Published online May 16, 2026. doi: 10.4253/wjge.v18.i5.118389
Revised: February 4, 2026
Accepted: March 10, 2026
Published online: May 16, 2026
Processing time: 132 Days and 14.3 Hours
Endoscopic retrograde cholangiopancreatography (ERCP) is the first-line treat
To identify the clinical, radiological, and cholangiographic predictors of incom
This single-center retrospective study analyzed consecutive patients who un
A total of 245 patients (mean age 46.2 ± 14.8 years; 75.5% women) were included in the study. Complete clearance of CBD stones was achieved in 179 patients (73.1%) at the index ERCP. Multivariate analysis revealed that independent predictors of incomplete CBD stone clearance on ERCP included proximal CBD stone location [odds ratio (OR) 4.44, P = 0.003], stone-to-CBD diameter ratio > 1 (OR = 5.22, P = 0.033), presence of a CBD stricture (OR = 5.06, P = 0.049), and impacted stones (OR = 9.33, P = 0.003). Receiver operating characteristic curve analysis demonstrated that stone size (area under the curve: 0.750) and stone-to-CBD diameter ratio (area under the curve: 0.709) on ERCP were the strongest predictors of incomplete CBD stone clearance.
Proximal CBD stones, stone-to-duct size mismatch, CBD strictures, and impacted stones were predictors of incomplete CBD stone clearance, highlighting the need for careful planning and the use of advanced endoscopic techniques or surgery.
Core Tip: This retrospective study assessed clinical, radiological, and cholangiographic predictors of common bile duct (CBD) stone clearance during index endoscopic retrograde cholangiopancreatography (ERCP). Impacted stones, proximal stone location, CBD stricture, and a stone-to-CBD diameter ratio > 1 on ERCP independently predicted failure to achieve complete CBD stone clearance. A stone size of ≤ 11 mm on ERCP was identified as the optimal threshold for predicting successful clearance without the need for advanced techniques. Early identification of these predictors can assist in procedural planning, facilitate the timely use of advanced techniques or surgery, and avoid repeat ERCPs.
- Citation: Lone SA, Vaithiyam V, Vora K, Sirohi N, Sonika U, Dalal A, Kumar A, Srivastava S, Sachdeva S, Sharma BC. Predictors of incomplete common bile duct stone clearance at index endoscopic retrograde cholangiopancreatography. World J Gastrointest Endosc 2026; 18(5): 118389
- URL: https://www.wjgnet.com/1948-5190/full/v18/i5/118389.htm
- DOI: https://dx.doi.org/10.4253/wjge.v18.i5.118389
Choledocholithiasis, or the presence of stones within the common bile duct (CBD), is one of the most common biliary tract pathologies encountered in gastroenterology practice. It is the most frequent complication of gallstone disease, affecting approximately 5% of patients undergoing cholecystectomy[1]. The incidence of CBD stones increases with age and is most commonly associated with female sex, as well as anatomical, genetic, and metabolic factors. CBD stones can cause biliary pain, cholangitis, obstructive jaundice, and biliary pancreatitis, leading to significant morbidity and mortality[2-5]. If left untreated, CBD stones can result in long-term complications, such as biliary strictures and secondary biliary cirrhosis[6-8], necessitating their complete removal.
Different approaches to managing CBD stones include open surgical choledochotomy, endoscopic sphincterotomy, and laparoscopic CBD exploration. The European Society of Gastrointestinal Endoscopy (ESGE) recommends Endoscopic Retrograde Cholangiopancreatography (ERCP) as the primary and definitive treatment for patients with CBD stones who have undergone previous cholecystectomy. In patients with concomitant CBD stones and cholelithiasis, ESGE re
ERCP-based CBD stone management typically involves endoscopic sphincterotomy followed by stone extraction using a balloon or basket catheter. This approach achieves CBD clearance in 80%-90% of patients[10]. Despite the high clearance rate, initial failure rates range from 5% to 30%, depending on the definition of success and the patient population studied[11-13]. ESGE recommends endoscopic papillary large-balloon dilation (EPLBD), mechanical lithotripsy (ML), and cholangioscopy-assisted lithotripsy for patients in whom CBD stones cannot be cleared with standard extraction techniques[9].
Various studies have shown that stone-related factors, such as size, shape, and position, as well as impacted stones and biliary anatomical factors, including distal biliary strictures, angulated bile ducts, periampullary diverticula, or altered surgical anatomy, are associated with failed CBD clearance using standard extraction techniques[11,12,14].
However, these studies have primarily focused on preprocedural imaging, with limited attention to clinical or cholangiographic predictors of incomplete CBD stone clearance. Identification of such predictors could improve procedural planning, guide the use of additional techniques, optimize resource allocation, and enhance patient counselling. This may reduce the need for repeated procedures and facilitate early advanced endoscopic therapies or surgery. This study aimed to identify clinical, radiological, and cholangiographic predictors of incomplete CBD clearance at the index ERCP in patients undergoing elective stone removal.
This single-centre retrospective study using prospectively collected data was conducted at the Department of Gastroenterology, Govind Ballabh Pant Institute of Postgraduate Medical Education and Research, New Delhi, from January 2023 to October 2023. All patients aged ≥ 18 years who were diagnosed with choledocholithiasis by magnetic resonance cholangiopancreatography (MRCP) and underwent native CBD cannulation with attempted CBD stone removal during ERCP were included.
