Published online Mar 27, 2026. doi: 10.4240/wjgs.v18.i3.115137
Revised: November 14, 2025
Accepted: January 12, 2026
Published online: March 27, 2026
Processing time: 163 Days and 21.8 Hours
Splenic tuberculosis is a rare disease, most commonly presenting with fever, weight loss, anemia, and splenic lesions. However, these signs and symptoms lack specificity and are easily confused with other abdominal diseases. Particularly in patients who have received anti-tuberculosis treatment, there may be no specific clinical symptom, leading to misdiagnosis and missed diagnosis. Moreover, due to the absence of specific symptoms in such patients, definitive diagnosis based solely on ultrasound and magnetic resonance imaging is challenging, typically requiring postoperative pathological examination for confirmation. Here, we report a case of asymptomatic splenic tuberculosis, analyzed the diagnostic and therapeutic processes, and discuss key considerations in managing splenic tub
A 28-year-old male was admitted to Lishui Municipal Central Hospital on April 8, 2024, following the incidental discovery of an isolated splenic mass during a routine physical examination. Initial findings after admission suggested a cystic tumor within the spleen. After comprehensive diagnostic evaluations, the patient underwent laparoscopic partial splenectomy. The postoperative pathological diagnosis was a splenic tuberculosis. An interview with the patient revealed a history of tuberculosis that had been cured following anti-tuberculosis treatment, although no follow-up examination was conducted post-treatment. The patient’s recovery was uneventful and the postoperative prognosis was favorable.
Splenic tuberculosis should be considered for patients with risk factors for tub
Core Tip: Although rare, splenic tuberculosis should be considered for patients with risk factors for tuberculosis or a relevant history. A high index of suspicion should be maintained for splenic masses with an unclear diagnosis to avoid missed diagnosis of splenic tuberculosis. When necessary, percutaneous needle biopsy may be performed to confirm the diagnosis, thereby avoiding unnecessary surgical intervention. Alternatively, after thorough evaluation, partial splenectomy may be considered to preserve spleen function.
- Citation: Li ZK, Zhang K, Zhang HL, Lv XL, Guo JQ, Tan W. Splenic tuberculous mass following anti-tuberculosis therapy was misdiagnosed as a splenic tumor: A case report. World J Gastrointest Surg 2026; 18(3): 115137
- URL: https://www.wjgnet.com/1948-9366/full/v18/i3/115137.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v18.i3.115137
The incidence of tuberculosis in China is the third highest globally, with extrapulmonary tuberculosis accounting for 15%-20% of all cases. The abdomen is the most common site of extrapulmonary tuberculosis. Abdominal tuberculosis can affect almost any organ, most commonly the gastrointestinal tract, omentum, and lymph nodes[1]. However, splenic tuberculosis is relatively rare in clinical practice, often presenting as a space-occupying lesion on imaging, which can easily be misdiagnosed as a splenic tumor. Isolated splenic tuberculosis forming a tuberculoma is especially rare, and diagnosis often relies on pathological examination. Here, we reported a case of a suspected splenic tumor that was confirmed as splenic tuberculosis by a postoperative pathological examination.
A 28-year-old male was admitted to our hospital on April 8, 2024, due to an incidental finding of a splenic mass during a physical examination.
