INTRODUCTION
Anomalous origin of the coronary artery from opposite coronary sinus is infrequently observed during coronary angiography. Percutaneous coronary intervention (PCI) of anomalous coronaries is technically difficult and challenging. It requires a proper selection of hardware and adequate/appropriate expertise of the operator to perform the intervention. We hereby report a rare case of anomalous origin of left main coronary artery (LM) from the right coronary sinus, in which successful PCI of the left anterior descending (LAD) artery was performed. A long term 5-year follow-up of favorable clinical outcome and coronary arterial imaging is also demonstrated.
CASE REPORT
In August 2006, a 59-year-old male presented to the out-patient department with a history of chest pain, which first occurred 4 d previously during morning hours. He was a non-smoker, non-diabetic and had normal blood pressure. An ECG done by a local physician showed left bundle branch block (LBBB). A repeat ECG at our institute was within normal limits. His general physical and systemic examinations were unremarkable. His routine biochemistry was normal. Fasting lipid profile revealed total cholesterol 198 mg%, HDL 42 mg%, LDL 110 mg%, and triglycerides 236 mg%. Two-dimensional echocardiogram showed a left ventricular ejection fraction of 0.60, no regional wall motion abnormality and no mitral regurgitation. He underwent coronary angiography by trans-femoral route. The right coronary artery (RCA), which was cannulated with a Judkins Right 4, 6F catheter, was a normal and dominant vessel. The LM could not be visualized in the left coronary sinus with the Judkins Left 4, 6F catheter. Subsequently, it was found to be arising from the right coronary sinus. Both RCA and LM were arising from separate ostia. The LM had a retro-aortic course from the right coronary sinus before its bifurcation into LAD and left circumflex (LCx) arteries (Figure 1A and B). The LAD showed two type B lesions in proximal (Figure 1B) and distal segments (Figure 1C). The LCx, which was a non-dominant vessel, showed insignificant stenosis in the distal segment. A left ventriculogram showed an ejection fraction of 0.60 and no regional wall motion abnormality.
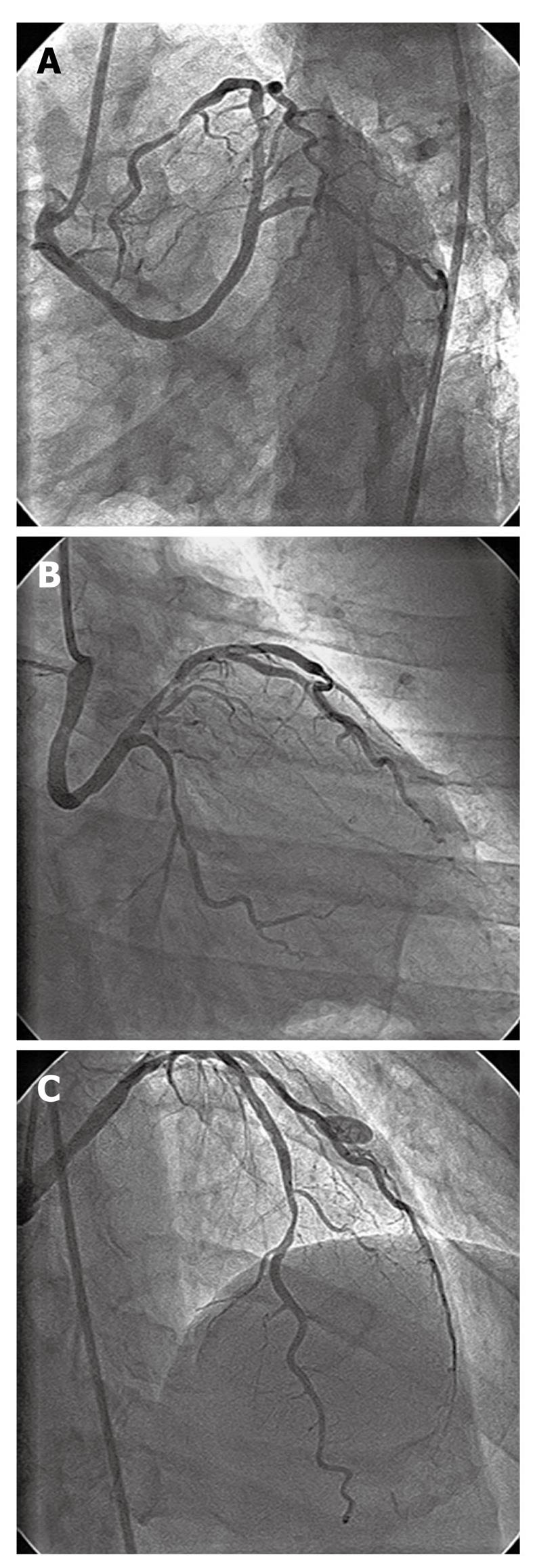
Figure 1 Left coronary angiogram after injection from right coronary sinus.
