Published online Apr 27, 2025. doi: 10.4240/wjgs.v17.i4.104443
Revised: January 25, 2025
Accepted: February 24, 2025
Published online: April 27, 2025
Processing time: 91 Days and 23.6 Hours
Acute appendicitis, a common condition with a higher prevalence among men, has shown an increasing incidence in recent years owing to lifestyle changes. It is characterized by right lower quadrant abdominal pain, rebound tenderness, and rapid onset. Its pathogenesis is complex and potentially linked to infection, en
To explore ETX and TLR4 expression in the blood of patients with acute appendicitis and its association with in postoperative incision infection.
A total of 153 patients with acute appendicitis treated at our hospital between April 2022 and March 2024 (n = 153) were included in the study. Patients were categorized into infected (n = 36) and uninfected (n = 117) groups according to the development of postoperative incision infections. General characteristics and blood levels of ETX and TLR4 were compared, and the factors influencing postoperative infection were identified using multivariate logistic regression. ETX and TLR4 predictive values were analyzed using receiver operating characteristic curves.
No statistically significant differences were observed between the two groups in terms of sex, age, or other general characteristics (P > 0.05). Compared to the uninfected group, the infected group had a higher proportion of patients with suppurative or gangrenous appendicitis, longer surgical times, longer incision lengths, and elevated ETX and TLR4 levels (P < 0.05). Multivariate logistic regression analysis identified pathological type, surgical method, surgical time, and incision length as factors influencing postoperative incision infection in acute appendicitis. Receiver operating characteristic curve analysis revealed that both ETX and TLR4 levels were predictive factors for postoperative incision infection, with higher prediction efficiency when combined.
Pathological type, surgical method, surgical time, and incision length significantly influence postoperative incision infection risk in patients with acute appendicitis. Elevated ETX and TLR4 levels serve as valuable predictors of post-appendectomy infections.
Core Tip: Clinical data from patients with acute appendicitis, with and without postoperative incision infections, were compared to analyze factors influencing incision infection. This study explored gram-negative bacteria release endotoxin and toll-like receptor 4 expression in the blood of patients with acute appendicitis, and identified reliable indicators for predicting postoperative incision infections. Pathological type, surgical method, surgical time, and incision length are significant factors influencing the postoperative incision infection risk.
- Citation: Su W, Yang T, Hu XJ, Song J, He JJ, Huang D, Zhang B, Zhao XJ, Tang F. Relationship between peripheral blood endotoxin, toll-like receptor 4 expression, and postoperative infection following surgery for acute appendicitis. World J Gastrointest Surg 2025; 17(4): 104443
- URL: https://www.wjgnet.com/1948-9366/full/v17/i4/104443.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v17.i4.104443
Acute appendicitis is a common condition, ranking as the leading cause of acute abdomen and showing a higher incidence among men[1]. Changes in dietary and lifestyle habits associated with improved living standards have contributed to a rising incidence of acute appendicitis[2]. This condition is primarily characterized by right lower quad
A total of 153 patients with acute appendicitis who underwent surgical treatment at our hospital between April 2022 and March 2024 were selected. Patients were categorized into two groups based on the presence or absence of postoperative incision infections: Infected (n = 36) and the uninfected (n = 117). The inclusion criteria were as follows: (1) Patients who met the diagnostic criteria for acute appendicitis[9]; (2) Patients who successfully underwent appendectomy; (3) Patients without infectious diseases prior to the surgery; and (4) Patients who provided informed consent to participate in the study. The exclusion criteria were as follows: (1) History of other gastrointestinal surgeries within 3 months; (2) Presence of infectious diseases or abnormal coagulation function prior to surgery; (3) Coexisting mental or communication disorders; or (4) Diagnosis of autoimmune diseases. This study was approved by the Medical Ethics Committee of our hospital.
After admission, patients with acute appendicitis were anesthetized, incised, the appendix explored and removed, the root of the appendix treated, the abdominal cavity cleaned, and the incision sutured. Clinical data for all patients, including sex, age, pathological type, and surgical method (acute appendicitis with mild disease and small inflammatory range were treated by laparoscopic surgery, while traditional open surgery was used for acute appendicitis with severe disease, extensive inflammation or other complications), surgical time, incision length, underlying diseases, blood routine, C-reactive protein levels, and ETX and TLR4 levels detected within 24 hours after surgery, were collected. Briefly, 5 mL of fasting venous blood was collected from each patient, placed in an anticoagulant tube, stored at negative 4 °C, and centrifuged at 3000 r/minute for 15 minutes. The resulting supernatant was collected for enzyme linked immunosorbent assay for measurement of the ETX and TLR4 levels. The reagent kit was purchased from Shanghai Ruifan Biotechnology Co., Ltd. and the iMark enzyme linked immunosorbent assay reader was purchased from Bio-Rad (Hercules, CA, United States).
