Published online Mar 18, 2026. doi: 10.5312/wjo.v17.i3.117393
Revised: December 29, 2025
Accepted: January 26, 2026
Published online: March 18, 2026
Processing time: 100 Days and 19.2 Hours
Osteoporotic vertebral compression fractures with bilateral pedicle fractures represent a rare and severe subtype. Unlike typical osteoporotic vertebral com
We report the case of a 93-year-old male who presented with low back pain and numbness in the right lower limb following a fall. Preoperative computed to
This surgical approach, performed under local anesthesia, offers a minimally invasive treatment option for osteoporotic vertebral fractures with bilateral pedicle fractures.
Core Tip: We present a case of a traumatic osteoporotic vertebral compression fracture accompanied by bilateral pedicle fractures, in which the patient's lower back pain and lower extremity symptoms were successfully alleviated through percutaneous vertebroplasty combined with bilateral headless cannulated screw fixation under local anesthesia. Compared to conventional approaches requiring general anesthesia, this technique is markedly less invasive, can be performed under local anesthesia, and may represent a novel minimally invasive alternative for the management of similar cases in the future.
- Citation: Long JQ, Yang H, Cheng YW, Shen T, Zou JY, Zhang GW. Percutaneous vertebroplasty and compression screw fixation for osteoporotic vertebral fractures with bilateral pedicle fractures: A case report. World J Orthop 2026; 17(3): 117393
- URL: https://www.wjgnet.com/2218-5836/full/v17/i3/117393.htm
- DOI: https://dx.doi.org/10.5312/wjo.v17.i3.117393
Osteoporosis is a common systemic skeletal disorder characterized by reduced bone mass and deterioration of bone microarchitecture, leading to an increased risk of fractures[1]. Osteoporotic vertebral compression fractures (OVCFs) are among the ten most significant global health conditions[2,3], potentially leading to a range of adverse outcomes, including chronic pain, kyphotic deformity, unintentional weight loss, depression, diminished quality of life, and even mortality[4,5]. Although the prognostic implications of different surgical interventions remain debated[6], percutaneous vertebroplasty (PVP) and percutaneous kyphoplasty are widely used to treat OVCFs due to their short operative time, suitability for local anesthesia, and rapid pain relief[4,7,8]. However, beyond typical OVCFs, Lotan and Hershkovich[9] identified a bipedicular dissociation fracture pattern in elderly patients with osteoporotic vertebral fractures, suggesting increased trauma severity and spinal instability. In contrast to typical OVCFs, bilateral pedicle fractures may result in neurological deficits[10]. Conservative treatment and standalone PVP have been shown to yield unsatisfactory the
A 93-year-old male patient of East Asian descent presented with low back pain and numbness in the right lower limb following a fall.
The patient presented with back pain accompanied by pain and numbness in the right lower limb following a fall at home 10 days earlier. The Visual Analogue Scale (VAS) score was 8 for low back pain and 7 for lower extremity pain. The pain was exacerbated by rotational movements and alleviated by supine rest. Numbness and pain in the right lower extremity were localized to the anterior thigh.
He has a history of hypertension and chronic obstructive pulmonary disease. Other than that, he has no history of other chronic diseases and no prior symptoms of low back pain, leg pain, or intermittent claudication.
The patient had no relevant personal or family medical history.
The physical examination revealed positive spinal percussion tenderness and a positive Lasegue’s sign in the right lower extremity. Additionally, the patient presents with numbness and pain in the anterior aspect of the thigh, without significant decrease in lower limb muscle strength, and no pathological signs are elicited.
Routine laboratory examinations revealed no significant abnormalities.
