Published online Mar 18, 2026. doi: 10.5312/wjo.v17.i3.114005
Revised: October 3, 2025
Accepted: December 23, 2025
Published online: March 18, 2026
Processing time: 188 Days and 13.3 Hours
Despite satisfactory results, controversy remains on whether meniscal allograft transplantation (MAT) prevents or even slows the progression of cartilage dege
To evaluate patient reported outcomes at various time points in patients who underwent an isolated MAT using a bone-block technique with suture-based bony fixation.
This case series includes seventeen patients with history of meniscectomy and corresponding compartmental knee pain that were treated with isolated MAT performed by a single orthopedic sports medicine surgeon. Patients were ex
Fifteen of 17 patients treated with MAT were evaluated at a minimum of 2 years (mean 4.7 years) of follow-up. Mean patient age was 22.2 ± 10.7 (14-56) years. There were 8 females (53%) and 7 males (47%) included in the statistical analysis. 13 patients had lateral transplants (87%) and 2 had medial transplants (13%). The reoperation rate was 13%; however, no patients required revision MAT or arthroplasty and graft survival was 100%. Average patient reported pain severity score, pain frequency score, and scores from 9 validated knee surveys were significantly improved at 6 months, 1 year, and final follow up compared to pre-operative baseline (P < 0.05).
Despite some limitations, meniscus transplantation with suture-based bone bridge fixation resulted in reliable improvements in knee pain and function at a minimum of 2 years of follow-up. Our study demonstrated 100% graft survival with low complication rates (13.3%). Suture fixation of the transplanted bone block in MAT is a viable technique with excellent clinical outcomes.
Core Tip: Meniscal allograft transplantation (MAT) with suture-based bone bridge fixation provides reliable improvements in pain and knee function, with durable results at mid-term follow-up. Patients experienced significant improvements in multiple validated outcome measures, low complication rates, and 100% graft survival without need for revision MAT or arthroplasty. These findings support suture-based fixation as a safe and effective technique for isolated MAT in young, active patients with symptomatic meniscal deficiency after meniscectomy.
- Citation: Renshaw A, Desai B, Few WE, Verma A, Willard J, Godshaw B, Jones D. Isolated meniscal allograft transplantation with suture-based fixation of a bone bridge: 15 cases with a 2-year minimum follow-up. World J Orthop 2026; 17(3): 114005
- URL: https://www.wjgnet.com/2218-5836/full/v17/i3/114005.htm
- DOI: https://dx.doi.org/10.5312/wjo.v17.i3.114005
Increased knowledge of the natural history and biomechanical consequences that meniscectomy has on the knee has resulted in more importance being placed on meniscal preservation. However, not all meniscal injuries are reparable, resulting in a group of patients with absent or nonfunctional menisci.
Despite attempts to preserve the meniscus, meniscectomy is occasionally required for tears that are not amenable to repair. The lack of a functional meniscus, whether due to a prior meniscal tear or meniscectomy, can be detrimental. A 20% loss of meniscal tissue has been shown to increase joint contact forces by up to 350%[1].
With physiologic gait, 6 × body weight is transmitted through the articular surface of the knee with 70% or more through the medial tibial plateau. During weight-bearing, the C-shaped lateral meniscus carries approximately 70% of the lateral tibial-femoral compartment load. The U-shaped medial meniscus has greater separation between its anterior and posterior horns compared to the lateral meniscus, and carries approximately 40% of the medial tibial-femoral com
First described by Zukor et al[4], the utilization of MAT has increased substantially with improvements in surgical technique and patient selection. Over the past several decades, there has been an increase in MAT data detailing surgical anatomy, indications, techniques, and outcomes[1,4]. MAT has previously been shown to yield favorable results and provide improved function and pain in the short- and mid-term term basis[5]. González-Lucena et al[2] found that MAT can provide significant functional improvement and pain relief in patients following meniscectomy.
Despite satisfactory results, controversy remains on whether MAT prevents or even slows the progression of cartilage degeneration in a previously meniscectomized compartment[3]. A biomechanical study by McDermott et al[6] demon
There are multiple described techniques for MAT, and these are broadly classified as either soft tissue or bone fixation, including bone-bridge and bone-plug techniques[8]. The soft tissue technique is advantageous in that graft preparation and passage is less technically challenging compared to the other techniques. However, cadaveric studies have de
The aim of this study was to evaluate patient reported outcomes at various time points in patients who underwent an isolated MAT using a bone-block technique with suture-based bony fixation. We hypothesized that isolated MAT would lead to significant improvements in patient reported outcomes with a low rate of complications.
Seventeen patients with previously meniscectomized knees and corresponding unicompartmental knee pain were prospectively studied after undergoing isolated MAT from November 2012 to May 2019 by a single surgeon. Patient reported outcomes measures were recorded pre-operatively and at 6 months, 12 months, and final follow up of at least 2 years. The study was determined to be exempt after review by the Institutional Review Board.
The ideal candidate for MAT is a young, post-meniscectomized patient with joint line pain, minimal cartilage degeneration, and anatomic alignment. Inclusion criteria were patients undergoing MAT without additional major procedures, minimum of 2 years follow up, and compliance with post-operative outcome scoring. We define major procedures as additional cartilage restoration, osteotomy (proximal tibial, tibial tubercle, or distal femoral), ligament reconstruction, and additional meniscal repair of the ipsilateral knee. Therefore, patients were excluded if they had additional pathology or factors that necessitated the need for additional surgical interventions in addition to MAT. The senior authors indications and contraindications for isolated MAT are outlined below in Table 1.
| BMI < 35 kg/m2 |
| Normal coronal and sagittal alignment of the knee |
| Normal ligamentous stability |
| No articular cartilage lesions in the compartment with corresponding pathologic meniscus |
| Patient willing and able to comply with all postoperative restrictions and rehabilitation protocols |
| Patient with realistic post-surgical expectations |
Various techniques have been employed for MAT over the past several decades. These include soft tissue, bone plug, and bone bridge techniques. The soft tissue technique utilizes allograft meniscus with suture fixation through the anterior and posterior roots and capsule[10]. This allows for a quicker and less technically demanding procedure with the disadvantage of not having bone to bone healing to secure the graft. Abat et al[11] compared a soft tissue suture-only technique to a bone plug technique and found more extrusion of the meniscus and higher re-tear rates in the suture-only group. Additionally, biomechanical studies have shown that bone plug fixation results in superior restoration of tibiofemoral contact pressures when compared to soft tissue fixation[12].