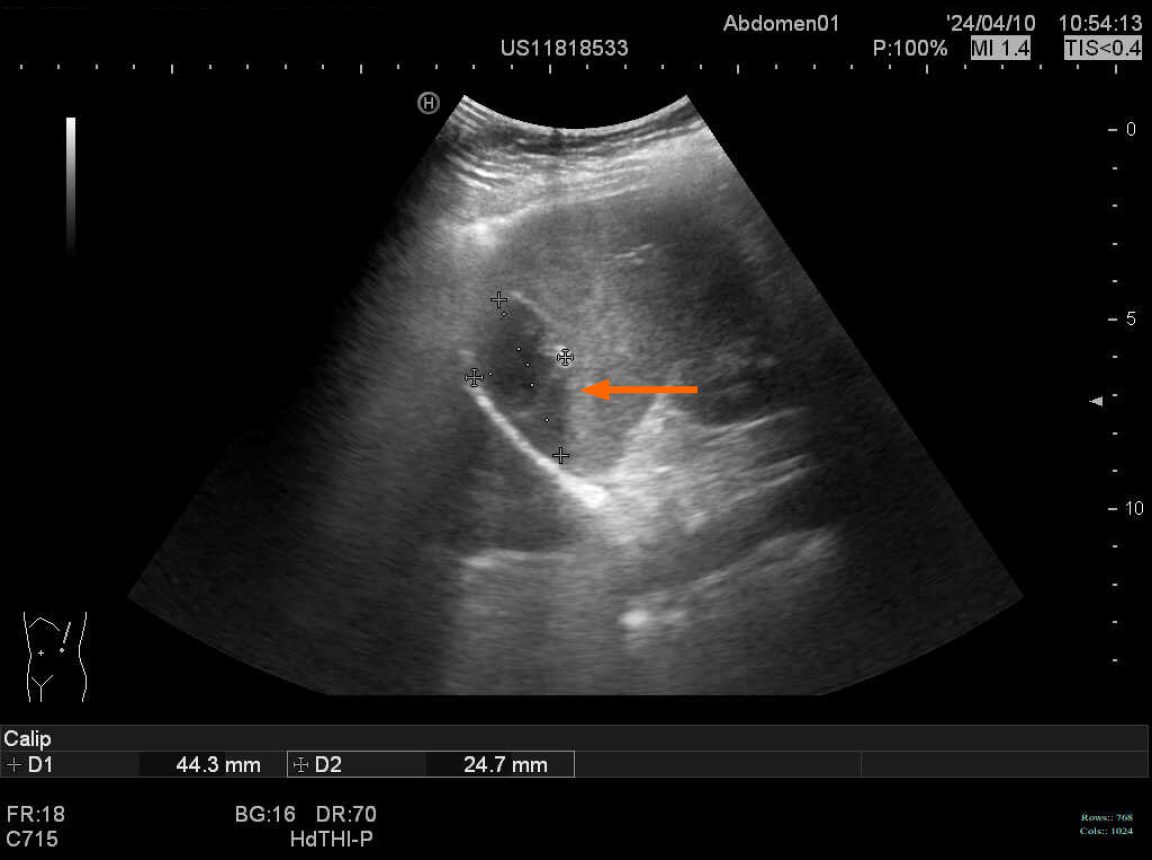
The patient underwent an examination at our hospital on April 15, 2024. Abdominal ultrasound revealed a cystic mass within the spleen, characterized by a 44 mm × 25 mm liquid hypoechoic area with poor acoustic transmission and visible echogenic bands (Figure 1). The patient reported no significant symptoms of abdominal pain, distension, fever, chills, diarrhea, or constipation.
The patient underwent 1.5 years of formal drug treatment locally for “pulmonary tuberculosis” over 2 years prior to admission, and reported that the tuberculosis had been controlled. However, this past medical history was not disclosed initially and was only obtained after postoperative follow-up inquiries.
The patient's personal and family medical histories were not relevant.
Upon admission, the patient’s physical examination was unremarkable: Normal heart rate, blood pressure, and temperature. The skin and mucous membranes showed no jaundice, no palpable superficial lymph node, and no significant abnormality of the heart or lungs. The abdomen was soft without tenderness or a palpable mass. Both the liver and spleen were not palpable.
The results of routine urine, stool, and occult blood tests, a rapid high-sensitivity C-reactive protein test, complete blood count, tumor markers (carcinoembryonic antigen, alpha-fetoprotein, cancer antigens 153, 199, 724), thyroid function, and glycosylated hemoglobin were all normal. Liver and kidney functions were within normal ranges, except for slightly reduced serum creatinine and elevated estimated glomerular filtration rate. Hepatitis C antibodies, hepatitis B, syphilis, and human immune deficiency virus tests were all negative.
