Published online Apr 27, 2025. doi: 10.4240/wjgs.v17.i4.101578
Revised: December 10, 2024
Accepted: February 10, 2025
Published online: April 27, 2025
Processing time: 190 Days and 18.4 Hours
Boerhaave syndrome, or spontaneous esophageal rupture, is a rare and life-threatening emergency, typically caused by a sudden increase in esophageal pressure due to violent coughing or vomiting. Early diagnosis is challenging as its symptoms often resemble those of other diseases. Understanding its pathological features and treatment strategies is therefore critical for clinical practice.
This report describes a case of spontaneous esophageal rupture triggered by violent coughing in a 55-year-old male with a history of smoking and hyper
Spontaneous esophageal rupture presents significant diagnostic and therapeutic challenges. Early recognition and timely intervention are crucial for improving prognosis. This case highlights the importance of imaging and surgical treatment, offering new insights for managing similar cases and providing valuable clinical guidance.
Core Tip: This study thoroughly reveals the pathology of spontaneous esophageal rupture induced by severe coughing. It systematically documents the complete diagnostic and treatment process of esophageal rupture for the first time. Advanced imaging techniques are employed to accurately locate esophageal injuries. A personalized surgical strategy is implemented, significantly improving treatment success rates. The findings offer innovative strategies for managing similar rare cases.
- Citation: Xiong SY, Liu CJ, Li YF, Zhang HL, Chen XW, Wang HM, Chen JC. Multimodal diagnostic and surgical approach to spontaneous esophageal rupture induced by severe coughing: A case report. World J Gastrointest Surg 2025; 17(4): 101578
- URL: https://www.wjgnet.com/1948-9366/full/v17/i4/101578.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v17.i4.101578
The esophagus is a crucial component of the digestive system, primarily responsible for transporting food from the mouth to the stomach. The health of the esophagus is directly linked to the digestive process and overall quality of life[1]. Esophageal diseases include esophagitis, esophageal cancer, foreign bodies in the esophagus, and esophageal rupture[2]. Among these, spontaneous esophageal rupture, also known as Boerhaave syndrome, is rare but considered a medical emergency due to its high mortality rate and severe complications[3]. This condition typically results from the sudden rupture of the esophageal wall, leading to severe pain and other life-threatening symptoms. A thorough understanding of its pathophysiology, diagnostic methods, and treatment strategies is crucial for improving patient survival rates[4].
Recent studies indicate that the mortality rate for spontaneous esophageal rupture is extremely high, particularly when there is a delay in diagnosis and treatment[5-7]. The urgency of the condition arises from the fact that once the esophagus ruptures, food, gastric acid, and saliva can enter the thoracic cavity, causing serious infections and inflammation, such as suppurative pleuritis. Therefore, prompt and accurate diagnosis is critical for effective treatment and prognosis. Spontaneous esophageal rupture is challenging to diagnose due to its diverse and nonspecific clinical manifestations, often leading to misdiagnosis as other chest or abdominal conditions. Diseases such as esophagitis, esophageal cancer, acute myocardial infarction, and gastroesophageal reflux disease share similar symptoms (e.g., chest pain, difficulty breathing). However, diagnosis requires thorough history taking, clinical assessment, and imaging studies [such as computed tomography (CT) scans or endoscopy]. Early and accurate diagnosis is especially critical in the absence of typical triggers, such as severe vomiting or coughing. Therefore, when faced with similar symptoms, heightened awareness and prompt diagnostic measures are essential[8-10].
Literature reports indicate that spontaneous esophageal rupture can be caused by severe vomiting, overeating, or direct trauma and may present with symptoms such as severe chest pain, dyspnea, and subcutaneous emphysema[11-13]. Treatment typically involves emergency surgery and the placement of a chest tube to prevent or manage infection[14]. Although esophageal rupture due to severe coughing is rarely reported, this suggests that there are still many unexplored and poorly understood areas in this field.
Despite the increasing number of studies and case reports on spontaneous esophageal rupture, existing literature primarily focuses on the general characteristics of the disease, with insufficient in-depth analysis and discussion of cases caused by specific factors. Current diagnostic criteria, treatment protocols, and patient management strategies for this condition remain inadequate, underscoring the need for further research to fill these knowledge gaps, particularly through detailed documentation and analysis of cases caused by specific triggers. Such research is essential to improve the diagnosis and treatment of these cases[15].
This study reports a case of spontaneous esophageal rupture induced by severe coughing, providing empirical data aimed at improving diagnostic and treatment strategies, as well as increasing healthcare professionals’ awareness of such cases. By enhancing early diagnosis and individualized treatment, the study aims to reduce mortality associated with this condition and improve patients’ quality of life.
The patient was conscious and reported severe pain in the aforementioned areas, accompanied by significant difficulty breathing.
This paper reports on a 59-year-old male patient who presented to Guangzhou Traditional Chinese Medicine Hospital on December 18, 2023, with severe pain in the left side of his back, chest, and upper abdomen following a severe coughing episode that occurred six hours prior.
No similar symptoms in the past, no significant medical history, denies smoking and alcohol consumption.
The patient maintains a regular lifestyle, has no family history of chronic diseases, and has not been exposed to harmful environments or chemicals.
