Published online Sep 18, 2024. doi: 10.5312/wjo.v15.i9.870
Revised: August 22, 2024
Accepted: August 28, 2024
Published online: September 18, 2024
Processing time: 178 Days and 1 Hours
Chronic inflammatory pain is associated with increased expression of interleukin (IL)-1, an inflammatory cytokine, and activity on its receptor (IL-1R). In response, the body produces IL-1R antagonist (IL-1Ra) to reduce this signaling. Autologous conditioned serum (ACS) is the only biologic therapy for spinal pathologies that enhances the action of endogenous IL-1Ra reserves to improve symptoms. This systematic review investigates the effectiveness of ACS in treating pain and dis
To evaluate the use of ACS as a conservative management option for spinal path
A systematic review of PubMed/Medline was performed to identify studies inve
Six articles were included, comprising 684 patients treated with epidural (n = 133) or transforaminal (n = 551) ACS injections. Patients had an average age of 54.0 years with slight female predominance (53.2%). The lumbar spine was most com
ACS injection is a safe and effective intervention for pain reduction in many spinal pathologies, including cervical and lumbar radiculopathies.
Core Tip: Injections of autologous conditioned serum (ACS) are an emerging conservative management strategy for reducing inflammation and pain in various osteoarthritic conditions. This therapy extracts and amplifies the novel anti-inflammatory molecule, interleukin-1 receptor antagonist, in a patient's serum for autologous treatment of inflammation. This study systematically reviews the literature for articles investigating the effectiveness of ACS in improving pain, disability, and quality of life in patients with spinal pathology.
- Citation: Rajkovic CJ, Merckling ML, Lee AW, Subah G, Malhotra A, Thomas ZD, Zeller SL, Wainwright JV, Kinon MD. Conservative management of spinal pathology with autologous conditioned serum: A systematic review of the literature. World J Orthop 2024; 15(9): 870-881
- URL: https://www.wjgnet.com/2218-5836/full/v15/i9/870.htm
- DOI: https://dx.doi.org/10.5312/wjo.v15.i9.870
Interleukin (IL)-1 is a known potentiator of osteoarthritis through biochemical enhancement of acute and chronic inflammation, thus precipitating tissue necrosis and the development of pain. Through stimulation of the IL-1 receptor (IL-1R), IL-1 induces pathological catabolic activity via the upregulation of cytokines, such as IL-6 and tumor necrosis factor α (TNF-α), and proteolytic enzymes, such as matrix metalloproteinases and ADAMTS-4[1]. IL-1 has also been reported to upregulate nociceptive pathways that induce hyperalgesia and neuropathic pain[2]. In pathologies of the spine, such as chronic radiculopathy, disc degeneration, and spinal stenosis, chronic inflammatory pain is associated with enhanced expression of IL-1 and activity of IL-1 on IL-1R[3-5]. To maintain balance between inflammatory stimuli and the subsequent host response, the body produces IL-1R antagonist (IL-1Ra), the only cytokine inhibitor naturally produced by the body, to reduce signaling at IL-1R[6,7]. Upregulation of IL-1Ra has been shown to inhibit necrosis of cartilage, muscle, and nervous tissue of the spine. At concentrations between ten and one thousand times in excess of normal serum, IL-1Ra can completely block IL-1R and IL-1 signaling[8,9].
Current recombinant biologics, such as AnakinraTM, rilonacept, and canakinumab, manipulate the IL-1 signaling cas
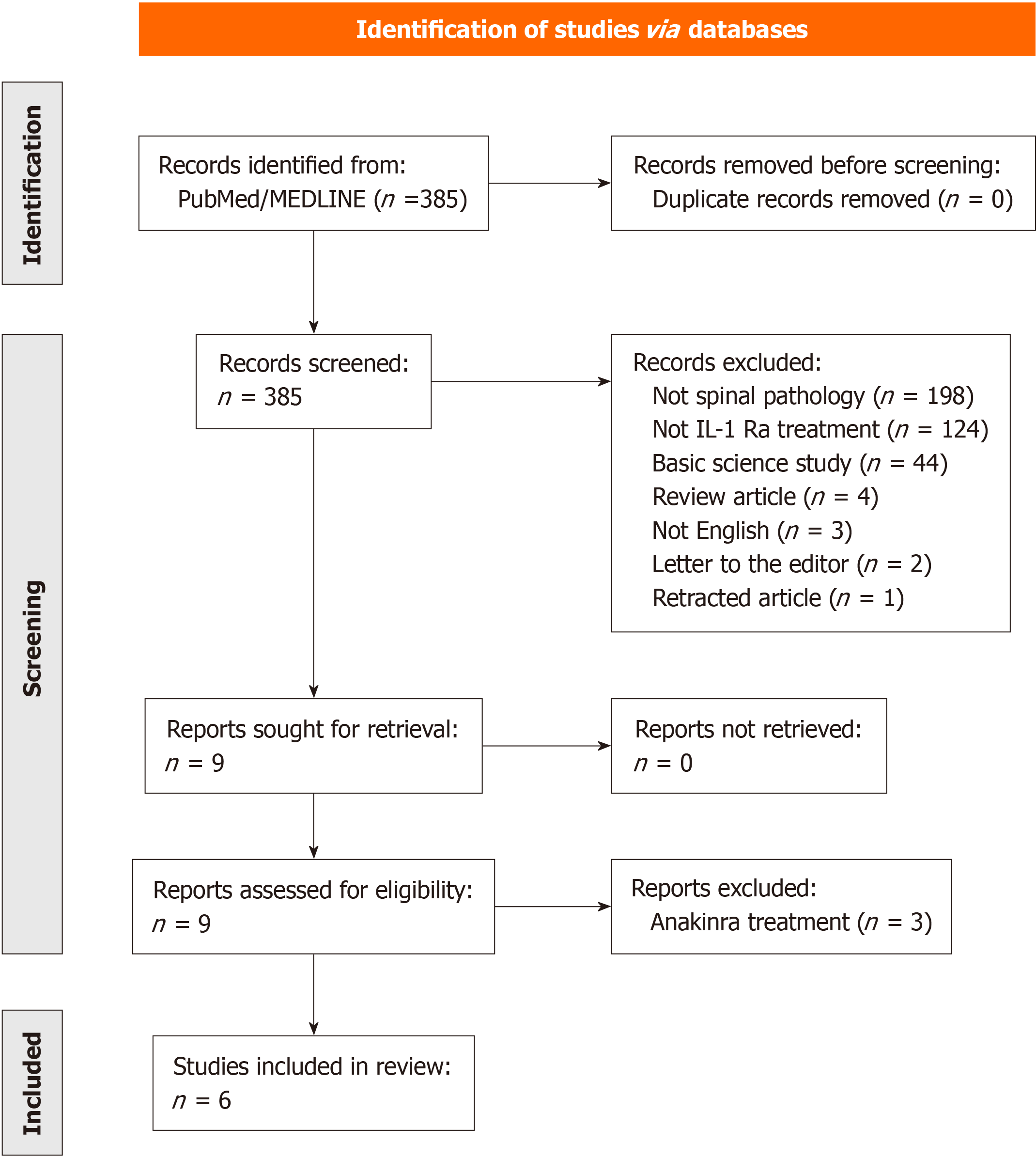
A systematic review of the literature was performed in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) (Figure 1). PubMed/Medline was interrogated for clinical studies investigating the administration of ACS for the treatment of any spinal pathology. This systematic review was not prospectively registered.