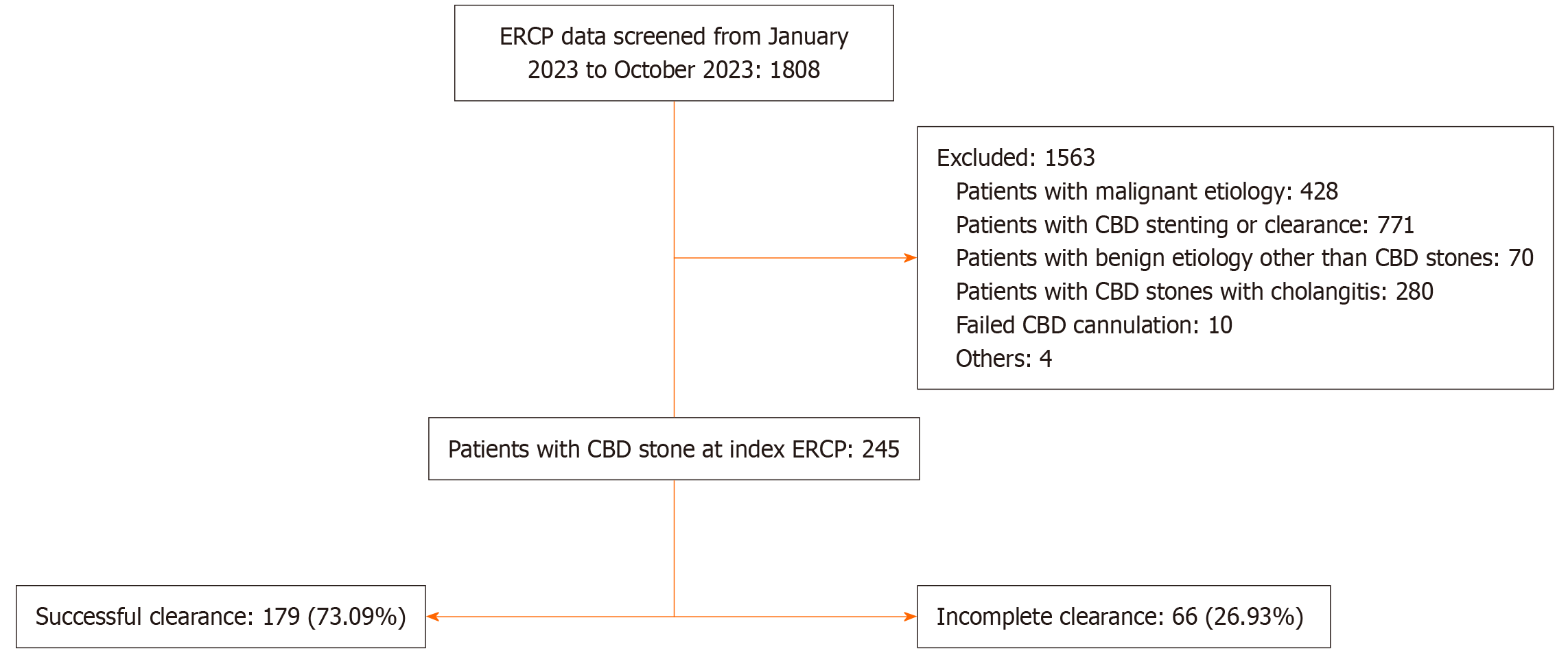
Patients with cholangitis, portal biliopathy, endoscopic ultrasound-guided biliary cannulation, prior ERCP, those who underwent cholangioscopy-guided therapies, and pregnant women were excluded (Figure 1). Patients with uncorrected coagulopathy or those receiving antiplatelet or antithrombotic medications were also excluded. The study was approved by the Institutional Ethics Committee of Maulana Azad Medical College (No. F.1/IEC/MAMC/117/05/2025/No. 493), New Delhi, India. The requirement for informed consent was waived owing to the retrospective nature of the study.
Demographic data (age and sex), clinical parameters (such as abdominal pain and jaundice), and laboratory values were recorded. All patients underwent transabdominal ultrasonography and MRCP as part of the pre-ERCP evaluation. Imaging parameters, including CBD diameter, stone size, stone location, and the presence or absence of biliary strictures, were obtained from preprocedural MRCP and intraprocedural cholangiographic images during ERCP. Endoscopic findings, including papillary morphology and cannulation feasibility, were documented by the operating endoscopist.
ERCP-guided CBD clearance: After obtaining written informed consent, ERCP was performed using a duodenoscope (190 Series; Olympus, Tokyo, Japan) in the prone position. All procedures were conducted under monitored intravenous anesthesia (low-dose propofol and midazolam), with continuous vital sign monitoring. ERCPs were performed by endoscopists with formal ERCP training and several years of independent practice (> 4000 ERCPs). Trainees participated in selected procedures under direct supervision in accordance with institutional training protocols. After intubation of the duodenoscope into the second part of the duodenum, the papilla was visualized, and standard guidewire-assisted cannulation of the CBD was performed.