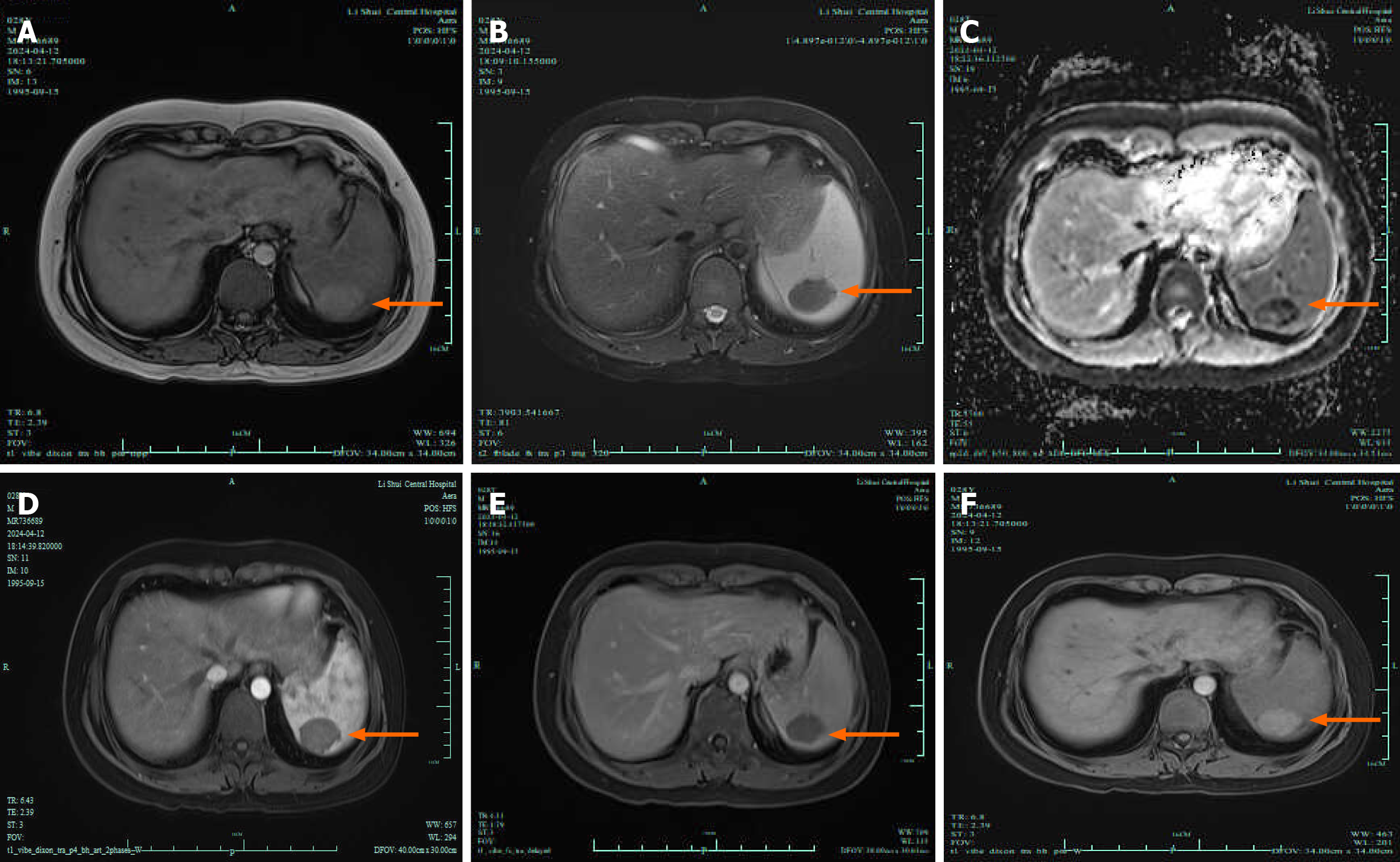
To clarify the diagnosis, enhanced magnetic resonance imaging (MRI) of the spleen was performed, which suggested “cystic lesions in the spleen, likely a complex cyst or old hemorrhage” (Figure 2). Additional testing included an electrocardiogram, which was normal, and chest computed tomography (CT), which revealed secondary pulmonary tub
The initial diagnosis on admission was a splenic space-occupying lesion. The differential diagnoses for common splenic space-occupying lesions are as follows.
Primary benign splenic tumors (predominantly hemangiomas and hamartomas): No systemic symptoms and normal tumor markers. Hemangiomas show “fast-in, slow-out” enhancement on CT/MRI, while hamartomas may contain fatty/calcified components.