Articles included in this review met the following inclusion criteria: (1) Article discusses spinal pathology; (2) Article applies an intervention of ACS administration; and (3) Pain, disability, or quality of life outcome is reported. Studies were excluded if they met any of the following exclusion criteria: (1) Unavailable in English; (2) Abstracts and unpublished studies; (3) Reviews; (4) Articles describing non-spinal pathology; and (5) Articles describing non-ACS IL-1 therapies.
Using PRISMA guidelines, PubMed/Medline database was queried on November 3, 2023 using search terms inclusive for spinal pathology and anti-IL-1R therapy including: “autologous conditioned serum”, “regenokine”, “orthokine”, “IL-1 receptor antagonist”, “IL-1Ra”, and “anti IL-1”. No limits were imposed on the year of publication. Full search terms used can be found in Supplementary material 1. No limits were placed on the year of publication of queried articles, and all articles included were peer-reviewed, published, and accessed without requiring contact with corresponding authors.
Articles were queried by author Rajkovic CJ, and seven authors (Rajkovic CJ, Merckling M, Lee AW, Subah G, Malhotra A, Thomas ZD, Zeller SL) independently screened each title, abstract, and manuscript for inclusion and exclusion criteria. Duplicate articles were screened and removed from the query. Bibliographies of the included articles were also screened using our inclusion and exclusion criteria for additional relevant studies. The screening results were confirmed by two additional reviewers (Rajkovic CJ and Zeller SL).
Two authors (Rajkovic CJ and Merckling M) independently extracted and recorded all data into two separate Google spreadsheets. Source articles were used to cross-check and verify the data in each spreadsheet. The following information was extracted from each article: The spinal pathology treated, the study design, the baseline characteristics of each cohort, the dosing regimen and route of administration of the ACS treatment, and any comparable interventions for conservative management of spinal pathology. For articles where the age or sex of the ACS cohort was only reported as a pooled statistic with other cohorts, the pooled statistic was used to estimate the overall age or sex distribution of the ACS cohort. Primary outcomes investigated included patient pain, disability, and quality of life scores. Secondary outcomes investigated included reported adverse events and analgesic use. Data that was only reported graphically was extracted using webplotdigitizer (https://automeris.io/WebPlotDigitizer/) software to estimate mean and standard deviation values. All statistical comparisons for reported outcomes were extracted from individual included studies, and no meta-analysis was performed between studies. The statistical methods of this study were reviewed by Dr. Elizabeth Drugge from New York Medical College.
Two reviewers (Subah G and Zeller SL) independently assessed the risk of bias of the studies included in this systematic review using the Joanna Briggs Institute critical appraisal checklist for both cohort studies and randomized control trials (RCT)[14]. This process involved considering 11 and 13 questions about cohort studies and RCT, respectively, to assess risk of bias. Studies with a score < 50% of questions answered “yes” were considered as high risk, a score between 50% and 69% as moderate risk, and a score ≥ 70% as low risk (Table 1).
| Manuscript type | Ref. | Related questions | Total | Risk of bias | ||||||||||||
| Randomized control trial | Was true randomization used for assignment of participants to treatment groups? | Was allocation to treatment groups concealed? | Were treatment groups similar at the baseline? | Were participants blind to treatment assignment? | Were those delivering the treatment blind to treatment assignment? | Were treatment groups treated identically other than the intervention of interest? | Were outcome assessors blind to treatment assignment? | Were outcomes measured in the same way for treatment groups? | Were outcomes measured in a reliable way? | Was follow-up complete and if not, were differences between groups in terms of their follow-up adequately described and analyzed? | Were participants analyzed in the groups to which they were randomized? | Was appropriate statistical analysis used? | Was the trial design appropriate and any deviations from the standard randomized control trial design (individual randomization, parallel groups) accounted for in the conduct and analysis of the trial? | |||
| Godek et al[13] | Y | Y | Y | Y | N | Y | N | Y | Y | Y | Y | Y | Y | 85% | Low | |
| Cohort studies | Were the two groups similar and recruited from the same population? | Were the exposures measured similarly to assign people to both exposed and unexposed groups? | Was the exposure measured in a valid and reliable way? | Were confounding factors identified? | Were strategies to deal with confounding factors stated? | Were the groups/participants free of the outcome at the start of the study (or at the moment of exposure)? | Were the outcomes measured in a valid and reliable way? | Was the follow-up time reported and sufficient to be long enough for outcomes to occur? | Was follow-up complete, and if not, were the reasons for loss to follow-up described and explored? | Were strategies to address incomplete follow-up utilized? | Was appropriate statistical analysis used? | N/A | N/A | |||