Difficult biliary cannulation was defined according to ESGE criteria as meeting one or more of the “5-5-1” criteria: > 5 minutes of attempted cannulation, > 5 attempts at the papilla, or > 1 unintentional pancreatic duct cannulation[9]. In such cases, advanced techniques, including needle-knife fistulotomy, transpancreatic septostomy, or the double-guidewire technique, were used. Following cannulation, CBD stones were confirmed by cholangiography. All patients underwent biliary sphincterotomy. Stone extraction was performed using a 12-15 mm stone extraction balloon (Extractor™ Pro XL; Boston Scientific). Additional procedures, such as EPLBD and ML, were performed based on cholangiographic findings. Stone extraction was considered unsuccessful after three attempts with the extraction balloon. A final check cholangiogram was performed to confirm ductal clearance. After ERCP, CBD stenting was performed in all patients with incomplete duct clearance, whereas in patients with complete clearance, stent placement was at the discretion of the endoscopist.
Complete CBD stone clearance: No residual filling defects on the final check cholangiogram.
Incomplete CBD stone clearance: Persistence of one or more filling defects on the final cholangiogram at the end of the index ERCP, necessitating repeat intervention.
Primary objective: To assess the rate of successful CBD stone clearance.
Secondary objectives: To identify predictors of failure in CBD stone clearance based on clinical or imaging findings.
Data were analyzed using SPSS software version 21.0 (IBM Corp., Armonk, NY, United States). All patient data were anonymized prior to analysis. Continuous variables were compared using Student’s t test, and categorical variables were compared using the χ2 test. Univariate and multivariate logistic regression analyses were performed to identify predictors of incomplete CBD clearance. Area under the curve (AUC) values with 95% confidence intervals (CIs) were calculated using the method described by DeLong et al[15]. Odds ratios with 95%CIs were calculated, and statistical significance was defined as P < 0.05.
During the study period, 1808 patients underwent ERCP at our institute; of these, 245 patients with CBD stones were included based on the inclusion and exclusion criteria (Figure 1). The mean age was 46.2 ± 14.8 years, and the majority were female (185, 75.5%). Abdominal pain was the most common presenting symptom (78%), followed by jaundice (24.9%). Twelve patients (4.9%) had a history of acute pancreatitis. Seventy-three patients had a prior history of cholecystectomy. Among patients with intact gallbladders, 104 (60.5%) had gallstones.
Primary CBD cannulation was achieved in 205 patients (80.3%), and advanced biliary cannulation techniques were required in 35 patients (13.7%). Needle-knife fistulotomy was the most common salvage technique (25, 9.8%). CBD cannulation could not be achieved in 10 patients (3.9%). Biliary sphincterotomy was performed in all patients, and papillary balloon dilatation was performed as required in 76 patients (31.1%). ML was performed in two patients. The mean CBD diameter on cholangiography was 12.0 ± 3.8 mm. More than three stones were observed in 22 patients. The mean stone diameter was 9.8 ± 4.8 mm. Complete CBD clearance was achieved in 179 patients (73.06%), whereas clearance was incomplete in 66 patients (26.93%) (Figure 1).
Abdominal pain was significantly more common in patients with incomplete CBD clearance than in those with successful clearance (87.9% vs 74.3%, P = 0.02). Baseline demographic and laboratory parameters did not differ significantly between the two groups. Patients in the incomplete clearance group had significantly larger CBD diameters on MRCP and a higher proportion of stones measuring > 12 mm (Table 1). Similarly, mean stone size was significantly greater in the incomplete clearance group, whereas the number of stones did not differ significantly between groups. On ERCP, patients with incomplete clearance more frequently had a bulky papilla, difficult cannulation, larger CBD diameter, proximally located stones, a stone-to-CBD diameter ratio > 1, impacted stones, and CBD strictures (Table 1).
