Published online Mar 18, 2026. doi: 10.5312/wjo.v17.i3.115288
Revised: November 9, 2025
Accepted: January 6, 2026
Published online: March 18, 2026
Processing time: 153 Days and 15.5 Hours
Obesity is increasingly common among patients undergoing total ankle arthroplasty (TAA), yet its influence on perioperative outcomes, implant survivorship, and patient-reported outcomes remains unclear.
To understand this relationship, which is essential for patient counseling, perioperative planning, and policy.
This systematic review, registered with the Open Science Framework and conducted per Preferred Reporting Items for Systematic Reviews and Meta-Analyses guidelines, searched PubMed, the Cochrane Library, and CINAHL through August 2025 using: (arthroplasty OR replacement) AND ankle AND (outcome OR complication) AND obesity. Eligible studies compared obese and non-obese TAA patients. Extracted data included perioperative complications, implant revision, survivorship, and patient-reported outcome measures. Risk of bias was assessed with the Newcastle-Ottawa Scale, and due to heterogeneity, results were narratively synthesized.
Fourteen studies encompassing over 20000 patients were included. Institutional series generally found no significant association between obesity and perioperative complications, while larger databases reported increased infection, thromboembolism, and systemic risks. Implant survival findings were mixed: Institutional cohorts showed no difference, whereas registry data indicated higher revision risk. Obese patients had lower baseline function but achieved comparable, meaningful improvements. Morbidly obese patients also improved without higher short-term complication rates.
Thus, obesity should not be a contraindication for TAA, though individualized counseling on risks and benefits is recommended.
Core Tip: Obesity should not preclude total ankle arthroplasty. Although large datasets show higher complication risks, obese and morbidly obese patients experience functional improvements comparable to non-obese individuals. Pain relief, mobility, and patient-reported outcomes improve meaningfully. With appropriate patient selection, counseling, and perioperative risk management, surgeons can make careful, inclusive decisions rather than excluding patients based solely on body mass, and individualized expectations across diverse clinical settings.
- Citation: Pinto I, Konstantinou P, Kostretzis L, Nikolaides AP, Ditsiou AZ, Chrysanthou C, Kapetanakis S, Ditsios K. Obesity and total ankle arthroplasty: Contraindication or consideration. World J Orthop 2026; 17(3): 115288
- URL: https://www.wjgnet.com/2218-5836/full/v17/i3/115288.htm
- DOI: https://dx.doi.org/10.5312/wjo.v17.i3.115288
Total ankle arthroplasty (TAA) has become an increasingly accepted treatment for end-stage ankle arthritis, offering pain relief and the possibility of preserving motion, in contrast to ankle arthrodesis, which eliminates joint mobility and may accelerate degeneration in adjacent joints[1]. As the procedure has become more common, attention has shifted toward the influence of patient-related factors on surgical risk, functional recovery, and implant longevity. Among these factors, obesity is of particular interest given its rising prevalence and its well-documented impact on other forms of joint replacement[2,3]. Despite theoretical concerns, the published evidence regarding the influence of obesity on TAA outcomes is inconsistent[4]. Some institutional cohorts have found no difference in complication rates or survivorship between obese and non-obese patients, while others, particularly those based on national databases, suggest higher rates of perioperative morbidity and even reduced implant survival[5,6]. The diversity of study designs, body mass index (BMI) definitions, outcome measures, and follow-up intervals has made interpretation difficult[7]. Furthermore, relatively few investigations distinguish between different classes of obesity, leaving uncertainty about whether risks increase in a dose-dependent manner.
Clarifying the relationship between obesity and outcomes after TAA is important for several reasons. Surgeons must be able to counsel patients realistically about the risks and expected benefits of surgery, especially as the prevalence of obesity continues to rise. Health systems are increasingly focused on value-based care, and identifying modifiable risk factors can help optimize patient selection and perioperative management. Finally, understanding whether obesity should influence candidacy for TAA has direct implications for clinical guidelines and policy decisions. For these reasons, we undertook a systematic review of a narrative synthesis of observational studies to assess the impact of obesity on outcomes following TAA. Our objective was to synthesize evidence regarding perioperative complications, implant revision and survivorship, and patient-reported outcomes in obese compared with non-obese populations. By providing a comprehensive overview of the available data, this review aims to guide clinicians and patients in shared decision-making and to highlight areas where further research is needed.
This systematic review was conducted in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses guidelines. The review protocol was prospectively registered with the Open Science Framework prior to data collection and analysis. The research question was structured using the population, intervention, comparison, and outcome framework, with the population defined as adult patients undergoing TAA, the intervention being the procedure itself in patients with obesity, the comparison group being non-obese patients, and the outcomes of interest including perioperative complications, implant survivorship, revision rates, and patient-reported outcome measures (PROMs).
A comprehensive electronic literature search was performed across three major databases: PubMed, the Cochrane Library, and CINAHL. The search covered all publications from database inception through August 2025. The Boolean query employed was: (arthroplasty OR replacement) AND ankle AND (outcome OR complication) AND obesity. No restrictions were placed on language or publication date during the initial search, although only articles published in English were considered for inclusion at the full-text review stage. In addition to database searching, the reference lists of relevant reviews and included articles were manually screened to identify additional eligible studies.