Incision infections were diagnosed based on the “diagnostic criteria for hospital infections (trial)”[10]. The following were assessed: (1) Superficial incision showed redness, burning, or purulent discharge, and bacterial culture showed positive results; (2) Pus appeared following deep incision puncture and drainage; (3) The wound naturally ruptured or was opened by a physician, with purulent discharge or local pain, with a body temperature of ≥ 38 °C; and (4) Further surgical exploration revealed the presence of a deep incision abscess through pathological tissue testing or imaging examination. If any of the above conditions were present, an incision infection was diagnosed.
The results were analyzed using the SPSS20.0 software. Measurement data is expressed as the mean ± SD and subjected to t-test. Quantitative data are represented as n (%), and χ2-tests were performed. Factors influencing postoperative infection were identified using multivariate logistic regression, and the predictive value of the ETX and TLR4 levels in the peripheral blood of patients with postoperative infection was analyzed using receiver operating characteristic (ROC) curves. P < 0.05 indicated a statistically significant difference.
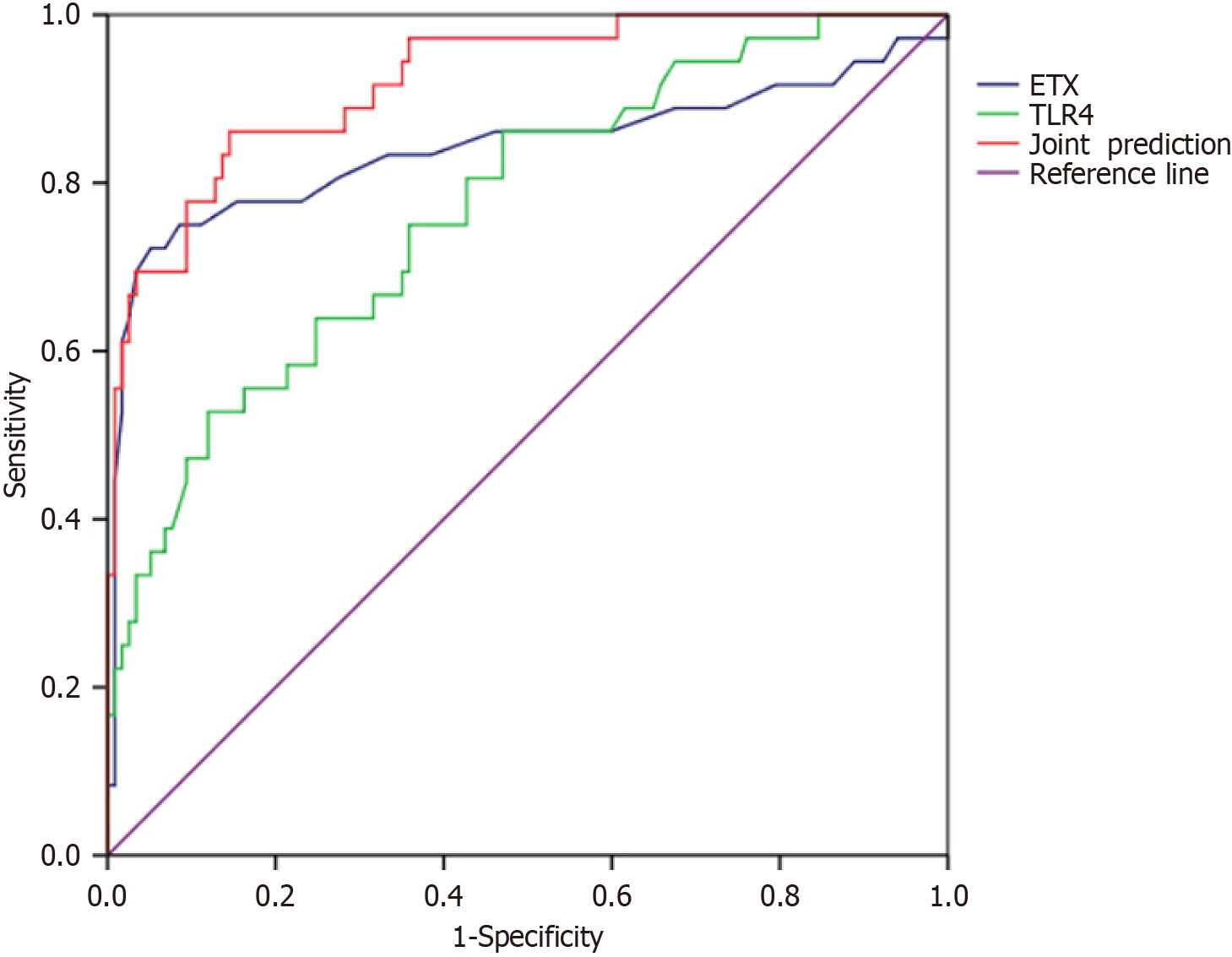
As shown in Table 1, 36 patients who developed postoperative infections were categorized into the infected group, while the remaining patients were assigned to the uninfected group. No statistically significant differences were observed between the two groups in terms of sex, age, or other factors (P > 0.05). Compared with the uninfected group, the infected group had a higher proportion of patients with purulent or gangrenous appendicitis, underwent traditional open surgery, and had longer surgical times and incision lengths (P < 0.05). The non-conditional logistic regression analysis of the risk factors for postoperative incision infection is summarized in Table 2. Using postoperative incision infection as the dependent variable and pathological type (uncomplicated = 0, suppurative or gangrenous = 1), surgical method (laparoscopic surgery = 0, traditional open surgery = 1), surgical time, and incision length as independent variables, multivariate unconditional logistic regression analysis was conducted. The pathological type, surgical method, surgical time, and incision length were factors that influenced postoperative incision infections in acute appendicitis. Laboratory data comparisons are presented in Table 3. The ETX and TLR4 levels in the infected group were found to be higher than in the uninfected group (P < 0.05). ROC curve analysis indicated that the area under the curve for evaluating postoperative incision infections in patients based on ETX and TLR4 levels were 0.841 and 0.769, respectively (Table 4, Figure 1). The area under the curve based on both ETX and TLR4 was 0.922, with a sensitivity and specificity of 86.11% and 85.54%, respectively.
| Index | Infected group (n = 36) | Uninfected group (n = 117) | t/χ2 | P value |
| Sex | 0.224 | 0.636 | ||
| Male | 21 | 63 | ||
| Female | 15 | 54 | ||