| Becker et al[15] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | 100% | Low | |
| Goni et al[16] | Y | Y | Y | N | N | Y | Y | Y | Y | Y | N | N/A | N/A | 73% | Low | |
| HS et al[17] | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | Y | N/A | N/A | 100% | Low | |
| Godek et al[19] | Y | Y | Y | N | N | Y | Y | Y | Y | Y | Y | N/A | N/A | 82% | Low | |
| Godek et al[18] | Y | Y | Y | N | N | N | Y | Y | Y | Y | Y | N/A | N/A | 73% | Low | |
Our search query retrieved 385 articles from PubMed/Medline, and 376 articles were excluded on initial screening for the following reasons: Not spinal pathology (n = 198), no IL-1Ra treatment (n = 124), basic science study (n = 44), review article (n = 4), not English (n = 3), letter to the editor (n = 2), and retracted article (n = 1). Of the remaining nine articles, three investigated anakinra treatment and were excluded. Six articles were finally included from 2007 to 2023, comprising 684 distinct patients who were treated with ACS for spinal pathology and 72 patients who were treated with comparative steroid injections. The mean (SD) follow-up for these patients was 21.7 (4.8) weeks following their first ACS injection. All ACS injections were performed either interlaminarly (n = 61 patients) or transforaminally (n = 623 patients). The included articles consisted of two pilot studies, two prospective cohort studies, one retrospective cohort study, and one RCT. Each study’s design, baseline clinical characteristics of the patient cohort, and investigated outcomes are summarized in Table 2. Among patients treated with ACS in the included articles, the average age was 54.0 years (n = 684 patients, range: 17-93), the average BMI was 26.4 kg/m2 (n = 120 patients), and 53.2% of patients were female. Pre-existing comorbidities were only reported by Godek et al[13], including two patients with diabetes, four patients with peripheral vascular disease, and two patients with bone metabolism disorders in the RCT of 100 subjects. At baseline, patients were described to have moderate-severe pain of at least six weeks duration in three studies[15–17] and any chronic radicular symptoms in the remaining three studies[13,18,19]. Patients were opioid or steroid-naive for at least six months in three of the six included studies[15,17,19], and oral nonsteroidal anti-inflammatory drugs were allowed during the treatment period for four of the six included studies[15–17,19]. The lumbar spine was the most common spinal segment treated, with 567 patients (82.9%) receiving ACS injections for either lumbar radiculopathy (n = 67 patients), lumbar DDD (n = 372 patients), or lumbar stenosis (n = 128 patients). Cervical ACS injections were performed in 109 patients (15.9%) for either cervical radiculopathy (n = 20 patients) or DDD (n = 89 patients), and only eight patients received thoracic ACS injections (1.2%) in our systematic review, exclusively for thoracic DDD. Radiographic severity at presentation was only evaluated in one study with Godek et al[19] reporting an average disc herniation size of 5.3 ± 2.4 mm. Risk of bias assessment was low for all included studies.
| Ref. | Study design | Sample size | Age (mean) | BMI (mean) | Female | Pathology | Intervention (s) | Latest follow-up | Outcomes measured | Conclusion |
| Becker et al[15] | Randomized prospective cohort study | ACS: n = 32, 5 mg Triamcinolone: n = 27, 10 mg Triamcinolone: n = 25 | 53.9 (range: 29-81) | Not reported | 38.10% | Lumbar radiculopathy | 3 weekly transforaminal injections of ACS, 5 mg triamcinolone, or 10 mg triamcinolone | 20 weeks post-final injection | VAS, ODI | Epidural ACS injection for unilateral lumbar radiculopathy significantly improved patient pain and disability compared to baseline to an extent potentially superior to ESI. No statistically significant difference in symptom improvement was observed between 5 mg and 10 mg epidural injection of triamcinolone |
| Goni et al[16] | Pilot study | ACS: n = 20; MPS: n = 20 | ACS: 42.25; MPS: 46.80 | Not reported | ACS: 40%; MPS: 45% | Cervical radiculopathy | A single 2-3 mL transforaminal injection of ACS or MPS | 6 months post-injection | VAS, NDI, NPDS, PCS, MCS | Patients with cervical radiculopathy treated with epidural ACS injection experienced sustained improvement of pain, disability and quality of life. ACS produced as good or better improvement of symptoms with longer duration of relief compared to epidural methylprednisolone |
| HS et al[17] | Prospective study | ACS: n = 20 | 37.15 | 24.92 kg/m2 | Not reported | Lumbar radiculopathy | A single 2 mL transforaminal injection of ACS | 6 months post-injection | VAS, SLRT, ODI, PCS, MCS | Epidural ACS injection can modify the disease course of unilateral lumbar radiculopathy by significantly improving pain, disability, and quality of life |
| Godek et al[19] | Pilot study | ACS: n = 15 | 38.8 | Not reported | 40% | Lumbar radiculopathy | 1-2 weekly transforaminal injections of 3-4 mL ACS | 6 months post-injection | VAS, ODI, SLRT, OLST, Analgesic use | ACS is a promising option for significantly improving pain and disability in patients with single-level lumbar radiculopathy. No radicular damage or sever adverse events were reported |