Two reviewers (Pinto I and Konstantinou P) independently screened the titles and abstracts of all retrieved records. Studies that clearly did not address TAA, obesity, or clinical outcomes were excluded at this stage. The full text of potentially eligible articles was then assessed against predefined inclusion and exclusion criteria. We included cohort studies, registry analyses, case-control studies, and randomized controlled trials that reported outcomes of TAA in obese vs non-obese patients, or that specifically analyzed obesity or BMI as a predictor variable. Exclusion criteria were narrative reviews, expert opinion articles, case reports, technique notes, studies focused exclusively on ankle arthrodesis, and studies without stratification by obesity or BMI.
Data were extracted independently by two reviewers (Pinto I and Konstantinou P) using a standardized form that captured study design, setting, sample size, demographics, BMI definitions and categories, number of obese vs non-obese patients, follow-up duration, and reported outcomes. Outcomes of interest included perioperative complications, long-term outcomes including revision and implant survivorship, and functional results based on validated PROMs. When available, adjusted effect estimates such as odds ratios, hazard ratios, or regression coefficients were extracted along with their 95% confidence intervals. Interrater reliability for study selection was assessed using Cohen’s kappa[8]. Values above 0.80 were interpreted as almost perfect agreement, 0.61-0.80 as substantial, 0.41-0.60 as moderate, 0.21-0.40 as fair, and 0.20 or lower as slight agreement.
Risk of bias for the included studies was assessed using the Newcastle-Ottawa Scale, which evaluates methodological quality across three domains: Selection of participants, comparability of cohorts, and ascertainment of outcomes[9]. Each study could achieve a maximum of nine stars, with higher scores indicating lower risk of bias. Assessments were conducted independently by two reviewers (Pinto I and Kostretzis L), and disagreements were resolved by consensus.
Given the heterogeneity of study designs, outcome measures, and follow-up durations, a quantitative meta-analysis was not feasible. Instead, results were synthesized narratively and presented in tabular form, highlighting differences between obese and non-obese cohorts across the main outcome categories. Where multiple studies addressed the same outcome with comparable methods, findings were qualitatively integrated to provide an overall impression of the direction and strength of evidence. No statistical conversions were undertaken, and data were reported as presented in the original studies. Missing summary statistics were not imputed. Outcomes from individual studies were organized by domain and summarized in tables detailing study characteristics and principal findings.
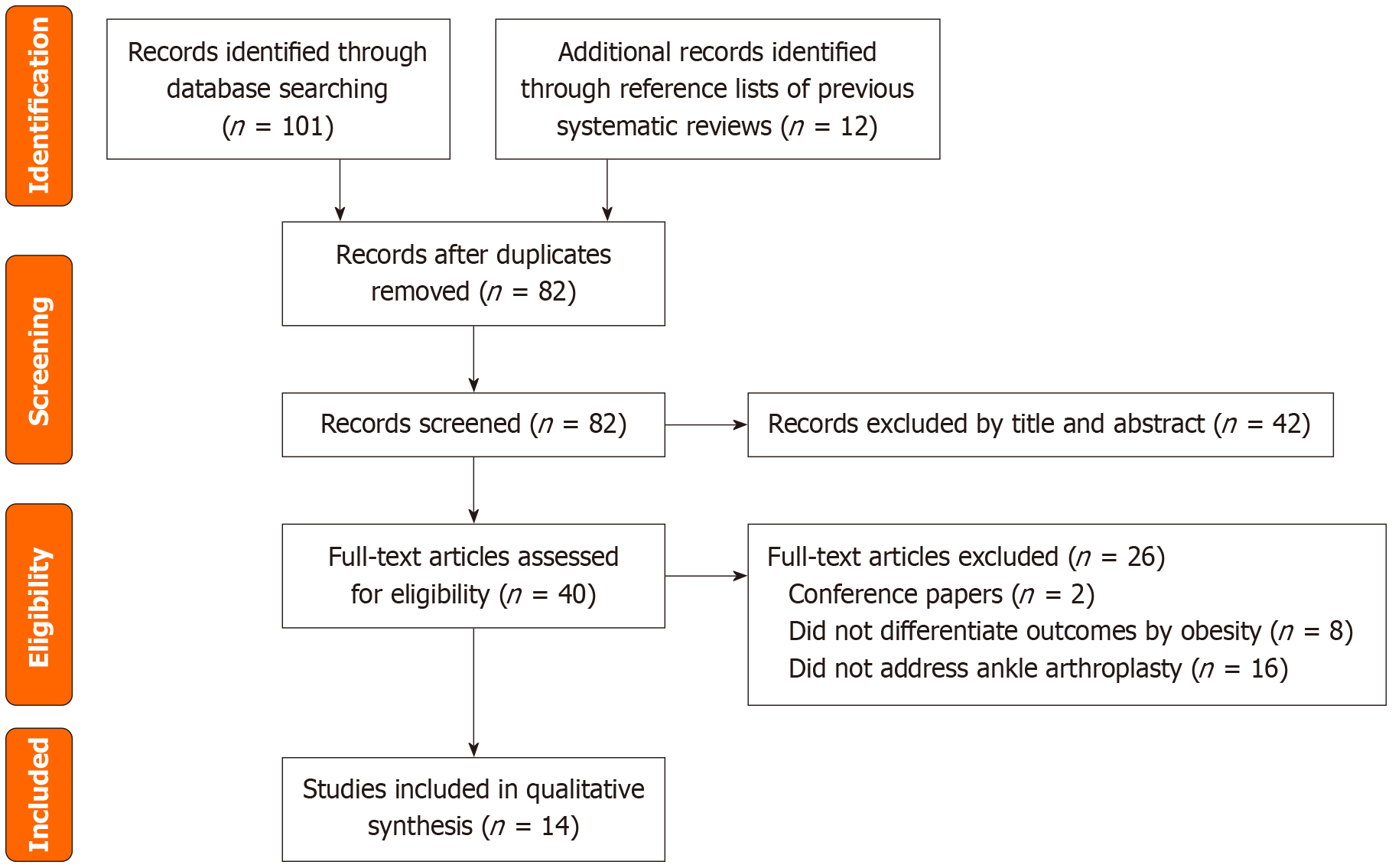