Upon arrival at the hospital, the patient’s vital signs were as follows: Blood pressure of 145/85 mmHg, heart rate of 110 beats per minute, respiratory rate of 22 breaths per minute, body temperature of 37.5 °C, and oxygen saturation of 92%.
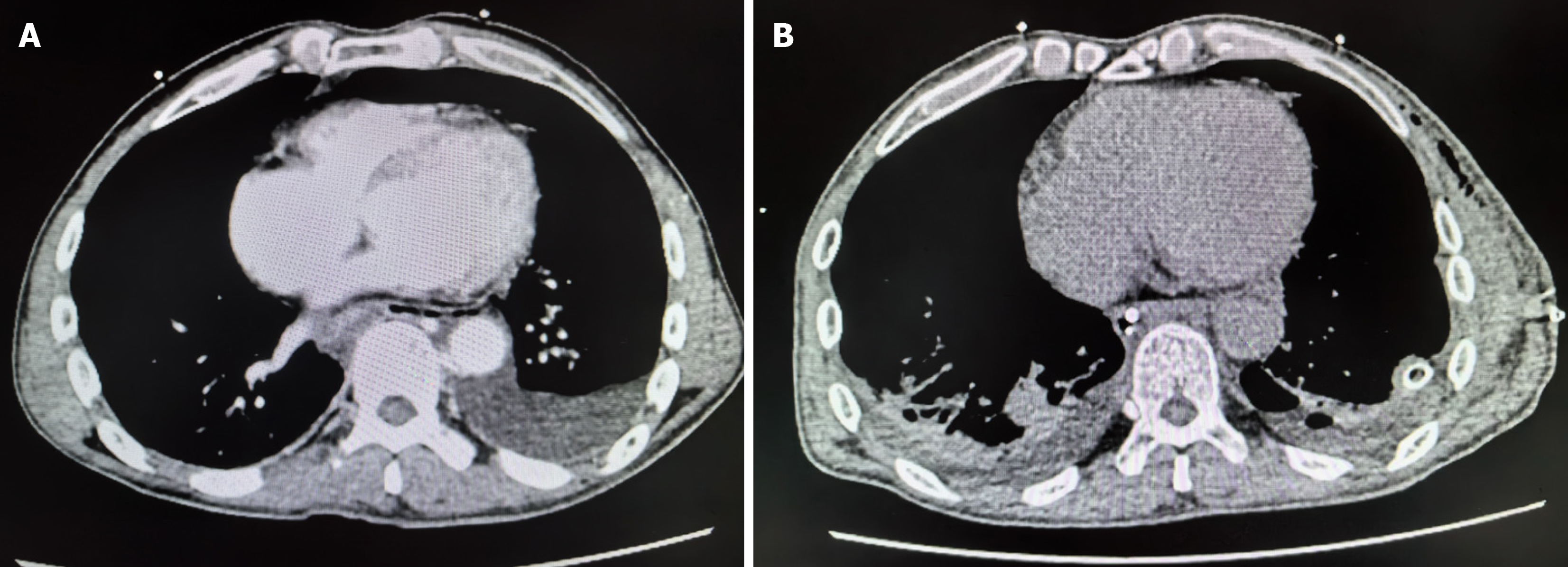
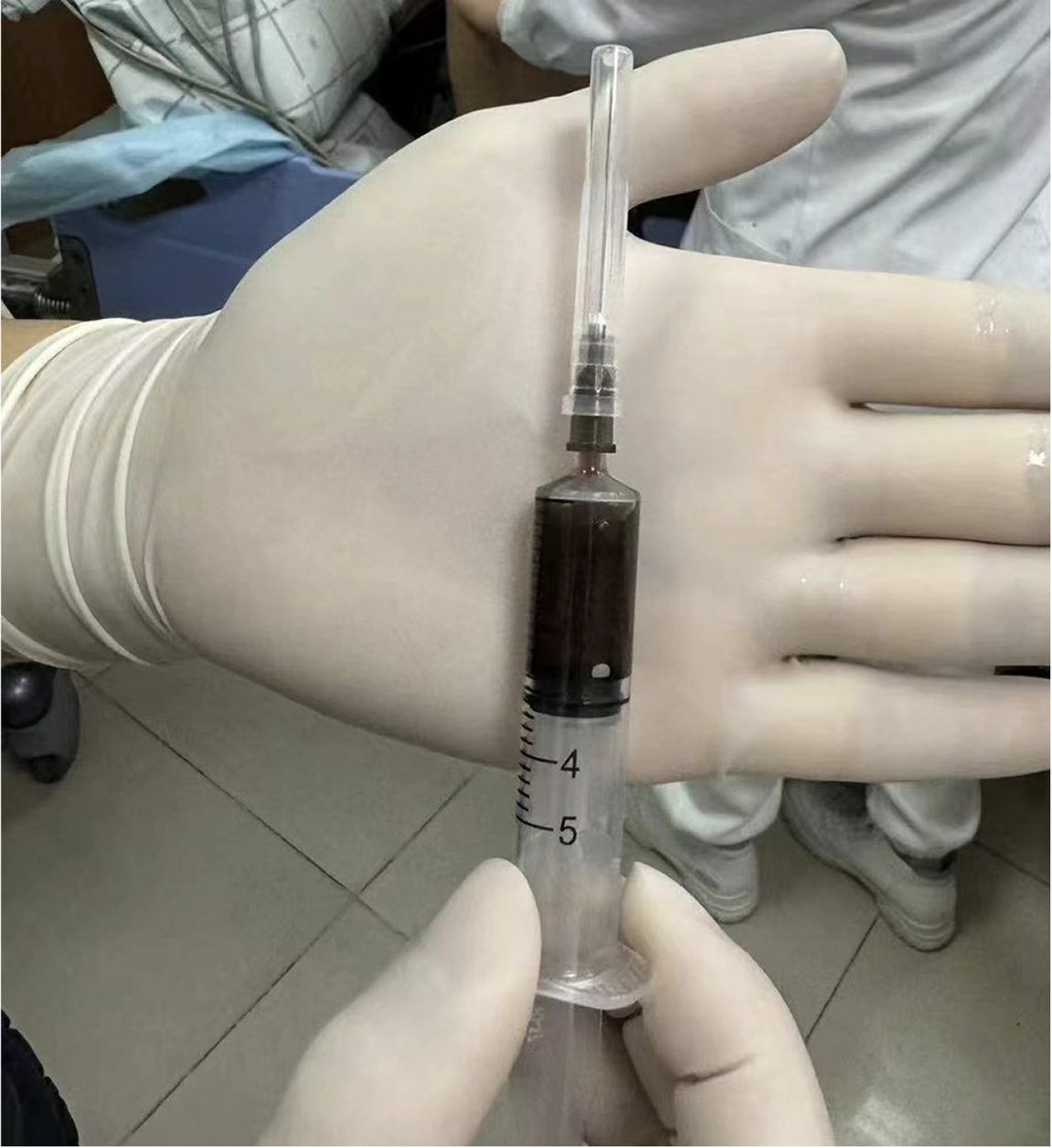
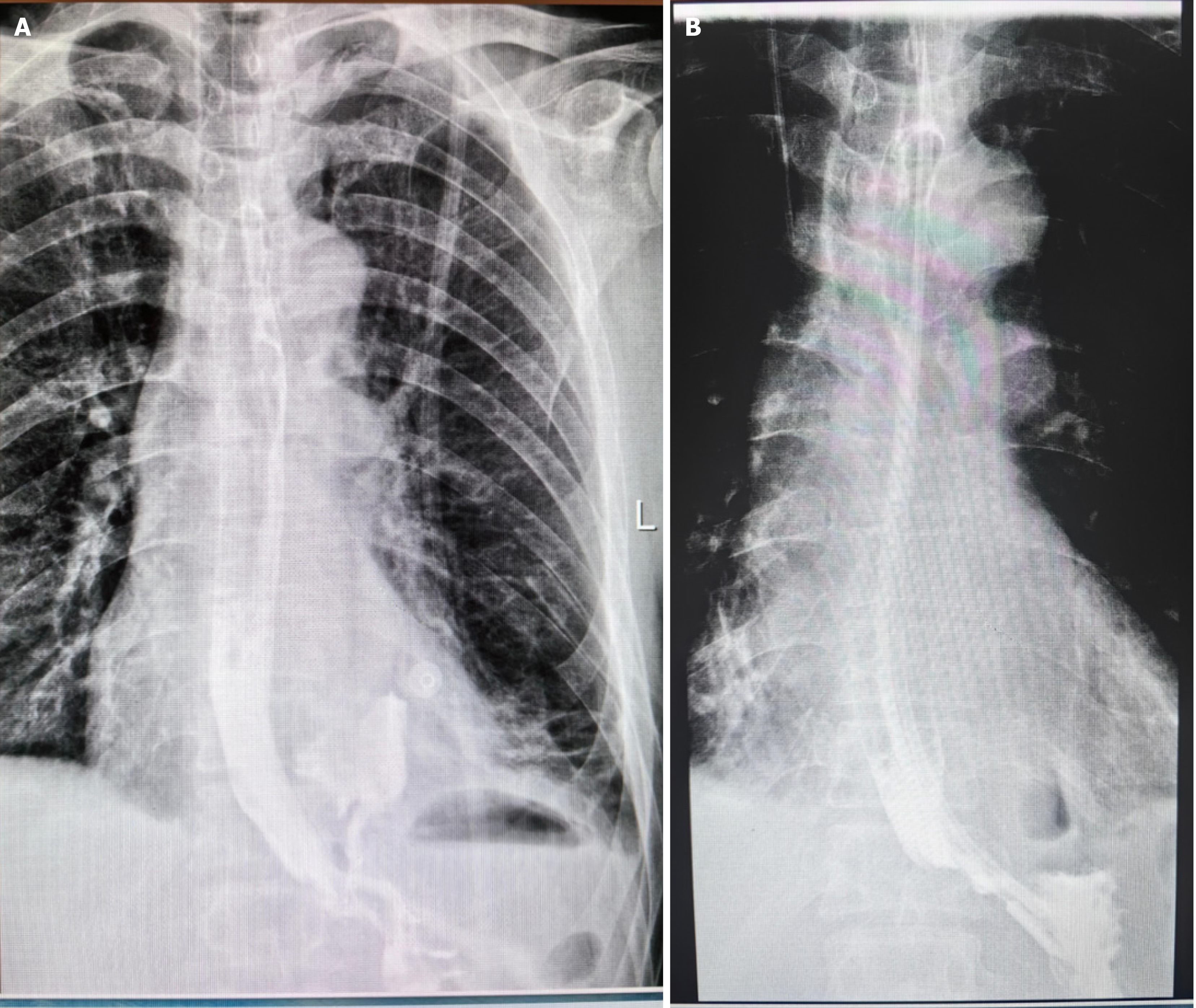
The initial imaging assessment, including a contrast-enhanced CT scan of the chest and abdomen (Figure 1A), revealed a small left-sided pneumothorax, approximately 30% compression of lung tissue, minor mediastinal emphysema, and signs of emphysema and bullae formation in both upper lungs. The preliminary diagnosis was esophageal rupture. Subsequently, a diagnostic thoracentesis was performed under ultrasound guidance (Figure 2), extracting dark, turbid fluid containing small esophageal debris. A chest tube was then inserted, draining approximately 700 mL of dark digestive fluid, accompanied by gastrointestinal decompression. An esophagogram (barium swallow test) revealed contrast leakage from the lower esophagus into the thoracic cavity (Figure 3A).
