Published online Apr 27, 2025. doi: 10.4240/wjgs.v17.i4.102607
Revised: January 17, 2025
Accepted: February 8, 2025
Published online: April 27, 2025
Processing time: 157 Days and 1.7 Hours
Single-port laparoscopic appendectomy is an advanced minimally invasive surgery that involves the use of upgraded instruments and equipment. We pre
To compare the short-term clinical outcomes of mSLAN with those of conventional three-port laparoscopic appendectomy (CLA) for patients with acute uncomplicated appendicitis.
This single-center, single-blind, prospective, randomized controlled trial included patients who underwent emergency laparoscopic appendectomy for acute uncom
A total of 72 patients were enrolled and randomly divided into 2 groups: The mSLAN group (n = 36) and the CLA group (n = 36). The 24-hour VAS scores, 24-hour postoperative inflammatory response marker levels, first postoperative exhaust times, first out-of-bed activity times, postoperative lengths of hospital stay, operative times, or hospitalization costs did not significantly differ between the two groups. No postoperative complications, including incision infection or hernia, abdominal abscess or intestinal obstruction, were observed during the 1-month postoperative follow-up in either group.
Compared with the CLA protocol, the mSLAN protocol for acute uncomplicated appendicitis yielded comparable short-term clinical outcomes, with a similar operative time and better cosmetic outcomes, indicating its potential for clinical application and superiority for patients with high cosmetic requirements. Further research is needed to evaluate the long-term outcomes.
Core Tip: In this study, the short-term clinical outcomes of modified single-port laparoscopic appendectomy using needle-type grasping forceps (SLAN) were compared with those of conventional three-port laparoscopic appendectomy. Our results demonstrated the feasibility, safety, effectiveness, and clinical application potential of the modified SLAN protocol, which is an alternative minimally invasive surgical protocol for patients with acute uncomplicated appendicitis.
- Citation: Chen Y, Guo SG, Fu XA, Fan ZQ, Yuan JQ, Zhang XX, Liu H, Liu Z, Huang YS, Song L. Modified single-port laparoscopic appendectomy using needle-type grasping forceps vs conventional three-port laparoscopic appendectomy for acute uncomplicated appendicitis. World J Gastrointest Surg 2025; 17(4): 102607
- URL: https://www.wjgnet.com/1948-9366/full/v17/i4/102607.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v17.i4.102607
Acute appendicitis, a well-known cause of abdominal pain, affects millions of patients worldwide, with an annual incidence rate of 96.5-100/100000, which remains one of the most common pathologies resulting in hospital admission, with hospitalization cost in the United States alone at 3 billion dollar annually[1,2]. Many treatment strategies are available for acute appendicitis, such as anti-inflammatory drugs, surgical interventions, and endoscopic retrograde appendicitis therapy[2-8]. Despite ongoing debates, each protocol has specific indications, advantages and limitations.
As the primary protocol for surgical intervention, appendectomy has been widely performed, and with the rapid development of minimally invasive surgical techniques, laparoscopic appendectomy has gradually replaced traditional open surgery. However, the surgical trauma and stress associated with conventional three-port laparoscopic appendectomy (CLA) are somewhat severe for acute uncomplicated appendicitis with slight inflammation. Thus, at our center, we designed a novel technique-single-port laparoscopic appendectomy with needle-type grasping forceps (SLAN) to improve surgical outcomes. In previous studies, researchers compared CLA with SLAN and reported that SLAN produced satisfactory surgical and cosmetic outcomes[9].
Nevertheless, the size of the trocar (5 mm) used in SLAN limits its application in patients with a severely edematous appendix, the narrow operating space affects the fluency of the operation, the absence of long ham-o-lock clips and sterile gauze increases the potential risk of inflammatory complications, and the duration of the procedure extends its learning curve, further limiting its clinical application. Further modifications are needed to ensure stable maintenance of pneumoperitoneum pressure and easy sterile sample removal; thus, significant progress needs to be made prior to the broad adaptation of SLAN. To solve the above problems, a modified protocol was designed. Two trocars were directly inserted into the abdominal cavity instead of via the initial open pathway to stabilize the pneumoperitoneum pressure; moreover, two trocars with sizes of 5 mm and 10 mm were used to improve the space of the surgical channel and facilitate the use of long ham-o-lock clips and gauze and the removal of the thickened appendix. The surgical details were also further modified to alleviate challenges related to the parallel relationship in single-port laparoscopic surgery and consequently improve the fluency of the surgery and shorten the surgical time.
However, the modified protocol extends the umbilical incision to 1.5 cm, and whether the short-term clinical results and cosmetic results of this procedure are comparable to those of the conventional three-port surgical protocol is unclear; thus, high-level medical evidence is needed. Therefore, this prospective, randomized controlled trial was designed to introduce this novel single-port protocol and evaluate its safety and efficacy.