Primary malignant splenic tumors (e.g., angiosarcoma): Rapid tumor progression may cause clinical manifestations, such as splenomegaly and abdominal pain. MRI shows blurred margins and mixed signal intensity, often accompanied by hemorrhage and necrosis, with heterogeneous enhancement after contrast administration.
Metastatic splenic tumors: History of primary malignancy (commonly hepatocellular carcinoma, gastric cancer, breast cancer, etc.). Some cases present with systemic symptoms like weight loss and fatigue. Tumor markers may be elevated. Typically multiple, round lesions with relatively clear margins, low density/signal on CT/MRI, and marginal en
Splenic lymphoma: May present with fever, night sweats, weight loss, etc. Blood tests may show abnormal lymphocyte counts. Imaging reveals diffuse splenomegaly or multiple/single nodules. Ultrasound shows hypoechoic lesions. CT/MRI shows uniform low density/signal intensity with mild enhancement post-contrast, but without obvious necrosis. Diagnosis confirmed by bone marrow aspiration or splenic biopsy.
Splenic abscess: Often associated with infectious triggers like sepsis or adjacent organ infections. Clinical presentation typically includes high fever, chills, and left upper quadrant pain. Marked elevation in white blood cell and neutrophil counts. Imaging shows a thick-walled cystic lesion with a fluid-filled dark area and bright spots. CT demonstrates an
Splenic cyst: Often asymptomatic with no elevated infection markers. CT shows a well-defined low-density lesion with no enhancement after contrast.
Splenic infarction: Commonly associated with atrial fibrillation or thrombosis history. Typically presents as sudden left upper quadrant pain. CT reveals a wedge-shaped low-density lesion pointing toward the splenic hilum, with no contrast enhancement.