| Godek et al[18] | Retrospective study | ACS: n = 497 | 57.1 ± 16.5 (range: 17-93) | Not reported | 57.70% | Cervical DDD (transforaminal injection): n = 89. Thoracic Spine DDD (transforaminal injection): n = 8. Lumbar Spine DDD (transforaminal injection): n = 271. Lumbar Spine DDD (interlaminar injection): n = 1. Lumbar Spine Stenosis (transforaminal injection): n = 118. Lumbar Spine Stenosis (interlaminar injection): n = 10 | Cervical: 4 doses of 3-4 mL transforaminal ACS injections. Thoracic: 6 doses of 3-4 mL transforaminal ACS injections. Lumbar: 4-6 doses of 4 mL ACS injected transforaminally or interlaminarly | 6 months post-final injection | Modified McNabb scale | ACS injection was well tolerated with very few and limited cases of adverse events. ACS injection produced satisfactory improvement in Modified McNabb Scale scores for patients with cervical or lumbar discopathy. Unsatisfactory results predominated in cases of lumbar spinal stenosis |
| Godek et al[13] | Randomized control trial | ACS: n = 100 | 46.29 + 13.61 | 26.67 ± 4.49 | 51% | Lumbar Radiculopathy due to DDD (interlaminar injection): n = 50. Lumbar Radiculopathy due to DDD (transforaminal injection): n = 50 | 2 weekly interlaminar or transforaminal injections of 8 mL ACS | 24 weeks post-final injection | NRS, ODI, RMQ, EQ-5D-5 L mobility, EQ-5D-5 L self-care, EQ-5D-5 L usual activities, EQ-5D-5 L pain/discomfort, EQ-5D-5 L anxiety/depression, EQ-5D-5 L-based LSS, EQ-5D-5 L VAS, EQ-5D-5 L Index | Epidural and transforaminal ACS injections both significantly improve patient outcomes compared to baseline. Treatment with transforaminal ACS injection produced statistically superior improvement in EQ-5D-5 L scores compared to epidural ACS injection |
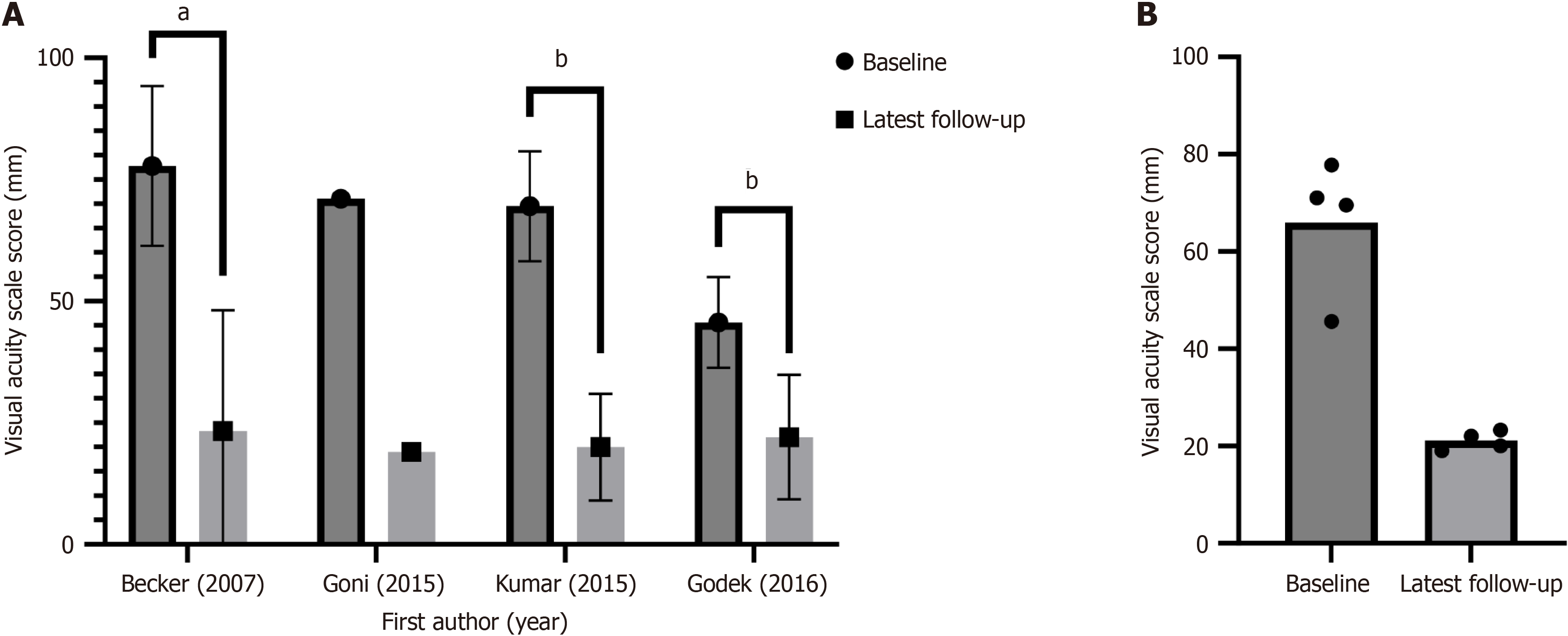
All included articles investigated pain relief following injection with ACS as a primary outcome. Specific metrics used to report pain included the visual acuity scale (VAS; four studies; Figure 2), numerical ranking scale (NRS; one study), and modified McNab scores (one study). All studies investigating ACS treatment of lumbar pathology reported significant pain reduction at final follow-up compared to baseline. Godek et al[19] reported a significant reduction in VAS score compared to baseline at both one month and three months (P = 0.002 and P < 0.0001, respectively) following transforaminal ACS injection for lumbar radiculopathy. Similarly, Becker et al[15] and HS et al[17] reported a significant reduction in baseline VAS scores at the end of 22 weeks and 24 weeks, respectively, for patients receiving transforaminal ACS injections for lumbar radiculopathy (P < 0.001 for both studies). Godek et al[13] observed a significant reduction in NRS scores at 24 weeks post-injection compared to baseline for both interlaminar and transforaminal injections in their RCT (6.1 vs 2.8, P < 0.0001 for interlaminar ACS injection; 6.1 vs 2.8, P < 0.0001 for transforaminal ACS injection). Among patients who received transforaminal ACS injections for cervical radiculopathy in a study by Goni et al[16], a 73.24% improvement (71.0 mm to 19.0 mm) in reported VAS scores was observed at six months following injection (P-value not reported).
Comparing ACS injection with ESI for treatment of lumbar pain, Becker et al[15] observed no significant difference in reported VAS scores between patients receiving ACS or 10 mg triamcinolone ESI at 22 weeks following their first injection (95%CI: -23.5, 4.9). When comparing ACS injection to a 5 mg triamcinolone ESI, the authors found that patients receiving ACS injection reported significantly lower mean (SD) VAS scores [23.3 (24.8) mm vs 36.8 (28.3) mm; P = 0.046]. Goni et al[16] reached a similar conclusion observing that patients receiving epidural ACS for cervical radiculopathy reported significantly lower VAS scores at their six-month follow-up than patients receiving methylprednisolone ESI (19.0 mm vs 27.5 mm; P = 0.027).
The modified McNab scores used by Godek et al[18] assessed both pain and disability using the following scoring system: (1) Excellent (no pain or mobility restriction and full level of activity); (2) Good (occasional pain and return to previous activity level); (3) Fair (improvement of pain with continued disability and reduced activity level); and (4) Poor (no pain improvement with continued disability and/or necessitated surgical intervention)[18]. For ease of comparison between different spinal pathologies, the authors defined a score of A or B as a satisfactory outcome. In cases of cervical and lumbar DDD, a satisfactory outcome at six-month follow-up was achieved in 61.8% and 56.5% of patients, respectively. These patients also had remarkably low rates of deterioration following initial improvement, with only 4.07% and 3.69% of patients showing a worsening of symptoms for cervical and lumbar DDD, respectively. In cases of thoracic DDD and lumbar spinal stenosis treated with transforaminal ACS injection, outcomes were less favorable with only 37.5% and 33.9% of patients achieving a satisfactory outcome. Patients with lumbar stenosis who were treated with interlaminar ACS injection fared better than those treated with transforaminal injection, achieving a 90% satisfactory outcome rate at six-month follow-up. However, this result was not statistically significant from baseline McNab scores because of a ten-patient cohort size.