The process of study selection was documented in a Preferred Reporting Items for Systematic Reviews and Meta-Analyses flow diagram (Figure 1). In total, 113 records were identified: 111 through database searches and an additional 12 through reference lists of previous systematic reviews. After removing duplicates, 82 studies remained, of which 42 were excluded based on title and abstract screening. Finally, a total of 14 articles met all eligibility criteria and were included in the qualitative synthesis (Table 1)[5,6,10-21]. Agreement between reviewers was high across screening stages, with a kappa of 0.833 during title and abstract screening and 0.832 during full-text review, both indicating almost perfect agreement. The 14 included studies were published between 2011 and 2025 and represented a combination of retro
| Ref. | Design | Level of evidence | Patients | Age (years), mean | Gender (n of males) | Obese patients (n) | Mean follow-up |
| Bakaes et al[10], 2024 | NSQIP database | III | 2026 | NR | NR | 26 | 30 days |
| Barg et al[19], 2011 | Single institution | IV | 118 | 59.8 ± 11.6 | 61 | 118 | 67.7 ± 27.0 months |
| Best et al[17], 2022 | NSQIP database | III | 294 | 64 ± 12 | 132 | 133 | 30 days |
| Bouchard et al[21], 2015 | Single institution | III | 87 | 62.44 ± 8.42 | 39 | 39 | 3.92 years |
| Cottom et al[13], 2019 | Single institution | III | 97 | 66.4 | 43 | 44 | 26.3 months |
| Cunningham et al[16], 2018 | Single institution | IV | 1024 | 63 ± 10.5 | 528 | 278 | 90 days |
| Sy et al[15], 2025 | NSQIP database | III | 1704 | 52.2 ± 9.5 | 937 | 899 | 30 days |
| Gross et al[20], 2016 | Single institution | III | 455 | 62.5 ± 8.2 | 204 | 189 | 3.7 years |
| Jennison et al[11], 2023 | National registry (United Kingdom) | III | 5562 | 67.8 ± 10.1 | 3308 | 1497 | 5.0 years |
| Kim et al[6], 2023 | Single institution | III | 1093 | 63.7 ± 8.52 | 558 | 478 | 5.6 years |
| Kwon et al[18], 2023 | NSQIP database | III | 1333 | 63.3 ± 11.2 | 707 | NR | 30 days |
| Sambandam et al[14], 2023 | NIS database | III | 5087 | 65.1 ± 10.3 | 2748 | 1033 | Inpatient |
| Schipper et al[5], 2016 | Single institution | III | 97 | 58.2 ± 9.1 | 52 | 49 | 8.2 ± 2.0 years |
| Werner et al[12], 2015 | PearlDiver database | III | 5361 | NR | 2593 | 1115 | 7.0 years (revision), 90 days (complications) |
Most institutional series and short-term cohorts did not find obesity to be an independent risk factor for perioperative complications. Gross et al[20] reported no difference in complication rates between obese and non-obese patients at a minimum of two years follow-up, while Bouchard et al[21] similarly found no association in a smaller cohort of 87 patients. Cunningham et al[16], in a prospective institutional cohort of 1024 patients, observed that BMI was not a predictor of 90-day readmission, emergency department visits, or wound complications. Cottom et al[13] and Kim et al[6], both single-institution series, also reported no significant differences in complication rates between groups. Analyses of the National Surgical Quality Improvement Program (NSQIP) database have reached similar conclusions. Best et al[17], Kwon et al[18], and Bakaes et al[10] all reported that BMI was not associated with 30-day complications, readmission, or reoperation, even when stratifying complications as major or minor.