| Age, years | 38.36 ± 7.19 | 39.01 ± 6.71 | 0.498 | 0.619 |
| Pathological type1 | 7.136 | 0.008 | ||
| Uncomplicated | 2 | 31 | ||
| Purulent or gangrenous | 34 | 86 | ||
| Operation method1 | 4.366 | 0.037 | ||
| Traditional open surgery | 34 | 93 | ||
| Laparoscopic surgery | 2 | 24 | ||
| Surgery time, minutes2 | 59.96 ± 7.41 | 51.91 ± 6.32 | 6.417 | < 0.001 |
| Incision length, cm1 | 5.36 ± 1.26 | 4.78 ± 0.99 | 2.890 | 0.004 |
| White blood cell count, × 109/L | 8.54 ± 1.03 | 8.35 ± 1.31 | 0.800 | 0.425 |
| Neutrophil count, % | 59.75 ± 10.30 | 56.40 ± 9.72 | 1.783 | 0.077 |
| CRP, mg/L | 18.31 ± 3.14 | 19.41 ± 4.03 | 1.502 | 0.135 |
| Diabetes | 10 | 32 | 0.003 | 0.960 |
| Hypertension | 8 | 27 | 0.011 | 0.915 |
| Factor | B | SE | Exp (B) | Wald | Sig |
| Pathological type | 2.243 | 0.842 | 9.419 (1.809-49.051) | 7.097 | 0.008 |
| Operation method | 1.859 | 0.851 | 6.418 (1.210-34.037) | 4.770 | 0.029 |
| Surgery time | 0.190 | 0.042 | 1.209 (1.114-1.312) | 20.805 | < 0.001 |
| Incision length | 0.470 | 0.232 | 1.601 (1.016-2.521) | 4.117 | 0.042 |
| Constant | -21.780 | 4.041 | - | 29.051 | < 0.001 |
| Group | ETX (EU/mL) | TLR4 (ng/mL) |
| Infected group (n = 36) | 0.36 ± 0.13 | 3.00 ± 0.83 |
| Uninfected group (n = 117) | 0.20 ± 0.06 | 2.17 ± 0.70 |
| T | 10.207 | 5.953 |
| P value | < 0.001 | < 0.001 |
| Index | Cutoff value | AUC | 95%CI | P value | Sensitivity, % | Specificity, % |
| ETX | 0.31 | 0.841 | 0.743-0.939 | < 0.001 | 72.22 | 94.85 |
| TLR4 | 2.94 | 0.769 | 0.679-0.858 | < 0.001 | 52.84 | 88.00 |
| Joint detection | - | 0.922 | 0.873-0.972 | < 0.001 | 86.11 | 85.54 |
Anatomically, the appendix is long and narrow, making the lumen susceptible to fecal and bacterial retention. When the lymphatic tissue of the intestinal wall becomes infected, inflammatory reactions may occur, often resulting in pain. Surgical resection remains the most effective treatment for appendicitis as it alleviates abdominal pain, improves gastrointestinal function, and enhances the patient’s quality of life. With recent advancements in medical technology, laparoscopic surgery has increasingly replaced traditional open surgery due to its benefits, including reduced incision size and pain. However, incision infection occasionally occurs after appendectomy and, in severe cases, a second surgery is required, which increases the physiological and psychological burden on patients.
Appendicitis with suppurative, gangrenous, and peripheral abscesses has a high risk of postoperative infection due to the fact that appendiceal infection is severe and may be accompanied by abdominal infection. The surgical incision associated with this surgery is in the right lower abdomen, where incomplete irrigation may have led to pelvic abscesses and abdominal infections. Patients who are older, malnourished, or have diabetes are prone to postoperative infections owing to low resistance. Additionally, factors such as improper surgical techniques, inadequate disinfection, insufficient incision protection, or suboptimal post-operative care further elevate the risk. The irregular, excessive, or inappropriate use of antibiotics also affects the prevention of infection, and ETX are cell wall components of gram-negative bacteria that are toxic to the host.