Bone plug techniques allow for bone-to-bone healing and independent placement of the anterior and posterior horns. The advantage of this graft is bone to bone healing at the horns, which may better resist hoop stresses, improve biomechanics, and yield less extrusion as compared to soft tissue fixation[11,12]. There are several disadvantages to this technique. The posterior horn bone plug can be difficult to maneuver into position and there may be limited bone stock at this area. As such, placement of the posterior horn graft may be non-anatomic or lack secure fixation thus hindering the clinical and functional result.
The bone bridge technique, as used by the senior surgeon, can be implemented in medial or lateral meniscal deficiency. It allows for bone-to-bone healing and preserves the anatomic attachment sites of the meniscal horns. In the opinion of the senior author, this helps prevent meniscal extrusion. In contrast to bone plug techniques, use of a bone bridge maintains the native anterior and posterior horns and reduces the potential for non-anatomic placement of bone plugs. Chen et al[13] showed that anatomic fixation of the meniscal horns prevents extrusion, provides a larger contact area for healing, and decreases peak contact pressure in the affected compartment. Other similar techniques have been described and referred to as “bone trough” techniques[14]. Although similar, there are slight differences in fixation methods and graft preparation between bone trough and our described bone bridge technique. Regardless, bone trough-type techniques have also been associated with excellent outcomes[9].
After obtaining a history and physical examination, high quality X-rays are obtained. AP standing, PA 45 degree standing, lateral, and long-leg alignment films are essential. AP and lateral X-rays with calibrated sizing markers are utilized to ensure that the correct size graft is prepared by the tissue bank. Shaffer et al[15] compared magnetic resonance imaging (MRI) to X-ray with regards to graft sizing accuracy and found that MRI is 83% accurate and X-ray is 79% accurate. The senior surgeon thus prefers to use X-ray for graft sizing as this is cheaper and easier to obtain, without sacrificing overall accuracy. Dienst et al[16] showed that size mismatches > 10% lead to unacceptable alterations in stress placed on the articular cartilage and graft, thus reenforcing the notion that these measurements must be accurate. Pollard et al[17] developed an accurate method for measuring size-matched grafts on X-ray. They showed that the medial meniscal length is 0.8 times the medial tibial plateau length and the lateral meniscal length is 0.7 times the lateral plateau length when measured on a lateral X-ray.
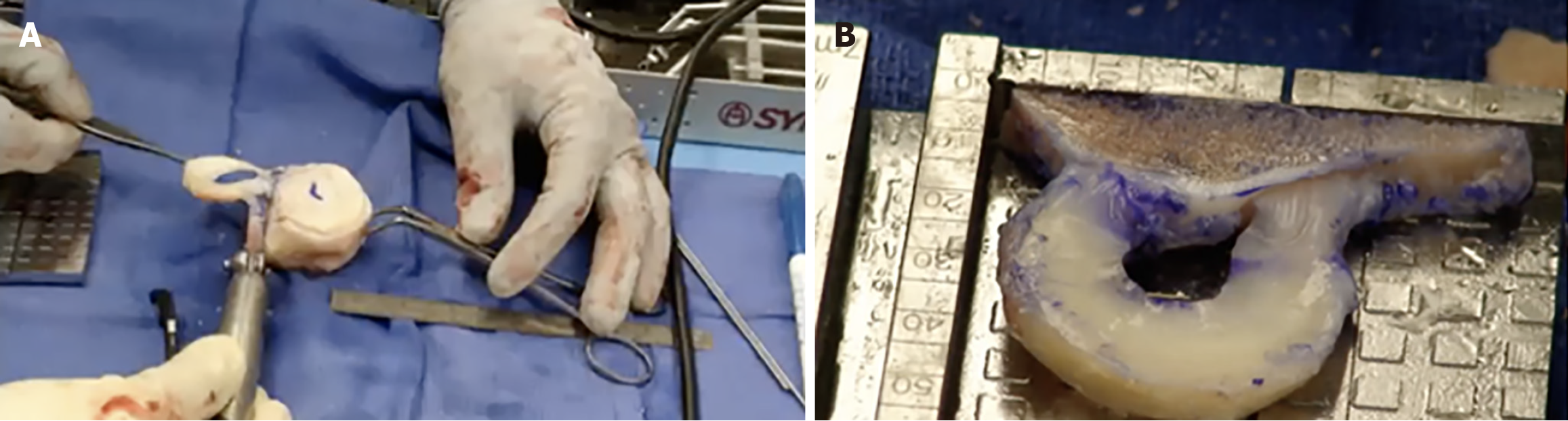
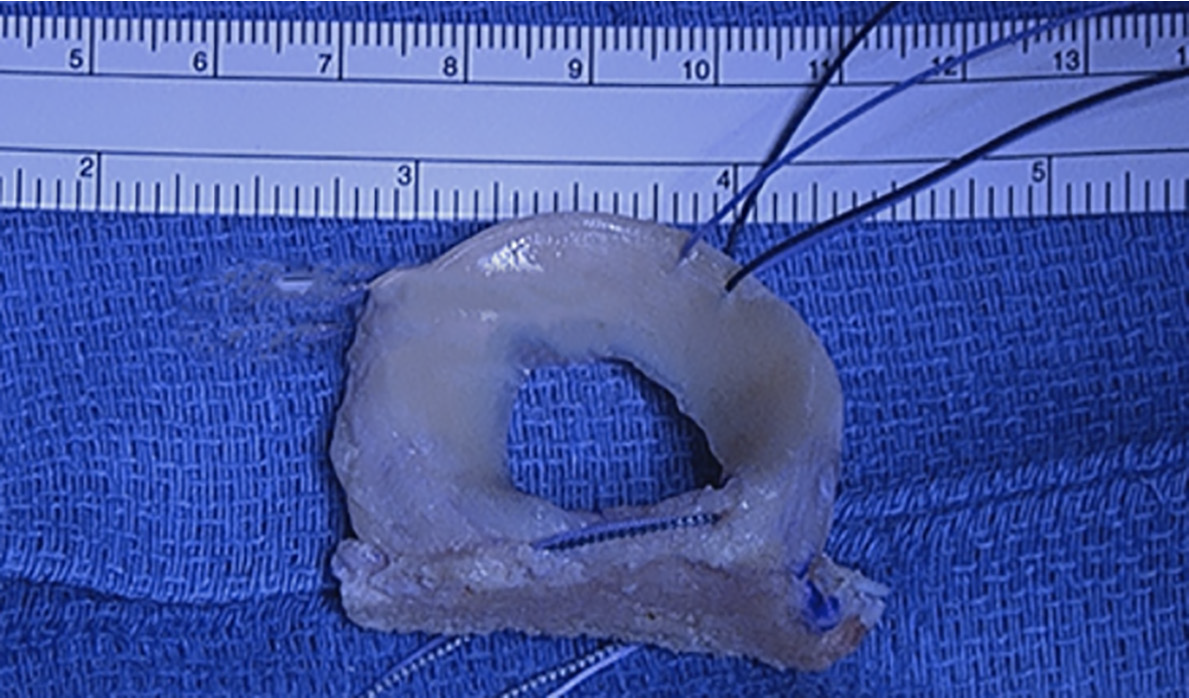
Following completion of pre-operative planning, the graft is prepared and delivered by the tissue bank. Meniscal allografts are aseptically processed fresh frozen allografts. Fresh frozen bulk proximal tibial grafts are selected as they have been shown to have lower failure rates compared to freeze-dried terminally irradiated grafts[18]. All capsular and ligamentous tissue is removed prior to shipment. The graft is prepped intraoperatively using a bone block sizing/cutting guide. The bone block attached to the meniscal roots should be 7-8 mm wide, approximately 45 mm in length, and 1 cm deep (Figure 1). The width of the bone block may vary based on the width of the anterior and posterior horns. Two vertical holes are then drilled anteriorly and posteriorly in the bone block using a 1.5 mm drill bit. These allow for passage of two #2 nonabsorbable sutures, which are used to fixate the bone block after insertion. These sutures are passed retrograde through the anterior hole, over the superior portion of the graft bone block, and antegrade through the posterior hole. A peripheral traction suture is placed in the meniscal body at the junction of the posterior 1/3 and anterior 2/3 of the graft (Figure 2). This suture is later used to reduce the soft tissue component of the graft into anatomic position.
