Published online Apr 27, 2025. doi: 10.4240/wjgs.v17.i4.102934
Revised: January 7, 2025
Accepted: February 8, 2025
Published online: April 27, 2025
Processing time: 138 Days and 16.7 Hours
Heart rate variability (HRV) represents efferent vagus nerve activity, which is suggested to be related to fundamental mechanisms of tumorigenesis and to be a predictor of prognosis in various cancers. Therefore, this study hypothesized that HRV monitoring could predict perioperative complication (PC) in colorectal cancer (CRC) patients.
To investigate the prognostic value of HRV in hospitalized CRC patients.
The observational studies included 87 patients who underwent CRC surgical procedures under enhanced recovery after surgery programs in a first-class hos
The complication rate was 14.9%. HRV was markedly abnormal after surgery, especially in the PC group. The frequency-domain parameters (including pNN50) and time-domain parameters [including high-frequency (HF)] of HRV were significantly different between the two groups postoperatively. The pNN50 was significantly greater at Pod1 in the PC group than that in the NPC group and returned to baseline at Pod2, suggesting that patients with complications exhibited autonomic nerve dysfunction in the early postoperative period. In the PC group, HFs were also enhanced from Pod1 and were significantly higher than in the NPC group; inflammatory biomarkers were significantly elevated at Pod2 and Pod3; the levels of nutritional indicators were significantly lower at Pod1 and Pod2; and the white blood cell count was slightly elevated at Pod3.
HRV is independently associated with postoperative complications in patients with CRC. Abnormal HRV could predicted an increased risk of postoperative complications in CRC patients. Continuous HRV could be used to monitor complications in patients with CRC during the perioperative period.
Core Tip: In this study, heart rate variability (HRV) was compared among 87 patients who underwent colorectal cancer (CRC) resection. Abnormal HRV predicted a greater risk of postoperative complications in CRC patients. Continuous HRV could be used to monitor complications in patients with CRC during the perioperative period.
- Citation: Ge MM, Wang LW, Wang J, Liu J, Chen P, Liu XX, Wang G, Gong GW, Jiang ZW. Prediction of perioperative complications in colorectal cancer via artificial intelligence analysis of heart rate variability. World J Gastrointest Surg 2025; 17(4): 102934
- URL: https://www.wjgnet.com/1948-9366/full/v17/i4/102934.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v17.i4.102934
Colorectal cancer (CRC) is the second most prevalent cancer in the world, with case of 1.4 million and death of 693900 annually[1]. The only way to cure this disease is surgical excision. Nevertheless, postoperative complications not only directly exacerbate the patient's condition but also hinder or defer subsequent treatment. For example, they may cause the adjuvant chemotherapy to be postponed, thus influencing the long - term prognosis of oncology patients. In addition, postoperative complications occur in up to 50% of patients and are related to higher morbidity and mortality rates, gr
HRV, defined as the variability between heartbeats, can be a noninvasive and standardized method to evaluate the prognosis of several diseases and ANS function[10,11]. HRV reflects complex coactions of the ANS, including vagus nerve, the sympathetic nervous system (SNS) and parasympathetic nervous system (PNS)[12]. SNS activities advance the heart rate, whereas the PNS reduce it[10,13]. In addition to autonomic balance, HRV can also reflect the regulation of blood pressure (BP), breathing, the intestine, the heart, and angiotasis[14,15]. High HRV indices generally indicate ef
It has reported that patients with low HRV before surgery have a higher occurrence of postoperative complications[19]. However, few studies have evaluated perioperative complication (PC) and autonomic nerve dysfunction in patients with CRC via HRV. Our previous study revealed that, compared with current clinical indicators, perioperative HRV is more sensitive in detecting the stress and ANS dysfunction induced by radical gastrectomy in gastric cancer patients[20]. However, whether HRV could predict PC needs to be explored. Therefore, our study was designed primarily to explore fluctuations in the HRV through a noninvasive smart device that can continuously monitor HRV, further predict fluctuations in HRV, and analyze the role of HRV in monitoring PC in CRC patients.
An observational study was conducted with patients with CRC from a first-class hospital. 87 patients who underwent CRC resection between December 2021 and December 2022 were enrolled consecutively. This study complies with the Declaration of Helsinki, written informed consent was given by all the subjects, and the study was approved by the local ethics committee. As reported in our previous study, patients were managed perioperatively via ERAS programs for colorectal resection in our department, including preoperative carbohydrate loading, multimode health education, no intestinal preparation for nonconstipated patients, laparoscopic surgery, early initiation of postoperative nutrition, shortened preoperative fasting time and oral carbohydrate administration, patient temperature maintenance, post
Medical diagnostic criteria for CRC: Colonoscopy is the universally applied gold standard for CRC screening, i.e., pre
The exclusion criteria were as follows: (1) Combined with breast or other endocrine or metabolic diseases; (2) The combination of coronary heart disease, atrial fibrillation, or heart, lung, liver, kidney, or other important organ failure; (3) Preoperative intestinal perforation, intestinal obstruction, intestinal necrosis, etc., or emergency surgery; (4) Inability to give full informed consent due to intellectual or behavioral disabilities; and (5) Other pathologies that, in the judgment of the researcher, would reduce the likelihood of following through with enrollment or complicate the enrollment process, such as frequent changes in the work environment and other conditions that may lead to loss of visits.