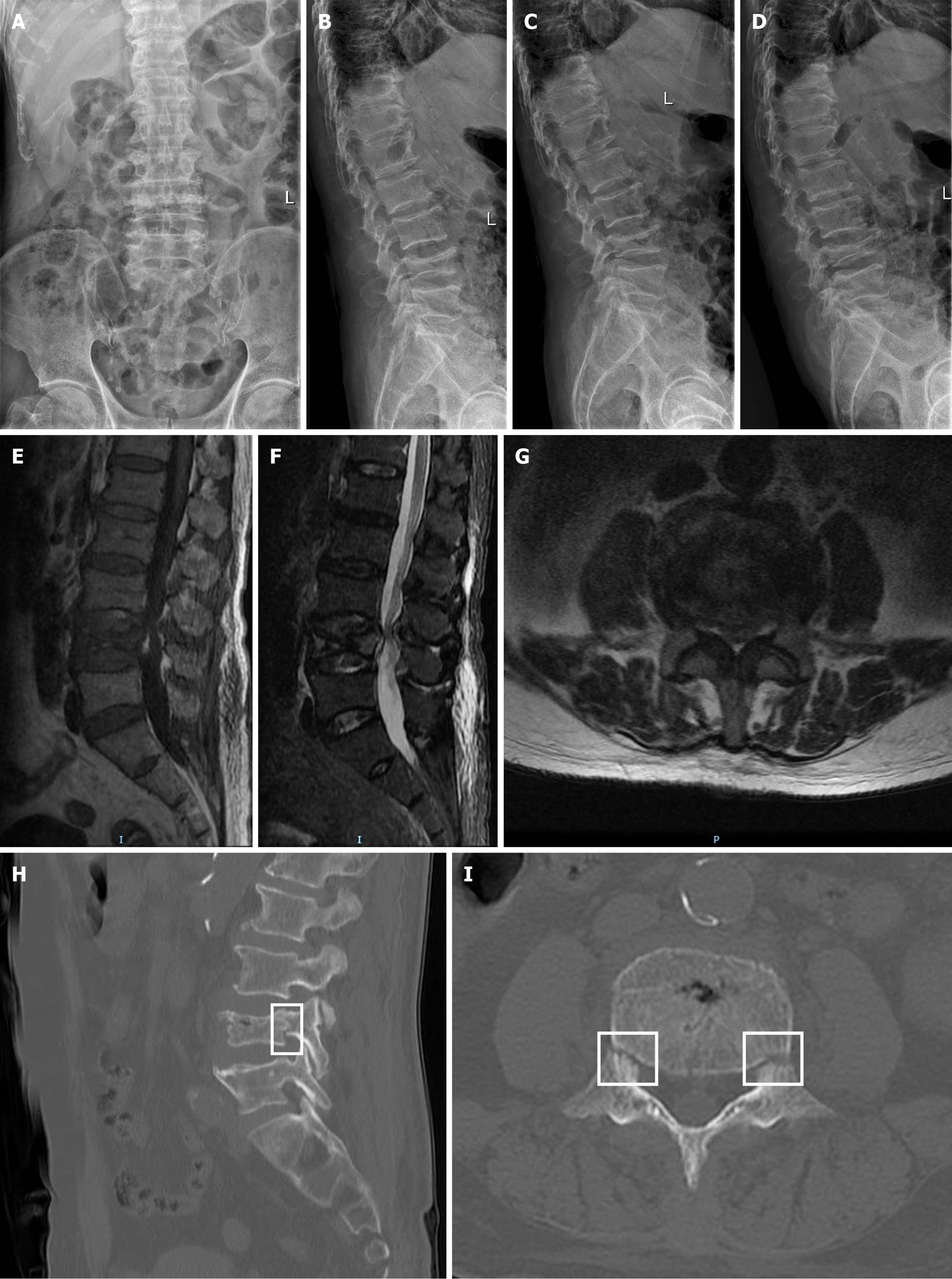
Anteroposterior and lateral digital radiographs (DR) of the lumbar spine demonstrated a reduction in L4 vertebral body height, consistent with a compression fracture (Figure 1A and B). Comparative analysis of hyperextension and hyper
Based on clinical manifestations and imaging findings, the final diagnosis was established as an L4 OVCF with bilateral pedicle fractures and spinal canal stenosis. Unlike typical cases of OVCF, this patient presented with neurological symptoms in the right lower extremity. Therefore, PVP alone may not have been sufficient to fully relieve the associated symptoms.
Following a literature review and multidisciplinary discussion, the patient underwent PVP combined with headless compression cannulated screw fixation under local anesthesia. For preoperative selection of pedicle screw parameters, the internal fixation screw length (50 mm) was determined by measuring the distance from the facet joint to the anterior-middle one-third of the vertebral body on preoperative CT imaging. The screw diameter (6.5 mm) was selected based on the standard pedicle screw dimensions typically used for this vertebral level.