In contrast, larger administrative databases have suggested increased perioperative risk. Werner et al[12], using the PearlDiver database of more than 5000 TAAs, found that obese patients had significantly higher odds of 90-day complications, including infection [odds ratio (OR) = 2.2], venous thromboembolism (OR = 3.6), and systemic complications (OR = 3.4). Sambandam et al[14], in an analysis of over 5000 patients from the National Inpatient Sample database, reported higher rates of in-hospital medical complications such as anemia and acute renal failure in obese and morbidly obese patients. Sy et al[15], also using the NSQIP database, noted that patients with obesity were nearly twice as likely to be discharged to a non-home destination following surgery, even after adjusting for preoperative functional and metabolic status.
Overall, while institutional cohorts and moderate-sized database analyses[10,17,18] consistently failed to show an effect of obesity on perioperative complications, larger administrative databases[12,14] demonstrated increased risks of medical morbidity in obese patients. Complication outcomes are presented in Table 2[6,10,12-18,20,21].
| Ref. | Overall rate | Infection/wound complications | 90-day readmission | ARF | ||||||||
| Obese | Non-obese | P value | Obese | Non-obese | P value | Obese | Non-obese | P value | Obese | Non-obese | P value | |
| Gross et al[20], 2016 | 11% | 16.5% | 0.196 | 0.5% | 2.26% | 0.431 | NR | NR | NR | NR | NR | NR |
| Bouchard et al[21], 2015 | Similar | Similar | 0.48 | 0% | 2.1% | NS | NR | NR | NR | NR | NR | NR |
| Cunningham et al[16], 2018 | NR | NR | NR | 1.82% | 3.85% | 0.28 | 1.32% | 4.1% | 0.99 | NR | NR | NR |
| Cottom et al[13], 2019 | 11.4% | 18.9% | 0.308 | NR | NR | NS | NR | NR | NR | NR | NR | NR |
| Kim et al[6], 2023 | 21.8% | 27% | 0.126 | 0.4% | 1.3% | 0.274 | NR | NR | NR | NR | NR | NR |
| Best et al[17], 2022 | 3.8% | 2.5% | 0.5301 | NR | NR | NR | NR | NR | NR | NR | NR | NR |
| Kwon et al[18], 2023 | Non-associated with BMI | NR | 0.6% | Non-associated with BMI | 1.4% | Non-associated with BMI2 | NR | NR | NR | |||
| Bakaes et al[10], 2024 | 2.6% | 12% | 0.436 | 7.8% | 15.7% | NS | NR | NR | NR | 0% | 0% | > 0.05 |
| Werner et al[12], 2015 | Significantly increased risk for obese patients | < 0.001 | 4.7% | 2.2% | < 0.001 | NR | NR | NR | NR | NR | NR | |
| Sambandam et al[14], 2023 | NR | NR | NR | NR | NR | NR | NR | NR | NR | 15 | 22 | 0.0023 |
| Sy et al[15], 2025 | NR | NR | NR | NR | NR | NR | BMI > 30 is associated with non-home dischargea,4 | < 0.01 | NR | NR | NR | |
Long-term institutional cohorts reported mixed findings. Schipper et al[5], in a single-surgeon series of 97 patients with a mean follow-up of eight years, found that obese patients had significantly higher odds of implant failure (adjusted OR = 2.8), a difference that was not apparent at intermediate follow-up but emerged only with longer-term observation. In contrast, several other institutional cohorts did not demonstrate a clear association. Barg et al[19], in a prospective series of 118 patients with a mean follow-up of six years, reported comparable implant survival between obese and non-obese patients (93% vs 94%). Gross et al[20], in 455 patients with a minimum two-year follow-up, observed no significant difference in revision rates by BMI status. Bouchard et al[21], in a cohort of 87 patients, reported slightly higher but non-significant revision rates in obese patients. Cottom et al[13], with a mean follow-up of two years, reported no revisions in either group, and Kim et al[6], in a United States institutional series of 1093 patients, also found no difference in implant survival across BMI categories. Database and registry analyses consistently suggested worse implant survival in obese patients. Werner et al[12] found that obesity was associated with higher odds of revision (OR = 1.6). Similarly, Jennison et al[11], in a United Kingdom registry study of more than 5500 patients, reported a significantly lower five-year survival rate for obese patients (88.9%) compared with non-obese patients.
In aggregate, institutional series provide conflicting results, with some suggesting increased risk of implant failure while others report no association. In contrast, both large database and registry studies consistently indicate that obesity is linked with higher revision risk or reduced implant survival. Taken together, these findings suggest that obesity may modestly increase the likelihood of late implant failure, although the strength of this effect remains uncertain. An overview of revision rates and implant survival findings is provided in Table 3[5,6,11-13,19-21].