Patients were managed perioperatively via ERAS programs for colorectal resection in our department, including preoperative and postoperative nutritional support, multimodal health education, no intestinal preparation for nonconstipated patients, shortened preoperative fasting time and oral carbohydrate administration, patient temperature maintenance, limited fluid resuscitation, postoperative pain assessment and multimodal analgesia, early mobilization, and early oral feeding.
Subjects who provided informed consent and were screened and qualified for enrollment but did not complete the course of treatment and observation period specified in the protocol for any reason or whose HRV data were discontinuous and had artifacts were regarded as dropout cases.
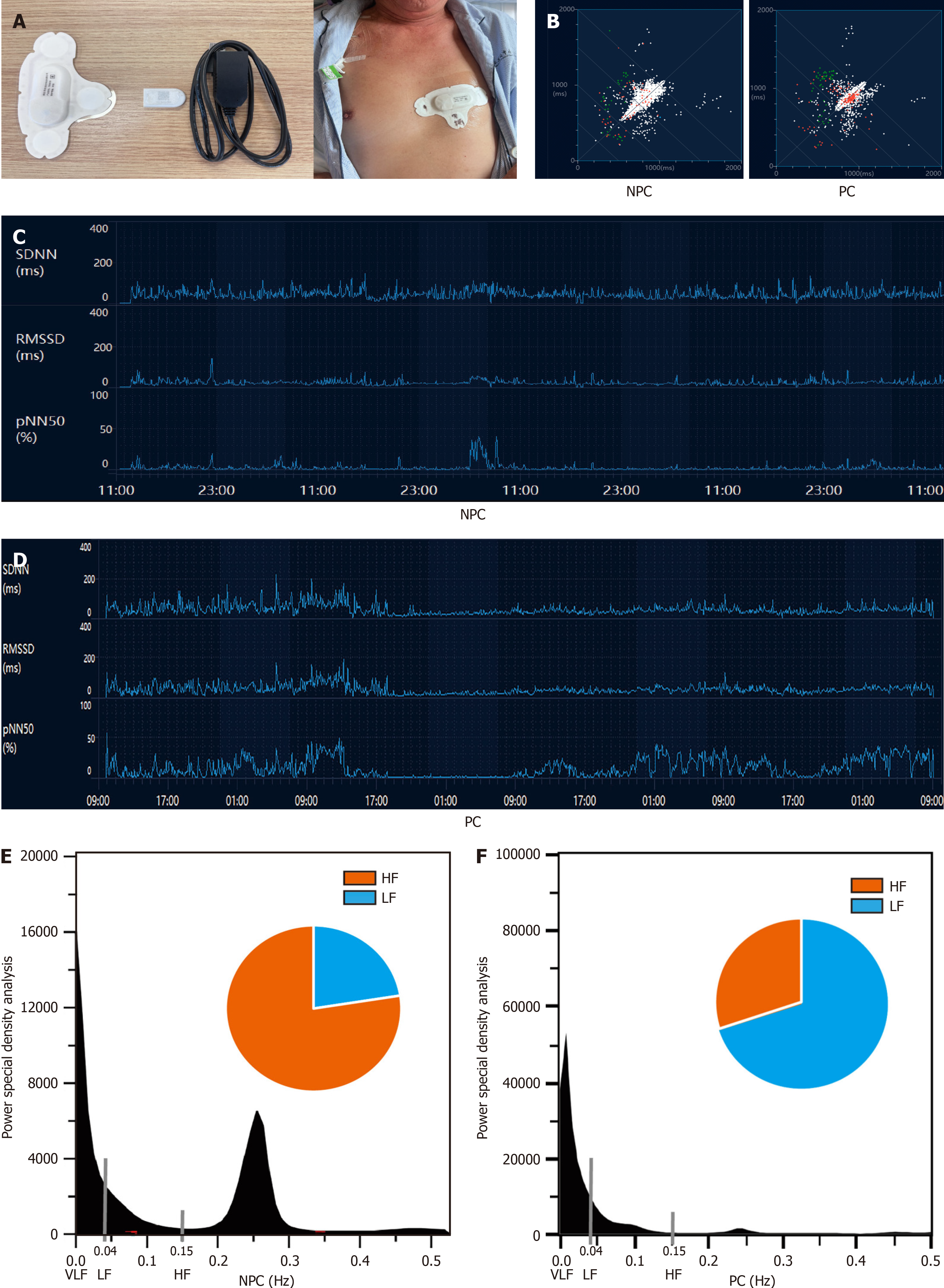
A smart device (Transcendent THoughts On Health, THOTH, http://www.thoth-health.com/, Suzhou, China) was used for HRV monitoring. After the patients were admitted to the hospital, the researchers cleaned the skin of the precardiac area with wet gauze, attached the registered smart device to the skin in the shape of a T (Figure 1A), and uploaded the full-course heart rate to the monitoring system through the wireless transmission device. We analyzed the HRV in both the time and frequency domains and collected data from 24 hours before the operation to 3 days after the operation. After the data collection, Holter System software was used for statistical analysis (Figure 1C-F).