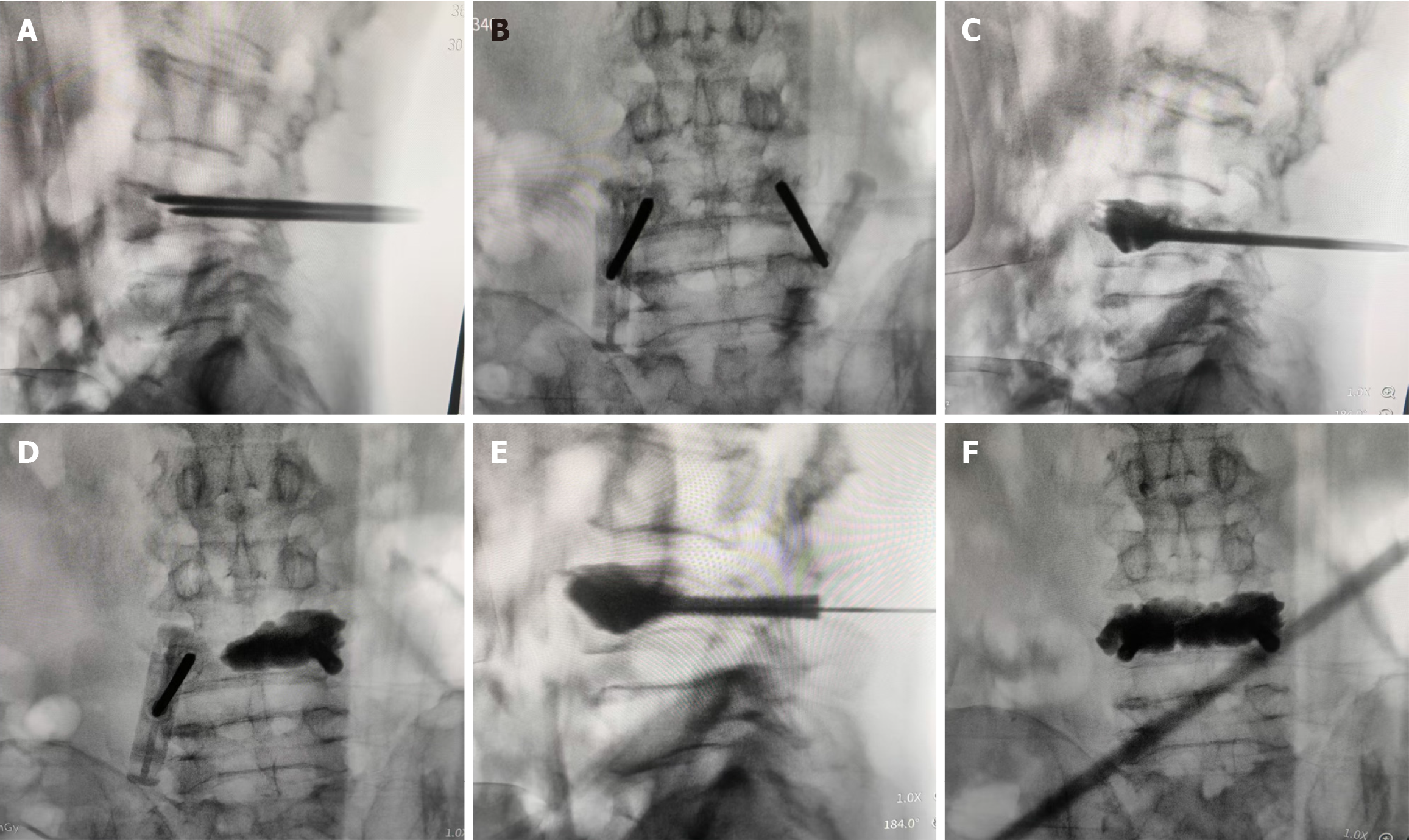
Preemptive analgesia was administered via intravenous injection of non-steroidal anti-inflammatory drugs prior to the surgical procedure. During the operation, bilateral pedicle punctures were performed. Puncture needles (inner diameter: 3.5 mm; manufacturer: Wego, China) were advanced into the anterior-to-middle third of the L4 vertebral body under fluoroscopic guidance (Figure 2A and B). Following intraoperative confirmation and unilateral injection of polymethyl methacrylate (PMMA), the pusher rod was withdrawn, and a 1.5-mm Kirschner wire was inserted through the puncture needle. A headless cannulated compression screw (diameter: 6.5 mm; length: 50 mm; Carewayer, China) was then introduced into the vertebral body along the Kirschner wire. The same procedure was performed on the contralateral side. Final fluoroscopic assessment confirmed adequate PMMA distribution (total volume: Approximately 6 mL) and proper screw positioning (Figure 2F). The surgical procedure lasted approximately 40 minutes, with an intraoperative blood loss of around 5 mL.