Splenic tuberculosis: Characterized by systemic tuberculosis symptoms (low-grade fever, night sweats). Imaging findings reveal multiple small nodules with calcification, mild contrast enhancement, and positive tuberculin skin test or gamma interferon release assay.
We concluded that the MRI findings of this lesion do not closely correspond with any of the aforementioned differential diagnoses. Hence, the nature of the lesion remains unclear.
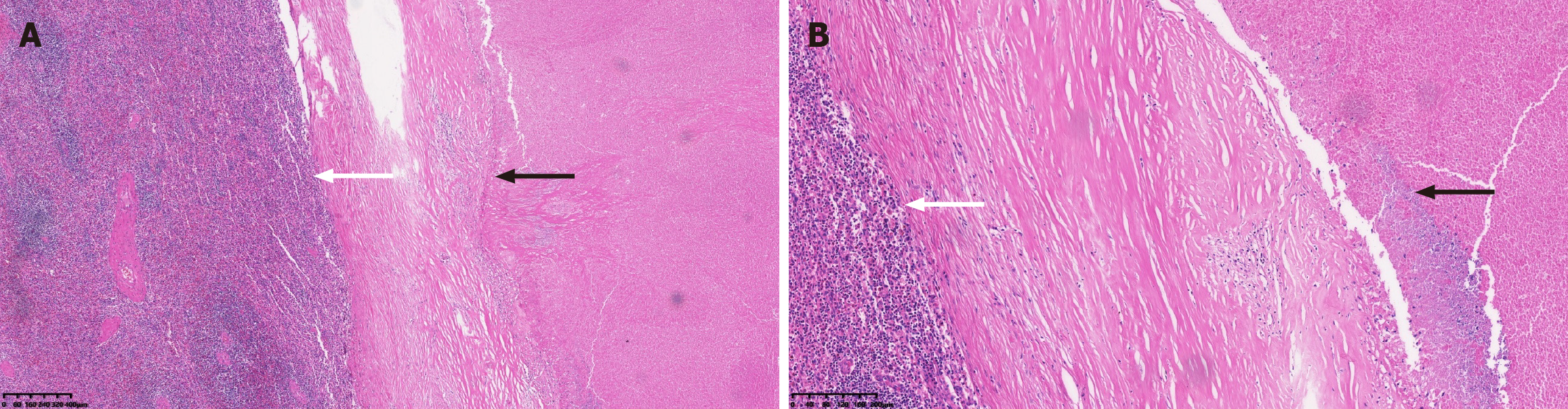
Postoperative pathological assessment: “Partial spleen” submitted for examination showed spleen tissue with two necrotic foci (the larger measuring 4.5 cm × 3 cm × 2.5 cm, with the smaller 1.3 cm in maximum diameter), clearly demarcated with fibrous encapsulation, and granuloma formation around the necrotic area. The patient’s clinical history combined with hematoxylin and eosin staining revealed that the morphology of the lesions was consistent with tub
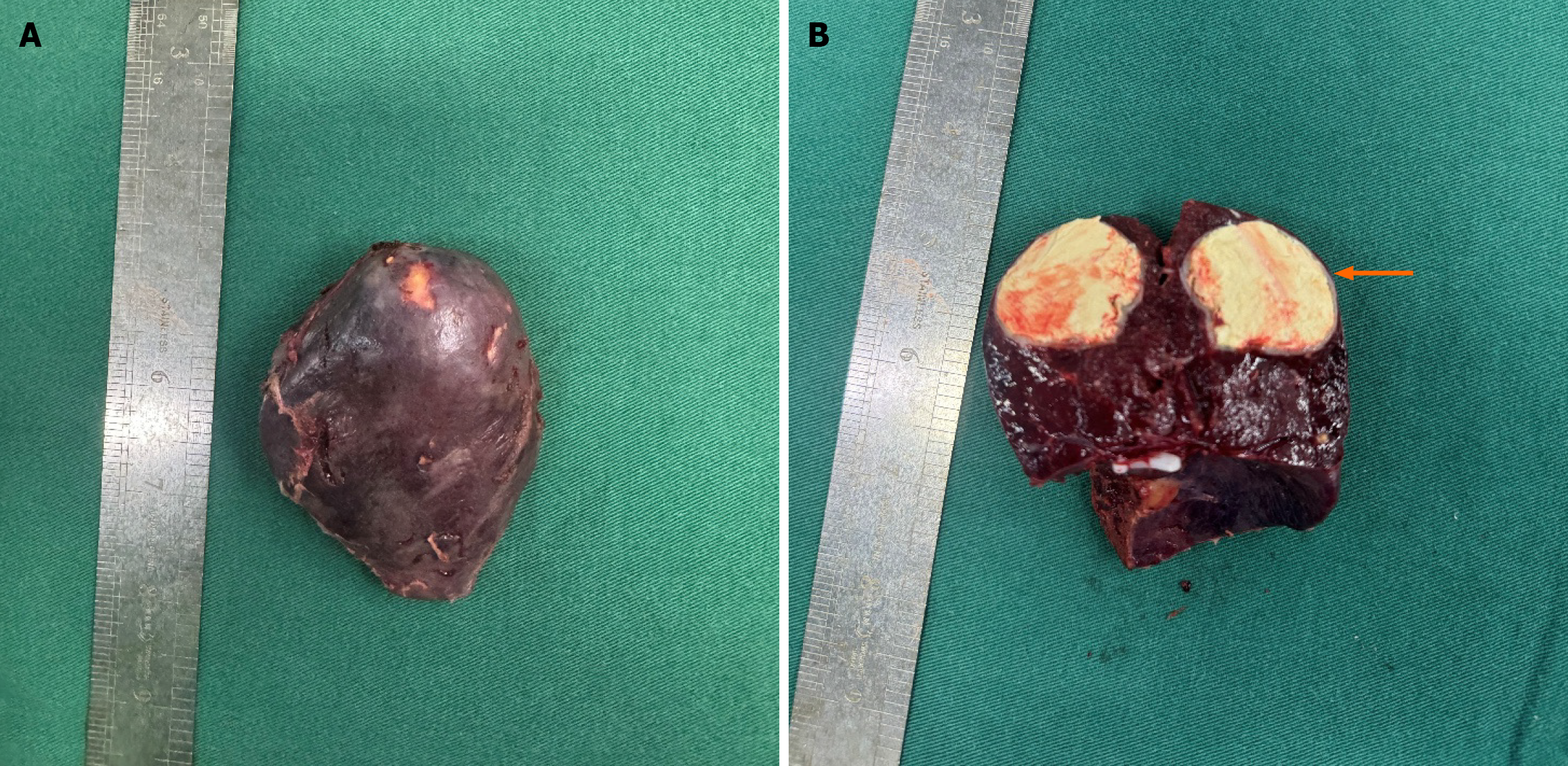
To clarify the diagnosis and eliminate a malignancy, after excluding contraindications for surgery, the patient underwent surgical treatment on April 15, 2024. Intraoperative laparoscopic exploration revealed extensive adhesions within the abdominal cavity involving the gastrointestinal tract, greater omentum, mesentery, and abdominal wall. The spleen was wrapped in omental adhesions, with a soft reddish texture, measuring approximately 10 cm × 9 cm × 5 cm. The spleen contained two solid masses, measuring approximately 3.5 cm × 2.5 cm and 1 cm, respectively, with a firm texture and clear boundaries; the cut surface was yellowish-white (Figure 4). After separating the adhesions, a partial splenectomy was performed laparoscopically. Postoperative recovery was uneventful with no complications.