In acute appendicitis, bacterial infection causes bacterial death and the release of ETX, which can cause endotoxemia and increase the risk of postoperative infection. ETX cause symptoms, such as fever and microcirculation disturbances, and aggravate postoperative infection. TLR4 is an important immune receptor that recognizes pathogen-associated molecules, including ETX. In acute appendicitis, TLR4 expression is upregulated in response to infection; however, overactivation leads to excessive inflammation, aggravating tissue injury, and postoperative infections. After recognizing ETX, TLR4 triggers the release inflammatory factors such as interleukin-1 and tumor necrosis factor α, which are important in the inflammatory response, but may also aggravate postoperative infection. ETX and TLR4 interact with each other in postoperative infection of acute appendicitis and influence the development of infection together. Among the 153 patients with acute appendicitis enrolled in this study, 36 developed postoperative infections, accounting for 23.53%, similar to the incision infection rate of 22.62% reported in a study by Dong et al[11]. This confirmed that the risk of incision infection after appendectomy was high, and it is necessary to conduct a risk assessment early after surgery and provide corresponding intervention measures to reduce the risk of infection.
The results of this study demonstrated that the infected group had a higher proportion of patients with suppurative or gangrenous appendicitis compared to the uninfected group. This finding highlights the importance of implementing tailored infection prevention and treatment strategies for patients with acute appendicitis based on their pathological presentation. Patients with suppurative or gangrenous appendicitis exhibit a more severe inflammatory response, and the large amount of exudate can lead to cellular adhesion, which increases the risk of abdominal infection and further increases the risk of pathogenic bacteria infecting the incision site[12]. The higher proportion of patients in the infected group who underwent traditional open surgery and the relatively larger surgical incisions observed in this group suggest that open surgery carries a greater risk of incision infections in patients with acute appendicitis. The increased exposure of larger surgical incisions to the surrounding environment may elevate the risk of pathogen exposure. In contrast, laparoscopic surgery, with its smaller incisions, reduces the risk of pathogen exposure and subsequently lowers the incidence of postoperative incision infections[13]. Therefore, when selecting surgical procedures, the patient’s pathological type and individual circumstances should be comprehensively considered. Operative time is another critical factor influencing postoperative incision infections, as prolonged surgical and incision exposure times increase the risk of pathogenic infection.