Based on the clinical presentation and auxiliary examination results, a final diagnosis of spontaneous esophageal rupture was confirmed.
Upon admission, the patient immediately received emergency management, including oxygen therapy to alleviate respiratory distress, analgesics to reduce pain, fasting, and gastrointestinal decompression to relieve gastrointestinal pressure. The patient underwent emergency esophageal repair surgery under general anesthesia. Preoperative evaluations included esophageal contrast radiography, chest CT, blood tests, and an electrocardiogram, which confirmed the location and size of the perforation in the lower esophagus. Prophylactic intravenous antibiotics were administered, and the anesthesia team performed a preoperative assessment, ultimately opting for general anesthesia.
The diagnosis was initially confirmed through esophageal contrast radiography and chest CT, which clarified the location and size of the esophageal rupture. Surgery was performed via a left thoracotomy, approximately 20 cm in length, selected for optimal surgical access. The procedure began with the removal of gastric contents and purulent material from the thoracic cavity, followed by thorough debridement. Gastroscopy was used to precisely locate the esophageal perforation, which was found above the diaphragm with a rupture measuring approximately 2.5 cm. A double-layer repair was performed using absorbable sutures, and a water test confirmed the absence of leaks at the anastomosis. The thoracic cavity was repeatedly irrigated postoperatively, with further reinforcement of the repair as needed. Postoperative gastroscopy confirmed a well-healed anastomosis, and a duodenal feeding tube was inserted.
The patient was transferred to the intensive care unit for close monitoring. Postoperative esophageal contrast radiography and chest/abdominal CT confirmed the success of the repair. A chest drainage tube was placed within 24 hours to drain accumulated fluid, and was removed after 72 hours based on imaging results. Pain management was provided through a fentanyl pump, initially set at 1 mcg/hour and adjustable up to 2 mcg/hour, with continuous administration for 3 days. Antimicrobial therapy included imipenem (0.5 g IV every 6-8 hours for 10 days) and metronidazole (500 mg IV every 8 hours for 10 days). Pancreatic secretion suppression was achieved with octreotide (0.1 mg subcutaneously every 8 hours for 6 days) and somatostatin (3-6 mg/hour continuous IV infusion for 60 hours). Omeprazole was administered for gastric protection. The patient was transitioned to a semi-liquid diet to reduce esophageal strain and support nutritional recovery. Laboratory results showed improvement in inflammatory markers (C-reactive protein, procalcitonin, total protein, and albumin).
During the follow-up period, imaging examinations indicated that the patient was recovering well. A follow-up CT scan on December 25, 2023, showed a significant reduction in the left-sided pneumothorax (Figure 1B). An esophagogram conducted on December 26, 2023, revealed no leakage of contrast material (Figure 3B). A chest digital radiography panoramic scan on December 29, 2023, demonstrated improvement in the left-sided hydropneumothorax and bilateral lower lung infiltration. On the same day, the chest tube was removed, and the patient was transitioned to a semi-liquid diet. The patient was successfully discharged on January 1, 2024, with plans for regular follow-up observations.
Spontaneous esophageal rupture, also known as Boerhaave syndrome, is a rare and life-threatening medical emergency. This condition is typically triggered by severe vomiting or coughing, although it can occasionally be caused by dysphagia or the ingestion of large objects. Esophageal motility disorders, excessive alcohol consumption, and certain eating disorders may increase esophageal pressure, thereby elevating the risk of rupture[16]. The rarity and nonspecific clinical presentation of spontaneous esophageal rupture make its diagnosis particularly challenging, often leading to misdiagnosis as other thoracic emergencies. Initial diagnosis generally relies on chest X-rays and CT scans, with contrast esophagography being the diagnostic gold standard[17]. However, the diagnosis is frequently delayed due to the varied clinical manifestations of the condition. It is crucial to maintain a high index of suspicion, especially in patients presenting with acute chest pain following severe vomiting or coughing[18].
The treatment strategy is determined based on the patient’s condition, the size and location of the rupture, and the presence of any infection. Treatment options range from conservative approaches, such as fasting, intravenous fluids, and antibiotic therapy, to more invasive procedures like primary repair, esophageal stent placement, or, in severe cases, esophagectomy[19]. The prognosis is highly dependent on the timeliness of diagnosis and treatment; early diagnosis and intervention are crucial for survival, while delays are associated with increased morbidity and mortality[20].