In addition to HRV, the collected variables included sex, age, BMI, underlying illnesses, surgical excision site, American Society of Anesthesiology (ASA) score, stage of cancer, etc. The study was approved by the Ethics Committee of the Affiliated Hospital of Nanjing University of Traditional Chinese Medicine (Ethics Approval No. 2022NL-210-02) and complied with the principles of the Declaration of Helsinki.
HRV measurement methods include Poincaré plots (Figure 1B), R–R interval histograms, time-domain analysis (power spectral density plot), and frequency-domain analysis (Figure 1C-F), among which time-domain and frequency-domain analysis methods are most widely used in clinical practice. The analyzed time-domain parameters included the standard deviation of N-N intervals (SDNN), the square root of the mean of the squared differences between adjacent normal RR intervals (RMSSD), and the percentage of NN50 count (number of consecutive RR intervals differing by > 50 ms in the entire recording) divided by the total number of all NN intervals (pNN50), which are based on the time difference. HRV frequencies can be summarized into three leading frequency bands: The very-low-frequency band, low-frequency (LF) band, and high-frequency band (HF). In addition, the ratio of LF power to HF power (LF/HF) reflects the balance between the SNS and PNS. All of these are frequency-domain parameters. In this study, one datum is obtained every day in the time-domain analysis, and each data point is the statistical result of all the obtained data on that day. In frequency-domain analysis, one data point is obtained in one day, which is a statistical result of monitored data on that day.
All the data were analyzed statistically using SPSS 19.0. The HRV data are shown as the mean ± SEM. All the data were tested for a normal distribution via the Shapiro-Wilk test. Nonnormally distributed data were described via the median (IQR) method. The longitudinal data were analyzed by paired-samples t test. The χ2 test was used to compare categorical variables. Spearman's rank correlation coefficient was also used to evaluate the correlation between postoperative complications and HRV parameters or inflammatory indicators. Significance was defined as P ≤ 0.05.
In this study, 87 patients who underwent CRC resection between December 2021 and December 2022 were enrolled consecutively; 13 patients were recorded as having PCs, and 74 patients had non-PC (NPCs). Table 1 outlines the patient characteristics. Comparisons of patients in the PC group vs. controls revealed no significant differences in age or sex distribution. Sex, BMI, ASA grade, surgical modality, underlying illness and disease stage were not significantly different between the two groups. The complications that occurred in 13 patients (14.9%), included anastomotic fistula, pulmonary complications, incisionostomy infection and urine retention.