This technique can be done arthroscopically if no additional procedures are required. Standard anterolateral and anteromedial portals are created and a diagnostic arthroscopy is performed.
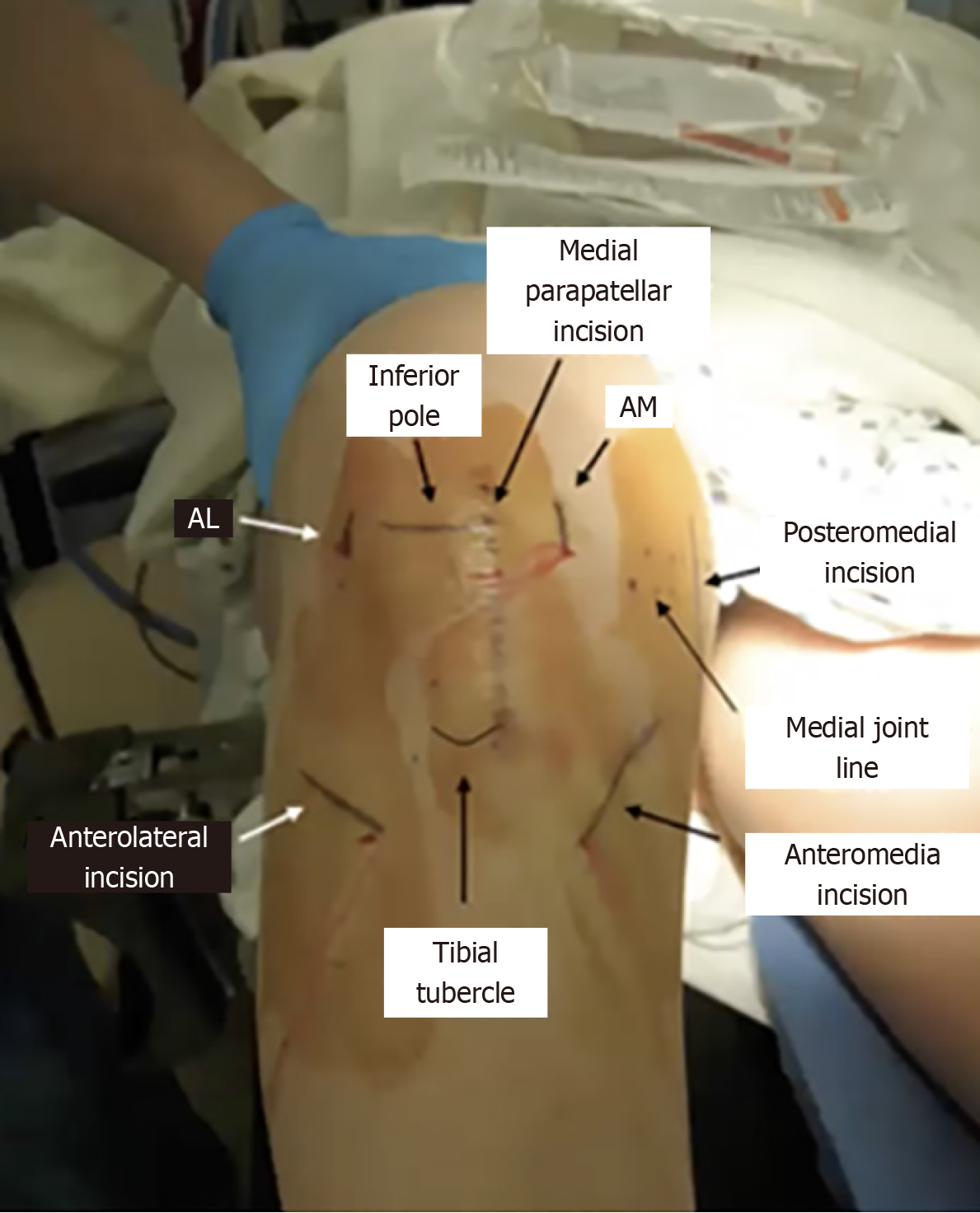
After the diagnostic arthroscopy, the affected meniscus is meticulously debrided. A small, 1-2 mm, rim of remnant meniscal tissue is left to allow for vascular ingrowth of the allograft. Additional posteromedial or posterolateral portals, depending on the laterality of the transplant, are utilized to aid in the total meniscectomy and graft passage. These portals are made in line with an approach for later inside out meniscal repair. Oblique or vertical anterolateral or anteromedial incisions are also used to drill tunnels for fixation of the bony portion of the graft. Additionally, a transpatellar tendon portal/mini arthrotomy is often used to allow for bone trough creation and graft insertion. This portal must be in line with the anterior and posterior horns of the native meniscus, and localization with the spinal needle is critical. The anterior and posterior horns should be preserved prior to this portal’s creation. Figure 3 shows examples of the incisions used to facilitate efficient performance of this surgical technique.