A: Separate ostial origin of anomalous left main coronary artery from right coronary sinus, having retro-aortic course; B: Proximal left anterior descending (LAD) artery having type B 70% tubular stenosis, proximal left circumflex artery having 50% diffuse stenosis; C: Distal LAD artery having type B 70% tubular stenosis.
Following a written informed consent for percutaneous revascularization, the patient was subjected to PCI of the LAD artery, in a second stage after 48 h. The anomalous LM was cannulated with an Eric Cohen Right (ECR) 4, 6F coronary guide catheter (an extra-backup support catheter for RCA from Medtronic, Inc., Minneapolis, Minnesota) and LAD lesions were crossed with an All Track Wire (ATW) coronary guide wire (Cordis Co., Miami, Florida). Both proximal and distal LAD lesions were pre-dilated with a 2.5 mm × 15 mm Sprinter balloon (Medtronic). The distal LAD lesion was stented with a 2.5 mm × 23 mm sirolimus-eluting Cypher stent (Cordis) (Figure 2A) and the proximal LAD lesion was stented with a 3 mm × 23 mm sirolimus-eluting Cypher stent (Cordis) (Figure 2B). He had an uneventful recovery and was discharged on day 2 of intervention with dual anti-platelet and statin therapy. He remained asymptomatic on follow-up. A check angiogram at 9 mo of follow-up showed patent LAD stents with no endoluminal loss. The check angiogram was performed for demonstration of patency of stents for academic reasons only. At 4 years of follow-up, a 64-slice MDCT coronary scan revealed good antegrade flow across the stented LAD segments and also demonstrated the retro-aortic course of the LM (Figure 3A and B). After the PCI, he remained asymptomatic throughout his 5 years of follow-up.
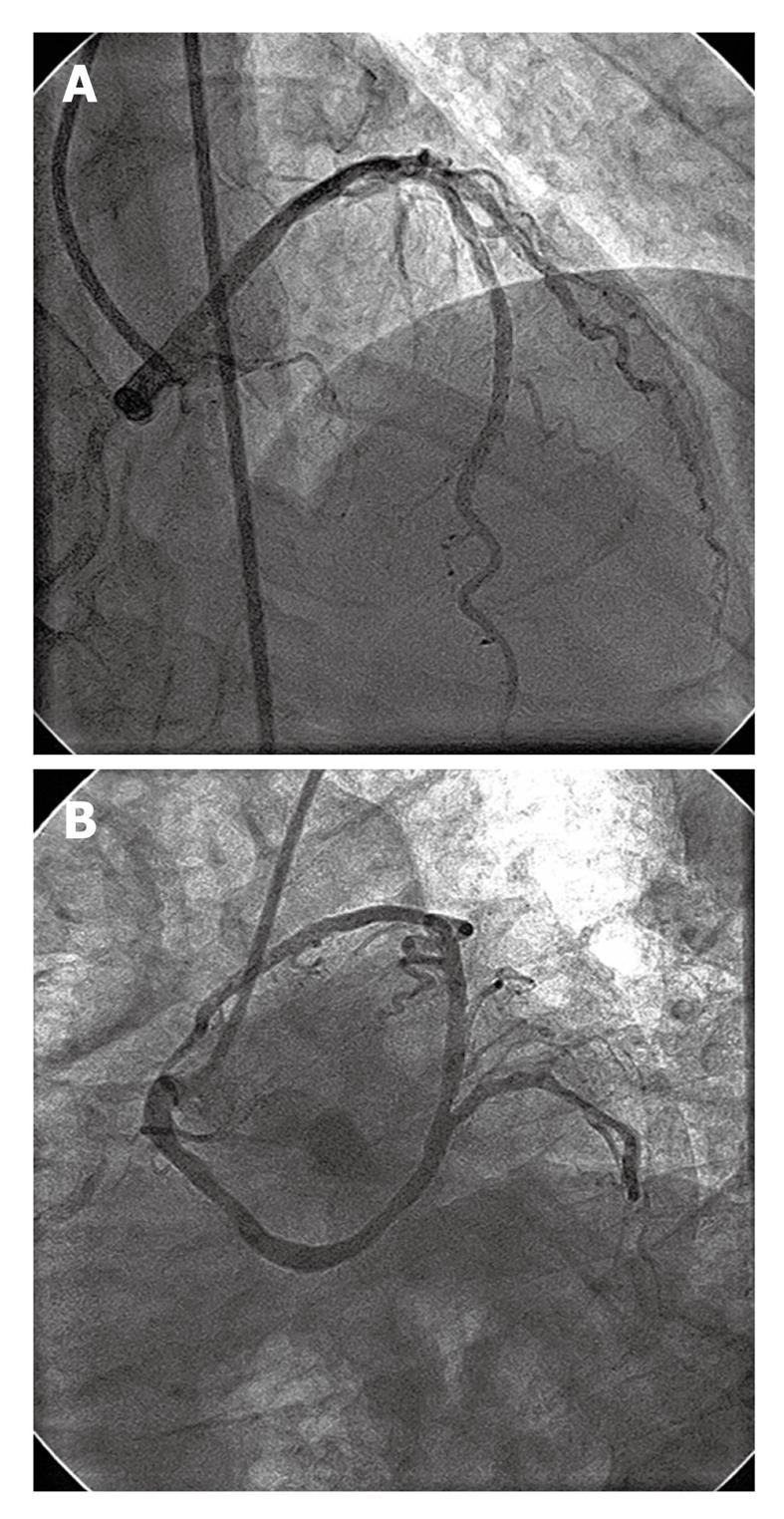
Figure 2 Left coronary angiogram following coronary stenting of left anterior descending artery.
A: Distal left anterior descending (LAD) lesion stented with 2.5 mm × 23 mm sirolimus-eluting stent; B: Proximal LAD lesion stented with 3 mm × 23 mm sirolimus-eluting stent.
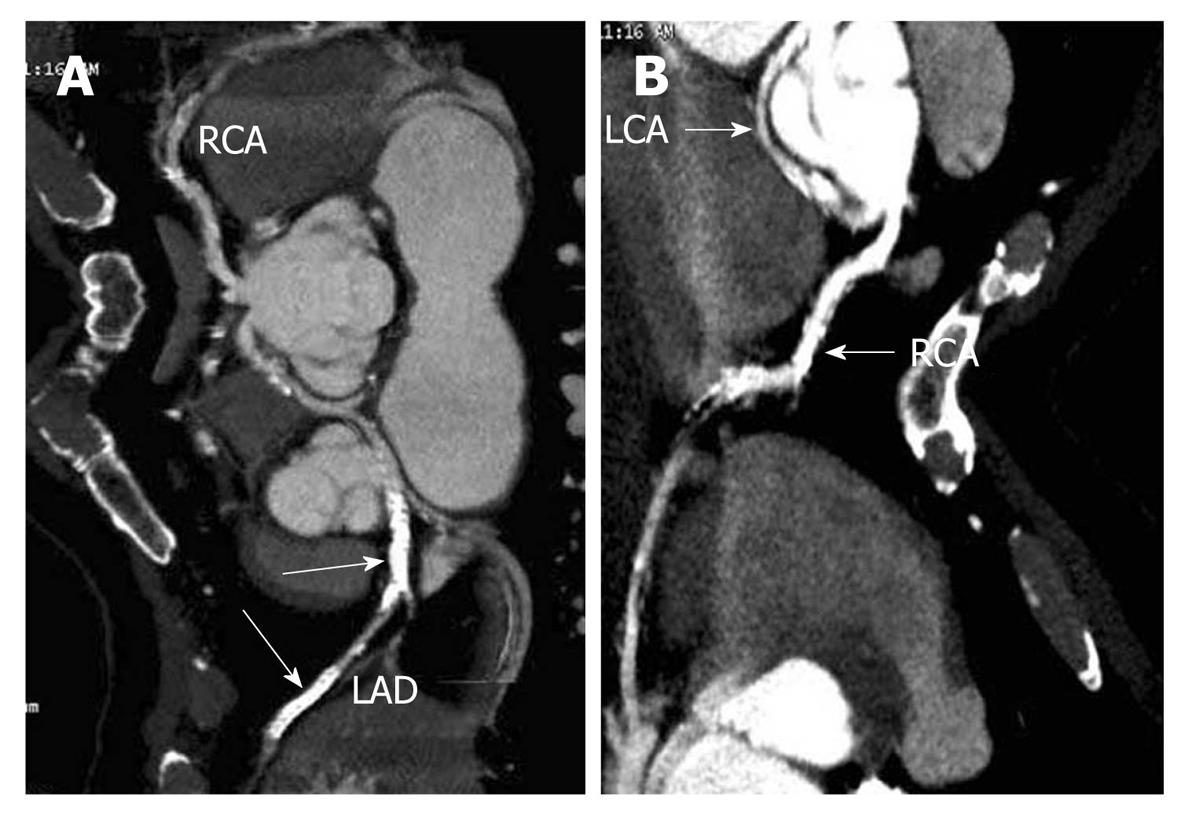
Figure 3 64-slice multi-detector computed tomography image of coronary arteries.