| Parameters | Not cleared (n = 66) | Cleared (n = 179) | P value |
| Demographic and clinical parameters | |||
| Age (years) | 49.5 (40-58) | 45 (33-58) | 0.1307 |
| Gender (male:female) | 17:49 | 43:136 | 0.908 |
| Pain abdomen | 58 (87.8) | 133 (74.3) | 0.0264 |
| Jaundice | 21 (31.8) | 40 (22.3) | 0.1302 |
| Baseline lab parameters | |||
| Hb (g/dL) | 11.9 (10.5-12.97) | 11.9 (10.9-12.7) | 0.83 |
| TLC (cells/mm3) | 7600 (6550-8790) | 7600 (6450-9100) | 0.85 |
| Platelets (cells × 105/mm3) | 2.3 (1.63-2.87) | 2.3 (1.7-3.0) | 0.59 |
| Total bilirubin (mg/dL) | 0.9 (0.5-2.05) | 0.7 (0.5-1.3) | 0.076 |
| ALT (IU/L) | 34 (20-94) | 42 (23-83) | 0.28 |
| AST (IU/L) | 38.5 (27-75.5) | 41 (26-78) | 0.97 |
| ALP (IU/L) | 188 (129-346) | 180 (127-312) | 0.86 |
| MRCP variables | |||
| CBD diameter > 15 mm | 13 (19.7) | 19 (10.6) | 0.06 |
| CBD diameter in mm | 11.93 ± 4.57 | 10.68 ± 3.41 | 0.02 |
| Stone number (> 3) | 3 (4.5) | 12 (6.7) | 0.52 |
| Stone size > 12 mm | 16 (24.2) | 16 (8.9) | 0.001 |
| Stone size (mm) | 9.97 ± 4.90 | 7.73 ± 3.36 | 0.0001 |
| Location of stone (proximal) | 12 (18.2) | 18 (10.1) | 0.57 |
| Stone to CBD diameter > 1 | 26 (39.3) | 28 (15.6) | 0.0014 |
| ERCP variables | |||
| PAD | 6 (9.1) | 17 (9.5) | 0.94 |
| Bulky papilla | 6 (9.1) | 5 (2.8) | 0.03 |
| Difficult cannulation | 16 (24.2) | 14 (7.8) | 0.001 |
| CBD diameter > 15 mm | 9 (13.6) | 20 (11.2) | 0.10 |
| CBD Diameter (mm) | 13.11 ± 5.10 | 11.72 ± 3.34 | 0.02 |
| Stone number (> 3) | 3 (4.5) | 19 (10.6) | 0.51 |
| Stone size (mm) | 13.77 ± 6.03 | 8.93 ± 3.89 | 0.0001 |
| Location of stone (proximal) | 8 (12.1) | 18 (10.05) | 0.02 |
| CBD stricture | 4 (6.1) | 3 (1.6) | 0.05 |
| Hepatolithiasis | 8 (12.1) | 10 (5.6) | 0.08 |
| Impacted stone | 16 (24.2) | 5 (2.8) | 0.0001 |
| Use of a basket for extraction | 1 (1.5) | 3 (1.7) | 0.94 |
| Balloon sphincteroplasty | 15 (19.7) | 61 (80.2) | 0.067 |
Multivariate logistic regression analysis showed that proximal CBD stone location [odds ratio (OR) = 4.44; 95%CI: 1.67-11.75; P = 0.003], stone-to-CBD diameter ratio > 1 on ERCP (OR = 5.22; 95%CI: 1.14-23.78; P = 0.033), presence of a CBD stricture (OR = 5.06; 95%CI: 1.006-25.52; P = 0.049), and impacted stones (OR = 9.33; 95%CI: 2.17-39.99; P = 0.003) were independent predictors of incomplete CBD clearance (Figure 2, Table 2). Other parameters, including preprocedural abdominal pain, CBD diameter on MRCP or ERCP, and stone size > 12 mm, were not significant predictors (Table 2).
| Variable | OR | 95%CI | P value |
| Pain abdomen | 2.35 | 0.71-7.76 | 0.159 |
| CBD diameter on MRCP | 1.14 | 0.92-1.42 | 0.219 |
| Stone size on MRCP | 1.32 | 0.98-1.77 | 0.066 |
| Stone size > 12 on MRCP | 0.53 | 0.10-2.79 | 0.454 |
| Stone-to-CBD diameter ratio > 1 on MRCP | 3.14 | 0.88-11.20 | 0.077 |
| Bulky papilla | 2.25 | 0.26-18.90 | 0.453 |
| Difficult cannulation | 3.07 | 0.64-14.60 | 0.158 |
| CBD diameter on ERCP | 1.03 | 0.82-1.30 | 0.759 |
| Proximal location of the stone on ERCP | 4.44 | 1.67-11.75 | 0.003 |
| Stone size on ERCP | 1.02 | 0.85-1.19 | 0.909 |
| Stone size > 12 on ERCP | 2.40 | 0.44-12.90 | 0.305 |
| Stone size/CBD diameter > 1 on ERCP | 5.22 | 1.14-23.78 | 0.033 |
| Stricture on ERCP | 5.06 | 1.006-25.52 | 0.049 |
| Impacted stone on ERCP | 9.33 | 2.17-39.99 | 0.003 |
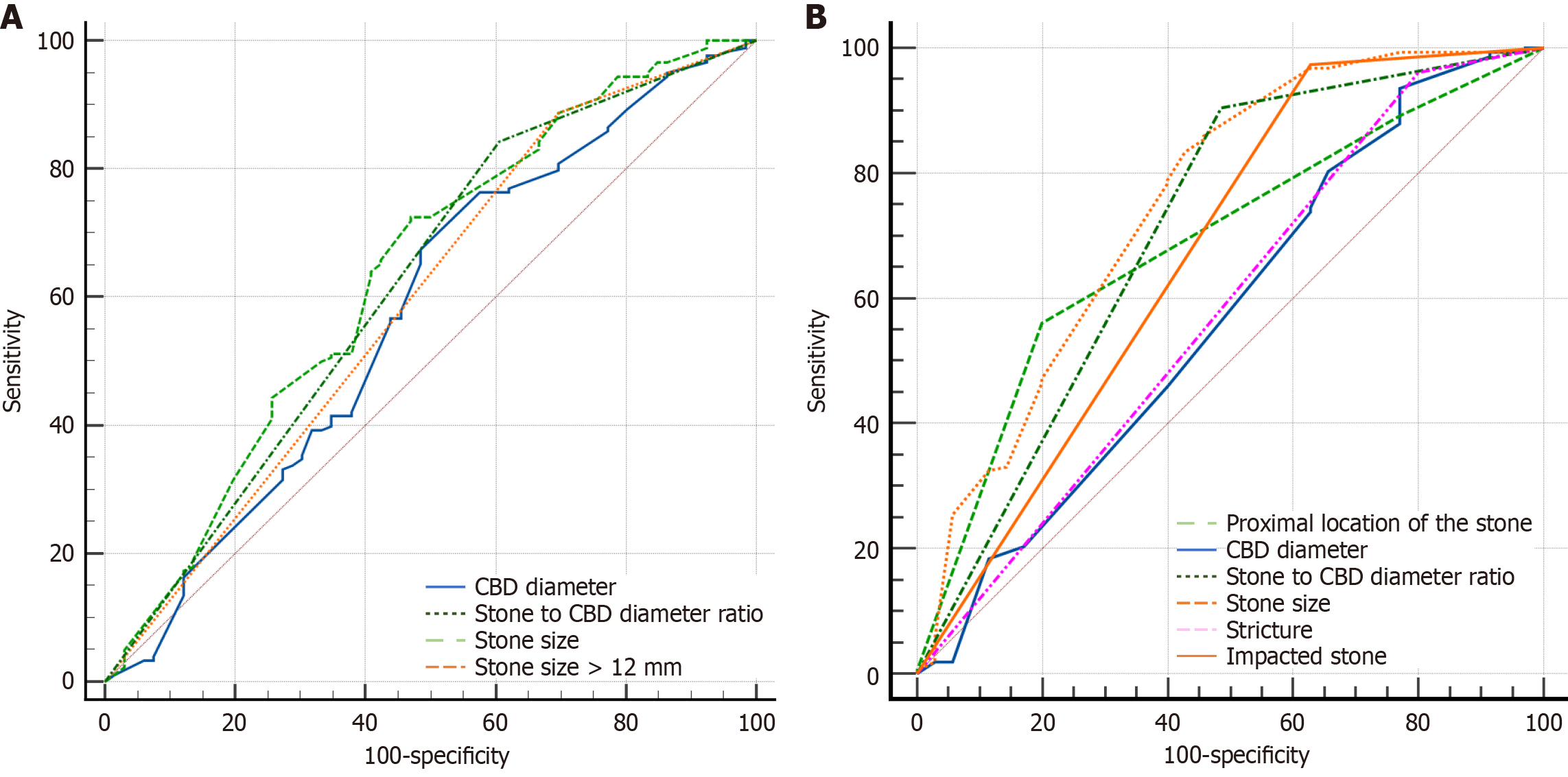