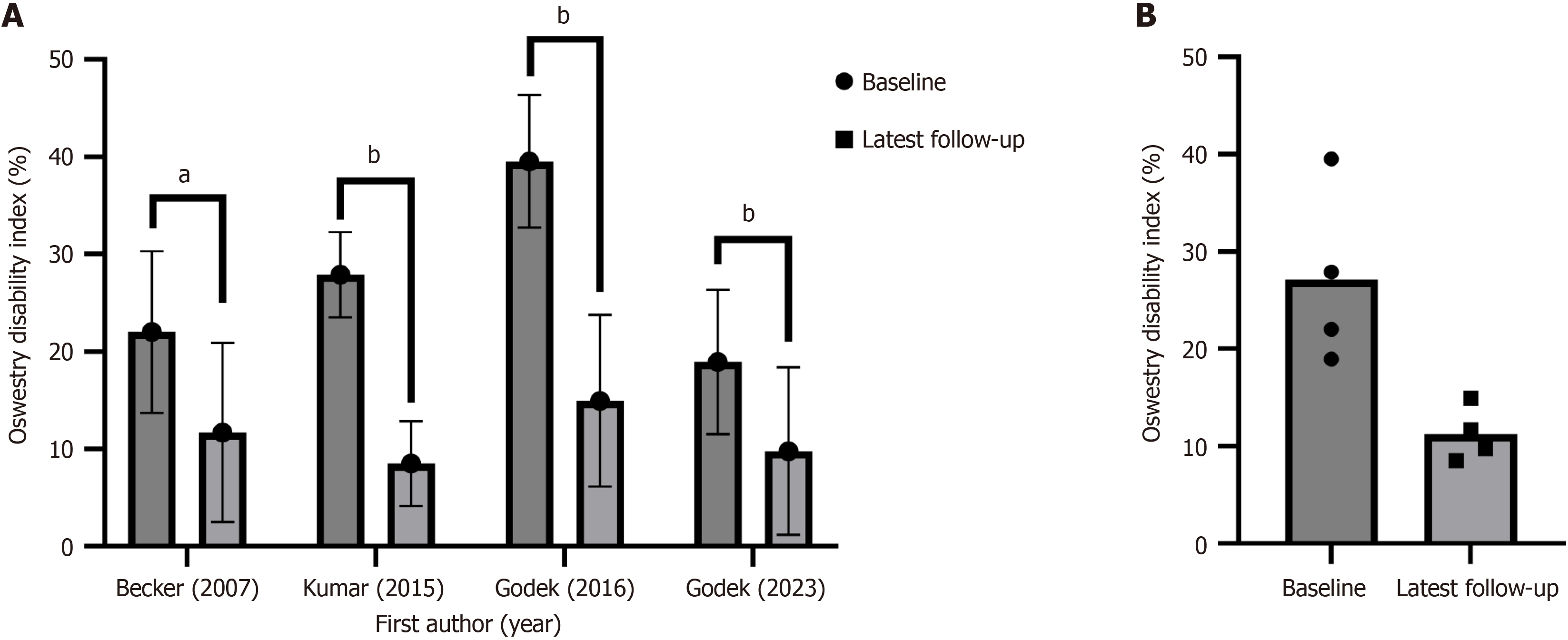
All included studies investigated disability following injection with ACS as a primary outcome. Disability metrics included the Oswestry Disability Index (ODI; four studies; Figure 3), the Roland Morris Questionnaire (one study), the neck disability index (NDI; one study), and the neck pain and disability scale (NPDS; one study). Similar to pain response following ACS injection, Godek et al[19], Godek et al[13], Becker et al[15], and HS et al[17] reported significantly improved ODI scores at 12 weeks (P = 0.005), 24 weeks (P < 0.0001), 22 weeks (P < 0.001), and 24 weeks (P < 0.001), respectively. To assess patient disability due to cervical radiculopathy, Goni et al[16] documented both NDI and NPDS scores at baseline and 24 weeks following cervical transforaminal ACS injection and demonstrated a 74.47% and 73.76% improvement in average scores, respectively (P-value not reported).
The efficacy of ACS injection compared to ESI was less conclusive regarding disability outcomes. While Goni et al[16] observed that patients receiving cervical ACS injection reported significantly lower NDI and NPDS scores (NDI 15.9 vs 30.4, P < 0.001; NPDS 18.55 vs 31.1, P < 0.001) than patients receiving methylprednisolone ESI at 24 weeks, Becker et al[15] found no significant difference between ODI scores (P = 0.95) of patients receiving epidural ACS, 5 mg triamcinolone ESI, or 10 mg triamcinolone ESI for lumbar radiculopathy at 22 weeks.
Quality of life was assessed using the Euro quality of life-five dimensions-five levels (EQ-5D-5 L) index (one study), the EQ-5D-5 L VAS (one study), the physical health component score (PCS) of the short form-36 (SF-36) questionnaire (two studies), and the mental health component score (MCS) of the SF-36 questionnaire (two studies). Comparing scores at baseline and 24 weeks post-injection, the RCT by Godek et al[13] observed a significantly improved EQ-5D-5 L index for patients receiving interlaminar (0.805 vs 0.913, P = 0.0001) and transforaminal (0.754 vs 0.895, P = 0.0001) ACS injections. Similarly, improvement from baseline to 24 weeks was also observed in EQ-5D-5 L VAS scores for interlaminar (66.14 vs 74.25, P = 0.0474) and transforaminal (60.14 vs 77.62, P < 0.0001) ACS injections. ACS injections were also shown to improve the average PCS of patients with cervical radiculopathy (27.35 at baseline to 49.08 at 24 weeks, P-value not reported) and lumbar radiculopathy (27.25 at baseline to 49.32 at 24 weeks, P < 0.001) in studies by Goni et al[16] and HS et al[17], respectively. Similarly, these two studies reported an improvement in MCS at 24 weeks for cases of cervical radiculopathy (36.22 at baseline to 47.12 at 24 weeks, P-value not reported) and lumbar radiculopathy (36.59 at baseline to 47.51 at 24 weeks, P < 0.001). Epidural ACS injections were also shown to outperform methylprednisolone ESI in improving PCS (49.08 vs 44.39, P = 0.004) and MCS (47.12 vs 42.42, P < 0.001) at 24 weeks following injection for cervical radiculopathy.