| Ref. | Revision rate | Survivorship | ||||
| Obese | Non-obese | P value | Obese | Non-obese | P value | |
| Schipper et al[5], 2016 | 42.9% | 31.3% | 0.041 | NS2 | NS2 | 0.3 |
| Barg et al[19], 2011 | 19.5% | - | NR | 93%3 | - | NR |
| Gross et al[20], 2016 | 4.1% | 3.0% | 0.861 | NR | NR | NR |
| Bouchard et al[21], 2015 | 17.9% | 8.4% | 0.48 | 4.5 years4 | 4.6 years4 | 0.47 |
| Cottom et al[13], 2019 | 0% | 0% | - | NR | NR | NR |
| Kim et al[6], 2023 | No association of BMI and implant failure | 0.896 | NR | NR | NR | |
| Werner et al[12], 2015 | Significantly increased risk for obese patients | 0.0045 | NR | NR | NR | |
| Jennison et al[11], 2023 | NR | NR | - | 88.9% | 94.0% | 0.026 |
Gross et al[20] reported that obese patients had lower absolute functional scores compared with non-obese patients at final follow-up; however, both groups experienced significant improvements in pain and function from baseline. Kim et al[6] similarly found that although obese patients reported worse preoperative and postoperative PROMs overall, the magnitude of improvement after surgery was comparable to that of non-obese controls. Finally, Bouchard et al[21] observed that obese patients presented with greater disability and worse function preoperatively, yet TAA significantly and similarly improved pain and disability scores in both obese and non-obese groups. Taken together, these studies indicated that while obese patients started and remained at lower absolute PROM levels compared with non-obese patients, they consistently achieved substantial and clinically meaningful improvements following TAA. Patient-PROMs are summarized in Table 4[6,20,21].
| Ref. | Functional measure | Preoperative | Statistical significance of difference (P value) | Postoperative | Main finding | Statistical significance of difference (P value) | ||
| Obese | Non-obese | Obese | Non-obese | |||||
| Gross et al[20], 2016 | SMFA function | 88.0 ± 17.4 | 81.9 ± 18.2 | 0.002 | 61.7 ± 19.9 | 54.9 ± 20.0 | Obese patients had lower absolute functional scores compared with non-obese patients at final follow-up | 0.009 |
| FADI | 61.2 ± 7.7 | 54.5 ± 14.1 | 0.014 | 24.5 ± 17.3 | 16.2 ± 15.7 | 0.003 | ||
| FAOS pain | 42.0 ± 18.4 | 46.3 ± 17.2 | 0.795 | 77.6 ± 18.5 | 84.8 ± 17.3 | 0.038 | ||
| SF-36 total | 44.7 ± 17.5 | 49.5 ± 17.9 | 0.03 | 63.6 ± 20.3 | 73.7 ± 20.8 | < 0.001 | ||
| Kim et al[6], 2023 | FADI, mean | 58.17 ± 8.35 | 52.62 ± 14.32 | 0.008 | 21.65 ± 16.26 | 17.71 ± 16.61 | Obese patients reported worse preoperative and postoperative PROMs overall | 0.041 |
| SMFA, mean | 37.92 ±13.13 | 33.18 ± 13.60 | 0.001 | 20.13 ± 13.69 | 15.36 ± 14.12 | < 0.001 | ||
| SF-36, mean | 47.10 ± 16.37 | 52.93 ± 18.07 | 0.002 | 64.78 ± 19.96 | 73.44 ± 19.92 | < 0.001 | ||
| AOFAS hindfoot, mean | 39.38 ± 15.73 | 42.33 ± 17.15 | 0.213 | 73.94 ± 15.8 | 77.74 ± 15.38 | 0.039 | ||
| FAOS pain, mean | 35.70 ± 16.98 | 46.85 ± 18.42 | < 0.001 | 76.28 ± 19.88 | 81.84 ± 18.85 | 0.006 | ||
| Bouchard et al[21], 2015 | AOS pain | 55.88 ± 18.00 | 52.92 ± 19.41 | 0.47 | 19.59 ± 18.50 | 19.00 ± 16.80 | Ankle arthroplasty significantly and similarly improved pain and disability scores in both obese and non-obese groups | 0.93 |
| AOS disability | 68.64 ± 14.09 | 59.79 ± 19.57 | NS | 28.21 ± 21.51 | 27.20 ± 19.33 | 0.82 | ||
| SF-36-PCS | 29.54 ± 6.92 | 34.48 ± 9.05 | 0.01 | 39.21 ± 10.30 | 40.30 ± 9.84 | 0.62 | ||
| SF-36-MCS | 50.86 ± 12.72 | 53.70 ± 11.24 | 0.32 | 50.51 ± 13.37 | 54.05 ± 9.27 | 0.30 | ||
Three studies stratified outcomes by obesity class, providing specific data on morbidly obese patients (BMI ≥ 40). Bakaes et al[10] found no significant differences in 30-day complications between non-obese, obese, and morbidly obese patients. Gross et al[20] reported that while obese and morbidly obese patients had lower absolute functional scores compared with non-obese individuals, implant survival did not differ significantly between groups. Similarly, Kim et al[6] observed that morbidly obese patients achieved significant postoperative improvements in PROMs, with the magnitude of functional gain comparable to other BMI groups, although postoperative scores remained lowest in absolute terms. These findings suggested that morbid obesity did not independently increase the risk of short-term complications or implant failure after TAA, but patients in this group might have had persistently lower functional scores despite achieving substantial improvements.
