Published online Apr 27, 2025. doi: 10.4240/wjgs.v17.i4.100851
Revised: January 23, 2025
Accepted: February 18, 2025
Published online: April 27, 2025
Processing time: 91 Days and 23.4 Hours
Colorectal cancer (CRC) is a common malignant tumor in the digestive system, whose main treatment comprises surgical resection, radiotherapy and che
To investigate the logistic regression analysis of bone metastasis after CRC surgery and related influencing factors.
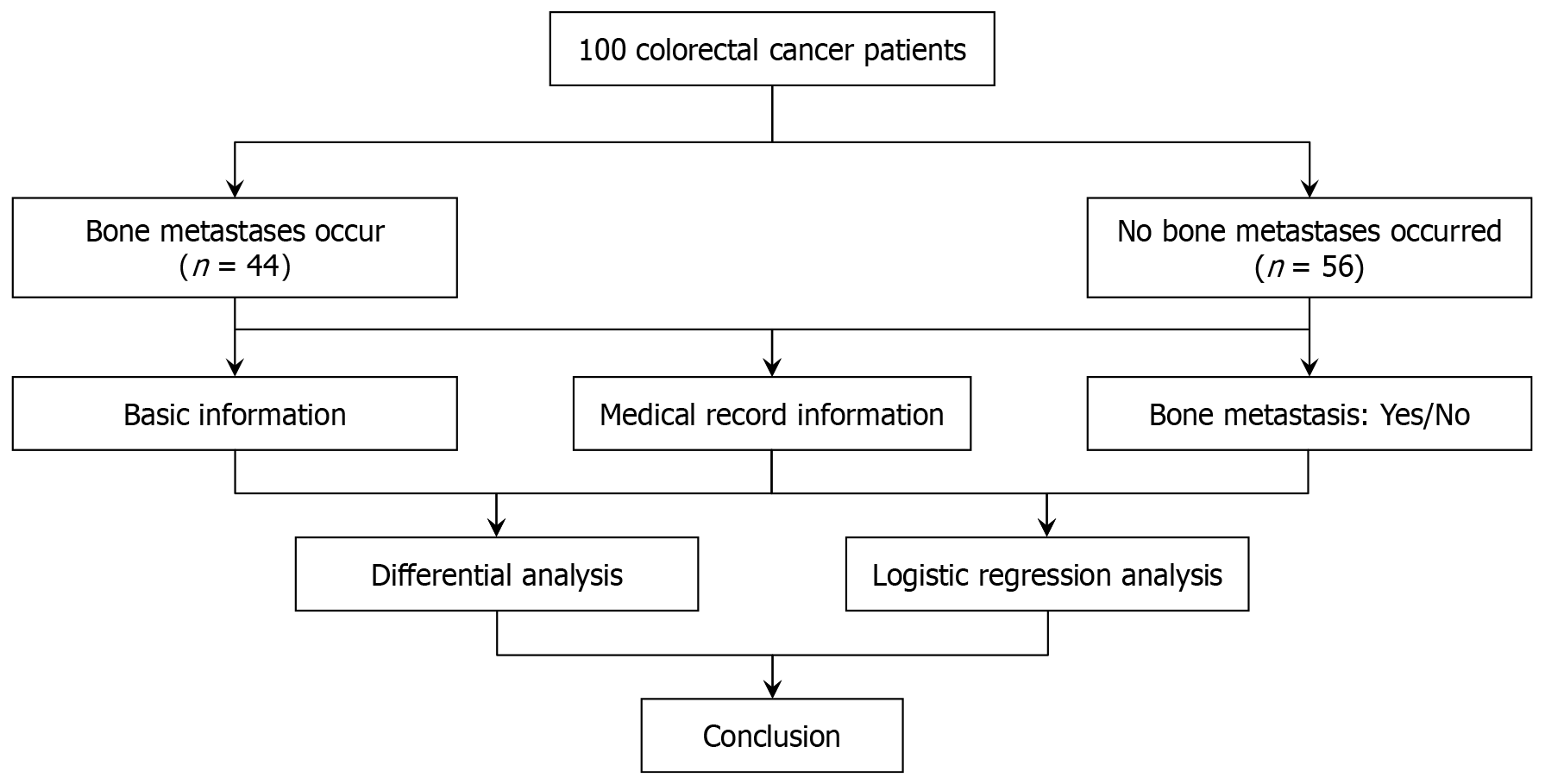
We selected 100 patients who underwent surgery for CRC and were admitted from February 2018 to February 2024, collected the general data of bone metastasis, and collected the pathological characteristics of patients with bone metastasis. Next, we divided them into groups with and without bone metastasis (Bone metastases group, n = 44; no bone metastases group, n = 56), compared the clinical data of the two groups, and analyzed the risk factors of bone metastasis using logistic regression analysis.