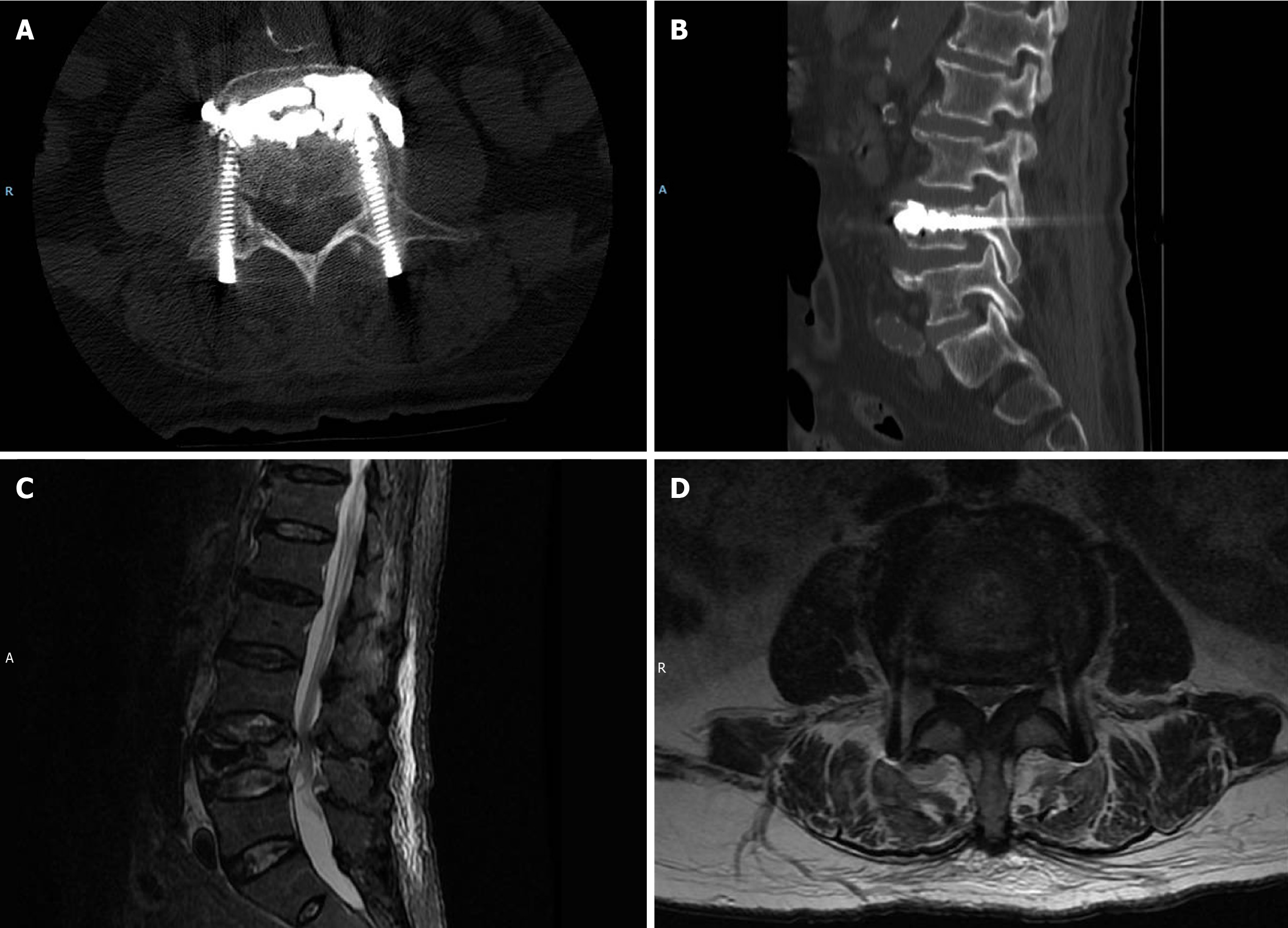
Postoperatively, the patient received symptomatic management with analgesics, mannitol, and corticosteroids. On the second postoperative day, ambulation was initiated with the assistance of a walker and a lumbar stabilization device (Video). The patient reported significant improvement in lumbar pain and right lower limb symptoms compared with preoperative levels. Additionally, the VAS score for low back pain decreased from 8 preoperatively to 2 postoperatively, and the score for lower extremity pain improved from 7 to 3. A postoperative review of imaging studies was conducted. CT confirmed satisfactory PMMA distribution and demonstrated that the screws traversed the pedicles, effectively achieving compression and closure at the fracture site (Figure 3A and B). Concurrently, postoperative MRI revealed increased spinal canal and right lateral recess space at the inferior L3/4 level compared to preoperative findings (Figure 3C and D).
Following discharge, the patient was prescribed teriparatide at 20 μg/day, along with daily supplementation of 1.5 g calcium carbonate and 0.5 μg calcitriol. The patient was also instructed to wear a lumbar brace for two months and to ambulate with a walker as needed, gradually discontinuing assistive devices as lower extremity muscle strength improved.