ETX is a complex of lipopolysaccharides and proteins that are primarily present in the cell walls of gram-negative bacteria. During the proliferation of gram-negative bacteria, the bacterial body undergoes lysis and ETX is released from the cell wall[14]. ETX has a strong stimulatory effect on neutrophils and macrophages in the body, which can lead to an increase in the levels of inflammatory factors, such as interleukin-6 and tumor necrosis factor, and participate in the inflammatory response[15]. TLR4 plays an important role in both acquired and innate immunity, as it can recognize the surface structure of various pathogens and participates in the body’s inflammatory and immune responses[16]. Studies have shown that increased peripheral blood TLR4 expression may indicate a severe inflammatory response. After infection, pathogens can stimulate the synthesis and release of TLR4. Heat shock proteins released after cell necrosis can be recognized by TLR4, causing a cascade reaction that further activates downstream inflammatory cytokines[17]. Other studies have shown that TLR4 can activate signaling pathways, mediate the activation of nuclear transcription factor kappa B, and promote T cell proliferation and synthesis of inflammatory factors, thereby increasing the risk of infection in the body[18]. In the present study, the expression levels of ETX and TLR4 in the peripheral blood of patients in the infected group were significantly higher than those in the uninfected group. This is because infection can lead to the release of a large amount of ETX, which can increase the stress response of cells through contact with mononuclear cells, thereby leading to increased synthesis of TLR4. After recognizing inflammatory signals, TLR4 promotes the expression of downstream inflammatory factors, leading to increased severity[19,20]. ROC curve analysis showed that the expression levels of peripheral blood ETX and TLR4 had a certain predictive value for postoperative incision infection in patients, and the combined predictive value of the two was higher, indicating that the postoperative detection of ETX and TLR4 expression levels in peripheral blood has practical value for predicting postoperative incision infection in patients with acute appendicitis. This study has certain limitations. The small sample size may have introduced statistical bias, limiting the generalizability of the findings to clinical practice. Furthermore, this study did not analyze patients with different pathological types and surgical procedures separately, making it difficult to identify the factors influencing postoperative infections in patients with different pathological types or surgical procedures.
Pathological type, surgical method, surgical time, and incision length are significant factors influencing the occurrence of incision infections following surgery for acute appendicitis. Additionally, peripheral blood ETX and TLR4 expression levels exhibit predictive value for incision infections after appendectomy.
| 1. | Borruel Nacenta S, Ibáñez Sanz L, Sanz Lucas R, Depetris MA, Martínez Chamorro E. Update on acute appendicitis: Typical and untypical findings. Radiologia (Engl Ed). 2023;65 Suppl 1:S81-S91. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 24] [Reference Citation Analysis (2)] |
| 2. | Yang B, Kong L, Ullah S, Zhao L, Liu D, Li D, Shi X, Jia X, Dalal P, Liu B. Endoscopic retrograde appendicitis therapy versus laparoscopic appendectomy for uncomplicated acute appendicitis. Endoscopy. 2022;54:747-754. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 62] [Cited by in RCA: 56] [Article Influence: 14.0] [Reference Citation Analysis (0)] |
| 3. | Xu ZB, Chen DC, Wang YY, Chen WB. [Evaluating the risk of acute complex appendicitis using a column chart model based on clinical and CT features]. Yingxiang Zhenduan Yu Jieru Fangshexue. 2024;33:96-101. [DOI] [Full Text] |
| 4. | Zhan YS, Zhu YR, Zhang SH, Tao Q. [Progress of prediction models related to acute appendicitis]. Zhonghua Putong Waikexue Wenxian (Dianzi Ban). 2023;17:151-154. [DOI] [Full Text] |