Among the 100 patients, the mean age was 54.33 ± 8.45 years, and most were male (54.55%). The proportion of patients with lytic bone changes was 43.18%. The most common location of combined bone metastasis was the pelvis, whereas only 5 patients had limb transfer. There was a higher incidence of lung than of pancreatic or liver metastases. Regression analysis showed that the primary location of the cancer was rectal cancer. Lymph node involvement, lung metastasis, and no postoperative chemotherapy were the risk factors for postoperative bone metastasis in patients who underwent surgery for CRC
Rectal cancer, lymph node involvement, complicated pulmonary metastasis, and no postoperative chemotherapy treatment can help predict high risk of bone metastasis in CRC.
Core Tip: Early identification of bone metastasis risk in colorectal cancer patients is critical, especially pre- and post-surgery. Targeted interventions for risk factors are essential. These may include bone-protecting drugs, dietary improvements, and exercise to boost bone health. Regular monitoring through imaging and tests helps detect early signs of bone metastasis, allowing for timely treatment and improved patient outcomes.
- Citation: Tang QY, Yu W. Logistic regression analysis of pathological features of bone metastasis in colorectal cancer and related influencing factors after surgery. World J Gastrointest Surg 2025; 17(4): 100851
- URL: https://www.wjgnet.com/1948-9366/full/v17/i4/100851.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v17.i4.100851
Colorectal cancer (CRC) is a prevalent malignancy in the digestive system, with a significant effect on global health. Recent epidemiological data indicate a rising trend in the incidence of bone metastasis among patients with CRC, which poses a substantial challenge to clinical management. Bone metastasis, occurring in a considerable subset of CRC cases, is associated with increased morbidity and reduced survival rates. Current research efforts are focused on identifying risk factors, understanding the molecular mechanisms, and developing targeted therapies to mitigate the effect of bone metastasis. Despite advancements, several challenges remain unresolved. These include the lack of early detection markers, the complexity of metastatic pathways, and the heterogeneity of patient responses to treatment. Furthermore, the limited understanding of the interaction between tumor cells and the bone microenvironment hinders the development of effective preventive and therapeutic strategies. Addressing these issues is crucial for improving patient outcomes and reducing the burden of CRC-associated bone metastasis.
At present, radical resection of CRC is the main way to cure it at an early stage[1]. However, some patients experienced cancer lesion recurrence, distant metastasis and postoperative metastasis of the lymph node, leading to surgical failure. The lung, liver, and pancreas are the main sites of cancer cell metastasis after CRC, whereas the incidence of bone metastasis is relatively rare[2,3]. However, with the continual aging of the population and the formation of bad national living habits, the risk of bone metastasis in patients with CRC after surgery has increased. If the risk factor of bone metastasis after CRC surgery can be identified, targeted intervention measures could be given earlier, which would help ensure the efficacy of surgery and postoperative recovery of patients. However, in previous studies, the description of the pathological characteristics of bone metastasis after CRC and the analysis of the risk factors leading to the occurrence of bone metastasis are rare. In view of this, the present study retrospectively analyzed the medical records of 100 patients undergoing CRC surgery in our hospital, summarized the pathological characteristics of bone metastasis in patients after CRC, and analyzed the risk factors.
This was a retrospective analysis of 100 patients with CRC admitted to the hospital from February 2018 to February 2024, including 64 men and 36 women, aged 34 to 68 years (mean age: 51.00 ± 11.25). All patients met the diagnostic criteria specified in the Spanish Society of Medical Oncology clinical guidelines for diagnosis and treatment of metastatic CRC (2018)[4]. Inclusion criteria were: (1) Patients could tolerate surgical treatment of rectal cancer; (2) Patients had not developed extensive tumor metastasis; and (3) Informed consent from patients and family members was obtained. Exclusion criteria were patients who had these characteristic: (1) Severe underlying disease and poor cardiopulmonary function; (2) Severe coagulation dysfunction that could not be corrected; (3) Tumors that had invaded the large vessels; (4) Large tumor volume and serious adhesion to surrounding tissues; (5) Mental diseases; (6) Estimated survival of < 3 months; or (7) Severe infection (Figure 1).