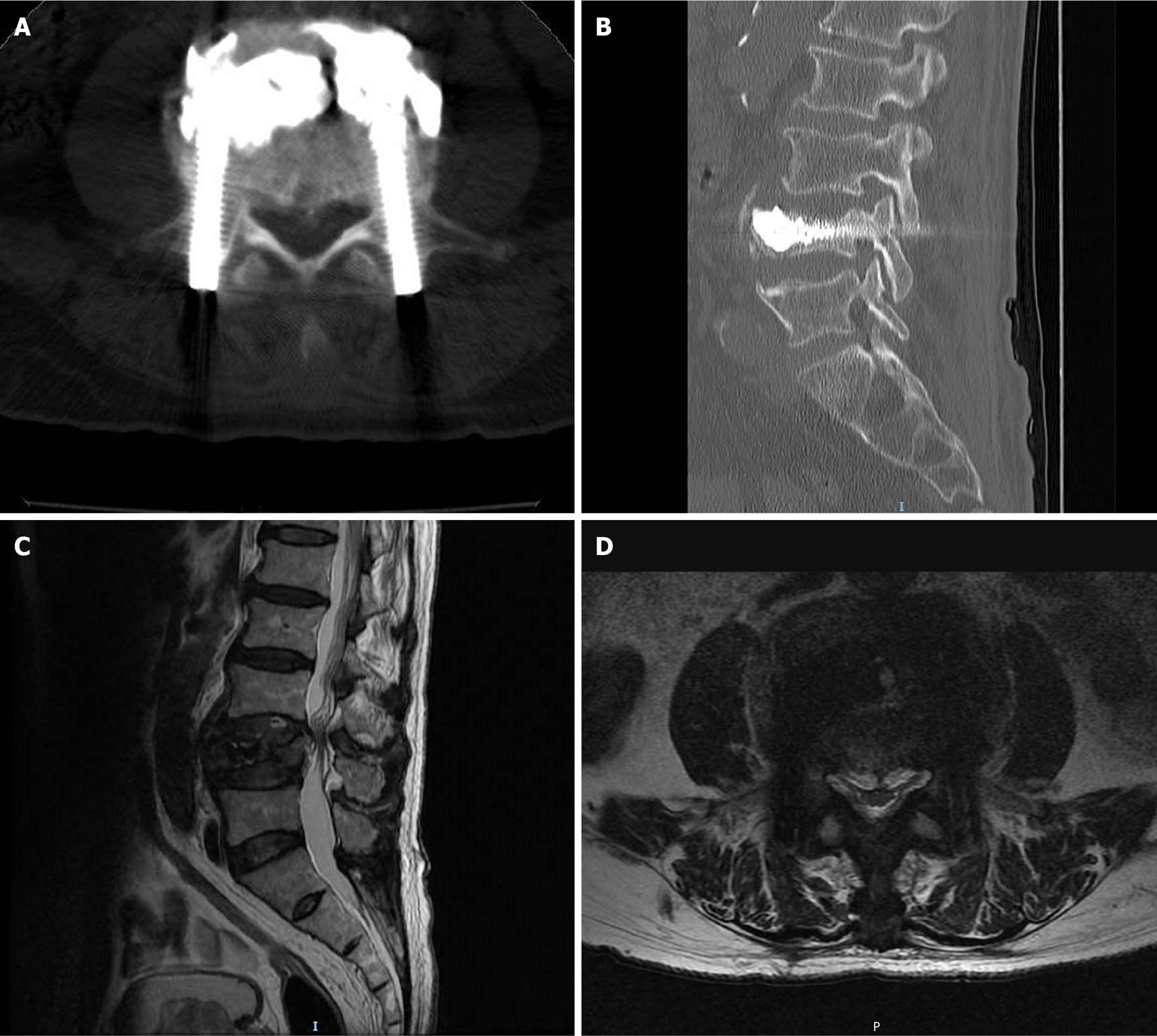
At the three-month follow-up visit, the patient presented to the outpatient clinic for evaluation. Lumbar pain had resolved (VAS 0), and only occasional numbness in the lower limb was reported (VAS 0-1). The numbness did not interfere with daily activities, and the patient ambulated independently without assistive devices. Follow-up MRI and CT demonstrated a hazy appearance at the bilateral pedicle fracture sites, indicative of complete bone healing (Figure 4A). Additionally, the spinal canal at the inferior L3/4 level remained essentially unchanged compared to prior imaging (Figure 4B).
In contrast to typical OVCFs, bilateral pedicle fractures at the junction between the vertebral arch and body have received comparatively limited attention. The etiology of this fracture pattern is multifactorial, with reported risk factors including prior lumbar spine surgery[11,12] and prolonged physical activity[13,14]. However, growing evidence suggests that bilateral pedicle stress fractures may also occur spontaneously[10,15,16], potentially associated with long-term corticosteroid use[17]. Due to the spinal instability caused by bilateral pedicle fractures, vertebral fusion using hydroxyapatite-enhanced pedicle screw fixation has been considered a more conventional treatment approach[15]. Although substantial advancements have been made in minimally invasive therapies for OVCFs-such as percutaneous stent-kyphoplasty using the SpineJack® system[18]-the management of OVCFs complicated by bilateral pedicle fractures remains a significant clinical challenge.