Once preparation of the meniscal graft is complete, a trough for placement of the bone block is created with a reciprocating saw. Cutting guides are commercially available for this portion; however, due to the senior author’s experience, he elects to cut the troughs free hand. The trough size is generally 7-8 mm in width and 1 cm in depth. Figure 4 show creation of the bone troughs as described. A rasp is used to assess the accuracy of the trough size. An ACL drill guide and guide pin are used to drill tunnels in the base of the bone trough. Two tunnels are created - one anterior and one posterior. These tunnels are drilled through the previously mentioned anteromedial or anterolateral incisions. Figure 5 illustrates placement of these drill tunnels.
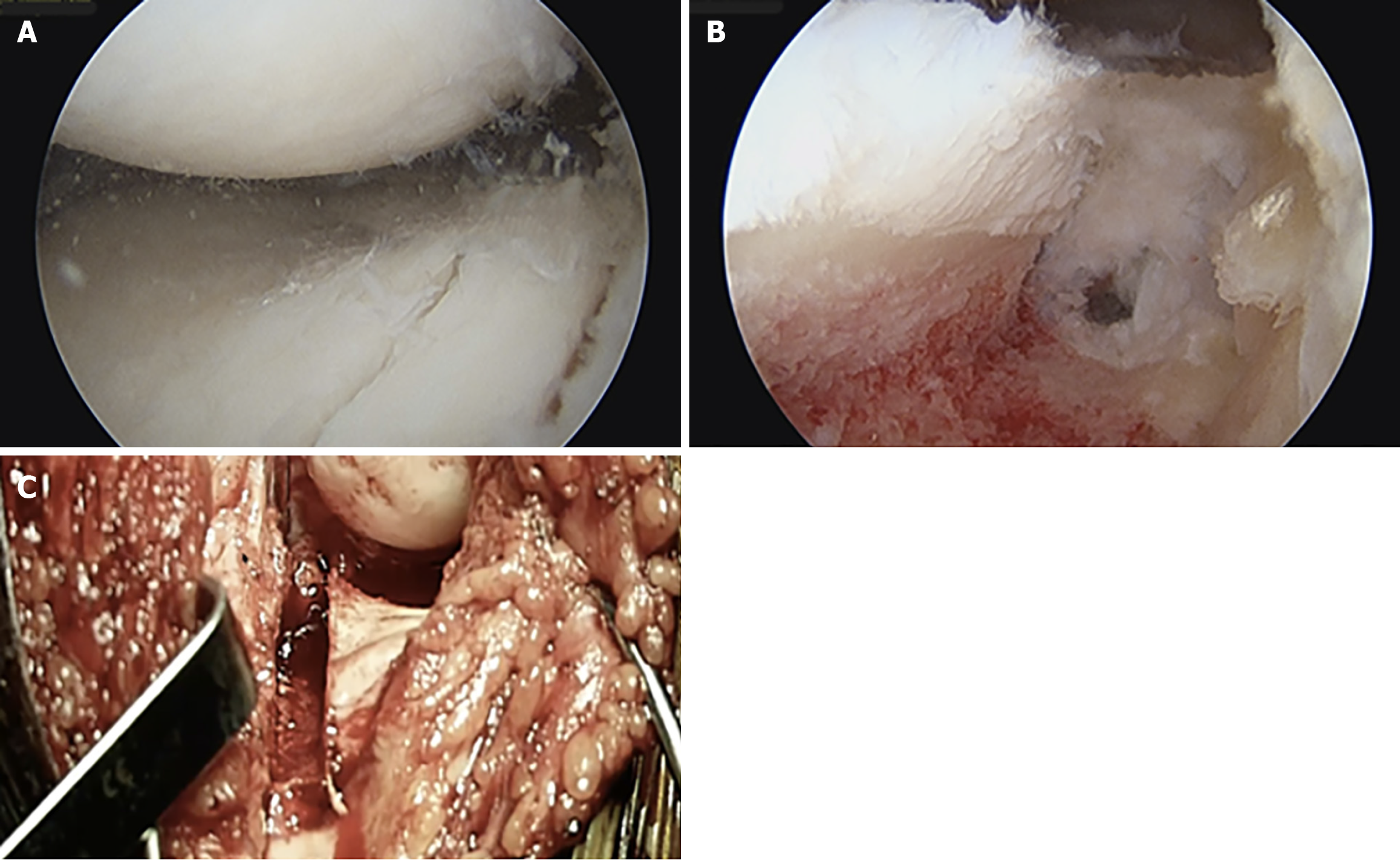
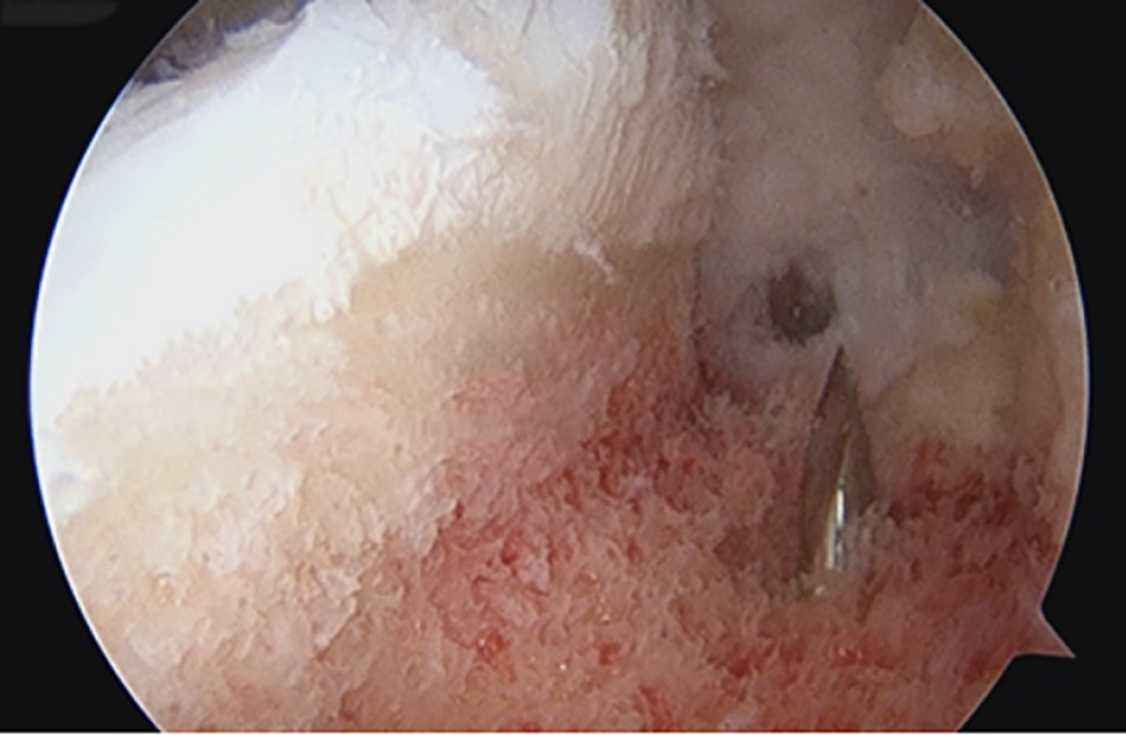
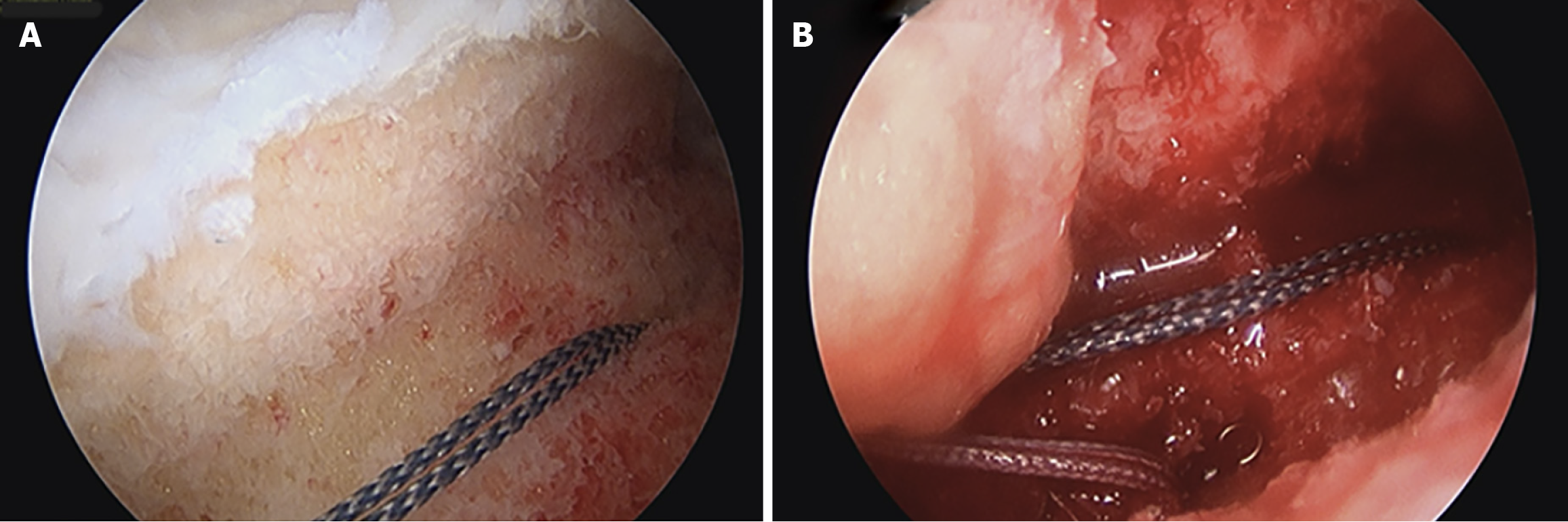
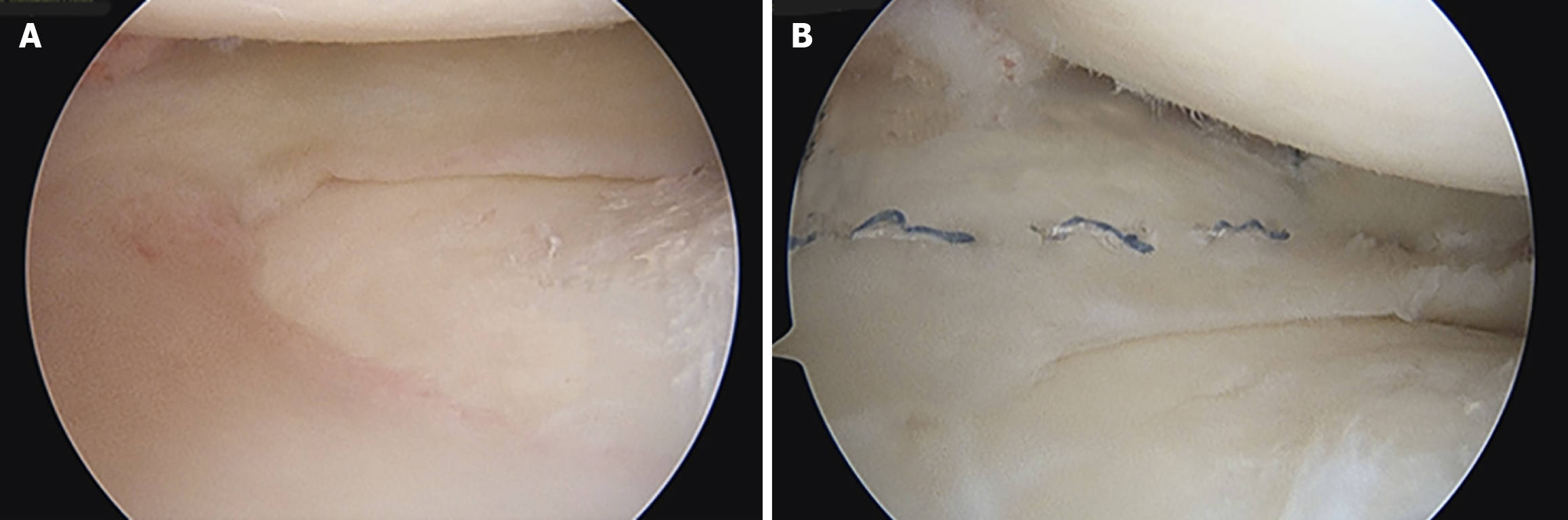
A Hewson suture passer with a doubled over passing suture is then passed through the drill tunnels. The passing sutures are retrieved through the trans patellar tendon incision/mini arthrotomy for later use (Figure 6). One additional passing suture is then passed in an outside-in fashion through the capsule by utilizing the previously created posterolateral or posteromedial incision. Again, this suture is retrieved through the trans-patellar tendon incision. The capsular passing suture is then used to pass the traction suture from the rim of the meniscal graft through the capsule. The passing sutures in the bone trough are used to pass sutures from the bony portion of the graft. Manual pressure, manipulation, and tensioning of the sutures fixed to the graft are used to reduce the graft into position. Figure 7A demonstrates a meniscal graft that has been successfully positioned. The bony portion of the graft is secured prior to soft tissue fixation. The sutures from the bone block are securely tied over a bone bridge that was created between the 2 drill tunnels. This completes the osseous fixation of the graft and if performed correctly, provides solid and stable fixation to allow for bony ingrowth of the graft.