| Parameters | Perioperative complications | Non-perioperative complications | P value |
| Gender | |||
| Male | 8 (14.5) | 47 (85.5) | 0.892 |
| Female | 5 (15.6) | 27 (84.4) | |
| Age | 61.85 ± 13.48 | 61.24 ± 10.70 | 0.857 |
| BMI | 22.54 ± 1.48 | 24.33 ± 3.20 | 0.052 |
| Underlying illnesses | |||
| Heart disease | 1 (6.8) | 5 (7.7) | 0.444 |
| Hypertension | 2 (40.5) | 30 (15.4) | |
| Diabetes | 1 (7.7) | 12 (16.2) | |
| Lung disease | 0 (0) | 1 (1.4) | |
| Nervous system disease | 0 (0) | 1 (1.4) | |
| Preoperative levels | |||
| White blood cell (109/L) | 6.35 ± 1.97 | 5.52 ± 1.75 | 0.130 |
| Albumin (g/L) | 39.35 ± 3.32 | 37.53 ± 4.62 | 0.329 |
| Hb (g/L) | 125.54 ± 19.54 | 122.55 ± 23.60 | 0.668 |
| Surgical excision sites | |||
| TME | 5 (41.7) | 27 (36.5) | 0.56 |
| Anterior resection | 4 (33.3) | 15 (20.3) | |
| Sigmoidectomy | 0 (0) | 6 (8.1) | |
| Left hemicolectomy | 1 (8.3) | 3 (4.1) | |
| Right hemicolectomy | 2 (16.7) | 23 (31.1) | |
| ASA Score | |||
| 1 | 3 (23.1) | 18 (24.3) | 0.936 |
| 2 | 7 (53.8) | 36 (48.6) | |
| 3 | 3 (23.1) | 20 (27.0) | |
| Stage of cancer | |||
| 0 | 0 | 1 (1.5%) | 0.719 |
| I | 2 (15.4) | 14 (20.6) | |
| II | 4 (30.8) | 29 (42.6) | |
| III | 7 (53.8) | 23 (33.8) | |
| IV | 0(0) | 1 (1.5) |
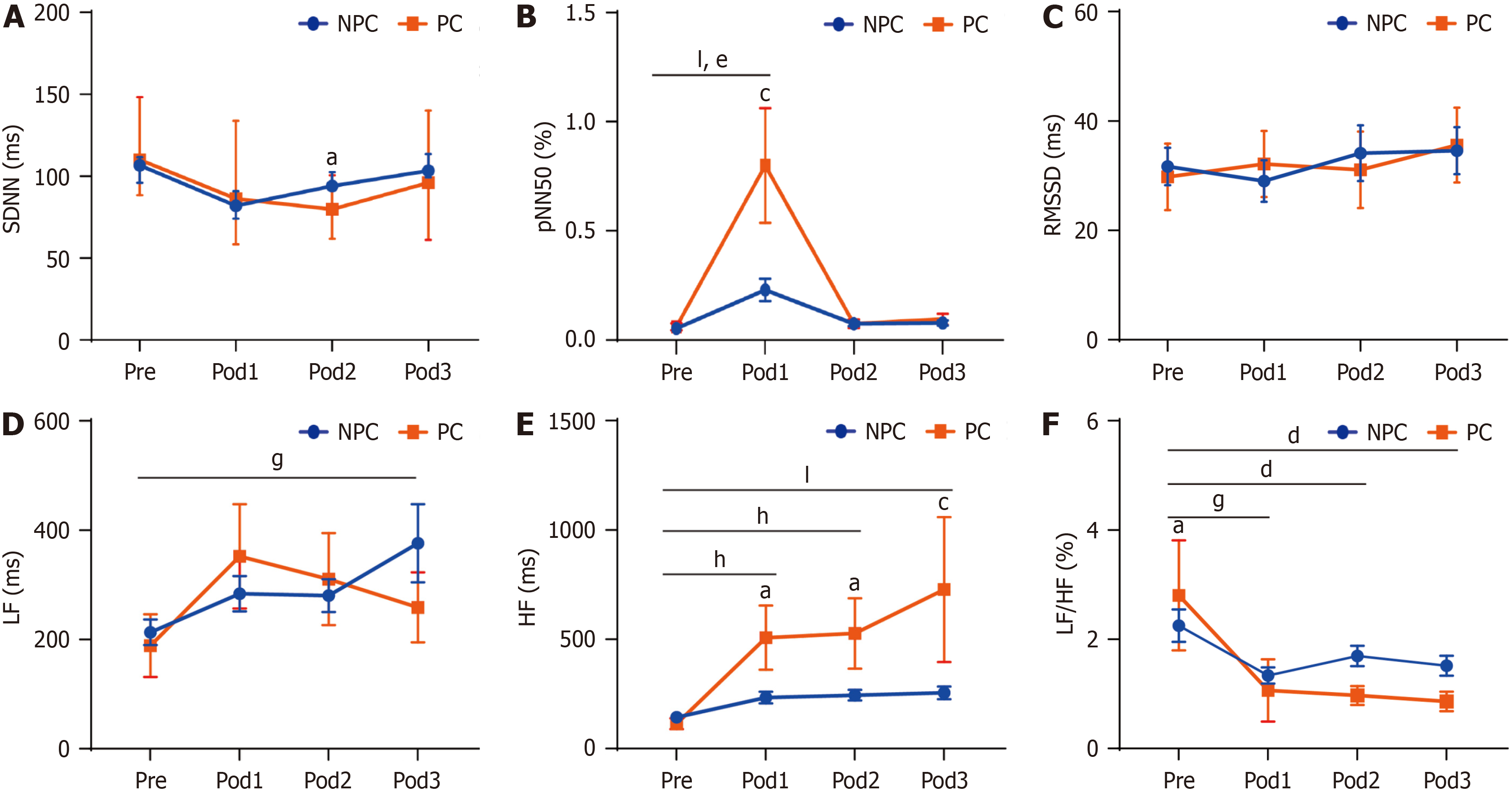
All the perioperative HRV parameters, recovered to preoperative levels throughout the day at postoperative day 3 (Pod3) (Figure 1), although a certain degree of difference existed. The SDNN significantly differed between the two groups at Pod2 (P < 0.01) (Figure 2A). pNN50 was increased at Pod1, especially pNN50, which was significantly elevated at Pod1 in the PC group (Figure 2B). Interestingly, pNN50 was significantly increased at Pod1 and recovered to preoperative levels at Pod2. Compared with the NPC group, pNN50 was not significantly different at Pod2 and Pod3, indicating that pNN50 at Pod1 may be a predictor of complications. In addition, the RMSSD differed somewhat between the two groups, but the difference was not statistically significant (Figure 2C).
In our study, we found that LF parameters were not statistically different between the PC and NPC groups (Figure 2D). HF increased from Pod1 in the PC group, and LF/HF decreased to different degrees after surgery in the two groups (Figure 2E and F). Fascinatingly, the parameter of HFs in the PC group was markedly greater than that in the NPC group, and the HF indices increased in a time-dependent manner in the PC group (Figure 2E). Moreover, in the PC group, the LF/HF ratio was higher preoperatively; however, the LF/HF ratio decreased at Pod1 in the NPC group, and the ratio increased began to Pod2 (Figure 2F). These results indicated that HRV may be a predictor of complications, especially pNN50 and HF.