A: Computed tomography (CT) image showing separate ostia of both right and left main coronary artery. The left anterior descending stents are marked with white arrow; B: CT image showing retro-aortic course of left main coronary artery. RCA: Right coronary artery; LCA: Left coronary artery; LAD: Left anterior descending.
DISCUSSION
Coronary artery anomalies are present since birth, but relatively few are symptomatic during childhood or later in life. Most of the anomalies are incidentally detected during selective coronary angiography. The incidence of coronary anomalies among individuals subjected for catheterization varies from 0.6% to 1.3% in various series[1]. Anomalous LM arising from the right coronary sinus is a rare anomaly, having the incidence of 0.017% in an angiographic series[1]. The course of anomalous LM can be inter-arterial, retro-aortic, septal or through the anterior free wall of the right ventricle[1]. It is more common to have an inter-arterial or septal course than the retro-aortic course[1-4]. The retro-aortic course, as present in the index case, is the less common anomaly of LM and is usually benign in nature in comparison to inter-arterial or septal course[1,4]; however, a few authors have reported adverse outcomes even with retro-aortic course[5-7]. This index case had angina secondary to atherosclerotic disease of the LAD and not because of anomalous retro-aortic course of LM, as the patient remained asymptomatic following intervention at long term follow-up. Anomalous coronary artery arising from the opposite coronary sinus is associated with angina, myocardial infarction and sudden cardiac death, even in the absence of significant atherosclerotic stenosis[8]. The pathogenesis of these clinical manifestations can be multi-factorial including anomalous coronary compression with inter-arterial course, slit-like coronary orifice with dynamic obstruction, acute angle take off, and presence and length of intramural segments of anomalous coronary vessel[8-10].
PCI of anomalous coronaries is difficult, technically challenging, and requires significant experience for successful intervention[11,12]. However, a failed PCI and subsequent bypass surgery in an acute myocardial infarction situation with anomalous left main coronary artery has even been described[13]. During the intervention, there is a need for coaxial alignment and adequate backup support of the guide catheter for successful outcome. Various authors have described different types of guide catheters, such as Amplatz Right, Amplatz Left, Multipurpose catheter, etc., for intervention in such situations[11,14,15]. In the described case, we used an ECR guide catheter, which provided a good backup support and also coaxial alignment during intervention. Even though there are reports about PCI of anomalous LM with inter-arterial or septal course[10,11,14,15], only a single case report of PCI of LM with retro-aortic course has been published[5]. To our knowledge, the index case is the second one in the published literature about PCI with regard to anomalous LM having a retro-aortic course.
The role of multi-detector computed tomography (MDCT) for detection of coronary stent patency[16] and delineation of anomalous coronary origin, course and relation[17] has been described in the literature. In the index case, MDCT has demonstrated the patency of the LAD drug-eluting stents and delineated the origin and course of anomalous LM.
In conclusion, we hereby report a rare case of anomalous LM originating from the right coronary sinus and having a retro-aortic course, in which a successful coronary stenting of the LAD artery was performed. Follow-up MDCT imaging demonstrated the long term patency of drug-eluting stents, and also delineated the origin and course of anomalous LM.
Peer reviewers: MG Bourassa, MD, Research Center, Montreal Heart Institute, Montreal, Quebec, H1T 1C8, Canada; Manel Sabaté, MD, PhD, Chief, Cardiology Department, Clinic University Hospital, c/Villarroel 170, 08036 Barcelona, Spain; Alfredo E Rodriguez, MD, PhD, FACC, FSCAI, Heard Institutional Cardiology, Otamendi Hospital, Post Graduate School of Medicine, Cardiac Unit, Azcuenaga 870, Buenos Aires, C1115AAB, Argentina; Rodrigo Bagur, Interventional Cardiology, Quebec Heart and Lung Institute, Laval University, 852, Av Du Chanoine-Scott #1, Quebec G1V3N6, Canada
S- Editor Cheng JX L- Editor Logan S E- Editor Zheng XM