To complete the soft tissue fixation of the graft, all-inside meniscal fixation devices are used for the posterior horn. To fixate the mid body and anterior horn, zone specific cannula devices are used to direct suture passage. A combination of vertical and horizontal mattress sutures facilitates stable fixation of the mid body and anterior horn. Figure 7B demonstrates final soft tissue fixation of a transplanted meniscal graft. Of note, it is essential to secure the bone block before placing these peripheral sutures in the meniscus. If the bone block is not secure, the peripheral sutures will malposition the block thus leading to non-anatomic graft placement.
The incisions are closed in standard fashion. A soft dressing and a cooling unit are then applied, followed by a hinged knee brace locked in 0 degrees of extension during ambulation.
The senior surgeon’s standard post-operative rehabilitation protocol for isolated MAT is outlined below in Table 2.
| Post-operative rehabilitation protocol |
| Begin physical therapy 3-5 days after surgery |
| Touch down weight bearing to 25% partial weight bearing is allowed for 6 weeks. Full weight bearing at 6 weeks. Upon initiation of full weight bearing an unloader brace is used to off-load the surgical compartment |
| While ambulating, the knee is locked in extension with a brace for 6 weeks |
| Range of motion from 0-45 degrees until 2 weeks post-operatively |
| Range of motion from 0-60 degrees from post-operative weeks 2-4 |
| Range of motion from 0-90 degrees from post-operative weeks 4-6 |
| Advance to range of motion as tolerated after post-operative week 6, avoiding forced flexion for 3-4 months |
| Return to work for a sedentary job can be as early as one week post-operatively. For strenuous work, it will take approximately 3-4 months |
| Low-impact exercises are allowed at 8 weeks with running after 6 months. Light to moderate sport is allowed at 6 months to 9 months with strenuous sport not recommended. Each case is unique and modifying return to work and sport to a certain degree is necessary for every patient |
At each time point, outcome data was collected for several different measures. Using paired t tests, the means of all outcome scores were compared from pre-operative to post operative at all recorded time points to determine significance in relation to pre-operative values. We set our significance at P = 0.05. Differences in patient-reported outcome measures (PROMs) were also assessed for minimum clinically important differences (MCID), patient-acceptable symptomatic state (PASS), and substantial clinical benefit (SCB)[19]. All analysis and data collection were carried out using Microsoft Excel software (Microsoft Corporation, Redmond, WA, United States).
Seventeen patients underwent isolated meniscus transplant in our study cohort. 2 patients were excluded due to lack of 2-year follow up. This left 15 patients who were evaluated at a minimum 2-year (average 4.7 year) follow-up using the Pain Severity and Pain Frequency scores, Lysholm score, PSF-12, MSF-12, International Knee Documentation Committee (IKDC), Knee Injury and Osteoarthritis Outcome Score (KOOS) including KOOS sub-scores of pain, activities of daily living (ADL), quality of life (QoL), symptom, and sport.
Table 3 lists the demographic information for the 15 patients included in our analysis. Table 4 provides a summary of the information found in Table 3. The average patient age was 22.2 ± 10.7 (14-56) years old. There were 8 females (53%) and 7 males (47%) included. 13 transplants were lateral (87%) and 2 were medial (13%). There were 2 complications requiring reoperation in the study period for a reoperation rate of 13.3%. One patient developed arthrofibrosis and one patient suffered a tear of the transplanted meniscus. The 2 patients who did not complete the minimum 2-year follow up did not require re-operation during the study period. If included, this would result in a complication rate of 11.7% (2/17). No patients in our cohort required revision MAT or conversion to arthroplasty. Overall graft survival rate was 100% (15/15).
| Patient | Age (years) | Sex | Laterality | Need for follow up procedure |
| 1 | 21 | Female | Lateral | No |
| 2 | 35 | Female | Lateral | No |
| 3 | 56 | Male | Medial | No |
| 4 | 14 | Male | Lateral | No |
| 5 | 14 | Male | Lateral | No |
| 6 | 17 | Male | Lateral | No |
| 7 | 17 | Female | Lateral | No |
| 8 | 23 | Female | Lateral | No |
| 9 | 19 | Male | Lateral | No |
| 10 | 25 | Female | Lateral | Yes (meniscal re-tear) |
| 11 | 19 | Female | Medial | Yes (arthrofibrosis) |
| 12 | 20 | Female | Lateral | No |
| 13 | 17 | Male | Lateral | No |
| 14 | 19 | Male | Lateral | No |
| 15 | 17 | Female | Lateral | No |
| Patients (n) | 15 |
| Average age (years) | 22.2 ± 10.7 (14-56) |
| Sex | Female 53% (8/15), male 47% (7/15) |
| Laterality | Lateral 87% (13/15), medial 13% (2/15) |
| Revision rate | 13% (2/15) |
| Avg follow up | 57 months (24-111) |
Table 5 lists the results for outcome measures pre-operatively and at 6 months, 1 year, and final follow up (minimum 2 years post-operatively). All measures listed in bold were found to be statistically significant with P values ≤ 0.05. Overall, patients demonstrated statistically significant improvement from pre-operative baseline at 6 months, 1 year, and final follow-up for all eleven domains evaluated (Table 5). These improvements were maintained at the most recent follow-up.