Adverse events of any kind were reported in 21 of the 684 patients (3.1%) included in this systematic review following ACS injection. No serious adverse events directly attributable to ACS injection, including infection, muscle atrophy, or hematoma, occurred in any of the patients in this review. The most severe adverse events reported were due to natural progression of disease, specifically four patients who eventually required emergency surgery due to persistent pain and foot paresis while receiving ACS therapy[18,19]. Further, three of the six studies included protocols for the treatment of persistent pain with over-the-counter analgesics taken as needed. The remaining adverse events were self-limited and resolved within 48 hours. These included headache (n = 4), dizziness (n = 4), syncope (n = 1), sweating (n = 3), tachycardia (n = 2), back stiffness (n = 1), and neck stiffness (n = 2). Godek et al[18] reported a mild complication rate of approximately 10% in its pooled cohort of osteoarthritis treatment, limited to mild myalgia, chills, weakness, and fevers resolving within 48 hours of injection[18]. In studies that compared ACS to ESI, the adverse event rates were similar between groups, with Becker et al[15] reporting one adverse event in each of its ACS and triamcinolone ESI treatment groups, and Goni et al[16] reporting 8 adverse events in its ACS treatment group and 11 adverse events in its methylprednisolone ESI treatment group (P = 0.53).
Despite the 200 billion dollars spent annually on its management, spine pain remains a leading cause of disability and the most common cause to seek emergency care[20]. Therefore, the need for continued advancements in managing chronic spine symptomatology is clear. While surgical intervention may be indicated in select patients depending on the nature and severity of their conditions, nonoperative treatment remains the first-line management for most mechanical and radicular pain generated by the spine[21]. In this review, all studies investigating ACS for mechanical lumbar, lumbar radicular, and cervical radicular pain unanimously reported significant pain reduction compared to baseline. Pain relief was sustained through final follow-up, ranging between 3 and 6 months from treatment.
Disrupting the inflammation-pain cycle of chronic spine pathologies is a mainstay of nonoperative treatment strategies, and ACS represents a particularly intriguing option for the treatment of spine-related pain due to its anti-inflammatory properties. ACS has been widely marketed for the treatment of knee osteoarthritis as OrthokineTM in Europe and Re
ESIs serve both diagnostic and therapeutic purposes in spinal pain management, including identifying the anatomic locus of pain, providing short- or long-term pain relief, or delaying the need for surgical intervention; however, there is no definitive consensus on the exact indications of ESI treatment[28]. Further, patients experience variable responses with regard to the extent and duration of pain relief following ESI[29]. Patients are also limited to 2-3 ESIs annually to avoid the complication of increased degenerative changes secondary to increased osteoclast-driven bone turnover seen with repetitive corticosteroid treatment. Despite these limitations, ESI is a mainstay in the nonoperative management of many spine conditions and served as a comparison to ACS in several of the reviewed studies. ACS produced better long-term reduction in lumbar radicular symptoms when compared to 5 mg triamcinolone ESI, although no significant difference was appreciated compared to the 10 mg triamcinolone dose[15]. In the context of cervical radiculopathy, ACS treatment outperformed the methylprednisolone ESI regarding pain relief, further suggesting the comparable if not superior efficacy of ACS injection compared to ESI for pain relief[16]. In addition, ACS injections do not have the same limitation on dosing frequency that is observed with ESI and can be repeated as many times as necessary if symptom relief con
Of note, not all etiologies of spinal pain achieved significant relief with ACS. Godek et al[18] reported an improvement of radicular symptoms when DDD was the underlying pathology, but significant relief was not achieved in those with radicular pain secondary to spinal stenosis. This limitation has also been observed in ESI for lumbar stenosis and is thought to be due to the addition of fluid volume to an already compressed spinal canal along with a lipomatosis effect stimulated by the steroid[32]. In the remainder of our review, three studies only investigated radiculopathy due to DDD, and two studies did not clarify underlying pathology, making the evaluation of ACS for the treatment of spinal stenosis difficult to assess.
In addition to pain relief, all included studies assessed improvement in disability. All studies reported significant improvement in disability when compared to baseline as measured by various disability indices; however, there were variable findings across studies when comparing ACS to ESI. In patients with cervical radiculopathy, NDI and NPDS scores were significantly less following ACS injections than following methylprednisolone ESI injections[16]; however, no significant difference in ODI scores was observed between ACS and either 5 or 10 mg triamcinolone ESI for lumbar radiculopathy at 22 weeks[15]. The comparison of disability reduction after ACS vs ESI is inconclusive as the studies utilized variable ESI medications and different disability measures. Thus, additional studies are needed to make this comparison.
All studies reporting quality of life measures demonstrated significant improvement following ACS injections when assessed by several different subjective tools. This benefit was seen specifically for patients suffering from cervical or lumbar radiculopathy. The improvement in MCS is particularly relevant considering the well documented association between radicular pain and declining mental health outcomes[33]. The inclusion of this outcome was an important factor in assessing the utility of ACS treatment for patients living with chronic radicular pain.
Another potential benefit of ACS is the minimization of steroid treatment in diabetic patients concerned with blood glucose management. While long-term diabetes management assessed through hemoglobin A1C levels has been shown to be unaffected by ESI treatment, a transient increase in blood glucose levels for several days following ESI has been well-documented[34]. ACS represents an alternative treatment option for chronic spine conditions in this patient po
Finally, ACS has a favorable safety profile, with an overall adverse event rate of 3.1%, and no serious adverse events attributable to ACS were identified in this review. Self-limited adverse events reported in the studies, such as headache, dizziness, and syncope, have also been well documented among ESIs[35] and are most likely related to the penetrating nature of injections rather than the injectate. The safety of ACS was shown to be comparable to that of ESI, and this review derived no indication of ACS injection carrying a higher risk profile than other forms of epidural injections.