Receiver operating characteristic (ROC) analysis of MRCP parameters showed that stone size had the highest AUC (0.635), followed by the stone size-to-CBD diameter ratio (AUC: 0.618), for predicting incomplete CBD clearance (Figure 3A). ROC analysis of ERCP parameters identified stone size (AUC: 0.750), stone-to-CBD diameter ratio (AUC: 0.709), proximal stone location (AUC: 0.688), and impacted stones (AUC: 0.673) as the most significant predictors of incomplete CBD clearance (Figure 3B). Based on ROC analysis, a stone size of ≤ 11 mm on ERCP was the optimal cutoff for predicting ductal clearance, with a Youden index of 0.38, sensitivity of 80.2%, and specificity of 57.5%.
Post-ERCP pancreatitis was the most common adverse event, occurring in 18 patients (7.3%). Perforation occurred in 12 patients (4.8%). Of these, three required surgical intervention, one was managed with an over-the-scope clip, and the remaining patients were treated conservatively. Post-ERCP bleeding and anesthesia-related complications (transient respiratory depression) were observed in one patient each.
In this retrospective observational study, we assessed clinical, radiological, and cholangiographic factors that predict incomplete clearance of CBD stones during initial ERCP in patients undergoing elective stone removal. The overall success rate of CBD stone extraction in our cohort was 73.06%, which is slightly lower than the commonly reported clearance rate of 80%-90%. This reduced clearance rate may be attributed to several factors, including the patient population being from a high-volume tertiary referral center with a higher proportion of complex cases, trainee involvement, and anatomical challenges. Nonetheless, clearance rates from various tertiary care referral centers were similar to those in our study[12,16,17].
Stone size is a traditional predictor of CBD clearance. Wan et al[18] reported that the overall success rate and the success rate of complete CBD clearance in the > 2 cm group were significantly lower than those in the < 2 cm group (77.8% vs 91.7% and 58.3% vs 83.3%, respectively). Kim et al[11] demonstrated that acute distal CBD angulation (≤ 135°) and a shorter distal CBD length (≤ 36 mm) were independent factors contributing to technical difficulty. The ESGE classified difficult biliary stones based on their features, such as diameter (> 1.5 cm), number, unusual shape (barrel-shaped), or location (intrahepatic, cystic duct), as well as anatomical factors, including narrowing of the bile duct distal to the stone, sigmoid-shaped CBD, impacted stone, shorter length of the distal CBD, or acute distal CBD angulation < 135°[9]. Our study identified four independent predictors of incomplete CBD stone clearance during initial ERCP based on cholangiographic parameters: Mid-third stone location, stone-to-CBD diameter ratio > 1, CBD stricture, and impacted stones. A prospective study showed that strictures distal to the stone (OR = 8.24), a smaller CBD/stone diameter ratio (OR = 0.348), larger stone diameter (OR = 1.187), impacted stones (OR = 1.117), and higher bilirubin levels (OR = 1.1) were independent predictors of failure of stone clearance[19]. We did not assess the characteristics of the distal CBD and CBD angulation in our study. Several prospective and retrospective studies have identified predictors of CBD clearance failure, including fever, elevated bilirubin, older age, interdiverticular papilla, larger stone size and CBD diameter, distal narrowing, hepatolithiasis, and the use of basket or ML[12,20-22].
