Published online Apr 27, 2025. doi: 10.4240/wjgs.v17.i4.103704
Revised: January 26, 2025
Accepted: February 24, 2025
Published online: April 27, 2025
Processing time: 121 Days and 19.4 Hours
Surgical advancements have transformed colorectal cancer treatment, with complete mesocolic excision (CME) becoming a crucial method to guarantee oncological safety and effectiveness. The article by Yadav emphasized the sig
Core Tip: In this recently published manuscript, Yadav emphasized the complementary role of D3 lymphadenectomy, which enhances lymphatic drainage clearance, aligning with the goal of complete mesocolic excision (CME) to achieve R0 resection. The authors advocated for the global standardization of CME and its integration into surgical training to ensure equitable access and improved outcomes in patients with colon cancer. This underscores the role of CME as a cornerstone of modern oncological surgery, which is essential for achieving excellent colorectal cancer treatment.
- Citation: Bae SU. Central vascular ligation and complete mesocolon excision vs D3 lymphadenectomy: Standardization of surgical technique. World J Gastrointest Surg 2025; 17(4): 103704
- URL: https://www.wjgnet.com/1948-9366/full/v17/i4/103704.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v17.i4.103704
Surgical advancements in the evolving field of colorectal cancer treatment have consistently demonstrated their sig
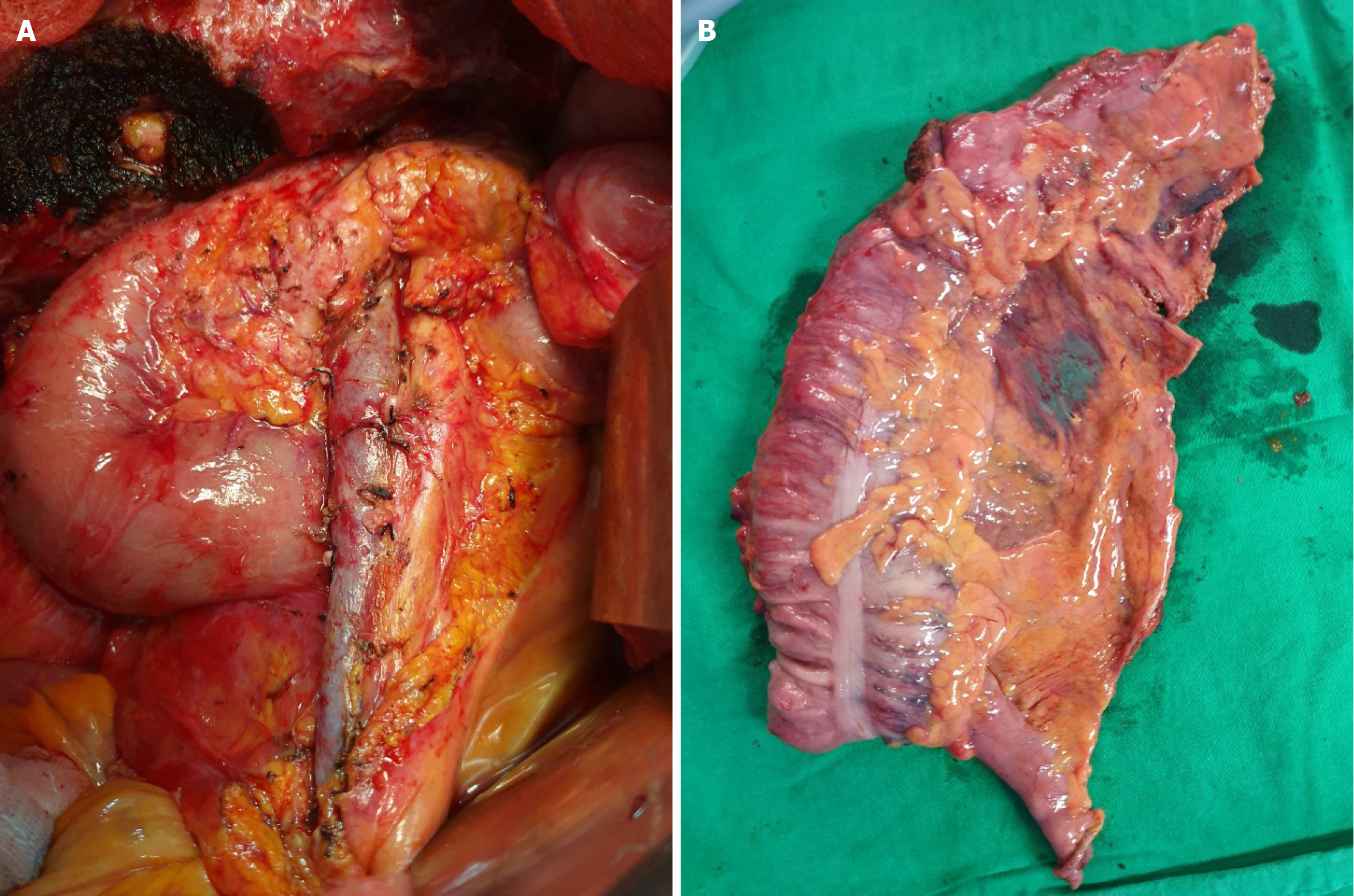
The primary principle of colon cancer surgery is the removal of primary tumors and achievement of adequate surgical margins and locoregional lymph node dissection (Figure 1). CME with central vascular ligation (CVL) has been introduced as a treatment for colonic cancer, based on the concept of complete mesorectal excision for rectal cancer, which has resulted in a higher 5-year survival rate and a reduced recurrence rate[2-4]. Similar to the notion of total mesorectal excision, this technique entails the en bloc resection of the tumor and its surrounding soft tissues by sharply dissecting the visceral plane from the parietal fascia layer, as well as the entire regional mesocolon, as a singular and intact structure[5]. This surgical model offers reduced local recurrence and improved survival rates compared with conventional colectomy[3,6].