This work is a single-center, single-blind, prospective, randomized controlled trial. Patients with a preoperative diagnosis of acute uncomplicated appendicitis (acute simple and suppurative appendicitis) who were hospitalized between April 2024 and August 2024 at Chaoyang Central Hospital in Liaoning Province, China, were prospectively enrolled. The preoperative diagnosis was based on each patient’s medical history, abdominal physical examination, preoperative laboratory tests, and abdominal ultrasound or computed tomography scans. The follow-up protocol was performed by two investigators (Yuan JQ and Song L). The home address and contact information of each patient were recorded in detail, and the office telephone number of the investigators was also disclosed to the patients. At discharge, the patients were advised to contact the investigators and visit the outpatient clinic in case of any physical complaints. Moreover, the patients were routinely followed up at an outpatient clinic via telephone interviews or via social networks 1 month after surgery to record postoperative complications, including incision infection, hernia, abdominal abscess or intestinal obstruction. Informed consent was obtained from all the included patients. The study protocol was approved by the Ethics Committee of Chaoyang Central Hospital, China Medical University (No. 2024-03) and was prospectively registered in the Chinese Clinical Trials Registry (No. ChiCTR2400081025). The reporting of this study conforms to the CONSORT 2010 statement[10].
In our previous retrospective analysis[8], the maximum 24-hour visual analog scale (VAS) pain score was 0.38 ± 0.79 for SLAN patients and 1.05 ± 10.86 for CLA patients (P = 0.0004). According to the sample size calculation, 34 patients were needed in each group to achieve 80% power to detect superiority using a one-sided, two-sample unequal-variance t test. The margin of superiority was -0.1. The actual difference between the means was assumed to be -0.67. The significance level (alpha) of the test was 0.025. The data were drawn from populations with standard deviations of 0.79 for group 1 and 0.86 for group 2. According to the sample size calculation and considering a 10% drop rate, 38 patients were needed for each group.
Random numbers were generated using SAS version 9.4 (SAS Institute Inc., NC, Cary, United States) and sealed in individual envelopes. The envelopes were randomly opened by a designated researcher before surgery. Patients with odd numbers were included in the modified SLAN (mSLAN) group, and patients with even numbers were included in the CLA group. The umbilicus and left and right lower quadrants of all patients were covered with sterile gauze to conceal the actual surgical protocol.
Inclusion criteria: (1) Preoperative diagnosis of acute uncomplicated appendicitis (acute simple and suppurative appendicitis); (2) 2-70 years of age; and (3) Agreed to participate in this study and signed a written informed consent form.
Exclusion criteria: (1) Intraoperative or postoperative diagnosis of acute complicated appendicitis (acute gangrene and perforated appendicitis) or malignant tumors requiring further treatment; (2) Refusal to undergo surgery; (3) Underwent open surgery (including conversion to open surgery); (4) Severe cardio-cerebrovascular disease or other surgical contraindications; (5) Lost to follow-up; (6) Insufficient case data; and (7) Refusal to participate (including midway withdrawal).
Discharge criteria: (1) No fever, abdominal distension, severe pain or other complications that require clinical intervention; (2) The incision healed well; and (3) Eating normally without difficulties in flatulence or defecation.
The primary endpoint was the 24-hour postoperative VAS score[11], and the secondary endpoints were as follows: (1) Operative time, 24-hour postoperative inflammatory response biomarkers [including white blood cells (WBCs); neutrophil ratio (NEU%); C-reactive protein (CRP); and interleukin-6 (IL-6)]; (2) Time to first postoperative exhaust; (3) Time to first out-of-bed activity; (4) Postoperative length of hospital stay; (5) Hospitalization cost; and (6) Incidence of postoperative complications, including incision infection or hernia, abdominal abscess, or intestinal obstruction.
A surgeon (Chen Y) from our center with extensive experience in laparoscopic procedures performed all the surgeries. All participants were informed of the purpose, protocol, potential risks and benefits of the study and provided written informed consent before surgery. Under general anesthesia, the patient was placed in a supine position, and the carbon dioxide (CO2) pneumoperitoneum pressure was set according to the patient’s age (13 mmHg for adults and 8 mmHg for children). The laparoscopic display screen was placed on the right side of the patient. Laparoscopes were manufactured by STORZ Corporation of Germany, disposable trocars and needle-type grasping forceps were manufactured by Hangzhou Kangji Medical Instrument Corporation of China, and disposable bags were manufactured by Hangzhou Weide Medical Technology Corporation of China. The appendix was sent for pathological examination after surgery.