Strategies to enhance CBD stone clearance include endoscopic papillary large balloon dilatation, ML, and cholangioscopy-guided laser lithotripsy. The effectiveness of ML decreases with increasing stone size. Garg et al[23] also reported that the stone-to-CBD diameter ratio is a predictor of incomplete stone clearance. In their retrospective study, they noted that ML is successful in patients with a CBD diameter greater than the stone size; in those who do not meet this criterion, stone size is not a predictor of failed clearance[23]. The limited use of ML (0.8%) in the present study is due to institutional preference for EPLBD in patients in whom standard stone extraction has failed, which affects the generalizability of the study results. A retrospective cohort study from Thailand found that CBD stones with diameters exceeding the distal CBD diameter by > 2 mm, along with square- and round-shaped stones, were independent pre
A large multicenter study using single-operator cholangioscopy-guided lithotripsy for difficult bile duct stones (largest stone diameter ≥ 15 mm, failed prior attempt at stone clearance, impacted or multiple stones, stones located in the hepatic duct, or stones above a stricture) showed that SOC-guided stone clearance was achieved in 80% of patients in a single session, with an overall success rate of 87%[24]. They also demonstrated no significant difference in stone clearance rates during the first procedure between electrohydraulic lithotripsy and laser lithotripsy (82%, 96/117 vs 74%, 29/39; P = 0.35)[25]. A comparative meta-analysis evaluating all available methods, including sphincterotomy, balloon sphincteroplasty, sphincterotomy with EPLBD, ML, and SOC-assisted lithotripsy for CBD clearance, found that cholangioscopy had the highest success rate for stone removal (Surface Under the Cumulative Ranking score, 0.99), followed by sphincterotomy with EPLBD (Surface Under the Cumulative Ranking score, 0.68). The effectiveness of these two techniques was notably greater when stones exceeded 15 mm, with similar rates of adverse events[26].
Furthermore, in high-volume centers, endoscopist fatigue and burnout may hypothetically influence procedural outcomes. It is hypothesized that patients scheduled earlier in the ERCP list typically receive more time, attention, and technical effort, whereas those scheduled later may be affected by cumulative operator fatigue and limited procedural capacity. This is an interesting and practical hypothesis, although it was not examined in the current study. Recognizing this factor is valuable, as it highlights a potential systemic contributor to procedural success that warrants further investigation.
This study had several limitations. First, its retrospective design is inherently subject to selection bias and limits causal inference. Exclusion of patients with cholangitis and the limited use of ML restrict generalizability. Second, assessment of cholangiographic parameters on MRCP and ERCP, including stone impaction, stone location, and CBD strictures, relied on interpretations by different endoscopists, introducing potential subjectivity. Third, long-term clinical outcomes such as symptom recurrence, need for repeat interventions, and delayed complications were not systematically captured, precluding assessment of the downstream impact of incomplete duct clearance. Furthermore, the moderate sample size limited the complexity of multivariable modelling and may have reduced the ability to detect weaker predictors. This study used an occlusion cholangiogram as a study endpoint, which reflects routine clinical practice; however, it has been shown that an occlusion cholangiogram may miss residual bile duct stones that MRCP might detect. Previous studies have reported residual CBD stone rates after complete clearance at ERCP ranging from 4.8% to 13.5%[27,28]. These limitations should be considered when interpreting the findings. Despite these limitations, this study has several strengths. The consistent procedural techniques and operator experience strengthened the internal validity of our findings. It emphasizes cholangiographic predictors identifiable during ERCP, which are immediately available to the endoscopist. This real-time, intra-procedural assessment distinguishes the present study from previous studies that focused predominantly on pre-procedural clinical or radiologic factors and supports timely escalation to advanced endoscopic techniques. Identification of ERCP-related predictors of incomplete CBD stone clearance addresses a significant and underexplored gap in endoscopic practice.
This study emphasizes practical steps to improve stone clearance outcomes during index ERCP. Incorporating routine pre-procedural MRCP review, particularly to evaluate CBD diameter, stone size, stone-to-duct ratios, and to identify possible strictures, can help triage cases to the appropriate expertise and equipment needed. Intra-procedural cholangiographic assessment should guide the immediate strategy, with early ML or SOC-guided lithotripsy considered when stones appear impacted, are disproportionately large relative to the CBD, or are located in difficult proximal segments. Finally, multicenter prospective studies are needed to validate these findings and identify predictors of incomplete CBD stone clearance. Future studies should also include long-term follow-up and outcomes for patients who do not achieve complete CBD clearance.