Some researchers in the field of surgery have introduced an equivalent lymphadenectomy principle that depends on tumor location and extent and defined the procedure as “modified CME with CVL”[7]. For malignancies that are in the early stages of development, the Japanese Society for Cancer of the Colon and Rectum suggests D2 resection, while D3 resection is recommended for more advanced disease[8]. Regarding the current lack of consensus on the precise boundaries in D2 vs D3 dissection, we acknowledge that this ambiguity arises from variations in surgical guidelines and practices across institutions and regions. As noted in our manuscript, the Japanese Society for Cancer of the Colon and Rectum defines D2 resection as the removal of pericolonic and regional lymph nodes and D3 dissection as the removal of lymph nodes along with the principal feeding vessels. This definition aligns with the broader goals of CME, which emphasize en bloc tumor resection with CME to optimize oncological outcomes. However, the integration of CME with D3 dissection remains under discussion. CME aims to achieve intact mesocolic resection along the embryological plane, ensuring comprehensive lymph node retrieval. In contrast, D3 dissection prioritizes systematic lymphadenectomy along the superior mesenteric vessels. Although these techniques share common oncological principles, their overlap and differentiation require further clarification. Despite the ongoing debate regarding the surgical extent of D3 lymphadenectomy and CME, we are of the opinion that these surgical techniques exhibit comparable oncological safety.
The feasibility and safety of the former have been demonstrated in numerous trials that compare standard laparoscopic and open CME for right-sided colon cancer. These trials have yielded satisfactory oncologic outcomes[9]. However, the execution of minimally invasive CME with CVL for right-sided colon cancer continues to be a difficult task. The feasibility and safety of the laparoscopic method were demonstrated in numerous studies that compared conventional laparoscopic surgery with open CME for right-sided colon cancer, resulting in acceptable oncologic outcomes[10-12]. Nevertheless, the minimally invasive approach to CME and CVL for right-sided colon cancer is difficult due to the complex variable vascular anatomy of the right colon and the technical limitations of laparoscopic instruments. Laparoscopic dissection of the lymph nodes surrounding the superior mesenteric vessels is particularly problematic.