We selected 100 patients who underwent surgery for CRC and were admitted from February 2018 to February 2024. The data collection process involved a systematic review of medical records, with specific attention to the following steps and methods: (1) Selection of medical records: Medical records were selected based on the diagnosis of CRC and the treatment period specified (February 2023 to April 2024); (2) Initial screening: Records were initially screened to ensure they met the inclusion criteria, which included a confirmed diagnosis of CRC and completion of treatment within the specified time frame; and (3) Detailed review: Each selected record was reviewed in detail to extract relevant information. This process was conducted by trained medical personnel who were familiar with the specific data points required for the study.
The survey has strict quality control, and the investigators involved in the survey had received professional training. After pre-experiment, the internal consistency reliability Cronbach’s α coefficient of the general data of the survey was 0.83, and of each dimension was 0.62-0.84. The retest reliability was 0.82, 0.70-0.85, and the content validity was 0.93.
The observational indicators include: (1) Analysis of postoperative bone metastasis in patients undergoing CRC surgery; (2) Univariate analysis of affected postoperative bone metastases in patients undergoing CRC surgery. According to whether the patients developed bone metastasis, the 100 patients with CRC were divided into bone metastasis (n = 44) and no bone metastasis (n = 56) groups, and the medical records of the two groups were compared; and (3) Multivariate analysis of affected postoperative bone metastases in patients undergoing CRC surgery.
All the data of this study were entered into SPSS 25.0 for analysis, including the expression form n (%). The χ2-test was used to measure whether data conformed to a normal distribution, and the expression form was mean ± SD. We also used a t-test and risk factor analysis using the logistic multiple regression model. P < 0.05 represents a statistically significant difference.
Among the 100 patients with CRC who underwent surgical treatment, the incidence of bone metastasis was 44.0% (44/100). These patients’ age ranged from 45 to 63 years (mean age 54.33 ± 8.45). The clinical data of the two groups are shown in Table 1. In terms of the factors affecting the postoperative development of bone metastases, significant differences were observed in tumor primary location, postoperative chemotherapy, combined pulmonary metastasis, and lymph node involvement (P < 0.05) (Table 2). For items that showed differences in the univariate tables, the multiple logistic regression model showed that the primary location of tumor was the rectum. Complicated lymph node involvement, complicated lung metastasis, and no postoperative chemotherapy were other risk factors affecting postoperative bone metastasis (P < 0.05) (Tables 3 and 4).
| Items | Cases (n = 44) | Proportion, % | |
| Age, years | 54.33 ± 8.45 | ||
| Sex | Male | 24 | 54.55 |
| Female | 20 | 45.45 | |
| The primary location of the tumor | Colon | 11 | 25.00 |
| Rectum | 33 | 75.00 | |
| Tumor diameter, cm | 4.02 ± 1.02 | ||
| Osteopathic changes | Osteolytic | 19 | 43.18 |
| Osteogenic | 14 | 31.82 | |
| Mixed bone destruction | 11 | 25.00 | |
| Type of bone metastasis | Single type | 15 | 34.09 |
| Multiple type | 29 | 65.91 | |
| Infiltration depth | T1-T2 | 14 | 31.82 |
| T3-T4 | 30 | 68.18 | |
| Lymphatic metastasis | Yes | 29 | 65.91 |
| No | 15 | 34.09 | |
| Location of bone metastases | Skull | 8 | 18.18 |
| Pelvis | 18 | 40.91 | |
| Trunk | 6 | 13.64 | |
| Four limbs | 5 | 11.36 | |
| Spinal column | 7 | 15.91 | |