| 1. | Collins C, Maguire D, Ireland A, Fitzgerald E, O'Sullivan GC. A prospective study of common bile duct calculi in patients undergoing laparoscopic cholecystectomy: natural history of choledocholithiasis revisited. Ann Surg. 2004;239:28-33. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 409] [Cited by in RCA: 333] [Article Influence: 15.1] [Reference Citation Analysis (0)] |
| 2. | Hakuta R, Hamada T, Nakai Y, Oyama H, Kanai S, Suzuki T, Sato T, Ishigaki K, Saito K, Saito T, Takahara N, Mizuno S, Kogure H, Watadani T, Tsujino T, Tada M, Abe O, Isayama H, Koike K. Natural history of asymptomatic bile duct stones and association of endoscopic treatment with clinical outcomes. J Gastroenterol. 2020;55:78-85. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 41] [Article Influence: 6.8] [Reference Citation Analysis (2)] |
| 3. | Miura F, Okamoto K, Takada T, Strasberg SM, Asbun HJ, Pitt HA, Gomi H, Solomkin JS, Schlossberg D, Han HS, Kim MH, Hwang TL, Chen MF, Huang WS, Kiriyama S, Itoi T, Garden OJ, Liau KH, Horiguchi A, Liu KH, Su CH, Gouma DJ, Belli G, Dervenis C, Jagannath P, Chan ACW, Lau WY, Endo I, Suzuki K, Yoon YS, de Santibañes E, Giménez ME, Jonas E, Singh H, Honda G, Asai K, Mori Y, Wada K, Higuchi R, Watanabe M, Rikiyama T, Sata N, Kano N, Umezawa A, Mukai S, Tokumura H, Hata J, Kozaka K, Iwashita Y, Hibi T, Yokoe M, Kimura T, Kitano S, Inomata M, Hirata K, Sumiyama Y, Inui K, Yamamoto M. Tokyo Guidelines 2018: initial management of acute biliary infection and flowchart for acute cholangitis. J Hepatobiliary Pancreat Sci. 2018;25:31-40. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 366] [Cited by in RCA: 320] [Article Influence: 40.0] [Reference Citation Analysis (2)] |
| 4. | Crockett SD, Wani S, Gardner TB, Falck-Ytter Y, Barkun AN; American Gastroenterological Association Institute Clinical Guidelines Committee. American Gastroenterological Association Institute Guideline on Initial Management of Acute Pancreatitis. Gastroenterology. 2018;154:1096-1101. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 757] [Cited by in RCA: 617] [Article Influence: 77.1] [Reference Citation Analysis (3)] |
| 5. | IAP/APA/EPC/IPC/JPS Working Group. International Association of Pancreatology Revised Guidelines on Acute Pancreatitis 2025: Supported and Endorsed by the American Pancreatic Association, European Pancreatic Club, Indian Pancreas Club, and Japan Pancreas Society. Pancreatology. 2025;25:770-814. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 45] [Article Influence: 45.0] [Reference Citation Analysis (3)] |
| 6. | Kim J, Lee YS, Lee JC, Hwang JH. Choledocholithiasis as a risk factor for cholangiocarcinoma: a nationwide retrospective cohort study. BMC Gastroenterol. 2025;25:138. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 7. | Sivanesan U, Varma V, Lee SY. Pyogenic hepatic abscesses secondary to choledocholithiasis eight years post-cholecystectomy: A case report. Eur J Radiol Open. 2020;7:100292. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 8. | Kukar M, Wilkinson N. Surgical Management of Bile Duct Strictures. Indian J Surg. 2015;77:125-132. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 9] [Article Influence: 0.7] [Reference Citation Analysis (1)] |
| 9. | Manes G, Paspatis G, Aabakken L, Anderloni A, Arvanitakis M, Ah-Soune P, Barthet M, Domagk D, Dumonceau JM, Gigot JF, Hritz I, Karamanolis G, Laghi A, Mariani A, Paraskeva K, Pohl J, Ponchon T, Swahn F, Ter Steege RWF, Tringali A, Vezakis A, Williams EJ, van Hooft JE. Endoscopic management of common bile duct stones: European Society of Gastrointestinal Endoscopy (ESGE) guideline. Endoscopy. 2019;51:472-491. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 587] [Cited by in RCA: 456] [Article Influence: 65.1] [Reference Citation Analysis (2)] |
| 10. | Sivak MV Jr. Endoscopic management of bile duct stones. Am J Surg. 1989;158:228-240. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 75] [Cited by in RCA: 62] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 11. | Kim HJ, Choi HS, Park JH, Park DI, Cho YK, Sohn CI, Jeon WK, Kim BI, Choi SH. Factors influencing the technical difficulty of endoscopic clearance of bile duct stones. Gastrointest Endosc. 2007;66:1154-1160. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 104] [Cited by in RCA: 92] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 12. | Kamuni A, Kumar L, Giri S, Angadi S, Nanjegowda SK, Bhrugumalla S. Predictors Of Failure Of Endoscopic Retrograde Cholangiopancreatography In Clearing Bile Duct Stones During Index Procedure - A Prospective Study. Arq Gastroenterol. 2024;61:e23112. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 6] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 13. | El Menabawey T, Mulay A, Graham D, Phillpotts S, Sethi A, Webster GJ. Predictors of success of conventional ERCP for bile duct stones and need for single-operator cholangioscopy. Endosc Int Open. 2023;11:E943-E951. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 9] [Reference Citation Analysis (0)] |