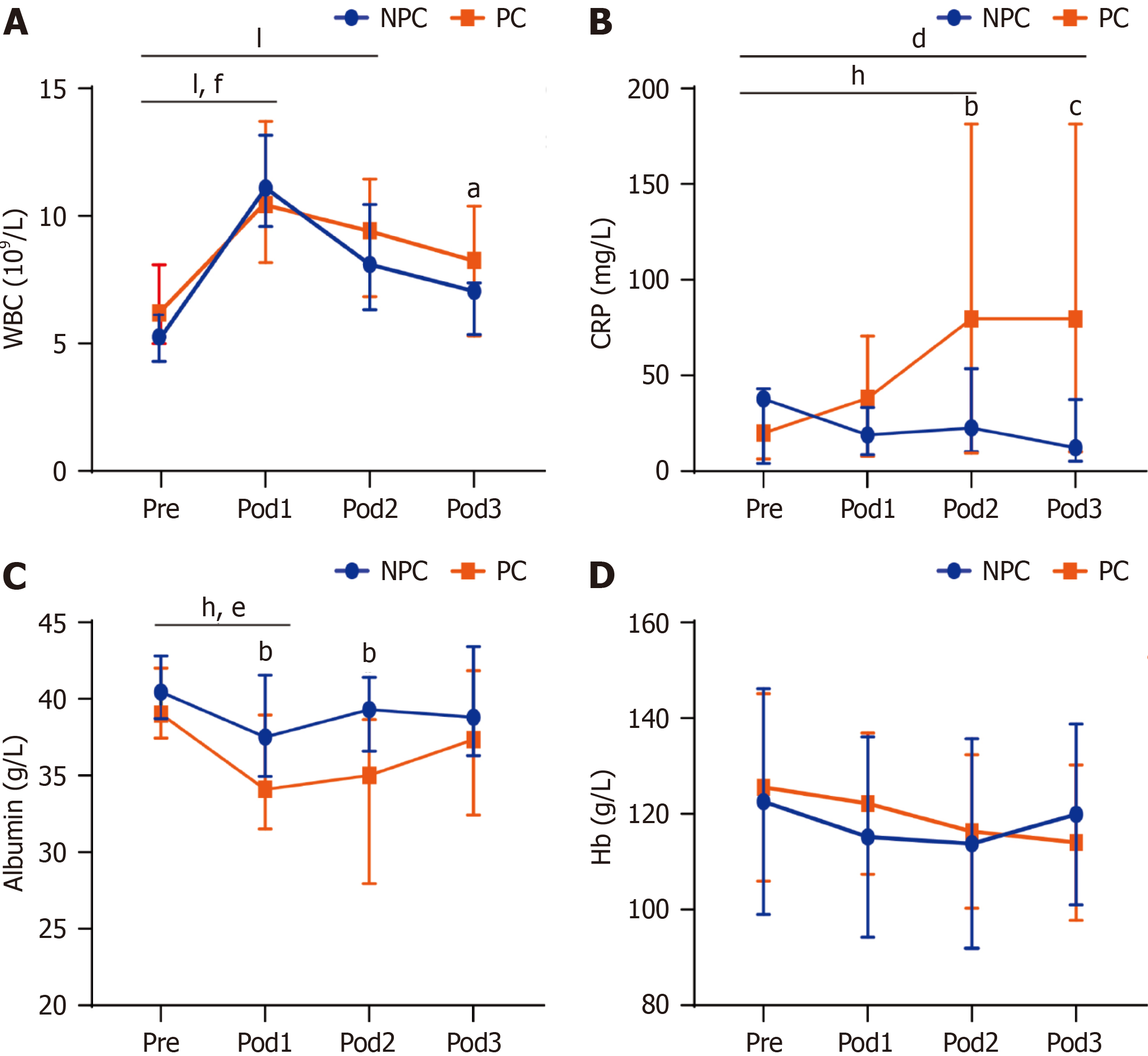
Inflammatory markers were identified as sensitive markers for the early detection of complications (Figure 3 and Table 2). Compared with those before surgery, the inflammatory markers white blood cell (WBC) and C-reactive protein (CRP) increased significantly at different times after surgery. We found that the WBC count was significantly greater at Pod1 compared with Pre, indicating a markedly augmented inflammatory reaction at Pod1 (Figure 3A). However, there were no significant differences between the two groups except at Pod3. In addition, the CRP level increased after surgery in the PC group and significantly decreased at Pod2. Moreover, the level of CRP in the PC group was statistically greater at Pod2 and Pod3, comparing to that in the NPC group, which suggested that abnormally elevated CRP at Pod2 and Pod3 may be a predictor of complications (Figure 3B). Furthermore, albumin in the NPC group was higher than that in the PC group, especially at Pod1 and Pod2 (P < 0.01) (Figure 3C). These results indicated that the serum albumin level may be a risk factor for postoperative complications. However, Hb showed no statistical difference between the two groups (Figure 3D). All of these results suggested that abnormal inflammatory markers (CRP and albumin) were present in the PC group, indicating that abnormal inflammatory markers may be predictors of complications.