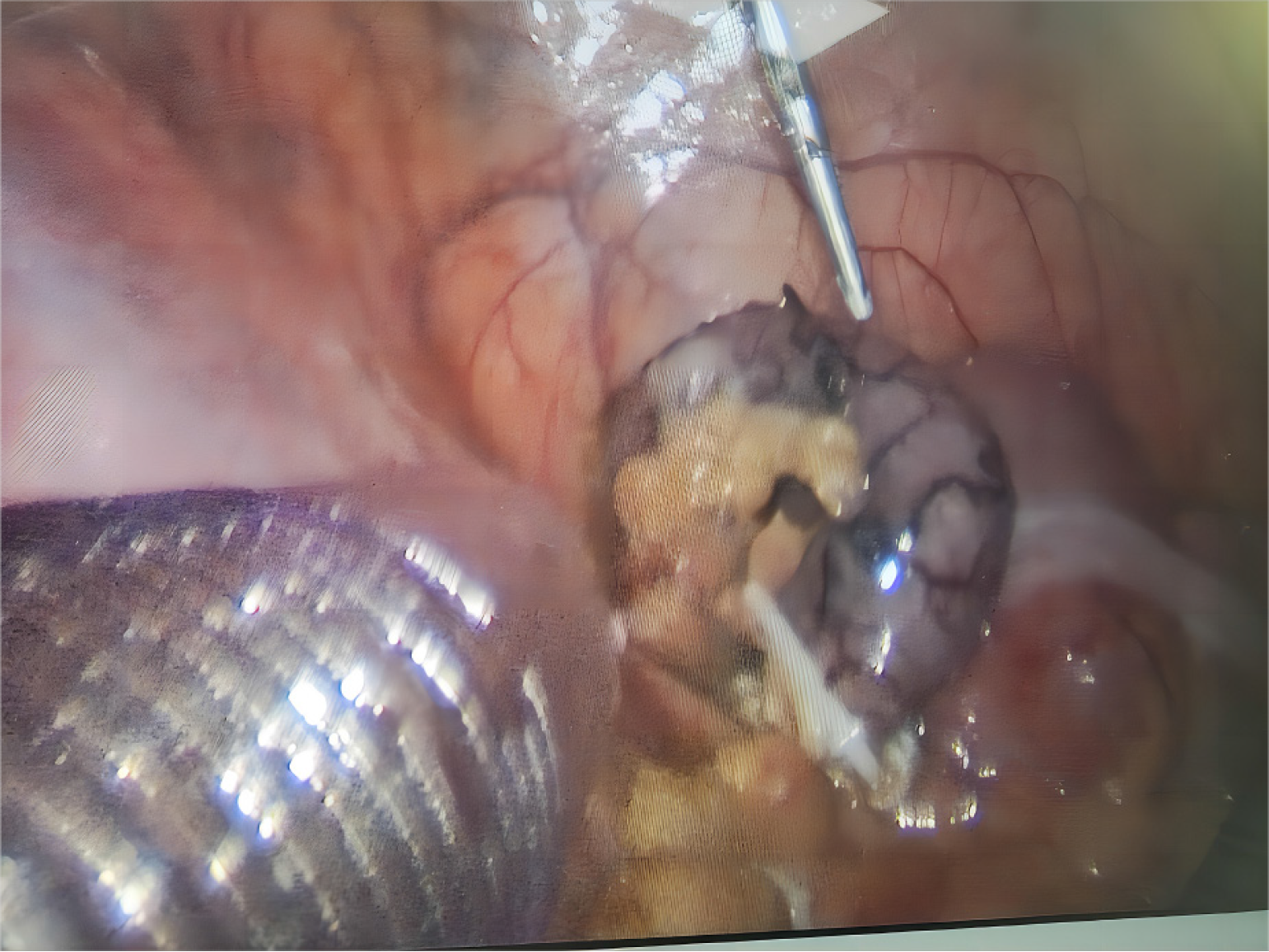
A mSLAN protocol was used. A 10 mm long umbilical incision was made, CO2 pneumoperitoneum was established, and a 10 mm disposable trocar was inserted into the abdominal cavity. The patient was repositioned such that the head was angled 30° downward and the body was tilted 30° to the left. The surgeon stood to the lower left, and the assistant stood to the upper left. A 5 mm caliber 30° laparoscope (Karl Storz SE and Co. KG, Tuttlingen, Germany) was placed to explore the abdomen, ensuring assessment of the status of the abdominal infection, determination of adhesions, and visualization of the appendix. The incision was lengthened along the left of the umbilicus by 5 mm, and a 5 mm trocar was then inserted to place a 30° laparoscopic lens and to display surgical fields, while needle-type grasping forceps (Approval No. zsyjx 20140056; Hangzhou Kangji Medical Instrument Co., Ltd., Hangzhou, China) were inserted at the McBurney site. Next, the 10 mm trocar was moved forward to the right iliac fossa until it was observed in the surgical field (Figure 1).