When selecting diagnostic tools, while various imaging techniques each have their strengths and limitations, CT scanning is preferred due to its high resolution and ability to rapidly provide critical information for decision-making. Although chest X-rays are cost-effective, they have lower resolution; magnetic resonance imaging offers better soft tissue contrast but requires longer scanning times; ultrasound is radiation-free and suitable for bedside use but is dependent on operator experience for detecting deep-seated lesions; nuclear medicine scans provide functional and metabolic information but are expensive and time-consuming. CT scanning can quickly and accurately identify the size and location of pneumothorax and detect other lung abnormalities, excelling particularly in bubble analysis. Enhanced CT also clearly delineates blood supply to tissues and vessels, aiding in the identification of concomitant vascular lesions. These advantages make CT an ideal choice in emergency settings, enabling prompt and accurate diagnosis, which in turn facilitates quicker treatment decisions and improves patient outcomes (Supplementary Table 1).
We conducted a literature review using the search terms “Spontaneous Esophageal Rupture” and “Coughing” in the PubMed database, analyzing six representative studies from 1963 to 2024. Table 1 summarizes the clinical presentations, diagnostic methods, treatment options, and prognoses of the patients in these studies.
| Journal | Ref. | PMID | Year | Case presentation | Diagnosis | Treatment | Outcome |
| Case Rep Emerg Med | Aga et al[14] | 26949552 | 2016 | Esophageal rupture after swallowing a chicken nugget | CT scan | IV fluids, antibiotics, esophageal stent, VATS drainage | Unspecified |
| Nagoya J Med Sci | Sakatoku et al[15] | 31849387 | 2019 | Thoracic empyema after spontaneous esophageal rupture, recurrent episodes | CT, Endoscopy | Conservative therapy, subtotal esophagectomy | Resolved, no recurrence |
| Radiol Case Rep | Rajic and Schandl[19] | 35345564 | 2022 | Pneumomediastinum after masturbation, not directly related to esophageal rupture but relevant for differential diagnosis | Clinical observation | Not applicable | Not applicable |
| Am J Otolaryngol | Stevens et al[20] | 20015755 | 2010 | Tracheal rupture by vomiting, highlights diagnostic considerations similar to esophageal rupture | CT scan | Conservative management | Resolved |
| Cureus | Canelas Mendes et al[16] | 37905259 | 2023 | Geriatric presentation of Boerhaave’s syndrome | Chest X-ray, CT angiography | Thoracic drainage, antibiotics, esophageal prosthesis | Discharged after 48 days |
| J Am Coll Surg | Bakhos et al[18] | 25053221 | 2014 | Spontaneous pneumomediastinum analysis, discussing management strategies | Retrospective review | Conservative management | Excellent prognosis, low recurrence risk |
Aga et al’s study emphasizes the need for heightened awareness of spontaneous esophageal rupture, even in the absence of typical symptoms (e.g., vomiting or severe coughing)[14]. Although their research focused on swallowing disorders as the primary trigger, our case suggests that severe coughing, as an atypical trigger, can also lead to esophageal rupture, expanding the range of potential causes. Thus, our findings challenge traditional views on esophageal rupture triggers and suggest a broader spectrum of factors should be considered in diagnosis. Sakatoku et al’s study highlights the importance of individualized treatment, presenting both conservative and surgical approaches[15]. Our case supports the effectiveness of conservative treatment in the absence of major complications but emphasizes the significant role of severe coughing as a trigger, offering a new perspective on early diagnosis and personalized treatment. However, Sakatoku et al[15] did not explore the impact of atypical triggers on treatment decisions, a gap our study addresses. Rajic and Schandl[19] cautioned that esophageal rupture may be confused with other chest conditions, such as pneumothorax or subcutaneous emphysema, complicating diagnosis. Our case faced similar challenges, particularly in the absence of typical triggers, underscoring the key role of imaging in excluding esophageal rupture. Although previous literature touches on this issue, there is a lack of specific guidance on improving diagnostic accuracy in atypical cases. Stevens et al[20] expanded the scope of esophageal rupture triggers, noting that vomiting could cause tracheal rupture in children. Similarly, our study suggests that severe coughing can also be a trigger, further supporting the wide range of potential causes for esophageal rupture. While Stevens et al[20] focused on vomiting, our research highlights the risk of coughing, emphasizing the importance of multiple triggers in esophageal rupture. Canelas Mendes et al[16] explored the atypical presentation of esophageal rupture in elderly patients, emphasizing the risk of misdiagnosis. Our study further corroborates this, particularly in cases with atypical histories and symptoms, where careful consideration is necessary. Bakhos et al[18] considered mediastinal emphysema typically benign did not require excessive intervention. However, our study suggests that mediastinal emphysema could be an early sign of esophageal rupture, warranting increased vigilance. Compared to Bakhos et al[18], our research advocates for further investigation into the possibility of esophageal rupture in similar cases.
In conclusion, this study reports a case of spontaneous esophageal rupture triggered by severe coughing, challenging the traditional view that only vomiting is a primary cause and expanding the spectrum of potential triggers. While the literature has primarily focused on typical triggers, our study underscores the importance of maintaining heightened awareness of atypical presentations, especially in the absence of clear triggers.