| Bone metastasis organs | Liver | 11 | 25.00 |
| Lung | 26 | 59.09 | |
| Pancreas | 7 | 15.91 |
| Variables | Bone metastases (n = 44) | No bone metastases (n = 56) | t/χ2 | P value | |
| Age | ≤ 60 | 24 (54.55) | 36 (64.29) | 0.974 | 0.324 |
| > 60 | 20 (45.45) | 20 (42.86) | |||
| Sex | Male | 24 (54.55) | 40 (71.43) | 3.048 | 0.081 |
| Female | 20 (45.45) | 16 (28.57) | |||
| The primary location of the tumor | Colon | 11 (25.00) | 30 (53.57) | 8.315 | 0.004 |
| Rectum | 33 (75.00) | 26 (46.43) | |||
| Tumor diameter | < 5 cm | 31 (70.45) | 34 (60.71) | 1.028 | 0.311 |
| ≥ 5 cm | 13 (29.55) | 22 (39.29) | |||
| Osteopathic changes | Osteolytic | 19 (43.18) | 15 (26.79) | 2.985 | 0.225 |
| Osteogenic | 14 (31.82) | 22 (39.29) | |||
| Mixed bone destruction | 11 (25.00) | 19 (33.93) | |||
| Infiltration depth | T1-T2 | 14 (31.82) | 27 (48.21) | 2.738 | 0.098 |
| T3-T4 | 30 (68.18) | 29 (51.79) | |||
| Postoperative chemotherapy | Yes | 11 (25.00) | 45 (80.36) | 30.644 | < 0.001 |
| No | 33 (75.00) | 11 (19.64) | |||
| Combined lung metastases | Yes | 26 (59.09) | 18 (32.14) | 7.262 | 0.007 |
| No | 18 (40.91) | 38 (67.86) | |||
| Concomitant liver metastasis | Yes | 11 (25.00) | 24 (42.86) | 3.454 | 0.063 |
| No | 33 (75.00) | 32 (57.14) | |||
| Concomitant pancreatic metastasis | Yes | 7 (15.91) | 11 (19.64) | 0.233 | 0.630 |
| No | 37 (84.09) | 45 (80.36) | |||
| Lymph node involvement | Yes | 29 (65.91) | 19 (33.93) | 10.096 | 0.002 |
| No | 15 (34.09) | 37 (66.07) |
| Independent variable | Assignment |
| The primary location of the tumor | “rectum” = 1, “colon” = 0 |
| Lymph node involvement | “yes” = 1, “no” = 0 |
| Pulmonary metastasis | “yes” = 1, “no” = 0 |
| Postoperative chemotherapy | “yes” = 1, “no” = 0 |
| Factor | Partial regression coefficient | SE | Wald | OR | 95%CI | P value |
| The primary location of the tumor was a rectal cancer | 1.128 | 0.322 | 17.527 | 2.456 | 1.644-3.674 | < 0.001 |
| With combined lymph node involvement | 1.144 | 0.311 | 10.214 | 2.024 | 1.159-3.654 | < 0.001 |
| Combined lung metastases | 1.134 | 0.241 | 14.327 | 3.124 | 2.124-5.544 | < 0.001 |
| No chemotherapy was administered after surgery | 1.412 | 0.224 | 21.236 | 3.544 | 1.664-6.922 | < 0.001 |
Bone metastasis, as a malignant tumor originating outside the bone tissue, is transferred to bone tissue, causing bone injury and pain[5]. At present, the clinically accepted mechanisms of bone metastasis include: (1) Primary tumor cells infiltrate the vasculature; (2) Tumor cells are released into the blood circulation; (3) Tumor cells stay in the vascular wall in the bone marrow; (4) Tumor cells overflow through endothelial cells and proliferate outside the vessels; and (5) Blood transport is established in the metastatic tumor cells, forming bone metastasis[6]. After bone metastasis, owing to symptoms such as pathological fracture and pain, patients experience adverse events such as limited limitation and decreased quality of life, which have a negative effect on the efficacy of surgery and their prognosis for recovery[7].
In this study, by compiling the pathological data of patients with bone metastasis following CRC in our hospital, we found that male patients with invasion of T 3 to T 4 were more likely to develop bone metastases[8,9]; the patients with bone metastases had osteolytic change and primary tumor of rectal cancer, 43.18% and 75.00%, respectively; and the incidence of patients with multiple bone metastases was higher than that of solitary bone metastases[10,11]. Through logistic regression analysis, we found that the primary location of tumor was rectal cancer, lung metastasis, no postoperative chemotherapy, and lymph node involvement were risk factors for bone metastasis in patients undergoing CRC surgery (P < 0.05).