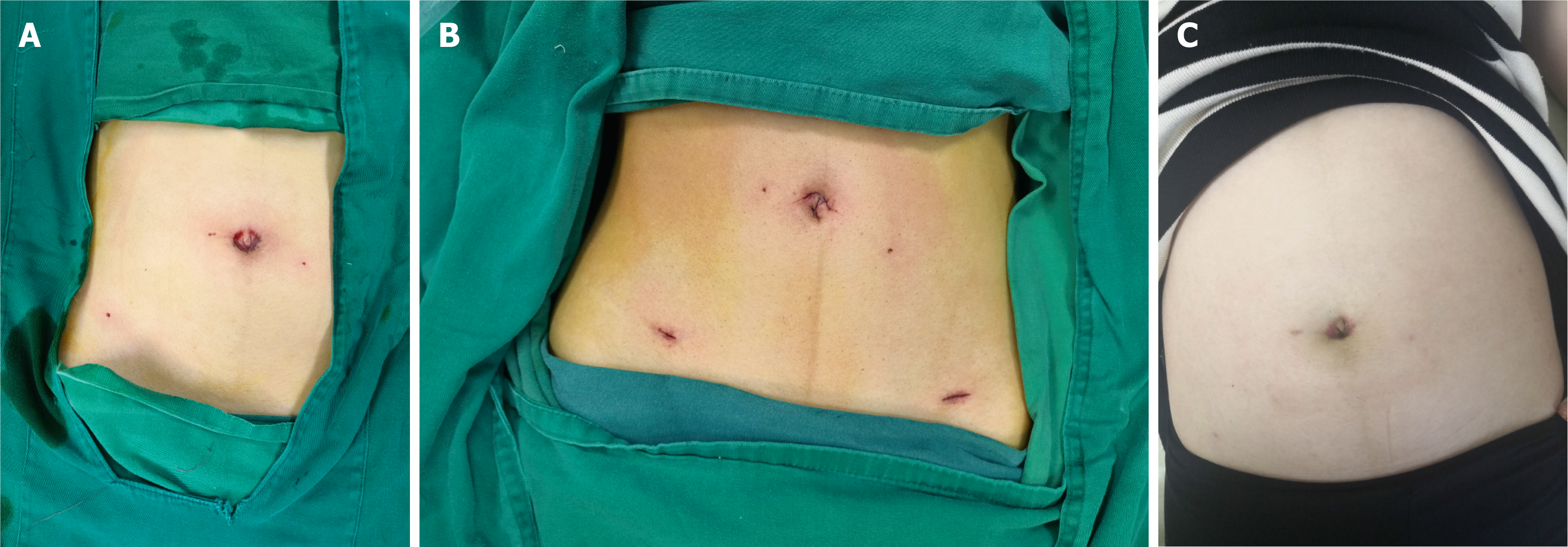
A sterile gauze was inserted through the 10 mm trocar to prevent bleeding and exudation. An ultrasound scalpel was used to free the mesentery of the appendix. Longer Ham-o-lock absorbable clips were inserted to clip the root and distal end of the appendix, after which the appendix was resected. To ensure that no bleeding or secondary injury occurred, the sterile gauze was removed, and the appendix was removed and carefully placed in a disposable bag through the 10 mm trocar. The CO2 pneumoperitoneum was resolved, and the skin around the umbilical incision was disinfected with iodophor and alcohol in sequence. The incision was sutured with 3-0 absorbable threads (Figure 2A). The detailed procedures and intraoperative imaging data were reported previously[12].
The CLA protocol was performed in this group. First, a 12 mm long umbilical incision was made, and CO2 pneumoperitoneum was established. A 12 mm disposable trocar was then inserted to serve as the main port for the operation and removal of the appendix. Next, the patient was repositioned so that the head was angled 30° downward and the body was slightly tilted 30° to the left. The surgeon stood to the upper left, and the assistant stood to the lower left. A 10 mm disposable trocar was then placed at the converse McBurney site for laparoscopic observation, a 5 mm trocar was inserted at the McBurney site for assisted operations (Figure 2B), and the remaining procedures, such as laparoscopic exploration and appendectomy, were similar to the mSLAN protocol previously described.
All clinical data were analyzed using statistical product and service solutions 26.0 software (IBM Corp., Armonk, NY, United States). The count data are expressed as numbers and were analyzed using χ2 tests; the measurement data are expressed as the means ± SDs and were analyzed using independent samples t tests, and the collected data were normally distributed. A P value < 0.05 indicated statistical significance.
A total of 72 patients were eventually enrolled, and 4 patients were excluded from the study because of an intraoperative diagnosis of acute perforated appendicitis (n = 2), a postoperative pathologic diagnosis of a malignant tumor (n = 1), or midway withdrawal (n = 1). The patients’ baseline demographics and preoperative clinical data are shown in Table 1. The patients’ baseline data, including age, sex, body mass index, American Society of Anesthesiologists physical status classification[13], disease course, or preoperative outcomes, including VAS scores or inflammatory markers (WBC, NEU%, CRP and IL-6), did not significantly differ between the two groups, indicating strong comparability.
| Variable | mSLAN group (n = 36) | CLA group (n = 36) | P value |
| Age, years | 36.92 ± 15.4 | 38.08 ± 20.13 | 0.783 |
| Sex, male/female | 20/16 | 19/17 | 0.815 |
| BMI, kg/m2 | 23.86 ± 3.23 | 24.15 ± 4.4 | 0.748 |
| ASA | 1.5 ± 0.51 | 1.53 ± 0.51 | 0.817 |
| Disease course, hours | 21.39 ± 17.53 | 19.71 ± 17.04 | 0.681 |
| Preoperative data | |||
| WBC, × 109/L | 12.42 ± 4.6 | 12.59 ± 4.75 | 0.877 |
| NEU, % | 80.33 ± 11.31 | 78.75 ± 10.95 | 0.549 |
| CRP, μg/L | 16.08 ± 24.63 | 19.53 ± 26.49 | 0.569 |
| IL-6, ng/L | 90.45 ± 301.61 | 95.41 ± 279.34 | 0.942 |
| VAS scores | 2.92 ± 0.28 | 2.89 ± 0.4 | 0.733 |
As Table 2 shows, the 12- and 24-hour postoperative VAS scores fluctuated between 1 and 2 points in both groups, indicating a mild response, and the difference was not significant (P = 0.091). The first times to postoperative exhaust and out-of-bed activity fluctuated by approximately 20 and 15 hours, respectively, in both groups, and the differences were not significant (P = 0.41; P = 0.575, respectively). The 24-hour postoperative inflammatory marker levels, including WBC, NEU%, CRP, and IL-6 levels, did not significantly differ between the two groups (P = 0.419; P = 0.371, respectively). Similarly, the operative time, postoperative length of hospital stay and hospitalization cost were not significantly different between the two groups (P = 0.172; P = 0.664; P = 0.194, respectively). After the 1-month postoperative follow-up, no complications, including incision infection, hernia, abdominal abscess, or intestinal obstruction, were observed in either group.