Recently, Lotan and Hershkovich[9] proposed a new subtype of osteoporotic fracture-OVCF with bilateral pedicle separation fractures-which closely resembles the condition observed in this case. This fracture type predominantly affects the lower thoracic and lumbar regions, particularly T11-L3, and is strongly associated with severe trauma, spinal instability[9], and neurological symptoms in the lower extremities[10]. In the present case, the patient experienced low back pain and lower extremity symptoms following trauma and was diagnosed with an L4 OVCF with bilateral pedicle fractures, accompanied by lumbar spinal stenosis at the L3/4 level (Figure 1).
To date, there is no clear consensus regarding the optimal treatment of OVCF with bilateral pedicle fractures. Some patients with uncomplicated OVCF may present with lower extremity symptoms, and PVP on the symptomatic side has been reported to significantly alleviate radicular leg pain[19]. However, that study included only seven successfully treated patients and lacked robust data support. Consequently, for symptomatic patients with OVCF and bilateral pedicle fractures, the primary treatment approach has traditionally involved open lumbar decompression and fusion with internal fixation, which effectively relieves neural compression but is associated with high surgical invasiveness[20,21].
However, Lotan et al[22] proposed a novel surgical technique combining balloon kyphoplasty (BKP) with percutaneous pedicle screw fixation performed under general anesthesia. Similar to the technique used in this case, their approach involved restoring vertebral height with BKP, injecting PMMA, and stabilizing the fracture site with pedicle screws to achieve indirect decompression. Their data demonstrated that five patients underwent surgical intervention, all of whom experienced favorable clinical and functional outcomes.
Additionally, a comparable technique-stent-screw-assisted internal fixation (SAIF), has been reported in the manage
This case report describes a 93-year-old patient with multiple chronic comorbidities. In elderly individuals, surgical procedures performed under general anesthesia carry a significantly elevated risk. Following a comprehensive review of the literature and multidisciplinary discussion, PVP combined with headless compression cannulated screw fixation was performed under local anesthesia to minimize surgical risk. Anterior column stability was achieved by PMMA injection, while the fracture sites were compressed, fixed, and anchored within the PMMA using headless cannulated compression screws (Figure 2). These screws are designed with different thread pitches at each end and an unthreaded central shaft, allowing the threaded ends to draw fracture fragments together and generate compression[28]. Moreover, the use of smaller-diameter headless cannulated compression screws enabled a more minimally invasive approach, suitable for local anesthesia.
Importantly, a comprehensive postoperative evaluation was conducted to assess the necessity of additional decom
As previously noted, OVCFs with bilateral pedicle fractures are indicative of increased spinal instability. In such cases, neither conservative management nor kyphoplasty alone appears sufficient to restore vertebral stability or promote effective fracture healing. Compared to open surgery, BKP combined with percutaneous pedicle screw fixation under general anesthesia significantly reduces surgical trauma; however, it still involves the inherent risks associated with general anesthesia. In contrast to the BKP with percutaneous pedicle screw and SAIF, our surgical approach effectively reduces operative duration and can be performed under local anesthesia, despite not employing stents or balloon-assisted vertebral height restoration. This approach-achieved by further reducing screw diameter to minimize soft tissue dis
Undoubtedly, this procedure carries risks associated with cement leakage, similar to those observed in vertebroplasty. Based on our experience, adequate bone cement volume should be used to fill the space between the superior and inferior endplates of the vertebral body in the coronal plane, ideally extending to or beyond the midline. In the sagittal plane, cement distribution should avoid approaching the posterior margin of the vertebral body. Intraoperatively, it is essential to ensure that the needle tip reaches the anterior to middle third of the vertebral body and to avoid premature injection of PMMA to reduce the risk of cement extravasation. PMMA administration must be halted immediately if the cement nears the posterior vertebral cortex, with careful fluoroscopic monitoring of its distribution throughout the procedure.
Additionally, this surgical approach involves inherent risks such as stress fractures in adjacent spinal segments and long-term internal fixation failure. Therefore, standardized anti-osteoporosis treatment and structured postoperative rehabilitation guidance are critically important to support fracture healing and maintain surgical outcomes.