To take these risk factors in turn: (1) The primary tumor site was rectal cancer. Because of the complex lymphatic reflux route of the rectum, the lower vein returns to the inferior vena cava, without a valve, leading to the characteristics of slow blood velocity. When tumor cells detach, they easily adhere to the location and form metastases[12-15]. The rectal lymphatic drainage for the inferior mesenteric artery lymph nodes is situated not only in the mesentery, but also laterally and below. When the drainage way is more complex, surgery is more difficult; thus, the postoperative risk for bone metastases of patients with rectal cancer is higher than that of those with colon cancer; (2) No postoperative chemotherapy: Postoperative adjuvant chemotherapy measures can eliminate the remaining lesions in the operation, and reduce the probability of recurrence and metastasis of cancer lesions in patients with CRC after surgery; (3) Lymph node involvement: Lymph nodes are one of the immune organs of the human body and can remove toxic and harmful substances. When tumor cells invade the body, the patient’s immune system is damaged, increasing the risk of immune disorders, induced lymphocyte dysplasia, and tumor metastasis; and (4) Lung metastasis: Because of the specific anatomy of the lung, when tumor cells invade the lung, they can then (through the lung) invade the shoulder blade, sternum, and (through the pulmonary vein) the left atrium, with systemic circulation as the path to the whole body. Thus, combined lung metastasis in CRC patients means higher probability of bone metastasis[16-18].
This study has some limitations. The study’s retrospective design and reliance on existing medical records may introduce selection bias and limit data accuracy. With only 100 patients, the sample size was small, potentially affecting the generalizability and statistical power of the findings. The study also lacked a specified follow-up duration for bone metastasis, which could influence the timing and detection of metastatic events. Additionally, the analysis did not account for potential confounding variables or variations in treatment modalities, which might affect the risk of bone metastasis. The study’s focus on patients with CRC may limit the applicability of the findings to other cancer types. Furthermore, the lack of functional outcome measures means the study did not assess the effect of bone metastasis on quality of life. Despite these limitations, our findings provide valuable insights into the risk factors for bone metastasis and highlights areas for further research.
Bone metastases are common in CRC patients with deeper tumor invasion, those with multiple osteolytic lesions, and those who have multiple bone metastases. The primary tumor location being the rectum, lymph node involvement, combined lung metastasis, and no postoperative chemotherapy are risk factors for postoperative bone metastasis in patients with CRC, and can contribute to the early clinical identification of the high risk of bone metastasis in these patients.
| 1. | Carli F, Bousquet-Dion G, Awasthi R, Elsherbini N, Liberman S, Boutros M, Stein B, Charlebois P, Ghitulescu G, Morin N, Jagoe T, Scheede-Bergdahl C, Minnella EM, Fiore JF Jr. Effect of Multimodal Prehabilitation vs Postoperative Rehabilitation on 30-Day Postoperative Complications for Frail Patients Undergoing Resection of Colorectal Cancer: A Randomized Clinical Trial. JAMA Surg. 2020;155:233-242. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 469] [Cited by in RCA: 408] [Article Influence: 68.0] [Reference Citation Analysis (0)] |
| 2. | Zhang Y, Zhang Z, Wei L, Wei S. Construction and validation of nomograms combined with novel machine learning algorithms to predict early death of patients with metastatic colorectal cancer. Front Public Health. 2022;10:1008137. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 34] [Cited by in RCA: 30] [Article Influence: 7.5] [Reference Citation Analysis (0)] |
| 3. | Gómez-España MA, Gallego J, González-Flores E, Maurel J, Páez D, Sastre J, Aparicio J, Benavides M, Feliu J, Vera R. SEOM clinical guidelines for diagnosis and treatment of metastatic colorectal cancer (2018). Clin Transl Oncol. 2019;21:46-54. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 46] [Cited by in RCA: 41] [Article Influence: 5.9] [Reference Citation Analysis (1)] |
| 4. | Han J, Wang Z, Dai Y, Li X, Qian Q, Wang G, Wei G, Zeng W, Ma L, Zhao B, Wang Y, Yang K, Ding Z, Hu X. [Preliminary report on prospective, multicenter, open research of selective surgery after expandable stent combined with neoadjuvant chemotherapy in the treatment of obstructive left hemicolon cancer]. Zhonghua Wei Chang Wai Ke Za Zhi. 2018;21:1233-1239. [PubMed] |