The patient’s recovery was uneventful and he was discharged on April 24, 2024. Postoperative follow-up examinations at regular intervals yielded favorable results.
Extrapulmonary tuberculosis rarely occurs in a single organ[2], especially in immunocompetent patients. Consequently, data on the incidence of splenic tuberculosis in immunocompetent patients is extremely scarce[3]. Splenic tuberculosis is a rare manifestation of extrapulmonary tuberculosis, often presenting challenges for diagnosis and treatment. This paper discussed the epidemiology, clinical manifestations, diagnostic methods, treatment strategies, and prognosis of splenic tuberculosis, in conjunction with the presented case.
Splenic tuberculosis is a component of systemic tuberculosis, which often coexists with tuberculosis of other organs, and is typically classified as primary or secondary[4]. The main route of splenic tuberculosis infection is via hematogenous spread, but can also occur through the lymphatics or direct extension from an adjacent infected organ. Splenic tuberculosis is more common in patients with conditions that reduce immunity, such as acquired immunodeficiency syndrome, diabetes, immunosuppressive treatment, or corticosteroid use[5,6]. Therefore, secondary splenic tuberculosis is clinically more common than primary tuberculosis. The spleen is a common site for miliary tuberculosis[7], often as a manifestation of disseminated disease. Primary splenic tuberculosis refers to cases where the spleen is the sole or primary affected organ outside the initial infection focus, however, it is technically a secondary tuberculosis that appears only in the spleen (hence, also called isolated splenic tuberculosis). Some reports have suggested that all cases of splenic tuberculosis are secondary to infection from other organs. Primary splenic tuberculosis is less common than secondary splenic tuberculosis and is mostly documented in case reports. Tuberculoma, a secondary form of tuberculosis in adults, typically consists of a single, cheese-like necrotic focus surrounded by fibrous tissue, forming a ball-shaped lesion. In this case, the patient’s splenic tuberculosis also presented as an isolated lesion > 3 cm, which is a rare situation, rendering preoperative diagnosis more difficult.
The clinical presentation of splenic tuberculosis lacks specificity, often leading to a delayed diagnosis. Common symptoms include fever[8], weight loss, abdominal pain, and night sweats, sometimes accompanied by hepatosplenomegaly. Typical clinical manifestations may include left upper abdominal pain with fever, general discomfort, and weight loss, often with a chronic course. However, relatively few reports in the literature have cited these typical clinical manifestations, as the common systemic symptoms of splenic tuberculosis mainly include fever (82.3% of cases), malaise, and weight loss (44.12% of cases)[9]. Localized symptoms, such as pain in the left upper abdominal region, are most common, while the absence of localized symptoms is rare. In the present case, a physical examination finding of splenic occupancy and imaging were suggestive of a large isolated nodule, causing us to overlook the possibility of splenic tuberculosis. Retrospective analysis of this case revealed that the patient had a history of pulmonary tuberculosis and had received anti-tuberculosis treatment, while there were no obvious special symptom per se. With such cases, we should keep in mind that splenic occupation should not exempt the possibility of tuberculosis, especially if there is a history of tuberculosis and other high-risk factors. Hence, the patient’s history should be carefully considered and appropriate investigations should be conducted, especially appropriate imaging, to improve the diagnosis.