Nevertheless, further accumulation of clinical cases is warranted to validate the efficacy and safety of this surgical approach. Although this technique achieves indirect neural decompression by reducing and fixing the pedicle, complete resolution of lower extremity symptoms cannot be guaranteed in all cases. Compression fixation may result in foraminal stenosis or fail to achieve anatomical reduction, potentially leading to new or persistent nerve compression. In cases involving severe pedicle fracture displacement or inadequate indirect decompression with ongoing neurological sy
We reported a case of OVCF accompanied by bilateral pedicle fractures. Following PVP combined with transpedicular headless compression cannulated screw fixation, the patient experienced substantial relief from low back pain and right lower limb radicular symptoms. Compared with conventional treatment strategies, this technique is minimally invasive and eliminates the need for general anesthesia and decompressive surgery in elderly patients. However, the number of reported cases remains limited. Further follow-up and accumulation of additional cases are necessary to comprehensively evaluate the feasibility, safety, and long-term outcomes of this approach.
All authors would like to extend their sincere appreciation to the patient and his family for kindly granting permission to use the clinical data and materials for publication and academic exchange purposes.
| 1. | Ensrud KE, Crandall CJ. Osteoporosis. Ann Intern Med. 2017;167:ITC17-ITC32. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 315] [Cited by in RCA: 569] [Article Influence: 63.2] [Reference Citation Analysis (0)] |
| 2. | Dai C, Liang G, Zhang Y, Dong Y, Zhou X. Risk factors of vertebral re-fracture after PVP or PKP for osteoporotic vertebral compression fractures, especially in Eastern Asia: a systematic review and meta-analysis. J Orthop Surg Res. 2022;17:161. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 80] [Cited by in RCA: 111] [Article Influence: 27.8] [Reference Citation Analysis (0)] |
| 3. | Hu L, Sun H, Wang H, Cai J, Tao Y, Feng X, Wang Y. Cement injection and postoperative vertebral fractures during vertebroplasty. J Orthop Surg Res. 2019;14:228. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 28] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 4. | Long Y, Yi W, Yang D. Advances in Vertebral Augmentation Systems for Osteoporotic Vertebral Compression Fractures. Pain Res Manag. 2020;2020:3947368. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 20] [Cited by in RCA: 91] [Article Influence: 15.2] [Reference Citation Analysis (0)] |
| 5. | Jalava T, Sarna S, Pylkkänen L, Mawer B, Kanis JA, Selby P, Davies M, Adams J, Francis RM, Robinson J, McCloskey E. Association between vertebral fracture and increased mortality in osteoporotic patients. J Bone Miner Res. 2003;18:1254-1260. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 187] [Cited by in RCA: 207] [Article Influence: 9.0] [Reference Citation Analysis (0)] |
| 6. | Longo UG, Loppini M, Denaro L, Maffulli N, Denaro V. Osteoporotic vertebral fractures: current concepts of conservative care. Br Med Bull. 2012;102:171-189. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 59] [Cited by in RCA: 79] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 7. | Yuan WH, Hsu HC, Lai KL. Vertebroplasty and balloon kyphoplasty versus conservative treatment for osteoporotic vertebral compression fractures: A meta-analysis. Medicine (Baltimore). 2016;95:e4491. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 52] [Cited by in RCA: 63] [Article Influence: 6.3] [Reference Citation Analysis (0)] |
| 8. | Tao W, Hu Q, Nicolas YSM, Nuo X, Daoyu H, Zhen J, Jinpeng S, Jun L. Is unilateral transverse process-pedicle percutaneous kyphoplasty a better choice for osteoporotic thoracolumbar fractures in the old patients? BMC Surg. 2021;21:252. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 15] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 9. | Lotan R, Hershkovich O. A Novel Bipedicular Dissociation Fracture Pattern of Vertebral Osteoporotic Fractures of the Elderly. J Am Acad Orthop Surg Glob Res Rev. 2024;8:e23.00241. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 10. | Schmid T, Heini P, Benneker L. A rare case of non-traumatic, multi-level, bilateral pedicle fractures of the lumbar spine in a 60-year-old patient. Eur Spine J. 2017;26:197-201. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 14] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 11. | Ha KY, Kim YH. Bilateral pedicle stress fracture after instrumented posterolateral lumbar fusion: a case report. Spine (Phila Pa 1976). 2003;28:E158-E160. [PubMed] |