| Variable | mSLAN group (n = 36) | CLA group (n = 36) | P value |
| Postoperative 12-hour VAS scores | 1.81 ± 0.58 | 1.94 ± 0.48 | 0.268 |
| Postoperative 24-hour VAS scores | 1.28 ± 0.45 | 1.47 ± 0.51 | 0.091 |
| Postoperative 24-hour laboratory test outcomes | |||
| WBC, × 109/L | 9.18 ± 3.38 | 9.79 ± 3.72 | 0.465 |
| NEU, % | 73.8 ± 8.99 | 72.99 ± 10.35 | 0.725 |
| CRP, mg/L | 49.09 ± 36.51 | 58.43 ± 58.41 | 0.419 |
| IL-6, pg/L | 11.07 ± 17.22 | 15.66 ± 25.35 | 0.371 |
| First postoperative exhaust time, hours | 20.22 ± 8.62 | 22.24 ± 11.76 | 0.41 |
| First out-of-bed activity time, hours | 15.51 ± 6.39 | 16.38 ± 6.57 | 0.575 |
| Operative time, minutes | 38.67 ± 14.05 | 34.5 ± 11.44 | 0.172 |
| Postoperative hospital stay, days | 3.06 ± 1.13 | 3.17 ± 1.04 | 0.664 |
| Cost of hospitalization, yuan | 10776.75 ± 1117.8 | 10417.51 ± 1207.42 | 0.194 |
Acute appendicitis is one of the most well-known causes of abdominal pain worldwide, and appropriately selected minimally invasive surgical protocols can reduce surgical trauma and psychologically burden for patients, resulting in a smooth recovery process[3,14]. Single-port laparoscopic appendectomy is an advanced minimally invasive surgery, and because upgraded instruments and equipment are used, good aesthetic outcomes can be achieved[15,16]. However, the size of the incision used in existing single-port approaches is approximately 1.5 to 2.5 cm[17,18], and this incision can be further improved for patients with high cosmetic requirements. Moreover, the surgical difficulties caused by the parallel operation relationship of single-port laparoscopic surgery urgently need solutions. Notably, the selection of the surgical technique should be tailored to each patient’s unique circumstances, the surgeon’s expertise, and the patient’s preferences[19]. Patients with acute uncomplicated appendicitis tend to prefer a single-port laparoscopic protocol that is less traumatic and characterized by wide surgical fields and a high level of patient comfort. Technical advancements are needed to ensure that patients receive the most effective and safest care possible.
In recent years, we have continuously modified surgical procedures and updated surgical instruments to improve surgeon comfort, increase surgical safety, and expand surgical indications. The aim of this prospective study was to demonstrate the feasibility, safety, effectiveness, and clinical application potential of the mSLAN protocol by comparing the short-term clinical outcomes with those of the CLA protocol.
Pain at the surgical incision is one of the most common surgical complications. As minimally invasive surgical techniques have gradually replaced laparotomies, smaller incisions are associated with less postoperative pain and therefore more manageable physical and psychological burdens. Moreover, the length of the incision made for the mSLAN procedure in our center was smaller than that made for the CLA procedure (1.5 cm vs 2.7 cm); however, does this modification lead to less postoperative pain?
The VAS is commonly used to score pain intensity. Scores range from 0 to 10; a score of 0 indicates no pain, a score less than 3 points indicates tolerable pain, and a score of 10 indicates severe pain[11]. Previous studies have suggested that single-port laparoscopic surgery may be associated with severe postoperative pain[20]; however, we noted low postoperative VAS scores in both groups, indicating mild pain. Although the 12- and 24-hour postoperative VAS scores and the times to first out-of-bed activity were not significantly different between patients who underwent the mSLAN procedure and those who underwent the CLA procedure, the less intense pain associated with this novel technique was sufficient for it to gain acceptance.
Postoperative inflammation is well known to slow the recovery process and cause a series of complications, such as fever, incision infection, and ileus. The inflammatory response after appendectomy can be caused by appendicitis or surgical trauma. In this study, we evaluated the inflammatory response after appendectomy via an integrated analysis of inflammatory markers, including WBC, NEU%, CRP and IL-6.