Imaging studies are valuable for the clinical diagnosis of splenic tuberculosis. Ultrasound and CT can detect splenic abnormalities. The most common ultrasound finding is a single or multiple hypoechoic lesions, where regular hypoechoic lesions often suggest tuberculous nodules, while irregular hypoechoic lesions may indicate a tuberculous splenic abscess. However, in most cases, the appearance of these lesions is not specific, thereby limiting diagnostic accuracy. CT of the abdomen has advantages over ultrasound for the detection of lesions, especially splenic abscesses and small calcifications. There are four types of CT presentations for splenic tuberculosis: Miliary, abscess, nodular, and fibrous-calcified. Isolated splenic tuberculosis commonly presents as nodular lesions, although lesions > 3 cm are particularly rare[10]. Due to the nonspecific nature of splenic tuberculosis, ultrasound and CT can identify splenic abnormalities, with ultrasound suggesting hypoechoic lesions and CT often showing low-density lesions[11,12]. However, these findings are not definitive for determining the nature of the lesion. Compared to CT or ultrasound, enhanced MRI combined with T2-weighted imaging can better reflect lesion characteristics, and diffusion-weighted imaging can improve the prediction of malignant lesions[13]. Overall, the imaging appearance of splenic tuberculosis is dependent on the route of infection, lesion size, and disease stage, thereby rendering the imaging findings more complex. In this case, ultrasound suggested a cystic area within the spleen, while MRI suggested cystic lesions, which was coupled with the lack of a detailed inquiry into a history of tuberculosis. The finding of splenic occupational lesions and the lack of specificity of the imaging findings led us to overlook the possibility of tuberculosis lesions in this case and not perform further specific tuberculosis investigations, which further increased the likelihood of a misdiagnosis.
Differential diagnoses include metastatic and primary splenic tumors, lymphoma, splenic abscess, and other con
The cornerstone of treatment for splenic tuberculosis is anti-tuberculosis therapy (ATT), typically for 6-9 months[17], depending on the patient’s response and complications. According to the literature, splenic tuberculosis can often be treated successfully with ATT alone, which reduces spleen size and resolves symptoms without the need for sple
Although rare, splenic tuberculosis should be considered for patients presenting with fever and splenomegaly, especially those with risk factors for tuberculosis or a relevant history. Comprehensive diagnostic evaluation, including imaging and histopathological examination, is crucial for accurate diagnosis. Our case emphasized the need to maintain a high level of suspicion for splenic occupations with an unclear diagnosis, which can also be preceded by a puncture biopsy to clarify the diagnosis if necessary to avoid unnecessary surgical treatment, or surgical treatment can be considered after a detailed evaluation.
| 1. | Chakroun A, Koubaa M, Hammami F, Feki W, Rekik K, Marrakchi C, Mnif Z, Smaoui F, Jemaa MB. Characteristics of Patients Having Splenic Involvement in Tuberculosis. Eur J Med Educ Technol. 2021;14:em2103. [DOI] [Full Text] |
| 2. | Li T, Yan X, Du X, Huang F, Wang N, Ni N, Ren J, Zhao Y, Jia Z. Extrapulmonary tuberculosis in China: a national survey. Int J Infect Dis. 2023;128:69-77. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 63] [Reference Citation Analysis (1)] |
| 3. | Andaloussi S, Annattah S, Eljiar M, Dalero O, Hassani ZA, Elmadi A. Isolated splenic tuberculosis in an immunocompetent child: A case report. Int J Surg Case Rep. 2025;127:110906. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 4. | Gupta A. Splenic tuberculosis: a comprehensive review of literature. Pol Przegl Chir. 2018;90:49-51. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 15] [Article Influence: 1.9] [Reference Citation Analysis (1)] |
| 5. | Kumar S, Pai AG, Tungenwar PN, Bhandarwar AH. Isolated primary tuberculosis of spleen-A rare entity in the immuno-competent patient. Int J Surg Case Rep. 2017;30:93-96. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 12] [Article Influence: 1.2] [Reference Citation Analysis (1)] |