| Preop (n = 15) | 6 months (n = 15) | P value | 1 year (n = 15) | P value | 2+ years (average = 4.7 years) (n = 15) | P value | |
| Pain frequency | 6.9 ± 2.5 | 3.2 ± 2.5 | P < 0.001 | 3.1 ± 2.2 | P < 0.001 | 3.4 ± 3.6 | P = 0.001 |
| Pain severity | 6.2 ± 2.6 | 3.4 ± 2.5 | P = 0.002 | 3.3 ± 2.9 | P < 0.001 | 2.9 ± 2.5 | P < 0.001 |
| IKDC function | 37.1 ± 15.7 | 59.4 ± 17.2 | P = 0.001 | 70.1 ± 22.1 | P < 0.001 | 74.2 ± 17.7 | P < 0.001 |
| Lysholm | 52.2 ± 20.6 | 72.5 ± 17.9 | P = 0.001 | 80.1 ± 15.4 | P < 0.001 | 83.1 ± 17.7 | P < 0.001 |
| KOOS pain score | 53.9 ± 14.2 | 80.4 ± 15.3 | P < 0.001 | 84.4 ± 15.6 | P < 0.001 | 86.1 ± 15.0 | P < 0.001 |
| KOOS symptom | 45.7 ± 16.5 | 68.6 ± 16.8 | P = 0.004 | 82.6 ± 17.8 | P < 0.001 | 82.4 ± 16.3 | P < 0.001 |
| KOOS ADL | 65.5 ± 18.9 | 88.4 ± 13.3 | P < 0.001 | 90.7 ± 13.6 | P < 0.001 | 89.4 ± 12.2 | P < 0.001 |
| KOOS sport | 26.3 ± 25.5 | 52.1 ± 28.0 | P = 0.021 | 66.0 ± 30.0 | P < 0.001 | 69.7 ± 27.7 | P < 0.001 |
| KOOS QoL | 30.8 ± 23.9 | 53.3 ± 18.4 | P = 0.014 | 62.1 ± 30.7 | P = 0.002 | 66.0 ± 29.0 | P = 0.001 |
| PSF12 score | 36.9 ± 9.1 | 43.5 ± 9.4 | P = 0.036 | 48.2 ± 9.2 | P = 0.003 | 49.5 ± 7.7 | P < 0.001 |
| MSF12 score | 45.7 ± 12.1 | 54.5 ± 10.3 | P = 0.008 | 55.7 ± 9.3 | P = 0.001 | 56.3 ± 7.7 | P = 0.002 |
This study demonstrates that MAT performed in the post-meniscectomized patient with persistent compartmental knee pain improves patient reported outcomes and pain scores at a minimum of 2 years, and average of 4.75 years (range 24-111 months), post-operatively. These improvements were maintained through each patient’s most recent follow-up.
Wagner et al[19] determined MCID, PASS, and SCB thresholds for patients undergoing primary MAT who were assessed with Lysholm, IKDC, and KOOS subscales. Notably, the statistically significant improvements in PROMs observed in their study were also found to be clinically significant at all time points. Improvements in Lysholm (Δ = 30.9, MCID 10.3), IKDC (Δ = 37.1, MCID 12.1), KOOS pain (Δ = 32.2, MCID 11.0), KOOS symptoms (Δ = 36.7, MCID 11.0), KOOS ADL (Δ = 23.9, MCID 10.5), KOOS sport (Δ = 43.4, MCID 16.2), and KOOS QoL (Δ = 35.2, MCID 13.6) exceeded MCID threshold. The PASS threshold was achieved for each of these domains except KOOS ADL. Additionally, SCB was achieved for IKDC (Δ = 37.1, SCB 29.1), KOOS pain (Δ = 32.2, SCB 25.1), KOOS symptoms (Δ = 36.7, SCB 19.6), KOOS ADL (Δ = 23.9, SCB 17.9), and KOOS sport (Δ = 43.4, SCB 37.5) at the time of last follow-up.
MAT has been shown to be a viable surgical option, not only in its effectiveness but also in its safety, for patients with a meniscus-deficient knee[20]. All soft tissue graft fixation is a viable technique and is generally considered less technically challenging to perform than bony fixation. Parkinson et al[20] showed that soft tissue graft fixation can result in midterm revision-free survival of up to 82%. In their study, high grade cartilage lesions present at the time of MAT were associated with higher failure rates. Abat et al[11] showed a higher rate of meniscal extrusion and graft tears in all-suture fixated grafts. Numerous studies have demonstrated clinical and biomechanical benefits to bony graft fixation[1,8,9]. Proposed advantages of bony fixation include the ability to maintain both the anterior and posterior meniscal roots on a single bone graft thus providing inherent stability and maintaining anatomic spacing[6]. However, there are reported disadvantages to bone fixation techniques. The bone plug technique often requires a larger arthrotomy as well as precise bone resection to achieve reliable press-fit of the graft[1]. Inadequate bone stock using bone plug techniques can also compromise the ability to maintain a reliable press-fit. We feel that the disadvantages of both bone plug and all soft-tissue fixation methods are mitigated by our described bone bridge technique.
Although the overall outcomes following MAT are promising, there have been poor outcomes reported in those with concomitant pathology, including full-thickness cartilage lesions, as well as patients undergoing medial MAT[20]. These concomitant pathologies have been shown to lead to higher rates of revision surgery from rapid failure of the MAT[21]. Conversely, this does not preclude the treating surgeon from performing associated procedures as the knee pathology dictates. A meta-analysis by Hergan et al[22] demonstrated satisfactory patient outcomes after MAT. They found no difference in outcomes in patients undergoing medial vs lateral MAT and no statistically significant differences between patients undergoing isolated MAT as compared to those undergoing MAT with associated procedures. Our present study did not explore outcomes in patients undergoing concomitant procedures. However, these studies highlight the importance of adhering to strict surgical indications while simultaneously correcting concomitant pathology (cartilage procedures, osteotomies, or ligament reconstruction) to optimize outcomes and longevity of the graft[23].
One of the largest studies of MAT outcomes reported an overall survival rate of MAT’s as 95% at 5 years[1]. Within the study period, nearly one third of the patient population underwent secondary surgery, with most reoperations being arthroscopic debridement. This study also demonstrated that reoperation within 2 years of the index procedure was associated with an odds ratio of 8.4 for future arthroplasty or revision MAT, while most patients undergoing secondary surgery still experienced excellent outcomes.
The findings presented herein support the conclusions of numerous preceding studies, demonstrating that when performed in a suitable patient population, isolated MAT (specifically with utilization of a bone bridge fixation) provides durable and sustained improvements in clinical outcomes. Additionally, with our technique, high graft survival and low complication rates can be achieved. Future studies with long-term follow-up and survivorship studies are needed to promote this procedure as a viable option in this difficult to treat patient population.
Our study is not without limitations. Given the rarity of isolated MAT, our patient cohort is small. Because the study was limited to isolated MAT, we were unable to determine how other pathologies present at the time of surgery may impact outcomes. However, we feel that only including isolated MAT’s can better elucidate the true treatment effect while minimizing confounding variables.