Risk of bias assessment using the Newcastle-Ottawa Scale indicated that most studies scored between six and nine stars, reflecting a generally moderate to low risk of bias (Table 5)[5,6,11-21]. Two studies[16,17] achieved nine stars and were rated at low risk, while two large database analyses[12,14] scored six stars, indicating moderate risk. The most common limitations were a lack of multivariable adjustment for confounders, reliance on administrative coding for exposure or outcomes, and restricted follow-up periods that limited evaluation of long-term implant survivorship. Institutional series were often limited by small sample size and generalizability, whereas registry and database studies, although larger, were constrained by coding accuracy and missing clinical detail.
| Ref. | Selection (0-4) | Comparability (0-2) | Outcome (0-3) | Total NOS | Risk of bias |
| Bakaes et al[10], 2024 | 4 | 1 | 3 | 8/9 | Low |
| Barg et al[19], 2011 | 3 | 0 | 3 | 6/9 | Moderate |
| Best et al[17], 2022 | 4 | 2 | 3 | 9/9 | Low |
| Bouchard et al[21], 2015 | 4 | 1 | 3 | 8/9 | Low |
| Cottom et al[13], 2019 | 4 | 0 | 3 | 7/9 | Moderate |
| Cunningham et al[16], 2018 | 4 | 2 | 3 | 9/9 | Low |
| Sy et al[15], 2025 | 4 | 2 | 2 | 8/9 | Low |
| Gross et al[20], 2016 | 4 | 0 | 3 | 7/9 | Moderate |
| Jennison et al[11], 2023 | 4 | 2 | 2 | 8/9 | Low |
| Kim et al[6], 2023 | 4 | 1 | 2 | 7/9 | Moderate |
| Kwon et al[18], 2023 | 4 | 2 | 2 | 8/9 | Low |
| Sambandam et al[14], 2023 | 4 | 0 | 2 | 6/9 | Moderate |
| Schipper et al[5], 2016 | 4 | 2 | 2.5 | 8/9 | Low |
| Werner et al[12], 2015 | 3.5 | 0 | 2.5 | 6/9 | Moderate |
This systematic review synthesized evidence from 14 studies examining the effect of obesity on outcomes following TAA. Obesity was associated with a modestly increased risk of perioperative complications and possibly reduced long-term implant survival in some large database and registry studies, while smaller institutional cohorts often found no such association. Across all settings, however, patient-reported outcomes consistently demonstrated that obese patients achieved substantial and clinically meaningful improvements in pain and function.
Our review adds to a growing body of work exploring modifiable risk factors in TAA. The prevalence of obesity continues to rise globally, and it is increasingly encountered among patients presenting with end-stage ankle arthritis. Concerns regarding obesity stem from both biomechanical and systemic considerations. The tibiotalar joint has a smaller articular surface compared with the hip or knee, leading to higher contact stresses under equivalent loads[22,23]. In obese individuals, the increased axial load across this relatively small surface magnifies mechanical stress at the bone-implant interface, which may accelerate polyethylene wear, promote talar component subsidence, and contribute to premature loosening. At the same time, obesity is associated with systemic inflammation, impaired wound healing, and increased risk of medical complications, which could compromise both early recovery and long-term implant survival[24,25]. This evidence has even prompted some centers to introduce BMI thresholds for elective arthroplasty, though such policies remain controversial[26,27].
Regarding perioperative complications, smaller institutional and mid-sized database studies generally reported no significant association between obesity and adverse outcomes[16,17,20]. These cohorts, often based on prospectively maintained clinical data, benefited from detailed variable capture and adjustment for confounders. Conversely, larger administrative datasets identified higher odds of systemic complications, wound problems, and infection among obese patients[12,14]. This discrepancy likely reflects differences in data granularity and methodology: Institutional studies provide precise clinical documentation, whereas large administrative datasets, though extensive, are prone to misclassification bias arising from coding-based definitions of exposure and outcome. Notably, Sy et al[15] also observed that obesity predicted non-home discharge, implying that even in the absence of increased complications, excess body weight may prolong recovery and increase postoperative resource use.
The evidence on revision and implant survivorship showed a similar dichotomy. Several institutional series[6,19-21] reported no significant effect of obesity on implant survival, although sample sizes were limited and follow-up was relatively short in many of these studies. In contrast, Schipper et al’s long-term single-surgeon cohort[5] did report significantly higher failure rates among obese patients, suggesting that risks may accumulate over time. Furthermore, both large-scale database and registry analyses consistently demonstrated an association between obesity and increased revision risk or reduced implant survival[11,12]. Collectively, these data support the hypothesis that while obesity may not always be detectable as a risk factor in smaller or mid-term series, its impact becomes evident in larger and longer-term datasets.
Findings on functional outcomes were remarkably consistent across studies. Gross et al[20], Kim et al[6], and Bouchard et al[21] each demonstrated that obese patients exhibited lower preoperative function and continued to report lower absolute PROMs postoperatively; however, the magnitude of improvement was comparable to that observed in non-obese cohorts. This indicates that obesity does not attenuate the expected symptomatic relief or functional gains following TAA, even though postoperative scores remain lower in absolute terms. From a counselling standpoint, these data highlight that obese patients can anticipate substantial, clinically meaningful improvement, but expectations should be framed in relation to their baseline status. Noteworthy, studies stratifying by obesity class[6,10,20] suggest that morbidly obese patients achieve substantial improvements after TAA without higher short-term complication or implant failure rates, though their absolute functional scores remain lower than those of non-obese patients.