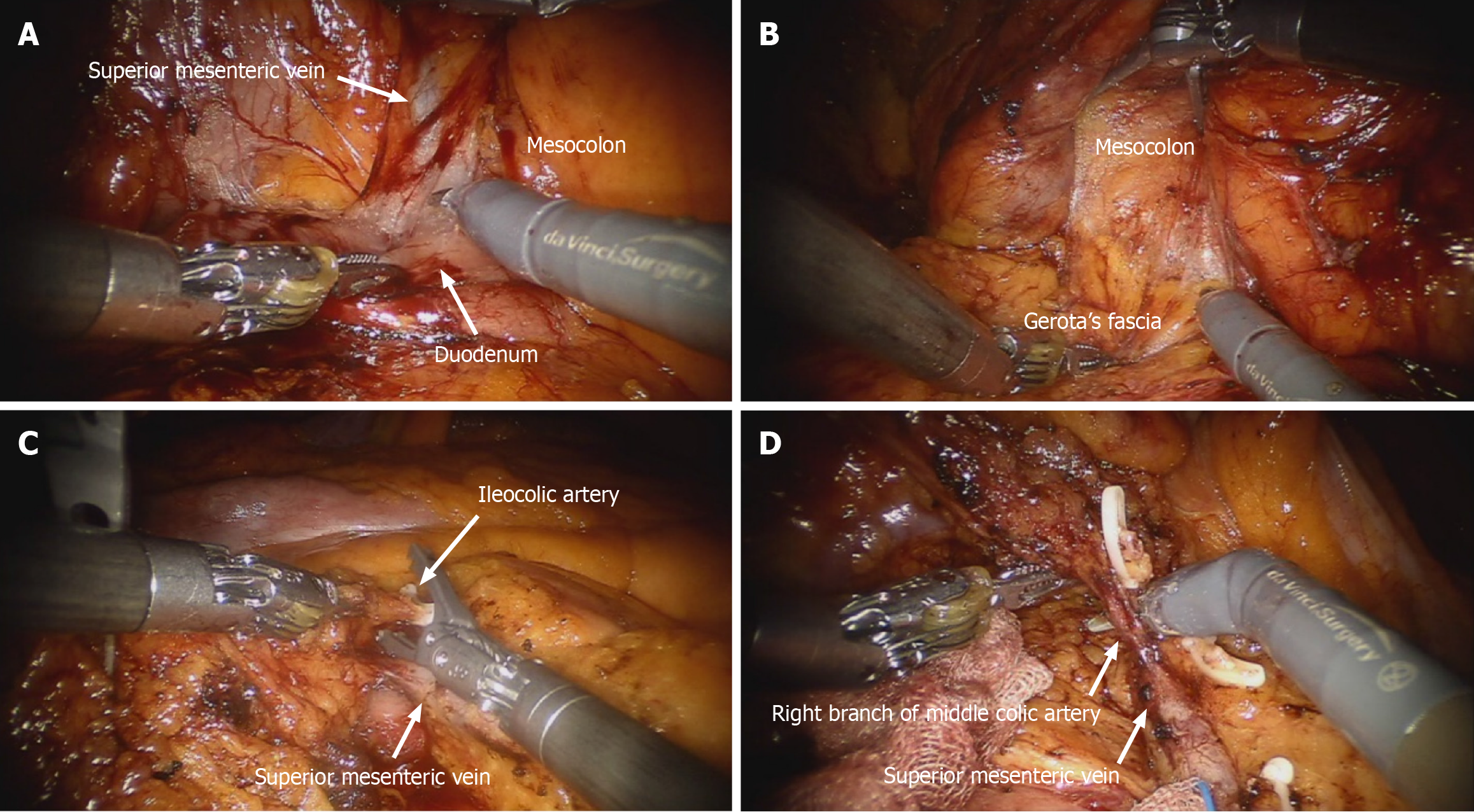
Despite reports comparing the outcomes of laparoscopic CME and CVL, the overall adoption rate of laparoscopic procedures remains low. The intrinsic limitations of laparoscopic surgery were addressed by the development of a surgical robotic system, which was subsequently implemented in the colorectal domain to address the challenges associated with laparoscopic rectal cancer surgery in a constricted pelvic (Figure 2). However, it remains uncertain whether robotic surgery offers substantial clinical advantages over laparoscopic surgery in the treatment of colonic malignancy[13-17]. Robotic colectomy for right-sided colon cancer may provide several advantages. First, it facilitates secure and accurate lymphatic dissection along the superior mesenteric trunk. Second, this method facilitated appropriate mesocolic resection with improved visibility and consistent traction.
Intracorporeal anastomosis was ultimately made feasible and secure by the robotic technique. Nevertheless, there is insufficient evidence to support the claim that robotic CME and CVL outperform laparoscopic surgery in terms of clinical and oncological outcomes. Park et al[18] conducted a randomized clinical trial to compare the clinical and long-term outcomes of robot-assisted and conventional laparoscopic right colectomy with CME and CVL. They found comparable results. Nonetheless, robotic colectomy was linked to extended surgical duration and increased costs, leading to the conclusion that its advantages did not justify the elevated expenditure. The robotic group demonstrated a substantially lower conversion rate, reduced duration of hospital stay, and diminished blood loss, as demonstrated by a recent meta-analysis by Tschann et al[19]. However, the long-term oncological outcomes were similar between the two groups. In their propensity score–matched prospective nonrandomized study, Ferri et al[20] conducted a cost-effectiveness analysis and identified no significant difference in total costs between the robotic and laparoscopic groups. In order to determine the advantages of robot-assisted colon surgery, it is imperative to conduct additional investigations and randomized trials that focus on specific primary endpoints, such as intracorporeal anastomosis, CME with CVL, and cost-effectiveness.