As stated in previous studies, single-port laparoscopic surgery may result in more severe surgical trauma and elevated levels of inflammatory markers, such as IL-6 and CRP, postoperatively[20]. Nevertheless, the levels of inflammatory biomarkers (WBC, NEU%, CRP and IL-6) before and after surgery did not significantly differ. As a novel technical protocol, the modified SLAN procedure is safe; does not cause considerable surgical trauma, postoperative inflammatory responses, or postoperative infectious complications; and is not associated with a slow recovery (3.06 days vs 3.17 days). In addition, needle-type grasping forceps were supported by our project fund, whereas other traditional surgical instruments do not incur additional hospital costs. Considering the similar postoperative hospital stay durations for the two procedures, the hospitalization cost increased only slightly (10776.75 yuan vs 10417.51 yuan).
Postoperative gastrointestinal function recovery is a source of concern after abdominal surgery. Early gastrointestinal function recovery can facilitate early oral feeding and promote enhanced recovery after surgery and even early discharge[21]. Postoperative gastrointestinal dysfunction is associated with inflammation, surgical trauma and stress, as mentioned previously. This study revealed no significant differences between the two groups in terms of the time to first posto
The surgical duration reflects not only the severity of the disease and the complexity of the surgery but also the popularity of the surgical protocol. According to previous studies[20,22,23], the long duration of single-port appendectomy may be closely related to the parallel operative angle of single-port surgery, which limits the generalizability of this technique. Although the initial SLAN protocol calls for a substantially smaller surgical incision, the use of two 5 mm caliber trocars limits the applicability of the procedure in patients with severe edema and appendicitis, precludes the insertion of long Ham-o-lock clips, leads to instability in the pneumoperitoneum pressure, and prevents aseptic smooth removal of the specimen, resulting in a long, limited, unsafe procedure.
Unlike in the initial SLAN protocol, a 1.5 cm umbilical incision was used in the modified protocol, a CO2 pneumoperitoneum was routinely established, and two trocars (10 mm and 5 mm caliber) were used to maintain stable pneumoperitoneum pressure. In particular, the substitution of a 10 mm trocar allowed the convenient placement of long ham-o-lock clips and gauze into the abdominal cavity. The procedure used to remove the appendix was the same as that used in the CLA, ensuring an aseptic and safe procedure, shortening the surgical time and expanding the surgical indications. Notably, the 10 mm trocar was moved forward from the right iliac fossa intraoperatively, thus avoiding obstructing the laparoscopic view of the CO2 pneumoperitoneum and preventing instrument collision due to poor cooperation between the surgeon and assistant during surgery. Thus, the surgical procedure was safer and smoother.
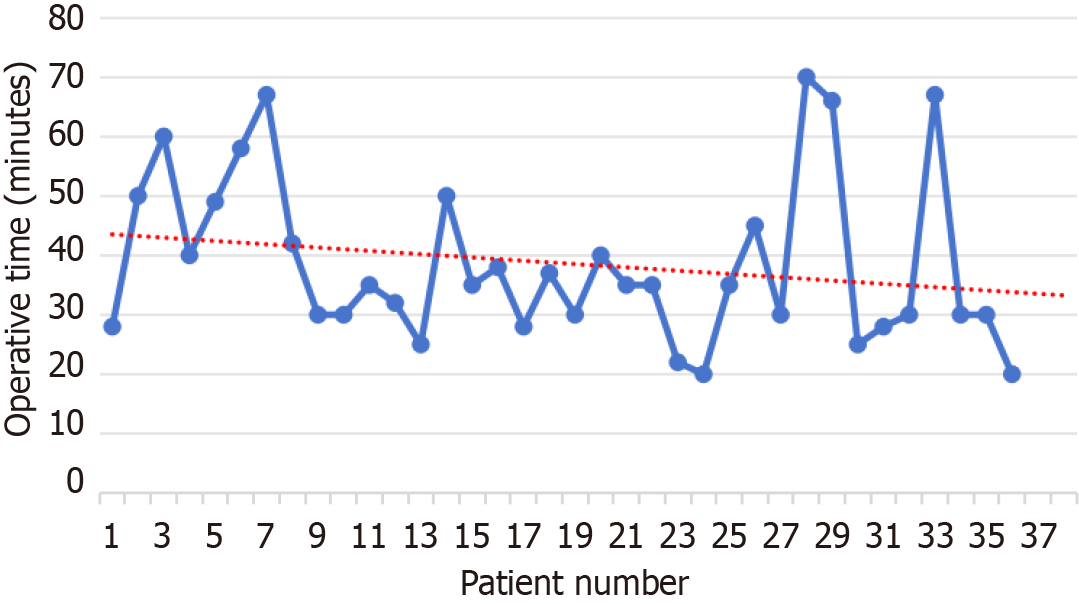
Our study revealed that the mean surgical time was significantly shorter in the mSLAN group than in the traditional SLAN group (38.67 minutes vs 66.25 minutes)[9] and tended to decrease, suggesting that surgeons were gradually mastering the technique (Figure 3).
In addition, the new SLAN protocol was modified to be more efficiently converted to the CLA protocol. For example, one patient was intraoperatively diagnosed with acute perforated appendicitis, and the mSLAN protocol was discontinued. Subsequently, incisions were made at the McBurney and converse McBurney sites; thus, no additional surgical incisions were needed, thereby maintaining the surgical duration.