This review has several limitations. Follow-up duration varied substantially, with many database analyses restricted to in-hospital or 30-day outcomes, limiting evaluation of long-term implant survivorship. Exposure and outcome as
Despite these limitations, the review has notable strengths. It represents the most comprehensive synthesis to date of obesity and outcomes after TAA, encompassing 14 studies and more than 20000 patients across multiple health systems and geographic regions. The systematic approach, prospective protocol registration, and duplicate screening and extraction procedures minimize the risk of selection and reporting bias. By including both detailed institutional cohorts and large-scale registry and administrative database analyses, the review provides a balanced assessment of risks and benefits in real-world practice.
Future research should focus on prospective multicentre studies with sufficient power to stratify by obesity class and follow patients over the long term. Such studies would allow for a more nuanced understanding of how varying degrees of obesity influence both functional recovery and implant survival following TAA. In addition, future investigations should take into consideration that the use of standardised definitions for complications, revisions, and PROMs would greatly facilitate comparisons across studies and enhance the reproducibility of findings. Consistent terminology and outcome reporting frameworks would also enable more robust meta-analyses and support the development of evidence-based clinical guidelines. Moreover, integrating registry data with detailed clinical variables - such as implant type, alignment, surgical technique, and soft-tissue quality - could help elucidate the mechanisms through which obesity influences both short- and long-term outcomes. Future research should also explore modifiable risk factors and evaluate the effectiveness of targeted interventions aimed at improving outcomes in obese and morbidly obese patients. This includes the assessment of risk-reduction strategies such as preoperative weight optimisation, management of comorbid conditions, and the implementation of tailored rehabilitation protocols that address the unique biomechanical and physiological challenges faced by this population. Collaborative multicentre or registry-based studies with large, diverse patient cohorts may further strengthen the external validity of findings and help guide individualised perioperative care strategies.
This systematic review found that obesity should not be considered a contraindication for TAA. Evidence from large registry and administrative database studies suggests that obese patients may face higher risks of perioperative complications and late implant failure, whereas institutional series often report no significant association. Importantly, across all settings, obese patients consistently achieved substantial and clinically meaningful improvements in pain and function, even if their absolute scores remained lower than those of non-obese patients. Surgeons should counsel obese patients regarding both the potential risks and the expected functional gains, while future research should focus on prospective multicenter studies with long-term follow-up and adequate adjustment for confounding factors to better define the impact of obesity on implant outcomes.
| 1. | Kwon DG, Chung CY, Park MS, Sung KH, Kim TW, Lee KM. Arthroplasty versus arthrodesis for end-stage ankle arthritis: decision analysis using Markov model. Int Orthop. 2011;35:1647-1653. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 24] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 2. | Baum G, Jacobs H, Lazovic D, Maus U, Hoffmann F, Seeber GH. The influence of obesity on functional outcomes and patient satisfaction 8 weeks after total knee arthroplasty: results of the prospective FInGK study. BMC Musculoskelet Disord. 2022;23:949. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 8] [Reference Citation Analysis (0)] |
| 3. | Aggarwal VA, Sambandam S, Wukich D. The Impact of Obesity on Total Hip Arthroplasty Outcomes: A Retrospective Matched Cohort Study. Cureus. 2022;14:e27450. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 10] [Reference Citation Analysis (0)] |
| 4. | Varga C, Váncsa S, Agócs G, Hegyi P, Gidró BT, Szőke G, Domos G, Rodler E, Kocsis G, Holnapy G. Obesity and Ankle Prosthesis Revision: A Systematic Review and Meta-analysis. Foot Ankle Int. 2023;44:1305-1318. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 5. | Schipper ON, Denduluri SK, Zhou Y, Haddad SL. Effect of Obesity on Total Ankle Arthroplasty Outcomes. Foot Ankle Int. 2016;37:1-7. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 53] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 6. | Kim BI, Anastasio AT, Wixted CM, DeOrio JK, Nunley JA 2nd, Easley ME, Adams SB Jr. Total Ankle Arthroplasty: Does Obesity Matter? Foot Ankle Int. 2023;44:587-595. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 17] [Article Influence: 5.7] [Reference Citation Analysis (0)] |
| 7. | Wu YL, Li D, Vermund SH. Advantages and Limitations of the Body Mass Index (BMI) to Assess Adult Obesity. Int J Environ Res Public Health. 2024;21:757. [RCA] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 169] [Reference Citation Analysis (0)] |
| 8. | Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics. 1977;33:159-174. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 60504] [Cited by in RCA: 42786] [Article Influence: 873.2] [Reference Citation Analysis (4)] |