The ongoing refinement of colorectal cancer treatment by the surgical community underscores the importance of CME as a symbol of advancement. Its demonstrated efficacy coupled with its capacity to standardize and enhance outcomes worldwide makes it an essential component of contemporary oncological surgery. Yadav’s work[1] serves as a reminder of the need to adopt evidence-based practices and standardize surgical strategies globally. CME is not simply a surgical procedure; rather, it embodies the pinnacle of contemporary oncological standards. The current challenge involves establishing it as a universal practice, integrating it into surgical education, and making it available to all patients irrespective of location. Overall, the future of colon cancer surgery remains promising.
| 1. | Yadav K. Laparoscopic right radical hemicolectomy: Central vascular ligation and complete mesocolon excision vs D3 lymphadenectomy - How I do it? World J Gastrointest Surg. 2024;16:1521-1526. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (2)] |
| 2. | Benz SR, Feder IS, Vollmer S, Tam Y, Reinacher-Schick A, Denz R, Hohenberger W, Lippert H, Tannapfel A, Stricker I. Complete mesocolic excision for right colonic cancer: prospective multicentre study. Br J Surg. 2022;110:98-105. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 49] [Reference Citation Analysis (0)] |
| 3. | Hohenberger W, Weber K, Matzel K, Papadopoulos T, Merkel S. Standardized surgery for colonic cancer: complete mesocolic excision and central ligation--technical notes and outcome. Colorectal Dis. 2009;11:354-64; discussion 364. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1347] [Cited by in RCA: 1142] [Article Influence: 67.2] [Reference Citation Analysis (0)] |
| 4. | Wibe A, Møller B, Norstein J, Carlsen E, Wiig JN, Heald RJ, Langmark F, Myrvold HE, Søreide O; Norwegian Rectal Cancer Group. A national strategic change in treatment policy for rectal cancer--implementation of total mesorectal excision as routine treatment in Norway. A national audit. Dis Colon Rectum. 2002;45:857-866. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 467] [Cited by in RCA: 425] [Article Influence: 17.7] [Reference Citation Analysis (0)] |
| 5. | Bae SU, Jeong WK, Baek SK. Complete mesocolic excision and central vascular ligation for locally invasive right-sided colon cancer by an open approach-a video vignette. Colorectal Dis. 2021;23:326-327. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 6. | Bertelsen CA, Neuenschwander AU, Jansen JE, Wilhelmsen M, Kirkegaard-Klitbo A, Tenma JR, Bols B, Ingeholm P, Rasmussen LA, Jepsen LV, Iversen ER, Kristensen B, Gögenur I; Danish Colorectal Cancer Group. Disease-free survival after complete mesocolic excision compared with conventional colon cancer surgery: a retrospective, population-based study. Lancet Oncol. 2015;16:161-168. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 301] [Cited by in RCA: 355] [Article Influence: 29.6] [Reference Citation Analysis (2)] |
| 7. | Cho MS, Baek SJ, Hur H, Soh Min B, Baik SH, Kyu Kim N. Modified complete mesocolic excision with central vascular ligation for the treatment of right-sided colon cancer: long-term outcomes and prognostic factors. Ann Surg. 2015;261:708-715. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 62] [Cited by in RCA: 74] [Article Influence: 6.7] [Reference Citation Analysis (0)] |
| 8. | Watanabe T, Itabashi M, Shimada Y, Tanaka S, Ito Y, Ajioka Y, Hamaguchi T, Hyodo I, Igarashi M, Ishida H, Ishiguro M, Kanemitsu Y, Kokudo N, Muro K, Ochiai A, Oguchi M, Ohkura Y, Saito Y, Sakai Y, Ueno H, Yoshino T, Fujimori T, Koinuma N, Morita T, Nishimura G, Sakata Y, Takahashi K, Takiuchi H, Tsuruta O, Yamaguchi T, Yoshida M, Yamaguchi N, Kotake K, Sugihara K; Japanese Society for Cancer of the Colon and Rectum. Japanese Society for Cancer of the Colon and Rectum (JSCCR) guidelines 2010 for the treatment of colorectal cancer. Int J Clin Oncol. 2012;17:1-29. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 606] [Cited by in RCA: 582] [Article Influence: 41.6] [Reference Citation Analysis (4)] |