| 5. | Liu Y, Wang C, Zhou KJ, Deng L, Zheng L, Pu J. [Analysis of incision infection and treatment in children with acute suppurative appendicitis after operation]. Zhongguo Bingyuan Shengwuxue Zazhi. 2023;18:323-326, 331. [DOI] [Full Text] |
| 6. | Xu GX, Xu L, Zhou SL, Zhao HZ, Wu YM. [Clinical Analysis of Laparoscopic Treatment of 34 Cases of Appendicitis and Surrounding Abscesses in Adults with Purulent and Fecal Stones]. Zhongguo Xiandai Putong Waike Jinzhan. 2023;26:542. [DOI] [Full Text] |
| 7. | Tang X, Fu P, Han L, Zhang L, Chang P, Yu XY, Feng YW, Wang GE. [Endotoxin adsorption therapy in patients with sepsis or infectious shock due to gram-negative bacterial infections in abdominal cavity:a multicenter randomized controlled trial]. Xibu Yixue. 2022;34:729-734. [DOI] [Full Text] |
| 8. | Wang YH, You TH, Wu ZM, Suo D, Huang LQ, Gao LM, Dai MF, Zheng J. [Clinical application of serum procalcitonin and high sensitive C-reactive protein in peritoneal dialysis-associated peritonitis infected by Gram negative bacteria]. Zhongguo Yiyao Daobao. 2024;21:108-113. [DOI] [Full Text] |
| 9. | Zhong LZ, Zhao SD, Qiu WY, Li ZF, Liu GW, Chao JL. [64-slice Spiral CT Signs in the Diagnosis of Acute Appendicitis Pathological Subtype]. Xiandai Yiyong Yingxiangxue. 2024;33:1474-1477. [DOI] [Full Text] |
| 10. | Miao JY, Liu Q, Zhang CH, Zhao XB, Xu WX, Zheng ZY. [Study on Risk Factors for Incision Infection in Emergency Surgery for Acute Appendicitis in Children]. Linchuang Junyi Zazhi. 2021;49:1375-1377, 1382. [DOI] [Full Text] |
| 11. | Dong YW, Yin ZH, Song ZG, Zhang K, Cao GT. [The evaluation value of PCT, ETX, IL-6 for incision infection after appendectomy]. Zhongguo Yishi Zazhi. 2024;26:585-587. [DOI] [Full Text] |
| 12. | An HX, Wang HR. [Clinical observation of laparoscopic appendectomy for acute suppurative appendicitis]. Zhongguo Xiandai Yaowu Yingyong. 2023;17:54-56. [DOI] [Full Text] |
| 13. | Song L, Huang H, Li RJ, Gao L, Wang PG. [Pathogen analysis of postoperative incision infection in patients with acute appendicitis and predictive value of combined detection of NLR, PCT, and CRP]. Xiandai Shengwu Yixue Jinzhan. 2023;23:3359-3364. [DOI] [Full Text] |
| 14. | Zhang HP, He XF, Ren NN. [Diagnostic significance of high-sensitivity C-reactive protein, procalcitonin and endotoxin in infectious diseases]. Zhejiang Yixue. 2024;46:1401-1404. [DOI] [Full Text] |
| 15. | Shen XQ, Yu GL, Zhao Y. [Effect of dexmedetomidine combined with diazosin on postoperative hyperalgesia and gastrointestinal function recovery in patients with acute intestinal obstruction]. Zhuanhua Yixue Zazhi. 2023;12:44-47, 63. [DOI] [Full Text] |
| 16. | Chen SL, Liu R, Liu QS, Hu SY, Zhang Y. [Research progress on mechanism of TLR4 in carcinogenesis of inflammatory bowel disease]. Chin Pharmacological Bull. 2023;39:626-630. [DOI] [Full Text] |
| 17. | Li FF, Yang JY, Han RR, Mu YJ, Gao L, Jing H, Qian LX. [Relationship between Changes in Peripheral Blood TLR4 MyD88 NF-κB and PG Levels and Hp Infection Lesion Progression and Inflammatory Response in Patients with Atrophic Gastritis]. Hebei Yixue. 2023;29:1629-1634. [DOI] [Full Text] |
| 18. | Żukowska A, Ciechanowicz A, Kaczmarczyk M, Brykczyński M, Żukowski M. Toll-like receptor polymorphisms (TLR2 and TLR4) association with the risk of infectious complications in cardiac surgery patients. Adv Clin Exp Med. 2023;32:57-63. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 19. | Zhang S, Chong HF, Jiao RB, Zhou P. [Value of CD64 index combined with IL-1β and TLR4 in the diagnosis of postoperative infection of colorectal cancer]. Linchuang Jianyan Zazhi. 2024;42:177-181. [DOI] [Full Text] |
| 20. | Zamora R, Chavan S, Zanos T, Simmons RL, Billiar TR, Vodovotz Y. Spatiotemporally specific roles of TLR4, TNF, and IL-17A in murine endotoxin-induced inflammation inferred from analysis of dynamic networks. Mol Med. 2021;27:65. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 16] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/