Regarding diagnosis, the symptoms of esophageal rupture are often nonspecific, such as chest pain, difficulty breathing, and subcutaneous emphysema, which can also be seen in other chest conditions. Existing literature highlights the risk of misdiagnosis, potentially delaying treatment and increasing patient risk (e.g., Rajic and Schandl[19], Stevens et al[20]). Therefore, physicians should prioritize detailed history-taking, physical examination, and imaging to rule out esophageal rupture in cases with nonspecific symptoms.
In terms of treatment, conservative therapy, endoscopic stenting, and surgery each have their own advantages and limitations. Individualized treatment is critical, especially for patients with early diagnosis and no significant complications, where conservative management may suffice, while surgical intervention is necessary for extensive ruptures or severe complications. Sakatoku et al’s study also supports this, stressing that treatment plans should be adjusted based on the patient’s specific condition[15].
Furthermore, the research by Cornejo et al[21] demonstrates the application of endoscopic and laparoscopic techniques, while Doğuç et al[22] explores the potential of artificial intelligence in early diagnosis. These technological advancements offer new possibilities for early diagnosis and treatment of esophageal rupture, suggesting that future research may benefit from these emerging technologies.
This study reports a case of spontaneous esophageal rupture induced by severe coughing, providing preliminary insights into the diverse causes of this condition. However, because the study is based on a single case, the generalizability of the findings is limited, making it difficult to apply them to all similar situations. Specifically, the selection of this case and individual differences may affect the reliability and applicability of the conclusions, potentially introducing bias in understanding the pathological features and treatment responses of other patient populations.
Although the study offers a relatively comprehensive analysis through imaging and clinical evaluation, its single-center design and small sample size may not capture the full variability of the disease. This limitation reduces the external validity of the results, making it challenging to fully reflect the diverse clinical presentations and treatment needs of spontaneous esophageal rupture. Therefore, future research should involve multi-center, large-scale studies to validate these findings and improve the reliability and generalizability of the results.
Moreover, while existing research provides some preliminary understanding of the pathological mechanisms, the lack of systematic studies on the underlying mechanisms means the pathophysiological processes of the disease remain unclear. Future studies should focus on more in-depth experimental and clinical research to better define the mechanisms of spontaneous esophageal rupture, providing a stronger theoretical foundation for more accurate diagnosis and treatment.
The clinical significance of this study lies in its reminder to clinicians to maintain a high level of vigilance, particularly when managing patients presenting with nonspecific chest symptoms and lacking typical triggers. Although the clinical diagnosis of esophageal rupture has traditionally relied on typical triggers, such as severe vomiting or swallowing difficulties, this study demonstrates, through case presentation, that atypical triggers such as severe coughing can also lead to esophageal rupture. This finding broadens the understanding of the potential causes of esophageal rupture and suggests that clinicians should consider a wider range of possibilities to avoid missed or misdiagnosis. Therefore, this study emphasizes that the clinical diagnosis of esophageal rupture should not be confined to traditional diagnostic criteria but should also include heightened awareness of atypical symptoms.
Furthermore, this study highlights the importance of individualized treatment strategies, especially when dealing with spontaneous esophageal rupture, an acute and severe condition. The research indicates that early diagnosis and precise treatment can significantly improve patient outcomes, particularly in early cases without major complications, where conservative treatment can effectively control the condition. However, for patients with more severe presentations, prompt surgical intervention is essential. Therefore, this study provides clinical guidance on how to select treatment options based on the patient's specific condition and trigger, underscoring the critical role of rapid and accurate treatment decisions in improving survival rates and reducing complications.
The diagnostic challenge of spontaneous esophageal rupture primarily arises from its nonspecific clinical manifestations, such as chest pain, difficulty breathing, and subcutaneous emphysema, which overlap with various chest diseases. Therefore, clinicians need to conduct a comprehensive evaluation combining patient history, physical examination, and imaging studies (such as chest X-ray and esophagography) to accurately rule in or out the diagnosis. Additionally, due to the rarity of this condition, it may not be considered in the initial differential diagnosis, leading to delayed diagnosis and increased patient risk. Treatment strategies should be individualized based on the patient's clinical condition, the size and location of the rupture, and any associated complications, in order to optimize treatment outcomes and improve prognosis.
This study not only provides important guidance for current clinical practice but also offers new perspectives and directions for future research. Firstly, future studies should further explore the impact of atypical triggers on the pathogenesis of esophageal rupture, such as coughing, excessive straining, and other factors, particularly in high-risk populations such as the elderly and patients with pulmonary diseases. These studies will help identify at-risk groups earlier in clinical settings, thereby improving early diagnosis rates of the disease.
Additionally, with ongoing advancements in technology, the application of artificial intelligence and imaging techniques holds great promise for the early diagnosis of esophageal rupture. By analyzing large volumes of imaging data, artificial intelligence can assist clinicians in making more accurate diagnoses in a shorter amount of time, especially when dealing with atypical cases. Future research should also explore how emerging technologies such as modern endoscopy, laparoscopy, and artificial intelligence can be integrated to achieve more precise diagnoses and personalized treatment plans. This integration could improve treatment outcomes and shorten recovery times for patients.