| 9. | Bae SU, Saklani AP, Lim DR, Kim DW, Hur H, Min BS, Baik SH, Lee KY, Kim NK. Laparoscopic-assisted versus open complete mesocolic excision and central vascular ligation for right-sided colon cancer. Ann Surg Oncol. 2014;21:2288-2294. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 93] [Cited by in RCA: 98] [Article Influence: 8.2] [Reference Citation Analysis (0)] |
| 10. | Shin JK, Kim HC, Lee WY, Yun SH, Cho YB, Huh JW, Park YA, Chun HK. Laparoscopic modified mesocolic excision with central vascular ligation in right-sided colon cancer shows better short- and long-term outcomes compared with the open approach in propensity score analysis. Surg Endosc. 2018;32:2721-2731. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 26] [Cited by in RCA: 39] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 11. | Bae SU, Kim CN. Laparoscopic Complete Mesocolic Excision and Central Vascular Ligation for Right-sided Colon Cancer Using the Retroperitoneal Approach. Dis Colon Rectum. 2015;58:816. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 8] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 12. | Bae SU, Jeong WK, Baek SK. Reduced-port laparoscopic complete mesocolic excision and intracorporeal anastomosis for right-sided colon cancer - a video vignette. Colorectal Dis. 2020;22:1768-1769. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 2] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 13. | Park JS, Choi GS, Park SY, Kim HJ, Ryuk JP. Randomized clinical trial of robot-assisted versus standard laparoscopic right colectomy. Br J Surg. 2012;99:1219-1226. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 252] [Cited by in RCA: 287] [Article Influence: 20.5] [Reference Citation Analysis (3)] |
| 14. | Tyler JA, Fox JP, Desai MM, Perry WB, Glasgow SC. Outcomes and costs associated with robotic colectomy in the minimally invasive era. Dis Colon Rectum. 2013;56:458-466. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 76] [Cited by in RCA: 73] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 15. | Baek SK, Carmichael JC, Pigazzi A. Robotic surgery: colon and rectum. Cancer J. 2013;19:140-146. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 93] [Cited by in RCA: 82] [Article Influence: 6.3] [Reference Citation Analysis (0)] |
| 16. | Bae SU, Jeong WK, Baek SK. Intra-operative near-infrared fluorescence imaging for robotic complete mesocolic excision and central vascular ligation in right-sided colon cancer - a video vignette. Colorectal Dis. 2019;21:1459. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 17. | Bae SU, Yang SY, Min BS. Totally robotic modified complete mesocolic excision and central vascular ligation for right-sided colon cancer: technical feasibility and mid-term oncologic outcomes. Int J Colorectal Dis. 2019;34:471-479. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 19] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 18. | Park JS, Kang H, Park SY, Kim HJ, Woo IT, Park IK, Choi GS. Long-term oncologic after robotic versus laparoscopic right colectomy: a prospective randomized study. Surg Endosc. 2019;33:2975-2981. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 39] [Cited by in RCA: 91] [Article Influence: 11.4] [Reference Citation Analysis (0)] |
| 19. | Tschann P, Szeverinski P, Weigl MP, Rauch S, Lechner D, Adler S, Girotti PNC, Clemens P, Tschann V, Presl J, Schredl P, Mittermair C, Jäger T, Emmanuel K, Königsrainer I. Short- and Long-Term Outcome of Laparoscopic- versus Robotic-Assisted Right Colectomy: A Systematic Review and Meta-Analysis. J Clin Med. 2022;11:2387. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 26] [Cited by in RCA: 44] [Article Influence: 11.0] [Reference Citation Analysis (5)] |
| 20. | Ferri V, Quijano Y, Nuñez J, Caruso R, Duran H, Diaz E, Fabra I, Malave L, Isernia R, d'Ovidio A, Agresott R, Gomez P, Isojo R, Vicente E. Robotic-assisted right colectomy versus laparoscopic approach: case-matched study and cost-effectiveness analysis. J Robot Surg. 2021;15:115-123. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 30] [Article Influence: 5.0] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/