In summary, the short-term outcomes of the CLA protocol and the modified SLAN protocol were comparable. Through improvements in the technical protocol and the application of a 10 mm trocar and disposable bag, the pneumoperitoneum pressure was effectively maintained, the surgical space was sufficiently increased, the surgical duration was greatly reduced, the surgical indications were expanded, and the incidence of postoperative complications was significantly reduced. Although the size of the umbilical incision was increased to 1.5 cm compared with that of the initial protocol, the cosmetic effect was not inferior (Figure 2A); moreover, the cosmetic effect at 1 month after surgery remained favorable (Figure 2C). The mSLAN protocol has high potential for clinical application and generalization, especially for patients with high cosmetic requirements. Our technical protocol and present study have several limitations. First, the needle-type grasping forceps are soft and easy to twist (Figure 4). Second, the abdominal drainage tube cannot be placed during single-port surgery, and surgeons should promptly switch to three-port surgery if severe disease is identified in the abdomen. Third, our study is a single-blinded, small-sample, single-center study, which may introduce subjective bias in terms of outcomes such as pain scores and potentially impact the detection of postoperative complications; moreover, the rates of long-term complications, such as incisional hernias and adhesive intestinal obstructions, are unclear. Thus, additional studies with double-blinded, larger sample sizes conducted at multiple centers with long-term follow-up results are needed to evaluate long-term clinical outcomes and increase statistical power.
The CLA protocol and the modified SLAN protocol had comparable short-term clinical outcomes as well as similar surgical durations and better cosmetic outcomes; thus, the modified SLAN protocol has notable clinical application potential and superiority for patients with high cosmetic requirements. In the future, long-term clinical outcomes need to be evaluated, and more practical and reliable surgical instruments need to be designed and developed.
| 1. | Moris D, Paulson EK, Pappas TN. Diagnosis and Management of Acute Appendicitis in Adults: A Review. JAMA. 2021;326:2299-2311. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 283] [Cited by in RCA: 226] [Article Influence: 45.2] [Reference Citation Analysis (1)] |
| 2. | Lamm R, Kumar SS, Collings AT, Haskins IN, Abou-Setta A, Narula N, Nepal P, Hanna NM, Athanasiadis DI, Scholz S, Bradley JF 3rd, Train AT, Pucher PH, Quinteros F, Slater B. Diagnosis and treatment of appendicitis: systematic review and meta-analysis. Surg Endosc. 2023;37:8933-8990. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 24] [Reference Citation Analysis (109)] |
| 3. | Di Saverio S, Podda M, De Simone B, Ceresoli M, Augustin G, Gori A, Boermeester M, Sartelli M, Coccolini F, Tarasconi A, De' Angelis N, Weber DG, Tolonen M, Birindelli A, Biffl W, Moore EE, Kelly M, Soreide K, Kashuk J, Ten Broek R, Gomes CA, Sugrue M, Davies RJ, Damaskos D, Leppäniemi A, Kirkpatrick A, Peitzman AB, Fraga GP, Maier RV, Coimbra R, Chiarugi M, Sganga G, Pisanu A, De' Angelis GL, Tan E, Van Goor H, Pata F, Di Carlo I, Chiara O, Litvin A, Campanile FC, Sakakushev B, Tomadze G, Demetrashvili Z, Latifi R, Abu-Zidan F, Romeo O, Segovia-Lohse H, Baiocchi G, Costa D, Rizoli S, Balogh ZJ, Bendinelli C, Scalea T, Ivatury R, Velmahos G, Andersson R, Kluger Y, Ansaloni L, Catena F. Diagnosis and treatment of acute appendicitis: 2020 update of the WSES Jerusalem guidelines. World J Emerg Surg. 2020;15:27. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 923] [Cited by in RCA: 739] [Article Influence: 123.2] [Reference Citation Analysis (7)] |
| 4. | Xu Z, Jin L, Wu W. Clinical efficacy and safety of endoscopic retrograde appendicitis treatment for acute appendicitis: A systematic review and meta-analysis. Clin Res Hepatol Gastroenterol. 2023;47:102241. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (115)] |
| 5. | Yang B, Kong L, Ullah S, Zhao L, Liu D, Li D, Shi X, Jia X, Dalal P, Liu B. Endoscopic retrograde appendicitis therapy versus laparoscopic appendectomy for uncomplicated acute appendicitis. Endoscopy. 2022;54:747-754. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 62] [Cited by in RCA: 56] [Article Influence: 14.0] [Reference Citation Analysis (0)] |
| 6. | de Almeida Leite RM, Seo DJ, Gomez-Eslava B, Hossain S, Lesegretain A, de Souza AV, Bay CP, Zilberstein B, Marchi E, Machado RB, Barchi LC, Ricciardi R. Nonoperative vs Operative Management of Uncomplicated Acute Appendicitis: A Systematic Review and Meta-analysis. JAMA Surg. 2022;157:828-834. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 92] [Cited by in RCA: 76] [Article Influence: 19.0] [Reference Citation Analysis (8)] |
| 7. | Herrod PJJ, Kwok AT, Lobo DN. Randomized clinical trials comparing antibiotic therapy with appendicectomy for uncomplicated acute appendicitis: meta-analysis. BJS Open. 2022;6. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 33] [Cited by in RCA: 31] [Article Influence: 7.8] [Reference Citation Analysis (108)] |