| 9. | Wells GA, Shea BJ, O’Connell D, Peterson J, Welch V, Losos M, Tugwell P. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. 2020. [cited 3 August 2025]. Available from: https://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. |
| 10. | Bakaes Y, Gonzalez T, Hardin JW, Benjamin Jackson Iii J. Effect of body mass index on acute postoperative complications following Total Ankle Arthroplasty (TAA). Foot Ankle Surg. 2024;30:226-230. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 11. | Jennison T, Ukoumunne OC, Lamb S, Sharpe I, Goldberg A. Risk Factors for Failure of Total Ankle Replacements: A Data Linkage Study Using the National Joint Registry and NHS Digital. Foot Ankle Int. 2023;44:596-603. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 13] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 12. | Werner BC, Burrus MT, Looney AM, Park JS, Perumal V, Cooper MT. Obesity Is Associated With Increased Complications After Operative Management of End-Stage Ankle Arthritis. Foot Ankle Int. 2015;36:863-870. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 49] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 13. | Cottom JM, Plemmons BS, Douthett SM. Relationship Between Body Mass Index and Complications in Total Ankle Arthroplasty: A Single Surgeon's Experience in Ninety-Seven Replacements. J Foot Ankle Surg. 2019;58:687-691. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 8] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 14. | Sambandam S, Senthil T, Serbin P, Viswanathan VK, Mounasamy V, Wukich D. Analysis of Baseline Characteristics, Length of Stay, Cost of Care, Complications and Subgroup Analysis of Patients Undergoing Total Ankle Arthroplasty-A Large Database Study. J Foot Ankle Surg. 2023;62:310-316. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 11] [Reference Citation Analysis (0)] |
| 15. | Sy E, Albright RH, Sorensen T, Sorensen MD, Klein EE, Weil L Jr, Fleischer AE. Obesity is highly associated with a non-home discharge following total ankle arthroplasty. J Foot Ankle Surg. 2025;64:205-207. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 16. | Cunningham D, Karas V, DeOrio J, Nunley J, Easley M, Adams S. Patient Risk Factors Do Not Impact 90-Day Readmission and Emergency Department Visitation After Total Ankle Arthroplasty: Implications for the Comprehensive Care for Joint Replacement (CJR) Bundled Payment Plan. J Bone Joint Surg Am. 2018;100:1289-1297. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 27] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 17. | Best MJ, Nguyen S, Shafiq B, Ficke JR. Risk Factors for Complications, Longer Hospital Stay, and Readmission After Total Ankle Arthroplasty. Foot Ankle Spec. 2022;15:142-149. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 13] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 18. | Kwon NF, Danilkowicz RM, Kim J, Grimm NL, Adams SB. Short-Term Complications Following Total Ankle Arthroplasty and Associated Risk Factors: A NSQIP Database Analysis. Foot Ankle Spec. 2023;16:214-220. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 14] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 19. | Barg A, Knupp M, Anderson AE, Hintermann B. Total ankle replacement in obese patients: component stability, weight change, and functional outcome in 118 consecutive patients. Foot Ankle Int. 2011;32:925-932. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 76] [Cited by in RCA: 59] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 20. | Gross CE, Lampley A, Green CL, DeOrio JK, Easley M, Adams S, Nunley JA 2nd. The Effect of Obesity on Functional Outcomes and Complications in Total Ankle Arthroplasty. Foot Ankle Int. 2016;37:137-141. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 39] [Cited by in RCA: 57] [Article Influence: 5.7] [Reference Citation Analysis (1)] |
| 21. | Bouchard M, Amin A, Pinsker E, Khan R, Deda E, Daniels TR. The impact of obesity on the outcome of total ankle replacement. J Bone Joint Surg Am. 2015;97:904-910. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 32] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 22. | Filardi V. Tibio talar contact stress: An experimental and numerical study. J Orthop. 2020;17:44-48. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 10] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 23. | Noori NB, Ouyang JY, Noori M, Altabey WA. A Review Study on Total Ankle Replacement. Appl Sci. 2022;13:535. [DOI] [Full Text] |
| 24. | Pierpont YN, Dinh TP, Salas RE, Johnson EL, Wright TG, Robson MC, Payne WG. Obesity and surgical wound healing: a current review. ISRN Obes. 2014;2014:638936. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 60] [Cited by in RCA: 187] [Article Influence: 15.6] [Reference Citation Analysis (1)] |
| 25. | Rahman A, Abid Hasan HM, Ali R, Ullah H, Ahmad S, Saqib M. Impact of Obesity on Joint Replacement Surgery Outcomes: A Comparative Study. Cureus. 2025;17:e80623. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 26. | Orr SV, Pereira GC, Christiansen BA. Justification of Body Mass Index cutoffs for hip and knee joint arthroplasty among California orthopedic surgeons. J Orthop Surg Res. 2025;20:125. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 27. | Ricciardi BF, Giori NJ, Fehring TK. Clinical Faceoff: Should Orthopaedic Surgeons Have Strict BMI Cutoffs for Performing Primary TKA and THA? Clin Orthop Relat Res. 2019;477:2629-2634. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 38] [Article Influence: 5.4] [Reference Citation Analysis (0)] |