| Parameters | Perioperative complications | Non-perioperative complications | P value | |
| Pre | WBC (109/L) | 6.35 ± 1.97 | 5.52 ± 1.75 | 0.130 |
| CRP (mg/L) | 1.97 ± 2.25 | 5.84 ± 11.91 | 0.291 | |
| Albumin (g/L) | 39.35 ± 3.32 | 37.53 ± 4.62 | 0.329 | |
| Hb (g/L) | 125.54 ± 19.54 | 122.55 ± 23.60 | 0.668 | |
| Pod1 | WBC (109/L) | 10.87 ± 3.20 | 11.45 ± 3.61 | 0.589 |
| CRP (mg/L) | 46.37 ± 80.47 | 25.48 ± 27.46 | 0.088 | |
| Albumin (g/L) | 32.09 ± 10.53 | 37.53 ± 4.62 | 0.003b | |
| Hb (g/L) | 122.15 ± 14.77 | 115.17 ± 20.96 | 0.253 | |
| Pod2 | WBC (109/L) | 9.20 ± 2.75 | 8.38 ± 2.86 | 0.338 |
| CRP (mg/L) | 73.66 ± 81.07 | 36.56 ± 41.77 | 0.017b | |
| Albumin (g/L) | 33.97 ± 7.52 | 39.27 ± 4.23 | 0.001c | |
| Hb (g/L) | 116.31 ± 16.04 | 113.78 ± 21.90 | 0.692 | |
| Pod3 | WBC (109/L) | 8.31 ± 3.04 | 6.76 ± 2.01 | 0.037a |
| CRP (mg/L) | 89.50 ± 86.65 | 16.35 ± 16.04 | < 0.001c | |
| Albumin (g/L) | 37.15 ± 6.31 | 38.97 ± 6.96 | 0.414 | |
| Hb (g/L) | 114.00 ± 16.20 | 119.87 ± 18.90 | 0.328 | |
Furthermore, we analyzed the correlations between postoperative complications and HRV and inflammatory markers. We found that changes in HRV parameters (including pNN50 at Pod1 and HF at Pod3) and inflammatory biomarkers (including albumin levels at Pod1 and Pod2, CRP at Pod2 and Pod3, and WBC at Pod3) were correlated with post
HRV represents vagus nerve activity, is inversely correlated with the underlying mechanisms of tumorigenesis, and has been shown to have predictive value in the prognosis of several cancers[5]. The relationship between HRV and complications in patients with CRC after surgery has not been reported. In previous studies, the HRV parameters were based on a 10-s ECG rather than long-range monitoring. In our study, we used continuous and longer-range monitoring to observe the HRV of patients with CRC perioperatively in real time. This study investigated whether continuous, long-range monitoring to observe HRV could predict postoperative complications in patients with CRC. Analysis of the HRV data of the patients with CRC enrolled in our study revealed that pNN50 and HF can be highly interrelated with PC, especially those measured at Pod1. However, the laboratory test indicator CRP significantly differed beginning on the Pod2. The results showed that the pNN50 and HF can be considered fairer indicators for predicting PC in patients with CRC.
Surgical operations are thought to elicit complex physiological stress responses that involve the activation of endocrine, metabolic, immunological mediators and inflammatory which are the main causes of mortality[21]. Postoperative complications are risk factors for mortality in CRC patients and are often accompanied by severe stress responses[22]. Although we use the EARS program in the perioperative period to reduce stress[20], postoperative complications cannot be avoided. The usual methods for monitoring postoperative complications are dependent on laboratory test indicators, such as serum cortisol, CRP, WBC, and corresponding scales[23]. Recently, HRV has been used to detect autonomic function, inflammation status, and stress and has been used to prevent and monitor several diseases. Among these metrics, pNN50 is closely correlated with PNS activity, especially continuous pNN50. In our study, the time-domain parameter pNN50 revealed that the patients in the PC group had significantly greater vagus nerve activity at Pod1, suggesting more active parasympathetic nerve at Pod1 in the PC group. Both SNS and PNS activity contribute to the SDNN; the SDNN indicates total HRV, and a higher SDNN reflects greater health and physiological resilience[15,24]. Our study revealed that the peak SDNN was greater in the NPC group at Pod2, suggesting that a higher SDNN at Pod2 predicts good short-term outcomes. HF is a well-known that HRV indices can imply the functional relevance of vagal and parasympathetic activity, especially during stress[24]. The HF in the PC group was statistically increased than that in the NPC group from Pod1, and it exhibited greater vagal activity indexed by the HF power of HRV in the PC group. These results indicated that higher vagal activity at Pod1 may predict an increased risk of complications.
