Neumeister MW, Winters JN, Maduakolum E. Phalangeal and Metacarpal Fractures of the Hand: Preventing Stiffness. Plast Reconstr Surg Glob Open. 2021;9:e3871. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 14] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 12. | Thomas TL, Kachooei AR, Ilyas AM. Intramedullary K-wires versus Alternate Techniques for Metacarpal Shaft and Neck Fractures: A Systematic Review and Meta-analysis. J Hand Microsurg. 2023;15:376-387. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 13. | Guidi M, Frueh FS, Besmens I, Calcagni M. Intramedullary compression screw fixation of metacarpal and phalangeal fractures. EFORT Open Rev. 2020;5:624-629. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 25] [Article Influence: 4.2] [Reference Citation Analysis (0)] |
| 14. | DelPrete CR, Chao J, Varghese BB, Greenberg P, Iyer H, Shah A. Comparison of Intramedullary Screw Fixation, Plating, and K-Wires for Metacarpal Fracture Fixation: A Meta-Analysis. Hand (N Y). 2025;20:691-700. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 10] [Article Influence: 10.0] [Reference Citation Analysis (0)] |
| 15. | Hug U, Fiumedinisi F, Pallaver A, van de Wall BJM, Beeres FJP, Giesen T, Liechti R. Intramedullary screw fixation of metacarpal and phalangeal fractures - A systematic review of 837 patients. Hand Surg Rehabil. 2021;40:622-630. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 33] [Article Influence: 6.6] [Reference Citation Analysis (0)] |
| 16. | Peckston DC, Faulkner H, Graham DJ, Sivakumar BS. Intramedullary Compression Screw Fixation of Proximal Phalanx Fractures: An Updated Systematic Review. Hand (N Y). 2025;15589447251329597. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 17. | Chao J, Patel A, Shah A. Intramedullary Screw Fixation Comprehensive Technique Guide for Metacarpal and Phalanx Fractures: Pearls and Pitfalls. Plast Reconstr Surg Glob Open. 2021;9:e3895. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 30] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 18. | Boulton CL, Salzler M, Mudgal CS. Intramedullary cannulated headless screw fixation of a comminuted subcapital metacarpal fracture: case report. J Hand Surg Am. 2010;35:1260-1263. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 52] [Cited by in RCA: 80] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
| 19. | Hassan K, Blumenthal S, Jehle CC, Sobel AD. Intramedullary Fixation of Hand Fractures and Arthrodeses. J Hand Surg Am. 2024;49:42-49. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 4] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 20. | Megahed AA, Khalifa AA, Ragheb YF, Saleh WR. Surgical techniques for intramedullary headless screw fixation of metacarpal and proximal phalanx fractures. J Musculoskelet Surg Res. 2026;10:123-130. [RCA] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 21. | Bain GI, Polites N, Higgs BG, Heptinstall RJ, McGrath AM. The functional range of motion of the finger joints. J Hand Surg Eur Vol. 2015;40:406-411. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 71] [Cited by in RCA: 77] [Article Influence: 7.0] [Reference Citation Analysis (0)] |
| 22. | American Society of Hand Therapists. Clinical Assessment Recommendations. [cited 3 August 2025]. Available from: https://asht.org/practice/clinical-assessment-recommendations. |
| 23. | Moradi A, Menendez ME, Kachooei AR, Isakov A, Ring D. Update of the Quick DASH Questionnaire to Account for Modern Technology. Hand (N Y). 2016;11:403-409. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 12] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 24. | Ibrahim K, May CR, Patel HP, Baxter M, Sayer AA, Roberts HC. Implementation of grip strength measurement in medicine for older people wards as part of routine admission assessment: identifying facilitators and barriers using a theory-led intervention. BMC Geriatr. 2018;18:79. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 18] [Cited by in RCA: 47] [Article Influence: 5.9] [Reference Citation Analysis (0)] |
| 25. | Humar P, Thayer J, Bengur FB, Villalvazo Y, Hu M, Unadkat J. Early Return of Motion in Patients With Intramedullary Screw Placement for Metacarpal and Phalangeal Fracture Fixation. Ann Plast Surg. 2024;92:S136-S141. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 26. | Gehring MB, Wolfe B, Kahan R, Malliaris SD, Washington KM, Folchert MD, Ipaktchi K, Greyson MA, Lauder A, Iorio ML. Intramedullary Fixation for Metacarpal Fractures: A Multi-Institutional Prospective Outcomes Study. J Hand Surg Glob Online. 2025;7:48-55. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 8] [Reference Citation Analysis (0)] |