| 12. | Ampe N, Meersman P, Ghysen D, Kegelaers B, Gorris C, Debeuf J, Van Wambeke P, Schreurs M. Lumbar Pedicular Stress Fracture Post-laminectomy: a Case Report. SN Compr Clin Med. 2022;4:221. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 13. | Amari R, Sakai T, Katoh S, Sairyo K, Higashino K, Tachibana K, Yasui N. Fresh stress fractures of lumbar pedicles in an adolescent male ballet dancer: case report and literature review. Arch Orthop Trauma Surg. 2009;129:397-401. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 32] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 14. | Parvataneni HK, Nicholas SJ, McCance SE. Bilateral pedicle stress fractures in a female athlete: case report and review of the literature. Spine (Phila Pa 1976). 2004;29:E19-E21. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 34] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 15. | Kim HS, Kim SW, Lee WT. Spondylolisthesis accompanying bilateral pedicle stress fracture at two vertebrae. J Korean Neurosurg Soc. 2012;51:388-390. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 11] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 16. | Han SH, Hyun SJ, Jahng TA, Kim KJ. Posterior osteosynthesis of a spontaneous bilateral pedicle fracture of the lumbar spine. J Neurosurg Spine. 2016;24:398-401. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 12] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 17. | Hajjioui A, Khazzani H, Sbihi S, Bahiri R, Benchekroune B, Hajjaj-Hassouni N. Spondylolisthesis on bilateral pedicle stress fracture in the lumbar spine: a case study. Ann Phys Rehabil Med. 2011;54:53-58. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 18] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 18. | Karner M, Osterhoff G, Sprengel K, Pape HC, Scherer J. The Use of Percutaneous Stent-Kyphoplasty (SpineJack®) in Osteoporotic and Non-Osteoporotic Vertebral Fractures: A Retrospective Analysis of 310 Implants From a Level-1 Trauma Center in Switzerland. Global Spine J. 2025;16:21925682251347225. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 19. | Han S, Park HS, Pee YH, Oh SH, Jang IT. The clinical characteristics of lower lumbar osteoporotic compression fractures treated by percutaneous vertebroplasty: a comparative analysis of 120 cases. Korean J Spine. 2013;10:221-226. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 7] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 20. | Doita M, Ando Y, Hirata S, Ishikawa H, Kurosaka M. Bilateral pedicle stress fracture in a patient with osteoporotic compression fracture. Eur Spine J. 2009;18 Suppl 2:206-209. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 22] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 21. | Ebot J, Bohnen AM, Abode-Iyamah K. Bilateral Acute Osteoporotic Lumbar Pedicle Fracture Presenting with Associated Neurological Deficit: A Case Report and Review of Literature. Cureus. 2020;12:e7273. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 2] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 22. | Lotan R, Shpigelman A, Hershkovich O. A Novel Intravertebral Fixation Technique of Lumbar Osteoporotic Vertebral Bipedicular Dissociation Fractures. J Am Acad Orthop Surg Glob Res Rev. 2025;9:e24.00372. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 23. | Yonezawa N, Yonezawa Y, Nishimura T, Yamashiro T, Shimozaki K, Mori A, Demura S, Tsuchiya H. Vertebra-Pediculoplasty: A New Approach to Treatment of Split-Type and Delayed-Union Osteoporotic Vertebral Fracture with a Risk of Cement Dislodgement. World Neurosurg. 2021;155:e55-e63. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 10] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 24. | Cianfoni A, Distefano D, Isalberti M, Reinert M, Scarone P, Kuhlen D, Hirsch JA, Bonaldi G. Stent-screw-assisted internal fixation: the SAIF technique to augment severe osteoporotic and neoplastic vertebral body fractures. J Neurointerv Surg. 2019;11:603-609. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 51] [Article Influence: 6.4] [Reference Citation Analysis (0)] |
| 25. | La Barbera L, Cianfoni A, Ferrari A, Distefano D, Bonaldi G, Villa T. Stent Screw-Assisted Internal Fixation (SAIF) of Severe Lytic Spinal Metastases: A Comparative Finite Element Analysis of the SAIF Technique. World Neurosurg. 2019;128:e370-e377. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 21] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 26. | Distefano D, Scarone P, Isalberti M, La Barbera L, Villa T, Bonaldi G, Hirsch JA, Cianfoni A. The 'armed concrete' approach: stent-screw-assisted internal fixation (SAIF) reconstructs and internally fixates the most severe osteoporotic vertebral fractures. J Neurointerv Surg. 2021;13:63-68. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 38] [Article Influence: 6.3] [Reference Citation Analysis (0)] |
| 27. | La Barbera L, Cianfoni A, Ferrari A, Distefano D, Bonaldi G, Villa T. Stent-Screw Assisted Internal Fixation of Osteoporotic Vertebrae: A Comparative Finite Element Analysis on SAIF Technique. Front Bioeng Biotechnol. 2019;7:291. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 29] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 28. | Berk T, Zderic I, Schwarzenberg P, Pastor T, Lesche F, Halvachizadeh S, Richards RG, Gueorguiev B, Pape HC. Evaluation of cannulated compression headless screws as an alternative implant for superior pubic ramus fracture fixation: a biomechanical study. Int Orthop. 2023;47:1079-1087. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 7] [Article Influence: 2.3] [Reference Citation Analysis (0)] |