In addition, the WBC count was significantly greater on Pod3 in the PC group than in the NPC group. CRP levels were significantly increased from the first day after surgery in the PC group (although some differences were not statistically significant), indicating that a higher CRP level can be used to predict the risk of postoperative complications. The Toon Health Study, which examined 1728 nonsmoking individuals aged 30-79 years from 2009 to 2012, expressed that HRV is highly relevant to an elevation in CRP[25]. However, our study revealed that abnormal pNN50 and HF test results appeared earlier than abnormal WBC and CRP test result did. These results are consistent with the theory of the ANS via an inflammatory reaction of the vagus nerve (the major nerve of the PNS), which is responsible for a quick reflexive response to inflammation[26]. This study showed that models using HRV as a parameter (including pNN50 and HF) were more sensitive than those using inflammatory markers for confirming postoperative complications. These results indicated that HRV was a more accurate indicator of postoperative complications in surgical patients than inflammatory markers. In addition, our team has routinely conducted the perioperative HRV monitoring in patients who have un
There are several limitations to the present study. First, our use of minimally invasive surgery (including Da Vinci robotic surgery and 3D laparoscopic), which minimizes the postoperative complication rate[27], resulted in a relatively small number of participants in the study. Second, we did not analyze the correlation of different complications with HRV due to the small number of samples. Third, factors such as patients' preoperative health status, medication regi
In conclusion, our study indicated that continuous and long-term monitoring of the perioperative HRV of CRC patients may be valuable for predicting postoperative complications. Abnormal HRV occurs earlier than abnormal inflammatory markers. In addition, our study indicated that HRV could objectively reflect the change of autonomic nerve function perioperatively in patients with CRC and might be a worthy way for predicting PC and guiding clinical application in the context of precision medicine and artificial intelligence medicine. However, it would be meaningful to design larger, multicenter trials and investigate the predictive value of HRV in the context of other types of oncological surgeries.
We are grateful to all the participants for their assistance with the experiments.
| 1. | Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J Clin. 2021;71:209-249. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 76817] [Cited by in RCA: 69227] [Article Influence: 13845.4] [Reference Citation Analysis (18)] |
| 2. | Kirchhoff P, Clavien PA, Hahnloser D. Complications in colorectal surgery: risk factors and preventive strategies. Patient Saf Surg. 2010;4:5. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 342] [Cited by in RCA: 291] [Article Influence: 18.2] [Reference Citation Analysis (0)] |
| 3. | Govaert JA, Fiocco M, van Dijk WA, Scheffer AC, de Graaf EJ, Tollenaar RA, Wouters MW; Dutch Value Based Healthcare Study Group. Costs of complications after colorectal cancer surgery in the Netherlands: Building the business case for hospitals. Eur J Surg Oncol. 2015;41:1059-1067. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 80] [Cited by in RCA: 67] [Article Influence: 6.1] [Reference Citation Analysis (0)] |
| 4. | McDermott FD, Heeney A, Kelly ME, Steele RJ, Carlson GL, Winter DC. Systematic review of preoperative, intraoperative and postoperative risk factors for colorectal anastomotic leaks. Br J Surg. 2015;102:462-479. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 736] [Cited by in RCA: 633] [Article Influence: 57.5] [Reference Citation Analysis (1)] |
| 5. | De Couck M, Gidron Y. Norms of vagal nerve activity, indexed by Heart Rate Variability, in cancer patients. Cancer Epidemiol. 2013;37:737-741. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 63] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 6. | Guo Y, Koshy S, Hui D, Palmer JL, Shin K, Bozkurt M, Yusuf SW. Prognostic Value of Heart Rate Variability in Patients With Cancer. J Clin Neurophysiol. 2015;32:516-520. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 64] [Cited by in RCA: 50] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 7. | De Couck M, Caers R, Spiegel D, Gidron Y. The Role of the Vagus Nerve in Cancer Prognosis: A Systematic and a Comprehensive Review. J Oncol. 2018;2018:1236787. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 61] [Cited by in RCA: 53] [Article Influence: 6.6] [Reference Citation Analysis (0)] |
| 8. | Hu S, Lou J, Zhang Y, Chen P. Low heart rate variability relates to the progression of gastric cancer. World J Surg Oncol. 2018;16:49. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 34] [Cited by in RCA: 30] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 9. | Kloter E, Barrueto K, Klein SD, Scholkmann F, Wolf U. Heart Rate Variability as a Prognostic Factor for Cancer Survival - A Systematic Review. Front Physiol. 2018;9:623. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 125] [Cited by in RCA: 89] [Article Influence: 11.1] [Reference Citation Analysis (0)] |