| 14. | Troncone E, Mossa M, De Vico P, Monteleone G, Del Vecchio Blanco G. Difficult Biliary Stones: A Comprehensive Review of New and Old Lithotripsy Techniques. Medicina (Kaunas). 2022;58:120. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 50] [Cited by in RCA: 42] [Article Influence: 10.5] [Reference Citation Analysis (1)] |
| 15. | DeLong ER, DeLong DM, Clarke-Pearson DL. Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics. 1988;44:837-845. [PubMed] [DOI] [Full Text] |
| 16. | Sabbah M, Nakhli A, Bellil N, Ouakaa A, Bibani N, Trad D, Elloumi H, Gargouri D. Predictors of failure of endoscopic retrograde pancreatocholangiography during common bile duct stones. Heliyon. 2020;6:e05515. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 11] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 17. | Aujla UI, Ladep N, Dwyer L, Hood S, Stern N, Sturgess R. Endoscopic papillary large balloon dilatation with sphincterotomy is safe and effective for biliary stone removal independent of timing and size of sphincterotomy. World J Gastroenterol. 2017;23:8597-8604. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 13] [Cited by in RCA: 16] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 18. | Wan XJ, Xu ZJ, Zhu F, Li L. Success rate and complications of endoscopic extraction of common bile duct stones over 2 cm in diameter. Hepatobiliary Pancreat Dis Int. 2011;10:403-407. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 10] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 19. | Üsküdar O, Parlak E, Dışıbeyaz S, Köksal AS, Cıçek B, Kılıç ZM, Ödemiş B, Şaşmaz N. Major predictors for difficult common bile duct stone. Turk J Gastroenterol. 2013;24:423-429. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 11] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 20. | Almadi MA, Eltayeb M, Thaniah S, Alrashed F, Aljebreen MA, Alharbi OR, Azzam N, Aljebreen AM. Predictors of failure of endoscopic retrograde cholangiography in clearing bile duct stone on the initial procedure. Saudi J Gastroenterol. 2019;25:132-138. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 14] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 21. | Ramírez García J. [Factors related to therapeutic failure in the extraction of bile duct stones for endoscopic retrograde colangiopancreatography ERCP]. Rev Gastroenterol Peru. 2011;31:330-334. [PubMed] |
| 22. | Ödemiş B, Kuzu UB, Öztaş E, Saygılı F, Suna N, Coskun O, Aksoy A, Sırtaş Z, Arı D, Akpınar Y. Endoscopic Management of the Difficult Bile Duct Stones: A Single Tertiary Center Experience. Gastroenterol Res Pract. 2016;2016:8749583. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 10] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 23. | Garg PK, Tandon RK, Ahuja V, Makharia GK, Batra Y. Predictors of unsuccessful mechanical lithotripsy and endoscopic clearance of large bile duct stones. Gastrointest Endosc. 2004;59:601-605. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 117] [Cited by in RCA: 95] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 24. | Wongkanong C, Patumanond J, Ratanachu-Ek T, Junrungsee S, Tantraworasin A. Common bile duct stone-related parameters and their potential prognostic values for stone extraction requiring endoscopic papillary large balloon dilation. JGH Open. 2023;7:16-23. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 25. | Maydeo AP, Rerknimitr R, Lau JY, Aljebreen A, Niaz SK, Itoi T, Ang TL, Reichenberger J, Seo DW, Ramchandani MK, Devereaux BM, Lee JK, Goenka MK, Sud R, Nguyen NQ, Kochhar R, Peetermans J, Goswamy PG, Rousseau M, Bhandari SP, Angsuwatcharakon P, Tang RSY, Teoh AYB, Almadi M, Lee YN, Moon JH; SpyGlass AMEA Registry Group. Cholangioscopy-guided lithotripsy for difficult bile duct stone clearance in a single session of ERCP: results from a large multinational registry demonstrate high success rates. Endoscopy. 2019;51:922-929. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 41] [Article Influence: 5.9] [Reference Citation Analysis (0)] |
| 26. | Facciorusso A, Gkolfakis P, Ramai D, Tziatzios G, Lester J, Crinò SF, Frazzoni L, Papanikolaou IS, Arvanitakis M, Blero D, Lemmers A, Eisendrath P, Fuccio L, Triantafyllou K, Gabbrielli A, Devière J. Endoscopic Treatment of Large Bile Duct Stones: A Systematic Review and Network Meta-Analysis. Clin Gastroenterol Hepatol. 2023;21:33-44.e9. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 29] [Article Influence: 9.7] [Reference Citation Analysis (0)] |
| 27. | Fujita A, Nakahara K, Michikawa Y, Morita R, Suetani K, Sato J, Igarashi Y, Araki R, Ikeda H, Matsunaga K, Watanabe T, Itoh F. Pancreatic duct guidewire placement for biliary cannulation as a risk factor for stone residue after endoscopic transpapillary stone removal. BMC Gastroenterol. 2020;20:285. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 7] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 28. | Wang X, Dai C, Jiang Z, Zhao L, Wang M, Ma L, Tan X, Liu L, Wang X, Fan Z. Endoscopic retrograde cholangiopancreatography versus laparoscopic exploration for common bile duct stones in post-cholecystectomy patients: a retrospective study. Oncotarget. 2017;8:82114-82122. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 5] [Article Influence: 0.6] [Reference Citation Analysis (0)] |