In summary, the clinical findings of this study offer new insights into the early diagnosis and treatment of esophageal rupture, laying a foundation for future related research. Further investigations will not only deepen our understanding of this condition but also drive the development of more efficient and accurate treatment strategies, ultimately improving patients’ quality of life and prognosis.
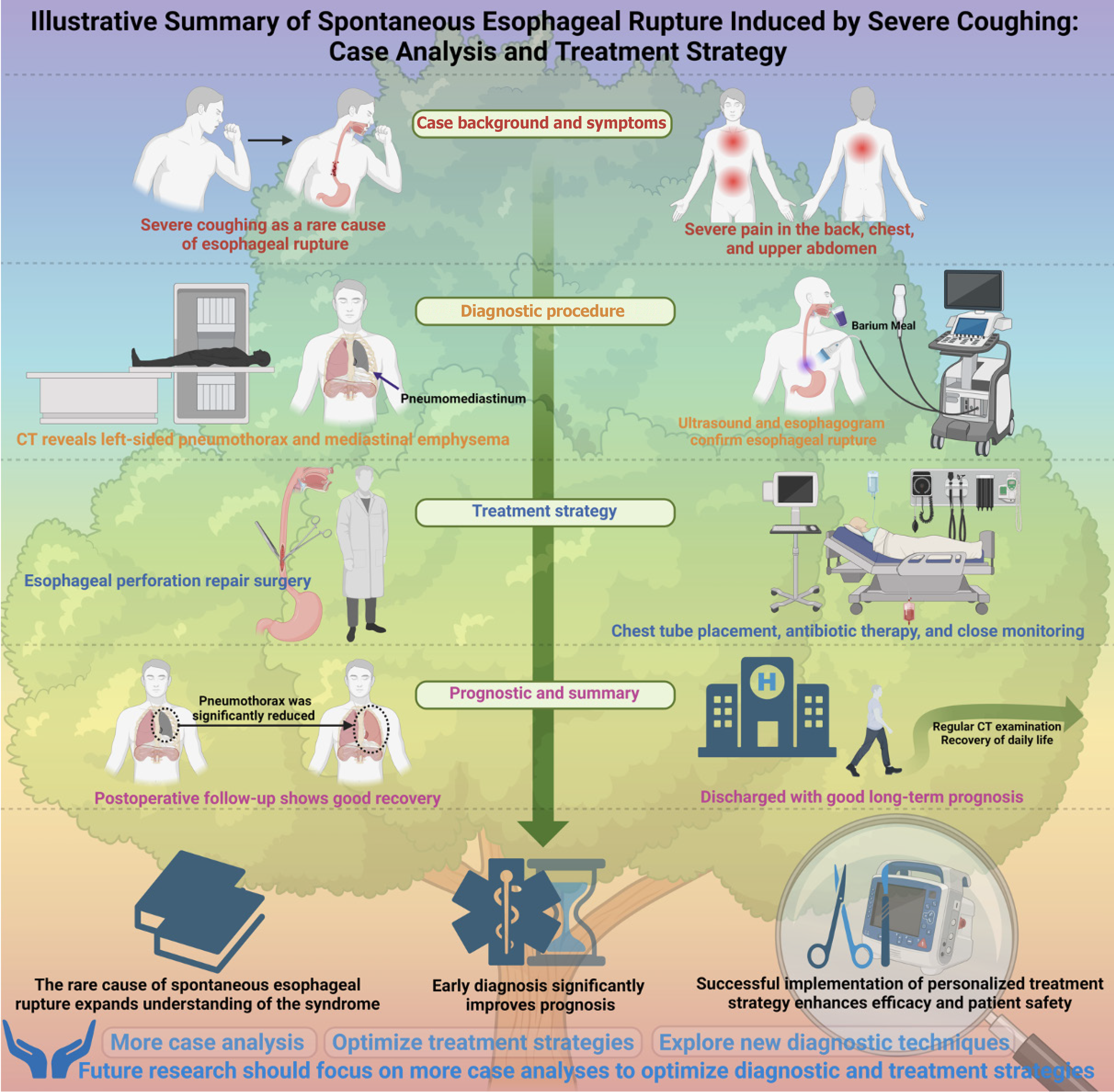
This study emphasizes the importance of early recognition of spontaneous esophageal rupture (Boerhaave syndrome), particularly when atypical symptoms are present. Clinicians must maintain a high level of vigilance, as this condition is often misdiagnosed or diagnosed late due to its nonspecific symptoms. Early identification not only helps prevent the progression of the disease but can also significantly improve patient prognosis (Figure 4). Furthermore, this study highlights the critical role of individualized treatment strategies. Given the variations in clinical presentations among different patients, standardized treatment protocols often fail to meet the needs of all patients. Therefore, developing personalized treatment plans is essential for improving efficacy and reducing complications. Clinicians should be prepared to adjust treatment approaches flexibly based on the patient’s response, thereby enhancing overall treatment outcomes.