| 8. | Pata F, Nardo B, Ielpo B, Di Martino M, Murzi V, Di Saverio S, Yang B, Ortenzi M, Pisanu A, Pellino G, Podda M. Endoscopic retrograde appendicitis therapy versus appendectomy or antibiotics in the modern approach to uncomplicated acute appendicitis: A systematic review and meta-analysis. Surgery. 2023;174:1292-1301. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 19] [Article Influence: 6.3] [Reference Citation Analysis (105)] |
| 9. | Chen Y, Guo S, Liu Y, Yuan J, Fan Z. Single-port laparoscopic appendectomy using a needle-type grasping forceps compared with conventional three-port laparoscopic appendectomy for patients with acute uncomplicated appendicitis: a single-center retrospective study. J Int Med Res. 2022;50:3000605221119647. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 7] [Article Influence: 1.8] [Reference Citation Analysis (108)] |
| 10. | Schulz KF, Altman DG, Moher D; CONSORT Group. CONSORT 2010 statement: updated guidelines for reporting parallel group randomised trials. BMJ. 2010;340:c332. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7710] [Cited by in RCA: 7014] [Article Influence: 438.4] [Reference Citation Analysis (4)] |
| 11. | Price DD, McGrath PA, Rafii A, Buckingham B. The validation of visual analogue scales as ratio scale measures for chronic and experimental pain. Pain. 1983;17:45-56. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2923] [Cited by in RCA: 2564] [Article Influence: 59.6] [Reference Citation Analysis (3)] |
| 12. | Chen Y, Fan ZQ, Fu XA, Zhang XX, Yuan JQ, Guo SG. Modified technical protocol for single-port laparoscopic appendectomy using needle-type grasping forceps for acute simple appendicitis: A case report. World J Gastrointest Surg. 2024;16:3328-3333. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Reference Citation Analysis (0)] |
| 13. | Hocevar LA, Fitzgerald BM. American Society of Anesthesiologists Staging. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. [PubMed] |
| 14. | Bhangu A, Søreide K, Di Saverio S, Assarsson JH, Drake FT. Acute appendicitis: modern understanding of pathogenesis, diagnosis, and management. Lancet. 2015;386:1278-1287. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 949] [Cited by in RCA: 768] [Article Influence: 69.8] [Reference Citation Analysis (4)] |
| 15. | Li C, Liu Y, Jiang Y, Xu Y, Wang Z. Single-incision compared with conventional laparoscopy for appendectomy in acute appendicitis: a systematic review and meta-analysis. Int J Colorectal Dis. 2022;37:1925-1935. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 11] [Reference Citation Analysis (0)] |
| 16. | Han Y, Yuan H, Li S, Wang WF. Single-incision versus conventional three-port laparoscopic appendectomy for acute appendicitis: A meta-analysis of randomized controlled trials. Asian J Surg. 2024;47:864-873. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 9] [Reference Citation Analysis (2)] |
| 17. | Kim BJ, Kim JW, Choi YS, Park YG, Kim BG, Park JM, Lee SE, Park BK, Suh SW, Chi KC. Minimization of Wound With the Assistance of a Needle Grasper in Single-Incision Laparoscopic Appendectomy. Surg Innov. 2019;26:536-544. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 18. | Jin HY, Lee CS, Lee YS. Single Incision Laparoscopic Appendectomy Using a New Multi-joint Articulating Instrument. J Gastrointest Surg. 2021;25:2437-2438. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 13] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 19. | Deng H, Hu J. Single-port vs. three-port for laparoscopic appendectomy. Asian J Surg. 2024;47:5355-5356. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 20. | Golebiewski A, Anzelewicz S, Wiejek A, Lubacka D, Czauderna P. A Prospective Randomized Controlled Trial of Single-Port and Three-Port Laparoscopic Appendectomy in Children. J Laparoendosc Adv Surg Tech A. 2019;29:703-709. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 16] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 21. | Alsharqawi N, Alhashemi M, Kaneva P, Baldini G, Fiore JF Jr, Feldman LS, Lee L. Validity of the I-FEED score for postoperative gastrointestinal function in patients undergoing colorectal surgery. Surg Endosc. 2020;34:2219-2226. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 29] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 22. | Cirocchi R, Cianci MC, Amato L, Properzi L, Buononato M, Di Rienzo VM, Tebala GD, Avenia S, Iandoli R, Santoro A, Vettoretto N, Coletta R, Morabito A. Laparoscopic appendectomy with single port vs conventional access: systematic review and meta-analysis of randomized clinical trials. Surg Endosc. 2024;38:1667-1684. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 13] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 23. | Zaman S, Mohamedahmed AYY, Srinivasan A, Stonelake S, Sillah AK, Hajibandeh S, Hajibandeh S. Single-port laparoscopic appendicectomy versus conventional three-port approach for acute appendicitis: A systematic review, meta-analysis and trial sequential analysis of randomised controlled trials. Surgeon. 2021;19:365-379. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 17] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/