Published online Apr 27, 2025. doi: 10.4240/wjgs.v17.i4.100617
Revised: January 22, 2025
Accepted: February 26, 2025
Published online: April 27, 2025
Processing time: 113 Days and 21.9 Hours
Laparoscopic surgery, with the advantage of less trauma, has been predominantly performed to treat pediatric inguinal hernia. However, the traditional three-port laparoscopic surgery remains extremely traumatic for children, whereas single-port laparoscopic surgery causes less damage to children than traditional laparo
To analyze the association of single-incision laparoscopic herniorrhaphy needle treatment with surgical outcomes, postoperative complications, and serum in
This retrospective study included 113 pediatric patients with inguinal hernia who underwent surgery at the Children’s Hospital, Capital Institute of Pediatrics, from April 2022 to May 2023. Participants were categorized into the observation group (single-incision laparoscopic herniorrhaphy needle, n = 60) and the control group (two-port laparoscopic surgery, n = 53). Comparative analyses involved surgical duration, intraoperative blood loss, and length of hospital stay. C-reactive protein (CRP) and white blood cell count (WBC) levels were measured preoperatively and 24 hours postoperatively. Postoperative pain was evaluated with the face, legs, activity, cry, and Consolability scale. Further, the incidence of complications, recurrence, and reoperation rates was assessed. Logistic regression was employed to determine independent risk factors related to poor prognosis.
The observation group demonstrated significantly reduced intraoperative blood loss and shorter hospitalization compared to the control group (P < 0.05). Both groups demonstrated increased CRP and WBC levels postoperatively, but the observation group exhibited significantly lower levels (P < 0.05). Further, pain scores at 24 hours postoperatively were significantly lower in the observation group (P < 0.05). Additionally, the observation group experienced fewer adverse events, recurrence rates, and reoperations compared to the control group (P < 0.05). Logistic regression analysis determined increased postoperative stress markers and surgical technique as inde
Single-incision laparoscopic herniorrhaphy needle treatment for pediatric inguinal hernia exhibits significant efficacy, effectively reduces postoperative complications, ensures a more concealed surgical incision, and promotes faster postoperative recovery than conventional two-port laparoscopy. This approach merits wider application.
Core Tip: Single-port laparoscopic hernia needle treatment of inguinal oblique hernia is less harmful to children and is conducive to their recovery immediately after surgery. A single-port laparoscopic hernia needle exhibits a milder inflammatory state than the two-port laparoscopy, with fewer adverse reactions. Increased postoperative stress indexes and surgical procedures are independent risk factors for recurrence in children.
- Citation: Wang XQ, Kong CH. Single-incision laparoscopic herniorrhaphy needle treatment for pediatric inguinal hernia: Surgical outcome, postoperative complications, and serum inflammation effects. World J Gastrointest Surg 2025; 17(4): 100617
- URL: https://www.wjgnet.com/1948-9366/full/v17/i4/100617.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v17.i4.100617
Pediatric indirect inguinal hernia is a prevalent clinical condition, particularly during the neonatal period. This condition originates from the underdeveloped and weakened abdominal wall structures in neonates. Activities that increase intra-abdominal pressure, such as crying or defecation, facilitate the descent of intestinal tissues into the scrotum, thereby forming an inguinal hernia[1,2]. Epidemiological data indicate a male-to-female incidence ratio of approximately 15: 1, with a higher prevalence on the right side. The primary etiological factor includes the congenital failure of the processus vaginalis to undergo complete closure[3]. Surgical intervention is the primary treatment for this condition. Without timely management, the hernia may progressively enlarge with the child’s growth, thereby increasing the risk of severe complications. These complications include herniated content incarceration, which causes ischemia of the intestines and omentum. This may progress to necrotizing bowel obstruction in extreme cases, posing significant morbidity risks[4,5].
In recent years, the continuous evolution of minimally invasive techniques has resulted in the widespread adoption of laparoscopic surgery in managing pediatric indirect inguinal hernia. This approach not only facilitates the determination of contralateral occult hernias but also significantly reduces surgical trauma, which provides improved protection of important structures, such as the fallopian tubes and spermatic vessels, thereby minimizing bodily harm[6,7].
However, traditional laparoscopic procedures typically require either three (a primary operative port, an auxiliary port, and an observation port) or two incisions (a primary operative port and an observation port), which still causes notable trauma for pediatric patients[8]. In contrast, single-port laparoscopic surgery, which involves a single small incision without additional ports, provides several advantages, including reduced trauma, accelerated postoperative recovery, and improved surgical outcomes. Hence, this technique has been gradually accepted in clinical practice[9].
Emerging evidence confirms the efficacy of single-port laparoscopic surgery in treating patent processus vaginalis in pediatric patients. In particular, previous studies have revealed its favorable therapeutic outcomes[10]. However, the procedure presents significant technical challenges, and research on its application for pediatric indirect inguinal hernia remains relatively limited, emphasizing the need for further investigation and improvement of this promising approach.
This study investigated the association of single-port laparoscopic hernia needle surgery with surgical outcomes, postoperative complications, and serum inflammatory markers in pediatric patients with indirect inguinal hernias to provide valuable reference data for its future clinical application.
This study retrospectively analyzed 113 pediatric patients with indirect inguinal hernia undergoing surgical treatment at Children’s Hospital Capital Institute of Pediatrics from April 2022 to May 2023. Patients were categorized based on surgical approach into the observation group (treated with a single-port laparoscopic hernia needle, n = 60) and the control group (treated with the two-port laparoscopic method, n = 53).
Inclusion criteria were patients: (1) Who were clinically diagnosed with indirect inguinal hernia through ultrasound examination; (2) Who had unilateral hernia; (3) Who met the surgical treatment standards; and (4) Who had complete medical records. Exclusion criteria were patients: (1) Who did not meet surgical treatment standards; (2) Who had severe hepatic or renal dysfunction; (3) Who were diagnosed with other malignant tumors; and (4) Who had immune deficiency disorders.
All patients underwent comprehensive preoperative assessments, including blood tests, coagulation tests, cardiac ultrasound, electrocardiogram, and chest X-ray. This study excluded patients who did not meet surgical treatment criteria. All patients received general anesthesia in a supine position. A 0.5-cm incision was created at the umbilicus, through which a 5-mm Trocar was inserted to establish pneumoperitoneum with an intra-abdominal pressure maintained at 8-10 mmHg, which served as the observation port.
The control group underwent two-port laparoscopic treatment. A 3-mm incision was created on the right abdominal wall near the umbilicus or slightly lower. A 2-0 non-absorbable suture with a needle was used to puncture the peritoneum under the thin right abdominal wall. The needle was guided through the peritoneum’s outer interlayer using an operating clamp, which encircles once around the internal ring, thereby expelling gas from the hernia sac. The suture was tightened and tied distally after ensuring complete closure of the internal ring. The umbilical incision was sutured, and the other incision was closed with adhesive tape to reduce tension and prevent scar hyperplasia.
Patients in the observation group underwent single-incision laparoscopic herniorrhaphy using a specialized needle technique. The procedure started by creating a 1-mm incision at the projected location of the internal inguinal ring on the abdominal wall. A dura mater puncture needle preloaded with a 2-0 non-absorbable suture was inserted perpendicularly through the incision, which advanced to the outer interlayer of the peritoneum. The needle was guided beneath the fallopian tube and spermatic vein to pierce the peritoneum, leaving the suture within the abdominal cavity.
The needle was then carefully withdrawn to the outer interlayer of the peritoneum and reinserted through the opposite side of the internal ring. The suture was retrieved and pulled out of the body to achieve a complete internal inguinal ring closure while ensuring proper air evacuation from the hernia sac. The suture was securely tied externally, with the ends buried subcutaneously. To evaluate for contralateral occult hernias, the procedure was repeated if required. The laparo
Both the observation and control groups received standardized postoperative care, which included rehabilitation training, pharmacological interventions, and other management measures, to ensure optimal recovery.
(1) Surgical parameters: Surgical duration, intraoperative blood loss, and hospital stay were compared between the two pediatric cohorts; (2) Stress response indicators: C-reactive protein (CRP) and white blood cell (WBC) levels were measured preoperatively and 24 hours postoperatively for both groups; (3) Pain assessment: Postoperative pain was assessed using the face, legs, activity, cry, and Consolability scale[11], which evaluates five behavioral indicators-facial expression, leg movement, activity level, crying, and consolability-each scored on a 0-2 scale, with a total score ranging from 0 to 10. Scores of > 7 indicate severe pain, 3-7 denote moderate pain, and < 3 represent mild pain; (4) Postoperative complications: The occurrence of postoperative complications, including incision infections, scrotal edema, hydrocele, and subcutaneous edema, was recorded and compared between groups; (5) Follow-up analysis: A 6-month follow-up was conducted to evaluate and compare recurrence and reoperation rates between the two groups; and (6) Prognostic evaluation: Patients were categorized into good and poor prognosis groups based on recurrence outcomes. Logistic regression analysis was conducted to determine independent predictors of poor prognosis.
Statistical package for the social sciences version 19.0 software was used for statistical analysis, and GraphPad 7 software was utilized for graphical representation. Count data were expressed as percentages and analyzed using χ2 tests. Further, intergroup comparisons were conducted using independent t-tests. Pre- and post-treatment comparisons were performed using paired t-tests. Logistic regression analysis was conducted to identify independent predictors of poor prognosis. Statistical significance was set at a P-value of < 0.05.
The two groups of pediatric patients demonstrated comparable baseline characteristics, with no statistically significant differences in terms of gender, age, body mass index, or disease staging (P > 0.05, Table 1).
| Variable | Observation group (n = 60) | Control group (n = 53) | χ2 | P value |
| Gender | 0.022 | 0.883 | ||
| Male | 32 (52.33) | 29 (54.72) | ||
| Female | 28 (46.67) | 24 (45.28) | ||
| Age (years) | 0.228 | 0.633 | ||
| ≥ 7 | 29 (48.33) | 28 (52.83) | ||
| < 7 | 31 (51.67) | 25 (47.17) | ||
| BMI (kg/m2) | 0.029 | 0.864 | ||
| ≥ 18 | 33 (55.00) | 30 (56.60) | ||
| < 18 | 27 (45.00) | 23 (43.40) | ||
| Disease duration (years) | 0.001 | 0.987 | ||
| ≥ 1 | 25 (41.67) | 22 (41.51) | ||
| < 1 | 35 (53.33) | 31 (58.49) | ||
| Affected area | 0.006 | 0.939 | ||
| Left side | 31 (51.67) | 27 (50.94) | ||
| Right side | 29 (48.33) | 26 (49.06) |
Surgical duration was not significantly different between the observation and control groups (P > 0.05). Conversely, patients in the observation group experienced significantly less intraoperative blood loss and shorter hospital stays than those in the control group (P < 0.05, Table 2).
| Variable | Observation group (n = 60) | Control group (n = 53) | t | P value |
| Operation time | 27.37 ± 1.03 | 27.16 ± 1.01 | 1.091 | 0.277 |
| Intraoperative blood loss | 3.3 ± 0.24 | 5.31 ± 0.25 | 43.57 | < 0.001 |
| Hospitalization time | 2.13 ± 0.34 | 5.23 ± 0.47 | 40.49 | < 0.001 |
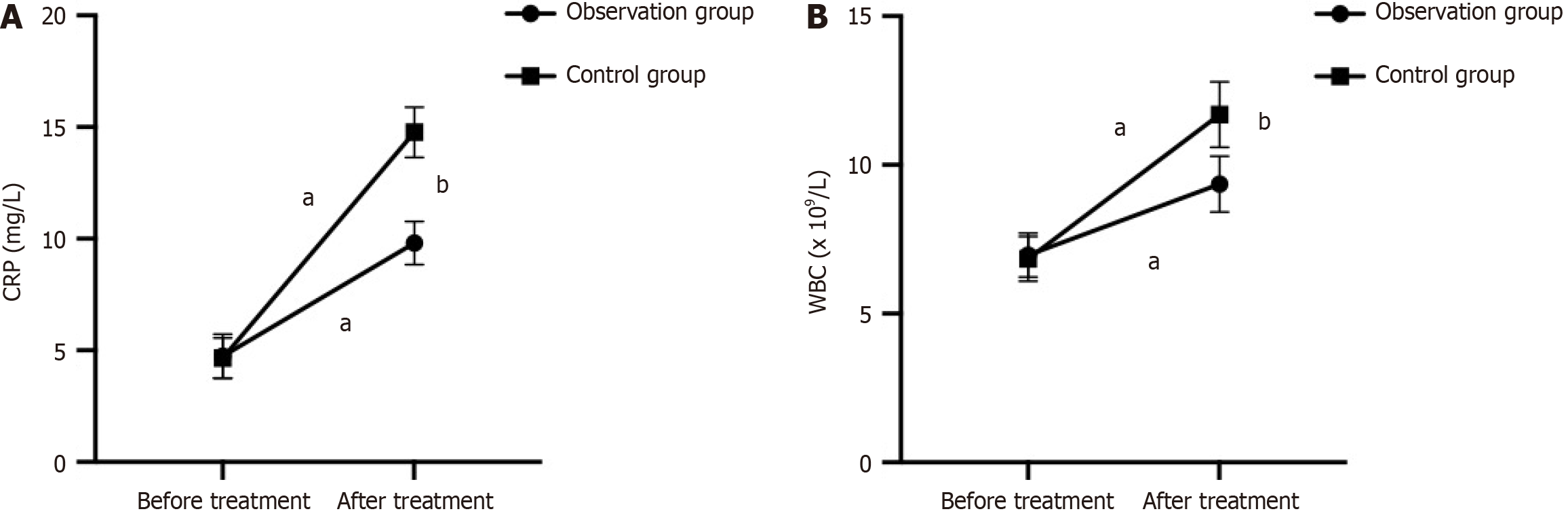
Preoperative CRP and WBC levels were comparable between the observation and control groups (P > 0.05). Both groups demonstrated higher CRP and WBC levels postoperatively than at baseline. However, the observation group demonstrated significantly lower CRP and WBC levels than the control group 24-hour postoperatively (P < 0.05, Figure 1).
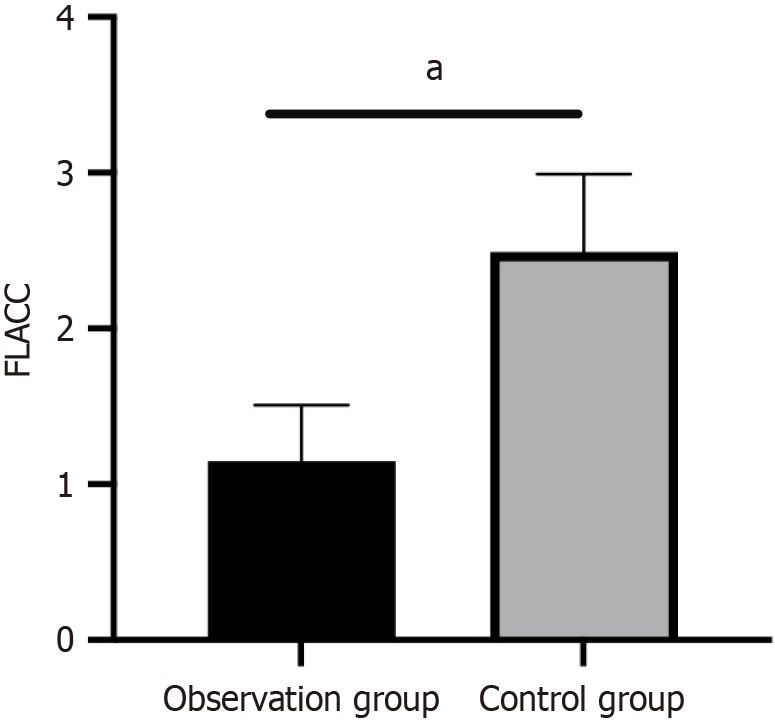
The 24-hour postoperative pain score for the observation group was 1.15 ± 0.36 points, which was significantly lower than the control group at 2.49 ± 0.5 points (P < 0.05, Figure 2).
The observation group demonstrated significantly lower complication rates (5.00%) than the control group (22.64%, P < 0.05). Further, specific complications, which included incision infection, scrotal edema, scrotal effusion, and subcutaneous edema, occurred less frequently in the observation group (Table 3).
| Variable | Observation group (n = 60) | Control group (n = 53) | χ2 | P value |
| Wound infection | 0 | 4 (7.55) | - | - |
| Scrotal edema | 2 (3.33) | 3 (5.66) | - | - |
| Scrotal effusion | 1 (1.67) | 3 (5.66) | - | - |
| Subcutaneous edema | 0 | 2 (3.77) | - | - |
| Total incidence | 3 (5.00) | 12 (22.64) | 7.608 | 0.006 |
A 6-month follow-up indicated significantly lower recurrence and reoperation rates in the observation group than in the control group (P < 0.05, Table 4).
| Variable | Observation group (n = 60) | Control group (n = 53) | χ2 | P value |
| Recurrence | 13 (21.67) | 22 (41.51) | 5.183 | 0.022 |
| Second surgery | 8 (13.33) | 17 (32.08) | 5.737 | 0.017 |
Pediatric patients were categorized into the good- and poor-prognosis groups based on recurrence status. Logistic regression analysis was conducted to identify independent risk factors related to poor prognosis. Univariate analysis revealed significant differences in terms of postoperative stress markers, and surgical technique between the two groups
| Variable | Good prognosis group (n = 78) | Poor prognosis group (n = 35) | χ2 | P value | |
| Gender | 0.739 | 0.390 | |||
| Male (n = 61) | 40 (51.28) | 21(60.00) | |||
| Female (n = 52) | 38 (48.72) | 14 (40.00) | |||
| Age (years) | 0.911 | 0.340 | |||
| ≥ 7 (n = 57) | 37 (47.44) | 20 (57.14) | |||
| < 7 (n = 56) | 41 (52.56) | 15 (42.86) | |||
| BMI (kg/m2) | 0.371 | 0.543 | |||
| ≥ 18 (n = 63) | 42 (53.85) | 21 (60.00) | |||
| < 18 (n = 50) | 36 (46.15) | 14 (40.00) | |||
| Disease duration (years) | 0.033 | 0.855 | |||
| ≥ 1 (n = 47) | 32 (41.03) | 15 (42.86) | |||
| < 1 (n = 66) | 46 (58.97) | 20 (57.14) | |||
| Stress response index | |||||
| CRP | 11.48 ± 2.54 | 13.6 ± 2.47 | 4.137 | < 0.001 | |
| WBC | 10.00 ± 1.45 | 11.47 ± 1.25 | 5.191 | < 0.001 | |
| Surgical plan | 5.183 | 0.023 | |||
| Two-port laparoscopic hernia needle (n = 53) | 31 (39.74) | 22 (62.86) | |||
| Single-port laparoscopic hernia needle (n = 60) | 47 (60.26) | 13 (37.14) |
| Variable | β | SE | Wals | P value | Exp(B) | 95%CI | |
| Lower limit | Upper limit | ||||||
| CRP | 0.244 | 0.099 | 6.040 | 0.014 | 1.277 | 1.051 | 1.551 |
| WBC | 0.705 | 0.195 | 12.123 | 0.000 | 2.024 | 1.382 | 2.964 |
| Surgical plan | -1.923 | 0.543 | 12.541 | 0.000 | 0.146 | 0.050 | 10.424 |
Inguinal hernia, which includes direct and indirect hernias, is a prevalent condition in general surgery. Indirect inguinal hernias are particularly predominant in pediatric and young adult populations and are characterized by abdominal content protrusion through the inguinal canal, with potential extension into the scrotum. This makes them especially susceptible to complications such as incarceration[12]. Indirect inguinal hernia cannot resolve spontaneously and exhibits limited responsiveness to pharmacological treatment, requiring surgical intervention as the primary therapeutic approach, unlike some conditions. Traditional open abdominal surgery has been predominantly used, but it is associated with significant surgical trauma, which hinders recovery, particularly in pediatric patients[13].
The development and improvement of minimally invasive techniques have revolutionized the surgical management of pediatric indirect inguinal hernia. Laparoscopic surgery has been popular because of its multiple advantages, including reduced postoperative pain, smaller incisions, and improved preservation of critical anatomical structures such as the iliac and hypogastric nerves, spermatic vessels, inguinal nerves, and fallopian tubes[14,15]. Furthermore, laparoscopy provides the distinct advantage of determining occult hernias, thereby reducing the risk of missed diagnoses. One of the challenges in the surgical management of pediatric indirect inguinal hernia is the possibility of recurrence, which is largely affected by the completeness of internal inguinal ring closure. Laparoscopic surgery provides superior visualization of the spermatic cord and internal ring, thereby facilitating precise high hernial sac ligation. This improved accuracy not only enhances surgical outcomes but also minimizes recurrence rates.
This study assessed the efficacy and safety of single-port laparoscopic herniorrhaphy compared to conventional two-port laparoscopic surgery in pediatric patients with indirect inguinal hernia. The results revealed that the observation group undergoing single-port laparoscopic herniorrhaphy experienced significantly reduced intraoperative blood loss and shorter hospital stays than the control group, indicating that this approach causes less surgical trauma and promotes faster postoperative recovery.
The advantages of single-port laparoscopic herniorrhaphy originate from its minimally invasive design. Traditional two-port laparoscopic surgery involves inserting two to three trocars as operating and observation ports, which increases procedural complexity and associated tissue damage[16]. In contrast, the single-port technique uses a dura mater puncture needle for high hernial sac ligation, which consolidates the operating and observation functions into a single-port. This reduces trauma and visible scarring. Furthermore, the procedure requires only one trocar, and the laparoscope was used to magnify internal structures, enabling precise and efficient internal inguinal ring closure with circular sutures subcutaneously tied outside the body[17].
Previous studies have reported the benefits of single-port laparoscopy in appendectomy, demonstrating shorter hospital stays and lower rates of wound infections compared to conventional methods[18]. These results are congruent with our conclusions, highlighting the advantages of single-port laparoscopic surgery. However, our study represents the first comprehensive and detailed evaluation of its application in pediatric indirect inguinal hernia. Some researchers have proposed bilateral approaches near the umbilicus to minimize visible scarring, but the proximity and parallel alignment of surgical instruments and the laparoscope pose technical challenges, thereby limiting its feasibility and broader clinical adoption. Therefore, the single-port approach provides a viable, efficient, and less invasive alternative for pediatric hernia repair.
Laparoscopic surgery is recognized for its minimally invasive nature while inevitably inducing various degrees of surgical trauma. The early inflammatory response serves as a crucial indicator of the extent of tissue injury. To further investigate the effect of single-port laparoscopic herniorrhaphy on pediatric patients, we compared stress biomarkers and postoperative complications between the observation and control groups.
CRP, a key acute-phase reactant that is synthesized in the liver, is significantly increased in response to stress stimuli[19]. Its levels correlate with acute tissue injury, where higher concentrations indicate greater damage. CRP levels decrease rapidly as inflammation resolves, making it a sensitive, although non-specific, marker for tissue injury[20,21].
WBCs, which are central to the immune response, contribute to both innate and adaptive immunity. Leukocyte extravasation is a hallmark of the inflammatory process[22]. Our results revealed that postoperative CRP and WBC levels increased significantly in both groups. However, these elevations were markedly lower in the observation group, indicating that both surgical approaches provoke inflammatory responses, but single-port laparoscopic herniorrhaphy exerts a milder inflammatory state. This attenuation may be related to the decreased number of surgical ports, causing less tissue trauma and a diminished stress response[23].
Furthermore, our results indicated significantly lower recurrence and reoperation rates in the observation group than in the control group. This indicates that both surgical techniques are effective in treating pediatric indirect inguinal hernia, but single-port laparoscopic herniorrhaphy provides superior outcomes in terms of recurrence and reoperation rates. The improved efficacy of single-port laparoscopic herniorrhaphy may originate from its ability to detect contralateral occult hernias and achieve a more comprehensive high hernial sac ligation, thereby reducing the risk of recurrence and the need for subsequent surgical interventions[24].
Finally, to further determine factors that affect prognosis, we categorized children into the good and poor prognosis groups based on recurrence and analyzed independent risk factors for recurrence. Increased postoperative stress indicators were considered independent risk factors for recurrence, possibly associated with increased infection, although the exact mechanism warrants further investigation. Conversely, single-port laparoscopic herniorrhaphy was an inde
In summary, single-port laparoscopic herniorrhaphy for pediatric indirect inguinal hernia exhibits significant efficacy, effectively reduces postoperative complications, provides more concealed incisions, and promotes faster recovery compared to conventional two-port laparoscopy. Thus, it is worth promoting. However, the study’s limited sample size and single comparison method may introduce bias, requiring further research.
| 1. | Yeap E, Pacilli M, Nataraja RM. Inguinal hernias in children. Aust J Gen Pract. 2020;49:38-43. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 29] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 2. | Zhao J, Yu C, Lu J, Wei Y, Long C, Shen L, Lin T, He D, Wei G, Kou L, Wu S. Laparoscopic versus open inguinal hernia repair in children: A systematic review. J Minim Access Surg. 2022;18:12-19. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 22] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 3. | Schmedding A, Alsweed A, Muensterer O, Leonhardt J. The Status of Laparoscopic Inguinal Hernia Surgery in Children: A Nationwide Assessment. Children (Basel). 2022;9. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 10] [Reference Citation Analysis (0)] |
| 4. | Olesen CS, Andersen K, Öberg S, Deigaard SL, Rosenberg J. Timing of inguinal hernia repair in children varies greatly among hernia surgeons. Dan Med J. 2020;68. [PubMed] |
| 5. | Chongxi R, Hongqiao W, Fengying L, Xin W, Hongxia Q, Lijun X. Single-incision approach for bilateral inguinal hernia repair in children: A retrospective study. Medicine (Baltimore). 2020;99:e19376. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 6. | Pelizzo G, Bernardi L, Carlini V, Pasqua N, Mencherini S, Maggio G, De Silvestri A, Bianchi L, Calcaterra V. Laparoscopy in children and its impact on brain oxygenation during routine inguinal hernia repair. J Minim Access Surg. 2017;13:51-56. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 21] [Article Influence: 2.3] [Reference Citation Analysis (1)] |
| 7. | Kara YA, Yağız B, Balcı Ö, Karaman A, Özgüner İF, Karaman İ. Comparison of Open Repair and Laparoscopic Percutaneous Internal Ring Suturing Method in Repairing Inguinal Hernia in Children. Cureus. 2021;13:e14262. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 9] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 8. | Hang T, Ma Q, Hong Z, Wang J, Ling Z, Lin H. Single-port laparoscopy-assisted trans-scrotal hernia sac ligation for pediatric male inguinal hernia. Front Surg. 2022;9:944004. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 9. | Hernández-Rodríguez RA, Rosell Echevarría MJ, Ravelo Díaz FD, Villamil V, Pérez-Etchepare Figueroa EL. Mid- to long-term results of SuPerLap single-port treatment in inguinal hernia. Cir Pediatr. 2022;35:14-17. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 10. | Li G, Gao H, Yu S, Guo Y, Hu T, Liu Y, Du G, Huang G, Zhang W. Single-port robotic-assisted laparoscopic synchronous surgery in pediatric patent processus vaginalis. BMC Surg. 2024;24:109. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 11. | Turco A, Cerulo M, Del Conte F, Coppola V, Severino G, Escolino M, Esposito C. Correlation between FLACC scale score and analgesic requirement in children undergoing Minimally Invasive Surgery. Pediatr Med Chir. 2023;45. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 12. | Haggui B, Hidouri S, Ksia A, Mosbahi S, Messaoud M, Sahnoun L, Mekki M, Belghith M, Nouri A. Femoral hernia in children: How to avoid misdiagnosis? Afr J Paediatr Surg. 2021;18:164-167. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 13. | Kabbani OM, Alhabdan KA, Almahbub AY, Kabbani NM, Ardah HI, Mahmoud AHM. Comparison of Postoperative Outcome in Children Undergoing Inguinal Hernia Repair Using Regional With General Versus General Anesthesia Alone: A Single Center Study. Cureus. 2023;15:e37382. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 14. | Risteski T, Memeti S. Benefits of Contralateral Patent Processus Vaginalis Closure During Laparoscopic Surgery for Inguinal Hernia in Female Children. Pril (Makedon Akad Nauk Umet Odd Med Nauki). 2022;43:69-75. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 15. | Hoyuela C, Juvany M, Carvajal F. Single-incision laparoscopy versus standard laparoscopy for colorectal surgery: A systematic review and meta-analysis. Am J Surg. 2017;214:127-140. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 43] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 16. | Li Y, Jin Z, Tang C, Gong Y, Huang L, Du Q, Xia X, Zhu D, Zhou W, Li Z, Wang W, Liu Y, Zheng Z. Comparison of trans-umbilical single-port laparoscopic complete extraperitoneal closure and laparoscopic intracorporeal closure for pediatric inguinal hernia: a randomized controlled study. Front Pediatr. 2024;12:1509895. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 17. | He CS, Su Y, Liu MX, Qin YB, Ji YH, Huang WQ, Huang GZ, Yang GZ, Hu ZL, Li SL. Causes of recurrence of paediatric inguinal hernia after single-port laparoscopic closure. Pediatr Surg Int. 2024;40:49. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Cited by in RCA: 9] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 18. | Cirocchi R, Cianci MC, Amato L, Properzi L, Buononato M, Di Rienzo VM, Tebala GD, Avenia S, Iandoli R, Santoro A, Vettoretto N, Coletta R, Morabito A. Correction: Laparoscopic appendectomy with single port vs conventional access: systematic review and meta-analysis of randomized clinical trials. Surg Endosc. 2024;38:2305. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 19. | Chen R, Tang S, Lu Q, Zhang X, Zhang W, Chen Z, Qi S. A 9-year experience study of single-port micro-laparoscopic repair of pediatric inguinal hernia using a simple needle. Hernia. 2020;24:639-644. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 11] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 20. | Prassas D, Rolfs TM, Vaghiri S, Kounnamas A, Knoefel WT, Krieg A. Single-port versus multi-port totally extraperitoneal (TEP) inguinal hernia repair: A meta-analysis of randomized controlled trials. Medicine (Baltimore). 2022;101:e30820. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |
| 21. | Li X, Hu X, Hu Y, Jie Y. Single-port versus traditional three-port laparoscopic total extraperitoneal inguinal hernia repair: A single-centre, prospective, randomised study. J Int Med Res. 2024;52:3000605241257418. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 7] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 22. | Ma Y, Cai J, Li S, Wang W, Liu L. Single-Port Laparoscopic Assisted Transcrotal Orchidopexy for Palpable Inguinal Canalicular Cryptorchidism Accompany With Indirect Inguinal Hernia. Front Pediatr. 2018;6:293. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 9] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 23. | Fazeli A, Davari HA, Hosseinpour M. A Modified Approach for Single-Port Laparoscopic Repair of Inguinal Hernias in Children. Adv Biomed Res. 2020;9:63. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 5] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 24. | Zhang L, Zhang R, Zhang J, Hu H, Chen Z, Fu Y, Li S. To use a simple hernia needle for single-port laparoscopic percutaneous inguinal hernia repair in children: a 5-year experience study. Front Pediatr. 2023;11:1298643. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 6] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/