| 1. | Dorcaratto D, Grande L, Ramón JM, Pera M. [Quality of life of patients with cancer of the oesophagus and stomach]. Cir Esp. 2011;89:635-644. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 8] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 2. | Liao F, Zhu Z, Pan X, Li B, Zhu Y, Chen Y, Shu X. Safety and Efficacy of Nonoperative Treatment in Esophageal Perforation Caused by Foreign Bodies. Clin Transl Gastroenterol. 2022;13:e00451. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 11] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 3. | Zhukovskiy V, Trutyak I, Pidhirnyi Y, Filip Z, Pankiv M, Kozopas V. Problematic issues of diagnosis and treatment of Boerhaave’s syndrome. ЕМ. 2024;20:226-232. [DOI] [Full Text] |
| 4. | Kwiatkowska NM, Kaminska A, Sielewicz M, Kasprzyk M, Piwkowski C. Boerhaave syndrome complicated by subsequent esophageal stenosis and esophageal fistula. Kardiochir Torakochirurgia Pol. 2023;20:274-276. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Reference Citation Analysis (0)] |
| 5. | Dong S, Xie S, Zhou Y. Spontaneous Rupture of Esophageal Diverticulum-A Case Report and Literature Review. Diagnostics (Basel). 2022;13. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 6. | Kircheva DY, Vigneswaran WT. Successful primary repair of late diagnosed spontaneous esophageal rupture: A case report. Int J Surg Case Rep. 2017;35:49-52. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 7] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 7. | Mavroudis CD, Kucharczuk JC. Acute Management of Esophageal Perforation. Curr Surg Rep. 2014;2:34. [RCA] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 8] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 8. | Morgom M, Saeed L, Ali H, Elhassan H. The Hidden Tear: Improving Diagnostic Accuracy for Spontaneous Esophageal Perforation in the ED. Cureus. 2024;16:e65482. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 9. | Aldoseri R, Nasser M, Alshehabi M. A Case of an Atypical Presentation of Spontaneous Esophageal Rupture. Cureus. 2024;16:e57578. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 10. | Kiev J, Amendola M, Bouhaidar D, Sandhu BS, Zhao X, Maher J. A management algorithm for esophageal perforation. Am J Surg. 2007;194:103-106. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 56] [Cited by in RCA: 52] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 11. | Schalet R, Carro Cruz F, Berezowski I, Adams-Mardi C, Haile H, Schueler SA, Borum ML. Boerhaave Syndrome Mimicking Acute Coronary Syndrome. ACG Case Rep J. 2024;11:e01453. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 12. | Yajima S, Suzuki T, Shiratori F, Yamakawa T, Okubo K, Oshima Y, Shimada H. 606. The Changes of Thoracoscopic or Laparoscopic Approach for Spontaneous Esophageal Rupture in Japan. Dis Esophagus. 2024;37. [DOI] [Full Text] |
| 13. | Pan J, Ge Y, Feng T, Zheng C, Zhang X, Feng S, Sun T, Zhao F, Sha Z, Zhang H. Outcome of treatment modalities for spontaneous esophageal rupture: a meta-analysis and case series. Int J Surg. 2024;111:1135-1143. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 4] [Article Influence: 4.0] [Reference Citation Analysis (2)] |
| 14. | Aga Z, Avelino J, Darling GE, Leung JJ. An Unusual Case of Spontaneous Esophageal Rupture after Swallowing a Boneless Chicken Nugget. Case Rep Emerg Med. 2016;2016:5971656. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 3] [Article Influence: 0.3] [Reference Citation Analysis (1)] |
| 15. | Sakatoku Y, Fukaya M, Kawaguchi K, Fujieda H, Miyata K, Nagino M. Repeated episodes of thoracic empyema after spontaneous esophageal rupture. Nagoya J Med Sci. 2019;81:693-699. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Reference Citation Analysis (0)] |
| 16. | Canelas Mendes C, Duarte L, Madeira Lopes J. Boerhaave's Syndrome: An Unusual Geriatric Presentation. Cureus. 2023;15:e46212. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 17. | Danielyan SN, Rabadanov KM, Abakumov MM, Tarabrin EA. [Spontaneous rupture of the esophagus in a patient with chronic obstructive pulmonary disease]. Khirurgiia (Mosk). 2019;99-102. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 18. | Bakhos CT, Pupovac SS, Ata A, Fantauzzi JP, Fabian T. Spontaneous pneumomediastinum: an extensive workup is not required. J Am Coll Surg. 2014;219:713-717. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 40] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 19. | Rajic N, Schandl C. Spontaneous pneumomediastinum and subcutaneous emphysema after masturbation. Radiol Case Rep. 2022;17:1722-1726. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 20. | Stevens MS, Mullis TC, Carron JD. Spontaneous tracheal rupture caused by vomiting. Am J Otolaryngol. 2010;31:276-278. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 16] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 21. | Cornejo J, Cornejo J, Vargas M, Carvajal M, Perales P, Rodríguez G, Macias C, Canizares S, Silva P, Cubas RF, Jimenez MC, Lincango EP, Serrano L, Palomares R, Aspilcueta S, Castillo-larios R, Evans LA, De La Cruz-vargas JA, Risk M, Grossmann RJ, Elli EF. SY-MIS Project: Biomedical Design of Endo-Robotic and Laparoscopic Training System for Surgery on the Earth and Space. Emerg Sci J. 2024;8:372-393. [DOI] [Full Text] |
| 22. | Doğuç Ö, Silahtaroğlu G, Canbolat ZN, Hambarde K, Yiğitbaşı AA, Gökay H, Yılmaz M. Diagnosis of Covid-19 Via Patient Breath Data Using Artificial Intelligence. Emerg Sci J. 2023;7:105-113. [DOI] [Full Text] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/