This study is a systematic review and is thus limited by the heterogeneity of data in the included articles and the lack of compatibility between cohorts at baseline. As a result, a meta-analysis was not performed to compare data given the different pathologies and outcomes reported by each study. One limitation of this study is the limited reporting of pre
While further research is needed for the evaluation of ACS in various spinal conditions and its comparison to ESI, its risk to benefit profile has shown promise for nonoperative management of spine conditions. ACS therapy for mechanical and radicular symptoms has demonstrated value when compared to ESI. Examined studies showed improved long term relief, ability to repeat treatments without risk of bone destruction, and elimination of excessive corticosteroid treatments in diabetic patients. ESI continues to be a useful treatment option due to its cost effectiveness relative to ACS and its ability to serve as a diagnostic tool, however the future of spine care can benefit from the inclusion of ACS in the treatment algorithm of nonoperative management. Future research is needed to compare and recommend specific ACS treatment protocols with long term outcome data focused on clinical outcomes. Examination of cost effectiveness, avoidance of surgical intervention, and subjective quality of life measures should be included in these future studies.
| 1. | Lee AS, Ellman MB, Yan D, Kroin JS, Cole BJ, van Wijnen AJ, Im HJ. A current review of molecular mechanisms regarding osteoarthritis and pain. Gene. 2013;527:440-447. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 296] [Cited by in RCA: 300] [Article Influence: 23.1] [Reference Citation Analysis (7)] |
| 2. | Sommer C, Kress M. Recent findings on how proinflammatory cytokines cause pain: peripheral mechanisms in inflammatory and neuropathic hyperalgesia. Neurosci Lett. 2004;361:184-187. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 687] [Cited by in RCA: 640] [Article Influence: 29.1] [Reference Citation Analysis (1)] |
| 3. | Gajtkó A, Bakk E, Hegedűs K, Ducza L, Holló K. IL-1β Induced Cytokine Expression by Spinal Astrocytes Can Play a Role in the Maintenance of Chronic Inflammatory Pain. Front Physiol. 2020;11:543331. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9] [Cited by in RCA: 55] [Article Influence: 9.2] [Reference Citation Analysis (0)] |
| 4. | Kim H, Hong JY, Lee J, Jeon WJ, Ha IH. IL-1β promotes disc degeneration and inflammation through direct injection of intervertebral disc in a rat lumbar disc herniation model. Spine J. 2021;21:1031-1041. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 46] [Article Influence: 9.2] [Reference Citation Analysis (0)] |
| 5. | Sekiguchi M, Kikuchi S, Myers RR. Experimental spinal stenosis: relationship between degree of cauda equina compression, neuropathology, and pain. Spine (Phila Pa 1976). 2004;29:1105-1111. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 57] [Cited by in RCA: 57] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 6. | Liao Z, Grimshaw RS, Rosenstreich DL. Identification of a specific interleukin 1 inhibitor in the urine of febrile patients. J Exp Med. 1984;159:126-136. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 131] [Cited by in RCA: 139] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 7. | Kaneko N, Kurata M, Yamamoto T, Morikawa S, Masumoto J. The role of interleukin-1 in general pathology. Inflamm Regen. 2019;39:12. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 528] [Cited by in RCA: 443] [Article Influence: 63.3] [Reference Citation Analysis (5)] |
| 8. | Wehling P, Moser C, Frisbie D, McIlwraith CW, Kawcak CE, Krauspe R, Reinecke JA. Autologous conditioned serum in the treatment of orthopedic diseases: the orthokine therapy. BioDrugs. 2007;21:323-332. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 112] [Cited by in RCA: 122] [Article Influence: 6.4] [Reference Citation Analysis (1)] |
| 9. | Firestein GS, Berger AE, Tracey DE, Chosay JG, Chapman DL, Paine MM, Yu C, Zvaifler NJ. IL-1 receptor antagonist protein production and gene expression in rheumatoid arthritis and osteoarthritis synovium. J Immunol. 1992;149:1054-1062. [DOI] [Full Text] |
| 10. | Evans CH, Chevalier X, Wehling P. Autologous Conditioned Serum. Phys Med Rehabil Clin N Am. 2016;27:893-908. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 37] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 11. | Curtis A, Beswick A, Jenkins L, Whitehouse M. Is there a role for autologous conditioned serum injections in osteoarthritis? A systematic review and meta-analysis of randomised controlled trials. Osteoarthritis Cartilage. 2024;. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 12. | Frisbie DD, Kawcak CE, Werpy NM, Park RD, McIlwraith CW. Clinical, biochemical, and histologic effects of intra-articular administration of autologous conditioned serum in horses with experimentally induced osteoarthritis. Am J Vet Res. 2007;68:290-296. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 223] [Cited by in RCA: 173] [Article Influence: 9.1] [Reference Citation Analysis (0)] |
| 13. | Godek P, Szczepanowska-Wolowiec B, Golicki D. Comparison of Analgesic Efficacy between Epidural and Perineural Administration of Autologous Conditioned Serum in the Conservative Treatment of Low Back Pain Due to Lumbar Degenerative Disc Disease: A Randomized, Open-Label, Controlled Clinical Trial. Brain Sci. 2023;13. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 14. | Higgins JP, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327:557-560. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 15. | Becker C, Heidersdorf S, Drewlo S, de Rodriguez SZ, Krämer J, Willburger RE. Efficacy of epidural perineural injections with autologous conditioned serum for lumbar radicular compression: an investigator-initiated, prospective, double-blind, reference-controlled study. Spine (Phila Pa 1976). 2007;32:1803-1808. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 65] [Cited by in RCA: 73] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 16. | Goni VG, Singh Jhala S, Gopinathan NR, Behera P, Batra YK, R H H A, Guled U, Vardhan H. Efficacy of Epidural Perineural Injection of Autologous Conditioned Serum in Unilateral Cervical Radiculopathy: A Pilot Study. Spine (Phila Pa 1976). 2015;40:E915-E921. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 18] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 17. | H S RK, Goni VG, Y K B. Autologous Conditioned Serum as a Novel Alternative Option in the Treatment of Unilateral Lumbar Radiculopathy: A Prospective Study. Asian Spine J. 2015;9:916-922. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 22] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 18. | Godek P, Szajkowski S, Golicki D. Evaluation of the Effectiveness of Orthokine Therapy: Retrospective Analysis of 1000 Cases. Ortop Traumatol Rehabil. 2020;22:107-119. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 5] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 19. | Godek P. Use of Autologous Serum in Treatment of Lumbar Radiculopathy Pain. Pilot Study. Ortop Traumatol Rehabil. 2016;18:11-20. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 15] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 20. | Casiano VE, Sarwan G, Dydyk AM, Varacallo M. Back Pain. 2023 Dec 11. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. [PubMed] |