| 6. | Guo HW, Liu XQ, Cheng YL. Solitary splenic tuberculosis: A case report. World J Clin Cases. 2022;10:10260-10265. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 7. | Chege J, Otieno DO, Nyamai N, Muchiri LW, Ndonga A. Isolated splenic tuberculosis mimicking a solid splenic neoplasm in an immunocompetent patient: A surgical case report. Int J Surg Case Rep. 2025;135:111917. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 8. | Sethi J, Shrivastava A, Gupta KL. Fever of unknown origin due to primary tubercular splenic abscess in a low-income/middle-income country. BMJ Case Rep. 2018;2018:bcr2018225990. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 9. | Lestari DA, Rahadiani N, Syaiful RA. Isolated spleen tuberculosis in an immunocompetent patient, a rare case report. Int J Surg Case Rep. 2021;83:105966. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 5] [Article Influence: 1.0] [Reference Citation Analysis (1)] |
| 10. | Matondang SBRE, Wibowo TA, Hilmy IA, Siregar TP, Yonathan IWM. Isolated pancreatic tuberculosis with splenic tuberculosis mimicking lymphoma malignum: A case report. Radiol Case Rep. 2023;18:1775-1778. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 3] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 11. | Gourtsoyianni S, Laniado M, Ros-Mendoza L, Mansueto G, Zamboni GA. The Spectrum of Solitary Benign Splenic Lesions-Imaging Clues for a Noninvasive Diagnosis. Diagnostics (Basel). 2023;13:2120. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 12] [Reference Citation Analysis (1)] |
| 12. | Sahoo S, Naik S, Mishra B, Durgeshwar G, Panigrahi MK, Bhuniya S. Tuberculous splenic abscess in the immunocompetent host: a report and review of literature. Monaldi Arch Chest Dis. 2020;90. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 13. | Jang KM, Kim SH, Hwang J, Lee SJ, Kang TW, Lee MW, Choi D. Differentiation of malignant from benign focal splenic lesions: added value of diffusion-weighted MRI. AJR Am J Roentgenol. 2014;203:803-812. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 30] [Article Influence: 2.5] [Reference Citation Analysis (1)] |
| 14. | Grover S, Arya Y, Gaba S, Gupta M, Syal A. Isolated Splenic Tuberculosis: A Diagnostic Conundrum. Cureus. 2021;13:e12958. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 6] [Reference Citation Analysis (1)] |
| 15. | Ray S, Kundu S, Goswami M, Sarkar D, Saha M. Isolated tubercular splenic abscess: can we defer splenectomy? Our single experience with anti-tuberculous therapy alone. Indian J Med Microbiol. 2012;30:101-103. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 10] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 16. | Singh GR, Sinha A, Anushweta, Sharma R, Saurabh K, Haldar D. Rare Extrapulmonary Tuberculosis: Covert symptoms and Diagnostic Dilemma. Niger Med J. 2024;65:92-100. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |
| 17. | Khan F, Neffati N, Elzouki A. Splenic tuberculosis in immunocompetent patient: A case report and literature review. Libyan J Med Sci. 2018;2:120-122. [DOI] [Full Text] |
| 18. | Ranjan R, Rai A, Gunasekaran J, Paul TR, Gupta RM. A Case of Isolated Splenic Tuberculosis Presenting as a Splenic Abscess Complicated by Rupture Leading to Splenectomy in an Immunocompetent Male. Cureus. 2024;16:e61088. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (1)] |
| 19. | Romboli A, Annicchiarico A, Morini A, Castro Ruiz C, Pagliai L, Montali F, Costi R. Laparoscopic Partial Splenectomy: A Critical Appraisal of an Emerging Technique. A Review of the First 457 Published Cases. J Laparoendosc Adv Surg Tech A. 2021;31:1130-1142. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 11] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 20. | Xing D, Li P, Yang Y, Yao J. Retrospective assessment of the clinical efficacy of laparoscopic partial splenectomy. Exp Ther Med. 2023;25:210. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 8] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 21. | Xiao L, Xia X, Wang T. Extrapulmonary tuberculosis with predominantly hepatic and splenic masquerading as malignancy. Hepatobiliary Surg Nutr. 2024;13:1084-1086. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (1)] |