| 5. | Sastre J, Orden V, Martínez A, Bando I, Balbín M, Bellosillo B, Palanca S, Peligros Gomez MI, Mediero B, Llovet P, Moral VM, Viéitez JM, García-Alfonso P, Calle SG, Ortiz-Morales MJ, Salud A, Quintero G, Lopez C, Díaz-Rubio E, Aranda E; Spanish Cooperative Group for the Treatment of Digestive Tumors (TTD). Association Between Baseline Circulating Tumor Cells, Molecular Tumor Profiling, and Clinical Characteristics in a Large Cohort of Chemo-naïve Metastatic Colorectal Cancer Patients Prospectively Collected. Clin Colorectal Cancer. 2020;19:e110-e116. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 26] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 6. | Löffler MW, Nussbaum B, Jäger G, Jurmeister PS, Budczies J, Pereira PL, Clasen S, Kowalewski DJ, Mühlenbruch L, Königsrainer I, Beckert S, Ladurner R, Wagner S, Bullinger F, Gross TH, Schroeder C, Sipos B, Königsrainer A, Stevanović S, Denkert C, Rammensee HG, Gouttefangeas C, Haen SP. A Non-interventional Clinical Trial Assessing Immune Responses After Radiofrequency Ablation of Liver Metastases From Colorectal Cancer. Front Immunol. 2019;10:2526. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 36] [Cited by in RCA: 33] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 7. | Smedman TM, Guren TK, Line PD, Dueland S. Transplant oncology: assessment of response and tolerance to systemic chemotherapy for metastatic colorectal cancer after liver transplantation - a retrospective study. Transpl Int. 2019;32:1144-1150. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 27] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 8. | Shin AE, Giancotti FG, Rustgi AK. Metastatic colorectal cancer: mechanisms and emerging therapeutics. Trends Pharmacol Sci. 2023;44:222-236. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 522] [Cited by in RCA: 481] [Article Influence: 160.3] [Reference Citation Analysis (0)] |
| 9. | Li J, Ma X, Chakravarti D, Shalapour S, DePinho RA. Genetic and biological hallmarks of colorectal cancer. Genes Dev. 2021;35:787-820. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 461] [Cited by in RCA: 405] [Article Influence: 81.0] [Reference Citation Analysis (7)] |
| 10. | Biller LH, Schrag D. Diagnosis and Treatment of Metastatic Colorectal Cancer: A Review. JAMA. 2021;325:669-685. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2229] [Cited by in RCA: 1870] [Article Influence: 374.0] [Reference Citation Analysis (11)] |
| 11. | Baidoun F, Elshiwy K, Elkeraie Y, Merjaneh Z, Khoudari G, Sarmini MT, Gad M, Al-Husseini M, Saad A. Colorectal Cancer Epidemiology: Recent Trends and Impact on Outcomes. Curr Drug Targets. 2021;22:998-1009. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 240] [Cited by in RCA: 209] [Article Influence: 41.8] [Reference Citation Analysis (8)] |
| 12. | Patel SG, Karlitz JJ, Yen T, Lieu CH, Boland CR. The rising tide of early-onset colorectal cancer: a comprehensive review of epidemiology, clinical features, biology, risk factors, prevention, and early detection. Lancet Gastroenterol Hepatol. 2022;7:262-274. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 664] [Cited by in RCA: 554] [Article Influence: 138.5] [Reference Citation Analysis (6)] |
| 13. | Mahmoud NN. Colorectal Cancer: Preoperative Evaluation and Staging. Surg Oncol Clin N Am. 2022;31:127-141. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 97] [Cited by in RCA: 81] [Article Influence: 20.3] [Reference Citation Analysis (0)] |
| 14. | Zygulska AL, Pierzchalski P. Novel Diagnostic Biomarkers in Colorectal Cancer. Int J Mol Sci. 2022;23:852. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 224] [Cited by in RCA: 185] [Article Influence: 46.3] [Reference Citation Analysis (2)] |
| 15. | Eng C, Jácome AA, Agarwal R, Hayat MH, Byndloss MX, Holowatyj AN, Bailey C, Lieu CH. A comprehensive framework for early-onset colorectal cancer research. Lancet Oncol. 2022;23:e116-e128. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 192] [Cited by in RCA: 163] [Article Influence: 40.8] [Reference Citation Analysis (8)] |
| 16. | Fan A, Wang B, Wang X, Nie Y, Fan D, Zhao X, Lu Y. Immunotherapy in colorectal cancer: current achievements and future perspective. Int J Biol Sci. 2021;17:3837-3849. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 344] [Cited by in RCA: 319] [Article Influence: 63.8] [Reference Citation Analysis (8)] |
| 17. | Hampel H, Kalady MF, Pearlman R, Stanich PP. Hereditary Colorectal Cancer. Hematol Oncol Clin North Am. 2022;36:429-447. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 28] [Reference Citation Analysis (0)] |
| 18. | Kreidieh M, Mukherji D, Temraz S, Shamseddine A. Expanding the Scope of Immunotherapy in Colorectal Cancer: Current Clinical Approaches and Future Directions. Biomed Res Int. 2020;2020:9037217. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 40] [Cited by in RCA: 40] [Article Influence: 6.7] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/