| 21. | Chou R, Loeser JD, Owens DK, Rosenquist RW, Atlas SJ, Baisden J, Carragee EJ, Grabois M, Murphy DR, Resnick DK, Stanos SP, Shaffer WO, Wall EM; American Pain Society Low Back Pain Guideline Panel. Interventional therapies, surgery, and interdisciplinary rehabilitation for low back pain: an evidence-based clinical practice guideline from the American Pain Society. Spine (Phila Pa 1976). 2009;34:1066-1077. [PubMed] [DOI] [Full Text] |
| 22. | Baltzer AW, Moser C, Jansen SA, Krauspe R. Autologous conditioned serum (Orthokine) is an effective treatment for knee osteoarthritis. Osteoarthritis Cartilage. 2009;17:152-160. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 186] [Cited by in RCA: 220] [Article Influence: 12.9] [Reference Citation Analysis (0)] |
| 23. | Damjanov N, Barac B, Colic J, Stevanovic V, Zekovic A, Tulic G. The efficacy and safety of autologous conditioned serum (ACS) injections compared with betamethasone and placebo injections in the treatment of chronic shoulder joint pain due to supraspinatus tendinopathy: a prospective, randomized, double-blind, controlled study. Med Ultrason. 2018;20:335-341. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 31] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 24. | Darabos N, Haspl M, Moser C, Darabos A, Bartolek D, Groenemeyer D. Intraarticular application of autologous conditioned serum (ACS) reduces bone tunnel widening after ACL reconstructive surgery in a randomized controlled trial. Knee Surg Sports Traumatol Arthrosc. 2011;19 Suppl 1:S36-S46. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 69] [Cited by in RCA: 73] [Article Influence: 4.9] [Reference Citation Analysis (0)] |
| 25. | Meijer H, Reinecke J, Becker C, Tholen G, Wehling P. The production of anti-inflammatory cytokines in whole blood by physico-chemical induction. Inflamm Res. 2003;52:404-407. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 114] [Cited by in RCA: 122] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 26. | Wright-Carpenter T, Opolon P, Appell HJ, Meijer H, Wehling P, Mir LM. Treatment of muscle injuries by local administration of autologous conditioned serum: animal experiments using a muscle contusion model. Int J Sports Med. 2004;25:582-587. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 100] [Cited by in RCA: 85] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 27. | Khan AN, Jacobsen HE, Khan J, Filippi CG, Levine M, Lehman RA Jr, Riew KD, Lenke LG, Chahine NO. Inflammatory biomarkers of low back pain and disc degeneration: a review. Ann N Y Acad Sci. 2017;1410:68-84. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 128] [Cited by in RCA: 264] [Article Influence: 33.0] [Reference Citation Analysis (0)] |
| 28. | Carassiti M, Pascarella G, Strumia A, Russo F, Papalia GF, Cataldo R, Gargano F, Costa F, Pierri M, De Tommasi F, Massaroni C, Schena E, Agrò FE. Epidural Steroid Injections for Low Back Pain: A Narrative Review. Int J Environ Res Public Health. 2021;19. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 34] [Cited by in RCA: 45] [Article Influence: 9.0] [Reference Citation Analysis (0)] |
| 29. | Buchner M, Zeifang F, Brocai DR, Schiltenwolf M. Epidural corticosteroid injection in the conservative management of sciatica. Clin Orthop Relat Res. 2000;149-156. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 84] [Cited by in RCA: 65] [Article Influence: 2.5] [Reference Citation Analysis (1)] |
| 30. | Hecht M. Regenokine Treatment: Effectiveness vs. Platelet-Rich Plasma. Healthline. 2020. Available from: https://www.healthline.com/health/regenokine. |
| 31. | Carreon LY, Bratcher KR, Ammous F, Glassman SD. Cost-effectiveness of Lumbar Epidural Steroid Injections. Spine (Phila Pa 1976). 2018;43:35-40. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 15] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 32. | Radcliff K, Kepler C, Hilibrand A, Rihn J, Zhao W, Lurie J, Tosteson T, Vaccaro A, Albert T, Weinstein J. Epidural steroid injections are associated with less improvement in patients with lumbar spinal stenosis: a subgroup analysis of the Spine Patient Outcomes Research Trial. Spine (Phila Pa 1976). 2013;38:279-291. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 39] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 33. | Mansfield M, Thacker M, Taylor JL, Bannister K, Spahr N, Jong ST, Smith T. The association between psychosocial factors and mental health symptoms in cervical spine pain with or without radiculopathy on health outcomes: a systematic review. BMC Musculoskelet Disord. 2023;24:235. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 11] [Reference Citation Analysis (0)] |
| 34. | Even JL, Crosby CG, Song Y, McGirt MJ, Devin CJ. Effects of epidural steroid injections on blood glucose levels in patients with diabetes mellitus. Spine (Phila Pa 1976). 2012;37:E46-E50. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 57] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 35. | Manchikanti L. Effectiveness of Therapeutic Lumbar Transforaminal Epidural Steroid Injections in Managing Lumbar Spinal Pain. Pain Phys. 2012;15:E199-E245. [RCA] [DOI] [Full Text] [Cited by in Crossref: 97] [Cited by in RCA: 109] [Article Influence: 7.8] [Reference Citation Analysis (0)] |
| 36. | Godek P, Paprocka-Borowicz M, Ptaszkowski K. Comparative Efficacy of Ultrasound-Guided Cervical Fascial Infiltration versus Periarticular Administration of Autologous Conditioned Serum (Orthokine) for Neck Pain: A Randomized Controlled Trial Protocol Description. Med Sci Monit. 2024;30:e942044. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
Open-Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/