| 10. | Keren O, Yupatov S, Radai MM, Elad-Yarum R, Faraggi D, Abboud S, Ring H, Groswasser Z. Heart rate variability (HRV) of patients with traumatic brain injury (TBI) during the post-insult sub-acute period. Brain Inj. 2005;19:605-611. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 90] [Cited by in RCA: 72] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 11. | Guan L, Wang Y, Claydon VE, Mazowita G, Wang Y, Brant R, Collet JP. Autonomic Parameter and Stress Profile Predict Secondary Ischemic Events After Transient Ischemic Attack or Minor Stroke. Stroke. 2019;50:2007-2015. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 24] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 12. | Zhou X, Ma Z, Zhang L, Zhou S, Wang J, Wang B, Fu W. Heart rate variability in the prediction of survival in patients with cancer: A systematic review and meta-analysis. J Psychosom Res. 2016;89:20-25. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 130] [Cited by in RCA: 103] [Article Influence: 10.3] [Reference Citation Analysis (0)] |
| 13. | Martínez-Navarro I, Sánchez-Gómez JM, Collado-Boira EJ, Hernando B, Panizo N, Hernando C. Cardiac Damage Biomarkers and Heart Rate Variability Following a 118-Km Mountain Race: Relationship with Performance and Recovery. J Sports Sci Med. 2019;18:615-622. [PubMed] |
| 14. | De Couck M, Mravec B, Gidron Y. You may need the vagus nerve to understand pathophysiology and to treat diseases. Clin Sci (Lond). 2012;122:323-328. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 52] [Cited by in RCA: 68] [Article Influence: 4.9] [Reference Citation Analysis (1)] |
| 15. | Shaffer F, Ginsberg JP. An Overview of Heart Rate Variability Metrics and Norms. Front Public Health. 2017;5:258. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5460] [Cited by in RCA: 3662] [Article Influence: 406.9] [Reference Citation Analysis (0)] |
| 16. | Stein PK, Pu Y. Heart rate variability, sleep and sleep disorders. Sleep Med Rev. 2012;16:47-66. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 243] [Cited by in RCA: 352] [Article Influence: 23.5] [Reference Citation Analysis (0)] |
| 17. | Joshi R, Kommers D, Oosterwijk L, Feijs L, van Pul C, Andriessen P. Predicting Neonatal Sepsis Using Features of Heart Rate Variability, Respiratory Characteristics, and ECG-Derived Estimates of Infant Motion. IEEE J Biomed Health Inform. 2020;24:681-692. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 82] [Cited by in RCA: 55] [Article Influence: 9.2] [Reference Citation Analysis (0)] |
| 18. | Li K, Cardoso C, Moctezuma-Ramirez A, Elgalad A, Perin E. Heart Rate Variability Measurement through a Smart Wearable Device: Another Breakthrough for Personal Health Monitoring? Int J Environ Res Public Health. 2023;20. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 50] [Cited by in RCA: 39] [Article Influence: 13.0] [Reference Citation Analysis (0)] |
| 19. | Reimer P, Máca J, Szturz P, Jor O, Kula R, Ševčík P, Burda M, Adamus M. Role of heart-rate variability in preoperative assessment of physiological reserves in patients undergoing major abdominal surgery. Ther Clin Risk Manag. 2017;13:1223-1231. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 17] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 20. | Cheng W, Liu J, Zhi M, Shen D, Shao M, Zhang C, Wang G, Jiang Z. Stress and autonomic nerve dysfunction monitoring in perioperative gastric cancer patients using a smart device. Ann Noninvasive Electrocardiol. 2022;27:e12903. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 9] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 21. | Kücükakin B, Gögenur I, Reiter RJ, Rosenberg J. Oxidative stress in relation to surgery: is there a role for the antioxidant melatonin? J Surg Res. 2009;152:338-347. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 48] [Cited by in RCA: 64] [Article Influence: 3.8] [Reference Citation Analysis (0)] |
| 22. | Giglia MD, Stein SL. Overlooked Long-Term Complications of Colorectal Surgery. Clin Colon Rectal Surg. 2019;32:204-211. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 65] [Cited by in RCA: 51] [Article Influence: 7.3] [Reference Citation Analysis (0)] |
| 23. | Slankamenac K, Slankamenac M, Schlegel A, Nocito A, Rickenbacher A, Clavien PA, Turina M. Impact of postoperative complications on readmission and long-term survival in patients following surgery for colorectal cancer. Int J Colorectal Dis. 2017;32:805-811. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53] [Cited by in RCA: 49] [Article Influence: 5.4] [Reference Citation Analysis (0)] |
| 24. | Lopresti AL. Association between Micronutrients and Heart Rate Variability: A Review of Human Studies. Adv Nutr. 2020;11:559-575. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 16] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 25. | Saito I, Hitsumoto S, Maruyama K, Eguchi E, Kato T, Okamoto A, Kawamura R, Takata Y, Nishida W, Nishimiya T, Onuma H, Osawa H, Tanigawa T. Impact of heart rate variability on C-reactive protein concentrations in Japanese adult nonsmokers: The Toon Health Study. Atherosclerosis. 2016;244:79-85. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 17] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 26. | Zhou XL, Wang H, Wu S, Li J, Wu F, Lu W, Zhao JW, Li YH. Comparison of the effects of moxibustion and acupuncture of combined "Biao-Ben" acupoints on intestinal sensitivity and autonomic nervous system function in rats with diarrhea-predominant irritable bowel syndrome. Zhen Ci Yan Jiu. 2023;48:1134-1141. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 27. | Zhao J, Hu J, Jiang Z, Wang G, Liu J, Wang H, Fang P, Liu X, Wang J, Li J. Outcome of Discharge Within 72 Hours of Robotic Gastrectomy Using Enhanced Recovery After Surgery Programs. J Laparoendosc Adv Surg Tech A. 2018;28:1279-1286. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 7] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/