| 27. | Poggetti A, Fagetti A, Lauri G, Cherubino M, Borelli PP, Pfanner S. Outcomes of 173 metacarpal and phalangeal fractures treated by intramedullary headless screw fixation with a 4-year follow-up. J Hand Surg Eur Vol. 2021;46:466-470. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 20] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 28. | Morway GR, Rider T, Jones CM. Retrograde Intramedullary Screw Fixation for Metacarpal Fractures: A Systematic Review. Hand (N Y). 2023;18:67-73. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 32] [Article Influence: 10.7] [Reference Citation Analysis (0)] |
| 29. | Anene CC, Thomas TL, Matzon JL, Jones CM. Complications Following Intramedullary Screw Fixation for Metacarpal Fractures: A Systematic Review. J Hand Surg Am. 2024;49:1043.e1-1043.e16. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 16] [Article Influence: 8.0] [Reference Citation Analysis (0)] |
| 30. | ten Berg PW, Mudgal CS, Leibman MI, Belsky MR, Ruchelsman DE. Quantitative 3-dimensional CT analyses of intramedullary headless screw fixation for metacarpal neck fractures. J Hand Surg Am. 2013;38:322-330.e2. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 55] [Cited by in RCA: 81] [Article Influence: 6.2] [Reference Citation Analysis (0)] |
| 31. | Borbas P, Dreu M, Poggetti A, Calcagni M, Giesen T. Treatment of proximal phalangeal fractures with an antegrade intramedullary screw: a cadaver study. J Hand Surg Eur Vol. 2016;41:683-687. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 44] [Article Influence: 4.4] [Reference Citation Analysis (0)] |
| 32. | del Piñal F, Moraleda E, Rúas JS, de Piero GH, Cerezal L. Minimally invasive fixation of fractures of the phalanges and metacarpals with intramedullary cannulated headless compression screws. J Hand Surg Am. 2015;40:692-700. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 102] [Cited by in RCA: 163] [Article Influence: 14.8] [Reference Citation Analysis (0)] |
| 33. | Bekisz JM, Chinta SR, Cuccolo NG, Thornburg D, Bass JL, Agrawal NA. Articular Surface Damage Following Headless Intramedullary Nail Fixation of Proximal Phalanx Fractures. J Hand Surg Am. 2025;50:1004.e1-1004.e6. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 3] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 34. | Urbanschitz L, Dreu M, Wagner J, Kaufmann R, Jeserschek JM, Borbas P. Cartilage and extensor tendon defects after headless compression screw fixation of phalangeal and metacarpal fractures. J Hand Surg Eur Vol. 2020;45:601-607. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 33] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 35. | Colzani G, Tos P, Battiston B, Merolla G, Porcellini G, Artiaco S. Traumatic Extensor Tendon Injuries to the Hand: Clinical Anatomy, Biomechanics, and Surgical Procedure Review. J Hand Microsurg. 2016;8:2-12. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 34] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 36. | Mahylis JM, Burwell AK, Bonneau L, Marshall LM, Mirarchi AJ. Drill Penetration Injury to Extensor Tendons: A Biomechanical Analysis. Hand (N Y). 2017;12:301-306. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 8] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 37. | Vanmierlo B, Vandekerckhove B, Popleu L, Eijnde BO, Duerinckx J, Goubau JF. Fully Threaded Versus Partially Threaded Intramedullary Headless Compression Screw Fixation for Proximal Third Fractures of the Proximal Phalanx: A Biomechanical Study. J Hand Surg Am. 2025;50:1520.e1-1520.e8. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 38. | Dyrna FGE, Avery DM 3rd, Yoshida R, Lam D, Oeckenpöhler S, Cote MP, Obopilwe E, Rodner CM, Mazzocca AD. Metacarpal shaft fixation: a biomechanical comparison of dorsal plating, lag screws, and headless compression screws. BMC Musculoskelet Disord. 2021;22:335. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 21] [Article Influence: 4.2] [Reference Citation Analysis (0)] |
| 39. | Sivakumar BS, Vaotuua DL, McCarron L, Graham DJ. Cost Analysis of Intramedullary Screw versus Plate Osteosynthesis for Phalangeal and Metacarpal Fractures: An Observational Study. J Hand Surg Asian Pac Vol. 2023;28:369-376. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |