Published online Mar 27, 2025. doi: 10.4240/wjgs.v17.i3.102543
Revised: December 22, 2024
Accepted: January 14, 2025
Published online: March 27, 2025
Processing time: 126 Days and 2.7 Hours
Gastroparesis is a chronic motility disorder characterized by delayed gastric emptying in the absence of mechanical obstruction. Patients with refractory gastroparesis often require enteral nutrition support, but traditional feeding methods such as nasojejunal tubes and percutaneous gastrojejunostomy tubes have significant limitations including frequent displacement, infection, and im
To explore patients’ experience post insertion of laparoscopic Roux-en-Y jeju
Eight patients with idiopathic gastroparesis who underwent Roux-en-Y jeju
Post-procedure, all patients reported improvements in nausea/vomiting, and 87.5% noted reduced abdominal pain. Weight stabilized and oral intake improved in 75% of patients. Most (87.5%) described improved social confidence, increased energy, and better work/school functioning. Three patients (37.5%) eventually maintained adequate oral nutrition without jejunostomy. Minor complications included leakage (37.5%) and hypergranulation tissue. Half the cohort used supplemental gastric venting. Most patients (87.5%) preferred Roux-en-Y jejunostomy over previous feeding tubes and would undergo the procedure again.
Despite some challenges, Roux-en-Y jejunostomy led to notable improvements in symptoms, nutrition, and quality of life for most patients with refractory gastroparesis. It may be a viable option for long-term enteral nutrition support in carefully selected patients. Further research is needed to optimize patient selection and manage complications.
Core Tip: This qualitative study provides novel insights into patient experiences with Roux-en-Y jejunostomy for refractory gastroparesis. While traditional feeding tubes often have limitations, this surgical approach showed promising outcomes for symptom control and quality of life. Notable findings improvement and/or resolution of nausea/vomiting in most patients, with 37.5% eventually maintaining adequate oral nutrition without jejunostomy. The study highlights the potential of Roux-en-Y jejunostomy as a viable long-term feeding option in carefully selected patients, while also identifying ongoing challenges such as leakage and hypergranulation tissue that require proactive management.
- Citation: Salehi O, Gao WL, Kenfield C, Hebbard G. Roux-en-Y jejunostomy in gastroparesis: Insight into patient perspectives and outcomes. World J Gastrointest Surg 2025; 17(3): 102543
- URL: https://www.wjgnet.com/1948-9366/full/v17/i3/102543.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v17.i3.102543
Gastroparesis is a debilitating gastrointestinal disorder characterized by delayed gastric emptying in the absence of mechanical obstruction resulting in abdominal pain, nausea, vomiting, early satiety and postprandial fullness[1,2]. It can lead to malnutrition and repeated hospitalizations[3-5]. While the aetiology of gastroparesis can be attributed to various underlying diseases such as autonomic neuropathy due to diabetes, connective tissue disorders or post-surgical complications, a subset of patients present with idiopathic gastroparesis where the exact aetiology remains elusive[6]. In the absence of an identifiable cause, management of idiopathic gastroparesis can be difficult. Initial strategies include dietary modification, analgesia, use of antiemetics and prokinetics to promote gastric emptying[7,8]. If these interventions are insufficient to maintain a patient’s weight, enteral nutrition may be used to ensure adequate caloric intake[9].
While various methods of enteral nutrition are available including nasogastric, nasojejunal, percutaneous endoscopic gastrostomy with a jejunal extension (percutaneous endoscopic transgastric jejunostomy), they have limitations in tolerability and quality of life impact[9,10]. Surgical jejunostomy is an alternate option but is more invasive and can be associated with complications including leakage, infection and dislodgement which has been described in other patient cohorts requiring enteral nutrition[11-13]. There has been little research exploring subjective experience post jejunostomy insertion in patients with gastroparesis.
In paediatric patients with delayed gastric emptying, Roux-en-Y jejunostomy has been shown to be an effective, safe, and well-tolerated surgical procedure for providing long-term enteral nutrition compared to other enteral feeding tubes[14]. It has been demonstrated to improve nutritional status, promote weight gain, and reduce symptoms associated with delayed gastric emptying in children[15]. There is minimal literature exploring patient experience in adults undergoing this procedure with gastroparesis. In our cohort, patients were also offered insertion of a venting gastrostomy which can be effective in managing symptoms in patients with gastroparesis[16,17]. The aim of this study is to explore patient experience post insertion of laparoscopic Roux-en-Y jejunostomy in a cohort of eight adult patients with idiopathic gastroparesis.
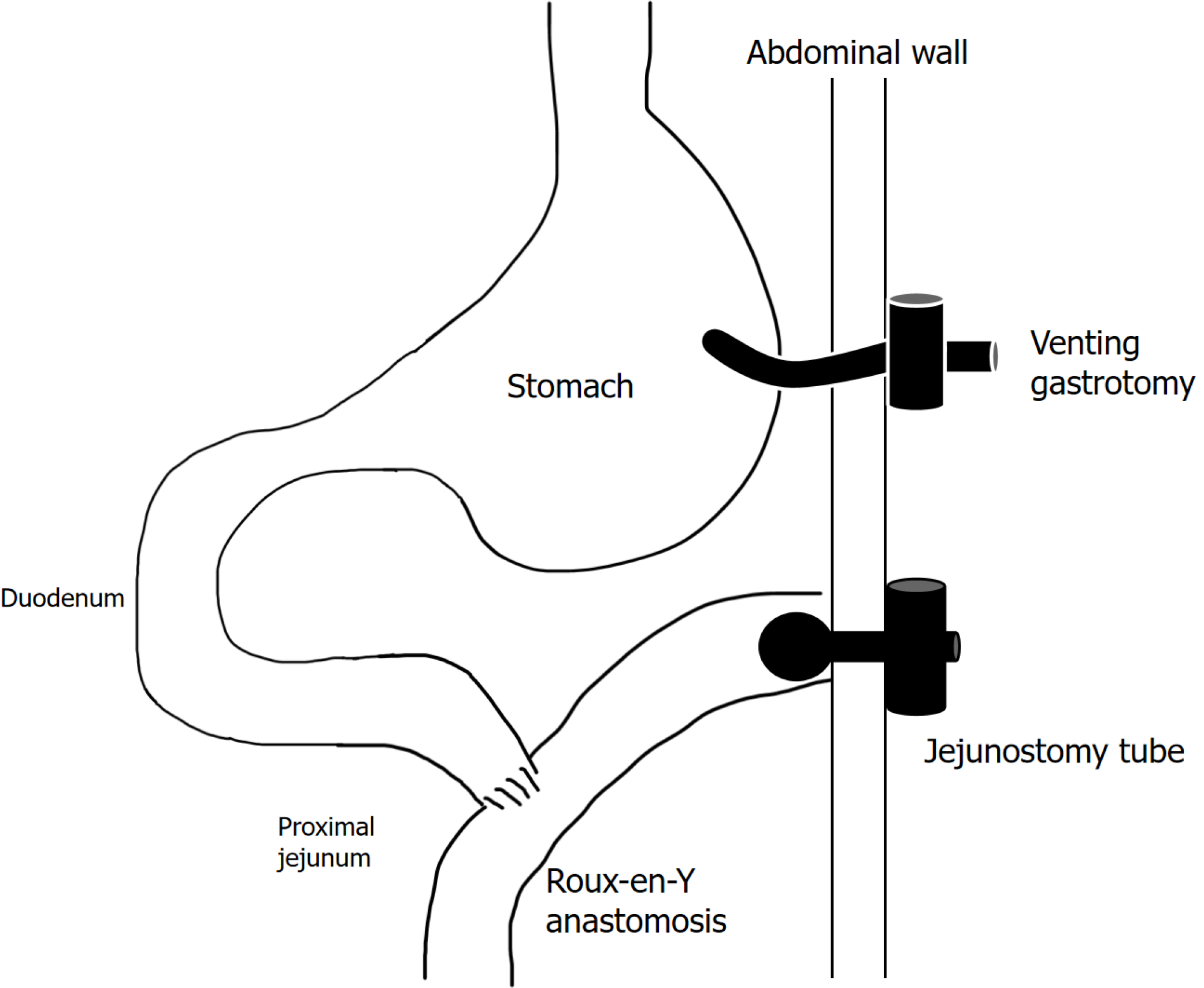
The procedure involves creating a jejunal limb approximately 15-40 cm distal to the ligament of Treitz, which is then anastomosed to the proximal jejunum in a Y-configuration as shown in Figure 1. This allows for the direct delivery of nutrients into the jejunum, bypassing the stomach. The Roux-en-Y anastomosis is combined with bringing the jejunal loop to the abdominal wall, where a jejunostomy feeding tube is inserted. This configuration helps to divert intestinal contents away from the stoma and reduce leakage as well as easier tube replacement. The procedure is designed to provide long-term enteral nutrition support while minimising complications associated with other feeding tube methods. By bypassing the dysfunctional stomach in patients with delayed gastric emptying, the Roux-en-Y jejunostomy promotes improved nutrient absorption and symptom relief. The jejunostomy feeding tube allows for easy and direct access to the jejunum for feeding and medication administration. Four patients also had a venting gastrostomy inserted to allow for enhanced drainage of gastric contents minimising post prandial nausea and fullness. The decision for concurrent venting gastrostomy placement was based on: (1) Severity of pre-operative nausea/vomiting symptoms; (2) Prior response to temporary nasogastric decompression; (3) Degree of gastric retention on imaging; and (4) Patient preference after counselling regarding additional tube management requirements.
Patients remained nil by mouth for 24 hours post-procedure. Tube feeding was initiated at 10 mL/hour and gradually increased based on tolerance. Initial feeding regimens utilized peptide-based formula, transitioning to polymeric feeds if tolerated. Feeding rates and schedules were individualized based on symptoms and nutritional requirements. Early mobilization and oral hygiene care were emphasized. Patients received structured education on tube care, feeding techniques, and complication recognition before discharge. Regular follow-up occurred at weeks 2, 6, and 12 post-procedure, then ever 3-12 months depending on patient progress.
This was a retrospective qualitative study exploring the experiences of eight patients with idiopathic gastroparesis who underwent Roux-en-Y jejunostomy placement over 2019-2022. Participants were purposely recruited from a functional gut disorder clinic based in Australia. Diagnosis was confirmed via gastric emptying scintigraphy demonstrating delayed gastric emptying in the absence of mechanical obstruction. The inclusion criteria were: (1) A diagnosis of idiopathic gastroparesis; (2) Having undergone Roux-en-Y jejunostomy placement between 2019 - 2022; and (3) Having had pre
Patients underwent a semi-structured interview by an author (Salehi O) not involved in their care or clinical decision making to reduce risk of bias. The following topics were explored: (1) Pre-procedure symptoms and motivation for jejunostomy insertion; (2) Post-operative recovery and complications; (3) Impact on daily life including work/study, social life and sleep; (4) Weight changes and feeding regimen; (5) Comparison to prior feeding tubes; and (6) Overall experience and willingness to undergo the procedure again and/or recommend it to others. Interviews lasted 45-60 minutes and were audio-recorded with participant consent. Recordings were professionally transcribed verbatim. Thematic analysis was performed using an iterative coding process by two researchers (Salehi O, Gao WL) inde
Patients presented with severe gastroparesis symptoms and had difficulties with or failed prior enteral feeding approaches (Table 1). Nasal and throat irritation was common with nasogastric/nasojejunal tubes (7/8; 87.5%), while half had complications, including gastric perforation, leakage and infection, with gastrostomy tubes (4/8; 50%). The most frequently cited reasons for pursuing Roux-en-Y jejunostomy were to reduce social stigma and optimize nutrition (6/8; 75% each). Four patients (50%) also had a venting gastrostomy inserted. Post-procedure, patients reported improvements in nausea/vomiting (8/8; 100%) and abdominal pain (7/8; 87.5%) (Table 2). Weight stabilised and oral intake improved in 75% (6/8) of patients. Most (7/8; 87.5%) described improved social confidence, increased energy, and better work/school functioning. Specific domains showing improvement included social functioning, with reduced feeding tube visibility and increased confidence in public settings, and physical wellbeing with better symptom control and weight stabilization (Table 3). As one patient described: “Having the jejunostomy was life-changing. I could finally focus on work and socializing instead of constantly worrying about nutrition and tubes falling out”.
| Case | Age/sex | Previous feeding tubes | Reason (s) for procedure |
| 1 | 72 males | NJT | Recurrent NJT blockage and persistent nasal/throat irritation |
| Nasal/throat irritation, recurrent blockage, kinking | |||
| PEG | |||
| Recurrent infections | |||
| 2 | 22 females | NJT | Less social stigma as is more discrete; long term solution to maintaining weight |
| Recurrent sinus infection, nasal bleeding | |||
| Social stigma - people constantly staring | |||
| 3 | 27 females | NJT | Optimise nutrition; medication administration; persistent throat/nasal irritation from NJT |
| Nasal ulceration/wounds | |||
| Throat irritation | |||
| Recurrent blockage | |||
| Social stigma | |||
| PEG | |||
| Hypergranulation tissue | |||
| 4 | 18 females | NJT | Persistent nausea/vomiting; less social stigma; optimise nutrition |
| Nasal/throat irritation | |||
| Social stigma | |||
| 5 | 28 females | NJT | Optimise nutrition; improve symptoms |
| Recurrent “flipping” | |||
| Nasal/throat irritation | |||
| PEG | |||
| Dislodgement causing gastric perforation and multiple operations | |||
| 6 | 28 females | NJT | Persistent nausea/vomiting; optimise nutrition |
| Nasal/throat irritation | |||
| Blockage | |||
| PEG | |||
| Leakage | |||
| Feeding jejunostomy | |||
| Leakage | |||
| 7 | 31 females | NJT | Optimise nutrition; less leakage and dislodgement |
| Recurrent blockage | |||
| Dislodgement | |||
| PEG-J | |||
| Feed reflux | |||
| Leakage | |||
| Jejunal extension dislodgement | |||
| 8 | 26 males | NJT | Optimise nutrition; reduce leakage and pain |
| Recurrent sinus infection | |||
| Dislodgement | |||
| Social stigma | |||
| PEG-J | |||
| Balloon displacement | |||
| Pain | |||
| Leakage |
| Case | Symptoms | Complications | Nutrition | Life impact | Venting gastrostomy | Jejunostomy in situ or removed? | Procedure again? | Follow up duration |
| 1 | Minimal nausea/vomiting | Persistent abdominal pain | Reduced EN frequency due to pain | Less social stigma - “it’s great not to be stared at by strangers all the time” | No | Jejunostomy eventually removed due to persistent abdominal pain - has returned to NJT | No | 2 years |
| Worsening abdominal pain | Minimal oral intake - could tolerate sips of clear fluids | Mindful of heavy lifting due to strain on abdomen | ||||||
| 2 | Improved nausea and abdominal pain | Nil | Continuous EN feeds | Less social stigma | No | In situ | Yes | 1 year |
| Weight stable | Currently studying at university | |||||||
| 3 | Improved nausea and abdominal pain | Leakage | Able to maintain weight | “Life changing” | Yes | In situ | Yes | 3 years |
| Has been able to travel overseas | ||||||||
| Hypergranulation tissue requiring multiple debridements | Overnight EN | Working full time | ||||||
| Improved oral intake | Maintaining social life | |||||||
| Difficult to exercise due to pain | ||||||||
| 4 | Improved nausea and abdominal pain | Leakage | Cyclical EN feeds initially | Energy levels much improved | Yes | Removed - able to maintain adequate oral nutrition | Yes | 3 years |
| Less social stigma | ||||||||
| Now able to maintain weight with oral intake | Currently studying at university | |||||||
| Avoids tight fitting clothing due to leakage | ||||||||
| 5 | Improved nausea and abdominal pain | Cuff burst requiring jejunostomy exchange | Difficulty tolerating EN via jejunostomy due to abdominal pain - required a period of TPN whilst analgesia regimen optimised | Less social stigma | Yes | In situ | Yes | 3 years |
| Hospital admission due to poorly controlled pain | Improved energy levels | |||||||
| 6 | Nausea improved, occasional vomiting | Initially had issues with leakage however resolved with jejunostomy exchange | Cyclical EN feeds | Great quality of life | No | In situ | Yes | 2 years |
| Currently working | ||||||||
| Mild abdominal pain | Approximately 20% oral intake | High energy levels | ||||||
| Weight stable | Improved social life | |||||||
| 7 | Improved nausea and abdominal pain | Hypergranulation tissue | Continuous EN feeds initially however now able to maintain nutrition via oral intake | Maintain oral nutrition | Yes | Removed - able to maintain adequate oral nutrition | Yes | 1.5 years |
| Social and work life much improved | ||||||||
| Less leakage compared to previous feeding tubes | ||||||||
| 8 | Improved nausea and abdominal pain | Nil | Cyclical EN initially however symptoms improved to the point where could tolerate oral intake | Regained independence | No | Removed - able to maintain adequate oral nutrition | Yes | 2 years |
| Socially discrete | ||||||||
| Improved function at work | ||||||||
| Able to maintain nutrition orally |
| Specific domains | |
| Improvements | |
| Social functioning | Reduce visibility of the feeding tube |
| Increased confidence in public settings | |
| Better ability to participate in social activities | |
| Work/study | Improved attendance |
| Better concentration | |
| Reduced interruptions for tube management | |
| Physical wellbeing | Better symptom control |
| Improved energy levels | |
| Weight stabilization | |
| Independence | Easier self-care |
| Greater mobility | |
| Reduced hospital visits | |
| Ongoing challenges | |
| Physical activity | Exercise limitations due to tube position concerns about tube displacement during activity |
| Travel considerations | |
| Social life | Concerns about body image |
| Managing feeding schedule around social activities | |
| Work/study | Managing feeding schedules at work/class |
| Finding private spaces for tube care | |
| Explaining medical needs to employers/educational institution | |
| Sleep | Finding comfortable sleeping positions |
| Managing overnight feeds | |
| Concern about tube displacement during sleep | |
Supplemental gastric venting was used in half the cohort (4/8; 50%). Three patients (2/8; 37.5%) were eventually able to maintain adequate nutrition via oral intake and had their jejunostomy tubes removed. However, one patient (1/8; 12.5%) experienced severe abdominal pain six months post-procedure, leading to jejunostomy removal. Minor leakage occurred in 3/8 (37.5%) of cases. Ongoing challenges included limitations with physical activity, managing feeding schedules around work and social activities, and sleep disruption (Table 3). Despite these challenges, most (7/8; 87.5%) patients preferred the Roux-en-Y jejunostomy over previous feeding tubes and stated they would undergo the procedure again. Overall, despite some issues, Roux-en-Y jejunostomy led to notable improvements in symptoms, nutrition and life experience for this cohort of gastroparesis patients. As one participant noted: “The recovery was difficult at times, but it was worth it. The pain and nausea are so much better now”.
This case series describes patient experiences following Roux-en-Y jejunostomy placement in eight patients with refractory gastroparesis. Despite some challenges, patients generally reported positive experiences regarding symptom control, nutrition, work/study and social stigma compared to previous feeding tubes. Most patients expressed that they would undergo the procedure again. These findings suggest that Roux-en-Y jejunostomy may be a viable option for providing long-term enteral nutrition support in carefully selected gastroparesis patients. Gastroparesis is a complex disorder that profoundly impacts quality of life. Patients struggle with debilitating symptoms, malnutrition, and psychosocial distress[1]. Comorbid psychiatric conditions, such as anxiety and depression affect up to 50% of patients with gastroparesis[18,19]. While none of the patients in our series had a formal eating disorder diagnosis, restrictive eating behaviors may be observed in gastroparesis, potentially as a response to chronic symptoms[20,21]. This can further complicate management and highlights the need for multidisciplinary support.
Enteral nutrition is often required to maintain adequate nutrition in gastroparesis, but traditional feeding tubes have limitations[2]. Nasogastric and nasojejunal tubes are poorly tolerated due to nasal and throat discomfort, frequent dislodgement, and visible appearance[3]. Percutaneous endoscopic transgastric jejunostomy tubes can reduce some of these issues but are prone to retrograde migration into the stomach and may need repeat procedures for repositioning and/or replacement[22,23]. Direct surgical jejunostomy tubes provide post-pyloric access but carry risks of dehiscence, leakage, and need for regular replacement[11,24]. The Roux-en-Y jejunostomy approach may offer certain advantages in this challenging patient population. The jejunostomy tube positioning within a small bowel limb may have contributed to less dysfunction and greater longevity compared to other enteral access techniques. Importantly, patients described meaningful improvements in their day-to-day lives, with increased independence, less social stigma, and better overall functioning. While several domains showed improvement, including social functioning and physical wellbeing, patients continued to face challenges in areas such as physical activity and sleep (Table 3). Notably, three patients were able to have their jejunostomy tubes removed due to improved oral intake. This suggests the procedure may have potential to serve as a bridge to oral nutrition for certain patients, in conjunction with other gastroparesis management strategies.
The procedure was generally well tolerated. Some patients described mild leakage and pain but generally preferred the Roux-en-Y jejunostomy compared to previous feeding tubes. Half of the patients also had insertion of a venting gastrostomy to allow gastric decompression to manage symptoms. In our experience, early recognition and management of complications is crucial. For leakage, we found that careful attention to stoma care, use of barrier films/powders, and adjustment of feeding schedules/rates could help minimize impact. Hypergranulation tissue was managed with silver nitrate application and topical steroids when needed. Regular assessment of tube position and function, along with patient education on proper care techniques, helped prevent more serious complications. The concurrent use of venting gastrostomy in selected patients appeared to improve symptom control, though this requires careful consideration of the added complexity of managing two tubes.
One patient required jejunostomy tube removal six months post insertion due to persistent abdominal pain post-procedure of unclear aetiology despite extensive investigation which was unrevealing. This highlights the importance of careful patient selection and the need to consider underlying chronic pain syndromes or other comorbidities that may impact outcomes. Given the profound impact of gastroparesis on quality of life, interventions that improve patient well-being are highly significant[6]. While Roux-en-Y jejunostomy was not a perfect solution, this study suggests it can be a reasonable option for some patients struggling with other feeding tube modalities. The concurrent insertion of a venting gastrostomy may also be helpful in symptom management however the relevant risks and added burden of managing a second tube need to be taken into consideration. Rigorous patient selection, preoperative counselling, and ongoing multidisciplinary support are key to optimising outcomes.
Several studies have explored patient experiences with enteral feeding tubes, providing insight into the impacts on quality of life and daily living[25-28]. Patients and caregivers describe various lifestyle disruptions with percutaneous endoscopic gastrostomy and nasal tubes including leakage and infection, disturbed sleep, limitations on activities, clothing, and social life. Patients also commonly described frustration, embarrassment, and stigma[25-28]. In our cohort, all patients had used previous feeding tubes as described in Table 1. Common issues included nasal/throat irritation, blockage, leakage and social stigma. Limited studies have explored experiences with jejunostomy tubes, particularly in adults. Cullis et al[15] performed a systematic review assessing whether Roux-en-Y feeding jejunostomy is a safe and effective operation in children. It was concluded that up to 50% of patients experience minor complications and the procedure can provide enteral nutrition effectively. Of note no studies analyzed in the review included patient and/or caregiver quality of life outcomes.
This study has several strengths. Firstly, our patient-centred approach provides valuable insights directly from the participants’ perspectives, offering a nuanced understanding of the lived experience with Roux-en-Y jejunostomy that quantitative measures alone might not capture. The inclusion of patients with prior experience of other feeding methods allows for a comparative assessment of different enteral nutrition approaches, enhancing the context of our findings. Our evaluation encompassed multiple aspects of patient experience, including symptom control, nutrition, quality of life, and psychosocial factors, providing a holistic view of the procedure’s impact. By focusing on patients with refractory gastroparesis, this study addresses an important gap in the literature for managing difficult-to-treat cases. The extended follow-up period, ranging from several months to years post-surgery, allowed us to observe not only immediate post-operative effects but also the evolving long-term impact of the procedure on patients’ lives. This longitudinal perspective is particularly valuable in assessing the durability of benefits and identifying any late-onset challenges. Finally, our findings have the potential to inform clinical practice by guiding patient selection, pre-operative counselling, and post-operative management for Roux-en-Y jejunostomy in gastroparesis patients. These strengths collectively contribute to a more comprehensive understanding of this surgical intervention in the context of refractory gastroparesis management.
Based on our experience, optimal candidates for Roux-en-Y jejunostomy share several important characteristics. Primary consideration should be given to patients who have demonstrably failed conservative management and simpler feeding approaches. Candidates should demonstrate good understanding of post-operative care requirements and show motivation to participate in their ongoing care. A stable psychiatric status is essential, as the demands of managing this feeding method can be challenging. Strong social support has also proven to be a crucial factor in successful outcomes. Preoperative counselling plays a vital role in setting appropriate expectations and preparing patients for this procedure. Discussions should thoroughly cover the expected recovery timeline and help patients understand the potential need for concurrent venting gastrostomy. Emphasis should be placed on the importance of proper tube care and the management strategies for possible complications. Patients need to understand how the procedure will impact their daily activities and what long-term maintenance requirements they will need to accommodate. This comprehensive counselling approach helps ensure patients are well-prepared for both the immediate post-operative period and long-term management of their jejunostomy.
There are several important limitations in our study. The small sample size of eight patients and single-centered design limit generalizability of the findings. Patients were recruited from a specialized clinic, which may have introduced selection bias. To mitigate interviewer bias, the researcher conducting interviews was not directly involved in patient care or clinical decision-making. The small sample size of eight patients and single-centered design limit generalizability of the findings. While our results provide valuable initial insights, larger multi-center studies are needed to better understand outcomes across diverse patient populations.
However, the lack of blinding and potential for social desirability bias influencing patient responses cannot be excluded. Future studies would benefit from multiple independent interviewers and more rigorous blinding procedures. The qualitative design also inherently lacks objective outcome measures. Larger, prospective comparative studies are needed to better define the role of Roux-en-Y jejunostomy alongside other enteral access techniques for gastroparesis. Additionally, quantitative evaluation of quality of life, stigma, nutritional parameters, psychological factors and patient-reported experience metrics using validated instruments would further enrich understanding of real-world benefits vs risks and burden from the patient perspective.
In conclusion, this qualitative retrospective cohort study offers valuable patient-centered insights into Roux-en-Y jejunostomy as a potential option for long-term enteral support in gastroparesis. While the procedure had challenges and was not a panacea, the quality-of-life improvements described by most patients, along with the ability of some to transition to oral nutrition, justify further research to optimize patient selection, post-operative care, nutritional outcomes and complication management with this approach. Future research priorities should include: (1) Long-term outcome studies examining tube longevity, complication rates, and quality of life impacts beyond the initial post-operative period; (2) Comparative effectiveness studies vs other feeding tube approaches; (3) Investigation of patient factors (age, disease severity, comorbidities) that may predict procedural success; and (4) Evaluation of optimal patient selection criteria and pre/post-operative management protocols. Additionally, studies incorporating validated instruments to measure quality of life, stigma, and nutritional outcomes would provide more robust evidence to guide clinical decision-making. Roux-en-Y jejunostomy may be a viable therapeutic option for carefully selected patients with gastroparesis requiring long-term tube feeding.
| 1. | Huang IH, Schol J, Khatun R, Carbone F, Van den Houte K, Colomier E, Balsiger LM, Törnblom H, Vanuytsel T, Sundelin E, Simrén M, Palsson OS, Bangdiwala SI, Sperber AD, Tack J. Worldwide prevalence and burden of gastroparesis-like symptoms as defined by the United European Gastroenterology (UEG) and European Society for Neurogastroenterology and Motility (ESNM) consensus on gastroparesis. United European Gastroenterol J. 2022;10:888-897. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 39] [Reference Citation Analysis (0)] |
| 2. | Camilleri M, Chedid V, Ford AC, Haruma K, Horowitz M, Jones KL, Low PA, Park SY, Parkman HP, Stanghellini V. Gastroparesis. Nat Rev Dis Primers. 2018;4:41. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 332] [Cited by in RCA: 269] [Article Influence: 33.6] [Reference Citation Analysis (7)] |
| 3. | Wang YR, Fisher RS, Parkman HP. Gastroparesis-related hospitalizations in the United States: trends, characteristics, and outcomes, 1995-2004. Am J Gastroenterol. 2008;103:313-322. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 272] [Cited by in RCA: 223] [Article Influence: 12.4] [Reference Citation Analysis (4)] |
| 4. | Rangan V, Ukleja A. Gastroparesis in the Hospital Setting. Nutr Clin Pract. 2021;36:50-66. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 5] [Article Influence: 1.0] [Reference Citation Analysis (1)] |
| 5. | Patel J, Bains K, Kalra S, Singh I, Kohli I, Dukovic D, Chaudhry H, Sohal A, Yang J, Tringali S. The Effects of Malnutrition on Inpatient Outcomes in Patients With Gastroparesis: A Nationwide Analysis. Cureus. 2023;15:e47082. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 6. | Bekkelund M, Sangnes DA, Gunnar Hatlebakk J, Aabakken L. Pathophysiology of idiopathic gastroparesis and implications for therapy. Scand J Gastroenterol. 2019;54:8-17. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 22] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 7. | El Halabi M, Parkman HP. 2023 update on the clinical management of gastroparesis. Expert Rev Gastroenterol Hepatol. 2023;17:431-441. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 15] [Reference Citation Analysis (0)] |
| 8. | Camilleri M, Parkman HP, Shafi MA, Abell TL, Gerson L; American College of Gastroenterology. Clinical guideline: management of gastroparesis. Am J Gastroenterol. 2013;108:18-37; quiz 38. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 958] [Cited by in RCA: 781] [Article Influence: 60.1] [Reference Citation Analysis (8)] |
| 9. | Limketkai BN, LeBrett W, Lin L, Shah ND. Nutritional approaches for gastroparesis. Lancet Gastroenterol Hepatol. 2020;5:1017-1026. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 31] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 10. | Parrish CR, Yoshida CM. Nutrition Intervention for the Patient with Gastroparesis: An Update. Pract Gastroenterol. 2005;29:29-66. |
| 11. | Tapia J, Murguia R, Garcia G, de los Monteros PE, Oñate E. Jejunostomy: techniques, indications, and complications. World J Surg. 1999;23:596-602. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 100] [Cited by in RCA: 87] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 12. | Young MT, Troung H, Gebhart A, Shih A, Nguyen NT. Outcomes of laparoscopic feeding jejunostomy tube placement in 299 patients. Surg Endosc. 2016;30:126-131. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 34] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 13. | Hsiung T, Chao WP, Chai SW, Chou TC, Wang CY, Huang TS. Laparoscopic vs. open feeding jejunostomy: a systemic review and meta-analysis. Surg Endosc. 2023;37:2485-2495. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 14. | van Braak H, Gorter RR, van Wijk MP, de Jong JR. Laparoscopic Roux-en-Y feeding jejunostomy as a long-term solution for severe feeding problems in children. Eur J Pediatr. 2023;182:601-607. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (1)] |