Meniscus transplantation performed with suture-based bone bridge fixation resulted in reliable improvements in knee pain and function at a minimum of 2 years of follow-up. Our study demonstrated 100% graft survival with low complication rates. Suture fixation of the transplanted bone block in MAT is a viable technique with excellent clinical outcomes.
| 1. | Frank RM, Cole BJ. Meniscus transplantation. Curr Rev Musculoskelet Med. 2015;8:443-450. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 40] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 2. | González-Lucena G, Gelber PE, Pelfort X, Tey M, Monllau JC. Meniscal allograft transplantation without bone blocks: a 5- to 8-year follow-up of 33 patients. Arthroscopy. 2010;26:1633-1640. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 68] [Cited by in RCA: 68] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 3. | Cummins JF, Mansour JN, Howe Z, Allan DG. Meniscal transplantation and degenerative articular change: an experimental study in the rabbit. Arthroscopy. 1997;13:485-491. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 65] [Cited by in RCA: 54] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 4. | Zukor DJ, Cameron JC, Brooks PJ. The fate of human meniscal allografts. In: Ewing JW, editor. Articular Cartilage and Knee Joint Function: Basic Science and Arthroscopy. New York: Raven Press, 1990: 147-152. |
| 5. | Wirth CJ, Peters G, Milachowski KA, Weismeier KG, Kohn D. Long-term results of meniscal allograft transplantation. Am J Sports Med. 2002;30:174-181. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 237] [Cited by in RCA: 194] [Article Influence: 8.1] [Reference Citation Analysis (0)] |
| 6. | McDermott ID, Lie DT, Edwards A, Bull AM, Amis AA. The effects of lateral meniscal allograft transplantation techniques on tibio-femoral contact pressures. Knee Surg Sports Traumatol Arthrosc. 2008;16:553-560. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 100] [Cited by in RCA: 82] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 7. | LaPrade RF, Wills NJ, Spiridonov SI, Perkinson S. A prospective outcomes study of meniscal allograft transplantation. Am J Sports Med. 2010;38:1804-1812. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 69] [Cited by in RCA: 68] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 8. | Kim JM, Bin SI, Lee BS, Kim NK, Song JH, Choi JW, Lee CR. Long-term Survival Analysis of Meniscus Allograft Transplantation With Bone Fixation. Arthroscopy. 2017;33:387-393. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 50] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 9. | Alhalki MM, Howell SM, Hull ML. How three methods for fixing a medial meniscal autograft affect tibial contact mechanics. Am J Sports Med. 1999;27:320-328. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 177] [Cited by in RCA: 149] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 10. | Kim SH, Lipinski L, Pujol N. Meniscal Allograft Transplantation With Soft-Tissue Fixation Including the Anterior Intermeniscal Ligament. Arthrosc Tech. 2020;9:e137-e142. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 9] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 11. | Abat F, Gelber PE, Erquicia JI, Pelfort X, Gonzalez-Lucena G, Monllau JC. Suture-only fixation technique leads to a higher degree of extrusion than bony fixation in meniscal allograft transplantation. Am J Sports Med. 2012;40:1591-1596. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 93] [Cited by in RCA: 100] [Article Influence: 7.1] [Reference Citation Analysis (0)] |
| 12. | Ambra LF, Mestriner AB, Ackermann J, Phan AT, Farr J, Gomoll AH. Bone-Plug Versus Soft Tissue Fixation of Medial Meniscal Allograft Transplants: A Biomechanical Study. Am J Sports Med. 2019;47:2960-2965. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 32] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 13. | Chen MI, Branch TP, Hutton WC. Is it important to secure the horns during lateral meniscal transplantation? A cadaveric study. Arthroscopy. 1996;12:174-181. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 191] [Cited by in RCA: 169] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 14. | Chahla J, Olivetto J, Dean CS, Serra Cruz R, LaPrade RF. Lateral Meniscal Allograft Transplantation: The Bone Trough Technique. Arthrosc Tech. 2016;5:e371-e377. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 16] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 15. | Shaffer B, Kennedy S, Klimkiewicz J, Yao L. Preoperative sizing of meniscal allografts in meniscus transplantation. Am J Sports Med. 2000;28:524-533. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 144] [Cited by in RCA: 113] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 16. | Dienst M, Greis PE, Ellis BJ, Bachus KN, Burks RT. Effect of lateral meniscal allograft sizing on contact mechanics of the lateral tibial plateau: an experimental study in human cadaveric knee joints. Am J Sports Med. 2007;35:34-42. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 139] [Cited by in RCA: 124] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 17. | Pollard ME, Kang Q, Berg EE. Radiographic sizing for meniscal transplantation. Arthroscopy. 1995;11:684-687. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 284] [Cited by in RCA: 252] [Article Influence: 8.1] [Reference Citation Analysis (0)] |
| 18. | Bates MD, Springer BD. Extensor mechanism disruption after total knee arthroplasty. J Am Acad Orthop Surg. 2015;23:95-106. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 39] [Cited by in RCA: 62] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 19. | Wagner KR, Kaiser JT, Knapik DM, Condron NB, Gilat R, Meeker ZD, Sivasundaram L, Yanke AB, Cole BJ. Patient-Specific Variables Associated with Failure to Achieve Clinically Significant Outcomes After Meniscal Allograft Transplantation at Minimum 5 Year Follow-Up. Arthroscopy. 2023;39:2327-2338. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 18] [Article Influence: 6.0] [Reference Citation Analysis (0)] |
| 20. | Parkinson B, Smith N, Asplin L, Thompson P, Spalding T. Factors Predicting Meniscal Allograft Transplantation Failure. Orthop J Sports Med. 2016;4:2325967116663185. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 27] [Cited by in RCA: 42] [Article Influence: 4.2] [Reference Citation Analysis (0)] |
| 21. | Shelbourne KD, Gray T. Results of anterior cruciate ligament reconstruction based on meniscus and articular cartilage status at the time of surgery. Five- to fifteen-year evaluations. Am J Sports Med. 2000;28:446-452. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 303] [Cited by in RCA: 276] [Article Influence: 10.6] [Reference Citation Analysis (0)] |
| 22. | Hergan D, Thut D, Sherman O, Day MS. Meniscal allograft transplantation. Arthroscopy. 2011;27:101-112. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 76] [Cited by in RCA: 67] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 23. | Wang H, Gee AO, Hutchinson ID, Stoner K, Warren RF, Chen TO, Maher SA. Bone Plug Versus Suture-Only Fixation of Meniscal Grafts: Effect on Joint Contact Mechanics During Simulated Gait. Am J Sports Med. 2014;42:1682-1689. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 43] [Article Influence: 3.6] [Reference Citation Analysis (0)] |