| 15. | Cullis PS, Buckle RE, Losty PD. Is Roux-en-Y Feeding Jejunostomy a Safe and Effective Operation in Children? A Systematic Review Exploring Outcomes. J Pediatr Gastroenterol Nutr. 2022;74:e74-e82. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 5] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 16. | Kim CH, Nelson DK. Venting percutaneous gastrostomy in the treatment of refractory idiopathic gastroparesis. Gastrointest Endosc. 1998;47:67-70. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 69] [Cited by in RCA: 54] [Article Influence: 1.9] [Reference Citation Analysis (3)] |
| 17. | Petrov RV, Bakhos CT, Abbas AE, Malik Z, Parkman HP. Endoscopic and Surgical Treatments for Gastroparesis: What to Do and Whom to Treat? Gastroenterol Clin North Am. 2020;49:539-556. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 31] [Cited by in RCA: 22] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 18. | Woodhouse S, Hebbard G, Knowles SR. Psychological controversies in gastroparesis: A systematic review. World J Gastroenterol. 2017;23:1298-1309. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 38] [Cited by in RCA: 58] [Article Influence: 6.4] [Reference Citation Analysis (2)] |
| 19. | Hasler WL, Parkman HP, Wilson LA, Pasricha PJ, Koch KL, Abell TL, Snape WJ, Farrugia G, Lee L, Tonascia J, Unalp-Arida A, Hamilton F; NIDDK Gastroparesis Clinical Research Consortium. Psychological dysfunction is associated with symptom severity but not disease etiology or degree of gastric retention in patients with gastroparesis. Am J Gastroenterol. 2010;105:2357-2367. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 116] [Cited by in RCA: 94] [Article Influence: 5.9] [Reference Citation Analysis (4)] |
| 20. | Burton Murray H, Jehangir A, Silvernale CJ, Kuo B, Parkman HP. Avoidant/restrictive food intake disorder symptoms are frequent in patients presenting for symptoms of gastroparesis. Neurogastroenterol Motil. 2020;32:e13931. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 75] [Cited by in RCA: 55] [Article Influence: 9.2] [Reference Citation Analysis (0)] |
| 21. | Hollis E, Murray HB, Parkman HP. Relationships among symptoms of gastroparesis to those of avoidant/restrictive food intake disorder in patients with gastroparesis. Neurogastroenterol Motil. 2024;36:e14725. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 14] [Article Influence: 7.0] [Reference Citation Analysis (0)] |
| 22. | Hitawala AA, Mousa OY. Percutaneous Gastrostomy and Jejunostomy. 2023 May 29. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. [PubMed] |
| 23. | Johnson DY, Gallo CJR, Agassi AM, Sag AA, Martin JG, Pabon-Ramos W, Ronald J, Suhocki PV, Smith TP, Kim CY. Percutaneous gastrojejunostomy tubes: Identification of predictors of retrograde jejunal limb migration into the stomach. Clin Imaging. 2021;70:93-96. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 24. | Okida LF, Salimi T, Ferri F, Henrique J, Lo Menzo E, Szomstein S, Rosenthal RJ. Complications of feeding jejunostomy placement: a single-institution experience. Surg Endosc. 2021;35:3989-3997. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 16] [Article Influence: 3.2] [Reference Citation Analysis (0)] |
| 25. | Green SM, Townsend K, Jarrett N, Westoby C, Fader M. People with enteral tubes and their carers' views of living with a tube and managing associated problems: A qualitative interview study. J Clin Nurs. 2019;28:3710-3720. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 18] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 26. | Xue M, Zhai X, Liu S, Xu N, Han J, Zhou M. The experience of family caregivers of patients receiving home nasogastric tube feeding in China: A descriptive qualitative study. J Hum Nutr Diet. 2022;35:14-22. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 23] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 27. | Zamanillo Campos R, Colomar Ferrer MT, Ruiz López RM, Sanchís Cortés MP, Urgelés Planella JR. Specific Quality of Life Assessment by the NutriQoL® Questionnaire Among Patients Receiving Home Enteral Nutrition. JPEN J Parenter Enteral Nutr. 2021;45:490-498. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 13] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 28. | Martin L, Blomberg J, Lagergren P. Patients' perspectives of living with a percutaneous endoscopic gastrostomy (PEG). BMC Gastroenterol. 2012;12:126. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 21] [Cited by in RCA: 27] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
Open Access: This article is an open-access article that was selected by an in-house editor and fully peer-reviewed by external reviewers. It is distributed in accordance with the Creative Commons Attribution NonCommercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: https://creativecommons.org/Licenses/by-nc/4.0/